Lecture - Renal Development
| Embryology - 7 Jun 2026 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
| <html5media height="520" width="360">File:Urogenital_sinus_001.mp4</html5media> | Urogenital Sinus and Renal Development
This animation gives an overview of both early renal and genital (urogenital) development associated with the urogenital sinus.
The urinary system is developmentally and anatomically associated with genital development, often described as the urogenital system.
|
Objectives
- Understand the 3 main stages of kidney development.
- Understand development of the nephron and renal papilla.
- Brief understanding of the mechanisms of nephron development.
- Understand the development of the cloaca, ureter and bladder.
- Brief understanding of abnormalities of the urinary system.
Lecture Resources
| Movies | ||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
| References | |
|---|---|
| Hill, M.A. (2020). UNSW Embryology (20th ed.) Retrieved Haziran 7, 2026, from https://embryology.med.unsw.edu.au | 2017 | 2016 | 2016 PDF | 2015 | 2015 PDF | |
| Moore, K.L., Persaud, T.V.N. & Torchia, M.G. (2015). The developing human: clinically oriented embryology (10th ed.). Philadelphia: Saunders. | The following chapter links only work with a UNSW connection. |
 Schoenwolf, G.C., Bleyl, S.B., Brauer, P.R., Francis-West, P.H. & Philippa H. (2015). Larsen's human embryology (5th ed.). New York; Edinburgh: Churchill Livingstone. Schoenwolf, G.C., Bleyl, S.B., Brauer, P.R., Francis-West, P.H. & Philippa H. (2015). Larsen's human embryology (5th ed.). New York; Edinburgh: Churchill Livingstone.
|
The following chapter links only work with UNSW Library subscription (with student Zpass log-in). |

Nussey, S. and Whitehead, S. (2001). Endocrinology - An Integrated Approach. UK Oxford: BIOS Scientific Publishers. ISBN-10: 1-85996-252-1 |
Detailed Table of Contents | Bookshelf Link |
| 2016 Lecture Video Recording |
|---|
| This 2016 lecture video recording is similar in content to the current 2017 online lecture.
<html5media height="600" width="800">File:2016Lecture-Renal.mp4</html5media> Click to play new window - 2016 Lecture Video (50 MB) |
Background
- mesoderm - then intermediate mesoderm
- endoderm - cloaca, urogenital sinus, hindgut, allantois
- Vascular Development
- Gastrointestional
- Cloacal development
- endocrine - covered in future lecture/lab
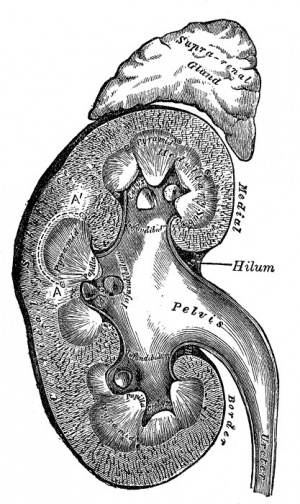
Renal Anatomy
Each adult human kidney typically contains about 750,000 nephrons, though the total number can vary significantly from as few as 250,000 to as many as 2,000,000.
Kidney
- Nephron - Functional unit of kidney
- Humans up to 1 million
- Filtration of waste from blood
- Endocrine
- Blood pressure regulation
Urine Transport/Storage
- Ureter - transport to bladder
- Urinary Bladder - storage
- Urethra - transport to exterior
Germ layers
- Endoderm - lining bladder also lines allantois
- Mesoderm - Intermediate mesoderm (lies between somites and lateral plate)
- Ectoderm - innervation
Intermediate Mesoderm
|
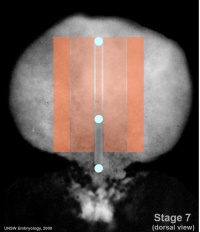
Intermediate mesoderm (dark orange) lies outside paraxial mesoderm (pale orange) Week 3 embryonic disc. |
Mesonephric Duct
- Begins as the pronephric duct.
- Mesonephros development becomes the mesonephric duct.
- Gives off lateral branches, the utereric bud.
- Grows within intermediate mesoderm to fuse with the cloaca.
- Mesonephric duct finally forms the male internal genital tract.
In development, both the mesonephric duct and the cloaca continue to differentiate and undergo extensive remodelling (and renaming)
Mesonephric duct forms - epididymis, ductus deferens, seminal vesicle
Ureteric Bud
- arise near the cloacal connection of the mesonephric duct
- branch from the mesonephric duct laterally into the intermediate mesoderm
- induce the surrounding mesoderm to differentiate - metanephric blastema
- this mesoderm will in turn signal back to differentiate the ureteric bud
Epithelial - mesenchymal interaction
Ureteric Bud forms - ureter, pelvis, calyces, collecting ducts
Metanephric Blastema
- forms glomeruli, capsule, nephron tubules
- this development continues through fetal period
Nephros Development
The 3 main stages and pairs form in sequence within the intermediate mesoderm:
- pronephros
- mesonephros
- metanephros
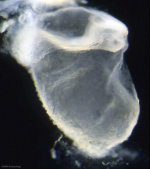
Pronephros
- week 3-4 few cells in cervical region (fish type kidney)
- Human E19, Mouse E7.5 - pronephric duct forms first with associated nephrogenic mesenchyme
- grows rostro caudally cervical -> cloaca
- Human E22 nephrogenic mesenchyme differentiates to form pronephroi not functional in mammals, degenerates rapidly
|
|
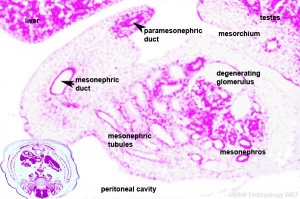
Mesonephros
- Human E24, Mouse E9.5 caudal to pronephros
- forms by induction from pronephros
- pronephric duct now becomes mesonephric duct (also called Wolffian Duct)
| GIT Stage 13 |
| Page | Play |
Metanephros
- Human E35-37, Mouse E11 epithelia bud at end of mesonephric duct ureteric bud and associated metanephric mesenchyme.
- This will eventually form the adult kidney.
| Urogenital |
| Page | Play |
Ureteric Bud
- extends laterally from the mesonephric duct
- induced by metanephric mesenchyme to differentiate
- forms collecting tubules, renal pelvis, ureter
Metanephric Mesenchyme
- the intermediate mesoderm lying at the tip of the ureteric bud.
- induced by ureteric bud to differentiate forms nephron
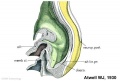
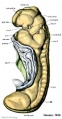
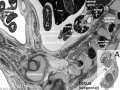
Week 5 and Week 8
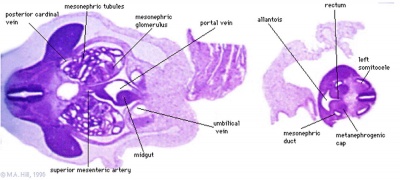
|
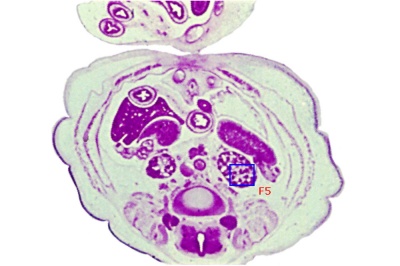
|
| Embryo Stage 13 mesonephros (week 5) | Embryo Stage 22 metanephros (week 8) |
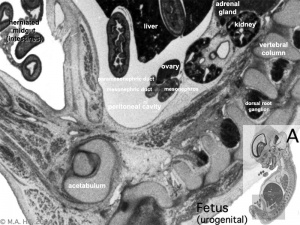
Fetal
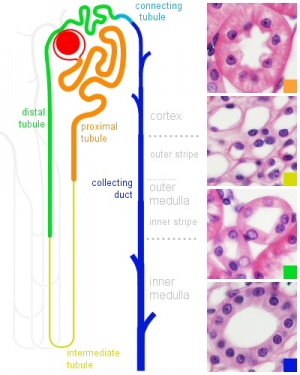
Nephron
| Nephron |
| Page | Play |
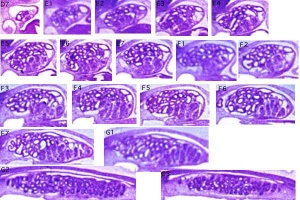
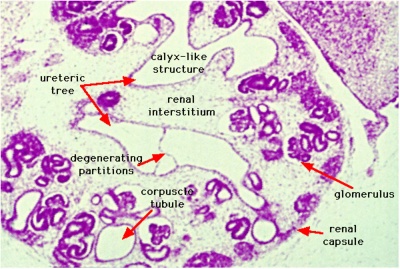
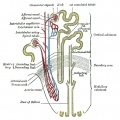
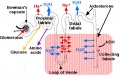
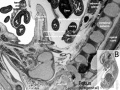
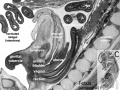
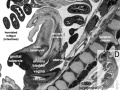
Early Renal Development
Legend
- Ureteric Bud - developing ureter, pelvis, calyces, collecting ducts
- Metanephric Blastema (intermediate mesoderm) - developing glomeruli, capsule, nephron tubules
Development has four developmental stages:
- vesicle (V) stage (13-19 weeks)
- S-shaped body (S) stage ( 20-24 weeks)
- capillary loop (C) stage (25-29 weeks)
- maturation (M) stage (infants aged 1-6 months)
Links: Nephron Movie | Urogenital Sinus Movie | Renal System Development
Nephron Development
- disorganised mesenchymal cells become a highly organised epithelial tubule
- Condensation - groups of about 100 cells condense tightly together to form a distinct mass
- Epithelialisation - condensed cells lose their mesenchymal character and gain epithelial
- At end of this period formed a small epithelial cyst complete with a basement membrane, cell-cell junctions and a defined cellular apico-basal polarity.
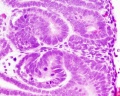
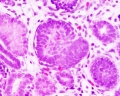
Early morphogenesis
|
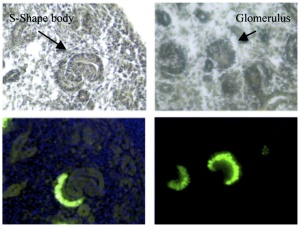
Renal - podocyte development |
| Glomerulus Development | |||
|---|---|---|---|
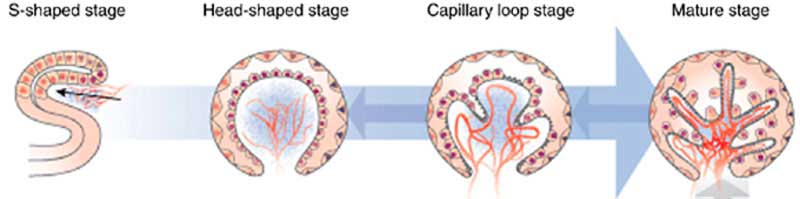
| |||
| S-shaped stage | Head-shaped stage | Capillary loop stage | Mature glomerulus |
| Developing podocytes acquire podocyte markers and blood vessels and mesenchyme invade (arrow). The podocytes (round nuclei) separate from the parietal epithelial cells (triangular nuclei) forming what will become Bowman's space. | the glomerulus now consists of a ball of cell surrounded by developing podocytes. | this stage of glomerular development includes the infolding of the surface layer in order to enlarge the area available for filtration as well as the development of foot processes that interdigitate between podocytes and abut the underlying GBM which is being synthesized as a collaboration between the podocyte and underlying endothelial and mesangial cells. | the mature glomerulus has maximized filtration surface area by developing intertwining finger-like projections coated by fenestrated endothelial cells on the inside, a specialized strong thin GBM in the middle, and interdigitating podocyte foot processes connected by slit diaphragms on the outer surface. |
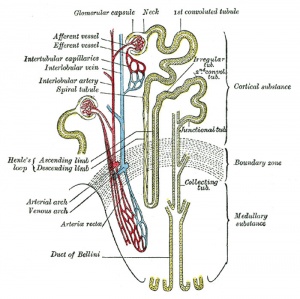
Adult nephron structure
| Key structure of the adult nephron is the glomerulus (renal corpuscle), which represents the vascular/renal interface.
Related Images: Nephron histology overview | glomerulus structure | vascular and renal poles |
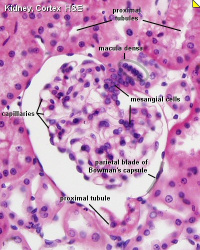
Glomerulus structure |
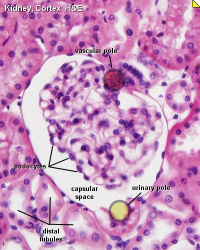
Vascular and renal poles |
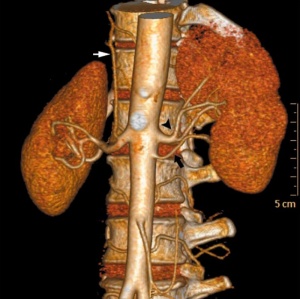
Renal Vascular
Renal Arteries
|
|
- Arise with ascent and inferior branches lost
- Sequential, 25% population have 2 or more renal arteries
- branch of abdominal aorta, divides into 4-5 branches
- each gives off small branches to suprarenal glands, ureter, surrounding cellular tissue and muscles
- Frequently a second renal artery (inferior renal) from abdominal aorta at a lower level, supplies lower portion of kidney.
Renal Venous
These vascular changes embryonic to adult shown below are shown for information purposes and not assessable.
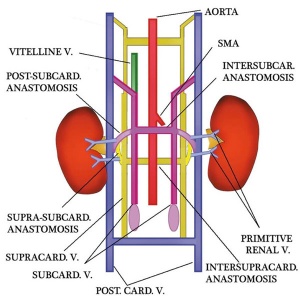
|
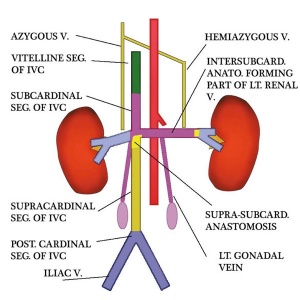
|
| Embryo renal venous | Adult renal venous |
Endocrine Kidney
Covered also in Endocrine Development lecture
- Renin - Increase Angiotensin-aldosterone system
- Prostaglandins - decrease Na+ reabsorption
- Erythropoietin - (Epo) increase erythrocyte (rbc) production
- 1,25 (OH)2 vitamin D - Calcium homeostasis
- Prekallikreins - (plasma protein inactive precursor of kallikrein)
- Increase kinin production (altered vascular permeability)
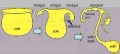
Cloaca
|
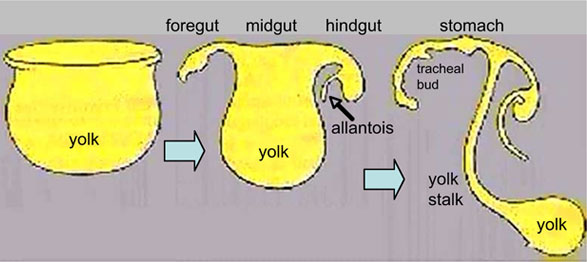
This cartoon sequence shows the changing organisation of the endoderm from week 3 to 5. |
Common urogenital sinus
- Endoderm lining
- superior end continuous with allantois
- common urogenital sinus and mesonephric duct fuse (connect)
- differentiates to form the bladder
- inferior end forms urethra
- this will be different in male and female development
Urinary Bladder
|
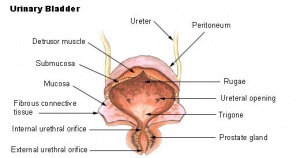
Adult bladder |
Bladder Structure
| Histology | Adult histology | Detrusor Muscle |
|---|---|---|
Described anatomically by 4 layers from outside inward:
|
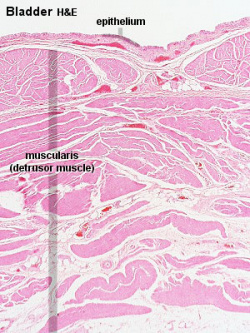
|
Adult detrusor muscle consists of three layers of smooth (involuntary) muscle fibres.
|
Ureter Development
- Ureteric bud origin
- Adult ureter is a thick-walled muscular tube, 25 - 30 cm in length, running from the kidney to the urinary bladder.
- Anatomically two parts the abdominal part (pars abdominalis) and pelvic part (pars pelvina).
- Ureter has three layers: outer fibrous layer (tunica adventitia), muscular layer (tunica muscularis) and mucous layer (tunica mucosa).
- The muscular layer can also be subdivided into 3 fibre layers: an external longitudinal, a middle circular, and an internal longitudinal.
Urethra Development
- Further development of the urinary system varies depending on the sex of the embryo.
- Males - the pelvic urethra forms the membranous urethra, the prostatic urethra and penile urethra. (The sex of the above animation and sections is male)
- Females - the pelvic urethra forms the membranous urethra and the vestibule of the vagina.
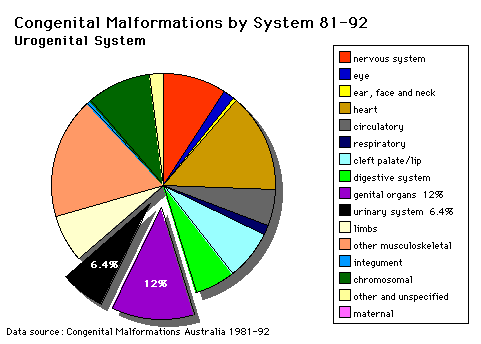
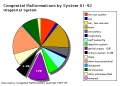
Abnormalities
| ICD10 Congenital malformations of the urinary system (Q60-Q64) | ||||
|---|---|---|---|---|
| The International Classification of Diseases (ICD) World Health Organization's classification used worldwide as the standard diagnostic tool for epidemiology, health management and clinical purposes. Includes this section on XVII Congenital Malformations. | ||||
| Q60 Renal agenesis and other reduction defects of kidney
Incl.: atrophy of kidney: congenital infantile congenital absence of kidney
| ||||
| Q61 Cystic kidney disease
Excl.: acquired cyst of kidney (N28.1) Potter's syndrome (60.6)
| ||||
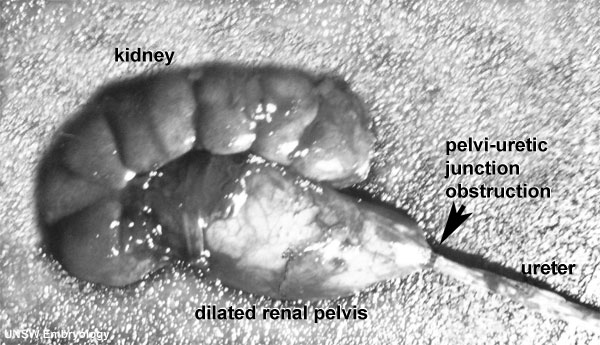
Q62 Congenital obstructive defects of renal pelvis and congenital malformations of ureter
| ||||
| Q63 Other congenital malformations of kidney
Excl.: congenital nephrotic syndrome (N04.-)
| ||||
Q64 Other congenital malformations of urinary system
| ||||
| World Health Organisation. International Statistical Classification of Diseases and Related Health Problems. (1992) 10th Revision (ICD-10). Geneva: WHO ICD-10 - 2016 Online (English) | ||||
| ||||
| ICD10 - Gastrointestinal | Genital | Renal | Integumentary |
Horseshoe Kidney
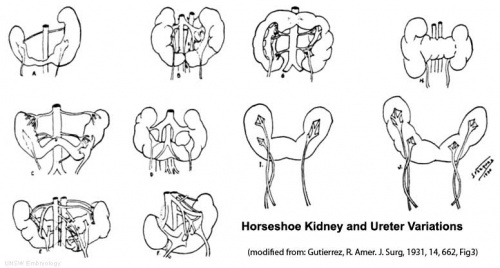
|
|
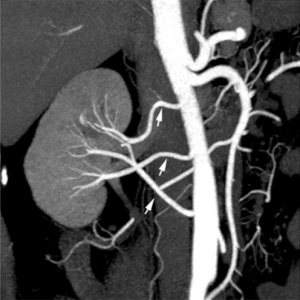
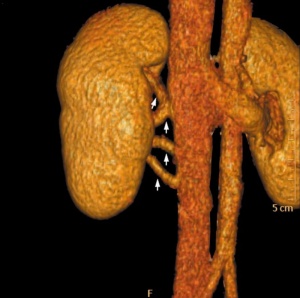
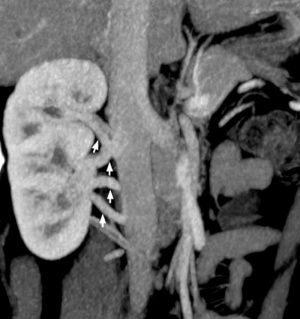
Kidney Vascular
Supernumerary renal arteries
Supernumerary renal vein
Urorectal Septum Malformation
- thought to be a deficiency in caudal mesoderm which in turn leads to the malformation of the urorectal septum and other structures in the pelvic region.
- Recent research has also identified the potential presence of a persistent urachus prior to septation of the cloaca (common urogenital sinus).
Bladder
- absent or small bladder -
associated with renal agenesis.
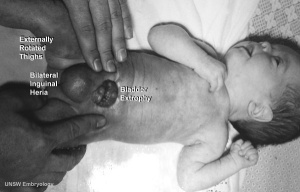
Bladder Exstrophy
- developmental abnormality associated with bladder development.
- origins appear to occur not just by abnormal bladder development, but by a congenital malformation of the ventral wall of abdomen (between umbilicus and pubic symphysis).
- There may also be other anomolies associated with failure of closure of abdominal wall and bladder (epispadias, pubic bone anomolies).
Ureter and Urethra
- Ureter - Duplex Ureter
- Urethra- Urethral Obstruction and Hypospadias
Hydronephrosis
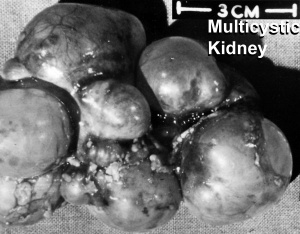
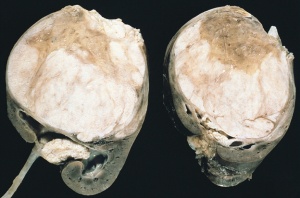
Polycystic Kidney Disease
- diffuse cystic malformation of both kidneys
- cystic malformations of liver and lung often associated, Often familial disposition
- Two types
- Infantile (inconsistent with prolonged survival)
- Adult (less severe and allows survival)
- Autosomal dominant PKD disease - recently identified at mutations in 2 different human genes encoding membrane proteins (possibly channels)
Wilms' Tumor
- (nephroblastoma) Named after Max Wilms, a German doctor who wrote first medical articles 1899
- most common type of kidney cancer children
- WT1 gene - encodes a zinc finger protein
- Both constitutional and somatic mutations disrupting the DNA-binding domain of WT1 result in a potentially dominant-negative phenotype
- some blastema cells (mass of undifferentiated cells) persist to form a ‘nephrogenic rest’
- Most rests become dormant or regress but others proliferate to form hyperplastic rests
- any type of rest can then undergo a genetic or epigenetic change to become a neoplastic rest
- can proliferate further to produce a benign lesion (adenomatous rest) or a malignant Wilms’ tumour
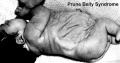
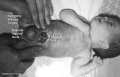
Prune Belly Syndrome
- lower urinary tract obstruction
- mainly male
- fetal urinary system ruptures leading to collapse and "prune belly" appearance.
Additional Images
References
Textbooks
- The Developing Human: Clinically Oriented Embryology (8th Edition) by Keith L. Moore and T.V.N Persaud - Moore & Persaud Chapter 13 p303-346
- Larsen’s Human Embryology by GC. Schoenwolf, SB. Bleyl, PR. Brauer and PH. Francis-West - Chapter 10 p261-306
- Before We Are Born (5th ed.) Moore and Persaud Chapter14 p289-326
- Essentials of Human Embryology, Larson Chapter 10 p173-205
- Human Embryology, Fitzgerald and Fitzgerald Chapter 21-22 p134-152
Online Textbooks
- Developmental Biology by Gilbert, Scott F. Sunderland (MA): Sinauer Associates, Inc.; c2000 Chapter 14 Intermediate Mesoderm | Figure 14.18. General scheme of development in the vertebrate kidney | Figure 23-23. Mechanism of mesenchymal inductive effect on the ureteric bud | Figure 14.21. Ureteric bud growth is dependent on GDNF and its receptor
- Molecular Cell Biology by Lodish, Harvey; Berk, Arnold; Zipursky, S. Lawrence; Matsudaira, Paul; Baltimore, David; Darnell, James E. New York: W. H. Freeman & Co.; c1999 Reciprocal Epithelial-Mesenchymal Interactions Regulate Kidney Development | Figure 23-21. Embryonic development of the kidney
Reviews
- Quaggin SE, Kreidberg JA. Development of the renal glomerulus: good neighbors and good fences. Development. 2008 Feb;135(4):609-20. PMID: 18184729
- Brenner-Anantharam A, Cebrian C, Guillaume R, Hurtado R, Sun TT, Herzlinger D. Tailbud-derived mesenchyme promotes urinary tract segmentation via BMP4 signaling. Development. 2007 May;134(10):1967-75. PMID: 17442697
- Forefronts Symposium on Nephrogenetics: from development to physiology March 8-11, 2007 Danvers, MA A meeting to synthesize an integrated view of the normal development and function of the kidney from the genetic standpoint.
- Costantini F. Renal branching morphogenesis: concepts, questions, and recent advances. Differentiation. 2006 Sep;74(7):402-21. PMID: 16916378
Search
- Bookshelf intermediate mesoderm | kidney development | renal development | ureteric bud | nephron development | bladder development
- Pubmed intermediate mesoderm | kidney development | renal development | ureteric bud | nephron development | bladder development
Terms
| Renal Terms | ||
|---|---|---|
| ||
|
| 2018 ANAT2341 - Timetable | Course Outline | Moodle | Tutorial 1 | Tutorial 2 | Tutorial 3 |
Labs: 1 Preimplantation and Implantation | 2 Reproductive Technology Revolution | 3 Group Projects | 4 GM manipulation mouse embryos | 5 Early chicken eggs | 6 Female reproductive tract | 7 Skin regeneration | 8 Vertebral development | 9 Organogenesis Lab | 10 Cardiac development | 11 Group projects | 12 Stem Cell Journal Club |
|
Lectures: 1 Introduction | 2 Fertilization | 3 Week 1/2 | 4 Week 3 | 5 Ectoderm | 6 Placenta | 7 Mesoderm | 8 Endoderm | 9 Research Technology | 10 Cardiovascular | 11 Respiratory | 12 Neural crest | 13 Head | 14 Musculoskeletal | 15 Limb | 16 Renal | 17 Genital | 18 Endocrine | 19 Sensory | 20 Fetal | 21 Integumentary | 22 Birth | 23 Stem cells | 24 Revision |
| Student Projects: Group Projects Information Project 1 | Project 3 | Project 4 | Project 5 | 2018 Test Student | Copyright |