BGD Tutorial - Applied Embryology and Teratology
| Embryology - 2 May 2026 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
This Medicine Phase 2 tutorial introduces the topics of Applied Embryology and Teratology. This one and a half hour presentation uses your existing knowledge of normal human development in an applied clinical manner in relation to our existing knowledge of teratogens. In addition, you should begin considering the variables that will not change and those that will in future medical practice. Due to time limitations, only a brief coverage can be given of any one topic
Self-Directed Learning boxes on this page will not be discussed within the tutorial. You should also return here and later work through the linked online resources for more detailed descriptions and an understanding of these issues. This current page appears in the lefthand menu under Medicine as BGD 2 Tutorial.
Tinycc page - http://tiny.cc/BGD2_Tutorial
Similar content was covered in the previous online tutorials in
2019 | 2018 | 2018 PDF | 2017 | 2016 | 2015 | 2014 | 2012 | 2015 PDF | 2014 PDF | 2012 PDF | 2011 PDF and 2010.
| Whats in the News? | ||
|---|---|---|
|
Maternal deaths in Australia 2015-2017[1]
 Endocrine disrupting chemicals historical timeline[3]
| ||
This edition brings together the two previous modules and contains updates of a number of topics from them, including weight and body mass index (weight monitoring reviewed), fetal growth and wellbeing, risk of preterm birth, risk of pre-eclampsia (risk factors and prediction reviewed), family violence, hyperglycaemia (early testing reviewed), hepatitis C, thyroid dysfunction, vitamin D status and chromosomal anomalies (cell- free DNA testing reviewed). The new topic substance use has also been incorporated. See also The Australian Immunisation Handbook 10th edition (2015) Canberra: Australian Government Department of Health. ISBN: 978-1-74241-861-2 Online ISBN: 978-1-74241-862-9.. | ||
|
Objectives
Applied Embryology: birth statistics, unintended pregnancies, ART, abnormalities statistics, timeline of development, trophoblastic disease, embryonic development, placenta, fetal development, maternal diet, multiple pregnancies.
Teratology: definitions, critical periods, medications, chromosomal abnormalities, environmental factors and infections.
Textbooks

|
Moore, K.L., Persaud, T.V.N. & Torchia, M.G. (2015). The developing human: clinically oriented embryology (10th ed.). Philadelphia: Saunders. UNSW Students have online access to the current 10th edn. through the UNSW Library subscription.
|
|
Schoenwolf, G.C., Bleyl, S.B., Brauer, P.R., Francis-West, P.H. & Philippa H. (2015). Larsen's human embryology (5th ed.). New York; Edinburgh: Churchill Livingstone. UNSW Students have online access to the current 5th edn. through the UNSW Library subscription. |
Applied Embryology

The data below is based the 2016 data[2] and will be updated to the more recent 2017 data (published 2019). Earlier report data summaries are also available.[3][4][5][6][7][8][9]
This data should help you as a clinician and researcher to understand the current trends in reproductive medicine within Australia. Also see recent general population data in Australian Statistics.
|
|
Mothers
| Mothers - 2015 |
|---|
|
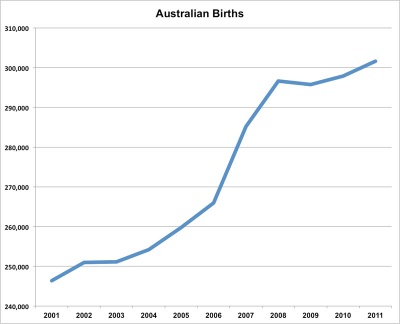
304,268 women gave birth in Australia — an increase of 13% since 2005 (267,795 women). Rate of women giving birth 62 per 1,000 women of reproductive age (15–44 years)
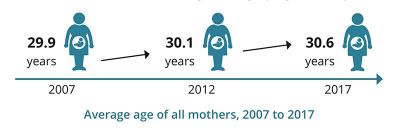
Average age of all women who gave birth continues to rise and was 30.6 (2017), compared with 29.7 in 2005.
The average age has also increased for Aboriginal and Torres Strait Islander mothers, from 24.9 in 2005 to 25.6 in 2015, with a median of 25 years. The proportion of mothers aged 35 and over has increased from 20% in 2005 to 22% (See also USA Data) The proportion of mothers aged under 25 has decreased from 19% to 15%. The average age of first‐time mothers also increased, from 28.1 in 2005 to 28.9 Multiple pregnancies - represented 1.5% of all pregnancies.
|
| Maternal Conditions |
|
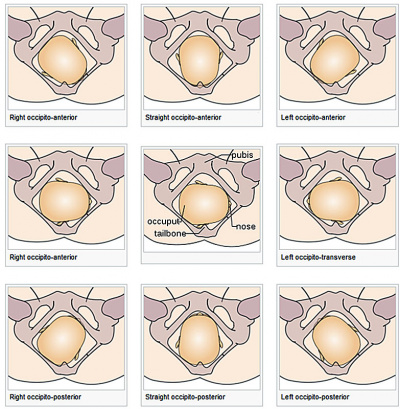
Birth - cephalic presentations
|
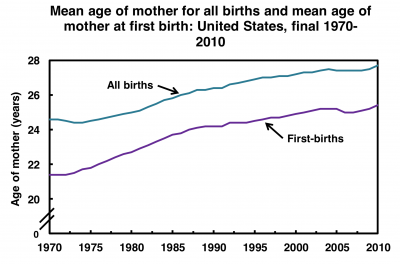
USA mean age of mother (1970-2010) |
Babies
| Babies |
|---|
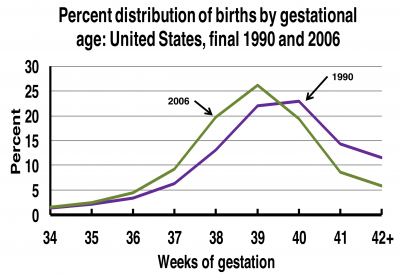
| Gestational Age |
|
| Birth Weight |
|
| Apgar Score |
Apgar score of 7 or more
|
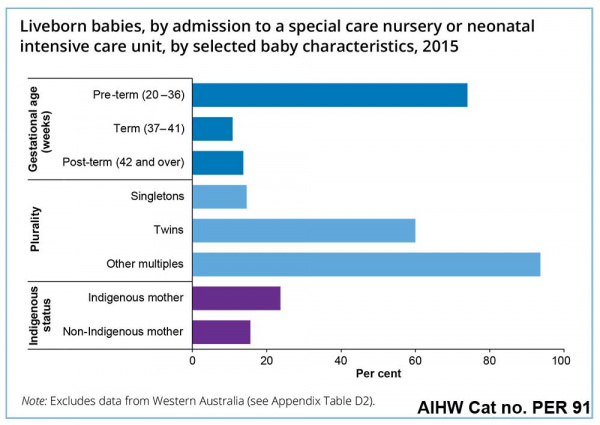
| Special care nurseries (SCN) or neonatal intensive care units (NICU) Admissions |
|
| stillbirth and perinatal death perinatal mortality |
2013 and 2014 - 622,037 babies were born in Australia and 6,037 of those babies died in the perinatal period
|
| 2013 National core maternity indicators |
|---|
|
2013 National core maternity indicators[10] This report provides a baseline for monitoring changes in the quality of maternity services across Australia using 10 national core maternity indicators.
|
Unintended Pregnancy
A recent 2018 USA study[11] of Unintended pregnancy and interpregnancy interval by maternal age, National Survey of Family Growth.
- 40% of pregnancies were unintended
- 36% followed an interpregnancy interval (IPI) less than 18 months.
- Within each maternal age group, the percentage of pregnancies that were unintended decreased as IPI increased.
Unintended pregnancy is either mistimed (woman wanted to be pregnant later) or unwanted (did not want to ever be pregnant).
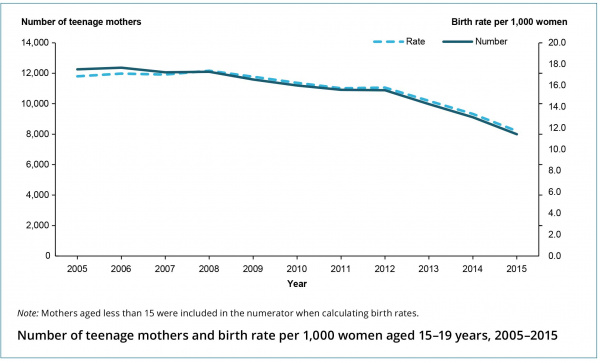
Australian Teenage Pregnancy Statistics (2015) AIHW
- Rate of teenage births in Australia is in decline, from 17.5 births per 1,000 women in 2005 to 11.4 in 2015
- Babies of teenage mothers were 1.3 times as likely to be of low birthweight than babies of 20-24 year old mothers
- Babies of teenage mothers were 1.2 times as likely to be preterm than babies of 20-24 year old mothers
- 1 in 4 teenage mothers smoked after 20 weeks of pregnancy
| Unintended and Teen Pregnancy | |
|---|---|
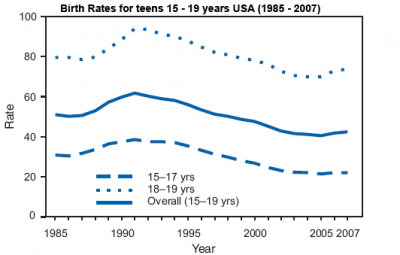
| 2001 USA - Approximately one-half of pregnancies in the United States were unintended (Finer 2006, Perspectives on Sexual and Reproductive Health).
An earlier 1995 USA National Survey of Family Growth (NSFG) found:
|
|
A recent Canadian retrospective study[12] of half a million births comparing pregnant women < 20 years of age (adolescent) were compared with those of women 20 to 35 years old.
| |
Links: CDC Unintended Pregnancy Prevention | Pregnancy Risk Assessment Monitoring System USA | The Measurement and Meaning of Unintended Pregnancy
Assisted Reproduction Technology
Assisted Reproduction Technology (ART) is also sometimes also used to identify In vitro fertilization (IVF) but now includes many new techniques. Assisted reproductive technology (ART) is a group of procedures that involve the in vitro (outside of body) handling of human oocytes (eggs) and sperm or embryos for the purposes of establishing a pregnancy. Each ART treatment involves a number of stages and is generally referred to as an ART treatment cycle. The embryos transferred to a women can either originate from the cycle in which they were created (fresh cycle) or be frozen and thawed before transfer (thaw cycle).
Assisted Reproductive Technology in Australia and New Zealand (2015)[13]
- 77,721 ART treatment cycles reported from Australian and New Zealand clinics in 2015 (71,479 and 6,242 respectively)
- 5.6% increase in Australia and 6.0% increase in New Zealand on 2014.
- 14.4 cycles per 1,000 women of reproductive age (15–44 years) in Australia
- 94.5% autologous cycles (own oocytes or embryos)
- 37.4% autologous frozen and thawed
- 39,006 women who undertook 73,481 autologous fresh and/or thaw cycles
- Over the last five years there has been an increasing trend in the proportion of cycles where all oocytes or embryos are cryopreserved for potential future use from (2011) 5.0% (2015) 17.2%
- 35.8 years - average age of women undergoing autologous cycles
- 40.6 years - average age of women undergoing ART treatment using donor oocytes or embryos
- 24.8% were aged 40 or older. The average age of the male partner of the women undergoing autologous and recipient cycles was ** 38.1 years - average age of the male partner
- 22.8% (17,726) resulted in a clinical pregnancy
- 18.1% (14,040) in a live delivery
- higher live delivery rate in younger women.
- under 30 - live delivery rate per embryo transfer 38.4% for autologous fresh cycles and 32.6% for autologous thaw cycles
- women aged over 44 - live delivery rate was 0.7% per embryo transfer for autologous fresh and 7.6% thaw cycles.
- higher live delivery rate in younger women.
- 14,791 babies born (including 14,655 liveborn babies)
- 78.8% were full-term singletons of normal birthweight.
- shift from cleavage stage transfers to blastocyst transfers (from 57.7% in 2011 to 73.5% in 2015)
- increase in vitrification as a cryopreservation method (from 73.0% of thaw blastocyst transfer cycles in 2011 to 86.1% in 2015).
- intracytoplasmic sperm injection (ICSI) has remained stable at around 63% of embryo transfer cycles in 2011-2015.
- 36% decrease in Multiple births from 6.9% in 2011 to 4.4% in 2015.
| Australia 2013 Data |
|---|
|
| Australia 2012 Data |
|
The following data from previous year
Assisted reproductive technology in Australia and New Zealand 2012[14] Nov 2014 |
| USA 2013 Data |
|---|
|
Early Development Issues
Abnormal Implantation
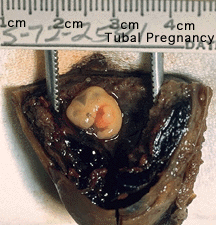
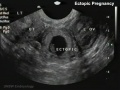
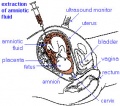
Ectopic Implantation (Pregnancy)
Abnormal implantation sites or Ectopic Pregnancy occurs if implantation is in uterine tube or outside the uterus.
Tubal pregnancy - 94% of ectopic pregnancies
|
|
This is also the most common cause of pregnancy-related deaths in the first trimester. A United Kingdom enquiry into maternal deaths[15], identified ectopic pregnancy as the fourth most common cause of maternal death (73% of early pregnancy deaths).
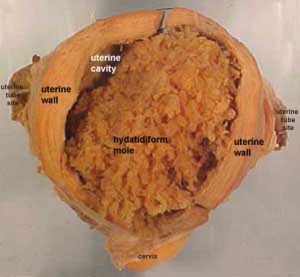
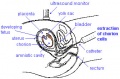
Hydatidiform Mole
Another type of abnormality is when only the conceptus trophoblast layers proliferates and not the embryoblast, no embryo develops, this is called a "hydatidiform mole", which is due to the continuing presence of the trophoblastic layer, this abnormal conceptus can also implant in the uterus. The trophoblast cells will secrete human chorionic gonadotropin (hCG), as in a normal pregnancy, and may appear maternally and by pregnancy test to be "normal". Prenatal diagnosis by ultrasound analysis demonstrates the absence of a embryo.
There are several forms of hydatidiform mole: partial mole, complete mole and persistent gestational trophoblastic tumor. Many of these tumours arise from a haploid sperm fertilizing an egg without a female pronucleus (the alternative form, an embryo without sperm contribution, is called parthenogenesis). The tumour has a "grape-like" placental appearance without enclosed embryo formation. Following a first molar pregnancy, there is approximately a 1% risk of a second molar pregnancy.
This topic is also covered in Placenta - Abnormalities
Twinning
- Twin deliveries and place of birth in NSW 2001-2005[16] "Both infant and maternal morbidity increase from 39 weeks gestation. Delivery of twins before 36 weeks at smaller hospitals (< 500 deliveries per annum) should be avoided. A twin pregnancy where there is a greater or equal to 20% difference in estimated fetal weights should be considered for referral to a tertiary obstetric unit."
Dizygotic Twinning
Dizygotic twins (fraternal, non-identical) arise from separate fertilization events involving two separate oocyte (egg, ova) and spermatozoa (sperm). Dizygotic twinning can be increased by Assisted Reproductive Technologies (ART) that use double embryo transfer techniques.
Monoygotic Twinning
Monoygotic twins (identical) produced from a single fertilization event (one fertilised egg and a single spermatazoa, form a single zygote), these twins therefore share the same genetic makeup. Occurs in approximately 3-5 per 1000 pregnancies, more commonly with aged mothers. The later the twinning event, the less common are initially separate placental membranes and finally resulting in conjoined twins.
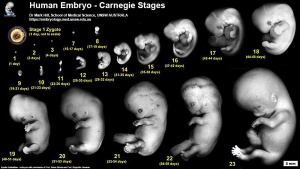
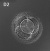
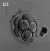
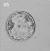
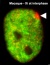
| Week | Week 1 (GA week 3) | Week 2 (GA week 4) | |||||||||||||
| Day | 0 | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 |
| Cell Number | 1 | 1 | 2 | 16 | 32 | 128 | bilaminar | ||||||||
| Event | Ovulation | Fertilization | First cell division | Morula | Early blastocyst | Late blastocyst
Hatching |
Implantation starts | X inactivation | |||||||
|
|
|
|
||||||||||||
| Monoygotic
Twin Type |
Diamniotic
Dichorionic |
Diamniotic
Monochorionic |
Monoamniotic
Monochorionic |
Conjoined | |||||||||||
Table based upon recent a recent twinning review.[17] Links: twinning
- Links: Twinning
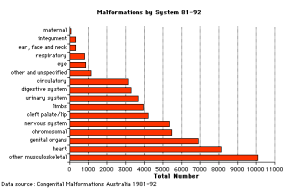
Abnormal Development
Embryological development is a robust biological system able to cope with many stresses without long-term consequences. When development does go wrong there are generally 3 major types groups: Genetic (inherited), Environmental (maternal) derived and Unknown (not determined or known) abnormalities. Also often not considered, is that pregnancy itself can also expose abnormalities in the mother (congenital heart disease, diabetes, reproductive disorders) that until the pregnancy had gone undetected.
Genetic abnormalities in medicine are still mainly about determining a family history and good prenatal/neonatal diagnosis. Realise that there exists in all of us genetic variations and some variations which eventually expand be expressed as a genetic disorder (CAG expansions).
| Abnormality Links | ||||
|---|---|---|---|---|
|
Prenatal diagnosis are the clinical tools used to determine both normal and abnormal development. There are a growing number of new diagnostic techniques that are being applied to human embryonic development.
| Prenatal Diagnosis Links | |
|---|---|
|
| NIPT - Non-Invasive Prenatal Testing |
|---|
| Fetal aneuploidy screening with cell-free DNA in late gestation[18]"The aim of this study was to evaluate clinical use of NIPT at gestational ages of 23 weeks and above. A cohort of 5579 clinical patients with singleton gestations of 23 weeks or greater submitting a blood sample for NIPT in an 18-month period were selected for this study. ...Of 5372 reported late-gestation samples, 151 (2.8%) were reported as aneuploidy detected or suspected. In late-gestation samples, the overall observed positive predictive value (PPV) for NIPT was 64.7%, with an observed PPV of 100% in the subset of cases with multiple clinical indications including abnormal ultrasound findings. NIPT is a highly accurate prenatal screening option for women after 23 weeks of gestation. Women who presented for NIPT in the latter stages of pregnancy more frequently specified clinical indications of abnormal ultrasound findings than women who entered screening earlier in pregnancy."
More? Fetal Cells in Maternal Blood | RACGP | NCHPEG |
While genetic abnormalities will have well-defined impacts upon development, environmentally derived effects can be harder to define and often variable depending on many different factors (timing, exposure level, and the combination effects with other factors). This combination effect can also be seen between genetic and environmental interacting to give an even broader spectrum of both major and minor abnormalities.
| Environmental Links | ||||||
|---|---|---|---|---|---|---|
|
International Classification of Diseases
The International Classification of Diseases (ICD) World Health Organization's classification used worldwide as the standard diagnostic tool for epidemiology, health management and clinical purposes. This includes the analysis of the general health situation of population groups. It is used to monitor the incidence and prevalence of diseases and other health problems. Within this classification "congenital malformations, deformations and chromosomal abnormalities" are (Q00-Q99) but excludes "inborn errors of metabolism" (E70-E90).
Australian Birth Anomalies System
- "The national collation and reporting of birth anomalies data has been suspended in recent years due to concerns about data quality and comparability."
- Variability among states and territories in scope of birth anomalies data collections: sources of birth anomalies notifications and definitions and classifications used; method of data collection and available resources.
- Variability among the states and territories in the timing and method of the provision of birth anomalies data to the AIHW National Perinatal Statistics Unit (NPSU) for national collation and reporting.
- New Australian Birth Anomalies System should be data for birth anomalies detected up to 1 year of age
- including data on terminations of pregnancies with birth anomalies and regardless of gestational age (i.e. including less than 20 weeks gestation)
- System will initially be based on data from the states able to detect birth anomalies at least up to 1 year of age (NSW, VIC, WA and SA), further extending the period of detection in the future.
- Congenital anomalies are coded using the British Paediatric Association Classification of Diseases (ICD-9-BPA), based on the International Classification of Diseases, 9th Revision (ICD-9).
- The Australian Congenital Anomalies Monitoring System (ACAMS) supersedes the National Congenital Malformations and Birth Defects Data Collection (NCM&BD).
| Congenital Anomalies in Australia 2002-2003 |
|---|
Congenital anomalies in Australia 2002-2003[19] was published in 2008 as part a new revised series on 33 selected congenital anomalies also monitored internationally by the International Clearinghouse of Birth Defects Surveillance and Research.
|
| External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation. |
Links: Australian Congenital Anomalies Monitoring System | Congenital Anomalies in Australia 2002-2003
NSW Data
Congenital Conditions Register
Scheduled congenital conditions (section 2) detected during pregnancy or in infants up to one year of age in NSW are required to be reported under the NSW Public Health Act 1991.
Scheduled congenital conditions include:
- All structural malformations. Examples include spina bifida, microcephaly, transposition of the great vessels, ventricular septal defects, pulmonary agenesis, polycystic lungs, duodenal atresia, exomphalos, hypospadias, cleft lip/palate, microphthalmia, limb reductions, polydactyly, birthmarks greater than 4 cms diameter, cystic hygroma and multisystem syndromes including at least one structural malformation.
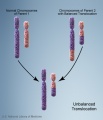
- Chromosomal abnormalities. Examples include Down syndrome and unbalanced translocations.
- Four medical conditions: cystic fibrosis, phenylketonuria, congenital hypothyroidism and thalassaemia major.
Congenital conditions that are not notifiable include:
- Minor anomalies occurring in isolation (Examples of minor anomalies include skin tags, deviated nasal septum, tongue tie, benign heart murmurs, clicky non-dislocating hips, sacral dimples, positional talipes, abnormal palmar creases, dysmorphic features).
- Birth injuries.
- Congenital infections which do not result in a structural malformation.
- Tumours and cysts.
- Conditions arising from prematurity or asphyxiation.
Links: NSW Health - Congenital Conditions Register - Reporting Requirements 2012 | PDF
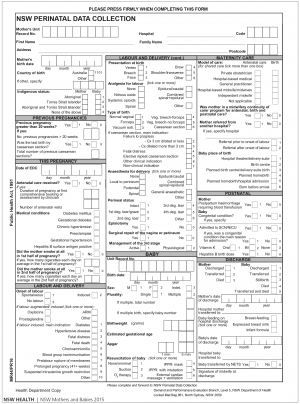
NSW Mothers and Babies Report 2015
NSW is one of the largest states in Australia by population. The New South Wales Perinatal Data Collection (PDC) is a population-based surveillance system covering all births in NSW public and private hospitals, as well as home births. It encompasses all live births, and stillbirths of at least 20 weeks gestation or at least 400 grams birth weight.[20]
- Number of births decreased from 97,245 in 2011 to 96,391 in 2015 (decrease of 0.9%).
- Percentage of teenage mothers fell from 3.2% in 2011 to 2.5% in 2015.
- Rate of normal vaginal birth decreased from 56.9% in 2011 to 56.0% in 2015.
- Operative and instrumental births were more common among privately than publicly insured mothers.
- Proportion of smoking mothers during pregnancy declined from 11.1% in 2011 to 8.9% in 2015.
- Majority of mothers planned to give birth in a hospital labour ward
- 87% per cent of mothers who planned to give birth in a birth centre actually did so.
- There were 187 homebirths in NSW reported in 2015.
- Premature babies (less than 37 weeks gestation) 7.9% (slight increase from 7.5% in 2011).
- Since 2011, the rate of low birth weight (less than 2,500 grams) has remained stable, ranging from 6.1% to 6.6%.
- Low birth weight rate was 6.6% in 2015.
- Between 2011 and 2015, the reported number of Aboriginal or Torres Strait Islander mothers giving birth increased from 2,975 to 3,823, an increase from 3.1% to 4.0% of all mothers.
- Aboriginal or Torres Strait Islander
- teenage mothers fell from 19.0% in 2011 to 15.4% in 2015.
- 45.0% of Aboriginal or Torres Strait Islander mothers reported smoking during pregnancy.
- Since 2011, rates of low birth weight and prematurity in Aboriginal or Torres Strait Islander babies has been over 11%. In 2015, 11.3% of Aboriginal or Torres Strait Islander babies were low birth weight and 12.7% were premature.
- Perinatal mortality rate of 9.6 per 1,000 births in Aboriginal or Torres Strait Islander mothers in 2015 is higher than the rate of 8.1 per 1,000 births experienced among babies born to non-Aboriginal or Torres Strait Islander mothers.
| Victoria - 10 most reported birth anomalies | |
|---|---|
| Based upon statistics from the Victorian Perinatal Data Collection Unit in Victoria between 2003-2004. | |
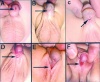
|
hypospadias (More? External Genital Male Development Movie) |

|
Obstructive Defects of the Renal Pelvis (obstructive defects of the renal pelvis, uteropelvic junction obstruction, pelvo-uterero junction obstruction) Term describing a developmental renal abnormality due to partial or complete blockage of the drainage of the kidney pelvis requiring surgical correction. The blockage can also have several causes including: unusual ureter twisting or bending, ureter compression by a blood vessel, malformations of the muscular wall. The blockage leads to an accumulation of urine in the affected region, with several potential effects: nephron damage from compression (hydronephrosis); decreased urine output leading to lack of amniotic fluid (oligohydramnios); respiratory development effects due to the lack of amniotic fluid.
(More? renal abnormalities | renal) |
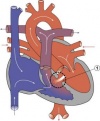
|
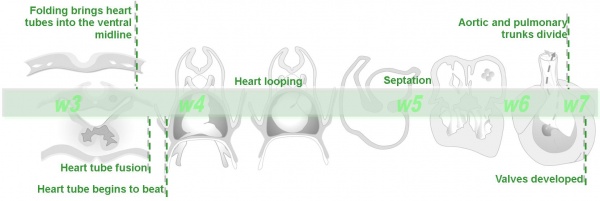
ventricular septal defect (More? ventricular septal defect)
Heart Development Timeline (see Basic Cardiac Embryology) |
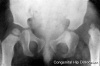
|
Developmental dysplasia of the hip or Congenital Dislocated Hip
(Developmental dysplasia of the hip (DDH), congenital hip dislocation, congenital hip dysplasia) Term describes a spectrum of musculoskeletal disorders of hip instability due either to the femoral head being able to move outside the acetabulum (luxation or dislocation), or abnormally within the acetabulum (subluxation or partial dislocation). This includes presentation following a normal examination of the hips in the newborn period (Ortolani and Barlow tests). When detected can be managed with splinting (Denis-Browne splint) allows the hip joint to develop normally and does not require surgery. If undetected and left untreated, the hip joint develops abnormally and surgical reduction is required. (More? Pelvis Development) |
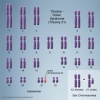
|
Trisomy 21 or Down syndrome - The most common genetic abnormality. (More? Trisomy 21) |
|
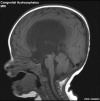
hydrocephalus rapid increase in head circumference or an unusually large head size due to excessive accumulation of cerebrospinal fluid in the brain.(More? hydrocephalus | Neural Abnormalities | NINDS - Hydrocephalus Fact Sheet | Hydrocephalus Support Association | USA National Hydrocephalus Foundation) |
|
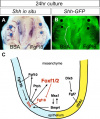
cleft palate - The palate separates the nasal cavity from the oral cavity, the abnormality has many different causes, and occurs more frequently in females (57%) than in males (43%). (More? cleft palate) |
|
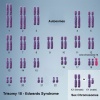
Trisomy 18 or Edward Syndrome - multiple abnormalities of the heart, diaphragm, lungs, kidneys, ureters and palate 86% discontinued (More? Trisomy 18) |
| Renal Agenesis/Dysgenesis - reduction in neonatal death and stillbirth since 1993 may be due to the more severe cases being identified in utero and being represented amongst the increased proportion of terminations (approximately 31%). (More? Renal Abnormalities - Renal Agenesis) | |
|
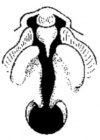
cleft lip and palate - occur with another defect in 33.7% of cases.(More? cleft lip and palate) |
| Links: Human Abnormal Development | Australian Statistics | Victoria 2004 | USA 2006 | Europe 2010 | |
| USA Statistics | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| European Statistics | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Genetic
Teratology
Prenatal Screening
How and why do things go wrong in development?
These notes cover abnormalities that can occur during development often described as congenital defects or birth defects. There are many different ways that developmental abnormalities can occur the 3 major types are Genetic (inherited), Environmental (maternal) and Unknown (not determined) derived abnormalities. The environmental factors that cause or lead to any of these abnormalities are described as Teratogens.
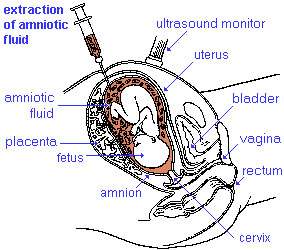
| Diagnosis Links: Prenatal Diagnosis | pregnancy test | amniocentesis | chorionic villus sampling | ultrasound | Alpha-Fetoprotein | Pregnancy-associated plasma protein-A | Fetal Blood Sampling | Magnetic Resonance Imaging | Computed Tomography | Non-Invasive Prenatal Testing | Fetal Cells in Maternal Blood | Preimplantation Genetic Screening | Comparative Genomic Hybridization | Genome Sequencing | Neonatal Diagnosis | Category:Prenatal Diagnosis | Fetal Surgery | Classification of Diseases | Category:Neonatal Diagnosis |
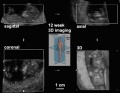
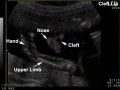
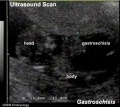
| Ultrasound | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
Ultrasound
|
Now consider the terms used to describe the different environmental effects that can occur during pregnancy that may influence outcomes.
- Teratogen (Greek, teraton = monster) any agent that causes a structural abnormality (congenital abnormalities) following fetal exposure during pregnancy. The overall effect depends on dosage and time of exposure.
- Absolute risk the rate of occurrence of an abnormal phenotype among individuals exposed to the agent. (e.g. fetal alcohol syndrome)
- Relative risk the ratio of the rate of the condition among the exposed and the nonexposed. (e.g. smokers risk of having a low birth weight baby compared to non-smokers) A high relative risk may indicate a low absolute risk if the condition is rare.
- Mutagen a chemical or agent that can cause permanent damage to the deoxyribonucleic acid (DNA) in a cell. DNA damage in the human egg or sperm may lead to reduced fertility, spontaneous abortion (miscarriage), birth defects and heritable diseases.
- Fetotoxicant is a chemical that adversely affects the developing fetus, resulting in low birth weight, symptoms of poisoning at birth or stillbirth (fetus dies before it is born).
- Synergism when the combined effect of exposure to more than one chemical at one time, or to a chemical in combination with other hazards (heat, radiation, infection) results in effects of such exposure to be greater than the sum of the individual effects of each hazard by itself.
- Toxicogenomics the interaction between the genome, chemicals in the environment, and disease. Cells exposed to a stress, drug or toxicant respond by altering the pattern of expression of genes within their chromosomes. Based on new genetic and microarray technologies.
Teratogens
- Infections, collectively grouped under the acronym TORCH for Toxoplasmosis, Other organisms (parvovirus, HIV, Epstein-Barr, herpes 6 and 8, varicella, syphilis, enterovirus) , Rubella, Cytomegalovirus and Hepatitis. See also the related topics on maternal hyperthermia and bacterial infections. (More? Postnatal Immunisation)
- Maternal diet the best characterised is the role of low folic acid and Neural Tube Defects (NTDs) see also abnormal neural development and Neural Tube Defects (NTDs). More recently the focus has been on dietary iodine levels and the role they also play on neural development.
- Maternal drugs effects either prescription drugs (therapeutic chemicals/agents, thalidomide limb development), non-prescription drugs (smoking), and illegal drugs (Cannabis/Marijuana, Methamphetamine/Amphetamine, Cocaine, Heroin, Lysergic Acid Diethylamide)
- Environment (smoking, chemicals, heavy metals, radiation) and maternal endocrine function (maternal diabetes, thyroid development) and maternal stress.
- Teratogen synergism, different environmental effects can act individually or in combination on the same developing system. For example, neural development can be impacted upon by alcohol (fetal alcohol syndrome), viral infection (rubella) and/or inadequate dietry folate intake (neural tube defects). These effects may also not be seen as a direct effect on a system or systems but result in a reduced birth weight and the potential postnatal developmental effects. Consider also this in relation to the increasing support to the fetal origins hypothesis.
- Alcohol - In utero alcohol effects on foetal, neonatal and childhood lung disease.[21]
Links:
| Abnormality Links: abnormal development | abnormal genetic | abnormal environmental | Unknown | teratogens | ectopic pregnancy | cardiovascular abnormalities | coelom abnormalities | endocrine abnormalities | gastrointestinal abnormalities | genital abnormalities | head abnormalities | integumentary abnormalities | musculoskeletal abnormalities | limb abnormalities | neural abnormalities | neural crest abnormalities | placenta abnormalities | renal abnormalities | respiratory abnormalities | hearing abnormalities | vision abnormalities | twinning | Developmental Origins of Health and Disease | ICD-11 | ||
|
| Environmental Links: Introduction | low folic acid | iodine deficiency | Nutrition | Drugs | Australian Drug Categories | USA Drug Categories | thalidomide | herbal drugs | Illegal Drugs | smoking | Fetal Alcohol Syndrome | TORCH | viral infection | bacterial infection | fungal infection | zoonotic infection | toxoplasmosis | Malaria | maternal diabetes | maternal hypertension | maternal hyperthermia | Maternal Inflammation | Maternal Obesity | hypoxia | biological toxins | chemicals | heavy metals | air pollution | radiation | Prenatal Diagnosis | Neonatal Diagnosis | International Classification of Diseases | Fetal Origins Hypothesis |
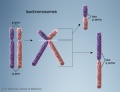
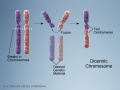
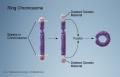
| Genetic Links: genetic abnormalities | maternal age | Trisomy 21 | Trisomy 18 | Trisomy 13 | Trisomy X | trisomy mosaicism | Monosomy | Fragile X | Williams | Alagille | Philadelphia chromosome | mitochondria | VACTERL | hydatidiform mole | epigenetics | Prenatal Diagnosis | Neonatal Diagnosis | meiosis | mitosis | International Classification of Diseases | genetics |
Critical Periods of Development
- Finally, when studying this topic remember the concept of critical periods of development that will affect the overall impact of the above listed factors. This can be extended to the potential differences between prenatal and postnatal effects, for example with infections and outcomes.
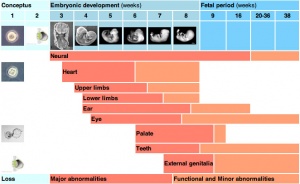
| Critical Periods of Human Development | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Conceptus | Embryonic development (weeks) | Fetal period (weeks) | ||||||||||||||||||
|
||||||||||||||||||||
| Neural | ||||||||||||||||||||
| Heart | ||||||||||||||||||||
| Upper limbs | ||||||||||||||||||||
| Lower limbs | ||||||||||||||||||||
| Ear | ||||||||||||||||||||
| Eye | ||||||||||||||||||||
| Palate | ||||||||||||||||||||
| Teeth | ||||||||||||||||||||
| External genitalia | ||||||||||||||||||||
| Loss | Major abnormalities | Functional and Minor abnormalities | ||||||||||||||||||
| ||||||||||||||||||||
Links: Embryonic Development | Timeline human development | Movie - Human Development annotated cartoon | Human - critical periods
Australian Drug Categories
Legal drugs are classified, usually by each country's appropriate regulatory body, on the safety of drugs during pregnancy. In Australia, the Therapeutic Goods Authority has classes (A, B1, B2, B3, C, D and X) to define their safety. (More? Australian Drug Categories) In the USA, since 2015 drugs are classified by the Food and Drug Administration (FDA) into new classes to define their safety. The Australian categorisation of medicines for use in pregnancy does not follow a hierarchical structure.
- Human data are lacking or inadequate for drugs in the B1, B2 and B3 categories
- Subcategorisation of the B category is based on animal data
- The allocation of a B category does not imply greater safety than a C category
- Medicines in category D are not absolutely contraindicated during pregnancy (e.g.anticonvulsants)
- Pregnancy Category A - Have been taken by a large number of pregnant women and women of childbearing age without an increase in the frequency of malformations or other direct or indirect harmful effects on the fetus having been observed.
- Pregnancy Category B1 - Drugs which have been taken by only a limited number of pregnant women and women of childbearing age, without an increase in the frequency of malformation or other direct or indirect harmful effects on the human fetus having been observed. Studies in animals have not shown evidence of an increased occurrence of fetal damage.
- Pregnancy Category B2 - Have been taken by only a limited number of pregnant women and women of childbearing age, without an increase in the frequency of malformation or other direct or indirect harmful effects on the human fetus having been observed. Studies in animals are inadequate or may be lacking, but available data show no evidence of an increased occurrence of fetal damage.
- Pregnancy Category B3 - Have been taken by only a limited number of pregnant women and women of childbearing age, without an increase in the frequency of malformation or other direct or indirect harmful effects on the human fetus having been observed. Studies in animals have shown evidence of an increased occurrence of fetal damage, the significance of which is considered uncertain in humans.
- Pregnancy Category C - Have caused or may be suspected of causing, harmful effects on the human fetus or neonate without causing malformations. These effects may be reversible.
- Pregnancy Category D - Have caused, are suspected to have caused or may be expected to cause, an increased incidence of human fetal malformations or irreversible damage. These drugs may also have adverse pharmacological effects.
- Pregnancy Category X - Have such a high risk of causing permanent damage to the fetus that they should NOT be used in pregnancy or when there is a possibility of pregnancy.
| US FDA - 2015 Pregnancy and Lactation Labeling (Drugs) 2015 |
|---|

|
| Since 2015 the labelling classes (A, B, C, D, and X) have been replaced with the new "FDA Pregnancy and Lactation Labeling Rule" (PLLR). |
| Links: USA Drug Categories | Pregnancy and Lactation Labeling (Drugs) Final Rule |
Infant Drug Clearance
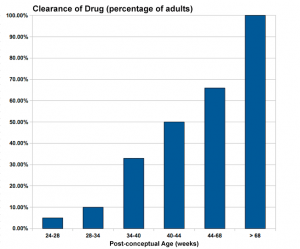
The drug clearance data below are only approximate calculated rates for the fetus and infant from NZ Drug Safety in Lactation
| Post-conceptual Age (weeks) | Clearance of Drug (percentage of adults) |
| 24-28 | 5% |
| 28-34 | 10% |
| 34-40 | 33% |
| 40-44 | 50% |
| 44-68 | 66% |
| > 68 | 100% |
Links: Abnormal Development - Drugs | Australian Fetal Risk Categories | USA FDA Fetal Risk Categories | Therapeutic Goods Authority | Australian Drug Evaluation Committee (ADEC) | TGA - Medicines Pregnancy Database | Appendix A: Therapeutic goods exempted from pregnancy classification | NSW Poisons Information Centre
References
- ↑ Australian Institute of Health and Welfare 2019. Australia’s mothers and babies 2017—in brief. Perinatal statistics series no. 35. Cat. no. PER 100. Canberra: AIHW.
- ↑ Australian Institute of Health and Welfare 2018. Australia’s mothers and babies 2016—in brief. Perinatal statistics series no. 34. Cat. no. PER 97. Canberra: AIHW.
- ↑ AIHW 2016. Australia's mothers and babies 2014—in brief. Perinatal statistics series no. 32. [ http://www.aihw.gov.au/publication-detail/?id=60129557656 Cat. no. PER 87]. Canberra: AIHW.
- ↑ AIHW 2015. Australia's mothers and babies 2013 - in brief. Perinatal statistics series no. 31. Cat. no. PER 72. Canberra: AIHW. PDF Viewed 13 December 2015. http://www.aihw.gov.au/publication-detail/?id=60129553770
- ↑ Hilder L, Zhichao Z, Parker M, Jahan S, Chambers GM 2014. Australia’s mothers and babies 2012. Perinatal statistics series no. 30. Cat. no. PER 69. Canberra: AIHW. Viewed 16 December 2014. http://www.aihw.gov.au/publication-detail/?id=60129550033
- ↑ Li Z, Zeki R, Hilder L & Sullivan EA 2013. Australia’s mothers and babies 2011. Perinatal statistics series no. 28. Cat. no. PER 59. Canberra: AIHW.
- ↑ Li Z, McNally L, Hilder L & Sullivan EA 2011. Australia's mothers and babies 2009 AIHW Perinatal statistics series no. 25 Cat. no. PER 52. Sydney: AIHW National Perinatal Epidemiology and Statistics Unit.
- ↑ Laws P & Sullivan EA 2010 Australia's mothers and babies 2008 AIHW Perinatal statistics series no. 24 Cat. no. PER 48. Sydney: AIHW National Perinatal Statistics Unit.
- ↑ Laws P & Sullivan EA 2009. Australia's mothers and babies 2007 AIHW Perinatal statistics series no. 23 Cat. no. PER 48. Sydney: AIHW National Perinatal Statistics Unit.
- ↑ AIHW National Perinatal Epidemiology and Statistics Unit and AIHW 2013. National core maternity indicators. Cat. no. PER 58. Canberra: AIHW.
- ↑ Ahrens KA, Thoma M, Copen C, Frederiksen B, Decker E & Moskosky S. (2018). Unintended pregnancy and interpregnancy interval by maternal age, National Survey of Family Growth. Contraception , , . PMID: 29501647 DOI.
- ↑ Fleming N, Ng N, Osborne C, Biederman S, Yasseen AS, Dy J, Rennicks White R & Walker M. (2013). Adolescent pregnancy outcomes in the province of Ontario: a cohort study. J Obstet Gynaecol Can , 35, 234-245. PMID: 23470111 DOI.
- ↑ Fitzgerald O, Harris K, Paul RC, Chambers GM. (2017) Assisted reproductive technology in Australia and New Zealand 2015. Sydney: National Perinatal Epidemiology and Statistics Unit, the University of New South Wales Sydney.
- ↑ Macaldowie A, Wang YA, Chughtai AA & Chambers GM 2014. Assisted reproductive technology in Australia and New Zealand 2012. Sydney: National Perinatal Epidemiology and Statistics Unit, the University of New South Wales. PDF
- ↑ Confidential Enquiry into Maternal Deaths (CEMD) Why Mothers Die 2000–2002 PDFPDF2
- ↑ Algert CS, Morris JM, Bowen JR, Giles W & Roberts CL. (2009). Twin deliveries and place of birth in NSW 2001-2005. Aust N Z J Obstet Gynaecol , 49, 461-6. PMID: 19780726 DOI.
- ↑ Hall JG. (2003). Twinning. Lancet , 362, 735-43. PMID: 12957099 DOI.
- ↑ Taneja PA, Prosen TL, de Feo E, Kruglyak KM, Halks-Miller M, Curnow KJ & Bhatt S. (2017). Fetal aneuploidy screening with cell-free DNA in late gestation. J. Matern. Fetal. Neonatal. Med. , 30, 338-342. PMID: 27124739 DOI.
- ↑ Abeywardana S & Sullivan EA 2008. Congenital anomalies in Australia 2002–2003. Birth anomalies series no. 3 Cat. no. PER 41. Sydney: AIHW National Perinatal Statistics Unit.
- ↑ Centre for Epidemiology and Evidence. New South Wales Mothers and Babies 2015. Sydney: NSW Ministry of Health, 2016.
- ↑ Gauthier TW & Brown LA. (2017). In utero alcohol effects on foetal, neonatal and childhood lung disease. Paediatr Respir Rev , 21, 34-37. PMID: 27613232 DOI.
Links
The following are links to relevant notes pages that cover the key embryology concepts in this tutorial. These pages and their links will provide further detailed information.
Applied Embryology
Timeline human development | Fetal Development | Birth | Apgar test | Neonatal Development | Week 2 Abnormalities - Trophoblastic Disease | Placenta Development | Neural Abnormalities | Abnormal Development - Folic Acid and Neural Tube Defects | Week 3 | Cardiovascular Abnormalities | Twinning | Blastocyst | Molecular Development
Teratology Links
Human Abnormal Development | Genetic Abnormalities | Environmental Factors | Drugs | Trisomy 21 (Down Syndrome) | Fetal Alcohol Syndrome | Viral Infection | Rubella Virus | Hyperthermia
Self-Directed Learning
| Self-Directed Learning 1 - Australian Statistics |
Once you have thought about the Australian statistics, now look at the latest report summary Australia’s mothers and babies 2012 and Australian Statistics.
|
| Self-Directed Learning 2 - Pregnancy |
|
| Self-Directed Learning 3 - Assisted Reproductive Technologies |
|
| Self-Directed Learning 4 - The First Few Weeks |
|
| Self-Directed Learning 5 - Abnormal Development |
|
| Self-Directed Learning 6 - Prenatal Diagnosis |
|
| Self-Directed Learning 7 - Medications in Pregnancy |
|
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- Department of Health and Ageing The National Maternity Services Plan 2010 | National Maternity Services Plan: 2010 -2011 Annual Report
- Australia AIHW National Perinatal Statistics Unit | Victorian Birth Defects Register (VBDR) | Victorian Birth Defects Register brochure
- National Perinatal Statistics Unit Congenital Anomalies Neural tube defects in Australia - An epidemiological report | Congenital Anomalies in Australia 2002-2003 | Congenital Anomalies in Australia 1998-2001 | Congenital Malformations Australia 1981-1997 | Congenital Malformations Australia 1995 and 1996 | Congenital Malformations Australia 1993 and 1994 | Congenital Malformations Australia 1981-1992
- Neonatal Networks
- Australian & New Zealand Neonatal Network (ANZNN) Neonatal Intensive Care Units
- Canada Canadian Neonatal Network
- European Neonatal Network EuroNeoNet
- USA and Other International Vermont Oxford Network
- Therapeutic Goods Authority TGA | Australian Drug Evaluation Committee (ADEC) | Prescribing Medicines in Pregnancy | Appendix A: Therapeutic goods exempted from pregnancy classification
- NSW Poisons Information Centre Poisons Information Centre
- USA Food and Drug Administration Evaluating the Risks of Drug Exposure in Human Pregnancies | Centers for Disease Control and Prevention (CDC, USA) Pregnancy Risk Assessment Monitoring System (PRAMS) collects state-specific, population-based data on maternal attitudes and experiences before, during, and shortly after pregnancy.
- Other Motherisk (Canada) Drugs, chemicals, radiation and herbal products in pregnancy | International Society for the Study of Trophoblastic Diseases Trophoblastic Diseases
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2026, Mayıs 2) Embryology BGD Tutorial - Applied Embryology and Teratology. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/BGD_Tutorial_-_Applied_Embryology_and_Teratology
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G