BGDA Practical 12 - Embryo to Fetus: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| (25 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
{{ | {{BGDALab12}} | ||
==Introduction== | ==Introduction== | ||
| Line 66: | Line 66: | ||
{{Stage 23 MRI movie}} | {{Stage 23 MRI movie}} | ||
===Cortex=== | ===Cortex=== | ||
| Line 84: | Line 75: | ||
| Human embryo, [[Week 8]], ({{GA}} week 10) [[Carnegie stage 22]] section from the neural tube at the level of the developing cortex. Inset (upper right) shows whole section overview and approximate level of section (red line). Grey box shows detailed image region of developing cerebrum layer thicknesses are shown in microns. | | Human embryo, [[Week 8]], ({{GA}} week 10) [[Carnegie stage 22]] section from the neural tube at the level of the developing cortex. Inset (upper right) shows whole section overview and approximate level of section (red line). Grey box shows detailed image region of developing cerebrum layer thicknesses are shown in microns. | ||
[[Neural_-_Cerebrum_Development|'''Developing Cortex''']] will form from the thin outer layer called the cortical plate. The underlying layers transient structures that continue to supply cells to the cortex through fetal period, most of these layers will eventually be lost, except for a thin ventricular layer. Cells migrate out along [[Neural_System_-_Glial_Development#Radial_Glia|'''radial glia''']] that establish the initial columnar and layered structure of the cortex. Layers are named according to the nervous system revised terminology (1970) | [[Neural_-_Cerebrum_Development|'''Developing Cortex''']] will form from the thin outer layer called the cortical plate. The underlying layers transient structures that continue to supply cells to the cortex through fetal period, most of these layers will eventually be lost, except for a thin ventricular layer. Cells migrate out along [[Neural_System_-_Glial_Development#Radial_Glia|'''radial glia''']] that establish the initial columnar and layered structure of the cortex. Layers are named according to the nervous system revised terminology (1970){{#pmid:5414696|PMID5414696}} | ||
[[Neural - Vascular Development|'''Developing Vascular''']] blood vessels can also be seen spanning the developing layers. In the adult, these vessels will be lined with non-fenestrated endothelial cells that together with other vascular cells (pericytes and vascular smooth muscle cells), glial cells (astrocytes and microglia) and neurons will form the "[[Neural_-_Vascular_Development#Blood-Brain_Barrier|'''blood-brain barrier''']]". | [[Neural - Vascular Development|'''Developing Vascular''']] blood vessels can also be seen spanning the developing layers. In the adult, these vessels will be lined with non-fenestrated endothelial cells that together with other vascular cells (pericytes and vascular smooth muscle cells), glial cells (astrocytes and microglia) and neurons will form the "[[Neural_-_Vascular_Development#Blood-Brain_Barrier|'''blood-brain barrier''']]". | ||
| Line 119: | Line 111: | ||
* [https://embryology.med.unsw.edu.au/embryology/Slides/Embryo_Stages/Stage22/33-rotate-spinal-cord/Human_Stage22_spinal_cord.html?zoom=5&lat=-4423&lon=951.35969&layers=B vertebral arch root] (cartilage stage) | * [https://embryology.med.unsw.edu.au/embryology/Slides/Embryo_Stages/Stage22/33-rotate-spinal-cord/Human_Stage22_spinal_cord.html?zoom=5&lat=-4423&lon=951.35969&layers=B vertebral arch root] (cartilage stage) | ||
* [https://embryology.med.unsw.edu.au/embryology/Slides/Embryo_Stages/Stage22/33-rotate-spinal-cord/Human_Stage22_spinal_cord.html?zoom=6&lat=-881.5&lon=3870.5&layers=B dorsal uniting ligament] (lying dorsal to the spinal cord and under the periderm) | * [https://embryology.med.unsw.edu.au/embryology/Slides/Embryo_Stages/Stage22/33-rotate-spinal-cord/Human_Stage22_spinal_cord.html?zoom=6&lat=-881.5&lon=3870.5&layers=B dorsal uniting ligament] (lying dorsal to the spinal cord and under the periderm) | ||
|} | |||
===Oral Cavity=== | |||
<gallery caption="Oral Cavity ([[Carnegie stage 23|stage 23]])"> | |||
File:Stage23 embryo oral cavity 01.jpg|Floor | |||
File:Stage23 embryo oral cavity 02.jpg|Floor (labeled) | |||
File:Stage23 embryo oral cavity 03.jpg|Roof | |||
File:Stage23 embryo oral cavity 04.jpg|Roof (labeled) | |||
File:Stage23 embryo oral cavity 06.jpg|Sagittal view | |||
</gallery> | |||
===Renal and Genital=== | |||
{| | |||
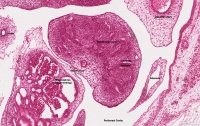
| width=505px|[[File:Stage 22 image 302.jpg|500px]] | |||
| Note the development, relative position and size of organs within the lower peritoneal cavity. The intra-abdominal portion of the placental cord can be seen on the right. | |||
* '''Mesonephros''' - {{renal}} middle transient stage of kidney has commenced degeneration. | |||
* '''Male gonad''' - {{testis}} sex cords developing as a precursor to seminiferous tubule differentiation. | |||
** developing mesonephric duct (Wolffian duct) will form the ductus deferens. | |||
** degenerating paramesonephric duct (Mullerian duct) due to {{AMH}} secretion. In female this would develop to form the uterus. | |||
[[File:Stage 22 image 301.jpg|200px]] | |||
|} | |} | ||
==Week 10 - Fetus (40mm)== | ==Week 10 - Fetus (40mm)== | ||
| Line 146: | Line 163: | ||
</gallery> | </gallery> | ||
{{10wkFetus}} | |||
===Adrenal=== | |||
* adrenal cortex (intermediate mesoderm) | |||
* adrenal medulla (neural crest) | |||
{| | |||
| <html5media height="500" width="560">File:Adrenal medulla.mp4</html5media> | |||
| Cartoon shows example of some neural crest medial migration during week 4 and 5 and the structures formed at the level of the body. | |||
* Cells staying dorsal to neural tube - dorsal root ganglia (DRG) | |||
* Cells migrating ventral to neural tube - sympathetic ganglia | |||
* Cells migrating peritoneal cavity wall - adrenal medulla | |||
* Cells migrate into GIT wall - enteric nervous system | |||
<br> | |||
{{Adrenal movie}} | |||
|} | |||
{| class="prettytable" | |||
| [[File:Human-adrenal gland 01.jpg|300px]] | |||
| [[File:Week10 adrenal.jpg|300px]] | |||
|- | |||
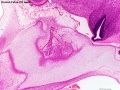
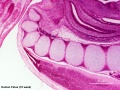
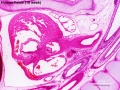
| '''Human Embryo''' (8 weeks, [[Carnegie stage 22|stage 22]]) adrenal gland showing the fetal and permanent adrenal cortex. Note that the medulla of the adrenal gland is not yet encapsulated by the cortex. 8-9 weeks post conception (wpc) adrenal cortex synthesizes cortisol under the regulation of ACTH (also stimulates androstenedione and testosterone secretion). | |||
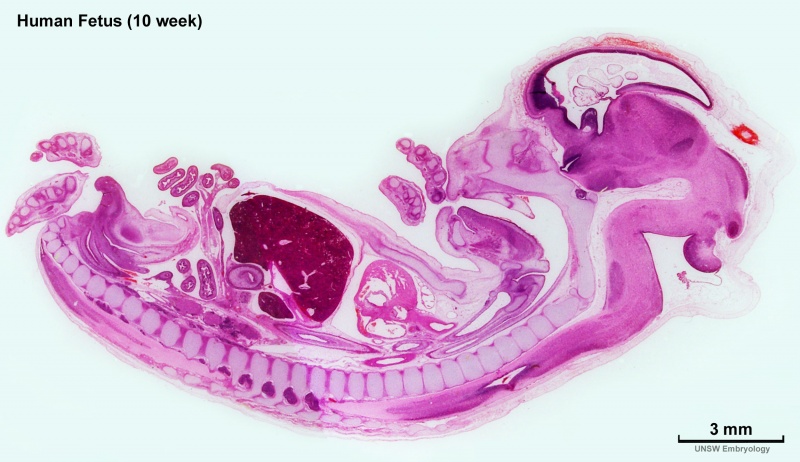
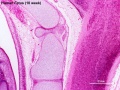
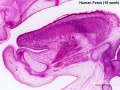
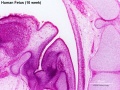
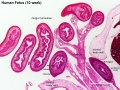
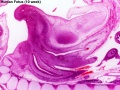
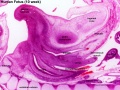
| '''Human Fetus '''(10 week, 40mm, parasagittal section) shows location of the developing adrenal gland. The spongy appearance at the centre of the adrenal is the degenerating fetal cortex. The dense region around the outside of the adrenal is the developing adult cortex.) | |||
|} | |||
<br> | |||
{{BGDA Practical 12 - Embryo to Fetus Interactive}} | |||
<br> | |||
{{BGDALab12}} | |||
==Additional Information== | |||
{{Med Prac additional Information}} | |||
<br><br> | |||
'''Links:''' [[Fetal Development - 10 Weeks]] [[Fetal Development - 12 Weeks]] | |||
===Human Fetal Adrenal Cortex=== | |||
{{ | {{#pmid:21051591}} | ||
:"Continuous efforts have been devoted to unraveling the biophysiology and development of the human fetal adrenal cortex, which is structurally and functionally unique from other species. It plays a pivotal role, mainly through steroidogenesis, in the regulation of intrauterine homeostasis and in fetal development and maturation. The steroidogenic activity is characterized by early transient cortisol biosynthesis, followed by its suppressed synthesis until late gestation, and extensive production of dehydroepiandrosterone (DHEA) and its sulfate (DHEA-S), precursors of placental estrogen, during most of gestation. The gland rapidly grows through processes including cell proliferation and angiogenesis at the gland periphery, cellular migration, hypertrophy, and apoptosis." | |||
===Trunk Muscle Development=== | |||
This recent study shows an example of trunk muscle development at the end of the embryonic period. | |||
{| | |||
| width=505px|[[File:Carnegie stage 22 - pectoralis major muscle.jpg|500px]] | |||
| '''Pectoralis Major Muscle Development'''{{#pmid:29726018|PMID29726018}} | |||
(A) Frontal view of the reconstructed pectoralis major portions of a stage {{CS23}} human embryo (56–60 days of development), specimen number {{CE950}}. All other muscles are hidden. Depicted are three heads of the pectoralis major: clavicular head (light blue), sternocostal head (red) and abdominal head (yellow) and bones (white). | |||
(B) Transverse section of the left shoulder region. The pectoralis major muscle is divided into three heads at this stage and is therefore even more partitioned than in adults (Gilroy et al. 2009). The tree heads of the left pectoralis muscle and the second rib and humerus of the same specimen as in (A) are tagged. | |||
Legend: AH, abdominal head; CH, clavicular head; PM, pectoralis major muscle; SCH, sternocostal head. Scale bar: ~5 mm. | |||
|} | |||
===Anti-Müllerian Hormone=== | |||
{{ | Anti-Müllerian Hormone ({{AMH}}) has several adult diagnostic uses. For example, a recent study has shown that salivary and serum androgens with anti-Müllerian hormone measurement can be used for the diagnosis of {{polycystic ovary syndrome}}.{{#pmid:29491484|PMID29491484}} | ||
{| | |||
|+ '''Anti-Müllerian Hormone Levels''' | |||
|-bgcolor="CEDFF2" | |||
! width=250px|Lower AMH | |||
! width=250px|Higher AMH | |||
|- | |||
| recurrent miscarriage{{#pmid:30917731|PMID30917731}} - Serum AMH levels may reflect quality, and quantity of the remaining {{oocyte}}s in these patients, and RM patients may have a low ovarian reserve, and a potentially poor oocyte quality. | |||
|valign=top| | |||
{{polycystic ovarian syndrome}}{{#pmid:29491484|PMID29491484}} - salivary and serum can be used for the diagnosis | |||
|-bgcolor="F5FAFF" | |||
| {{endometriosis}} | |||
| | |||
|} | |||
'''Predictive Utility in Assisted Reproductive Technologies Outcomes''' | |||
"Anti-Müllerian hormone (AMH) has become one of the most informative biochemical markers of the ovary and is considered the earliest and most sensitive marker of reproductive aging. The accuracy of AMH in predicting ovarian response to controlled ovarian stimulation has led to AMH-based prognostication counseling and individualization of assisted reproductive technology (ART) stimulation protocols to optimize ovarian response and minimize hyperstimulation risks. Although AMH is considered a good predictor of quantitative ART outcomes, its correlation with qualitative ART outcomes is still controversial. The aim of this review is to provide an updated overview of the clinical utility of AMH in predicting ART outcomes.{{#pmid:30994481|PMID30994481}} | |||
== | ===References=== | ||
<references/> | |||
{{ | {{BGDAFooter}} | ||
Latest revision as of 12:27, 27 May 2019
| Practical 12: Embryo to Fetus | Second Trimester | Third Trimester | Birth | Neonatal | Abnormalities |
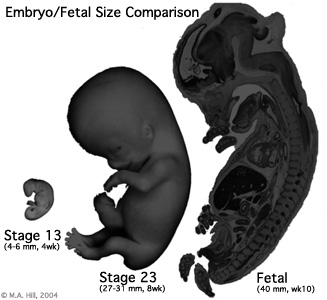
Introduction
Identify the development and form of the week 8 embryo (Stage 22 and 23). This 3D reconstruction animations showing specific systems and the histological sections from which these were prepared. There are also virtual slides and selected cross-sections showing specific features.
Then look at the week 10 early fetus and observe developmental changes. The selected mid-sagittal section shows the overall fetal anatomy and the gallery of excerpts have further detailed descriptions of these regions.
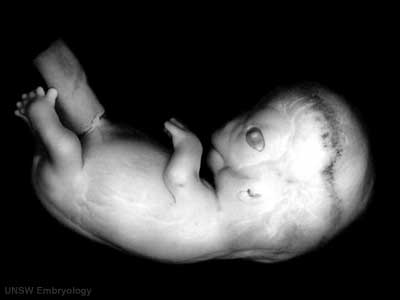
Week 8 - Stage 22
| stage 22, Week 8, 54 - 56 days, 23 - 28 mm
Mesoderm: heart prominence, ossification continues Head: nose, eye, external acoustic meatus Body:straightening of trunk, heart, liver, umbilicus: placental cord, midgut herniation, allantois, vitelline duct Limb: upper limbs longer and bent at elbow, foot plate with webbed digits, wrist, hand plate with separated digits Straightening of trunk, pigmented eye, eyelid, nose, external acoustic meatus, ear auricle, scalp vascular plexus, separated digits (fingers), thigh, ankle, umbilical cord |
Embryo Anatomy
Now examine selected regions of the Stage 22 embryo and their overall development in the 3D animations.
|
|
|
|
|
|
Virtual Slides
|
|
|
| ||||||||||||
|
|
| |||||||||||||
|
|
|
Week 8 - Stage 23
| Week 8, 56 - 60 days, 27 - 31 mm
scalp vascular plexus, eylid, eye, nose, auricle of external ear, mouth, sholder, arm, elbow, wrist, toes separated, sole of foot, umbilical cord Mesoderm: ossification continues Head: eyelids, external ears, rounded head Body: straightening of trunk, intestines herniated at umbilicus Limbs: hands and feet turned inward |
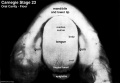
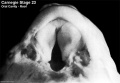
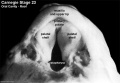
| Carnegie Stage 23 MRI movies | |||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
|
|
|
|
|
| |||||||||||||||||||||
| |||||||||||||||||||||||||||
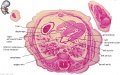
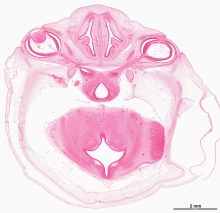
Cortex
| Week 8 Developing Cortex |
|---|
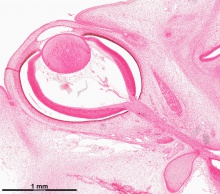
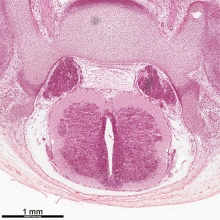
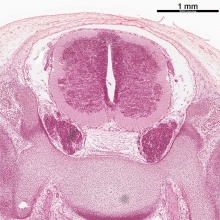
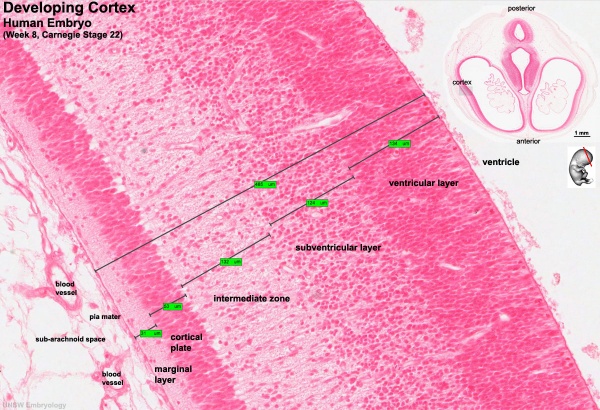
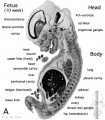
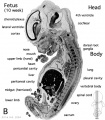
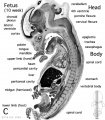
| Human embryo, Week 8, (GA week 10) Carnegie stage 22 section from the neural tube at the level of the developing cortex. Inset (upper right) shows whole section overview and approximate level of section (red line). Grey box shows detailed image region of developing cerebrum layer thicknesses are shown in microns.
Developing Cortex will form from the thin outer layer called the cortical plate. The underlying layers transient structures that continue to supply cells to the cortex through fetal period, most of these layers will eventually be lost, except for a thin ventricular layer. Cells migrate out along radial glia that establish the initial columnar and layered structure of the cortex. Layers are named according to the nervous system revised terminology (1970)[1]
Developing Ventricular Space is cerebrospinal fluid (CSF) filled and the lateral ventricles form within the cortical region. The inset image shows lying within the lateral ventricles, the choroid plexus the modified vascular structure that forms and secretes the CSF. Developing Meninges layers lie outside the neural tube. The thin pia mater that closely covers the entire brain. The mesh-like arachnoid mater and the sub-arachnoid space that will also be CSF filled. The dense dura mater lies outside these 2 layers and under the skull, it cannot be seen in the enlarged image. |
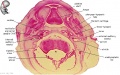
Spinal Cord
| Week 8 Developing Spinal Cord (virtual slide) | |||||
|---|---|---|---|---|---|
|
These listed features link to zoomed views of the virtual slide with the named feature generally in the centre of the view.
Use the (-) at the top left of the screen to see where this feature is located. | ||||
| Spinal Cord Features | Other Features
| ||||
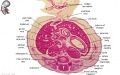
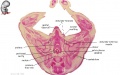
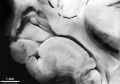
Oral Cavity
- Oral Cavity (stage 23)
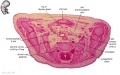
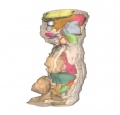
Renal and Genital
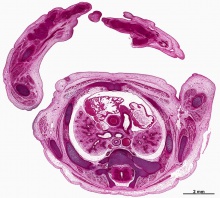
|
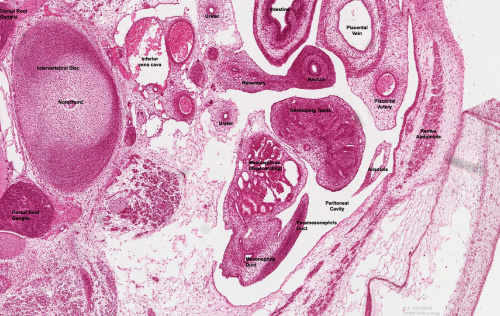
Note the development, relative position and size of organs within the lower peritoneal cavity. The intra-abdominal portion of the placental cord can be seen on the right.
|
Week 10 - Fetus (40mm)
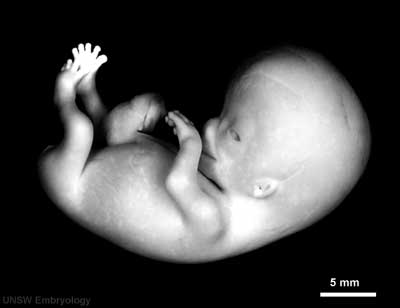
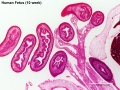
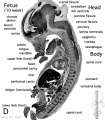
- Human Female Fetus (week 10)
There are 4 sections taken in the sagittal plane (moving from the right at Plane A towards the midline at Plane D). Click on the small images (or the text below) to open the linked large image pages.
Related Images
Fetus (week 10) Planes A (most lateral), B (lateral), C (medial) and D (midline) from lateral towards the midline.
- Human Fetus - most lateral | lateral | medial | midline
- Head - most lateral | lateral | medial | midline
- Cerebellum - most lateral | lateral | medial | midline
- Urogenital Unlabelled - most lateral | lateral | medial | midline
- Urogenital Labelled - most lateral | lateral | medial | midline
- Large Images - midline
- Image Source: UNSW Embryology, no reproduction without permission.
Adrenal
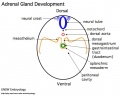
- adrenal cortex (intermediate mesoderm)
- adrenal medulla (neural crest)
| <html5media height="500" width="560">File:Adrenal medulla.mp4</html5media> | Cartoon shows example of some neural crest medial migration during week 4 and 5 and the structures formed at the level of the body.
|
|
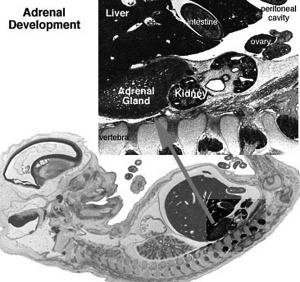
|
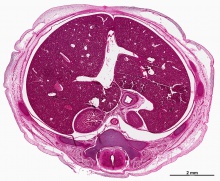
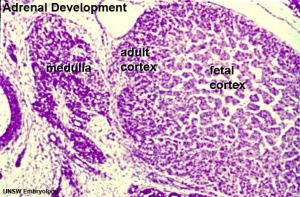
| Human Embryo (8 weeks, stage 22) adrenal gland showing the fetal and permanent adrenal cortex. Note that the medulla of the adrenal gland is not yet encapsulated by the cortex. 8-9 weeks post conception (wpc) adrenal cortex synthesizes cortisol under the regulation of ACTH (also stimulates androstenedione and testosterone secretion). | Human Fetus (10 week, 40mm, parasagittal section) shows location of the developing adrenal gland. The spongy appearance at the centre of the adrenal is the degenerating fetal cortex. The dense region around the outside of the adrenal is the developing adult cortex.) |
Embryo to Fetus Interactive Component
| Attempt the Quiz - Embryo to Fetus | ||
|---|---|---|
Here are a few simple Quiz questions that relate to Embryo to Fetus transition from the lecture and practical.
|
| Practical 12: Embryo to Fetus | Second Trimester | Third Trimester | Birth | Neonatal | Abnormalities |
Additional Information
| Additional Information - Content shown under this heading is not part of the material covered in this class. It is provided for those students who would like to know about some concepts or current research in topics related to the current class page. |
Links: Fetal Development - 10 Weeks Fetal Development - 12 Weeks
Human Fetal Adrenal Cortex
Ishimoto H & Jaffe RB. (2011). Development and function of the human fetal adrenal cortex: a key component in the feto-placental unit. Endocr. Rev. , 32, 317-55. PMID: 21051591 DOI.
- "Continuous efforts have been devoted to unraveling the biophysiology and development of the human fetal adrenal cortex, which is structurally and functionally unique from other species. It plays a pivotal role, mainly through steroidogenesis, in the regulation of intrauterine homeostasis and in fetal development and maturation. The steroidogenic activity is characterized by early transient cortisol biosynthesis, followed by its suppressed synthesis until late gestation, and extensive production of dehydroepiandrosterone (DHEA) and its sulfate (DHEA-S), precursors of placental estrogen, during most of gestation. The gland rapidly grows through processes including cell proliferation and angiogenesis at the gland periphery, cellular migration, hypertrophy, and apoptosis."
Trunk Muscle Development
This recent study shows an example of trunk muscle development at the end of the embryonic period.
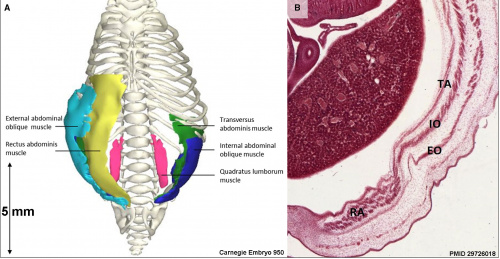
|
Pectoralis Major Muscle Development[2]
(A) Frontal view of the reconstructed pectoralis major portions of a stage 23 human embryo (56–60 days of development), specimen number 950. All other muscles are hidden. Depicted are three heads of the pectoralis major: clavicular head (light blue), sternocostal head (red) and abdominal head (yellow) and bones (white).
|
Anti-Müllerian Hormone
Anti-Müllerian Hormone (AMH) has several adult diagnostic uses. For example, a recent study has shown that salivary and serum androgens with anti-Müllerian hormone measurement can be used for the diagnosis of polycystic ovary syndrome.[3]
| Lower AMH | Higher AMH |
|---|---|
| recurrent miscarriage[4] - Serum AMH levels may reflect quality, and quantity of the remaining oocytes in these patients, and RM patients may have a low ovarian reserve, and a potentially poor oocyte quality. |
polycystic ovarian syndrome[3] - salivary and serum can be used for the diagnosis |
| endometriosis |
Predictive Utility in Assisted Reproductive Technologies Outcomes
"Anti-Müllerian hormone (AMH) has become one of the most informative biochemical markers of the ovary and is considered the earliest and most sensitive marker of reproductive aging. The accuracy of AMH in predicting ovarian response to controlled ovarian stimulation has led to AMH-based prognostication counseling and individualization of assisted reproductive technology (ART) stimulation protocols to optimize ovarian response and minimize hyperstimulation risks. Although AMH is considered a good predictor of quantitative ART outcomes, its correlation with qualitative ART outcomes is still controversial. The aim of this review is to provide an updated overview of the clinical utility of AMH in predicting ART outcomes.[5]
References
- ↑ . (1970). Embryonic vertebrate central nervous system: revised terminology. The Boulder Committee. Anat. Rec. , 166, 257-61. PMID: 5414696 DOI.
- ↑ Warmbrunn MV, de Bakker BS, Hagoort J, Alefs-de Bakker PB & Oostra RJ. (2018). Hitherto unknown detailed muscle anatomy in an 8-week-old embryo. J. Anat. , , . PMID: 29726018 DOI.
- ↑ 3.0 3.1 Sathyapalan T, Al-Qaissi A, Kilpatrick ES, Dargham SR, Keevil B & Atkin SL. (2018). Salivary and serum androgens with anti-Müllerian hormone measurement for the diagnosis of polycystic ovary syndrome. Sci Rep , 8, 3795. PMID: 29491484 DOI.
- ↑ McCormack CD, Leemaqz SY, Furness DL, Dekker GA & Roberts CT. (2019). Anti-Müllerian hormone levels in recurrent embryonic miscarriage patients are frequently abnormal, and may affect pregnancy outcomes. J Obstet Gynaecol , 39, 623-627. PMID: 30917731 DOI.
- ↑ Granger E & Tal R. (2019). Anti-Müllerian Hormone and Its Predictive Utility in Assisted Reproductive Technologies Outcomes. Clin Obstet Gynecol , 62, 238-256. PMID: 30994481 DOI.
BGDA: Lecture 1 | Lecture 2 | Practical 3 | Practical 6 | Practical 12 | Lecture Neural | Practical 14 | Histology Support - Female | Male | Tutorial
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 27) Embryology BGDA Practical 12 - Embryo to Fetus. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/BGDA_Practical_12_-_Embryo_to_Fetus
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G