Lecture - Respiratory Development
| Embryology - 17 May 2026 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
The lecture will introduce the development of the respiratory system and associated structures. The respiratory system does not carry out its physiological function (of gas exchange) until after birth, though the respiratory tract, diaphragm and lungs do begin to form early in embryonic development and continue through fetal development, only functionally maturing just before birth. The lungs continue to grow postnatally through childhood and some research finding suggest that there remains potential for growth in the adult.
- Current research suggests that both genetic and the developmental environment (fetal and postnatal) can influence the growth, differentiation and function of the respiratory system.
The respiratory "system" usually includes descriptions of not only the functional development of the lungs, but also related musculoskeletal (diaphragm) and vascular (pulmonary) development.
Key Concepts
- upper and lower respiratory tract.
- Embryonic origin of respiratory components (tract, lungs, diaphragm, muscles).
- Key stages in respiratory development.
- Time course of respiratory development.
- Respiration at birth.
- Postnatal development of respiration.
- Developmental abnormalities.
| Textbooks | |
|---|---|

|
Hill, M.A. (2020). UNSW Embryology (20th ed.) Retrieved Mayıs 17, 2026, from https://embryology.med.unsw.edu.au |

|
Moore, K.L., Persaud, T.V.N. & Torchia, M.G. (2015). The developing human: clinically oriented embryology (10th ed.). Philadelphia: Saunders.
|

|
Schoenwolf, G.C., Bleyl, S.B., Brauer, P.R., Francis-West, P.H. & Philippa H. (2015). Larsen's human embryology (5th ed.). New York; Edinburgh: Churchill Livingstone. |
| Additional Textbooks |
|
ECHO Lecture Recording
Mark Hill (talk) 12:12, 7 October 2018 (AEDT)
Due to lecturer illness, the lecture recording below is made available in place of the 2018 Lecture. It contains material similar to the respiratory theory information that would have been presented in the current series.
<html5media height="600" width="800">File:2014ANAT2341_Lecture_10_-_Respiratory Development.mp4</html5media>
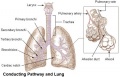
Respiratory Functional Unit
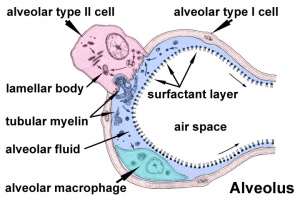
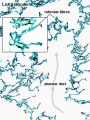
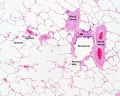
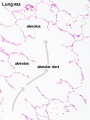
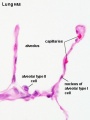
Alveolus
Alveolus (Latin alveolus = "little cavity", plural is alveoli)
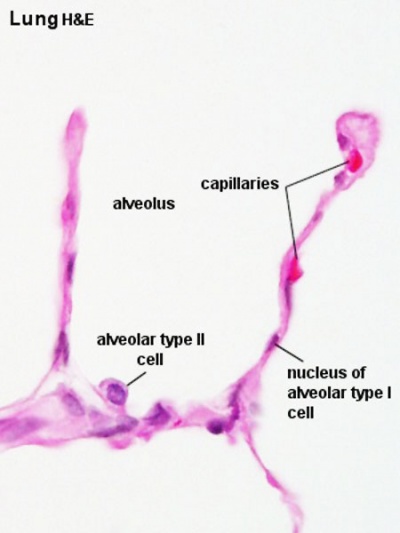
|
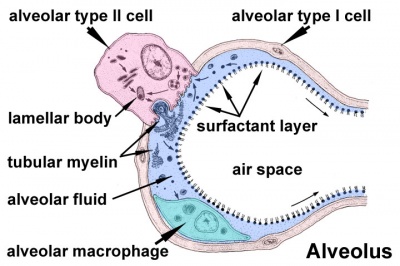
|
| Alveolus histology | Alveolus structure |
|
|
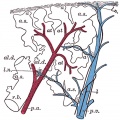
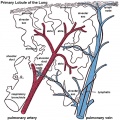
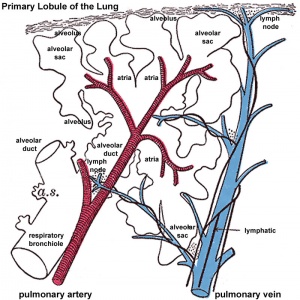
Primary Lobule
|
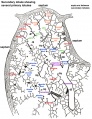
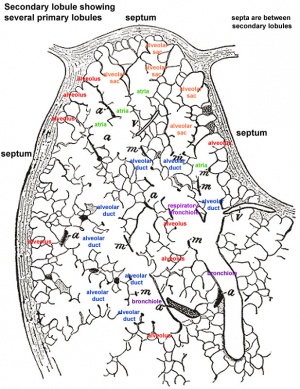
Secondary Lobule
|
Developmental Mechanisms
- Initiation - Budding of foregut endoderm to generate the trachea.
- Branching - A repeated mechanism of branching that is ongoing throughout development to form the conducting bronchioles then alveolar ducts.
- Surface area increase - Expansion of the surface area in late development generating eventually the thin air–blood barrier for gas exchange in the acini.
- Vascular development - Extension of a vascular capillary tree within the connective tissue and wall of the acini for gas exchange, and the lymphatic development for immunology of the lungs.
- Surfactant development - allows lung inflation and decreases the work of breathing and also related to immunology of the lungs.
- Musculoskeletal development - contributes the mechanical elements of ribs, intercostals and diaphragm required for breathing.
Developmental Overview
Germ Layers
- Endoderm and splanchnic mesoderm form majority of conducting and alveoli.
- Ectoderm will contribute the neural innervation.
- Mesoderm also contributes the supporting musculoskeletal components.
Week 4 - laryngotracheal groove forms on floor foregut.
Week 5 - left and right lung buds push into the pericardioperitoneal canals (primordia of pleural cavity)
Week 6 - descent of heart and lungs into thorax. Pleuroperitoneal foramen closes.
Week 7 - enlargement of liver stops descent of heart and lungs.
Month 3-6 - lungs appear glandular, end month 6 alveolar cells type 2 appear and begin to secrete surfactant.
Month 7 - respiratory bronchioles proliferate and end in alveolar ducts and sacs.
| Molecular Signaling |
|---|
| Early development is all about "branching". Fibroblast Growth Factors from the surrounding mesoderm acting through membrane receptors and Sox transcription factors are key regulators of early endodermal branching (Sox2 for initiation, Sox9 for tip maintenance and branching) |
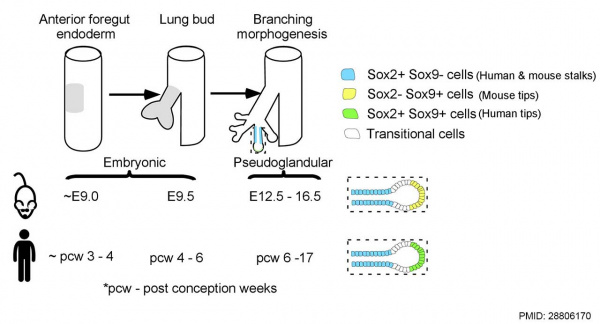
Human and mouse Sox expression[1] |
| Bmp4 acts as in an autocrine signalling mechanism to limit bud outgrowth. |
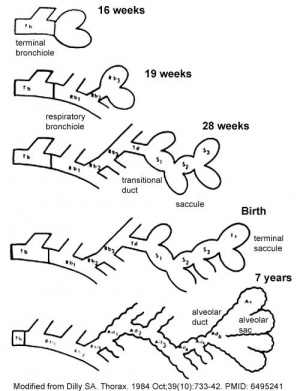
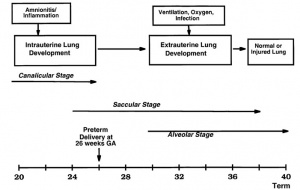
Development Stages
Note - the sequence is important rather than the actual timing, which is variable in the existing literature.
| Lung Stage | Human | Features | Vascular | |
|---|---|---|---|---|
| Embryonic | week 4 to 5 | lung buds originate as an outgrowth from the ventral wall of the foregut where lobar division occurs | extra pulmonary artery then lobular artery | |
| Pseudoglandular | week 5 to 17 | conducting epithelial tubes surrounded by thick mesenchyme are formed, extensive airway branching | Pre-acinar arteries | |
| Canalicular | week 16 to 25 | bronchioles are produced, increasing number of capillaries in close contact with cuboidal epithelium and the beginning of alveolar epithelium development | Intra-acinar arteries | |
| Saccular | week 24 to 40 | alveolar ducts and air sacs are developed | alveolar duct arteries | |
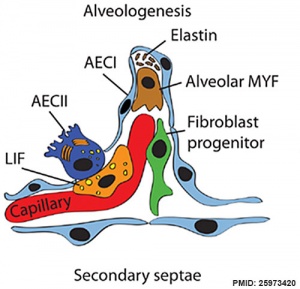
| Alveolar | late fetal to 8 years | secondary septation occurs, marked increase of the number and size of capillaries and alveoli | alveolar capillaries | |
| embryonic stage - pseudoglandular stage - canalicular stage - saccular stage - alveolar stage Links: Species Stage Comparison | respiratory | ||||
Embryonic
Week 4 to 5 - lung buds originate as an outgrowth from the ventral wall of the foregut where lobar division occurs.
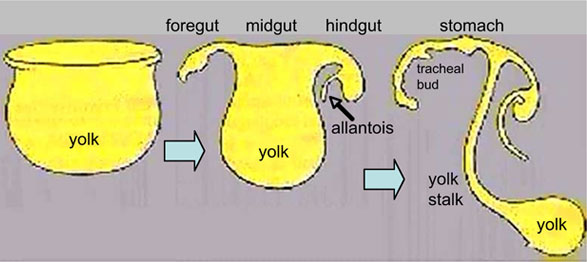
|
||
|
| |
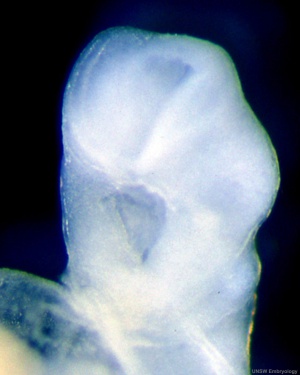
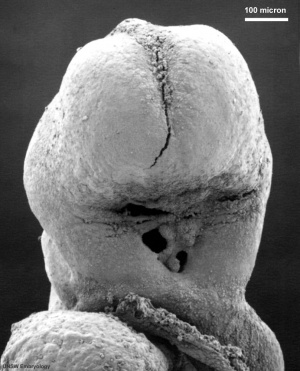
| Stomodeum (Week 4, stage 11) | Buccopharyngeal membrane (Week 4, stage 11) | |
(Week 5, stage 14)
- week 4 - 5
- Endoderm - tubular ventral growth from foregut pharynx.
- Mesoderm - mesenchyme of lung buds.
- Intraembryonic coelom - pleural cavities elongated spaces connecting pericardial and peritoneal spaces.
Stage 13 - Trachea and Lung buds
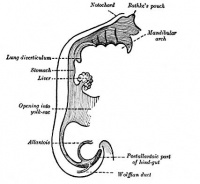
|
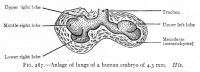
|
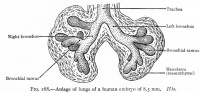
|
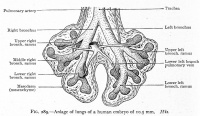
|
| Week 4 | Week 4-5 (Stage 12 to 13) | Week 5 (Stage 15 to 16) | Week 6 (Stage 16 to 17) |
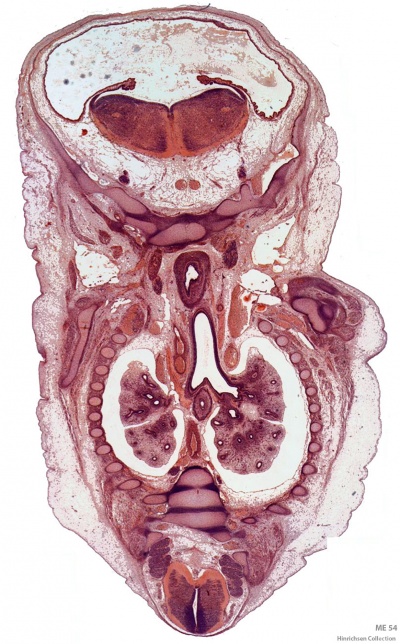
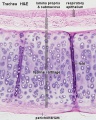
Pseudoglandular stage
Week 8 |
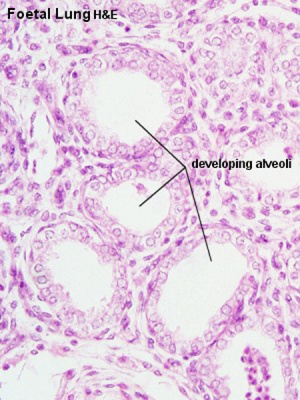
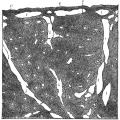
Fetal lung histology |
(This is what a gland looks like.)
Canalicular stage
|
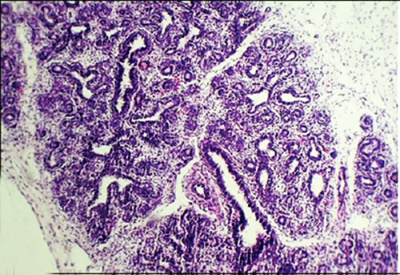
|
Saccular stage
- week 24 to near term.
- most peripheral airways form widened "airspaces", termed saccules.
- saccules widen and lengthen the airspace (by the addition of new generations).
- future gas exchange region expands significantly.
- Fibroblastic cells also undergo differentiation, they produce extracellular matrix, collagen, and elastin.
- May have a role in epithelial differentiation and control of surfactant secretion.
- Alveolar Cells Type II (Type II pneumocytes)
- begin to secrete surfactant, levels of secretion gradually increase to term.
- allows alveoli to remain inflated
- Vascular tree - also grows in length and diameter during this time.
Alveolar stage
|
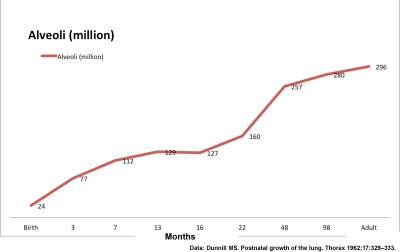
|
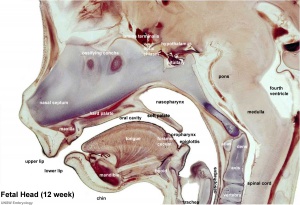
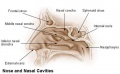
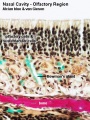
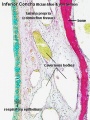
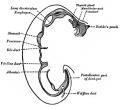
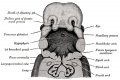
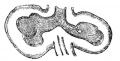
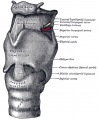
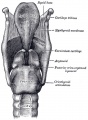
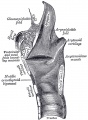
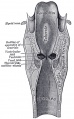
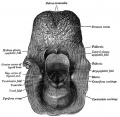
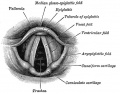
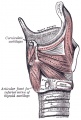
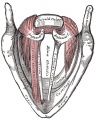
Upper Respiratory Tract
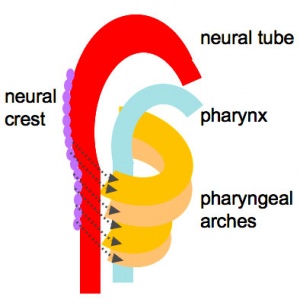
|

|
| Foregut cartoon | Pharynx |
Foregut Development - from the oral cavity the next portion of the foregut is initially a single gastrointestinal (oesophagus) and respiratory (trachea) common tube, the pharynx which lies behind the heart. Note that the respiratory tract will form from a ventral bud arising at this level.
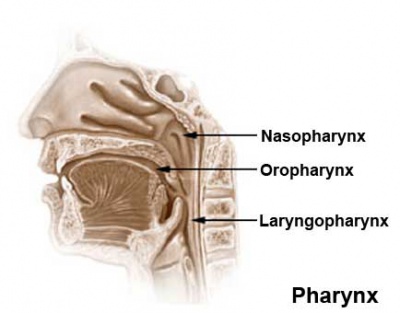
|
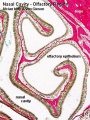
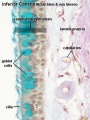
Note - Specialised olfactory epithelium for smell, a small region located in roof of nasal cavity. |
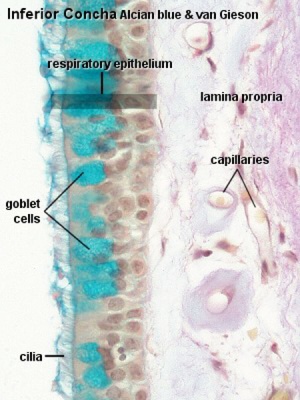
|
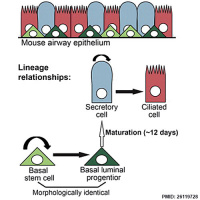
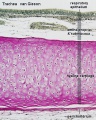
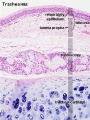
Respiratory epithelium
Respiratory epithelium development |
| Additional Information - Histology | ||
|---|---|---|
This will be covered in detail in your associated SH Practical class.
|
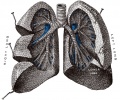
Lower Respiratory Tract
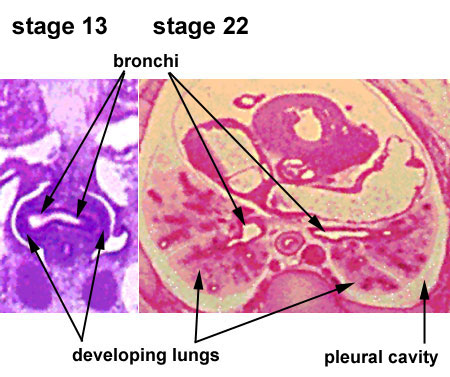
|
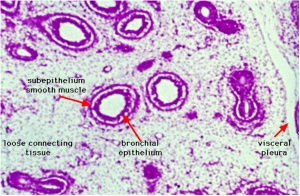
|
| Stage 13 (Week 4-5) | Stage 22 (Week 8) |
- lung buds ( endoderm epithelial tubes) grow/push into mesenchyme covered with pleural cells (lung border)
- generates a tree-like network by repeated:
- elongation
- terminal bifurcation
- lateral budding
Growth initially of branched "conducting" system of bronchial tree, followed by later development of the "functional units" of the alveoli.
| Additional Information - Histology | ||
|---|---|---|
| This will be covered in detail in your associated SH Practical class.
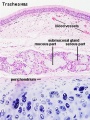
Respiratory Trachea Mucosa - formed by epithelium and underlying lamina propria.
Submucosa - connective tissue and submucosal glands
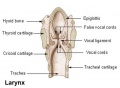
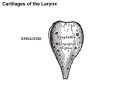
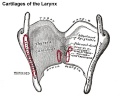
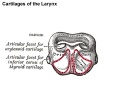
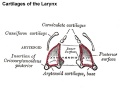
Cartilage
Hyaline Cartilage Development
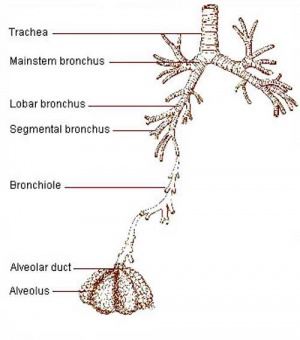
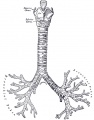
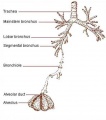
Bronchi Branching main bronchi -> lobar bronchi -> segmental bronchi (supply lung bronchopulmonary segments) -> bronchi -> bronchioles (smaller than 1 mm) -> respiratory bronchioles.
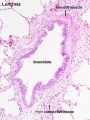
Bronchioles
Respiratory Bronchioles
|
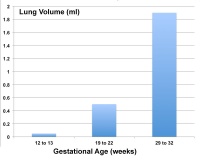
Fetal Lung Volume
Each human lung volume as determined by ultrasound and matched to gestational age [2]
|
|
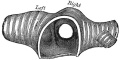
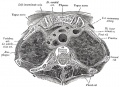
Pleural Cavity
- anatomical body cavity in which the lungs develop and lie.
- pleural cavity forms in the lateral plate mesoderm as part of the early single intraembryonic coelom.
- This cavity is initially continuous with pericardial and peritoneal cavities and form initially as two narrow canals.
- later becomes separated by folding (pleuropericardial fold, pleuroperitoneal membrane) and the later formation of the diaphragm.
- pleuropericardial fold - (pleuropericardial membrane) An early embryonic fold which restricts the communication between pleural cavity and pericardiac cavity, contains both the cardinal vein and phrenic nerve.
- pleuroperitoneal membrane - An early embryonic membrane that forms inferiorly at the septum transversum to separate peritoneal cavity from pleural cavity.
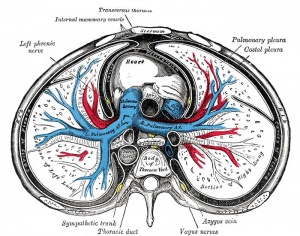
Pleura
- serous membrane covers the surface of the lung and the spaces between the lobes.
- arranged as a closed invaginated sac.
- two layers (pulmonary, parietal) continuous with each other, the potential space between them is the pleural cavity.
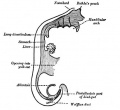
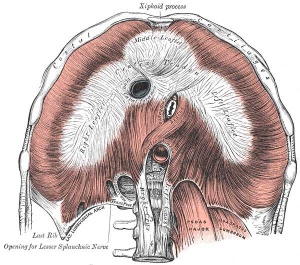
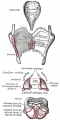
Diaphragm
- Not respiratory tract but musculoskeletal development, there are 5 embryonic elements that contribute to the diaphragm.
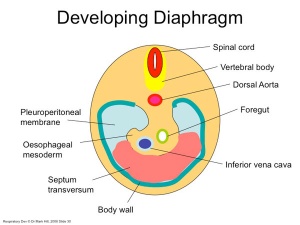
|
|
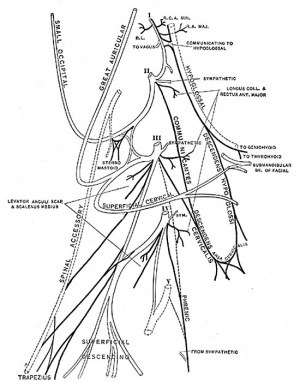
- Innervation of the human diaphragm is by the phrenic nerves
- arising from the same segmental levels from which the diaphragm skeletal muscles arise, segmental levels C3 to C5.
- The paired phrenic nerves are mixed nerves
- motor neurons for the diaphragm
- sensory nerves for other abdominal structures (mediastinum, pleura, liver, gall bladder).
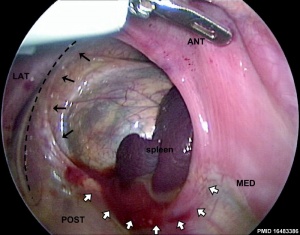
Bochdalek hernia - most common on the posterior left side (85%). Failure of the pleuroperitoneal foramen (foramen of Bochdalek) to close allows viscera into thorax. Intestine, stomach or spleen can enter the pleural cavity, compressing the lung.
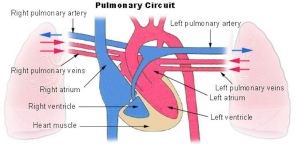
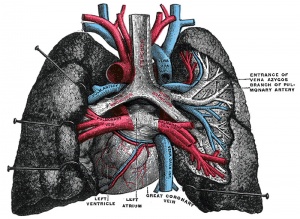
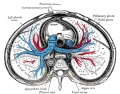
Pulmonary Circulation
- the pulmonary system not "functional" until after birth
- pulmonary arteries - 6th aortic arch arteries
- pulmonary veins - are incorporated into the left atrium wall
- bronchial arteries - branches from dorsal aorta
Fetal
Fetal Respiratory Movements
- Fetal respiratory movements (FRM) or Fetal breathing movements (FBM) are regular muscular contrations occurring in the third trimester.
- preparing the respiratory muscular system for neonatal function.
- may also have a role in late lung development.
The First Breath
- The respiratory system does not carry out its physiological function (gas exchange) prenatally and remain entirely fluid-filled until birth.
- At birth, fluid in the upper respiratory tract is expired and fluid in the lung aveoli is rapidly absorbed this event has also been called "dewatering of the lung".
- The lung epithelia has to now rapidly change from its prenatal secretory function to that of fluid absorbtion.
The exchange of lung fluid for air leads to:
- fall in pulmonary vascular resistance
- increase in pulmonary blood flow
- thinning of pulmonary arteries (stretching as lungs increase in size)
- blood fills the alveolar capillaries
In the heart - pressure in the right side of the heart decreases and pressure in the left side of the heart increases (more blood returning from pulmonary).
Postnatal
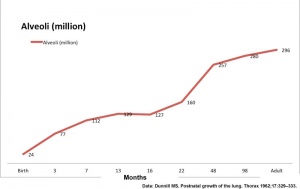
Alveoli
- At birth about 15% of adult alveoli number have formed
- 20 - 50 million to in the adult about 300 million.
- remaining subdivisions develop in the first few postnatal years
Respiratory Rate
- neonatal rate is higher (30-60 breaths/minute) than adult (12-20 breaths/minute).
- tachypnea - (Greek, rapid breathing) an increased respiratory rate of greater than 60 breaths/minute in a quiet resting baby
| Age | Rate (breaths/minute) |
| Infant (birth - 1 year) | 30 - 60 |
| Toddler (1 - 3 years) | 24 - 40 |
| Preschool (3 - 6 years) | 22 - 34 |
| School age (6 - 12 years) | 18 - 30 |
| Adolescent (12 - 18 years) | 12 - 16 |
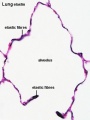
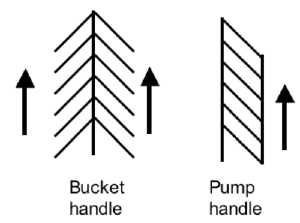
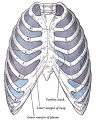
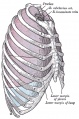
Rib Orientation
- Infant rib - is virtually horizontal, allowing diaphragmatic breathing only.
- Adult rib - is oblique (both anterior and lateral views), allows for pump-handle and bucket handle types of inspiration.
Respiratory Tract Abnormalities
Respiratory System - Abnormalities
- Meconium Aspiration Syndrome - (MAS) Meconium is the gastrointestinal contents that accumulate in the intestines during the fetal period. Fetal stress in the third trimester, prior to/at/ or during parturition can lead to premature meconium discharge into the amniotic fluid and sunsequent ingestion by the fetus and damage to respiratory function. Damage to placental vessels meconium myonecrosis may also occur.
- Newborn Respiratory Distress Syndrome - (Hyaline Membrane Disease) membrane-like substance from damaged pulmonary cells, absence of surfactant, if prolonged can be irreversible, intrauterine asphyxia, prematurity and maternal diabetes medline plus | eMedicine
- Tracheoesophageal Fistula - Tracheo-Oesophageal Fistula, Oesophageal Atresia - Oesophageal Atresia with or without tracheo-oesophageal fistula Fistula - an abnormal communication between 2 structures (organs, vessels, cavities) that do not normally connect.
- Lobar Emphysema (Overinflated Lung) - There is an overinflated left upper lobe There is a collapsed lower lobe The left lung is herniating across the mediastinum
- Congenital Diaphragmatic Hernia - (1 in 3,000 live births) Failure of the pleuroperitoneal foramen (foramen of Bochdalek) to close (left side), allows viscera into thorax -iIntestine, stomach or spleen can enter the pleural cavity, compressing the lung. rare (Morgagni hernia) -an opening in the front of the diaphragm. Congenital Diaphragmatic Hernia | GeneReviews
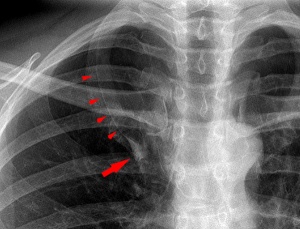
- Azygos Lobe - Common condition (0.5% of population). The right lung upper lobe expands either side of the posterior cardinal. There is also some course variability of the phrenic nerve in the presence of an azygos lobe.
- Congenital Laryngeal Webs - Laryngeal abnormality due to embryonic (week 10) incomplete recanalization of the laryngotracheal tube during the fetal period. Rare abnormality occuring mainly at the level of the vocal folds (glottis).
- Hyaline Membrane Disease - (Newborn Respiratory Distress Syndrome) a membrane-like substance from damaged pulmonary cells.
- Bronchopulmonary Dysplasia - A chronic lung disease which can occur following premature birth and related lung injury. Most infants who develop BPD are born more than 10 weeks before their due dates, weigh less than 1,000 grams (about 2 pounds) at birth, and have breathing problems.
- Asthma - Flow limitation during tidal expiration in early life significantly associated with the development of physician-diagnosed asthma by the age of 2 years. Infants with abnormal lung function soon after birth may have a genetic predisposition to asthma or other airway abnormalities that predict the risk of subsequent lower respiratory tract illness. PMID 8176553
- Cystic Fibrosis - Inherited disease of the mucus and sweat glands, causes mucus to be thick and sticky. Clogging the lungs, causing breathing problems and encouraging bacterial grow. (Covered elsewhere in the course)
- Environmental Factors see recent review below. <pubmed>20444669</pubmed>
Additional Information
| Respiratory Terms (expand to view) |
|---|
|
| Other Terms Lists |
|---|
| Terms Lists: ART | Birth | Bone | Cardiovascular | Cell Division | Endocrine | Gastrointestinal | Genital | Genetic | Head | Hearing | Heart | Immune | Integumentary | Neonatal | Neural | Oocyte | Palate | Placenta | Radiation | Renal | Respiratory | Spermatozoa | Statistics | Tooth | Ultrasound | Vision | Historic | Drugs | Glossary |
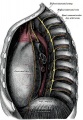
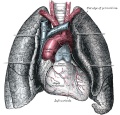
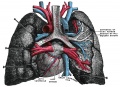
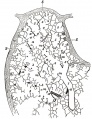
| Grays - Respiratory Images |
|---|
|
|
| Respiratory Histology |
|---|
Fetal Histology
|
| Adult Histology
|
|
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
| 2018 ANAT2341 - Timetable | Course Outline | Moodle | Tutorial 1 | Tutorial 2 | Tutorial 3 |
Labs: 1 Preimplantation and Implantation | 2 Reproductive Technology Revolution | 3 Group Projects | 4 GM manipulation mouse embryos | 5 Early chicken eggs | 6 Female reproductive tract | 7 Skin regeneration | 8 Vertebral development | 9 Organogenesis Lab | 10 Cardiac development | 11 Group projects | 12 Stem Cell Journal Club |
|
Lectures: 1 Introduction | 2 Fertilization | 3 Week 1/2 | 4 Week 3 | 5 Ectoderm | 6 Placenta | 7 Mesoderm | 8 Endoderm | 9 Research Technology | 10 Cardiovascular | 11 Respiratory | 12 Neural crest | 13 Head | 14 Musculoskeletal | 15 Limb | 16 Renal | 17 Genital | 18 Endocrine | 19 Sensory | 20 Fetal | 21 Integumentary | 22 Birth | 23 Stem cells | 24 Revision |
| Student Projects: Group Projects Information Project 1 | Project 3 | Project 4 | Project 5 | 2018 Test Student | Copyright |