Placenta - Maternal Decidua
| Embryology - 13 Mar 2026 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
This page gives an overview of aspects of maternal component of placental development, formed initially by the decidualization of the endometrium.
In week 2, the trophoblast shell cells proliferate and form a syncitiotrophoblast and cytotrophoblast layer around the conceptus. Syncitiotrophoblast cells migrate into the uterine wall, forming maternal blood-filled spaces (lacunae).
Decidualization is the process of converting endometrial stromal cells into decidual cells and requires at least 8–10 days of hormone stimulation. A similar "decidual" cellular change, but less significant, also occurs in the uterine lining after ovulation during the secretory phase of the non-pregnant uterus.
- initiated during the mid-secretory phase of the menstrual cycle
- in response to elevated progesterone levels
- acts mainly through progesterone receptor (PR) PR-A (other isoform is PR-B)
Placentation begins once the conceptus begins to implant in the uterine wall and the placenta will have both a fetal and a maternal component.
During pregnancy, both the maternal blood volume increases by about 50% and the uterine blood flow increases 10 to 12 fold. Flow increase is due to the trophoblast cell invasion of the spiral arteries opening them into blood-filled spaces of the placenta.
For the non-pregnant uterus background see Menstrual Cycle and Uterus Development.
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Maternal Decidua | Decidua Basalis |
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
|
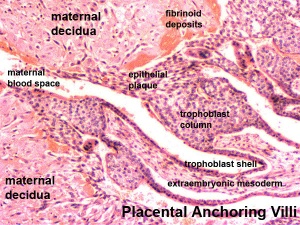
Maternal Decidua
The maternal uterine endometrium stromal cells (fibroblast-like) are transformed by steroid hormones (progesterone) and embryonic signals into the decidua.
The entire maternal decidua is divided into three regions: decidua basalis, decidua capsularis and decidua parietals (decidua vera).
These 3 regions are named by their positional relationship to the conceptus.
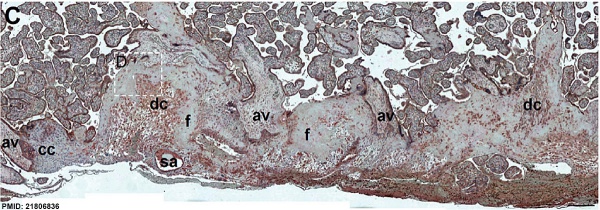
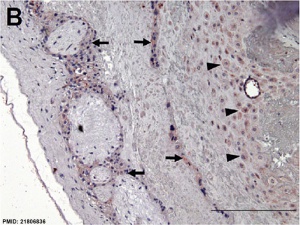
Immunostained placenta and decidua.[7]
SERPINE2 was extensively detected in decidual cells (dc), cytotrophoblasts, extravillous trophoblasts at the junction zone of the cell column (cc) and anchoring villi (av), and the endothelia of the spiral artery (sa); and weak staining was found in fibrinoids (f) and the villous mesenchyme.
Maternal Immune
How does the implanting conceptus avoid immune rejection by the maternal immune system? There are a number of maternal and embryonic mechanisms that are thought to act to prevent immune rejection of the implanting conceptus, though the complete mechanism(s) are unknown. This is particularly relevant to Assisted Reproductive Technology involving donor eggs.
Below are some examples of research on this topic.
Decidual Immune Cells
- Specialised immune cells.
| Decidual Macrophages (Mϕ) | Decidual T cells | Uterine Natural Killer cells |
|---|---|---|
|
|
|
Uterine Natural Killer Cells
See also article on peripheral NK cells. Tim-3 signaling in peripheral NK cells promotes maternal-fetal immune tolerance and alleviates pregnancy loss
Decidual Mast Cells
Immune system mast cells generally occur in two subtypes: (positive, +; negative, -) tryptase+/chymase- and tryptase+/chymase+.
In teh maternal placenta tryptase positive(+) mast cells are present.[8]
- FcεRIα+Kit+tryptase+chymase+ phenotype.
- release histamine following FcεRI aggregation.
A recent study of non-pregnant uterus identified the presence of a third mast cell subtype (tryptase-/chymase+). [9]
Chemokine Gene Silencing
- Remove the attraction of maternal immune cells.
A mouse study[10] has shown that the normal immune response to inflammation, accumulation of effector T cells in response to chemokine secretion does not occur during implantation. This is prevented locally by epigenetic silencing of chemokine expression in the decidual stromal cells.
Corticotropin-Releasing Hormone
- Kill the maternal immune cells.
Both maternal and implanting conceptus release CRH at the embryo implantation site. This hormone then binds to receptors on the surface of trophoblast (extravillous trophoblast) cells leading to expression of a protein (Fas ligand, FasL) that activates the extrinsic cell death pathway on any local maternal immune cells ( T and B lymphocytes, natural killer cells, monocytes and macrophages).[11] (Note - This cannot be the only mechanism, as mice with dysfunctional FasL proteins are still fertile).
Decidualization Factors
There are a number of known molecular signals involved in the conversion of uterine stromal cells into decimal cells.
Preimplantation Factor
- Preimplantation factor (PIF) secreted only by viable embryos.
- a 15 amino acid peptide MVRIKPGSANKPSDD
- regulates immunity, promoting embryo-decidual adhesion, and regulating adaptive apoptotic processes.[12]
Activin A
Member of the a transforming growth factor beta (TGFbeta) superfamily, contributes to human endometrial stromal cells (HESC) decidualization and has been localized to decidual cells in the human endometrium. (possibly also BMP2 and TGFbeta1)[13]
Prokineticin 1
Prokineticin 1 (PROK1) signalling via prokineticin receptor 1 (PROKR1) regulates Dickkopf 1 (DKK1) expression, a negative regulator of canonical Wnt signaling.[14]
Macrophage Inhibitory Cytokine
Macrophage inhibitory cytokine (MIC-1) or Growth/Differentiation Factor 15 (GDF15) or Bone Morphogenetic Protein, Placenta (PLAB)
Inhibits trophoblast invasion by blocking activation of MMP-2 and -9, as well as stimulating apoptosis.
OMIM: MIC-1
References
- ↑ Pollheimer J, Vondra S, Baltayeva J, Beristain AG & Knöfler M. (2018). Regulation of Placental Extravillous Trophoblasts by the Maternal Uterine Environment. Front Immunol , 9, 2597. PMID: 30483261 DOI.
- ↑ Jiang X, Du MR, Li M & Wang H. (2018). Three macrophage subsets are identified in the uterus during early human pregnancy. Cell. Mol. Immunol. , 15, 1027-1037. PMID: 29618777 DOI.
- ↑ Aplin JD, Beristain A, DaSilva-Arnold S, Dunk C, Duzyj C, Golos TG, Kemmerling U, Knöfler M, Mitchell MD, Olson DM, Petroff M, Pollheimer J, Reyes L, Schedin P, Soares MJ, Stencel-Baerenwald J, Thornburg KL & Lash GE. (2017). IFPA meeting 2016 workshop report III: Decidua-trophoblast interactions; trophoblast implantation and invasion; immunology at the maternal-fetal interface; placental inflammation. Placenta , 60 Suppl 1, S15-S19. PMID: 28456431 DOI.
- ↑ Liu JL & Wang TS. (2015). Systematic Analysis of the Molecular Mechanism Underlying Decidualization Using a Text Mining Approach. PLoS ONE , 10, e0134585. PMID: 26222155 DOI.
- ↑ Lima PD, Zhang J, Dunk C, Lye SJ & Croy BA. (2014). Leukocyte driven-decidual angiogenesis in early pregnancy. Cell. Mol. Immunol. , 11, 522-37. PMID: 25066422 DOI.
- ↑ Salker MS, Nautiyal J, Steel JH, Webster Z, Sućurović S, Nicou M, Singh Y, Lucas ES, Murakami K, Chan YW, James S, Abdallah Y, Christian M, Croy BA, Mulac-Jericevic B, Quenby S & Brosens JJ. (2012). Disordered IL-33/ST2 activation in decidualizing stromal cells prolongs uterine receptivity in women with recurrent pregnancy loss. PLoS ONE , 7, e52252. PMID: 23300625 DOI.
- ↑ 7.0 7.1 Chern SR, Li SH, Chiu CL, Chang HH, Chen CP & Tsuen Chen EI. (2011). Spatiotemporal expression of SERPINE2 in the human placenta and its role in extravillous trophoblast migration and invasion. Reprod. Biol. Endocrinol. , 9, 106. PMID: 21806836 DOI.
- ↑ Matsuno T, Toyoshima S, Sakamoto-Sasaki T, Kashiwakura JI, Matsuda A, Watanabe Y, Azuma H, Kawana K, Yamamoto T & Okayama Y. (2018). Characterization of human decidual mast cells and establishment of a culture system. Allergol Int , , . PMID: 29784282 DOI.
- ↑ De Leo B, Esnal-Zufiaurre A, Collins F, Critchley HOD & Saunders PTK. (2017). Immunoprofiling of human uterine mast cells identifies three phenotypes and expression of ERβ and glucocorticoid receptor. F1000Res , 6, 667. PMID: 28620462 DOI.
- ↑ Nancy P, Tagliani E, Tay CS, Asp P, Levy DE & Erlebacher A. (2012). Chemokine gene silencing in decidual stromal cells limits T cell access to the maternal-fetal interface. Science , 336, 1317-21. PMID: 22679098 DOI.
- ↑ Makrigiannakis A, Zoumakis E, Kalantaridou S, Coutifaris C, Margioris AN, Coukos G, Rice KC, Gravanis A & Chrousos GP. (2001). Corticotropin-releasing hormone promotes blastocyst implantation and early maternal tolerance. Nat. Immunol. , 2, 1018-24. PMID: 11590404 DOI.
- ↑ Paidas MJ, Krikun G, Huang SJ, Jones R, Romano M, Annunziato J & Barnea ER. (2010). A genomic and proteomic investigation of the impact of preimplantation factor on human decidual cells. Am. J. Obstet. Gynecol. , 202, 459.e1-8. PMID: 20452489 DOI.
- ↑ Stoikos CJ, Harrison CA, Salamonsen LA & Dimitriadis E. (2008). A distinct cohort of the TGFbeta superfamily members expressed in human endometrium regulate decidualization. Hum. Reprod. , 23, 1447-56. PMID: 18434375 DOI.
- ↑ <pubmed>21546446</pubmed>
Reviews
Articles
{{#pmid:27219485]]
Plaisier M. (2011). Decidualisation and angiogenesis. Best Pract Res Clin Obstet Gynaecol , 25, 259-71. PMID: 21144801 DOI.
Search PubMed
Search Pubmed: Maternal Decidua | Decidualization
Terms
| Placenta Terms (expand to view) |
|---|
with an incidence of about 2.8 per 1,000 pregnancies, there is also a rarer form of extra-abdominal varices.PMID 24883288
with an incidence of about 2.8 per 1,000 pregnancies, there is also a rarer form of extra-abdominal varices. PMID 24883288
|
| Other Terms Lists |
|---|
| Terms Lists: ART | Birth | Bone | Cardiovascular | Cell Division | Endocrine | Gastrointestinal | Genital | Genetic | Head | Hearing | Heart | Immune | Integumentary | Neonatal | Neural | Oocyte | Palate | Placenta | Radiation | Renal | Respiratory | Spermatozoa | Statistics | Tooth | Ultrasound | Vision | Historic | Drugs | Glossary |
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2026, March 13) Embryology Placenta - Maternal Decidua. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Placenta_-_Maternal_Decidua
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G