Respiratory System Development: Difference between revisions
No edit summary |
mNo edit summary |
||
| (195 intermediate revisions by 2 users not shown) | |||
| Line 1: | Line 1: | ||
{{Header}} | |||
== Introduction == | == Introduction == | ||
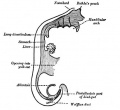
[[File:Stage14_respiratory_tract.jpg|thumb|300px|Respiratory system ([[Carnegie_stage_13|stage 13]])]] | [[File:Stage14_respiratory_tract.jpg|thumb|300px|Respiratory system overview ([[Carnegie_stage_13|stage 13]])]] | ||
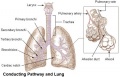
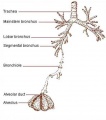
The respiratory system does not carry out its physiological function (of gas exchange) until after birth. The respiratory tract, diaphragm and lungs do form early in embryonic development. The respiratory tract is divided anatomically into 2 main parts: | The respiratory system does not carry out its physiological function (of gas exchange) until after birth. The respiratory tract, diaphragm and lungs do form early in embryonic development. The respiratory tract is divided anatomically into 2 main parts: | ||
# upper respiratory tract, consisting of the nose, nasal cavity and the pharynx | |||
# lower respiratory tract consisting of the larynx, trachea, bronchi and the lungs. | |||
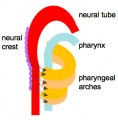
In the head/neck region, the pharynx forms a major arched cavity within the phrayngeal arches. The lungs go through 4 distinct histological phases of development and in late fetal development respiratory motions and amniotic fliud are thought to have a role in lung maturation. | |||
In the head/neck region, the pharynx forms a major arched cavity within the phrayngeal arches. The lungs go through 4 distinct histological phases of development and in late fetal development thyroid hormone, respiratory motions and amniotic fliud are thought to have a role in lung maturation. Branching is a key mechanism/process in lung development leading to alveolar saccules after about 23 branching generations (range of 18–30). | |||
The two main respiratory cell types, squamous alveolar type 1 and alveolar type 2 ({{surfactant}} secreting), both arise from the same bi-potetial progenitor cell.{{#pmid:24499815|PMID24499815}} The third main cell type are macrophages (dust cells) that arise from blood monocyte cells. | |||
Development of this system is not completed until the last weeks of Fetal development, just before birth. Therefore premature babies have difficulties associated with insufficient surfactant (end month 6 alveolar cells type 2 appear and begin to secrete surfactant). | Development of this system is not completed until the last weeks of Fetal development, just before birth. Therefore premature babies have difficulties associated with insufficient surfactant (end month 6 alveolar cells type 2 appear and begin to secrete surfactant). | ||
- | {{Respiratory Links}} | ||
== Some Recent Findings == | |||
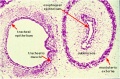
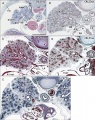
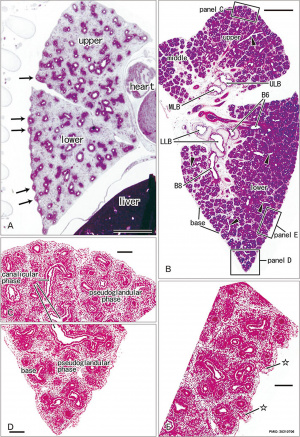
[[File:Pulmonary Pleura - pseudoglandular and canalicular stages 01.jpg|thumb|Pseudoglandular and canalicular stages{{#pmid:30310706|PMID30310706}}]] | |||
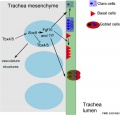
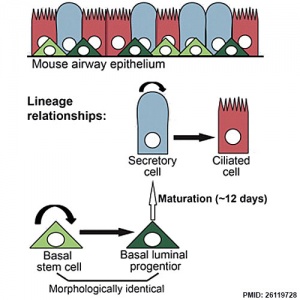
[[File:Respiratory epithelium cells cartoon.jpg|thumb|Respiratory epithelium cell development.{{#pmid:26119728|PMID26119728}}]] | |||
{| | |||
|-bgcolor="F5FAFF" | |||
| | |||
* '''Bronchial tree of the human embryo: Examination based on a mammalian model'''{{#pmid:37602519|PMID37602519}} "Imaging data of 41 human embryo specimens at Carnegie stages (CS) 16-23 (equivalent to 6-8 weeks after fertilization) belonging to the Kyoto collection were obtained using phase-contrast X-ray computed tomography. Three-dimensional bronchial trees were then reconstructed from these images." | |||
* '''Transcriptional control of lung alveolar type 1 cell development and maintenance by NK homeobox 2-1'''{{#pmid:31548395|PMID31548395}} "The extraordinarily thin alveolar type 1 (AT1) cell constitutes nearly the entire gas exchange surface and allows passive diffusion of oxygen into the blood stream. Despite such an essential role, the transcriptional network controlling AT1 cells remains unclear. Using cell-specific knockout mouse models, genomic profiling, and 3D imaging, we found that NK homeobox 2-1 (Nkx2-1) is expressed in AT1 cells and is required for the development and maintenance of AT1 cells. Without Nkx2-1, developing AT1 cells lose 3 defining features-molecular markers, expansive morphology, and cellular quiescence-leading to alveolar simplification and lethality. NKX2-1 is also cell-autonomously required for the same 3 defining features in mature AT1 cells. Intriguingly, Nkx2-1 mutant AT1 cells activate gastrointestinal (GI) genes and form dense microvilli-like structures apically. Single-cell RNA-seq supports a linear transformation of Nkx2-1 mutant AT1 cells toward a GI fate. Whole lung ChIP-seq shows NKX2-1 binding to 68% of genes that are down-regulated upon Nkx2-1 deletion, including 93% of known AT1 genes, but near-background binding to up-regulated genes. Our results place NKX2-1 at the top of the AT1 cell transcriptional hierarchy and demonstrate remarkable plasticity of an otherwise terminally differentiated cell type. {{respiratory}} | |||
* '''Complex Compound Inheritance of Lethal Lung Developmental Disorders Due to Disruption of the {{TBX}}-{{FGF}} Pathway'''{{#pmid:30639323|PMID30639323}} "Primary defects in lung branching morphogenesis, resulting in neonatal lethal pulmonary hypoplasias, are incompletely understood. To elucidate the pathogenetics of human {{lung}} development, we studied a unique collection of samples obtained from deceased individuals with clinically and histopathologically diagnosed interstitial neonatal lung disorders: acinar dysplasia (n = 14), congenital alveolar dysplasia (n = 2), and other lethal lung hypoplasias (n = 10). We identified rare heterozygous copy-number variant deletions or single-nucleotide variants (SNVs) involving {{TBX}}4 (n = 8 and n = 2, respectively) or FGF10 (n = 2 and n = 2, respectively) in 16/26 (61%) individuals. In addition to {{TBX}}4, the overlapping ∼2 Mb recurrent and nonrecurrent deletions at 17q23.1q23.2 identified in seven individuals with lung hypoplasia also remove a lung-specific enhancer region. Individuals with coding variants involving either {{TBX}}4 or {{FGF}}10 also harbored at least one non-coding SNV in the predicted lung-specific enhancer region, which was absent in 13 control individuals with the overlapping deletions but without any structural lung anomalies. The occurrence of rare coding variants involving TBX4 or FGF10 with the putative hypomorphic non-coding SNVs implies a complex compound inheritance of these pulmonary hypoplasias. Moreover, they support the importance of TBX4-FGF10-FGFR2 epithelial-mesenchymal signaling in human lung organogenesis and help to explain the histopathological continuum observed in these rare lethal developmental disorders of the {{lung}}." | |||
* '''Review - How high resolution 3-dimensional imaging changes our understanding of postnatal lung development'''{{#pmid:30390117|PMID30390117}} "During the last 10 + years biologically and clinically significant questions about postnatal lung development could be answered due to the application of modern cutting-edge microscopic and quantitative histological techniques. These are in particular synchrotron radiation based X-ray tomographic microscopy (SRXTM), but also 3Helium Magnetic Resonance Imaging, as well as the stereological estimation of the number of alveoli and the length of the free septal edge. First, the most important new finding may be the following: alveolarization of the lung does not cease after the maturation of the alveolar microvasculature but continues until young adulthood and, even more important, maybe reactivated lifelong if needed to rescue structural damages of the lungs. Second, the pulmonary acinus represents the functional unit of the lung. Because the borders of the acini could not be detected in classical histological sections, any investigation of the acini requires 3-dimensional (imaging) methods. Based on SRXTM it was shown that in rat lungs the number of acini stays constant, meaning that their volume increases by a factor of ~ 11 after birth. The latter is very important for acinar ventilation and particle deposition." | |||
* '''Development of the pulmonary pleura with special reference to the lung surface morphology: a study using human fetuses'''{{#pmid:30310706|PMID30310706}} "In and after the {{third trimester}}, the lung surface is likely to become smooth to facilitate respiratory movements. However, there are no detailed descriptions as to when and how the lung surface becomes regular. According to our observations of 33 fetuses at 9-16 weeks of gestation (crown-rump length [CRL], 39-125 mm), the lung surface, especially its lateral (costal) surface, was comparatively rough due to rapid branching and outward growing of bronchioli at the {{pseudoglandular stage}} of lung development. The pulmonary pleura was thin and, beneath the surface mesothelium, no or little mesenchymal tissue was detectable. Veins and lymphatic vessels reached the lung surface until 9 weeks and 16 weeks, respectively. In contrast, in 8 fetuses at 26-34 weeks of gestation (CRL, 210-290 mm), the lung surface was almost smooth because, instead of bronchioli, the developing alveoli faced the external surfaces of the lung. ... a smooth lung surface seemed to be established largely by the thick submesothelial tissue including veins and lymphatic vessels until 26 weeks." | |||
''' | * '''Review - Human lung development: recent progress and new challenges'''{{#pmid:30111617|PMID30111617}} "Recent studies have revealed biologically significant differences between human and {{mouse}} lung development, and have reported new in vitro systems that allow experimental manipulation of human lung models. At the same time, emerging clinical data suggest that the origins of some adult lung diseases are found in embryonic development and childhood. The convergence of these research themes has fuelled a resurgence of interest in human lung developmental biology. In this Review, we discuss our current understanding of human lung development, which has been profoundly influenced by studies in mice and, more recently, by experiments using in vitro human lung developmental models and RNA sequencing of human foetal lung tissue." | ||
== | |} | ||
{| class="wikitable mw-collapsible mw-collapsed" | |||
! More recent papers | |||
|- | |||
| [[File:Mark_Hill.jpg|90px|left]] {{Most_Recent_Refs}} | |||
Search term: [http://www.ncbi.nlm.nih.gov/pubmed/?term=Respiratory+Development ''Respiratory Development''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Lung+Embryology ''Lung Embryology''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Lung+Development ''Lung Development''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Alveolar+Embryology ''Alveolar Embryology''] | | |||
|} | |||
{| class="wikitable mw-collapsible mw-collapsed" | |||
! Older papers | |||
|- | |||
| {{Older papers}} | |||
* PDGF-A signaling is required for secondary alveolar septation and controls epithelial proliferation in the developing lung{{#pmid:29636361|PMID29636361}} "Platelet-derived growth factor A (PDGF-A) signaling through PDGF receptor α is essential for alveogenesis. Previous studies have shown that Pdgfa-/- mouse lungs have enlarged alveolar airspace with absence of secondary septation, both distinctive features of bronchopulmonary dysplasia. ...In the absence of PDGF-A, the number of PdgfraGFP+ cells was significantly decreased. In addition, proliferation of PdgfraGFP+ cells was reduced. During alveogenesis, PdgfraGFP+ myofibroblasts failed to form the α-smooth muscle actin rings necessary for alveolar secondary septation. These results indicate that PDGF-A signaling is involved in myofibroblast proliferation and migration." | |||
* '''Review - In utero alcohol effects on foetal, neonatal and childhood lung disease'''{{#pmid:27613232|PMID27613232}} "Maternal alcohol use during pregnancy exposes both premature and term newborns to the toxicity of alcohol and its metabolites. Foetal alcohol exposure adversely effects the lung. In contrast to the adult "alcoholic lung" phenotype, an inability to identify the newborn exposed to alcohol in utero has limited our understanding of its effect on adverse pulmonary outcomes. This paper will review advances in biomarker development of in utero alcohol exposure. We will highlight the current understanding of in utero alcohol's toxicity to the developing lung and immune defense. Finally, we will present recent clinical evidence describing foetal alcohol's association with adverse pulmonary outcomes including bronchopulmonary dysplasia, viral infections such as respiratory syncytial virus and allergic asthma/atopy." | |||
* '''Development and plasticity of alveolar type 1 cells'''{{#pmid:26586225|PMID26586225}} "Alveolar type 1 (AT1) cells cover >95% of the gas exchange surface and are extremely thin to facilitate passive gas diffusion. The development of these highly specialized cells and its coordination with the formation of the honeycomb-like alveolar structure are poorly understood. Using new marker-based stereology and single-cell imaging methods, we show that AT1 cells in the mouse lung form expansive thin cellular extensions via a non-proliferative two-step process while retaining cellular plasticity. In the flattening step, AT1 cells undergo molecular specification and remodel cell junctions while remaining connected to their epithelial neighbors. In the folding step, AT1 cells increase in size by more than 10-fold and undergo cellular morphogenesis that matches capillary and secondary septa formation, resulting in a single AT1 cell spanning multiple alveoli. Furthermore, AT1 cells are an unexpected source of VEGFA and their normal development is required for alveolar angiogenesis. Notably, a majority of AT1 cells proliferate upon ectopic SOX2 expression and undergo stage-dependent cell fate reprogramming." | |||
* '''Clonal Dynamics Reveal Two Distinct Populations of Basal Cells in Slow-Turnover Airway Epithelium'''{{#pmid:26119728|PMID26119728}} "We investigated the mouse tracheal epithelial lineage at homeostasis by using long-term clonal analysis and mathematical modeling. This pseudostratified epithelium contains basal cells and secretory and multiciliated luminal cells. Our analysis revealed that basal cells are heterogeneous, comprising approximately equal numbers of multipotent stem cells and committed precursors, which persist in the basal layer for 11 days before differentiating to luminal fate. We confirmed the molecular and functional differences within the basal population by using single-cell qRT-PCR and further lineage labeling. Additionally, we show that self-renewal of short-lived secretory cells is a feature of homeostasis. We have thus revealed early luminal commitment of cells that are morphologically indistinguishable from stem cells." | |||
* '''Notch3-Jagged signaling controls the pool of undifferentiated airway progenitors'''{{#pmid:25564622|PMID25564622}} "Basal cells are multipotent airway progenitors that generate distinct epithelial cell phenotypes crucial for homeostasis and repair of the conducting airways. Little is known about how these progenitor cells expand and transition to differentiation to form the pseudostratified airway epithelium in the developing and adult lung. Here, we show by genetic and pharmacological approaches that endogenous activation of Notch3 signaling selectively controls the pool of undifferentiated progenitors of upper airways available for differentiation. This mechanism depends on the availability of Jag1 and Jag2, and is key to generating a population of parabasal cells that later activates Notch1 and Notch2 for secretory-multiciliated cell fate selection." [[Developmental Signals - Notch|Notch]] | |||
* '''Alveolar progenitor and stem cells in lung development'''{{#pmid:24499815|PMID24499815}} "Alveoli are gas-exchange sacs lined by squamous alveolar type (AT) 1 cells and cuboidal, surfactant-secreting AT2 cells. Classical studies suggested that AT1 arise from AT2 cells, but recent studies propose other sources. Here we use molecular markers, lineage tracing and clonal analysis to map alveolar progenitors throughout the mouse lifespan. We show that, during development, AT1 and AT2 cells arise directly from a bipotent progenitor, whereas after birth new AT1 cells derive from rare, self-renewing, long-lived, mature AT2 cells that produce slowly expanding clonal foci of alveolar renewal." | |||
* '''Lung epithelial branching program antagonizes alveolar differentiation'''{{#pmid:24058167|PMID24058167}} "Mammalian organs, including the lung and kidney, often adopt a branched structure to achieve high efficiency and capacity of their physiological functions. Formation of a functional lung requires two developmental processes: branching morphogenesis, which builds a tree-like tubular network, and alveolar differentiation, which generates specialized epithelial cells for gas exchange. ...We thus propose that lung epithelial progenitors continuously balance between branching morphogenesis and alveolar differentiation, and such a balance is mediated by dual-function regulators, including Kras and Sox9. The resulting temporal delay of differentiation by the branching program may provide new insights to lung immaturity in preterm neonates and the increase in organ complexity during evolution." | |||
*''' Suppression of embryonic lung branching morphogenesis'''{{#pmid:20535580|PMID20535580}} "The role of HOM/C homeobox genes on rat embryonic lung branching morphogenesis was investigated using the lung bud explant culture system in an air/liquid interface. ...These results suggest a critical role for homeobox b3 and b4 genes in lung airway branching morphogenesis." | |||
* '''Retinoic acid-dependent network in the foregut controls formation of the mouse lung primordium'''{{#pmid:20484817|PMID20484817}}= "The developmental abnormalities associated with disruption of signaling by retinoic acid (RA), the biologically active form of vitamin A, have been known for decades from studies in animal models and humans. These include defects in the respiratory system, such as lung hypoplasia and agenesis. ....The data in this study suggest that disruption of Wnt/Tgfbeta/Fgf10 interactions represents the molecular basis for the classically reported failure to form lung buds in vitamin A deficiency." | |||
Clinical | |||
* '''Lung Function and Respiratory Symptoms at 11 Years in Extremely Preterm Children'''{{#pmid:20378729|PMID20378729}} "Following extremely preterm birth, impaired lung function and increased respiratory morbidity persist into middle childhood, especially those with bronchopulmonary dysplasia (BPD). Many of these children may not be receiving appropriate treatment." | |||
* '''Pediatric lung transplantation.'''{{#pmid:20371042|PMID20371042}} "Lung transplantation is an accepted therapy for selected pediatric patients with severe end-stage vascular or parenchymal lung disease. Collaboration between the patients' primary care physicians, the lung transplant team, patients, and patients' families is essential. The challenges of this treatment include the limited availability of suitable donor organs, the toxicity of immunosuppressive medications needed to prevent rejection, the prevention and treatment of obliterative bronchiolitis, and maximizing growth, development, and quality of life of the recipients. This article describes the current status of pediatric lung transplantation, indications for listing, evaluation of recipient and donor, updates on the operative procedure,graft dysfunction, and the risk factors, outcomes, and future directions." | |||
|} | |||
== Textbooks == | == Textbooks == | ||
* | * Moore, K.L., Persaud, T.V.N. & Torchia, M.G. (2015). <i>The developing human: clinically oriented embryology</i> (10th ed.). Philadelphia: Saunders. Chapter 10 [http://www.unsw.eblib.com.wwwproxy0.library.unsw.edu.au/patron/Read.aspx?p=2074364&pg=269 Respiratory System] | ||
* ''' | * Schoenwolf, G.C., Bleyl, S.B., Brauer, P.R., Francis-West, P.H. & Philippa H. (2015). ''Larsen's human embryology'' (5th ed.). New York; Edinburgh: Churchill Livingstone. Chapter 11 [http://www.unsw.eblib.com.wwwproxy0.library.unsw.edu.au/patron/Read.aspx?p=2074524&pg=269 Development of the Respiratory System and Body Cavities] | ||
* Before We Are Born (5th ed.) Moore and Persaud Chapter 13 p255-287 | * Before We Are Born (5th ed.) Moore and Persaud Chapter 13 p255-287 | ||
* Essentials of Human Embryology Larson Chapter 9 p123-146 | * Essentials of Human Embryology Larson Chapter 9 p123-146 | ||
* Human Embryology Fitzgerald and Fitzgerald Chapter 19,20 p119-123 | * Human Embryology Fitzgerald and Fitzgerald Chapter 19,20 p119-123 | ||
* Anatomy of the Human Body 1918 Henry Gray [ | * Anatomy of the Human Body 1918 Henry Gray [[Anatomy_of_the_Human_Body_by_Henry_Gray#947_Respiratory|The Respiratory Apparatus]] | ||
==Objectives== | ==Objectives== | ||
| Line 30: | Line 84: | ||
* Describe the developmental aberrations responsible for the following malformations: tracheo - oesophageal fistula (T.O.F); oesphageal atresia; diaphragmatic hernia; lobar emphysema. | * Describe the developmental aberrations responsible for the following malformations: tracheo - oesophageal fistula (T.O.F); oesphageal atresia; diaphragmatic hernia; lobar emphysema. | ||
== Development Overview == | == Development Overview == | ||
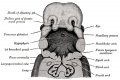
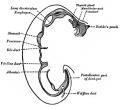
[[File:Bailey287.jpg|thumb]] | |||
'''Week 4''' - laryngotracheal groove forms on floor foregut. | '''Week 4''' - laryngotracheal groove forms on floor foregut. | ||
| Line 45: | Line 99: | ||
'''Month 7''' - respiratory bronchioles proliferate and end in alveolar ducts and sacs. | '''Month 7''' - respiratory bronchioles proliferate and end in alveolar ducts and sacs. | ||
===Lung Development=== | ===Mechanisms=== | ||
* '''Initiation''' - Budding of foregut [[endoderm]] to generate the trachea. | |||
* '''Branching''' - A repeated mechanism of branching that is ongoing throughout development to form the conducting bronchioles then alveolar ducts. | |||
* '''Surface area increase''' - Expansion of the surface area in late development generating eventually the thin air–blood barrier for gas exchange in the acini. | |||
* '''Vascular development''' - Extension of a vascular capillary tree within the connective tissue and wall of the acini for gas exchange, and the lymphatic development for immunology of the lungs. | |||
* '''Surfactant development''' - allows lung inflation and decreases the work of breathing and also related to immunology of the lungs. | |||
* '''Musculoskeletal development''' - contributes the mechanical elements of ribs, intercostals and [[Diaphragm Development|diaphragm]] required for breathing. | |||
==Lung Development Stages== | |||
The sequence is most important rather than the actual timing, which is variable both in development and in the existing literature. | |||
{{Lung_stage_table}} | |||
<br> | |||
{{Lung_stage_table2}} | |||
===Embryonic stage=== | |||
{| | |||
! Human Embryonic Lung Development | |||
|- | |||
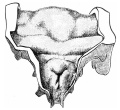
| [[File:Bailey287.jpg|300px]] | |||
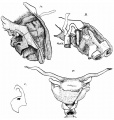
| [[File:Bailey288.jpg|300px]] | |||
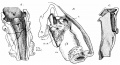
| [[File:Bailey289.jpg|300px]] | |||
|- | |||
| CRL 4.3 mm, Week 4-5, Stage {{CS12}} to {{CS13}} | |||
| CRL 8.5 mm, Week 5, Stage {{CS15}} to {{CS16}} | |||
| CRL 10.5 mm, Week 6 Stage {{CS16}} to {{CS17}} | |||
|} | |||
* Endoderm - tubular ventral growth from foregut pharynx. | |||
* Mesoderm - mesenchyme of lung buds. | |||
* Intraembryonic coelom - pleural cavities elongated spaces connecting pericardial and peritoneal spaces. | |||
* Vascular - extra pulmonary artery then lobular artery. | |||
===Pseudoglandular stage=== | |||
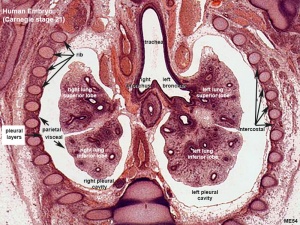
[[File:ME54 003.jpg|thumb|alt=respiratory histology week 8|Respiratory histology (week 8)]] | |||
{| | |||
| | |||
* week 5 - 17 | |||
* tubular branching of the human lung airways continues | |||
* by 2 months all segmental bronchi are present. | |||
* lungs have appearance of a glandlike structure. | |||
* stage is critical for the formation of all conducting airways. | |||
* lined with tall columnar epithelium, the more distal structures are lined with cuboidal epithelium. | |||
* Vascular - Pre-acinar arteries. | |||
|- | |||
| [[File:Human right lung 7-8 weeks.jpg|300px]] | |||
Human lung pseudoglandular stage{{#pmid:24693478|PMID24693478}} | |||
|} | |||
===Canalicular stage=== | |||
[[File:Lung_alveoli_development_cartoon.jpg|thumb|300px]] | |||
* week 16 - 24 | |||
** canalicular phase of the bronchus can be mixed with the pseudoglandular phase. | |||
* Lung morphology changes dramatically, beginning of alveolar epithelium development. | |||
* differentiation of the pulmonary epithelium results in the formation of the future air-blood tissue barrier. | |||
* Surfactant synthesis. | |||
* future gas exchange regions can be distinguished from the future conducting airways of the lungs. | |||
* Vascular - Intra-acinar arteries, canalization of the lung parenchyma by capillaries begins, increasing number of capillaries in close contact with cuboidal epithelium. | |||
===Saccular stage=== | |||
{| | |||
| | |||
* week 24 to near term. | |||
* most peripheral airways form widened airspaces, termed saccules. | |||
* saccules widen and lengthen the airspace (by the addition of new generations). | |||
* future gas exchange region expands significantly. | |||
* Fibroblastic cells also undergo differentiation, they produce extracellular matrix, collagen, and elastin. May have a role in epithelial differentiation and control of surfactant secretion | |||
* Vascular - alveolar duct arteries, vascular tree also grows in length and diameter during this time. | |||
| [[File:Alveolar-sac-01.jpg|300px]] | |||
Alveolar sac structure | |||
|} | |||
===Alveolar stage=== | |||
{| | |||
| | |||
* near term through postnatal period. | |||
* 1-3 years postnatally alveoli continue to form through a septation process increasing the gas exchange surface area. | |||
* microvascular maturation occurs during this period. | |||
* respiratory motions and amniotic fluid are thought to have a role in lung maturation. | |||
* Vascular - alveolar capillaries. | |||
Premature babies have difficulties associated with insufficient surfactant (end month 6 alveolar cells type 2 appear and begin to secrete surfactant). Lung growth continues postnatally to 20-23 years. | |||
| [[File:Respiratory secondary septum 01.jpg|alt=Respiratory secondary septum|300px]] | |||
Respiratory secondary septum{{#pmid:25973420|PMID25973420}} | |||
|} | |||
==Surfactant== | |||
Pulmonary surfactant or simply {{surfactant}} ('''surf'''ace '''act'''ive '''a'''ge'''nt''') begins to be produced at the {{canalicular stage}} and both production and turnover are key for development. It is a mixture of lipids and proteins secreted by Type 2 alveolar cells between alveolar epithelium that reduces surface tension (detergent) at the air-liquid interface. The function of this secretion is to prevent collapse of the lung at the end of expiration. In humans, these cells and their secretion develop towards the very end of the third trimester, just before birth. | |||
Surfactant is mainly phosphatidylcholine (PC) 80% in turn consisting of which dipalmitoyl-PC, palmitoyl-myristoyl-PC and palmitoyl-palmitoleoyl-PC together 75%, anionic phosphatidylglycerol and cholesterol are about 10% each.{{#pmid:27693601|PMID27693601}} | |||
The surfactant proteins (SP) SP-A to -D comprise only about 2-5%. Surfactant protein D (SP-D) a multimeric collectin (collagen-containing C-type lectin) involved in innate immunity (anti-microbial){{#pmid:29473039|PMID29473039}} and expressed in pulmonary and non-pulmonary epithelia.{{#pmid:28351530|PMID28351530}} Surfactant protein B (SP-B) and disaturated-phosphatidylcholine have both been shown to be higher in preterms with chorioamnionitis.{{#pmid:30270169|PMID30270169}} | |||
Clinically surfactants used for surfactant replacement therapy are animal-derived preparations, commonly bovine (beractant, bovactant, BLES) or less common porcine (butantan, poractant-α and surfacen).{{#pmid:30728009|PMID30728009}} | |||
==Respiratory Species Comparison== | |||
[[File:Mouse lung development 03.jpg|thumb|150px|alt=Mouse lung development|Mouse lung development{{#pmid:15005800|PMID15005800}}]] | |||
Different species undergo lung development stages over different time courses{{#pmid:28876535|PMID28876535}} and some species ( {{mouse}} and {{rat}}) do not possess any respiratory bronchioles, the acini and the ventilatory units are therefore the same entity. | |||
{{Respiratory Species Comparison table}} | |||
===Mouse=== | |||
Note that the model mouse respiratory system differs from human in size, distribution of cell types, and the time taken to develop. Additionally, the common laboratory {{mouse}} model (C57BL/6J} completely lacks respiratory breathing movements seen in the human fetus.{{#pmid:18980217|PMID18980217}} | |||
[[File:Lung human and mouse Sox expression.jpg|500px]] | |||
Human and mouse Sox expression{{#pmid:28806170|PMID28806170}} | |||
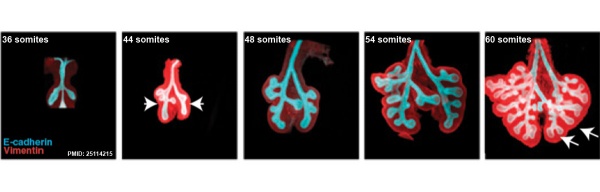
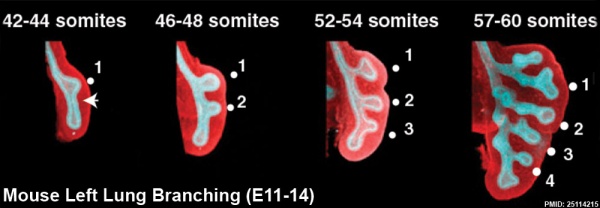
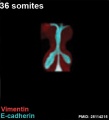
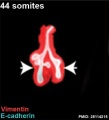
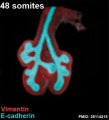
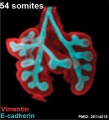
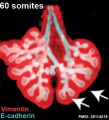
The following images are from a recent study of the development of bronchial branching in he mouse between E10 to E14.{{#pmid:25114215|PMID25114215}} | |||
Mesenchyme (red) and epithelium (blue) the study used knockout mice to show the role of Wnt signalling in branching morphogenesis. | |||
[[File:Mouse respiratory 36 to 60 somites.jpg|600px]] | |||
[[File:Mouse respiratory 44 to 60 somites.jpg|600px]] | |||
{| | |||
! colspan=4|Mouse lung E12.5 to E18.5 | |||
|- | |||
| [[File:Mouse whole lung E12.5.jpg|200px]] | |||
| [[File:Mouse whole lung E14.5.jpg|200px]] | |||
| [[File:Mouse lung E14.5 Sox9.jpg|200px]] | |||
| [[File:Mouse lung histology E18.5.jpg|200px]] | |||
|- | |||
| E12.5 lungs | |||
| E14.5 lungs | |||
| E14.5 Sox9 | |||
| E18.5 lungs | |||
|- | |||
| Reference{{#pmid:24191021|PMID24191021}} | |||
|} | |||
:'''Links:''' [[Developmental Signals - Wnt|Wnt]] | [[Mouse Development]] | |||
==Embryonic Respiratory Development== | |||
[[File:Lung_development_stage13-22.jpg]] | |||
==Pseudoglandular Respiratory Development== | |||
[[File:Human_lung_pseudoglandular.jpg|400px]] | |||
Pseudoglandular period identified in this paper (GA weeks 12 to 16) | |||
Human lung at pseudoglandular stage showing E- and N-cadherin and β-catenin localization.{{#pmid:21080917|PMID21080917}} | |||
==Endocrine Lung== | |||
{| | |||
! Neonatal Human | |||
! Fetal Rabbit | |||
|- | |||
| [[File:Neonatal human pulmonary neuroendocrine cell EM01.jpg|300px]] | |||
| [[File:Fetal rabbit neuroepithelial body 01.jpg|300px]] | |||
|- | |||
| Pulmonary neuroendocrine cell (EM){{#pmid:6376101|PMID6376101}} | |||
| Neuroepithelial body{{#pmid:6376101|PMID6376101}} | |||
|} | |||
'''Pulmonary neuroendocrine cells''' (PNECs) | |||
* develop in late embryonic to early fetal period.{{#pmid:6188605|PMID6188605}}{{#pmid:3906540|PMID3906540}} | |||
* later in mid-fetal period clusters of these cells form neuroepithelial bodies (NEBs). | |||
* first cell type to differentiate in the airway epithelium. | |||
** differentiation regulated by proneural genes - mammalian homolog of the achaete-scute complex (Mash-1) and hairy and enhancer of split1 (Hes-1).{{#pmid:20027181|PMID20027181}} | |||
* located in the fetal lung at bronchiole branching points. | |||
* may stimulate mitosis to increase branching. | |||
* secrete 2 peptides - gastrin-releasing peptide (GRP) and calcitonin gene related peptide (CGRP) | |||
:'''Links:''' [[Endocrine_-_Other_Tissues|Endocrine - Other Tissues]] | [http://www.omim.org/entry/137260 OMIM - GRP] | [http://www.omim.org/entry/606121 OMIM - CGRP] | |||
==Lung Histology== | |||
{| | |||
| [[File:Fetal_lung_histology.jpg]] | |||
|- | |||
| Fetal lung histology | |||
|} | |||
:'''Links:''' [[Respiratory System - Histology]] | |||
===Birth Changes=== | |||
At birth the lung epithelium changes from a prenatal secretory to a postnatal absorptive function. Several factors have been identified as influencing this transport change including: epinephrine, oxygen, glucocorticoids, and thyroid hormones (for review see{{#pmid:12235057|PMID12235057}}) | |||
==Upper Respiratory Tract== | |||
[[File:Gray0961.jpg|thumb|Adult upper respiratory tract conducting system]] | |||
<gallery> | |||
File:Gitbpm.jpg|stage 11 foregut | |||
File:Gray0982a.jpg|week 4 early respiratory endodermal bud | |||
File:Stage_22_image_167.jpg|Stage 22 trachea | |||
File:Head_arches_cartoon.jpg|Head arches cartoon | |||
File:Pharynx_cartoon.jpg|Pharynx | |||
File:Nasal cavities.jpg|Nasal cavities | |||
File:Pharynx.jpg|Pharynx | |||
File:Larynx.jpg|Larynx | |||
</gallery> | |||
* part of foregut development | |||
* anatomically the nose, nasal cavity and the pharynx | |||
* the pharynx forms a major arched cavity within the pharyngeal arches | |||
==Movies== | |||
The animations below allow a comparison of early and late embryonic lung development. Compare the size and relative position of the respiratory structures and their anatomical relationship to the developing gastrointestinal tract. | |||
{| border='0px' | |||
|- | |||
| {{Gastrointestinal stage 13 movie}} | |||
| [[Movie_-_Gastrointestinal_Tract_3D_stage_13|Early embryo (stage 13)]] | |||
3 dimensional reconstruction based upon a serial reconstruction from individual [[Carnegie stage 13]] embryo slice images. | |||
| {{Gastrointestinal stage 22 movie}} | |||
| [[Movie_-_Gastrointestinal_Tract_3D_stage_22|Late embryo (stage 22)]] | |||
3 dimensional reconstruction based upon a serial reconstruction from individual embryo slice images [[Carnegie stage 22]], 27 mm Human embryo, approximate day 56. | |||
|- | |||
|} | |||
==Lung Cardiovascular== | |||
:'''Links:''' [[Cardiovascular System Development]] | |||
===Pulmonary Circulation=== | |||
* pulmonary arteries and veins arise by vasculogenesis{{#pmid:11867341|PMID11867341}} | |||
'''Pulmonary Veins''' | |||
* vasculogenesis in the mesenchyme surrounding the terminal buds during the pseudoglandular stage. | |||
** vasculogenesis - describes the formation of new blood vessels from pluripotent precursor cells. | |||
* angiogenesis in the canalicular and alveolar stages. | |||
** angiogenesis - describes the formation of new vessels from pre-existing vessels. | |||
See also review{{#pmid:12430957|PMID12430957}} | |||
===Bronchial Circulation=== | |||
'''Bronchial Arteries''' | |||
* vascularising the walls of the airways and the large pulmonary vessels providing giving oxygen and nutrients. | |||
* extend within the bronchial tree to the periphery of the alveolar ducts. | |||
* not found in the lungs until around 8 weeks of gestation. | |||
** one or two small vessels extend from the dorsal aorta and run into the lung alongside the cartilage plates of the main bronchus. | |||
'''Bronchial Veins''' | |||
* small bronchial veins within the airway wall drain into the pulmonary veins. | |||
* large bronchial veins seen close to the hilum and drain into the cardinal veins and the right atrium. | |||
See review{{#pmid:12430957|PMID12430957}} | |||
==Molecular== | |||
{{Factor Links}} | |||
===TBX=== | |||
{| | |||
| [[File:Mouse respiratory Tbx4 and Tbx5.jpg|400px]] | |||
| [[File:Mouse- respiratory development 01.jpg|400px]] | |||
|- | |||
| Mouse respiratory Tbx4 and Tbx5 model{{#pmid:22876201|PMID22876201}} | |||
| Mouse respiratory development{{#pmid:20614584|PMID20614584}}]] | |||
|} | |||
* '''Nkx2-1''' (Titf1) - ventral wall of the anterior foregut, identifies the future trachea. | |||
===SOX=== | |||
* Sox2 is essential for the initiation of lung development from the endodermal gut tube, | |||
* Sox9 is essential for maintaining the tips and associated branching. | |||
Several different Sox types are required for different stages of respiratory development. Wnt/β-catenin signaling does not regulate Sox9 expression in the lung.{{#pmid:24191021|PMID24191021}} | |||
[[File:Lung human and mouse Sox expression.jpg|500px]] | |||
Human and mouse Sox expression{{#pmid:28806170|PMID28806170}} | |||
===FGF=== | |||
[[File:Mouse- respiratory development 04.jpg|thumb|Fibroblast growth factor signaling{{#pmid:20614584|PMID20614584}}]] | |||
* Localized Fgf10 expression not required for lung branching but prevents epithelial differentiation{{#pmid:23924632|PMID23924632}} "As the lung buds grow out, proximal epithelial cells become further and further displaced from the distal source of Fgf10 and differentiate into bronchial epithelial cells. Interestingly, our data presented here show that once epithelial cells are committed to the Sox2-positive airway epithelial cell fate, Fgf10 prevents ciliated cell differentiation and promotes basal cell differentiation." | |||
* '''Opposing Fgf and Bmp activities regulate the specification of olfactory sensory and respiratory epithelial cell fates'''{{#pmid:20392740|PMID20392740}} " In this study, we provide evidence that in both chick and mouse, Bmp signals promote respiratory epithelial character, whereas Fgf signals are required for the generation of sensory epithelial cells. Moreover, olfactory placodal cells can switch between sensory and respiratory epithelial cell fates in response to Fgf and Bmp activity, respectively. Our results provide evidence that Fgf activity suppresses and restricts the ability of Bmp signals to induce respiratory cell fate in the nasal epithelium." | |||
===BMP=== | |||
Bone morphogenic protein 4 (Bmp4) acts as in an autocrine signalling mechanism to limit bud outgrowth and is therefore involved in branching. | |||
* | ===Nkx2-1=== | ||
* | |||
* | '''Transcriptional control of lung alveolar type 1 cell development and maintenance by NK homeobox 2-1''' [https://www.pnas.org/content/116/41/20545.abstract?etoc PNAS] "Gas exchange in the lung relies on passive diffusion of oxygen and carbon dioxide across an extraordinarily thin epithelium that is nearly entirely made of the poorly understood alveolar type 1 (AT1) cell. Our study shows that all AT1 cells express and require NK homeobox 2-1 ([https://www.omim.org/entry/600635 Nkx2-1]) for their development and maintenance. Nkx2-1 mutant AT1 cells lose their characteristic molecular and cellular features and transform toward a gastrointestinal fate, highlighting remarkable plasticity of an otherwise terminally differentiated cell type. This work establishes NKX2-1 as the first overarching factor in the AT1 cell transcriptional hierarchy and paves the way for unraveling not only the unique biology of AT1 cells but also cell type-specific roles of a lineage transcription factor." See also 2012 review paper [https://cshperspectives.cshlp.org/content/4/5/a008318.full Signaling Networks Regulating Development of the Lower Respiratory Tract] | ||
The NKX2-1 gene encodes a transcription factor that is expressed during early development of {{thyroid}}, {{lung}}, and {{neural}} (forebrain regions including basal ganglia and {{hypothalamus}}). NKX2-1 was originally called thyroid transcription factor-1 (TTF1) due to the fact that it mediated thyroid-specific gene transcription. | |||
Links: [https://www.omim.org/entry/600635 OMIM Nkx2-1] | |||
===Other=== | |||
* '''Heparan sulfate in lung morphogenesis'''{{#pmid:20301217|PMID20301217}} "Heparan sulfate (HS) is a structurally complex polysaccharide located on the cell surface and in the extracellular matrix, where it participates in numerous biological processes through interactions with a vast number of regulatory proteins such as growth factors and morphogens. ...he potential contribution of HS to abnormalities of lung development has yet to be explored to any significant extent, which is somewhat surprising given the abnormal lung phenotype exhibited by mutant mice synthesizing abnormal HS." | |||
* '''Signaling via Alk5 controls the ontogeny of lung Clara cells'''{{#pmid:20147383|PMID20147383}} "Clara cells, together with ciliated and pulmonary neuroendocrine cells, make up the epithelium of the bronchioles along the conducting airways. Clara cells are also known as progenitor or stem cells during lung regeneration after injury. ...Using lung epithelial cells, we show that Alk5-regulated Hes1 expression is stimulated through Pten and the MEK/ERK and PI3K/AKT pathways. Thus, the signaling pathway by which TGFbeta/ALK5 regulates Clara cell differentiation may entail inhibition of Pten expression, which in turn activates ERK and AKT phosphorylation." | |||
* '''Wt1 and retinoic acid signaling in the subcoelomic mesenchyme control the development of the pleuropericardial membranes and the sinus horns'''{{#pmid:20185795|PMID20185795}} "Pericardium and sinus horn formation are coupled and depend on the expansion and correct temporal release of pleuropericardial membranes from the underlying subcoelomic mesenchyme. Wt1 and downstream Raldh2/retinoic acid signaling are crucial regulators of this process." | |||
:'''Links:''' [[Developmental_Signals_-_Sox|Sox]] | [http://www.ncbi.nlm.nih.gov/bookshelf/br.fcgi?book=stembook&part=specificationandpatterning StemBook - Specification and patterning of the respiratory system] | |||
== References == | == References == | ||
<references/> | <references/> | ||
===Reviews=== | |||
{{#pmid:30111617}} | |||
{{#pmid:29707503}} | |||
{{#pmid:29331337}} | |||
{{#pmid:28144783}} | |||
{{#pmid:27957616}} | |||
{{#pmid:24449833}} | |||
{{#pmid:24429276}} | |||
{{#pmid:27613232}} | |||
{{#pmid:22850882}} | |||
{{#pmid:20691848}} | |||
{{#pmid:20152174}} | |||
{{#pmid:16770071}} | |||
{{#pmid:12615030}} | |||
{{#pmid:12456356}} | |||
{{#pmid:6370120}} | |||
===Articles=== | ===Articles=== | ||
{{#pmid:18651668}} | |||
{{#pmid:16770071}} | |||
{{#pmid:11867341}} | |||
{{#pmid:10919986}} | |||
{{#pmid:10100986}} | |||
===Search PubMed=== | ===Search PubMed=== | ||
Search April 2010 | Search April 2010 | ||
* Respiratory System Development - All (30795) Review (3706) Free Full Text (7943) | |||
* Respiratory Development - All (28939) Review (5876) Free Full Text (7203) | |||
'''Search Pubmed:''' [http://www.ncbi.nlm.nih.gov/sites/entrez?db=pubmed&cmd=search&term=respiratory+system+development Respiratory System Development] | [http://www.ncbi.nlm.nih.gov/sites/entrez?db=pubmed&cmd=search&term=respiratory+development Respiratory Development] | |||
==Terms== | |||
{{Respiratory terms}} | |||
==Additional Images== | ==Additional Images== | ||
===Upper | ===Upper Respiratory Tract=== | ||
<gallery> | <gallery> | ||
File:Head_arches_cartoon.jpg|Head arches cartoon | File:Head_arches_cartoon.jpg|Head arches cartoon | ||
File:Pharynx_cartoon.jpg|Pharynx | File:Pharynx_cartoon.jpg|Pharynx | ||
| Line 77: | Line 472: | ||
File:Pharynx.jpg|Pharynx | File:Pharynx.jpg|Pharynx | ||
File:Larynx.jpg|Larynx | File:Larynx.jpg|Larynx | ||
File:Gray0953.jpg | |||
</gallery> | </gallery> | ||
===Lower | ===Lower Respiratory Tract=== | ||
<gallery> | <gallery> | ||
File:Model Sox9 lung development 01.jpg|Model Sox9 lung development PMID 24274029 | |||
File:Human right lung 7-8 weeks.jpg|Human right lung 7-8 weeks PMID 24693478 | |||
File:Mouse respiratory 36 somites.jpg|Mouse 36 somites PMID 25114215 | |||
File:Mouse respiratory 44 somites.jpg|Mouse 44 somites PMID 25114215 | |||
File:Mouse respiratory 48 somites.jpg|Mouse 48 somites PMID 25114215 | |||
File:Mouse respiratory 54 somites.jpg|Mouse 54 somites PMID 25114215 | |||
File:Mouse respiratory 60 somites.jpg|Mouse 60 somites PMID 25114215 | |||
</gallery> | |||
===Historic Images=== | |||
{{Historic Disclaimer}} | |||
<gallery> | |||
File:Gray0947.jpg | |||
File:Gray0982a.jpg|week 4 early respiratory endodermal bud | File:Gray0982a.jpg|week 4 early respiratory endodermal bud | ||
File:Gray0982b.jpg|week 4 later ventral endoderm growth | File:Gray0982b.jpg|week 4 later ventral endoderm growth | ||
File:Bronchi lungs.jpg|lower respiratory tract | File:Bronchi lungs.jpg|lower respiratory tract | ||
File:Respiratory tract.jpg|conducting system bronchi to lungs | File:Respiratory tract.jpg|conducting system bronchi to lungs | ||
File:Gray0974.jpg|secondary lobule from the human lung | |||
File:Gray0975.jpg|longitudinal section of a primary lung lobule | |||
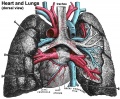
File:Historic-lungs.jpg|heart and lungs | |||
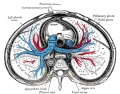
File:Gray0968.jpg|transverse section of the thorax showing the middle and posterior mediastinum | |||
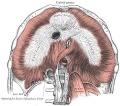
File:Gray0391.jpg|Adult diaphragm | |||
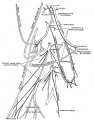
File:Gray0804.jpg|Adult cervical plexus (phrenic nerve shown lower right) | |||
</gallery> | |||
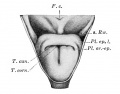
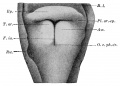
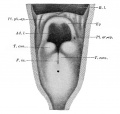
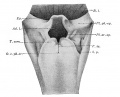
{{Ref-Frazer1910}} | |||
<gallery caption=Larynx> | |||
File:Frazer1910 fig01.jpg|embryo 5 mm | |||
File:Frazer1910 fig02.jpg|embryo 6 mm | |||
File:Frazer1910 fig03.jpg|embryo 7.5 mm | |||
File:Frazer1910 fig04.jpg|embryo 8.5 mm | |||
File:Frazer1910 fig05.jpg|embryo 12 mm | |||
File:Frazer1910 fig06.jpg|embryo 6.6 mm | |||
File:Frazer1910 fig07.jpg|embryo 22 mm | |||
File:Frazer1910 fig08.jpg|embryo 35 mm | |||
File:Frazer1910 fig09.jpg|embryo 9.5 mm | |||
File:Frazer1910 fig10.jpg|fig 10 | |||
File:Frazer1910 fig11.jpg|fig 11 | |||
File:Frazer1910 fig12.jpg|fig 12 | |||
File:Frazer1910 fig13.jpg|fig 13 | |||
File:Frazer1910 fig14.jpg|fig 14 | |||
File:Frazer1910 fig15.jpg|fig 15 | |||
File:Frazer1910 fig16.jpg|embryo 22 mm | |||
File:Frazer1910 fig17.jpg|fig 17 | |||
File:Frazer1910 fig18.jpg|embryo 18 mm | |||
File:Frazer1910 fig19.jpg|fig 19 | |||
</gallery> | |||
{{Ref-KeibelMall1912}} | |||
<gallery caption=“Respiratory Development"> | |||
File:Keibel_Mall_2_331.jpg|embryo 2.5 mm (Rob. Meyer No. 300) | |||
File:Keibel_Mall_2_332.jpg|Lung embryo 4.25 mm | |||
File:Keibel_Mall_2_333.jpg|Lung left embryo 4.25 mm | |||
File:Keibel_Mall_2_334.jpg|larynx entrance embryo 8 mm | |||
File:Keibel_Mall_2_335.jpg|larynx entrance embryo 8-9 mm (28-29 days) | |||
File:Keibel_Mall_2_336.jpg|larynx embryo 8-9 mm (28-29 days) | |||
File:Keibel_Mall_2_337.jpg|larynx entrance embryo 15-16 mm (40-42 days) | |||
File:Keibel_Mall_2_338.jpg|larynx entrance embryo 30 mm | |||
File:Keibel_Mall_2_339.jpg|larynx entrance embryo of 16/23 cm | |||
File:Keibel_Mall_2_340.jpg|larynx entrance embryo of 29/43 cm | |||
File:Keibel_Mall_2_341.jpg|Epithelial lung embryo 18.5 mm (Rob. Meyer No. 338) | |||
File:Keibel_Mall_2_342.jpg|Epithelial lung embryo 28.7 mm (Chr. 1) | |||
File:Keibel_Mall_2_343.jpg|Lung week 5 | |||
File:Keibel_Mall_2_344.jpg|Lung week 5 | |||
File:Keibel_Mall_2_345.jpg|lung embryo 10.5 mm (N) | |||
File:Keibel_Mall_2_346.jpg|ight lung fetus of 100 mm | |||
File:Keibel_Mall_2_347.jpg|mesodermal lungs embryo of 5 mm | |||
File:Keibel_Mall_2_348.jpg|Mesodermal lung embryo 7 mm (Chr. 1) | |||
File:Keibel_Mall_2_349.jpg|Mesodermal lung embryo 15 mm | |||
File:Keibel_Mall_2_350.jpg|Mesodermal lung embryo 15 mm | |||
File:Keibel_Mall_2_351.jpg|R Lung embryo 17.5 mm | |||
File:Keibel_Mall_2_352.jpg|L Lung embryo 17.5 mm | |||
File:Keibel_Mall_2_353.jpg|lobation of the lung | |||
</gallery> | </gallery> | ||
== | ==External Links== | ||
{{External Links}} | |||
{{Systems}} | |||
{{Glossary}} | |||
{{ | {{Footer}} | ||
[[Category:System | [[Category:System Development]] | ||
Latest revision as of 02:10, 25 August 2023
| Embryology - 22 Jun 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction

The respiratory system does not carry out its physiological function (of gas exchange) until after birth. The respiratory tract, diaphragm and lungs do form early in embryonic development. The respiratory tract is divided anatomically into 2 main parts:
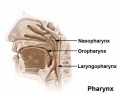
- upper respiratory tract, consisting of the nose, nasal cavity and the pharynx
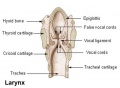
- lower respiratory tract consisting of the larynx, trachea, bronchi and the lungs.
In the head/neck region, the pharynx forms a major arched cavity within the phrayngeal arches. The lungs go through 4 distinct histological phases of development and in late fetal development thyroid hormone, respiratory motions and amniotic fliud are thought to have a role in lung maturation. Branching is a key mechanism/process in lung development leading to alveolar saccules after about 23 branching generations (range of 18–30).
The two main respiratory cell types, squamous alveolar type 1 and alveolar type 2 (surfactant secreting), both arise from the same bi-potetial progenitor cell.[1] The third main cell type are macrophages (dust cells) that arise from blood monocyte cells.
Development of this system is not completed until the last weeks of Fetal development, just before birth. Therefore premature babies have difficulties associated with insufficient surfactant (end month 6 alveolar cells type 2 appear and begin to secrete surfactant).
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Respiratory Development | Lung Embryology | Lung Development | Alveolar Embryology | |
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
Clinical
|
Textbooks
- Moore, K.L., Persaud, T.V.N. & Torchia, M.G. (2015). The developing human: clinically oriented embryology (10th ed.). Philadelphia: Saunders. Chapter 10 Respiratory System
- Schoenwolf, G.C., Bleyl, S.B., Brauer, P.R., Francis-West, P.H. & Philippa H. (2015). Larsen's human embryology (5th ed.). New York; Edinburgh: Churchill Livingstone. Chapter 11 Development of the Respiratory System and Body Cavities
- Before We Are Born (5th ed.) Moore and Persaud Chapter 13 p255-287
- Essentials of Human Embryology Larson Chapter 9 p123-146
- Human Embryology Fitzgerald and Fitzgerald Chapter 19,20 p119-123
- Anatomy of the Human Body 1918 Henry Gray The Respiratory Apparatus
Objectives
- Describe the development of the respiratory system from the endodermal and mesodermal components.
- Describe the main steps in the development of the lungs.
- Describe the development of the diaphragm and thoracic cavities.
- List the respiratory changes before and after birth.
- Describe the developmental aberrations responsible for the following malformations: tracheo - oesophageal fistula (T.O.F); oesphageal atresia; diaphragmatic hernia; lobar emphysema.
Development Overview
Week 4 - laryngotracheal groove forms on floor foregut.
Week 5 - left and right lung buds push into the pericardioperitoneal canals (primordia of pleural cavity)
Week 6 - descent of heart and lungs into thorax. Pleuroperitoneal foramen closes.
Week 7 - enlargement of liver stops descent of heart and lungs.
Month 3-6 - lungs appear glandular, end month 6 alveolar cells type 2 appear and begin to secrete surfactant.
Month 7 - respiratory bronchioles proliferate and end in alveolar ducts and sacs.
Mechanisms
- Initiation - Budding of foregut endoderm to generate the trachea.
- Branching - A repeated mechanism of branching that is ongoing throughout development to form the conducting bronchioles then alveolar ducts.
- Surface area increase - Expansion of the surface area in late development generating eventually the thin air–blood barrier for gas exchange in the acini.
- Vascular development - Extension of a vascular capillary tree within the connective tissue and wall of the acini for gas exchange, and the lymphatic development for immunology of the lungs.
- Surfactant development - allows lung inflation and decreases the work of breathing and also related to immunology of the lungs.
- Musculoskeletal development - contributes the mechanical elements of ribs, intercostals and diaphragm required for breathing.
Lung Development Stages
The sequence is most important rather than the actual timing, which is variable both in development and in the existing literature.
| Lung Stage | Human | Features | Vascular | |
|---|---|---|---|---|
| Embryonic | week 4 to 5 | lung buds originate as an outgrowth from the ventral wall of the foregut where lobar division occurs | extra pulmonary artery then lobular artery | |
| Pseudoglandular | week 5 to 17 | conducting epithelial tubes surrounded by thick mesenchyme are formed, extensive airway branching | Pre-acinar arteries | |
| Canalicular | week 16 to 25 | bronchioles are produced, increasing number of capillaries in close contact with cuboidal epithelium and the beginning of alveolar epithelium development | Intra-acinar arteries | |
| Saccular | week 24 to 40 | alveolar ducts and air sacs are developed | alveolar duct arteries | |
| Alveolar | late fetal to 8 years | secondary septation occurs, marked increase of the number and size of capillaries and alveoli | alveolar capillaries | |
| embryonic stage - pseudoglandular stage - canalicular stage - saccular stage - alveolar stage Links: Species Stage Comparison | respiratory | ||||
| Stage | Human | rabbit | sheep | mouse | rat | monkey |
|---|---|---|---|---|---|---|
| Embryonic | 4 to 7 weeks (E26 – E49) | n.d. – E18 | E17 – E30 | E9.5 – E12 | E11 – E13 | n.d. – E55 |
| Pseudoglandular | week 5 to 17 | E18 – E24 | E30 – E85 | E12 – E16.5 | E13 – E18.5 | E55 – E85 |
| Canalicular | week 16 to 25 | E23 – E27 | E80 – E120 | E16.5 – E17.5 | E18.5 – E20 | E75 – E115 |
| Saccular | week 24 to 38 | E27 – E30 | E110 – E140 | E17.5 – P4 | E21 – P4 | E105 – term |
| Alveolar (can be subdivided) | ||||||
| Alveolar Phase 1 | 36 weeks (preterm) – 3 years | E30 – term (E31) | E120 – term (E145) | P4 – P21 | P4 – P21 | E125 – greater P180 |
| Alveolar Phase 2 | term 3 – 21 years | term (E31) - n.d. | term (E145) - n.d. | P14 – young adulthood | P14 – young adulthood | P180 – young adulthood (7–8 years) |
| Table Data[10] Links: Human stages table | respiratory | ||||||
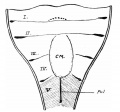
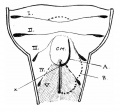
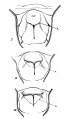
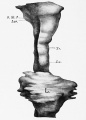
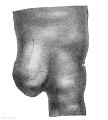
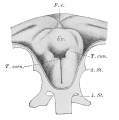
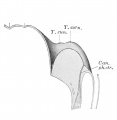
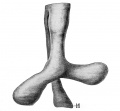
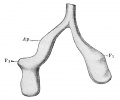
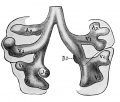
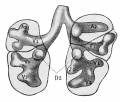
Embryonic stage
| Human Embryonic Lung Development | ||
|---|---|---|
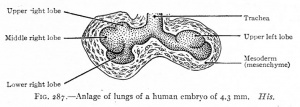
|
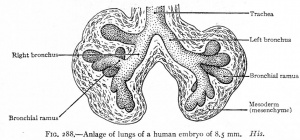
|
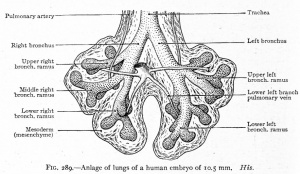
|
| CRL 4.3 mm, Week 4-5, Stage 12 to 13 | CRL 8.5 mm, Week 5, Stage 15 to 16 | CRL 10.5 mm, Week 6 Stage 16 to 17 |
- Endoderm - tubular ventral growth from foregut pharynx.
- Mesoderm - mesenchyme of lung buds.
- Intraembryonic coelom - pleural cavities elongated spaces connecting pericardial and peritoneal spaces.
- Vascular - extra pulmonary artery then lobular artery.
Pseudoglandular stage
|
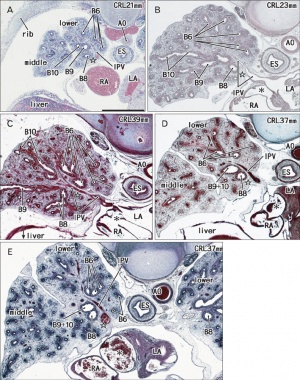
Human lung pseudoglandular stage[18] |
Canalicular stage
- week 16 - 24
- canalicular phase of the bronchus can be mixed with the pseudoglandular phase.
- Lung morphology changes dramatically, beginning of alveolar epithelium development.
- differentiation of the pulmonary epithelium results in the formation of the future air-blood tissue barrier.
- Surfactant synthesis.
- future gas exchange regions can be distinguished from the future conducting airways of the lungs.
- Vascular - Intra-acinar arteries, canalization of the lung parenchyma by capillaries begins, increasing number of capillaries in close contact with cuboidal epithelium.
Saccular stage
|
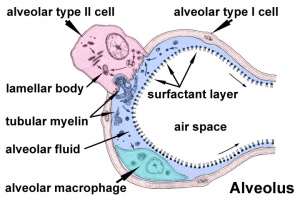
Alveolar sac structure |
Alveolar stage
Premature babies have difficulties associated with insufficient surfactant (end month 6 alveolar cells type 2 appear and begin to secrete surfactant). Lung growth continues postnatally to 20-23 years. |
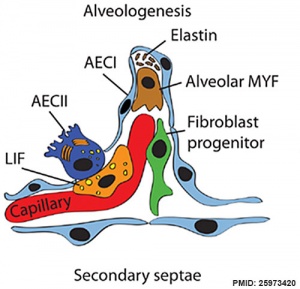
Respiratory secondary septum[19] |
Surfactant
Pulmonary surfactant or simply surfactant (surface active agent) begins to be produced at the canalicular stage and both production and turnover are key for development. It is a mixture of lipids and proteins secreted by Type 2 alveolar cells between alveolar epithelium that reduces surface tension (detergent) at the air-liquid interface. The function of this secretion is to prevent collapse of the lung at the end of expiration. In humans, these cells and their secretion develop towards the very end of the third trimester, just before birth.
Surfactant is mainly phosphatidylcholine (PC) 80% in turn consisting of which dipalmitoyl-PC, palmitoyl-myristoyl-PC and palmitoyl-palmitoleoyl-PC together 75%, anionic phosphatidylglycerol and cholesterol are about 10% each.[20]
The surfactant proteins (SP) SP-A to -D comprise only about 2-5%. Surfactant protein D (SP-D) a multimeric collectin (collagen-containing C-type lectin) involved in innate immunity (anti-microbial)[21] and expressed in pulmonary and non-pulmonary epithelia.[22] Surfactant protein B (SP-B) and disaturated-phosphatidylcholine have both been shown to be higher in preterms with chorioamnionitis.[23]
Clinically surfactants used for surfactant replacement therapy are animal-derived preparations, commonly bovine (beractant, bovactant, BLES) or less common porcine (butantan, poractant-α and surfacen).[24]
Respiratory Species Comparison
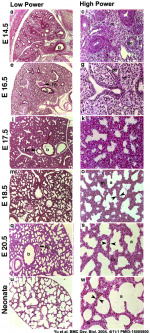
Different species undergo lung development stages over different time courses[26] and some species ( mouse and rat) do not possess any respiratory bronchioles, the acini and the ventilatory units are therefore the same entity.
| Respiratory Stages - Species Comparison - Stages Gestational age (days) | |||||
|---|---|---|---|---|---|
| Species | Term | Embryonic | Pseudoglandular | Canalicular | Saccular |
| human | 280 | < 42 | 52 - 112 | 112 - 168 | 168 |
| primate | 168 | < 42 | 57 - 80 | 80 - 140 | 140 |
| sheep | 150 | < 40 | 40 - 80 | 80 - 120 | 120 |
| rabbit | 32 | < 18 | 21 - 24 | 24 - 27 | 27 |
| rat | 22 | < 13 | 16 - 19 | 19 - 20 | 21 |
| mouse | 20 | < 9 | 16 | 18 | 19 |
| Data modified from[27]
Links: respiratory | Respiratory Comparison | Mouse Human Respiratory | Mouse respiratory stages | mouse | rat | rabbit | Timeline Comparisons | |||||
Mouse
Note that the model mouse respiratory system differs from human in size, distribution of cell types, and the time taken to develop. Additionally, the common laboratory mouse model (C57BL/6J} completely lacks respiratory breathing movements seen in the human fetus.[28]
Human and mouse Sox expression[29]
The following images are from a recent study of the development of bronchial branching in he mouse between E10 to E14.[30]
Mesenchyme (red) and epithelium (blue) the study used knockout mice to show the role of Wnt signalling in branching morphogenesis.
| Mouse lung E12.5 to E18.5 | |||
|---|---|---|---|

|
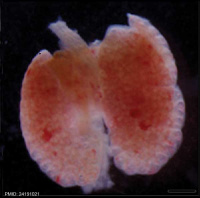
|
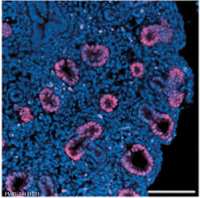
|
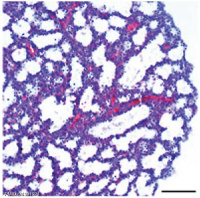
|
| E12.5 lungs | E14.5 lungs | E14.5 Sox9 | E18.5 lungs |
| Reference[31] | |||
- Links: Wnt | Mouse Development
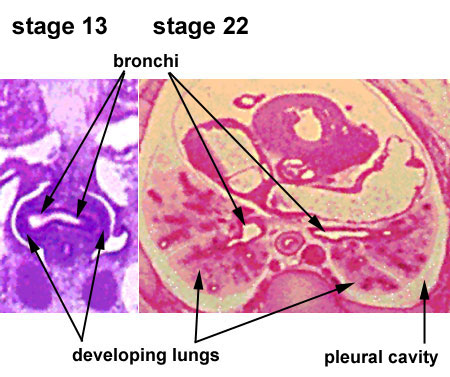
Embryonic Respiratory Development
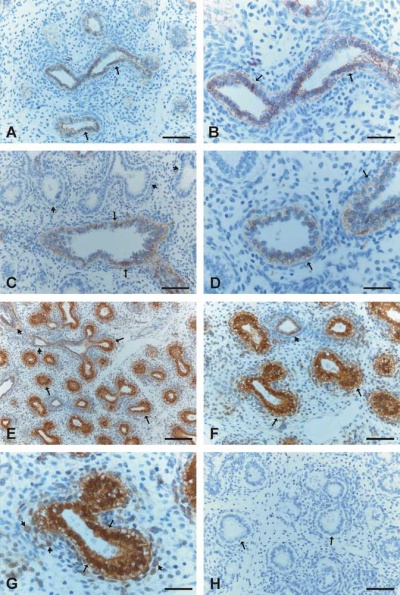
Pseudoglandular Respiratory Development
Pseudoglandular period identified in this paper (GA weeks 12 to 16)
Human lung at pseudoglandular stage showing E- and N-cadherin and β-catenin localization.[32]
Endocrine Lung
| Neonatal Human | Fetal Rabbit |
|---|---|
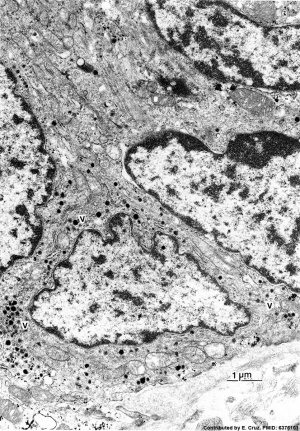
|
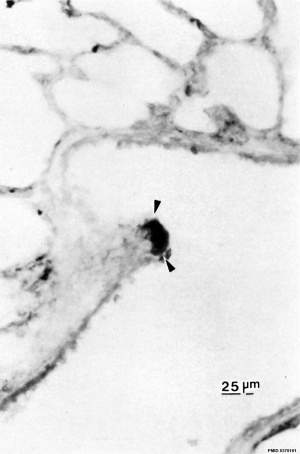
|
| Pulmonary neuroendocrine cell (EM)[33] | Neuroepithelial body[33] |
Pulmonary neuroendocrine cells (PNECs)
- develop in late embryonic to early fetal period.[34][35]
- later in mid-fetal period clusters of these cells form neuroepithelial bodies (NEBs).
- first cell type to differentiate in the airway epithelium.
- differentiation regulated by proneural genes - mammalian homolog of the achaete-scute complex (Mash-1) and hairy and enhancer of split1 (Hes-1).[36]
- located in the fetal lung at bronchiole branching points.
- may stimulate mitosis to increase branching.
- secrete 2 peptides - gastrin-releasing peptide (GRP) and calcitonin gene related peptide (CGRP)
- Links: Endocrine - Other Tissues | OMIM - GRP | OMIM - CGRP
Lung Histology
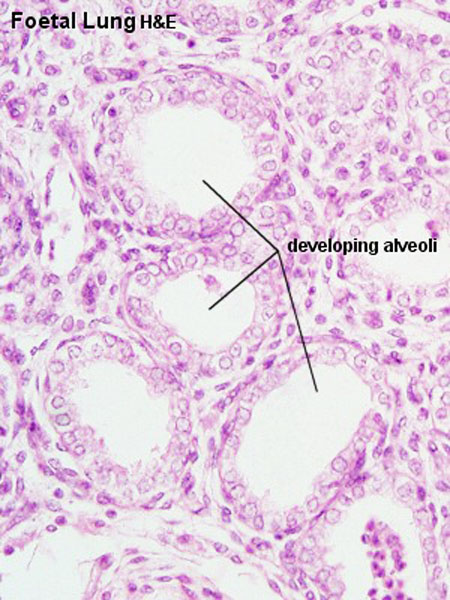
|
| Fetal lung histology |
Birth Changes
At birth the lung epithelium changes from a prenatal secretory to a postnatal absorptive function. Several factors have been identified as influencing this transport change including: epinephrine, oxygen, glucocorticoids, and thyroid hormones (for review see[37])
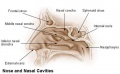
Upper Respiratory Tract
- part of foregut development
- anatomically the nose, nasal cavity and the pharynx
- the pharynx forms a major arched cavity within the pharyngeal arches
Movies
The animations below allow a comparison of early and late embryonic lung development. Compare the size and relative position of the respiratory structures and their anatomical relationship to the developing gastrointestinal tract.
|
Early embryo (stage 13)
3 dimensional reconstruction based upon a serial reconstruction from individual Carnegie stage 13 embryo slice images. |
|
Late embryo (stage 22)
3 dimensional reconstruction based upon a serial reconstruction from individual embryo slice images Carnegie stage 22, 27 mm Human embryo, approximate day 56. |
Lung Cardiovascular
Pulmonary Circulation
- pulmonary arteries and veins arise by vasculogenesis[38]
Pulmonary Veins
- vasculogenesis in the mesenchyme surrounding the terminal buds during the pseudoglandular stage.
- vasculogenesis - describes the formation of new blood vessels from pluripotent precursor cells.
- angiogenesis in the canalicular and alveolar stages.
- angiogenesis - describes the formation of new vessels from pre-existing vessels.
See also review[39]
Bronchial Circulation
Bronchial Arteries
- vascularising the walls of the airways and the large pulmonary vessels providing giving oxygen and nutrients.
- extend within the bronchial tree to the periphery of the alveolar ducts.
- not found in the lungs until around 8 weeks of gestation.
- one or two small vessels extend from the dorsal aorta and run into the lung alongside the cartilage plates of the main bronchus.
Bronchial Veins
- small bronchial veins within the airway wall drain into the pulmonary veins.
- large bronchial veins seen close to the hilum and drain into the cardinal veins and the right atrium.
See review[39]
Molecular
| Factor Links: AMH | hCG | BMP | sonic hedgehog | bHLH | HOX | FGF | FOX | Hippo | LIM | Nanog | NGF | Nodal | Notch | PAX | retinoic acid | SIX | Slit2/Robo1 | SOX | TBX | TGF-beta | VEGF | WNT | Category:Molecular |
TBX

|
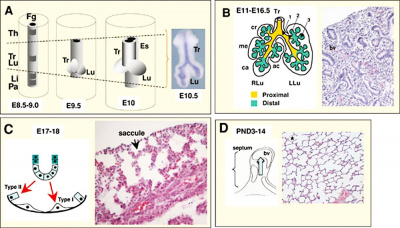
|
| Mouse respiratory Tbx4 and Tbx5 model[40] | Mouse respiratory development[41]]] |
- Nkx2-1 (Titf1) - ventral wall of the anterior foregut, identifies the future trachea.
SOX
- Sox2 is essential for the initiation of lung development from the endodermal gut tube,
- Sox9 is essential for maintaining the tips and associated branching.
Several different Sox types are required for different stages of respiratory development. Wnt/β-catenin signaling does not regulate Sox9 expression in the lung.[31]
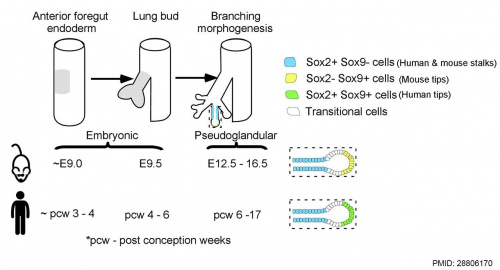
Human and mouse Sox expression[29]
FGF
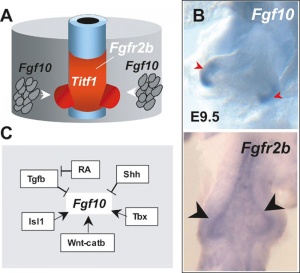
- Localized Fgf10 expression not required for lung branching but prevents epithelial differentiation[42] "As the lung buds grow out, proximal epithelial cells become further and further displaced from the distal source of Fgf10 and differentiate into bronchial epithelial cells. Interestingly, our data presented here show that once epithelial cells are committed to the Sox2-positive airway epithelial cell fate, Fgf10 prevents ciliated cell differentiation and promotes basal cell differentiation."
- Opposing Fgf and Bmp activities regulate the specification of olfactory sensory and respiratory epithelial cell fates[43] " In this study, we provide evidence that in both chick and mouse, Bmp signals promote respiratory epithelial character, whereas Fgf signals are required for the generation of sensory epithelial cells. Moreover, olfactory placodal cells can switch between sensory and respiratory epithelial cell fates in response to Fgf and Bmp activity, respectively. Our results provide evidence that Fgf activity suppresses and restricts the ability of Bmp signals to induce respiratory cell fate in the nasal epithelium."
BMP
Bone morphogenic protein 4 (Bmp4) acts as in an autocrine signalling mechanism to limit bud outgrowth and is therefore involved in branching.
Nkx2-1
Transcriptional control of lung alveolar type 1 cell development and maintenance by NK homeobox 2-1 PNAS "Gas exchange in the lung relies on passive diffusion of oxygen and carbon dioxide across an extraordinarily thin epithelium that is nearly entirely made of the poorly understood alveolar type 1 (AT1) cell. Our study shows that all AT1 cells express and require NK homeobox 2-1 (Nkx2-1) for their development and maintenance. Nkx2-1 mutant AT1 cells lose their characteristic molecular and cellular features and transform toward a gastrointestinal fate, highlighting remarkable plasticity of an otherwise terminally differentiated cell type. This work establishes NKX2-1 as the first overarching factor in the AT1 cell transcriptional hierarchy and paves the way for unraveling not only the unique biology of AT1 cells but also cell type-specific roles of a lineage transcription factor." See also 2012 review paper Signaling Networks Regulating Development of the Lower Respiratory Tract
The NKX2-1 gene encodes a transcription factor that is expressed during early development of thyroid, lung, and neural (forebrain regions including basal ganglia and hypothalamus). NKX2-1 was originally called thyroid transcription factor-1 (TTF1) due to the fact that it mediated thyroid-specific gene transcription.
Links: OMIM Nkx2-1
Other
- Heparan sulfate in lung morphogenesis[44] "Heparan sulfate (HS) is a structurally complex polysaccharide located on the cell surface and in the extracellular matrix, where it participates in numerous biological processes through interactions with a vast number of regulatory proteins such as growth factors and morphogens. ...he potential contribution of HS to abnormalities of lung development has yet to be explored to any significant extent, which is somewhat surprising given the abnormal lung phenotype exhibited by mutant mice synthesizing abnormal HS."
- Signaling via Alk5 controls the ontogeny of lung Clara cells[45] "Clara cells, together with ciliated and pulmonary neuroendocrine cells, make up the epithelium of the bronchioles along the conducting airways. Clara cells are also known as progenitor or stem cells during lung regeneration after injury. ...Using lung epithelial cells, we show that Alk5-regulated Hes1 expression is stimulated through Pten and the MEK/ERK and PI3K/AKT pathways. Thus, the signaling pathway by which TGFbeta/ALK5 regulates Clara cell differentiation may entail inhibition of Pten expression, which in turn activates ERK and AKT phosphorylation."
- Wt1 and retinoic acid signaling in the subcoelomic mesenchyme control the development of the pleuropericardial membranes and the sinus horns[46] "Pericardium and sinus horn formation are coupled and depend on the expansion and correct temporal release of pleuropericardial membranes from the underlying subcoelomic mesenchyme. Wt1 and downstream Raldh2/retinoic acid signaling are crucial regulators of this process."
References
- ↑ 1.0 1.1 Desai TJ, Brownfield DG & Krasnow MA. (2014). Alveolar progenitor and stem cells in lung development, renewal and cancer. Nature , 507, 190-4. PMID: 24499815 DOI.
- ↑ 2.0 2.1 Yamamoto M, Wilting J, Abe H, Murakami G, Rodríguez-Vázquez JF & Abe SI. (2018). Development of the pulmonary pleura with special reference to the lung surface morphology: a study using human fetuses. Anat Cell Biol , 51, 150-157. PMID: 30310706 DOI.
- ↑ 3.0 3.1 Watson JK, Rulands S, Wilkinson AC, Wuidart A, Ousset M, Van Keymeulen A, Göttgens B, Blanpain C, Simons BD & Rawlins EL. (2015). Clonal Dynamics Reveal Two Distinct Populations of Basal Cells in Slow-Turnover Airway Epithelium. Cell Rep , 12, 90-101. PMID: 26119728 DOI.
- ↑ Fujii S, Muranaka T, Matsubayashi J, Yamada S, Yoneyama A & Takakuwa T. (2023). Bronchial tree of the human embryo: Examination based on a mammalian model. J Anat , , . PMID: 37602519 DOI.
- ↑ Little DR, Gerner-Mauro KN, Flodby P, Crandall ED, Borok Z, Akiyama H, Kimura S, Ostrin EJ & Chen J. (2019). Transcriptional control of lung alveolar type 1 cell development and maintenance by NK homeobox 2-1. Proc. Natl. Acad. Sci. U.S.A. , 116, 20545-20555. PMID: 31548395 DOI.
- ↑ Karolak JA, Vincent M, Deutsch G, Gambin T, Cogné B, Pichon O, Vetrini F, Mefford HC, Dines JN, Golden-Grant K, Dipple K, Freed AS, Leppig KA, Dishop M, Mowat D, Bennetts B, Gifford AJ, Weber MA, Lee AF, Boerkoel CF, Bartell TM, Ward-Melver C, Besnard T, Petit F, Bache I, Tümer Z, Denis-Musquer M, Joubert M, Martinovic J, Bénéteau C, Molin A, Carles D, André G, Bieth E, Chassaing N, Devisme L, Chalabreysse L, Pasquier L, Secq V, Don M, Orsaria M, Missirian C, Mortreux J, Sanlaville D, Pons L, Küry S, Bézieau S, Liet JM, Joram N, Bihouée T, Scott DA, Brown CW, Scaglia F, Tsai AC, Grange DK, Phillips JA, Pfotenhauer JP, Jhangiani SN, Gonzaga-Jauregui CG, Chung WK, Schauer GM, Lipson MH, Mercer CL, van Haeringen A, Liu Q, Popek E, Coban Akdemir ZH, Lupski JR, Szafranski P, Isidor B, Le Caignec C & Stankiewicz P. (2019). Complex Compound Inheritance of Lethal Lung Developmental Disorders due to Disruption of the TBX-FGF Pathway. Am. J. Hum. Genet. , , . PMID: 30639323 DOI.
- ↑ Schittny JC. (2018). How high resolution 3-dimensional imaging changes our understanding of postnatal lung development. Histochem. Cell Biol. , 150, 677-691. PMID: 30390117 DOI.
- ↑ Nikolić MZ, Sun D & Rawlins EL. (2018). Human lung development: recent progress and new challenges. Development , 145, . PMID: 30111617 DOI.
- ↑ Gouveia L, Betsholtz C & Andrae J. (2018). PDGF-A signaling is required for secondary alveolar septation and controls epithelial proliferation in the developing lung. Development , 145, . PMID: 29636361 DOI.
- ↑ 10.0 10.1 Gauthier TW & Brown LA. (2017). In utero alcohol effects on foetal, neonatal and childhood lung disease. Paediatr Respir Rev , 21, 34-37. PMID: 27613232 DOI.
- ↑ Yang J, Hernandez BJ, Martinez Alanis D, Narvaez del Pilar O, Vila-Ellis L, Akiyama H, Evans SE, Ostrin EJ & Chen J. (2016). The development and plasticity of alveolar type 1 cells. Development , 143, 54-65. PMID: 26586225 DOI.
- ↑ Mori M, Mahoney JE, Stupnikov MR, Paez-Cortez JR, Szymaniak AD, Varelas X, Herrick DB, Schwob J, Zhang H & Cardoso WV. (2015). Notch3-Jagged signaling controls the pool of undifferentiated airway progenitors. Development , 142, 258-67. PMID: 25564622 DOI.
- ↑ Chang DR, Martinez Alanis D, Miller RK, Ji H, Akiyama H, McCrea PD & Chen J. (2013). Lung epithelial branching program antagonizes alveolar differentiation. Proc. Natl. Acad. Sci. U.S.A. , 110, 18042-51. PMID: 24058167 DOI.
- ↑ Yoshimi T, Hashimoto F, Takahashi S & Takahashi Y. (2010). Suppression of embryonic lung branching morphogenesis by antisense oligonucleotides against HOM/C homeobox factors. In Vitro Cell. Dev. Biol. Anim. , 46, 664-72. PMID: 20535580 DOI.
- ↑ Chen F, Cao Y, Qian J, Shao F, Niederreither K & Cardoso WV. (2010). A retinoic acid-dependent network in the foregut controls formation of the mouse lung primordium. J. Clin. Invest. , 120, 2040-8. PMID: 20484817 DOI.
- ↑ Fawke J, Lum S, Kirkby J, Hennessy E, Marlow N, Rowell V, Thomas S & Stocks J. (2010). Lung function and respiratory symptoms at 11 years in children born extremely preterm: the EPICure study. Am. J. Respir. Crit. Care Med. , 182, 237-45. PMID: 20378729 DOI.
- ↑ Solomon M, Grasemann H & Keshavjee S. (2010). Pediatric lung transplantation. Pediatr. Clin. North Am. , 57, 375-91, table of contents. PMID: 20371042 DOI.
- ↑ Abe S, Yamamoto M, Noguchi T, Yoshimoto T, Kinoshita H, Matsunaga S, Murakami G & Rodríguez-Vázquez JF. (2014). Fetal development of the minor lung segment. Anat Cell Biol , 47, 12-7. PMID: 24693478 DOI.
- ↑ Chao CM, El Agha E, Tiozzo C, Minoo P & Bellusci S. (2015). A breath of fresh air on the mesenchyme: impact of impaired mesenchymal development on the pathogenesis of bronchopulmonary dysplasia. Front Med (Lausanne) , 2, 27. PMID: 25973420 DOI.
- ↑ Bernhard W. (2016). Lung surfactant: Function and composition in the context of development and respiratory physiology. Ann. Anat. , 208, 146-150. PMID: 27693601 DOI.
- ↑ Sorensen GL. (2018). Surfactant Protein D in Respiratory and Non-Respiratory Diseases. Front Med (Lausanne) , 5, 18. PMID: 29473039 DOI.
- ↑ Vieira F, Kung JW & Bhatti F. (2017). Structure, genetics and function of the pulmonary associated surfactant proteins A and D: The extra-pulmonary role of these C type lectins. Ann. Anat. , 211, 184-201. PMID: 28351530 DOI.
- ↑ Verlato G, Simonato M, Giambelluca S, Fantinato M, Correani A, Cavicchiolo ME, Priante E, Carnielli V & Cogo P. (2018). Surfactant Components and Tracheal Aspirate Inflammatory Markers in Preterm Infants with Respiratory Distress Syndrome. J. Pediatr. , 203, 442-446. PMID: 30270169 DOI.
- ↑ Tridente A, De Martino L & De Luca D. (2019). Porcine vs bovine surfactant therapy for preterm neonates with RDS: systematic review with biological plausibility and pragmatic meta-analysis of respiratory outcomes. Respir. Res. , 20, 28. PMID: 30728009 DOI.
- ↑ Yu H, Wessels A, Chen J, Phelps AL, Oatis J, Tint GS & Patel SB. (2004). Late gestational lung hypoplasia in a mouse model of the Smith-Lemli-Opitz syndrome. BMC Dev. Biol. , 4, 1. PMID: 15005800 DOI.
- ↑ Lewin G & Hurtt ME. (2017). Pre- and Postnatal Lung Development: An Updated Species Comparison. Birth Defects Res , 109, 1519-1539. PMID: 28876535 DOI.
- ↑ Pinkerton KE & Joad JP. (2000). The mammalian respiratory system and critical windows of exposure for children's health. Environ. Health Perspect. , 108 Suppl 3, 457-62. PMID: 10852845
- ↑ Kleven GA & Ronca AE. (2009). Prenatal behavior of the C57BL/6J mouse: a promising model for human fetal movement during early to mid-gestation. Dev Psychobiol , 51, 84-94. PMID: 18980217 DOI.
- ↑ 29.0 29.1 Waghray A & Rajagopal J. (2017). Tips from the embryonic lung. Elife , 6, . PMID: 28806170 DOI.
- ↑ Kadzik RS, Cohen ED, Morley MP, Stewart KM, Lu MM & Morrisey EE. (2014). Wnt ligand/Frizzled 2 receptor signaling regulates tube shape and branch-point formation in the lung through control of epithelial cell shape. Proc. Natl. Acad. Sci. U.S.A. , 111, 12444-9. PMID: 25114215 DOI.
- ↑ 31.0 31.1 Rockich BE, Hrycaj SM, Shih HP, Nagy MS, Ferguson MA, Kopp JL, Sander M, Wellik DM & Spence JR. (2013). Sox9 plays multiple roles in the lung epithelium during branching morphogenesis. Proc. Natl. Acad. Sci. U.S.A. , 110, E4456-64. PMID: 24191021 DOI.
- ↑ Kaarteenaho R, Lappi-Blanco E & Lehtonen S. (2010). Epithelial N-cadherin and nuclear β-catenin are up-regulated during early development of human lung. BMC Dev. Biol. , 10, 113. PMID: 21080917 DOI.
- ↑ 33.0 33.1 DiAugustine RP & Sonstegard KS. (1984). Neuroendocrinelike (small granule) epithelial cells of the lung. Environ. Health Perspect. , 55, 271-95. PMID: 6376101
- ↑ Cutz E. (1982). Neuroendocrine cells of the lung. An overview of morphologic characteristics and development. Exp. Lung Res. , 3, 185-208. PMID: 6188605
- ↑ Cutz E, Gillan JE & Bryan AC. (1985). Neuroendocrine cells in the developing human lung: morphologic and functional considerations. Pediatr. Pulmonol. , 1, S21-9. PMID: 3906540
- ↑ McGovern S, Pan J, Oliver G, Cutz E & Yeger H. (2010). The role of hypoxia and neurogenic genes (Mash-1 and Prox-1) in the developmental programming and maturation of pulmonary neuroendocrine cells in fetal mouse lung. Lab. Invest. , 90, 180-95. PMID: 20027181 DOI.
- ↑ Barker PM & Olver RE. (2002). Invited review: Clearance of lung liquid during the perinatal period. J. Appl. Physiol. , 93, 1542-8. PMID: 12235057 DOI.
- ↑ Hall SM, Hislop AA & Haworth SG. (2002). Origin, differentiation, and maturation of human pulmonary veins. Am. J. Respir. Cell Mol. Biol. , 26, 333-40. PMID: 11867341 DOI.
- ↑ 39.0 39.1 Hislop AA. (2002). Airway and blood vessel interaction during lung development. J. Anat. , 201, 325-34. PMID: 12430957
- ↑ Arora R, Metzger RJ & Papaioannou VE. (2012). Multiple roles and interactions of Tbx4 and Tbx5 in development of the respiratory system. PLoS Genet. , 8, e1002866. PMID: 22876201 DOI.
- ↑ 41.0 41.1 Cardoso WV & Kotton DN. (2008). Specification and patterning of the respiratory system. , , . PMID: 20614584 DOI.
- ↑ Volckaert T, Campbell A, Dill E, Li C, Minoo P & De Langhe S. (2013). Localized Fgf10 expression is not required for lung branching morphogenesis but prevents differentiation of epithelial progenitors. Development , 140, 3731-42. PMID: 23924632 DOI.
- ↑ Maier E, von Hofsten J, Nord H, Fernandes M, Paek H, Hébert JM & Gunhaga L. (2010). Opposing Fgf and Bmp activities regulate the specification of olfactory sensory and respiratory epithelial cell fates. Development , 137, 1601-11. PMID: 20392740 DOI.
- ↑ Thompson SM, Jesudason EC, Turnbull JE & Fernig DG. (2010). Heparan sulfate in lung morphogenesis: The elephant in the room. Birth Defects Res. C Embryo Today , 90, 32-44. PMID: 20301217 DOI.
- ↑ Xing Y, Li C, Li A, Sridurongrit S, Tiozzo C, Bellusci S, Borok Z, Kaartinen V & Minoo P. (2010). Signaling via Alk5 controls the ontogeny of lung Clara cells. Development , 137, 825-33. PMID: 20147383 DOI.
- ↑ Norden J, Grieskamp T, Lausch E, van Wijk B, van den Hoff MJ, Englert C, Petry M, Mommersteeg MT, Christoffels VM, Niederreither K & Kispert A. (2010). Wt1 and retinoic acid signaling in the subcoelomic mesenchyme control the development of the pleuropericardial membranes and the sinus horns. Circ. Res. , 106, 1212-20. PMID: 20185795 DOI.
Reviews
Nikolić MZ, Sun D & Rawlins EL. (2018). Human lung development: recent progress and new challenges. Development , 145, . PMID: 30111617 DOI.
Furlow PW & Mathisen DJ. (2018). Surgical anatomy of the trachea. Ann Cardiothorac Surg , 7, 255-260. PMID: 29707503 DOI.
Mecham RP. (2018). Elastin in lung development and disease pathogenesis. Matrix Biol. , , . PMID: 29331337 DOI.
Schittny JC. (2017). Development of the lung. Cell Tissue Res. , 367, 427-444. PMID: 28144783 DOI.
Stabler CT & Morrisey EE. (2017). Developmental pathways in lung regeneration. Cell Tissue Res. , 367, 677-685. PMID: 27957616 DOI.
Herriges M & Morrisey EE. (2014). Lung development: orchestrating the generation and regeneration of a complex organ. Development , 141, 502-13. PMID: 24449833 DOI.
Stocks J, Hislop A & Sonnappa S. (2013). Early lung development: lifelong effect on respiratory health and disease. Lancet Respir Med , 1, 728-42. PMID: 24429276 DOI.
Gauthier TW & Brown LA. (2017). In utero alcohol effects on foetal, neonatal and childhood lung disease. Paediatr Respir Rev , 21, 34-37. PMID: 27613232 DOI.
Rackley CR & Stripp BR. (2012). Building and maintaining the epithelium of the lung. J. Clin. Invest. , 122, 2724-30. PMID: 22850882 DOI.
Warburton D, El-Hashash A, Carraro G, Tiozzo C, Sala F, Rogers O, De Langhe S, Kemp PJ, Riccardi D, Torday J, Bellusci S, Shi W, Lubkin SR & Jesudason E. (2010). Lung organogenesis. Curr. Top. Dev. Biol. , 90, 73-158. PMID: 20691848 DOI.
Morrisey EE & Hogan BL. (2010). Preparing for the first breath: genetic and cellular mechanisms in lung development. Dev. Cell , 18, 8-23. PMID: 20152174 DOI.
Burri PH. (2006). Structural aspects of postnatal lung development - alveolar formation and growth. Biol. Neonate , 89, 313-22. PMID: 16770071 DOI.
Merkus PJ. (2003). Effects of childhood respiratory diseases on the anatomical and functional development of the respiratory system. Paediatr Respir Rev , 4, 28-39. PMID: 12615030
Chinoy MR. (2003). Lung growth and development. Front. Biosci. , 8, d392-415. PMID: 12456356
Burri PH. (1984). Fetal and postnatal development of the lung. Annu. Rev. Physiol. , 46, 617-28. PMID: 6370120 DOI.
Articles
Mund SI, Stampanoni M & Schittny JC. (2008). Developmental alveolarization of the mouse lung. Dev. Dyn. , 237, 2108-16. PMID: 18651668 DOI.
Burri PH. (2006). Structural aspects of postnatal lung development - alveolar formation and growth. Biol. Neonate , 89, 313-22. PMID: 16770071 DOI.
Hall SM, Hislop AA & Haworth SG. (2002). Origin, differentiation, and maturation of human pulmonary veins. Am. J. Respir. Cell Mol. Biol. , 26, 333-40. PMID: 11867341 DOI.
Hall SM, Hislop AA, Pierce CM & Haworth SG. (2000). Prenatal origins of human intrapulmonary arteries: formation and smooth muscle maturation. Am. J. Respir. Cell Mol. Biol. , 23, 194-203. PMID: 10919986 DOI.
Sparrow MP, Weichselbaum M & McCray PB. (1999). Development of the innervation and airway smooth muscle in human fetal lung. Am. J. Respir. Cell Mol. Biol. , 20, 550-60. PMID: 10100986 DOI.
Search PubMed
Search April 2010
- Respiratory System Development - All (30795) Review (3706) Free Full Text (7943)
- Respiratory Development - All (28939) Review (5876) Free Full Text (7203)
Search Pubmed: Respiratory System Development | Respiratory Development
Terms
| Respiratory Terms (expand to view) |
|---|
|
| Other Terms Lists |
|---|
| Terms Lists: ART | Birth | Bone | Cardiovascular | Cell Division | Endocrine | Gastrointestinal | Genital | Genetic | Head | Hearing | Heart | Immune | Integumentary | Neonatal | Neural | Oocyte | Palate | Placenta | Radiation | Renal | Respiratory | Spermatozoa | Statistics | Tooth | Ultrasound | Vision | Historic | Drugs | Glossary |
Additional Images
Upper Respiratory Tract
Lower Respiratory Tract
Historic Images
| Historic Disclaimer - information about historic embryology pages |
|---|
| Pages where the terms "Historic" (textbooks, papers, people, recommendations) appear on this site, and sections within pages where this disclaimer appears, indicate that the content and scientific understanding are specific to the time of publication. This means that while some scientific descriptions are still accurate, the terminology and interpretation of the developmental mechanisms reflect the understanding at the time of original publication and those of the preceding periods, these terms, interpretations and recommendations may not reflect our current scientific understanding. (More? Embryology History | Historic Embryology Papers) |
Frazer JE. Development of the larynx. (1910) J Anat. 44: 156-191. PMID 17232839
- Larynx
Keibel F. and Mall FP. Manual of Human Embryology II. (1912) J. B. Lippincott Company, Philadelphia.
- “Respiratory
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
| System Links: Introduction | Cardiovascular | Coelomic Cavity | Endocrine | Gastrointestinal Tract | Genital | Head | Immune | Integumentary | Musculoskeletal | Neural | Neural Crest | Placenta | Renal | Respiratory | Sensory | Birth |
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, June 22) Embryology Respiratory System Development. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Respiratory_System_Development
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G