Abnormal Development - Cytomegalovirus: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| (5 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
{{Header}} | {{Header}} | ||
=KA62.3 Congenital cytomegalovirus infection= | =KA62.3 Congenital cytomegalovirus infection= | ||
{| | |||
|-bgcolor="FFCC00" | |||
! {{ICD-11}} {{ICD11weblink}}1515465998 Congenital cytomegalovirus infection] | |||
|-bgcolor="FEF9E7" | |||
| "A condition affecting neonates, caused by an infection with cytomegalovirus in utero. This condition is characterized by jaundice, low birth weight, splenomegaly, hepatomegaly, or pneumonia if symptoms develop shortly after birth, or may be asymptomatic. This condition commonly present later in life with loss of {{hearing}}, loss of {{vision}}, or developmental disabilities. Transmission is by vertical transmission. Confirmation is by detection of cytomegalovirus in neonatal urine, saliva, blood, or other body tissues within 2-3 weeks of birth." | |||
|} | |||
{{Viral Links}} | {{Viral Links}} | ||
==Introduction== | ==Introduction== | ||
| Line 13: | Line 14: | ||
HCMV infection is ranked as one of the most common infections in adults, with the seropositive rates ranging from 60–99% globally. In Western countries, adults with advanced AIDS prior to the introduction of highly active antiretroviral therapy (HAART) this virus also a cause of blindness (CMV retinitis) and death in patients. | In Australia, cytomegalovirus is the most common infectious cause and the second most common overall cause of congenital malformations and may be placental transmitted to the baby and can have serious consequences.<ref name=PregnancyCare2018>{{Ref-PregnancyCare2018}}</ref> HCMV infection is ranked as one of the most common infections in adults, with the seropositive rates ranging from 60–99% globally. In Western countries, adults with advanced AIDS prior to the introduction of highly active antiretroviral therapy (HAART) this virus also a cause of blindness (CMV retinitis) and death in patients. | ||
| Line 26: | Line 28: | ||
|-bgcolor="F5FAFF" | |-bgcolor="F5FAFF" | ||
| | | | ||
* '''Prenatal findings, neonatal symptoms and neurodevelopmental outcome of congenital cytomegalovirus infection in a university hospital in Montreal, Quebec'''{{#pmid:32031981|PMID32031981}} "Background Outcome of congenital cytomegalovirus (cCMV) infection in the absence of routine CMV screening and third-trimester scan in North America is scarcely documented. The aim of this study was to assess the severe outcomes related to cCMV according to the indication for screening. Methods This was a retrospective study of 84 mother-child pairs followed for cCMV between 2003 and 2017 at CHU Sainte-Justine in Montreal, Canada. Prenatal ultrasound, neonatal symptoms, neuroimaging and severe outcomes (cerebral palsy, severe cognitive impairment, bilateral hearing loss or neonatal death) were reviewed. Results Among 38 cases with abnormal prenatal ultrasound, 41.9% of live-born infants developed severe outcomes. Sixteen (42.1%) were detected in the third trimester. Among 16 cases diagnosed prenatally because of maternal history, all had normal prenatal ultrasound, and none developed severe outcomes. Among cases diagnosed postnatally because of neonatal symptoms, 25% developed severe outcomes. All infants who developed severe outcomes had moderate/severe neonatal symptoms. Conclusion Outcome of cCMV infection varies according to the reason for screening and timing of diagnosis. Any prenatal ultrasound anomaly might indicate a risk of severe outcome, and warrants a detailed ultrasound scan. However, late detection, or postnatal diagnosis, represented more than half of the cases, and awareness of this will help ensuring optimal management." | |||
* '''Survey of cellular immune responses to human cytomegalovirus infection in the microenvironment of the uterine-placental interface'''{{#pmid:31065796|PMID31065796}} "Congenital human cytomegalovirus (HCMV) infection is a leading cause of birth defects, yet there are no established treatments for preventing maternal-fetal transmission. During first trimester, HCMV replicates in basal decidua that functions as a reservoir for virus and source of transmission to the attached placenta and fetal hemiallograft but also contains immune cells, including natural killer cells, macrophages, and T cell subsets, that respond to pathogens, protecting the placenta and fetus. However, the specific cellular and cytokine responses to infection are unknown, nor are the immune correlates of protection that guide development of therapeutic strategies. Here we survey immune cell phenotypes in intact explants of basal decidua infected with a clinical pathogenic HCMV strain ex vivo and identify specific changes occurring in response to infection in the tissue environment. Using 4-color immunofluorescence microscopy, we found that at 3 days postinfection, virus replicates in decidual stromal cells and epithelial cells of endometrial glands. Infected cells and effector memory CD8+ T cells (TEM) in contact with them make IFN-γ. CD8+ TEM cells produce granulysin and cluster at sites of infection in decidua and the epithelium of endometrial glands. Quantification indicated expansion of two immune cell subtypes-CD8+ TEM cells and, to a lesser extent, iNKT cells. Approximately 20% of immune cells were found in pairs in both control and infected decidua, suggesting frequent cross-talk in the microenvironment of decidua. Our findings indicate a complex immune microenvironment in basal decidua and suggest CD8+ TEM cells play a role in early responses to decidual infection in seropositive women." | |||
* '''Sequelae of congenital cytomegalovirus (cCMV) following maternal primary infection are limited to those acquired in the first trimester of pregnancy'''{{#pmid:30596974|PMID30596974}} "Relationship between gestational age at maternal primary infection and outcome in cCMV was based on small retrospective studies between 1980 and 2011. They reported sequelae in 32% and 15% following maternal primary infection in first and second or third trimester respectively. ...These results suggest that CMV infection can be severe only when the virus hits the fetus in the embryonic or early fetal period. Recent guidelines recommend auditory follow-up for at least 5 years of all infected children. This raises parental anxiety and generates significant cost. We suggest that auditory and specialized neurologic follow-up may be recommended only to children infected from maternal infection in the first trimester." | * '''Sequelae of congenital cytomegalovirus (cCMV) following maternal primary infection are limited to those acquired in the first trimester of pregnancy'''{{#pmid:30596974|PMID30596974}} "Relationship between gestational age at maternal primary infection and outcome in cCMV was based on small retrospective studies between 1980 and 2011. They reported sequelae in 32% and 15% following maternal primary infection in first and second or third trimester respectively. ...These results suggest that CMV infection can be severe only when the virus hits the fetus in the embryonic or early fetal period. Recent guidelines recommend auditory follow-up for at least 5 years of all infected children. This raises parental anxiety and generates significant cost. We suggest that auditory and specialized neurologic follow-up may be recommended only to children infected from maternal infection in the first trimester." | ||
Latest revision as of 11:56, 17 February 2020
| Embryology - 20 Jun 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
KA62.3 Congenital cytomegalovirus infection
| ICD-11 Congenital cytomegalovirus infection |
|---|
| "A condition affecting neonates, caused by an infection with cytomegalovirus in utero. This condition is characterized by jaundice, low birth weight, splenomegaly, hepatomegaly, or pneumonia if symptoms develop shortly after birth, or may be asymptomatic. This condition commonly present later in life with loss of hearing, loss of vision, or developmental disabilities. Transmission is by vertical transmission. Confirmation is by detection of cytomegalovirus in neonatal urine, saliva, blood, or other body tissues within 2-3 weeks of birth." |
Introduction
Human cytomegalovirus (HCMV, Greek, cyto = "cell", megalo = "large") or Human Herpesvirus 5 (HHV-5) is a member of the herpes virus family. A viral infection that causes systemic infection and extensive brain damage and cell death by necrosis. Cytomegalovirus is the leading cause of congenital viral infection, with a range of incidence between 0·5–3% of live births worldwide. Approximately 30% of maternal infections during pregnancy can result in congenital infection. Neonates with congenital or perinatal cytomegalovirus infection can be asymptomatic and infection can also be transmitted postnatally from mother to infant by breastfeeding.
In Australia, cytomegalovirus is the most common infectious cause and the second most common overall cause of congenital malformations and may be placental transmitted to the baby and can have serious consequences.[2] HCMV infection is ranked as one of the most common infections in adults, with the seropositive rates ranging from 60–99% globally. In Western countries, adults with advanced AIDS prior to the introduction of highly active antiretroviral therapy (HAART) this virus also a cause of blindness (CMV retinitis) and death in patients.
Congenital cytomegalovirus infection is also a cause of non-hereditary congenital sensorineural hearing loss.[3]
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Abnormal Development Cytomegalovirus | Congenital Cytomegalovirus |
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
|
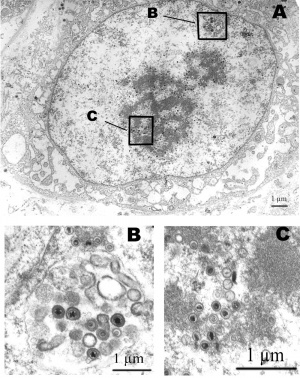
Cytomegalovirus Structure
- double-stranded linear DNA virus
- 235 Kb in size
Cytomegalovirus infected spermatozoa nucleus[1]
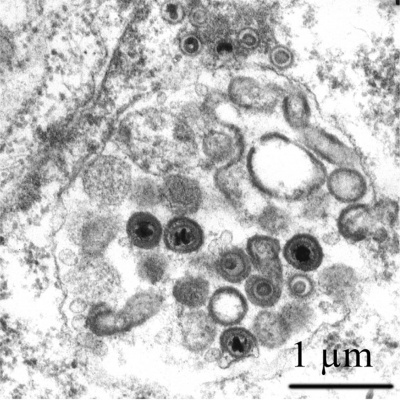
|
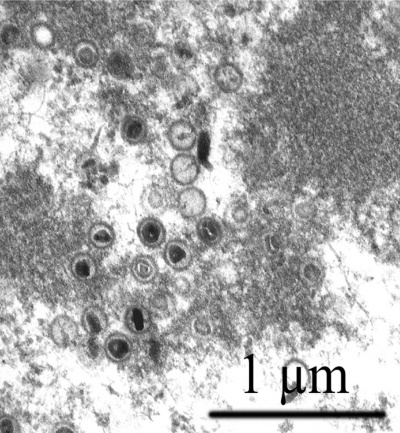
|
| Full and empty viral capsids | HCMV virions |
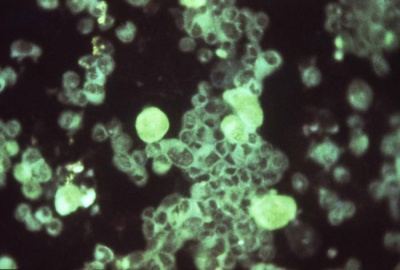
Cytomegalovirus Detection
Image shows human embryonic lung infected by cytomegalovirus demonstrated by an immunofluorescent technique. Viral infection causes systemic infection and extensive brain damage and cell death by necrosis.
A combination of tests has been used for prenatal diagnosis and there are some less reliable sonographic features to the infection.
- maternal serum - specific immunoglobulin (IgM) antibodies
- amniotic fluid - viral culture and PCR amplification of CMV DNA.
Cytomegalovirus History
- 1921 - first to suggest that the "cytomegalia" could be due to a viral agent.
- 1950 - demonstrated that infection may occur in utero.
- 1956-57 - several groups independently isolate human CMV strains.
- 1960 - the term "cytomegalovirus" introduced.
Cytomegalovirus Musculoskeletal
| A mouse model of effects of cytomegalovirus infection on development has shown induction of micrognathia and other musculoskeletal abnormalities by impacting on signalling pathways, involving FN, NF-kappaB2, RelA, RelB, and Shh and Smad7 proteins. | 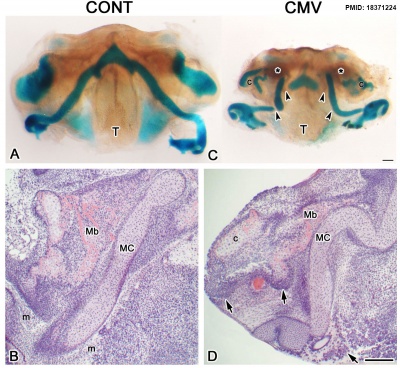
Cytomegalovirus induced micrognathia and abnormal skeletogenesis in mouse model.[20] |
Cytomegalovirus Placentitis
Clinical term for the cytomegalovirus infection of the placenta.
A earlier histological study[21] identified fixed connective tissue cells predominantly infected cell type in placental tissue. In addition, endothelial cells, macrophages and in some cases trophoblast infection. While a more recent in vitro study[22] suggests that all villi cell types are likely to be infected.
References
- ↑ 1.0 1.1 Naumenko VA, Tyulenev YA, Yakovenko SA, Kurilo LF, Shileyko LV, Segal AS, Zavalishina LE, Klimova RR, Tsibizov AS, Alkhovskii SV & Kushch AA. (2011). Detection of human cytomegalovirus in motile spermatozoa and spermatogenic cells in testis organotypic culture. Herpesviridae , 2, 7. PMID: 21711549 DOI.
- ↑ Department of Health (2018) Clinical Practice Guidelines: Pregnancy Care. Canberra: Australian Government Department of Health. (5 June 2019)
- ↑ Teissier N, Delezoide AL, Mas AE, Khung-Savatovsky S, Bessières B, Nardelli J, Vauloup-Fellous C, Picone O, Houhou N, Oury JF, Van Den Abbeele T, Gressens P & Adle-Biassette H. (2011). Inner ear lesions in congenital cytomegalovirus infection of human fetuses. Acta Neuropathol. , 122, 763-74. PMID: 22033878 DOI.
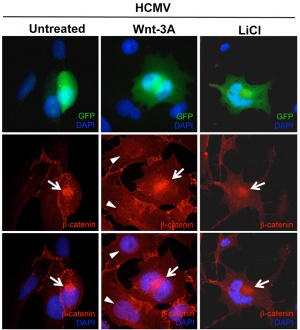
- ↑ 4.0 4.1 Angelova M, Zwezdaryk K, Ferris M, Shan B, Morris CA & Sullivan DE. (2012). Human cytomegalovirus infection dysregulates the canonical Wnt/β-catenin signaling pathway. PLoS Pathog. , 8, e1002959. PMID: 23071438 DOI.
- ↑ Minsart AF, Rypens F, Smiljkovic M, Kakkar F, Renaud C, Lamarre V, Boucher M & Boucoiran I. (2020). Prenatal findings, neonatal symptoms and neurodevelopmental outcome of congenital cytomegalovirus infection in a university hospital in Montreal, Quebec. J Perinat Med , , . PMID: 32031981 DOI.
- ↑ Tabata T, Petitt M, Fang-Hoover J & Pereira L. (2019). Survey of cellular immune responses to human cytomegalovirus infection in the microenvironment of the uterine-placental interface. Med. Microbiol. Immunol. , 208, 475-485. PMID: 31065796 DOI.
- ↑ Faure-Bardon V, Magny JF, Parodi M, Couderc S, Garcia P, Maillotte AM, Benard M, Pinquier D, Astruc D, Patural H, Pladys P, Parat S, Guillois B, Garenne A, Bussières L, Guilleminot T, Stirnemann J, Ghout I, Ville Y & Leruez-Ville M. (2018). Sequelae of congenital cytomegalovirus (cCMV) following maternal primary infection are limited to those acquired in the first trimester of pregnancy. Clin. Infect. Dis. , , . PMID: 30596974 DOI.
- ↑ Giannattasio A, Bruzzese D, Di Costanzo P, Capone E, Romano A, D'Amico A, Bravaccio C, Grande C, Capasso L & Raimondi F. (2018). Neuroimaging Profiles and Neurodevelopmental Outcome in Infants With Congenital Cytomegalovirus Infection. Pediatr. Infect. Dis. J. , 37, 1028-1033. PMID: 30222696 DOI.
- ↑ Britt WJ. (2018). Maternal Immunity and the Natural History of Congenital Human Cytomegalovirus Infection. Viruses , 10, . PMID: 30081449 DOI.
- ↑ Pass RF & Arav-Boger R. (2018). Maternal and fetal cytomegalovirus infection: diagnosis, management, and prevention. F1000Res , 7, 255. PMID: 29560263 DOI.
- ↑ Kawasaki H, Kosugi I, Meguro S & Iwashita T. (2017). Pathogenesis of developmental anomalies of the central nervous system induced by congenital cytomegalovirus infection. Pathol. Int. , 67, 72-82. PMID: 28074532 DOI.
- ↑ Gunkel J, van der Knoop BJ, Nijman J, de Vries LS, Manten GTR, Nikkels PGJ, Murk JL, de Vries JIP & Wolfs TFW. (2017). Congenital Cytomegalovirus Infection in the Absence of Maternal Cytomegalovirus-IgM Antibodies. Fetal. Diagn. Ther. , 42, 144-149. PMID: 28259882 DOI.
- ↑ Almishaal AA, Mathur PD, Hillas E, Chen L, Zhang A, Yang J, Wang Y, Yokoyama WM, Firpo MA & Park AH. (2017). Natural killer cells attenuate cytomegalovirus-induced hearing loss in mice. PLoS Pathog. , 13, e1006599. PMID: 28859161 DOI.
- ↑ Enders M, Daiminger A, Exler S, Ertan K, Enders G & Bald R. (2017). Prenatal diagnosis of congenital cytomegalovirus infection in 115 cases: a 5 years' single center experience. Prenat. Diagn. , 37, 389-398. PMID: 28207161 DOI.
- ↑ Bilavsky E, Pardo J, Attias J, Levy I, Magny JF, Ville Y, Leruez-Ville M & Amir J. (2016). Clinical Implications for Children Born With Congenital Cytomegalovirus Infection Following a Negative Amniocentesis. Clin. Infect. Dis. , 63, 33-8. PMID: 27114380 DOI.
- ↑ Oosterom N, Nijman J, Gunkel J, Wolfs TF, Groenendaal F, Verboon-Maciolek MA & de Vries LS. (2015). Neuro-imaging findings in infants with congenital cytomegalovirus infection: relation to trimester of infection. Neonatology , 107, 289-96. PMID: 25790782 DOI.
- ↑ Gabrielli L, Bonasoni MP, Santini D, Piccirilli G, Chiereghin A, Guerra B, Landini MP, Capretti MG, Lanari M & Lazzarotto T. (2013). Human fetal inner ear involvement in congenital cytomegalovirus infection. Acta Neuropathol Commun , 1, 63. PMID: 24252374 DOI.
- ↑ Polilli E, Parruti G, D'Arcangelo F, Tracanna E, Clerico L, Savini V, D'Antonio F, Rosati M, Manzoli L, D'Antonio D & Nigro G. (2012). Preliminary evaluation of the safety and efficacy of standard intravenous immunoglobulins in pregnant women with primary cytomegalovirus infection. Clin. Vaccine Immunol. , 19, 1991-3. PMID: 23100477 DOI.
- ↑ Lazzarotto T, Guerra B, Gabrielli L, Lanari M & Landini MP. (2011). Update on the prevention, diagnosis and management of cytomegalovirus infection during pregnancy. Clin. Microbiol. Infect. , 17, 1285-93. PMID: 21631642 DOI.
- ↑ Jaskoll T, Abichaker G, Sedghizadeh PP, Bringas P & Melnick M. (2008). Cytomegalovirus induces abnormal chondrogenesis and osteogenesis during embryonic mandibular development. BMC Dev. Biol. , 8, 33. PMID: 18371224 DOI.
- ↑ Sinzger C, Müntefering H, Löning T, Stöss H, Plachter B & Jahn G. (1993). Cell types infected in human cytomegalovirus placentitis identified by immunohistochemical double staining. Virchows Arch A Pathol Anat Histopathol , 423, 249-56. PMID: 8236822
- ↑ Tao L, Suhua C, Juanjuan C, Zongzhi Y, Juan X & Dandan Z. (2011). In vitro study on human cytomegalovirus affecting early pregnancy villous EVT's invasion function. Virol. J. , 8, 114. PMID: 21392403 DOI.
Textbooks
Baron S, editor. Medical Microbiology. 4th edition. Galveston (TX): University of Texas Medical Branch at Galveston; 1996. Available from: https://www.ncbi.nlm.nih.gov/books/NBK7627/
- Cytomegalovirus | Search "Cytomegalovirus"
Alberts B, Johnson A, Lewis J, et al. Molecular Biology of the Cell. 4th edition. New York: Garland Science; 2002. Available from: https://www.ncbi.nlm.nih.gov/books/NBK21054/
Disease Control Priorities in Developing Countries. 2nd edition. Jamison DT, Breman JG, Measham AR, et al., editors. Washington (DC): World Bank; 2006.
Reviews
Wood AM & Hughes BL. (2018). Detection and Prevention of Perinatal Infection: Cytomegalovirus and Zika Virus. Clin Perinatol , 45, 307-323. PMID: 29747890 DOI.
Leruez-Ville M & Ville Y. (2017). Fetal cytomegalovirus infection. Best Pract Res Clin Obstet Gynaecol , 38, 97-107. PMID: 27923540 DOI.
Carlson A, Norwitz ER & Stiller RJ. (2010). Cytomegalovirus infection in pregnancy: should all women be screened?. Rev Obstet Gynecol , 3, 172-9. PMID: 21364849
Yinon Y, Farine D & Yudin MH. (2010). Screening, diagnosis, and management of cytomegalovirus infection in pregnancy. Obstet Gynecol Surv , 65, 736-43. PMID: 21375790 DOI.
Mosca F & Pugni L. (2007). Cytomegalovirus infection: the state of the art. J Chemother , 19 Suppl 2, 46-8. PMID: 18073181
Hassan J & Connell J. (2007). Translational mini-review series on infectious disease: congenital cytomegalovirus infection: 50 years on. Clin. Exp. Immunol. , 149, 205-10. PMID: 17635529 DOI.
Degani S. (2006). Sonographic findings in fetal viral infections: a systematic review. Obstet Gynecol Surv , 61, 329-36. PMID: 16635273 DOI.
Revello MG & Gerna G. (2002). Diagnosis and management of human cytomegalovirus infection in the mother, fetus, and newborn infant. Clin. Microbiol. Rev. , 15, 680-715. PMID: 12364375
Articles
Nyholm JL & Schleiss MR. (2010). Prevention of maternal cytomegalovirus infection: current status and future prospects. Int J Womens Health , 2, 23-35. PMID: 21072294
Boppana SB, Ross SA, Novak Z, Shimamura M, Tolan RW, Palmer AL, Ahmed A, Michaels MG, Sánchez PJ, Bernstein DI, Britt WJ & Fowler KB. (2010). Dried blood spot real-time polymerase chain reaction assays to screen newborns for congenital cytomegalovirus infection. JAMA , 303, 1375-82. PMID: 20388893 DOI.
Riley HD. (1997). History of the cytomegalovirus. South. Med. J. , 90, 184-90. PMID: 9042169
Search Pubmed
Search Pubmed: Cytomegalovirus Virus | Congenital Cytomegalovirus Syndrome | Congenital Cytomegalovirus Infection | cytomegalovirus placentitis
| Environmental Links: Introduction | low folic acid | iodine deficiency | Nutrition | Drugs | Australian Drug Categories | USA Drug Categories | thalidomide | herbal drugs | Illegal Drugs | smoking | Fetal Alcohol Syndrome | TORCH | viral infection | bacterial infection | fungal infection | zoonotic infection | toxoplasmosis | Malaria | maternal diabetes | maternal hypertension | maternal hyperthermia | Maternal Inflammation | Maternal Obesity | hypoxia | biological toxins | chemicals | heavy metals | air pollution | radiation | Prenatal Diagnosis | Neonatal Diagnosis | International Classification of Diseases | Fetal Origins Hypothesis |
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- Centers for Disease Control and Prevention Cytomegalovirus (CMV) and Congenital CMV Infection | testing-diagnosis | The Congenital Disease Mothers Don't Know About
- PubMed Health Congenital cytomegalovirus
- MedlinePlus Congenital cytomegalovirus
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, June 20) Embryology Abnormal Development - Cytomegalovirus. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Abnormal_Development_-_Cytomegalovirus
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G