ANAT2341 Lab 2 - Week 2
| ANAT2341 Lab 2: Introduction | Fertilization | Week 1 | Week 2 | Online Assessment | Group Project |
Introduction
Hatching leaves the blastocyst now free of the zona pellucida and should have occured approximately at the end of the uterine tube or in the body of the uterus. It is now floating in the uterine glands rich mucus secretion and able to directly access this nutrition for continued growth. Note that all cells produced from the initial fertilization event are defined as the "conceptus" and will include cells with both embryonic and extraembryonic futures. In the conceptus, this is a period of blastocyst "hatching" rapid blastocyst differentiation into extraembryonic and embryonic tissues and proliferation. In placental animals, this is the first physical interaction between the conceptus and the maternal uterine wall with adplantation and the commencement of implantaion.
The blastocyst initially weakly adheres to the endometrial wall rolling across its surface. Increased adhesion may lead to attachment, adplantation, on the inner cell mass side of the blastocyst. This will be the site where implantation will begin and the placenta will develop. In humans, receptivity for implantation occurs about 6 days after the post-ovulatory progesterone surge and lasts about 2 to 4 days.
Trophoblast cells at the site of adplantation proliferate and form an additional layer the syncitiotrophoblast layer. This layer of cells rapidly divide, secrete enzymes that degrade the endometrial extracellular matrix and secrete human Chorionic Gonadotropin (hCG).
Implantation Dynamics
The uterine epithelium (white cells) are invaded by the trophoblast cells (green, syncitiotrophoblasts) with the inner cell mass now having 2 layers: an epiblast (blue) and hypoblast (yellow). The blastoceol is covered in cytotrophoblast cells (green).
Later in the movie the amniotic cavity forms adjacent to the epiblast layer(blue) and spaces in the syncitiotrophoblast layer are filled with maternal blood, lacunae.
| <html5media height="580" width="500">File:Week2_001.mp4</html5media> |
This animation shows the process of implantation, occurring during week 2 of development in humans. The beginning of the animation shows: the uterus lining (endometrium epithelium), the hatched blastocyst with a flat outer layer of trophoblast cells (green), the inner cell mass which has formed into the bilaminar embryo (epiblast and hypoblast) and the large fluid-filled space (blastocoel). green cells - trophoblast layer of the conceptus blue cells - epiblast layer of the bilaminar embryo yellow cells - hypoblast layer of the bilaminar embryo white cells - uterine endometrium epithelium red - maternal blood vessel
|
Carnegie Stage 4
This stage represents the beginning of implantation. The blastocyst initially attached to the uterine endometrium (adplantation), syncitiotrophoblasts then secrete enzymes that digest extracellular matrix, allowing the blastocyst to sink into the uterine wall, eventually being completely enclosed within the uterine wall. Note the majority of growth occurs in the trophoblastic shell. The inner cell mass divides initially into 2 layers; epiblast and hypoblast (bilaminar embryo). Hypoblast cells migrate around the original blastoceol cavity forming the primary yolk sac. A second cavity (amniotic) forms between the inner cell mass and the cytotrophoblast shell; this cavity is lined by epiblast cells.
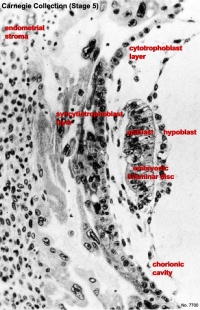
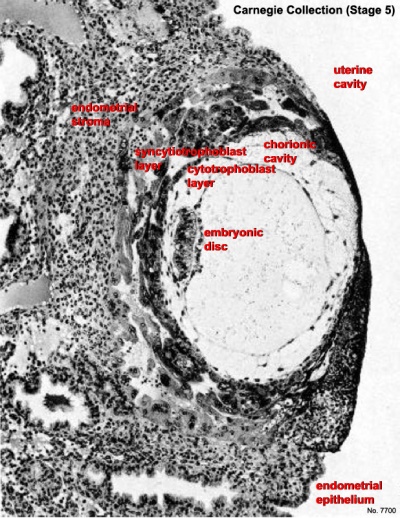
Carnegie Stage 5
|
Facts: Week 1 - 2, size 0.1 - 0.2 mm
Features: implantation completed, inner cell mass, bilaminar embryo, trophoblast development.
|
- Carnegie Stages: 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | 17 | 18 | 19 | 20 | 21 | 22 | 23 | About Stages | Timeline
| <html5media height="580" width="500">File:Chorion 001.mp4</html5media> |
Animation (left) shows the events following implantation and focuses on changes in the the spaces surrounding the embryonic disc, the extraembryonic coelom. The blastoceol cavity is converted into two separate spaces: the yolk sac and the chorionic cavity. The third space lies above the epiblast, the amniotic cavity.
|
|
| Quicktime movie |
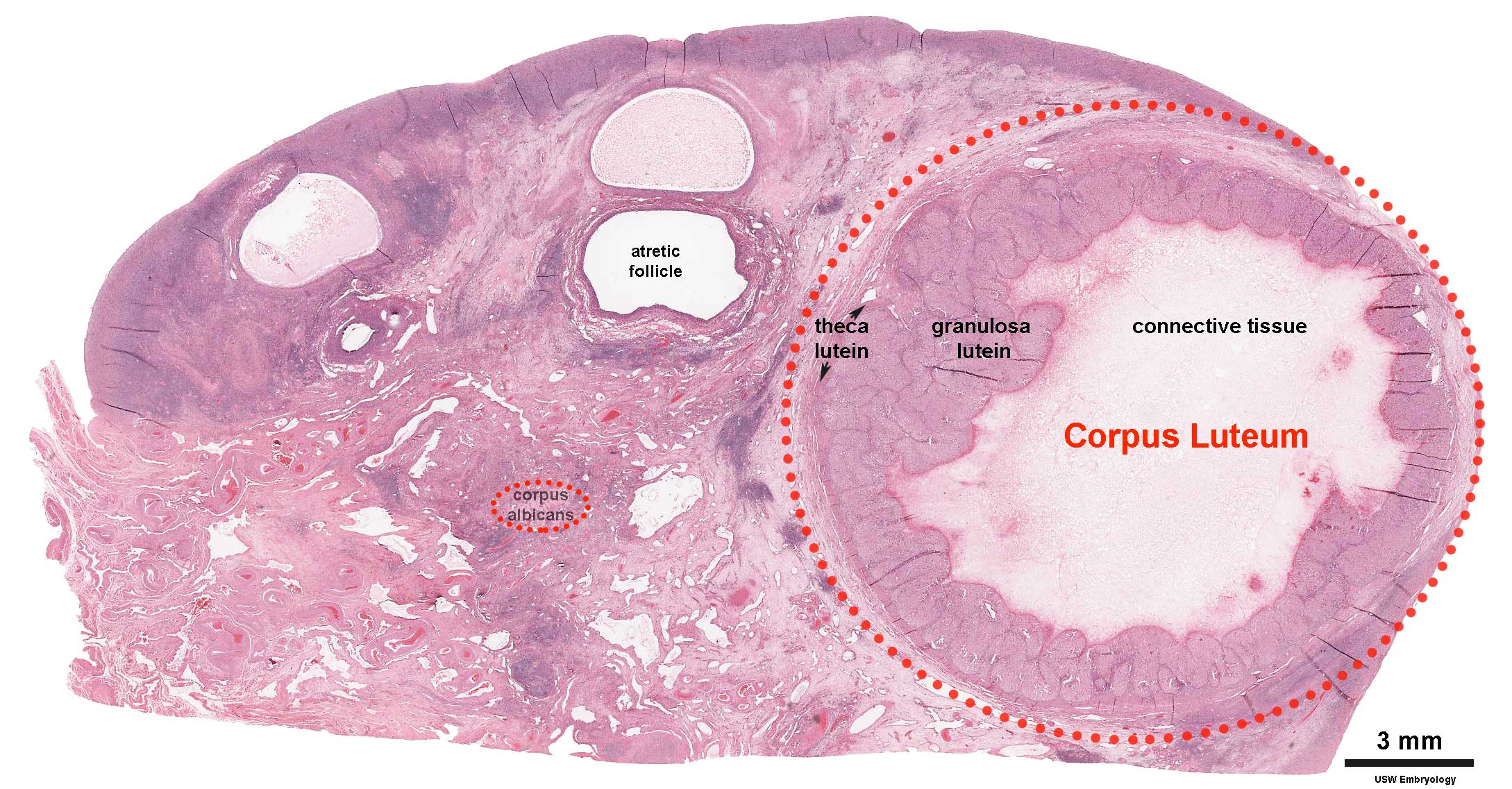
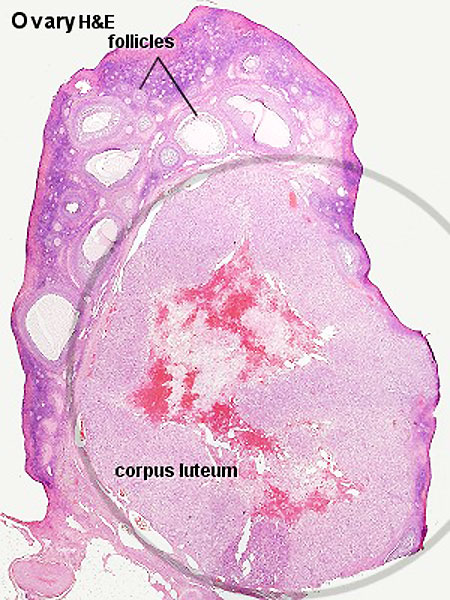
Corpus Luteum
An endocrine signal (hCG human Chorionic Gonadotropin) secreted from the implanting conceptus syncitiotrophoblast cells maintains the ovarian corpus luteum, which in turn provides hormonal support to the uterine functional lining, preventing menstruation. The corpus luteum is formed during the luteal phase (secretory phase) of the menstrual cycle by proliferation of both follicular granulosa cells (granulosa lutein cells) and thecal cells (theca lutein cells), which produce progesterone and oestrogens.
Following ovulation
- If implantation does not occur (non-pregnant), the remnant of the ovulating follicle will degenerate forming a corpus albicans.
- If implantation occurs (pregnancy), the remnant of the ovulating follicle will be maintained forming a corpus luteum.
If implantation does not begin until very late in the current menstrual cycle, or not at all, then that cycle will continue with loss of both the functional layer and the conceptus. Many human fertilization events never form an embryo or develop as a pregnancy.
Week 2 Movies
|
|
Timeline
| Event | ||
| Stage 5 | 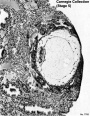 | |
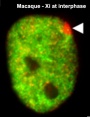 X inactivation X inactivation
| ||
| Stage 6 | ||
Implantation Sites - Normal and Abnormal
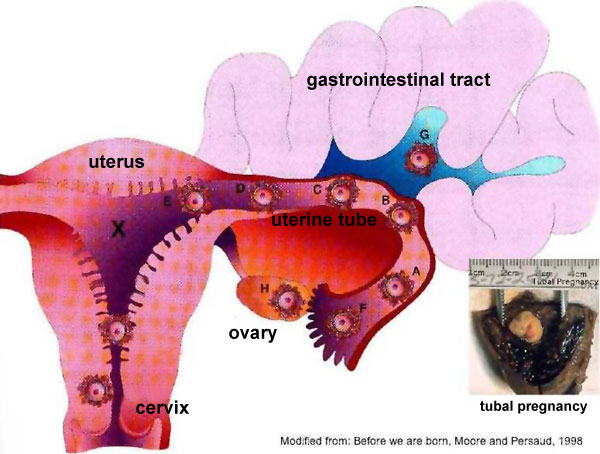
Sites of normal and abnormal blastocyst implantation.
Site of most common (normal) implantation is the posterior wall of uterus (shown by X). Abnormal implantation: tubal pregnancies (shown by A-F), ovarian (H), and abdominal (G). Implantation at the internal os generates the clinical condition placenta previa, (resulting in bleeding or placental separation during pregnancy). Note that spontaneous abortion of blastocysts is quite common and studies of blastocysts that do not implant indicate chromosomal abnormalities in many of these embryos.
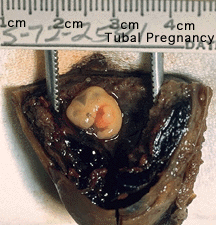
Abnormal implantation sites or Ectopic Pregnancy occurs if implantation is in uterine tube or outside the uterus.
- sites - external surface of uterus, ovary, bowel, gastrointestinal tract, mesentry, peritoneal wall
- If not spontaneous then, embryo has to be removed surgically
Tubal pregnancy - 94% of ectopic pregnancies
- if uterine epithelium is damaged (scarring, pelvic inflammatory disease)
- if zona pellucida is lost too early, allows premature tubal implantation
- embryo may develop through early stages, can erode through the uterine horn and reattach within the peritoneal cavity
Terms
- bilaminar- having 2 layers
- blastocyst- the developmental stage following morula, as this stage matures, the zona pellucia is lost allowing the conceptus to adplant and then implant into the uterine wall.
- corpus albicans - (Latin, corpus = body, albicans = whitish) The histological structure formed by luteolysis of the corpus luteum in the ovary. If implantation does not occur and the hormone hCG is not released the corpus luteum degenerates and the structure is white, not yellow, because of the absence of steroid hormone synthesis/accumulation.
- corpus luteum - (Latin, corpus = body, luteum = yellow) The remains of ovarian follicle formed after ovulation that acts as an endocrine organ (produce progesterone and oestrogens) supporting pregnancy and preventing menstruation (loss of the endometrial lining). Formed during the luteal phase (secretory phase) of the menstrual cycle by proliferation of both follicular granulosa cells (granulosa lutein cells) and thecal cells (theca lutein cells), which produce progesterone and oestrogens. If fertilization and pregnancy does not occur, the corpus luteum degenerates to form the corpus albicans. Regnier de Graaf (1641 – 1673) first observed it in the ovary of a cow as a yellow structure, the yellow colour is caused by accumulation of steroidal hormones. (More? Menstrual Cycle | Ovary Development)
- embryoblast - (inner cell mass)
- inner cell mass - (embryoblast) the clump of cells found inside the blastocyst. These cells will go in to form the embryo, these are the "stem cells" (we here about in the media) that are totipotential, they can form any tissue in the embryo. Mature oocyte-the female germ cell released at ovulation from the ovary.
- trilaminar embryonic disc - the 3 layered embryo stage.
- Trophoblasts - (Gr. trophe = nutrition) outer layer of cells on blastocyst that will generate the embryonic part of the placenta.
| ANAT2341 Lab 2: Introduction | Fertilization | Week 1 | Week 2 | Online Assessment | Group Project |
Additional Information
Birth Control
There are a number of different chemical and mechanical methods of birth control. The most comon is the "birth control pill" taken daily and made up of two hormones, estrogen and progestogen and these stop a woman's ovaries from releasing an egg each month (ovulation), which means that a pregnancy cannot begin. Recently the drug RU486, which is an abortive rather contraceptive drug, has been the centre of political and medical discussions in Australia.
Chemical
- Estrogen - the hormone estrogen in birth control pills act on the pituitary gland (supress FSH and LH) which then blocks ovulation.
- Progesterone - the hormone progesterone in birth control pills act on the uterus to both alter the lining to prevent implantation and forms a cervical mucus plug that mechanically blocks acceess of sperm. There is also an inhibition of sperm capacitation.
- Injectable Control - there are commercial (Lunelle, USA) injectable estrogen/progestin contraceptives administered on a monthly basis.
- Mifepristone (RU486) - is a progesterone receptor antagonist (antiprogesterone) which can prevent between 92-100 % of pregnancies on oral intake of a 10-600 mg dose within 72 h of unprotected intercourse. (alternative commercial name: Mifegyne)
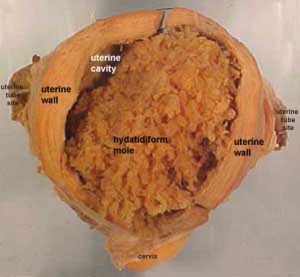
Hydatidiform Mole
| A placental tumor with no embryo development.
Several forms of hydatidiform mole: partial mole, complete mole and persistent gestational trophoblastic tumor. Many of these tumours arise from a haploid sperm fertilizing an egg without a female pronucleus (the alternative form, an embryo without sperm contribution, is called parthenogenesis). The tumour has a "grape-like" placental appearance without enclosed embryo formation. Following a first molar pregnancy, there is approximately a 1% risk of a second molar pregnancy. |
| ANAT2341 Lab 2: Introduction | Fertilization | Week 1 | Week 2 | Online Assessment | Group Project |
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2026, Mayıs 17) Embryology ANAT2341 Lab 2 - Week 2. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/ANAT2341_Lab_2_-_Week_2
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G