User:Z3516832
| Student Information (expand to read) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Individual Assessments | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
Please leave this template on top of your student page as I will add your assessment items here. Beginning your online work - Working Online in this course
Click here to email Dr Mark Hill | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lab 1 Assessment - Researching a Topic | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
In the lab I showed you how to find the PubMed reference database and search it using a topic word. Lab 1 assessment will be for you to use this to find a research reference on "fertilization" and write a brief summary of the main finding of the paper.
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lab 2 Assessment - Uploading an Image | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
OK you are now in a group
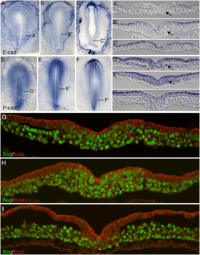
Initially the topic can be as specific or as broad as you want. Chicken embryo E-cad and P-cad gastrulation[1] References
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lab 4 Assessment - GIT Quiz | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
ANAT2341 Quiz Example | Category:Quiz | ANAT2341 Student 2015 Quiz Questions | Design 4 quiz questions based upon gastrointestinal tract. Add the quiz to your own page under Lab 4 assessment and provide a sub-sub-heading on the topic of the quiz. An example is shown below (open this page in view code or edit mode). Note that it is not just how you ask the question, but also how you explain the correct answer. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lab 5 Assessment - Course Review | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Complete the course review questionnaire and add the fact you have completed to your student page. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lab 6 Assessment - Cleft Lip and Palate | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lab 7 Assessment - Muscular Dystrophy | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lab 8 Assessment - Quiz | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| A brief quiz was held in the practical class on urogenital development. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lab 9 Assessment - Peer Assessment | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lab 10 Assessment - Stem Cells | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
As part of the assessment for this course, you will give a 15 minutes journal club presentation in Lab 10. For this you will in your current student group discuss a recent (published after 2011) original research article (not a review!) on stem cell biology or technology.
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lab 11 Assessment - Heart Development | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Read the following recent review article on heart repair and from the reference list identify a cited research article and write a brief summary of the paper's main findings. Then describe how the original research result was used in the review article.
<pubmed>26932668</pubmed>Development | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Lab Attendance
Z3516832 (talk) 14:34, 5 August 2016 (AEST)
Z3516832 (talk) 14:24, 26 August 2016 (AEST)
Z3516832 (talk) 13:46, 2 September 2016 (AEST)
New Subheading
https://embryology.med.unsw.edu.au/embryology/index.php/ANAT2341_Lab_1
PMID 27486480
embryology marsupial embryology
Lab 1 Assessment
To do 5 August, due 12 August 2016
Review of a publication on human fertilisation
<pubmed>26995337</pubmed>
Write a short summary of the papers main findings
During development, all vertebrate embryos pass through the somite stage, which is defined as any developmental stage between the formation of the first and last pairs of somites in embryos (Gilbert, 2003; Mu€ller and O’Rahilly, 2003). The somite stages can vary and is not very accurate, but correspond to CS9-CS13 and occur approximately during the third and fourth weeks after fertilization of the ovum.
This study uses 37 human embryos (already fertilized) that were obtained when pregnancy was terminated during the first trimester due to socioecomomic reasons and form part of the Kyoto Collection in Japan. These embryos are classified following the Carnegie Stage (CS) 11-CS13 which is approximately 28-33 days after fertilization. These embryos were selected due to their good conditions, they were undamaged, and then were measured and examined using the criteria provided by O’Rahilly and Mueller (1987).
The embryos were then subjected to histological serial sectioning. The historical sections were scanned digitally and the morphology and the following primordia were histologically observed: the epithelium and mesenchyme of thyroid, the epithelium around the respiratory primordium region, omental bursa, ventral pancreas, and liver parenchyma. The morphology that was observed in the 2D histological slides was reconstructed in 3D. With the 3D reconstructions, the authors were able to create a precise timeline of the differentiation events that occur during this developmental time and provided key insights into these developmental processes. Using 3D reconstructions the authors were also able to observe the precise mechanisms involved during the digestive tract development during the particular somite stages. For example with the digestive tract and derived primordial, the authors were able to observe the morphology and position of the tract within the body and construct a precise time line during which development occurs. This differs from previous morphometrical studies (e.g. O’Rahilly and Mu€ller, 1984b; Otani et al., 2008) which showed that the size and proportion of the digestive tract and organ primordial varied considerably among embryos at the same stage.
| Mark Hill 18 August 2016 - You have added the citation correctly and written a good brief summary of the article findings. The problem is the paper does not relate to fertilisation, that was the topic for this exercise.
|
Assessment 2/5 |
Lab 2 Assessment
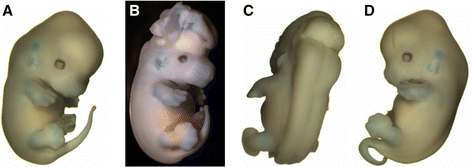
Dietary folic acid supplementation in mouse NTD models[1]
| Mark Hill 29 August 2016 - All information Reference, Copyright and Student Image template correctly included with the file and referenced on your page here. I have also added a References sub-heading so your citation list appears.
This is the citation link you should use here on your page: <ref name="PMID25154628"><pubmed>25154628</pubmed></ref> |
Assessment 5/5 |
Lab 3 Assessment
| Mark Hill 31 August 2016 - Lab 3 Assessment Quiz - Mesoderm and Ectoderm development. | Assessment 3/5 |
References
- ↑ <pubmed>25154628</pubmed>
Lab 4 Assessment
Gastrulation Development quiz
Lab 6 Assessment
Individual Assessment
Identify a known genetic mutation that is associated with cleft lip or palate.
MSX1 also known as the muscle segment homeobox (MSX1) gene plays a crucial role in epithelial-mesenchymal tissue interactions in craniofacial development
Identify a recent research article on this gene.
PMID 27259221 This recent research article by Paradowska-Stolarz [1] gives a small introduction on cleft palate deformities. The author states that cleft deformities are the most common facial malformations and observed in 10% of facial deformities. The cleft lip and/or palate is served in 1:700 live births. But we the reader do not know if this is a world wide phenomenon or occurs only in Poland. Males are two to three times more likely to have Clefts in the lip, alveolar bone and palate while in females isolated cleft of the palate is more frequent. Facial clefts are formed within 5 to 12 weeks during fetal development. It is still not known what is the full ethology of the cleft lip and/or palate however there is a large genetic factor that contributes to this deformity and there are a number of genes that are known to be involved in the palate formation. The author also states that there also may be a environmental trigger that also causes these facial malformations. The author states that 20% of cleft palate malformations are caused by the following genes: genes encoding signalling molecules (Bmp2, Bmp4, Bmp7, Shh, Wnt5a, Smad 2-4), growth factors (Egf, Egfr, Fgf1, Fgf2, Fgf8, Tgfα, Tgfβ1-3) and their receptors (Fgfr1, Fgfr2), transcription factors (Pax9, Tbx22, Msx1, Tbx1, Ap2α, Blx1-6, Lhx6, Gli 2-3, Hoxa2, Irf6, Pitx1, Pitx2, Prx1), cellular adhesion molecules (Pvrl1, cadherin E, connexin 43), and extra- cellular matrix ( bronexin, Col 1A2, Col2A1, Col11A1 Mmp2, Mmp3, Mmp9, Mmp13, Timp1-3) [46,49]. As well as these MSX1 and TGFβ3 genes are found to be the genes more strongly related to cleft palate anomalies.
Does this mutation affect developmental signalling in normal development?
References
- ↑ <pubmed>27259221</pubmed>
Lab 7 Assessment
Duchenne muscular dystrophy
PMID 27594988
Duchenne muscular dystrophy (DMD) is a recessive inherited muscular dystrophy that is caused by mutations in the gene that encodes dystrophin on the x chromosome. Dystrophin is a protein which is needed to keep muscle fiber integrity. This dystrophy is caused by mutations in the gene encoding dystrophin, a protein required for muscle fiber integrity. The DMD gene is expressed mainly in skeletal and cardiac muscle [1] . Many approaches have been tested from traditional gene addition to newer approaches which are based on cell manipulations at either gene transcription level, mRNA processing or at translation levels. Currently there are no efficient treatments to treat DMD.
Who is affected by DMD
DMD affects approximately 1 in 3500 live male births throughout the world. Due to the way that it is inherited, DMD affects mostly boys, but occasionally girls are affected. It is inherited as an x-linked disease that is characterized by a rapidly progressive muscle weakness.
DMD affects all ethnicities, nationalities and socioeconomic groups, although it occurs almost exclusively in males. Children with DMD show early signs of muscle weakness and begin walking relatively late in childhood. They develop a waddling gait and have difficulty in climbing stairs. Their muscles show a false or pseudo-hypertrophy, most notably in the calf muscles, where the muscles appear large but are actually replaced by fat or fibrous tissue.
Becker muscular dystrophy (BMD) results from mutations in the same gene as DMD but follows a milder clinical course, with later development of weakness and loss of function.
Medical Treatment of DMD The most advanced treatments include therapeutic treatments.Steroid treatment (also called glucocorticoids or corticosteroids) has been proven to slow the loss of muscle function and therefore temporarily prolong a boy’s mobility. On average boys taking steroids are able to walk for three years longer and the onset of breathing and heart problems and curvature of the spine may also be delayed. Since steroid treatment was introduced more than 20 years ago the life expectancy of individuals with DMD has increased considerably, but it is not known if this is due to the steroids or the introduction of other measures to manage the condition such as ventilation.
Mouse models for DMD
The mouse model is mdx mouse. A dystrophin deficient mutant was first described in 1984 as a naturally occuring deficient mutant and was described in a colony of C57BL/10 mice (C57BL/10ScSnJ) and has since been referred to as the “mdx-mouse”.
How is Duchenne diagnosed?
Duchenne is diagnosed in boys between the ages of 3 and 7. Parents noticed that their son is not at the same stage physcially as their peers and behind in developmental milestones. Young boys may appear to be clumsy and will often fall down during regular activity. Climbing stairs, running, and rising up from the floor become very difficult.
There is an online interactive tool that can help parents detect motor development delays - http://motordelay.aap.org/
Once Duchenne is suspected from the symptoms, there is a range of tests that can be done by a doctor to reach a diagnosis, which are listed below.
Creatine Kinase
The muscles contain an enzyme called creatine kinase (CK), and when muscles are damaged, this enzyme spills out into the bloodstream. Measuring CK levels in the blood verifies that there has been muscle damage, but does not give a definite diagnosis.
DNA testing
DNA is obtained from a blood sample and scientists are able to examine the dystrophin gene to find out exactly where the mutation has occurred.
Muscle biopsy
If DNA testing does not give a clear diagnosis a muscle biopsy may be needed. A surgeon removes a small sample of muscle and it is examined under a microscope to see if dystrophin protein is present.
References
- ↑ <pubmed>27594988</pubmed>