Introduction
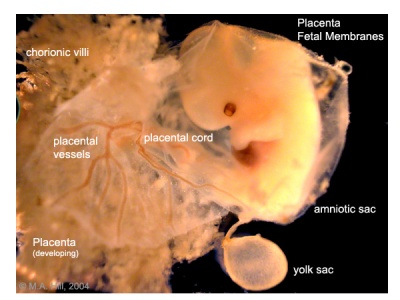
Human Placental Membranes
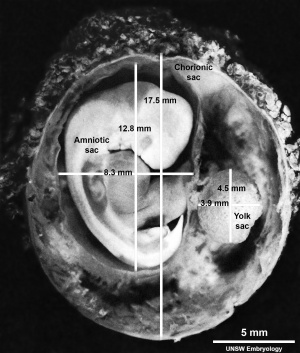
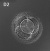
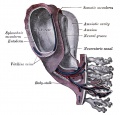
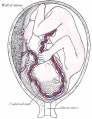
Stage17 embryo and membranes
The placental membranes is a term often used to describe the all the fetal components of the placenta (Greek, plakuos = flat cake).
This page will not cover the whole placenta, just the development of the extra-embryonic membranes that form the extra-embryonic coeloms (cavities or spaces); amnionic sac, chorionic sac, yolk sac and allantois.
In monozygotic twinning, depending upon when the twinning event occurred, each embryo will either share or have completely separate set of placental membranes.
Extra-embryonic Coeloms
|
|
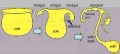
- Yellow - yolk sac, below the embryonic disc
- Blue - amniotic cavity, above the embryonic disc
- White - chorionic cavity, surrounding the amniotic and yolk sacs
Connecting stalk (body stalk) shown to the right linking to the developing placenta.
|
Coelomic Cavity Development
Some Recent Findings
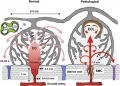
- Function and failure of the fetal membrane: Modelling the mechanics of the chorion and amnion[1] "The fetal membrane surrounds the fetus during pregnancy and is a thin tissue composed of two layers, the chorion and the amnion. While rupture of this membrane normally occurs at term, preterm rupture can result in increased risk of fetal mortality and morbidity, as well as danger of infection in the mother. Although structural changes have been observed in the membrane in such cases, the mechanical behaviour of the human fetal membrane in vivo remains poorly understood and is challenging to investigate experimentally. Therefore, the objective of this study was to develop simplified finite element models to investigate the mechanical behaviour and rupture of the fetal membrane, particularly its constituent layers, under various physiological conditions. It was found that modelling the chorion and amnion as a single layer predicts remarkably different behaviour compared with a more anatomically-accurate bilayer, significantly underestimating stress in the amnion and under-predicting the risk of membrane rupture. Additionally, reductions in chorion-amnion interface lubrication and chorion thickness (reported in cases of preterm rupture) both resulted in increased membrane stress. Interestingly, the inclusion of a weak zone in the fetal membrane that has been observed to develop overlying the cervix would likely cause it to fail at term, during labour. Finally, these findings support the theory that the amnion is the dominant structural component of the fetal membrane and is required to maintain its integrity. The results provide a novel insight into the mechanical effect of structural changes in the chorion and amnion, in cases of both normal and preterm rupture."
- The embryo reunited with its membranes in Göttingen[2] "An EMBO workshop entitled 'Embryonic-Extraembryonic Interfaces' took place in Göttingen, Germany, in May 2015. It showcased the enormous breadth of this area not only by touching on the molecular and cellular mechanisms of development, but also because of its coverage of particularly interesting evolutionary questions and of several medically related aspects. This Meeting Review discusses some highlights from the workshop and the emerging themes in the field."
|
| Older papers
|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
- Complete chorion-amnion separation presenting as a stuck fetus[3] "During feto-placental development, chorion-amnion fusion occurs in early second trimester and persistent separation of the membranes beyond 17 weeks' gestation is considered abnormal. Several reports have shown that complete chorion-amnion separation, defined as the amnion being separated from the chorion on at least three sides of the gestational sac, is associated with prenatal invasive procedures including amniocentesis. We would like to call attention to a case of complete chorion-amnion separation that occurred without any invasive procedures."
|
Reading

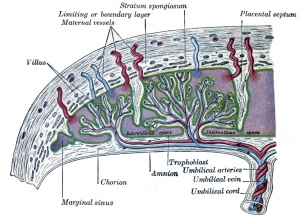
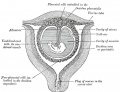
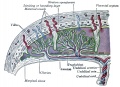
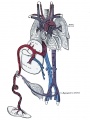
Historic image of placenta and fetus
- Human Embryology (2nd ed.) Larson Chapter 7 p151-188 Heart, Chapter 8 p189-228 Vasculature
- The Developing Human: Clinically Oriented Embryology (6th ed.) Moore and Persaud Chapter 14: p304-349
- Before we Are Born (5th ed.) Moore and Persaud Chapter 12; p241-254
- Essentials of Human Embryology Larson Chapter 7 p97-122 Heart, Chapter 8 p123-146 Vasculature
- Human Embryology Fitzgerald and Fitzgerald Chapter 13-17: p77-111
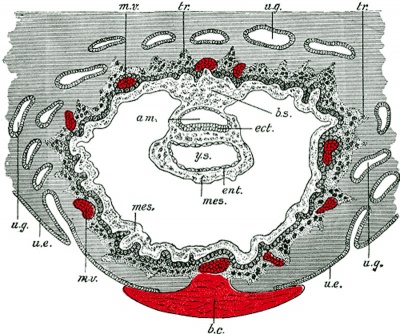
Day 8 to 9 early (Week 2) extra-embryonic coeloms (cavities)
Movies
- Links: Movies
Initial Conceptus Cavities
| <html5media height="580" width="500">File:Chorion 001.mp4</html5media>
|
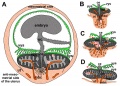
Animation shows the events following implantation and focuses on changes in the the spaces surrounding the embryonic disc, the extraembryonic coelom. Week 2 the blastoceol cavity is initially converted into a primary yolk sac by hypoblast layer. Week 2 to 3 then with gastrulation by endoderm and extra-embryonic mesoderm into two separate spaces: the yolk sac and the chorionic cavity. The third space lies above the epiblast, the amniotic cavity.
blue - epiblast layer
yellow - hypoblast layer
red cells - extraembryonic mesoderm layer
green - trophoblast layer
red spaces - blood-filled spaces, maternal lacunae
white cells - (left) endometrial gland (right) endometrial epithelium
|
Amnionic Sac
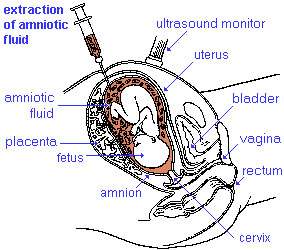
Amniocentesisis a prenatal diagnostic test, carried out by removing a small fluid sample.
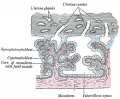
The amniotic sac (cavity) is initially lined by ectoderm and covered by extra-embryonic mesoderm. In the human embryo during week 3 to 4, folding of the embryonic disc draws the amniotic membrane ventrally over the embryo leading to the enclosing of the embryo within the amniotic sac. Embryonic and fetal development from this time onward occurs fully enclosed within the amniotic sac floating in the amniotic fluid.
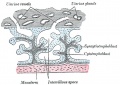
The membrane consists of three layers - epithelial monolayer, acellular connective tissue and fibroblast layer, see review[4]
Epithelial Monolayer
Cuboidal cell epithelium with a basement membrane. These cells are in direct contact with the amniotic fluid.
Secrete
- glycoproteins and collagen fibres to form the basal membrane.
- variety of growth factors and cytokines - epidermal growth factor, vascular endothelial growth factor, keratinocyte growth factor, basic fibroblast growth factor, transforming growth factors alpha and beta (TGF-α and TGF-β), interleukin-8 (IL-8), angiogenin, dipeptidyl peptidase IV (DPPIV/CD26), serine protease inhibitor (serpin) E1, also known as type 1 plasminogen activator inhibitor (PAI-1), insulin-like growth factors.
Connective Tissue
An underlying compact layer without cells of connective tissue bundles of collagen for membrane mechanical strength.
Fibroblast Layer
Under the acellular CT layer lies a thick layer of fibroblast cells forming a stroma.
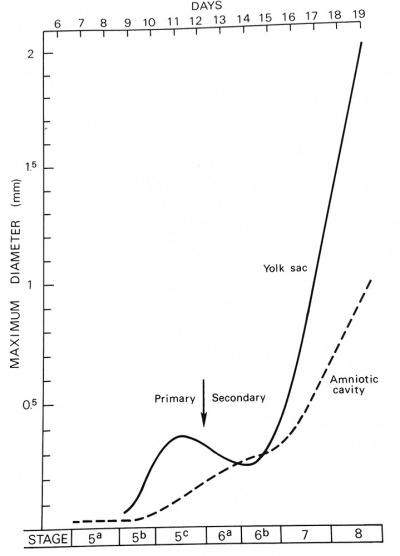
Yolk sac and amniotic cavity volume week 2 to 3 (stage 5, 6, 7 and 8).
Amniotic Fluid
The amniotic fluid has been described as having several functions:
- cushions the fetus against physical trauma.
- allows fetal growth free from restriction or distortion by the adjacent structures.
- provides a thermally stable environment.
- contributes to respiratory and gastrointestinal development.
- helps prevent infection.
- can provide a short-term source of nutrients and fluid to the embryo.[5]
Amniotic fluid is often assessed for both quality and quantity. The volume increases as the fetus grows and rate of change varies during the pregnancy.
- up to 8 weeks - increases at the rate of 10 ml/week
- 8 to 13 weeks - increases at the rate of 25 ml/week
- 13 to 21 weeks - increases at the rate of 60 ml/week
- 21 to 33 weeks - amniotic volume increase starts decreasing and eventually plateaus.
- 34 weeks (GA) - peaks at about 800 mL.
- 40 weeks (GA) - about 600 mL at term.
Fluid Facts
- Circulated by fetal inhaling and swallowing.
- Replaced by fetal exhalation and urination.
- Magnesium low levels associated with preeclampsia and diabetes.
- normal magnesium value at 16 weeks (GA) is 1.65 ± 0.16 mg/dL in amniotic fluid and 1.97 ± 0.23 mg/dL in serum.[6]
Amniotic Fluid Swallowing
In early embryonic development both the buccopharyngeal and cloacal membranes degenerated, allowing the GIT to be filled with amniotic fluid. Towards the end of the fetal period the fetus is now swallowing approximately 500 ml of amniotic fluid / day.
This swallowed amniotic fluid moves through the GIT from esophagus, to stomach, to small intestine, stopping at the large bowel. In the large bowel the majority of fluid (water) is absorbed, along with electrolytes, glucose, urea and hormones. This process may contribute to fetal nutrition and prepare the GIT for its postnatal function. The process of swallowing amniotic fluid has been suggested to also help regulate fluid volume.
- Links: Amniocentesis
Chorionic Sac
chorionic sac, chorionic cavity
The chorionic sac (cavity) is lined by extra-embryonic mesoderm and covered in trophoblast cells forming villi. In the human embryo during week 3 this space forms outside the yolk sac and surrounding the amniotic sac.
This forms a transient fluid-filled space that is lost by expansion of the amniotic sac, which eventually fuses to the chorionic membrane.
Yolk Sac
yolk sac
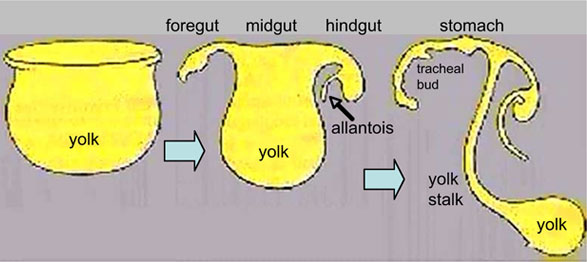
The ventral endoderm lines and extra-embryonic mesoderm covers the space called the yolk sac (yellow). Folding of the embryonic disc "pinches off" part of this yolk sac forming the first primitive gastrointestinal tract.
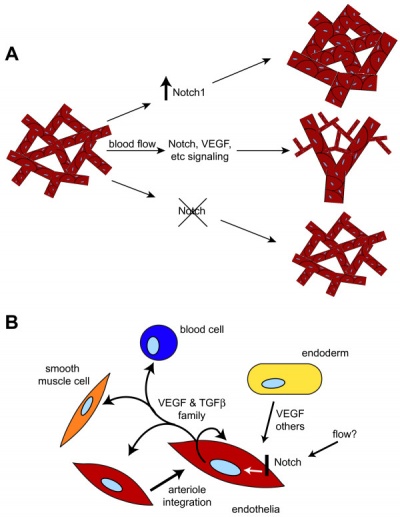
Notch and yolk sac blood vessels model[7]
- Links: Yolk Sac
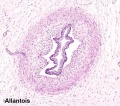
Allantois
An extra-embryonic membrane, endoderm in origin as an extension from the early hindgut, then cloaca into the connecting stalk of placental animals, connected to the superior end of developing bladder.
In reptiles and birds, acts as a reservoir for wastes and mediates gas exchange. In mammals is associated/incorporated with connecting stalk/placental cord fetal-maternal interface.
A recent comparative study looking at allantois structure in mouse, pig, rabbit and man[8] found the following:
- tissue interaction between endoderm and mesoderm required for allantoic development and vascular differentiation in species with a rudimentary allantoic diverticulum
- allantoic mesothelium plays a role in chorioallantoic attachment, allantoic differentiation and vascularization
- a pronounced diversity in the extraembryonic migratory pathways of primordial germ cells among mammals
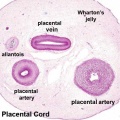
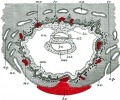
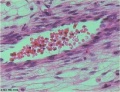
Placental cord cross-section
Term Membranes
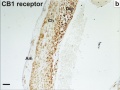
Cannabinoid Receptor 1 (CB1)
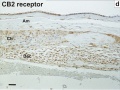
Cannabinoid Receptor 2 (CB2)
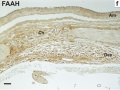
Fatty acid amide hydrolase (FAAH)
Abnormalities
Monoygotic Twinning
Monoygotic twins (identical) produced from a single fertilization event (one fertilised egg and a single spermatazoa, form a single zygote), these twins therefore share the same genetic makeup. Occurs in approximately 3-5 per 1000 pregnancies, more commonly with aged mothers.
The later the twinning event occurs, the less common are the initially separate placental membranes (diamniotic, dichorionic) and finally resulting in conjoined twins.
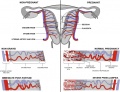
Table based upon recent a recent twinning review.[9] Links: twinning
Table based upon[9]
Chorioamnionitis
(CA) An intraamniotic puerperal infection described as having 3 forms: histologic, clinical (clinical chorioamnionitis, IAI), and subclinical. Intraamniotic infection is a common (2-4%) event in labor and the systemic inflammatory response can also lead to preterm birth and neonatal complications.
- Links: Placenta - Abnormalities
References
- ↑ Verbruggen SW, Oyen ML, Phillips AT & Nowlan NC. (2017). Function and failure of the fetal membrane: Modelling the mechanics of the chorion and amnion. PLoS ONE , 12, e0171588. PMID: 28350838 DOI.
- ↑ Stern C. (2015). The embryo reunited with its membranes in Göttingen. Development , 142, 2727-9. PMID: 26286940 DOI.
- ↑ Kasuga Y, Miyakoshi K, Ikenoue S, Kadohira I, Matsumoto T, Minegishi K & Yoshimura Y. (2013). Complete chorion-amnion separation presenting as a stuck fetus. Acta Obstet Gynecol Scand , 92, 990-1. PMID: 23647025 DOI.
- ↑ Favaron PO, Carvalho RC, Borghesi J, Anunciação AR & Miglino MA. (2015). The Amniotic Membrane: Development and Potential Applications - A Review. Reprod. Domest. Anim. , 50, 881-92. PMID: 26510939 DOI.
- ↑ Hall NJ, Drewett M & Burge D. (2019). Nutritional role of amniotic fluid: clues from infants with congenital obstruction of the digestive tract. Arch. Dis. Child. Fetal Neonatal Ed. , 104, F199-F201. PMID: 29666202 DOI.
- ↑ Bocos Terraz JP, Izquierdo Álvarez S, Bancalero Flores JL, González López A & Escanero Marcén JF. (2011). Magnesium concentration in amniotic fluid in the early weeks of the second trimester of pregnancy. BMC Res Notes , 4, 185. PMID: 21672230 DOI.
- ↑ Copeland JN, Feng Y, Neradugomma NK, Fields PE & Vivian JL. (2011). Notch signaling regulates remodeling and vessel diameter in the extraembryonic yolk sac. BMC Dev. Biol. , 11, 12. PMID: 21352545 DOI.
- ↑ Hassan W & Viebahn C. (2017). A correlative study of the allantois in pig and rabbit highlighting the diversity of extraembryonic tissues in four mammalian species, including mouse and man. J. Morphol. , 278, 600-620. PMID: 28165148 DOI.
- ↑ 9.0 9.1 Hall JG. (2003). Twinning. Lancet , 362, 735-43. PMID: 12957099 DOI.
Reviews
Tavian M, Biasch K, Sinka L, Vallet J & Péault B. (2010). Embryonic origin of human hematopoiesis. Int. J. Dev. Biol. , 54, 1061-5. PMID: 20711983 DOI.
Burton GJ, Hempstock J & Jauniaux E. (2001). Nutrition of the human fetus during the first trimester--a review. Placenta , 22 Suppl A, S70-7. PMID: 11312634 DOI.
Docherty SM, Iles RK, Wathen N & Chard T. (1996). The temporary anatomical structures prominent in the first trimester may be fulfilling exchange functions assigned to the placenta in the second and third trimester. Hum. Reprod. , 11, 1157-61. PMID: 8671414
Articles
Search PubMed
Search April 2010
- Placental Membranes - All (10083) Review (748) Free Full Text (1728)
Search Pubmed: Placental Membranes | amniotic sac development | chorionic sac development | yolk sac development | allantois development
Additional Images
see all online Placental materials
Fetal membrane and placenta cartoon
Placenta spiral artery conversion
Uterine and placental vasculature
Fetal circulation overview
Placental cord cross-section
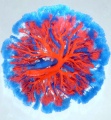
Human placenta viewed from the fetal side
Cord with one artery and one vein
Terms
| Placenta Terms (expand to view)
|
- after-birth - term used to describe the delivery of placenta and placental membranes following birth of the child.
- allantois - An extraembryonic membrane, endoderm in origin extension from the early hindgut, then cloaca into the connecting stalk of placental animals, connected to the superior end of developing bladder. In reptiles and birds, acts as a reservoir for wastes and mediates gas exchange. In mammals is associated/incorporated with connecting stalk/placental cord fetal-maternal interface.
- amniocentesis - Clinical term for a prenatal diagnostic test where an ultrasound guided needle is used to extract a sample of the amniotic fluid. Amniocentesis
- anastomosis - Term used to describe the connection between two tubes. Applied to describe the connection between peripheral blood vessels without an intervening capillary bed.
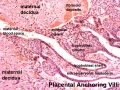
- anchoring villi - (stem villi) describes the placental villi (embryonic) that attach to the decidua (maternal) tissue. The tip of the villi consists of a column of trophoblast cells attached to an epithelial plaque.
- angioblasts form clusters or blood islands on surface of yolk sac.
- angiogenesis - Term describing the development of new vessels from already existing vessels, this process is secondary to vasculogenesis which is the initial formation of first blood vessels by differentiation of pluripotent mesenchymal cells (extraembryonic mesoderm).
- capsularis - portion of maternal decidua that covers the conceptus facing towards the uterine cavity.
- cerebroplacental ratio - (CPR) a doppler ultrasound measurement calculated as the simple ratio between the middle cerebral artery pulsatility index (MCA‐PI) and the umbilical artery pulsatility index (UA‐PI). Fetuses with an abnormal ratio are thought to be a predictor of adverse pregnancy outcome.
- chorioamnionitis - (CA) An intraamniotic puerperal infection described as having 3 forms: histologic, clinical (clinical chorioamnionitis, IAI), and subclinical. Intraamniotic infection is a common (2-4%) event in labor and the systemic inflammatory response can also lead to preterm birth and neonatal complications.
- chorion - The extraembryonic membrane generated from trophoblast and extraembryonic mesoderm that forms placenta. chorion and amnion are made by the somatopleure. The chorion becomes incorporated into placental development. The avian and reptilian chorion lies beside the egg shell and allows gas exchange.
- chorionic cavity - The fluid-filled extraembryonic coelom (cavity) formed initially from trophoblast and extraembryonic mesoderm that forms placenta. chorion and amnion are made by the somatopleure. The chorion becomes incorporated into placental development. The avian and reptilian chorion lies beside the egg shell and allows gas exchange. In humans, this cavity is lost during week 8 when the amniotic cavity expands and fuses with the chorion.
- chorion frondosum - (frondosum = leafy) The chorion found on conceptus oriented towards maternal blood supply where the majority of villi form and proliferate, will contribute the fetal component of the future placenta.
- chorion laeve - (laeve = smooth) The smooth chorion found on conceptus away from maternal blood supply (towards uterine epithelium and cavity) with very few villi present.
- chorionic somatomammotropin - (CSH, human lactogen) A hormone synthesized within the placenta by syncytiotrophoblast cells. This protein hormone (190 amino acid) has a structure is similar to pituitary growth hormone.
- chorionic villus sampling - (CVS) The taking a biopsy of the placenta, usually at the end of the second month of pregnancy, to test the fetus for genetic abnormalities.
- coelocentesis - A sampling of extracoelomic fluid usually for an early prenatal diagnostic technique.
- connecting stalk - the original extra-embryonic mesoderm structure attaching the embryonic disc to the chorion. The placental blood vessels form within this structure.
- cord blood - (human umbilical cord blood, HUCB) A term used to describe blood collected from the placenta usually after birth. Has been identified as a source of stem cells with potential therapeutic uses and is stored in Cord Blood Banks throughout the world.
- cord knotting Term describing umbilical or placental cord knotting. This occurs in about 1% prevents the passage of placental blood, pseudoknots also occur usually with no effect.
- cord presentation - A term used to describe at birth the presence of the umbilical cord between the fetal presenting part and the cervix, with or without membrane rupture.
- cord prolapse - A term used to describe at birth the descent of the umbilical cord through the cervix alongside (occult) or past (overt) the presenting part in the presence of ruptured membranes (incidence of 0.1% to 0.6%).
- cotyledon - (Greek, kotyle = a deep cup) In the embryos of seed plants, the "seed leaves," in which nutrients are stored for use after germination. In placental animals, the term is also to describe the leaf-like structure of the placenta surface.
- cytotrophoblast - The "cellular" trophoblast layer surrounding (forming a "shell") the early implanting conceptus. Beginning at uterine adplantation, proliferation and fusion of these cells is thought to form a second outer trophoblast layer, the syncytiotrophoblast. The cytotrophoblast layer contributes to formation of the placental villi, the functional component of the fetal placenta.
- decidua basalis - The term given to the uterine endometrium at the site of implantation where signaling transforms the uterine stromal cells (fibroblast-like) into decidual cells. This forms the maternal component of the placenta, the decidualization process gradually spreads through the remainder of the uterus, forming the decidua parietalis.
- decidua basalis reaction - Term describing the maternal endometrial changes that occur initially at the site of, and following, blastocyst implantation. Seen as a deposition of glycogen, fibrin and proliferation of blood vessels. See also decidualization.
- decidua capsularis - The term given to the uterine endometrium which has been converted to decidua surrounding the conceptus on the smooth chorion side.
- decidua parietalis - The term given to the remainder of the uterine endometrium, away from the site of implantation, that gradually becomes comverted to decidua.
- decidual cell - The uterine stromal cells (fibroblast-like) that differentiate in response to both steroid hormones (progesterone) and embryonic signals. These cells then alter uterine environment to support further embryonic development as well as producing cytokines related to prolactin (PRL) and have an innate immune function.
- decidual reaction - maternal endometrial reaction invoked in order to block the rapid extension of the implanting syncytium.
- decidualization - (decidualisation, decidual reaction) The process by which uterine stromal cells differentiate in response to both steroid hormones and embryonic signals into large epitheliod decidual cells. This process is essential for the progress of implantation and establishing fetal-maternal communication.
- DHEA - (dehydroepiandrosterone, androstenolone) precursor of sex steroid hormones and is converted to testosterone and estradiol. Postnatally, an abundant circulating steroid produced in the adrenal gland. The fetal adrenal cortex produces dehydroepiandrosterone sulfate (DHEA-S) used by the placenta to produce estrogens. DHEA, androstenedione, and testosterone can be metabolized to epiandrosterone, and etiocholanolone. PMID 15635500
- fetal drug addiction - occurs when drugs used maternally cross the placental barrier and can establish neural/physiological addiction in the unborn fetus. drugs
- fetal erythroblastosis - (Haemolytic Disease of the Newborn) A clinical term describing an immune response between fetal and maternal blood groups; from fetus Rh+ / maternal Rh-. The leakage of blood from fetus, particularly at birth, causes maternal anti-Rh antibodies, which is then dangerous for a 2nd or future pregnancies.
- fetal intra-abdominal umbilical vein varix - (FIUV, umbilical vein varix) focal dilatation of the umbilical venous diameter at the level of cord insertion, the dilatation diameter increases linearly with gestational age. Represent about 4% of umbilical cord abnormalities
with an incidence of about 2.8 per 1,000 pregnancies, there is also a rarer form of extra-abdominal varices.PMID 24883288
- fibrinoid layer - (Nitabuch's layer) A layer formed at maternal/fetal interface during placentation and is thought to act to prevent excessively deep conceptus implantation. Fibrin-type fibrinoid (maternal blood-clot product) and matrix-type fibrinoid (secreted by invasive extravillous trophoblast cells).
- floating chorionic villi - Term used to describe the placental microanatomy structure of chorionic villi that are not attached to the maternal decidua and float in the maternal blood-filled space (lacunae). Structurally the same as anchoring chorionic villi conceptus side that are attached to the maternal decidua.These villi go through the same stages of development: primary villi - secondary villi - tertiary villi
- hemotrophic nutrition - Term used to describe in late placenta development the transfer of blood-borne nutrition from maternal to embryo/fetuscompared to early histiotrophic nutrition.
- heterotopic pregnancy - (Greek, heteros = other) Clinical term for a very rare pregnancy of two or more embryos, consisting of both a uterine cavity embryo implantation and an ectopic implantation.
- histiotrophic nutrition - Term used to describe in early placenta development the intital transfer of nutrition from maternal to embryo (histiotrophic nutrition) compared to later blood-borne nutrition (hemotrophic nutrition). Histotroph is the nutritional material accumulated in spaces between the maternal and fetal tissues, derived from the maternal endometrium and the uterine glands. This nutritional material is absorbed by phagocytosis initially by blastocyst trophectoderm and then by trophoblast of the placenta. in later placental development nutrition is by the exchange of blood-borne materials between the maternal and fetal circulations, hemotrophic nutrition.
- Hofbauer cells - Cells found within placental villi connective tissue. Have a role as macrophages of mesenchymal origin with potentially additional functions (remodeling, vasculogenesis, regulation of stromal water content).
- Human chorionic corticotropin - (hCACTH) placental derived hormone equivilant to corticotropin (ACTH) from the pituitary.
- Human chorionic gonadotrophin - (hCG) like leutenizing hormone, supports corpus luteum, originally secreted by trophoblast cells.
- Human chorionic somatommotropin - (hCS, placental lactogen) hormone level increases in maternal blood through pregnancy, decreases maternal insulin sensitivity (raising maternal blood glucose levels and decreasing maternal glucose utilization) aiding fetal nutrition.
- Template:Hydatiform mole - A uterine tumour with "grape-like" placenta appearance without enclosed embryo formation, arises mainly from a haploid sperm fertilizing an egg without a female pronucleus. It is one form of gestational trophoblastic disease(GTD), a number of abnormalities including hydatiform mole, invasive mole, choriocarcinoma and placental site trophoblastic tumor (PSTT).
- hysterectomy – clinical term for the surgical removal of the uterus.
- Langhans layer - cytotrophoblast cell layer.
- maternal antibodies - antibodies from the mother's immune system that are capable of crossing placental barrier. They can provide immune protection to the embryo, but may also participate in immune disease (fetal erythroblastosis).
- maternal sinusoids - placental spaces around chorionic villi that are filled with maternal blood. This is the closest maternal/fetal exchange site.
- Nitabuch's layer - (fibrinoid layer) The layer formed at maternal/fetal interface during placentation and is thought to act to prevent excessively deep conceptus implantation. Fibrin-type fibrinoid (maternal blood-clot product) and matrix-type fibrinoid (secreted by invasive extravillous trophoblast cells).
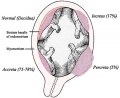
- Morbidly adherent placenta (MAP) A general clinical term used to describe the different forms of abnormal placental implantation (Accreta, Increta and Percreta).
- oligohydramnios - Clinical term for the accumulation a deficiency of amniotic fluid during pregnancy. See also polyhydramnios, an excess of amniotic fluid.
- persistent right umbilical vein - (PRUV) A placental cord abnormality associated with fetal abnormalities and poor neonatal prognosis. The estimated incidence of persistent right umbilical vein in a low-risk population is 1 : 526. PMID 12047534
- polyhydramnios - Clinical term for the accumulation of excess amniotic fluid during pregnancy. See also oligohydramnios, a deficiency of amniotic fluid.
- placenta - (Greek, plakuos = flat cake) The developmental organ formed from maternal and fetal contributions in animals with placental development. In human, the placenta at term is a discoid shape "flat cake" shape; 20 cm diameter, 3 cm thick and weighs 500-600 gm. Placenta are classified by the number of layers between maternal and fetal blood (Haemochorial, Endotheliochorial and Epitheliochorial) and shape (Discoid, Zonary, Cotyledenary and Diffuse). The placenta has many different functions including metabolism, transport and endocrine.
- placenta accreta - The abnormal placental adherence, either in whole or in part of the placenta with absence of decidua basalis, leading to retention as an after-birth to the underlying uterine wall. The incidence of placenta accreta also significantly increases in women with previous cesarean section compared to those without a prior surgical delivery.
- placental arteries - (umbilical arteries) In placental animals, the blood vessels which develop within the placental cord carrying relatively deoxygenated blood from the embryo/fetus to the placenta. In humans, there are two placental arteries continuous with the paired internal iliac arteries (hypogastric arteries) arising off the dorsal aortas. At birth this vessel regresses and form the remnant medial umbilical ligament.
- placental cord - (umbilical cord) The placental cord is the structure connecting the embryo/fetus to the placenta. It is initially extra-embryonic mesoderm forming the connecting stalk within which the placental blood vessels (arteries and veins) form. In human placental cords the placental blood vessels are initially paired, later in development only a single placental vein remains with a pair of placental arteries. This structure also contains the allantois, an extension from the hindgut cloaca then urogenital sinus. Blood collected from the placental cord following delivery is a source of cord blood stem cells.)
- placental diameter - is measured in the transverse section by calculating the maximum dimensions of the chorionic surface.
- placental growth factor - (PlGF) A growth factor of the vascular endothelial growth factor (VEGF) family, released from the placental trophoblast cells and other sources that stimulates blood vessel growth.
- placental malaria - The malarial infection of the placenta by sequestration of the infected red blood cells. This condition can be common in regions where malaria is endemic with women carrying their first pregnancy (primigravida).
- placenta membranacea - rare placental abnormality characterized by the presence of chorionic villi directly attached to and covering the fetal membranes. Placenta Membranacea
- placenta previa - placenta overlies internal os of uterus, abnormal bleeding, may require cesarian delivery.
- placental thickness - is measured at its mid-portion from the chorionic plate to the basilar plate, on a longitudinal plane (less than 4 cm at term). Excludes any abnormalities (fibroids, myometrial contractions, or venous lakes). The placental thickness approximates in millimeters to the weeks of gestation.
- placental vein - (umbilical vein) In placental animals, the blood vessels which develop within the placental cord carrying relatively oxygenated blood from the placenta to the embryo/fetus. In humans, there are initially two placental veins which fuse to form a single vein. The resence of paired veins in the placental cord can be indicative of developmental abnormalities.
- placentophagia - Term used to descrbe the maternal ingestion of afterbirth materials (placental membranes and amniotic fluid) that can occur following mammalian parturition (birth).
- primary villi - (primary chorionic villi) Term describing the earliest stage of embryonic placenta development. In humans, the conceptus during week 2 this first stage of chorionic villi development consists of only the trophoblastic shell cells (syncitiotrophoblasts and cytotrophoblasts) forming finger-like extensions into maternal decidua. Initially these finger-like projections cover the entire surface of chorionic sac and later become restricted to the placental surface. The villi stages are ongoing as the placenta continues to grow through both the embryonic and fetal development.
- pre-eclampsia - During pregnancy a combination of high blood pressure, protein in urine and fluid retention resulting in maternal sudden excessive swelling of the face, hands and feet. Eclampsia is the subsequent development of convulsions, kidney failure, liver failure, clotting problems or mortality.
- Rh alloimmunization - feto-maternal haemorrhage generally in late pregnancy results in an Rh-negative woman becoming sensitised to Rh-positive fetal cells that enter her circulation. Clinically treated with anti-D immune globulin prophylaxis, alloimmunization occurs in 9–10% of at-risk pregnancies. immune
- secondary villi - (secondary chorionic villi) Term describing the second stage of embryonic placenta development. In humans, the conceptus during week 3 onward this stage of chorionic villi development consists of the trophoblastic shell cells (syncytiotrophoblast and cytotrophoblasts) filled with extraembryonic mesoderm forming finger-like extensions into maternal decidua. Initially these finger-like projections cover the entire surface of chorionic sac and later become restricted to the placental surface. The villi stages are ongoing as the placenta continues to grow through both the embryonic and fetal development. Placental villi stages: primary villi - secondary villi - tertiary villi
- syncytiotrophoblast - A multinucleated cell currently thought to form by the fusion of another trophoblast cell the cytotrophoblasts, within the trophoblast layer (shell) of the implanting conceptus. In early development, these cells mediate implantation of the conceptus into the uterine wall and secrete the hormone (Template:Human Chorionic Gonadotrophin, hCG) responsible for feedback maintainance of the corpus luteum (in maternal ovary) and therefore maintaining early pregnancy.
- trophoblast - (trophectoderm, Greek, trophe = "nutrition" and blast = a primordial cell) cells that firstly support adplantation, implantation and endocrine support of pregnancy. Contribute to the extraembryonic tissues, fetal placenta and membranes. Initially form 2 populations individual cytotrophoblast cells and their fused multinucleate syncytiotrophoblast cells.
- Twin-twin transfusion syndrome - (TTTS) in monozygotic twins with monochorionic and diamniotic placenta, with intrauterine blood transfusion from one twin (donor) to another twin (recipient) where there is an imbalance of blood flow from the donor twin to the recipient twin. Clinically diagnosed by the alternate presence of polyhydramnios in one fetus and oligohydramnios in the co-twin, occurs in about 10% of monochorionic twins.
- umbilical cord (placental cord) fetal attachment cord 1-2 cm diameter, 30-90cm long, covered with amniotic attached to chorionic plate, umbilical vessels (artery, vein) branch into chorionic vessels. Vessels anastomose within the placenta.
- umbilical vein varix - (fetal intra-abdominal umbilical vein varix, FIUV) focal dilatation of the umbilical venous diameter at the level of cord insertion, the dilatation diameter increases linearly with gestational age. Represent about 4% of umbilical cord abnormalities
with an incidence of about 2.8 per 1,000 pregnancies, there is also a rarer form of extra-abdominal varices. PMID 24883288
- vasculogenesis - formation of first blood vessels by differentiation of pluripotent mesenchymal cells (extraembryonic mesoderm) followed by angiogenesis which is the development of new vessels from already existing vessels.
- vasculosyncytial membranes - localised areas of the placental villous membrane where the barrier thickness separating maternal and fetal circulations is reduced to as little as 1-2 microns. PMID 1287078
- villi - Plural of villus, which is a thin projection from a surface. The term in development is used to describe the individual functional units together of the fetal placenta.
- virus - small infectious agents that may cross the placental barrier. Can infect embryo and/or placenta and cause developmental abnormalities. (e.g. cytomegalovirus, rubella, measles).
- Wharton's jelly - placental cord (umbilical cord) gelatinous connective tissue composed of myofibroblast-like stromal cells, collagen fibers, and proteoglycans. Increases in volume (myxomatous, connective tissue embedded in mucus) at parturition (birth) to assist closure of placental blood vessels. Matrix cells from Wharton's jelly have recently been identified as a potential source of mesenchymal stem cells (MSC), also called mesenchymal stromal cell. This placental cord substance is named after Thomas Wharton (1614-1673) an English physician and anatomist who first described this placental tissue.
|
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2026, Mayıs 5) Embryology Placenta - Membranes. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Placenta_-_Membranes
- What Links Here?
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G