Human Abnormal Development: Difference between revisions
| Line 69: | Line 69: | ||
| 859 | | 859 | ||
|- | |- | ||
| [[ | | [[Neural_System_-_Abnormalities#Spina_Bifida_.28Meningomyelocele.29|Spina bifida without anencephaly]] | ||
| 2,858 | | 2,858 | ||
| 1,460 | | 1,460 | ||
Revision as of 00:15, 23 January 2013
Introduction
April 27 2024 How and why do things go wrong in development?
These notes cover abnormalities that can occur during development often described as congenital defects or birth defects. There are many different ways that developmental abnormalities can occur the 3 major types are Genetic (inherited), Environmental (maternal) and Unknown (not determined) derived abnormalities. The environmental factors that cause or lead to any of these abnormalities are described as Teratogens.
It is the group now classified as "unknown causes" that require further research to place them in one of the two other real categories.
Please note that abnormal development pages may contain clinical images not suitable for children.
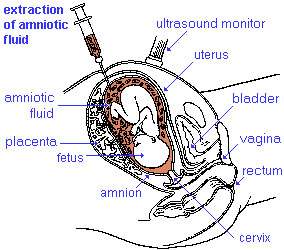
Prenatal Diagnosis
Prenatal diagnosis are the clinical tools used to determine both normal and abnormal development. There are a growing number of new diagnostic techniques that are being applied to human embryonic development.
| Diagnosis Links: Prenatal Diagnosis | pregnancy test | amniocentesis | chorionic villus sampling | ultrasound | Alpha-Fetoprotein | Pregnancy-associated plasma protein-A | Fetal Blood Sampling | Magnetic Resonance Imaging | Computed Tomography | Non-Invasive Prenatal Testing | Fetal Cells in Maternal Blood | Preimplantation Genetic Screening | Comparative Genomic Hybridization | Genome Sequencing | Neonatal Diagnosis | Category:Prenatal Diagnosis | Fetal Surgery | Classification of Diseases | Category:Neonatal Diagnosis |
| 2011 BGD Tutorial - Applied Embryology and Teratology | 2010 Tutorial
Genetic
| Genetic Links: genetic abnormalities | maternal age | Trisomy 21 | Trisomy 18 | Trisomy 13 | Trisomy X | trisomy mosaicism | Monosomy | Fragile X | Williams | Alagille | Philadelphia chromosome | mitochondria | VACTERL | hydatidiform mole | epigenetics | Prenatal Diagnosis | Neonatal Diagnosis | meiosis | mitosis | International Classification of Diseases | genetics |
| Cell Division - Meiosis | Cell Division - Mitosis
Environmental
While genetic abnormalities will have well-defined impacts upon development, environmentally derived effects can be harder to define and often variable depending on many different factors (timing, exposure level, and the combination effects with other factors). This combination effect can also be seen between genetic and environmental interacting to give an even broader spectrum of both major and minor abnormalities.
| Environmental Links: Introduction | low folic acid | iodine deficiency | Nutrition | Drugs | Australian Drug Categories | USA Drug Categories | thalidomide | herbal drugs | Illegal Drugs | smoking | Fetal Alcohol Syndrome | TORCH | viral infection | bacterial infection | fungal infection | zoonotic infection | toxoplasmosis | Malaria | maternal diabetes | maternal hypertension | maternal hyperthermia | Maternal Inflammation | Maternal Obesity | hypoxia | biological toxins | chemicals | heavy metals | air pollution | radiation | Prenatal Diagnosis | Neonatal Diagnosis | International Classification of Diseases | Fetal Origins Hypothesis |
Often not considered, is that pregnancy itself can also expose abnormalities in the mother (congenital heart disease, diabetes, reproductive disorders) that until then had gone undetected. This section of notes also includes links to prenatal diagnosis techniques, twinning and statistical information relating to abnormalities at birth from several different countries.
Undergraduate Science Projects
The links below are to Science student group projects prepared on the topics of prenatal diagnosis (2010) and abnormal development (2011).
- 2011 Student Projects: Turner Syndrome | DiGeorge Syndrome | Klinefelter's Syndrome | Huntington's Disease | Fragile X Syndrome | Tetralogy of Fallot | Angelman Syndrome | Friedreich's Ataxia | Williams-Beuren Syndrome | Duchenne Muscular Dystrolphy | Cleft Palate and Lip
- 2010 Student Projects: Ultrasound | Chorionic villus sampling | Amniocentesis | Percutaneous Umbilical Cord Blood Sampling | Fetal Fibronectin | Maternal serum alpha-fetoprotein
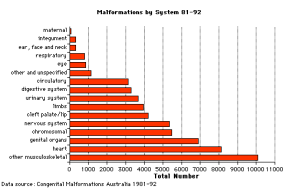
Statistics
Australia - Top 10
The ten most frequently reported birth defects in Victoria between 2003-2004.
- Hypospadias
- Obstructive Defects of the Renal Pelvis or Obstructive Genitourinary Defects
- Ventricular Septal Defect
- Congenital Dislocated Hip
- Trisomy 21 or Down syndrome
- Hydrocephalus
- Cleft Palate
- Trisomy 18 or Edward Syndrome - multiple abnormalities of the heart, diaphragm, lungs, kidneys, ureters and palate 86% discontinued.
- Renal Agenesis/Dysgenesis - reduction in neonatal death and stillbirth since 1993 may be due to the more severe cases being identified in utero and being represented amongst the increased proportion of terminations (approximately 31%).
- Cleft Lip and Palate - occur with another defect in 33.7% of cases.
USA - Selected
CDC National estimates for 21 selected major birth defects (2004–2006).
| Birth Defects | Cases per Births (1 in ...) | Estimated Annual Number of Cases |
|---|---|---|
| Anencephaly | 4,859 | 859 |
| Spina bifida without anencephaly | 2,858 | 1,460 |
| Encephalocele | 12,235 | 341 |
| Anophthalmia/microphthalmia | 5,349 | 780 |
| Common truncus | 13,876 | 301 |
| Transposition of great arteries | 3,333 | 1,252 |
| Tetralogy of Fallot | 2,518 | 1,657 |
| Atrioventricular septal defect | 2,122 | 1,966 |
| Hypoplastic left heart syndrome | 4,344 | 960 |
| Cleft palate without cleft lip | 1,574 | 2,651 |
| Cleft lip with and without cleft palate | 940 | 4,437 |
| Esophageal atresia/tracheoesophageal fistula | 4,608 | 905 |
| Rectal and large intestinal atresia/stenosis | 2,138 | 1,952 |
| Reduction deformity, upper limbs | 2,869 | 1,454 |
| Reduction deformity, lower limbs | 5,949 | 701 |
| Gastroschisis | 2,229 | 1,871 |
| Omphalocele | 5,386 | 775 |
| Diaphragmatic hernia | 3,836 | 1,088 |
| Trisomy 13 | 7,906 | 528 |
| Trisomy 21 (Down syndrome) | 691 | 6,037 |
| Trisomy 18 | 3,762 | 1,109 |
Neural Tube Defects
Neural tube defects that were just outside the top ten most common birth defects but are widely known.
- Spina Bifida - (73%) of parents choose to discontinue a pregnancy affected by spina bifida.
- Anencephaly - (94%) of parents choose to discontinue a pregnancy affected by anencephaly.
- Data: from the Victorian Perinatal Data Collection Unit
Links: Neural System - Abnormalities
Genetic (inherited)
| Genetic Links: genetic abnormalities | maternal age | Trisomy 21 | Trisomy 18 | Trisomy 13 | Trisomy X | trisomy mosaicism | Monosomy | Fragile X | Williams | Alagille | Philadelphia chromosome | mitochondria | VACTERL | hydatidiform mole | epigenetics | Prenatal Diagnosis | Neonatal Diagnosis | meiosis | mitosis | International Classification of Diseases | genetics |
Environmental (maternal)
| Environmental Links: Introduction | low folic acid | iodine deficiency | Nutrition | Drugs | Australian Drug Categories | USA Drug Categories | thalidomide | herbal drugs | Illegal Drugs | smoking | Fetal Alcohol Syndrome | TORCH | viral infection | bacterial infection | fungal infection | zoonotic infection | toxoplasmosis | Malaria | maternal diabetes | maternal hypertension | maternal hyperthermia | Maternal Inflammation | Maternal Obesity | hypoxia | biological toxins | chemicals | heavy metals | air pollution | radiation | Prenatal Diagnosis | Neonatal Diagnosis | International Classification of Diseases | Fetal Origins Hypothesis |
Critical Periods
The table below identifies approximate windows of time, "critical periods", that following exposure to teratogens can lead to developmental abnormalities (anomalies, congenital). In general, the effects for each system are more severe (major anomalies) in the embryonic period during organogenesis in the first trimester. Later teratogen exposure are less severe (minor anomalies) in the fetal period during continued growth and differentiation in the second and third trimester.
| Conceptus | Embryonic development (weeks) | Fetal period (weeks) | |||||||||||||||||
|
|||||||||||||||||||
| Neural | |||||||||||||||||||
| Heart | |||||||||||||||||||
| Upper limbs | |||||||||||||||||||
| Lower limbs | |||||||||||||||||||
| Ear | |||||||||||||||||||
| Eye | |||||||||||||||||||
| Palate | |||||||||||||||||||
| Teeth | |||||||||||||||||||
| External genitalia | |||||||||||||||||||
| Loss | Major abnormalities | Functional and Minor abnormalities | |||||||||||||||||
Teratology
Now consider how different environmental effects during pregnancy may influence developmental outcomes. The terms listed below are often used to describe these environmental effects
- Teratogen (Greek, teraton = monster) any agent that causes a structural abnormality (congenital abnormalities) following fetal exposure during pregnancy. The overall effect depends on dosage and time of exposure. (More? Critical Periods of Development)
- Absolute risk the rate of occurrence of an abnormal phenotype among individuals exposed to the agent. (e.g. fetal alcohol syndrome)
- Relative risk the ratio of the rate of the condition among the exposed and the nonexposed. (e.g. smokers risk of having a low birth weight baby compared to non-smokers) A high relative risk may indicate a low absolute risk if the condition is rare.
- Mutagen a chemical or agent that can cause permanent damage to the deoxyribonucleic acid (DNA) in a cell. DNA damage in the human egg or sperm may lead to reduced fertility, spontaneous abortion (miscarriage), birth defects and heritable diseases.
- Fetotoxicant is a chemical that adversely affects the developing fetus, resulting in low birth weight, symptoms of poisoning at birth or stillbirth (fetus dies before it is born).
- Synergism when the combined effect of exposure to more than one chemical at one time, or to a chemical in combination with other hazards (heat, radiation, infection) results in effects of such exposure to be greater than the sum of the individual effects of each hazard by itself.
- Toxicogenomics the interaction between the genome, chemicals in the environment, and disease. Cells exposed to a stress, drug or toxicant respond by altering the pattern of expression of genes within their chromosomes. Based on new genetic and microarray technologies.
Australian Birth Anomalies System
- "The national collation and reporting of birth anomalies data has been suspended in recent years due to concerns about data quality and comparability."
- Variability among states and territories in scope of birth anomalies data collections
- sources of birth anomalies notifications
- definitions and classifications used
- method of data collection
- available resources
- Variability among the states and territories in the timing and method of the provision of birth anomalies data to the AIHW National Perinatal Statistics Unit (NPSU) for national collation and reporting.
- New Australian Birth Anomalies System should be data for birth anomalies detected up to 1 year of age
- including data on terminations of pregnancies with birth anomalies
- regardless of gestational age (i.e. including less than 20 weeks gestation)
- System will initially be based on data from the states able to detect birth anomalies at least up to 1 year of age
- NSW, VIC, WA and SA
- further extending the period of detection in the future
(Modified from Australian Institute of Health and Welfare (AIHW))
- Links: Australian Congenital Anomalies Monitoring System (ACAMS) | Australian Institute of Health and Welfare (AIHW)
New Zealand
New Zealand Birth Defects Monitoring Programme (NZBDMP)
- monitoring the occurrence of birth defects among livebirths and fetal deaths in New Zealand.
- provide data on the prevalence of birth defects for ad hoc.
- provide annual data to the Ministry of Health and International Clearinghouse for Birth Defects Surveillance and Research (ICBDSR)
- investigate clusters of birth defects
- provide expert technical assistance and advice on the epidemiology of birth defects
USA Monitoring Programmes
Centers for Disease Control (CDC) conducted two birth defects surveillance systems[1] and each state also maintain their own programs (see External Links).
- Metropolitan Atlanta Congenital Defects Programme (MACDP)
- established in 1967
- an intensive surveillance system using several methods to identify infants born with birth defects in the Atlanta area.
- 40th Edition Surveillance Report February 2007
- Birth Defects Monitoring Programme (BDMP)
- a nationwide surveillance system that monitors 1 million births per year.
International Classification of Diseases
The International Classification of Diseases (ICD) is the standard diagnostic tool for epidemiology, health management and clinical purposes. This includes the analysis of the general health situation of population groups. It is used to monitor the incidence and prevalence of diseases and other health problems.
International Statistical Classification of Diseases and Related Health Problems 10th Revision (ICD-10) Version for 2010
Chapter XVII Congenital malformations, deformations and chromosomal abnormalities (Q00-Q99)
- Excl.: inborn errors of metabolism (E70-E90)
This chapter contains the following blocks:
- Q00-Q07 - Congenital malformations of the nervous system.
- Q10-Q18 - Congenital malformations of eye, ear, face and neck.
- Q20-Q28 - Congenital malformations of the circulatory system.
- Q30-Q34 - Congenital malformations of the respiratory system.
- Q35-Q37 - Cleft lip and cleft palate.
- Q38-Q45 - Other congenital malformations of the digestive system.
- Q50-Q56 - Congenital malformations of genital organs.
- Q60-Q64 - Congenital malformations of the urinary system.
- Q65-Q79 - Congenital malformations and deformations of the musculoskeletal system.
- Q80-Q89- Other congenital malformations.
- Q90-Q99 - Chromosomal abnormalities, not elsewhere classified.
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- USA National Center on Birth Defects and Developmental Disabilities
- Arizona Birth Defects Monitoring Program (ABDMP)
- California Birth Defects Monitoring Program (CBDMP)
- North Carolina Birth Defects Monitoring Program (NCBDMP)
- Louisiana Birth Defects Monitoring Network (http://new.dhh.louisiana.gov/index.cfm/page/771 LBDMN)
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 27) Embryology Human Abnormal Development. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Human_Abnormal_Development
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G
- ↑ <pubmed>7287285</pubmed>