Placenta - Cord
| Embryology - 28 May 2026 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
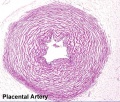
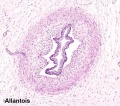
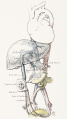
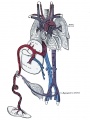
The placenta (Greek, plakuos = flat cake) named on the basis of this organs appearance. The placental cord (umbilical cord) is the connecting region between the functional placenta and the embryo/fetal umbilical region. The human cord varies greatly in overall length increasing to about 60 to 70 cm at term. This extra-embryonic structure contains the main placental blood vessels (one vein and two arteries), the yolk stalk (omphalomesenteric duct), and the allantois.
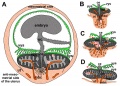
There are essentially 3 separate aortic/venous circulatory systems: umbilical, systemic and vitelline. In the human cord, only the left placental (umbilical) vein persists, while the right placental (umbilical) vein degenerates. The initial segment of the cord at the "umbilicus" also contains the mid-gut herniation, present during the embryonic period of development.
The umbilical system is lost at birth, the vitelline contributes to the portal system and the systemic (embryonic) is extensively remodelled to form the cardiovascular system.
Some Recent Findings

|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Placental Cord | Umbilical Cord | Placental Artery | Placental Vein | Hofbauer cell | single umbilical artery | Persistent right umbilical vein |
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
|
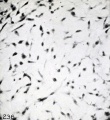
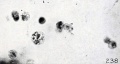
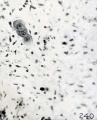
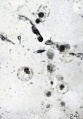
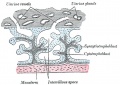
Hofbauer Cells

Hofbauer Cells (red asterisks)[4] |
|
| Historic Embryology - Hofbauer Cells | ||
|---|---|---|
Chapter 14. Hofbauer Cells in Normal and Pathologic Conceptuses Contributions to Embryology Carnegie Institution No.56 (1921)
|
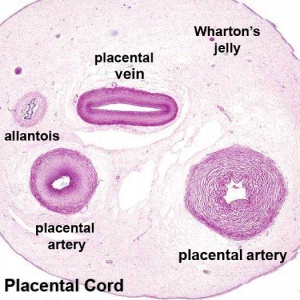
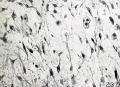
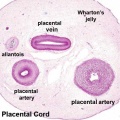
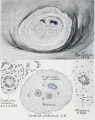
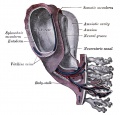
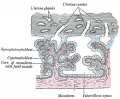
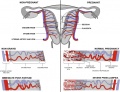
Wharton's Jelly
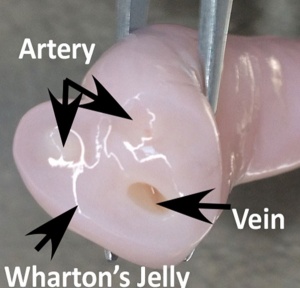
Placental cord cross-section showing Wharton's Jelly |
First described and named after Thomas Wharton (1614–1673) an English physician and anatomist.
|
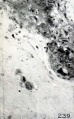
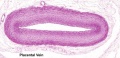
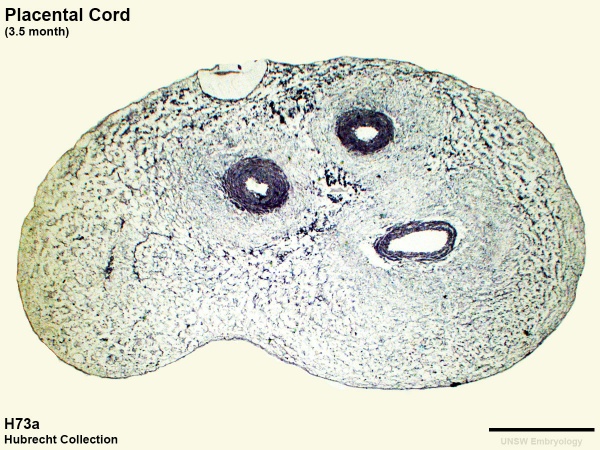
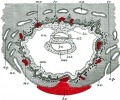
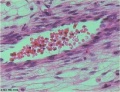
Placental Cord Histology
Human placental cord (3.5 month) cross-section.
Cord Length
The following are lengths and classifications at term.
- Normal range - 50 to 60 cm.
- Short cord - less than 35 cm.
- Long cords - over 70 cm can be associated with wrapping around the fetus and other abnormalities.[5]
Cord Coiling
A recent review of the published literature on cord coiling[6] states: "Previous studies that draw a link between abnormal cord coiling and clinical outcome are generally too small and/or selective to allow meaningful conclusions or applicability to low-risk populations."
The following suggested associations[7] should therefore be reconsidered.
- Hypocoiling - associated with increased incidence of fetal demise, intrapartum fetal heart rate decelerations, operative delivery for fetal distress, anatomic-karyotypic abnormalities and chorio-amnionitis.
- Hypercoiling - associated with increased incidence of fetal growth restriction, intrapartum fetal heart rate decelerations, vascular thrombosis and cord stenosis.
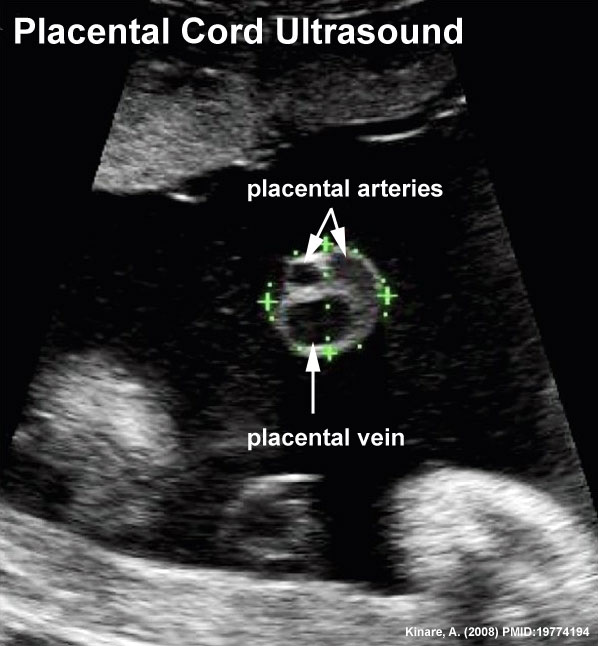
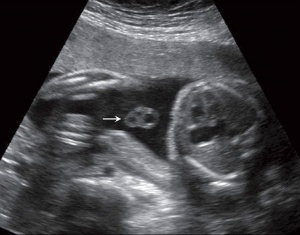
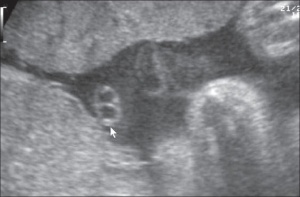
Placental Cord Ultrasound
There are a number of analyses that can be made by ultrasound scanning of the fetal placental cord. Some detected abnormalities (blood vessel number, blood flow[8]) have been associated with adverse developmental outcomes.
- Quantification of cord length, diameter, structural abnormalities.
- Quantification of placental blood vessel number and size.
- Quantification of uterine artery blood flow (doppler analysis).
Ultrasound image of transverse scan through the cord show the method of estimation of the cross-sectional area.
Cord Abnormalities
Cord Vessel Number
Persistent Right Umbilical Vein
Persistent right umbilical vein (PRUV) is a fairly rare anomaly, that can be diagnosed using a transverse section of the fetal abdomen or by three-dimensional ultrasound. A study of 15,237 obstetric ultrasound examinations performed after 15 weeks' gestation identified only 33 cases.[9] While a recent Australian study[10] in their population was 12/2360 = 0.5%, and was also higher than in other retrospective studies.
Some studies have identified associated fetal anomalies with this condition[11], including Template:Cardiac abnormalities.[12]
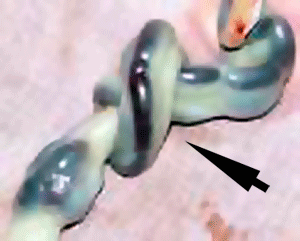
Cord Knotting
There are few abnormalities associated with umbilical cord development, other that abnormally short or long cords, which in most cases do not cause difficulties.
In some cases though, long cords can wrap around limbs or the fetus neck, which can then restrict blood flow or lead to tissue or nerve damage, and therefore effect develoment.
Cord knotting can also occur (1%) in most cases these knots have no effect, in some cases of severe knotting this can prevents the passage of placental blood.
Umbilical Cord Torsion
Rare umbilical cord torsion, even without knot formation can also affect placental blood flow, even leading to fetal demise.[13]
Fetal Umbilical Vein Varix
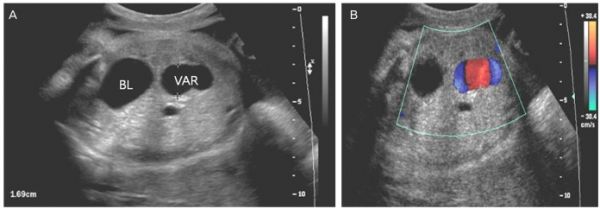
Fetal intra-abdominal umbilical vein varix (FIUV, umbilical vein varix) is a focal dilatation of the umbilical venous diameter at the level of cord insertion. The dilatation diameter has been shown to increase linearly with gestational age. Represent about 4% of umbilical cord abnormalities with an incidence of about 2.8 per 1,000 pregnancies.[14] There is also a rarer form of extra-abdominal varices, where the focal dilatation lies outside the fetal body wall.[15]
| |
| (A) Ultrasound transverse view of the lower fetal abdomen | (B) Color Doppler |
|---|---|
| Showing an umbilical vein varix that was approximately 16.9 mm at 33 weeks of gestation. | Shows some turbulence in the intravascular area and differentiates from other cystic lesions. BL, bladder; VAR, fetal umbilical vein varix. |
Cord Length
References
- ↑ Kim JH, Jin ZW, Murakami G, Chai OH & Rodríguez-Vázquez JF. (2018). Persistent right umbilical vein: a study using serial sections of human embryos and fetuses. Anat Cell Biol , 51, 218-222. PMID: 30310717 DOI.
- ↑ Yamaguchi M, Ohba T, Tashiro H, Yamada G & Katabuchi H. (2013). Human chorionic gonadotropin induces human macrophages to form intracytoplasmic vacuoles mimicking Hofbauer cells in human chorionic villi. Cells Tissues Organs (Print) , 197, 127-35. PMID: 23128164 DOI.
- ↑ Seval Y, Korgun ET & Demir R. (2007). Hofbauer cells in early human placenta: possible implications in vasculogenesis and angiogenesis. Placenta , 28, 841-5. PMID: 17350092 DOI.
- ↑ Lorenzi T, Turi A, Lorenzi M, Paolinelli F, Mancioli F, La Sala L, Morroni M, Ciarmela P, Mantovani A, Tranquilli AL, Castellucci M & Marzioni D. (2012). Placental expression of CD100, CD72 and CD45 is dysregulated in human miscarriage. PLoS ONE , 7, e35232. PMID: 22606231 DOI.
- ↑ <pubmed>11178630</pubmed>
- ↑ Jessop FA, Lees CC, Pathak S, Hook CE & Sebire NJ. (2014). Umbilical cord coiling: clinical outcomes in an unselected population and systematic review. Virchows Arch. , 464, 105-12. PMID: 24259031 DOI.
- ↑ de Laat MW, Franx A, van Alderen ED, Nikkels PG & Visser GH. (2005). The umbilical coiling index, a review of the literature. J. Matern. Fetal. Neonatal. Med. , 17, 93-100. PMID: 16076615 DOI.
- ↑ Shwarzman P, Waintraub AY, Frieger M, Bashiri A, Mazor M & Hershkovitz R. (2013). Third-trimester abnormal uterine artery Doppler findings are associated with adverse pregnancy outcomes. J Ultrasound Med , 32, 2107-13. PMID: 24277892 DOI.
- ↑ Hill LM, Mills A, Peterson C & Boyles D. (1994). Persistent right umbilical vein: sonographic detection and subsequent neonatal outcome. Obstet Gynecol , 84, 923-5. PMID: 7970470
- ↑ Krzyżanowski A, Swatowski D, Gęca T, Kwiatek M, Stupak A, Woźniak S & Kwaśniewska A. (2019). Prenatal diagnosis of persistent right umbilical vein - Incidence and clinical impact. A prospective study. Aust N Z J Obstet Gynaecol , 59, 77-81. PMID: 29498037 DOI.
- ↑ Weichert J, Hartge D, Germer U, Axt-Fliedner R & Gembruch U. (2011). Persistent right umbilical vein: a prenatal condition worth mentioning?. Ultrasound Obstet Gynecol , 37, 543-8. PMID: 20922781 DOI.
- ↑ Lide B, Lindsley W, Foster MJ, Hale R & Haeri S. (2016). Intrahepatic Persistent Right Umbilical Vein and Associated Outcomes: A Systematic Review of the Literature. J Ultrasound Med , 35, 1-5. PMID: 26635256 DOI.
- ↑ Hallak M, Pryde PG, Qureshi F, Johnson MP, Jacques SM & Evans MI. (1994). Constriction of the umbilical cord leading to fetal death. A report of three cases. J Reprod Med , 39, 561-5. PMID: 7966052
- ↑ 14.0 14.1 Lee SW, Kim MY, Kim JE, Chung JH, Lee HJ & Yoon JY. (2014). Clinical characteristics and outcomes of antenatal fetal intra-abdominal umbilical vein varix detection. Obstet Gynecol Sci , 57, 181-6. PMID: 24883288 DOI.
- ↑ Cassidy-Vu L, Clark S & Cuka N. (2019). Extra-abdominal umbilical vein varix in a newborn. BMJ Case Rep , 12, . PMID: 31061189 DOI.
Reviews
Krzyżanowski A, Swatowski D, Gęca T, Kwiatek M, Stupak A, Woźniak S & Kwaśniewska A. (2019). Prenatal diagnosis of persistent right umbilical vein - Incidence and clinical impact. A prospective study. Aust N Z J Obstet Gynaecol , 59, 77-81. PMID: 29498037 DOI.
Articles
Search PubMed
May 2010 search "Placental Cord Development]" All (650) Review (91) Free Full Text (119)
Search Pubmed: Placental Cord | Umbilical Cord | Placental Cord Development | Umbilical Cord Development | Hofbauer cells
Additional Images
see all online Placental materials
Historic
| Historic Disclaimer - information about historic embryology pages |
|---|
| Pages where the terms "Historic" (textbooks, papers, people, recommendations) appear on this site, and sections within pages where this disclaimer appears, indicate that the content and scientific understanding are specific to the time of publication. This means that while some scientific descriptions are still accurate, the terminology and interpretation of the developmental mechanisms reflect the understanding at the time of original publication and those of the preceding periods, these terms, interpretations and recommendations may not reflect our current scientific understanding. (More? Embryology History | Historic Embryology Papers) |
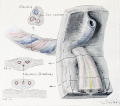
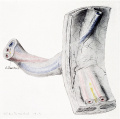
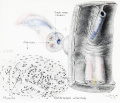
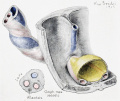
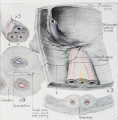
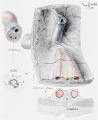
Cullen TS. Embryology, anatomy, and diseases of the umbilicus together with diseases of the urachus. (1916) W. B. Saunders Company, Philadelphia And London. Chapter I. Embryology of the Umbilical Region
- Cross-section of the Cord
- Cullen1916 fig24.jpg
Fig. 24 Embryo 15.0 cm
| Placenta Terms (expand to view) |
|---|
with an incidence of about 2.8 per 1,000 pregnancies, there is also a rarer form of extra-abdominal varices.PMID 24883288
with an incidence of about 2.8 per 1,000 pregnancies, there is also a rarer form of extra-abdominal varices. PMID 24883288
|
| Other Terms Lists |
|---|
| Terms Lists: ART | Birth | Bone | Cardiovascular | Cell Division | Endocrine | Gastrointestinal | Genital | Genetic | Head | Hearing | Heart | Immune | Integumentary | Neonatal | Neural | Oocyte | Palate | Placenta | Radiation | Renal | Respiratory | Spermatozoa | Statistics | Tooth | Ultrasound | Vision | Historic | Drugs | Glossary |
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2026, Mayıs 28) Embryology Placenta - Cord. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Placenta_-_Cord
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G