ANAT2241 Bone, Bone Formation and Joints
| ANAT2241 This practical support page content is not part of the virtual science practical class and provides additional information for student self-directed learning purposes. All practical class pages are located on Moodle - ANAT2241 |
General Objective
To recognise bone and understand its structure and to understand the processes by which bone can be formed. To know the structures of a synovial joint and a symphysis joint (intervertebral disc).
Specific Objectives
- To know the architecture of compact and spongy (cancellous) bone, the structure of the Haversian system (osteon), the importance and position of Haversian and Volkmann’s canals, interstitial systems.
- To understand the arrangement of compact and spongy bone in a long bone.
- To differentiate between osteoblasts, osteocytes and osteoclasts and understand their roles in bone formation.
- To identify and describe the processes of intramembranous and endochondral bone formation.
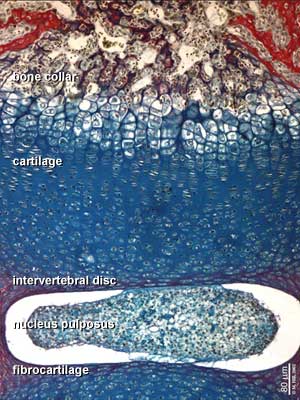
- To identify the components of a symphysis joint (intervertebral disc).
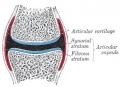
- To identify the components of a synovial joint.
Learning Activities
- Examine in the following virtual slides.
- Identify, draw & label the structures in your course manual and note their function.
Virtual Slides: Bone, Bone Formation and Joints | Histology Drawings
Introduction
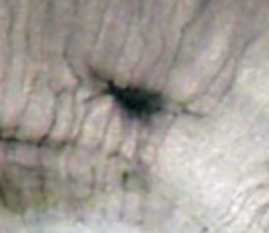
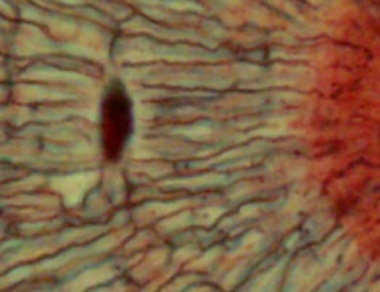
Our adult skeleton forms from a larger number of developmental elements that are replaced and fuse. In development there are 2 separate signaling pathways for pattern formation and the formation of bone itself. Furthermore bone formation can be divided into 2 specific forms that occur in anatomically different regions. This practical class will describe the development and structure of bone and finish with a study of abnormalities associated with bone.
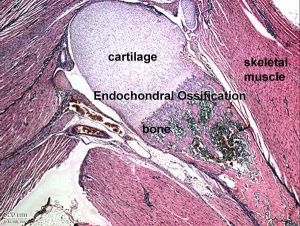
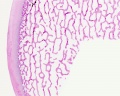
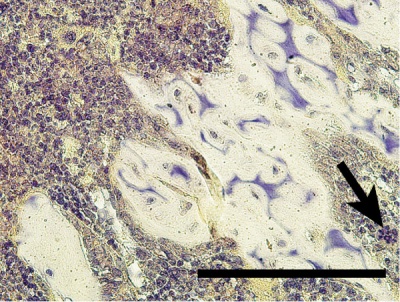
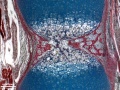
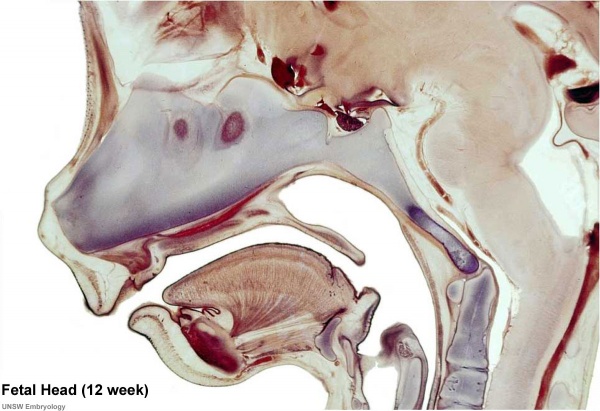
The image shown to the left shows a histological section through the developing lower limb at the level of a developing joint (knee), surrounding the developing bone are skeletal muscles and connective tissue of the limb.
Virtual Slidebox of Histology Decalcified rib, bone marrow | Developing bone | Paget's disease of bone
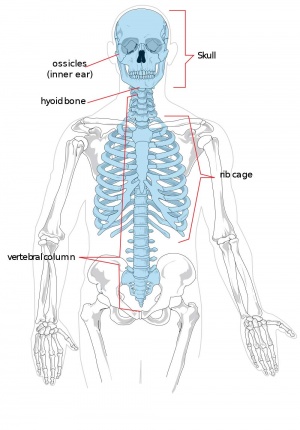
Skeleton Anatomy
--Mark Hill 14:45, 6 February 2013 (EST) This is a little cross-discipline for anatomy.
|

|
Bone Structure
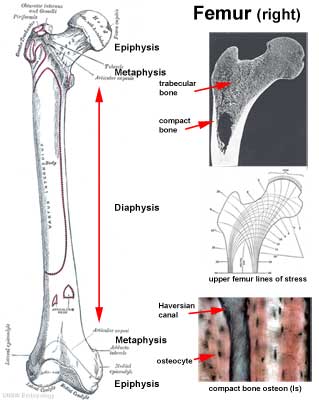
Terminology
- Diaphysis - shaft
- Epiphysis - expanded ends
- Metaphysis - connecting region (between diaphysis and epiphysial line)
- Medullary Cavity - (marrow) cavity within the bone.
More? Terms
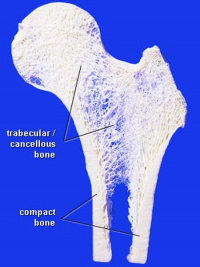
Compact Bone
- (dense) no spaces or hollows in the bone matrix visible to the eye.
- forms the thick-walled tube of the shaft (or diaphysis) of long bones, which surrounds the marrow cavity (or medullary cavity). A thin layer of compact bone also covers the epiphyses of long bones.
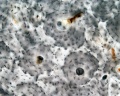
- Unstained Bone
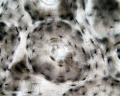
Open the images below to see a detailed view of Haversian system (osteon)
- ="Stained
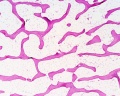
Trabecular Bone
- (cancellous or spongy bone) consists of delicate bars (spicules) and sheets of bone, trabeculae
- branch and intersect to form a sponge-like network
- ends of long bones (or epiphyses) consist mainly of trabecular bone.
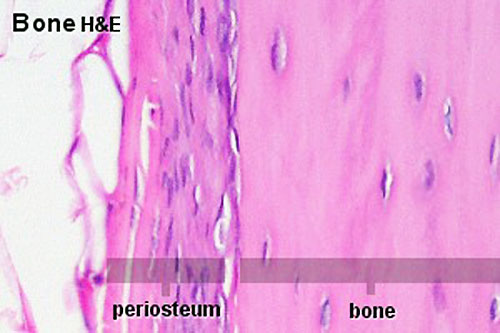
Periosteum
Connective tissue covering the surface of bone (except articular surfaces).
Endosteum
Connective tissue lining inner surface of bone.
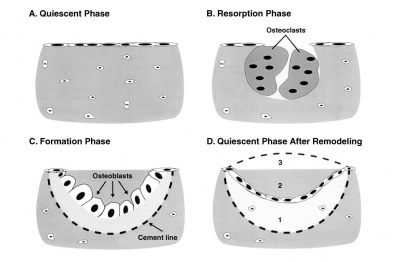
Bone Growth
- Appositional growth occurs at either the periosteum (outer surface), or the endosteum (inner surface).
- Osteoblasts secrete osteoid, a pre-bone material composed mainly of type I collagen that becomes mineralized.
- Early bone matrix deposited in development and during repair is woven rather than lamellar in appearance and structure.
- In development, there are 2 distinct types of bone formation (intramembranous and endochondral)
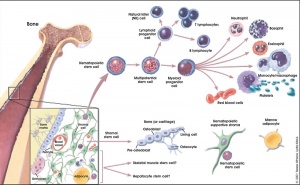
Bone Cells
Osteoblasts
- derive from osteogenic stem cells the osteoprogenitor cells that differentiate to form pre-osteoblast then osteoblasts maturing to an osteocyte
- osteoprogenitor cells - "resting cell" line the inner and outer surfaces of bone
Osteocytes
- mature bone-forming cells embedded in lacunae within the bone matrix
- osteoblasts and osteocytes - secrete organic matrix of bone (osteoid), converted into osteocytes when become embedded in matrix (which calcifies soon after deposition)
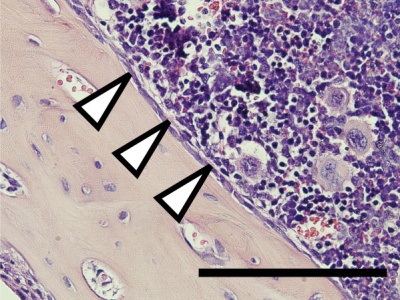
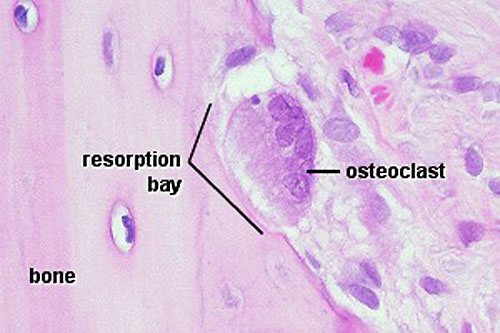
Osteoclasts
- bone-resorbing multinucleated macrophage-like cells
- origin- fusion of monocytes or macrophages, Blood macrophage precursor, Attach to bone matrix
- seal a small segment of extracellular space (between plasma membrane and bone surface), HCl and lysosomes secreted into this space by osteoclasts dissolves calcium phosphate crystals (give bone rigidity and strength)
- Resorptive bay - (Howship's lacuna) shallow bay lying directly under an osteoclast.
- do not mistake for megakaryocytes, found in bone marrow not associated with bone matrix.
- megakaryocytes are also multi-niucleated and form platelets
Bone Marrow
- red marrow - mainly haematopoietic (myeloid) tissue, newborn has all red marrow
- yellow marrow - mainly fat cells, found in diaphysis region of long bones
- stromal cells - all other support cells not involved in haematopoiesis
Chondroblasts and Chondrocytes
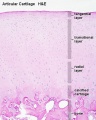
- immature and mature cartilage forming cells located at articular cartilage regions.
- Interstitial growth - occurs mainly in immature cartilage. Chondroblasts in existing cartilage divide and form small groups of cells (isogenous groups) which produce matrix to become separated from each other by a thin partition of matrix.
- Appositional growth - occurs also in mature cartilage. Mesenchymal cells surrounding the cartilage in the deep part of the perichondrium (or the chondrogenic layer) differentiate into chondroblasts.
- Links: Cartilage Histology
Bone Matrix
The bone matrix has 2 major components.
- Organic portion composed of mainly collagen Type 1 (about 95%) and amorphous ground substance.
- Inorganic portion (50% dry weight of the matrix) composed of hydroxyapatite crystals, calcium, phosphorus, bicarbonate, nitrate, Mg, K, Na.
- storage calcium and phosphate
- regulate blood calcium levels
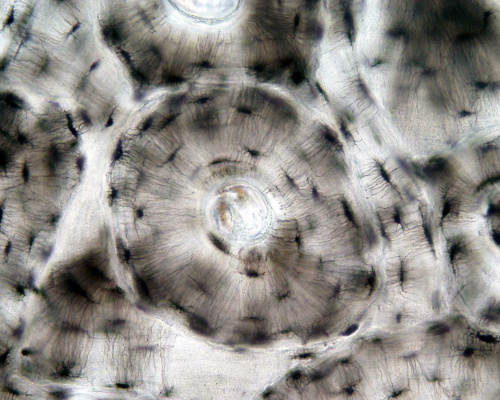
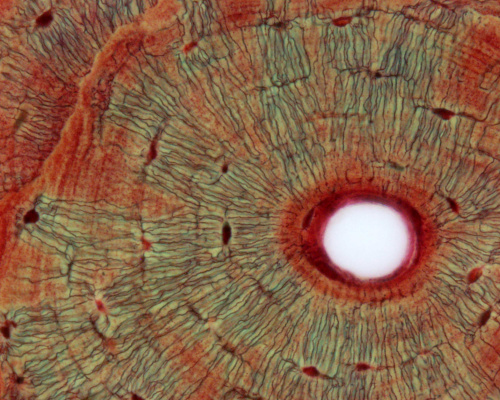
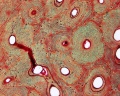
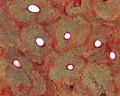
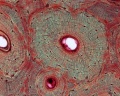
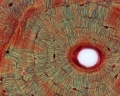
Haversian Systems
- also called osteons
- Volkmann's canals - interconnect Haversian systems
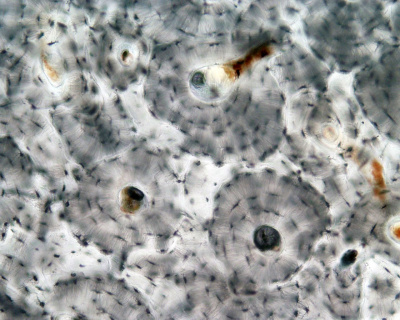
|
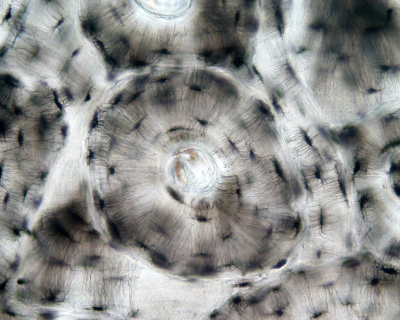
|
| Low Power (x10) | High Power (x20) |
Lamellae
- concentric - surrounding each Haversian System
- interstitial - bony plates that fill in between the haversian systems.
- circumferential - layers of bone that underlie the periosteum and endosteum
Cells
- osteocytes extending cytoplasmic processes into canaliculi
- Additional Histology images: low | medium | high
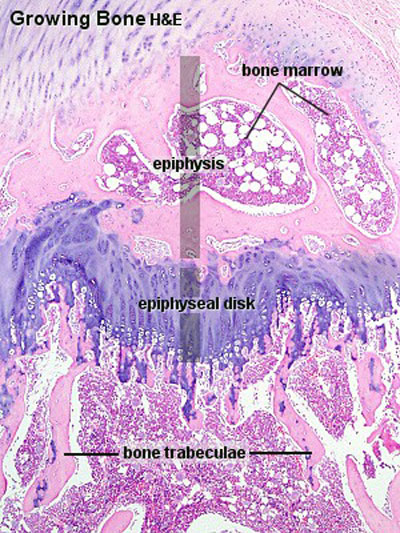
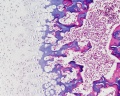
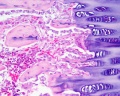
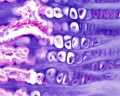
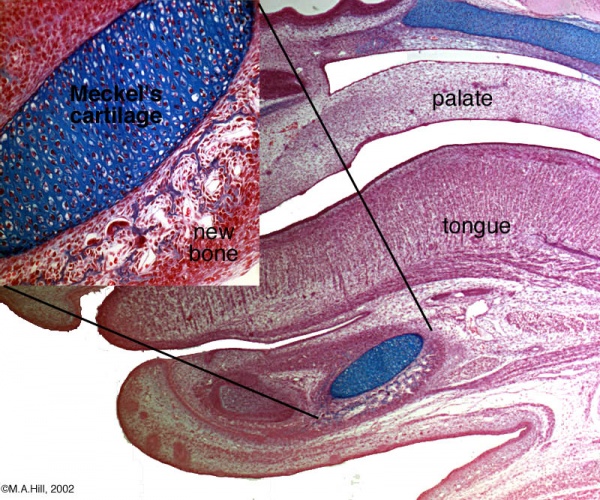
Endochondral ossification
Endochondral ossification slides: Developing bone | Bone, Developing (LS, Femur) Cat H&E
Dev Biology - endochondral ossification | endochondral ossification animation
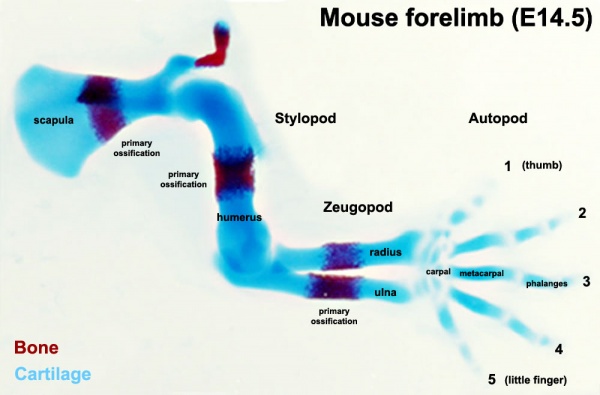
Primary ossification
Primary ossification in mouse limb (E14.5)
Gallery
- Bone Histology: Cartilage Histology | Histology Stains | Histology | cartilage | bone | bone timeline
- Trabecular bone trabecular | lamellar | trabecular - overview HE | trabecular - low HE | trabecular - med HE
- Endochondral ossification primary ossification | endochondral ossification
- Intramembranous ossification intramembranous - VG low | intramembranous - VG high | intramembranous - HE low | intramembranous - HE high
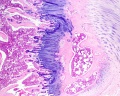
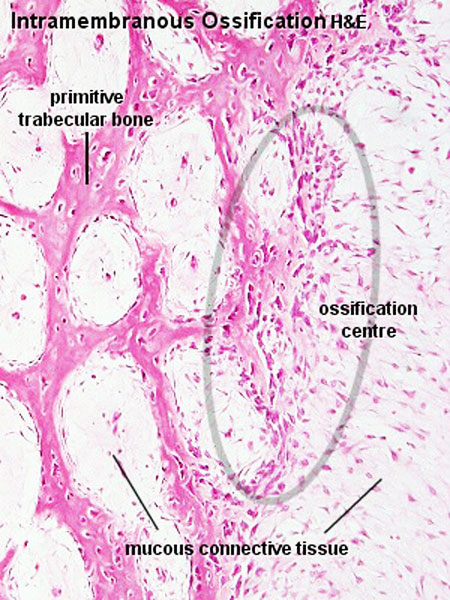
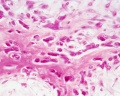
Intramembranous Ossification
Intramembranous ossification slides: Head (Neonatal) Rat H& Van Gieson
Blue histology - intramembranous
- Bone Histology: Cartilage Histology | Histology Stains | Histology | cartilage | bone | bone timeline
- Trabecular bone trabecular | lamellar | trabecular - overview HE | trabecular - low HE | trabecular - med HE
- Endochondral ossification primary ossification | endochondral ossification
- Intramembranous ossification intramembranous - VG low | intramembranous - VG high | intramembranous - HE low | intramembranous - HE high
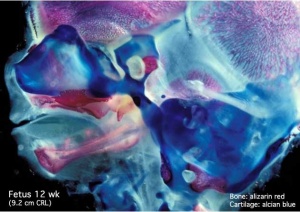
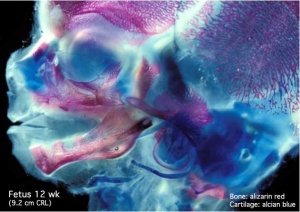
Human Fetal Head (12 week)
Histology Stains
Alizarin Red
- an anthraquinone derivative used to identify calcium in tissue sections
- calcium forms an Alizarin Red S-calcium complex in a chelation process and the end product is also birefringent.
- reaction can also identify magnesium, manganese, barium, strontium, and iron may interfere
- these elements usually in too low concentration to interfere with the staining
H&E
- acronym for hematoxylin and eosin stain
- hematoxylin - basic dye which colors basophilic structures with blue-purple hue (nucleus, DNA, RNA)
- eosin Y - acidic alcohol-based which colors eosinophilic structures bright pink (cytoplasm, extracellular matrix, protein)
H&Van Gieson
- Van Gieson's Stain is a mixture of picric acid and acid fuchsin used for differential staining of collagen and other connective tissue.
- Nuclei - stains brownish black to black
- Collagen (fibrous connective tissue) - stains pink or deep red
- Muscle, Cytoplasm, RBC and Fibrin - stains yellow
- Links: Histology Stains
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- Virtual Slidebox of Histology (USA) Skeletal system
- e-radiography Ossification
- UWA Blue Histology bone
Other Textbooks
- Anatomy of the Human Body (H. Gray, 1918.) historical anatomy text Osteology
- Molecular Biology of the Cell Bone Is Continually Remodeled by the Cells Within It | Image: Figure 22-52. Deposition of bone matrix by osteoblasts | Image: Figure 22-56. The development of a long bone
- Molecular Cell Biology Mutations in Collagen Reveal Aspects of Its Structure and Biosynthesis
- The Cell- A Molecular Approach Steroid Hormones and the Steroid Receptor Superfamily
- Clinical Methods: The History, Physical, and Laboratory Examinations 100. Alkaline Phosphatase and Gamma Glutamyltransferase
- Endocrinology: An Integrated Approach by Nussey, S.S. and Whitehead, S.A. Endocrinology: Definition and causes of osteoporosis
- Developmental Biology 6th ed. by Gilbert, Scott F. Figure 14.13. Schematic diagram of endochondral ossification | Aging: The Biology of Senescence
Search
- Pubmed ossification
Cross-Discipline
Embryology
Terms
- canaliculus - (plural, canaliculi) small channel in the bone matrix in which an osteocyte process lies and communicates with other osteocytes and the Haversian canal.
- cartilage - connective tissue from mesoderm in the embryo forms most of the initial skeleton which is replaced by bone. In adult, found on the surface of bone joints.
- Cbfa1 - Core-Binding Factor 1 (Runx2) transcription factor protein key to the differentiation of bone OMIM: Cbfa1
- centrum - the primordium of the vertebral body formed initially by the sclerotome.
- clavicle - (Latin, clavicle = little key) bone which locks shoulder to body.
- diaphysis - anatomical term that refers to the shaft of long bones.
- endochondrial ossification - the process of replacement of the cartilagenous framework by osteoblasts with bone.
- endosteum - inner layer of cells lining the medullary cavity of long bones and is highly vascularised. A similar cellular region and fibrous layer lies on the outside of the bone, the periosteum.
- epiphysis - anatomical term that refers to the expanded ends of long bones.
- extracellular matrix - material secreted by and surrounding cells. Consists if fibers and ground substance.
- fibroblast growth factors - (FGF) a family of at least 10 secreted proteins that bind membrane tyrosine kinase receptors. A patterning switch with many different roles in different tissues. (FGF8 = androgen-induced growth factor (AIGF)
- fibroblast growth factor receptor - receptors comprise a family of at least 4 related but individually distinct tyrosine kinase receptors (FGFR1- 4). They have a similar protein structure, with 3 immunoglobulin-like domains in the extracellular region, a single membrane spanning segment, and a cytoplasmic tyrosine kinase domain.
- haematopoiesis (Greek, haima = "blood"; poiesis = "to make") the process of blood cell formation. In the adult, this occurs only in the bone marrow. In the embryo this occurs in other locations (yolk sac, liver, spleen, thymus) until bone develops.
- Haversian canal - the central canal of an osteon (Haversian system) in compact bone, within which blood vessels and nerves travel throughout the bone.
- Haversian system - (osteon) the historic name for the functional unit of compact bone. Consists of a central canal (Haversian canal) surrounded by lamellar bone matrix within which osteocytes reside. Named after Clopton Havers (1650-1702) an English physician and anatomist. PMID 12999959
- Howship's lacuna - (resorptive bay) the historic name for the shallow bay or cavity lying directly under an osteoclast. This is the site of bone matrix resorption. Named after John Howship (1781–1841) a British anatomist who identified this region in 1820.
- lacuna - (Latin, lacuna = “ditch, gap” diminutive form of lacus = “lake”) lacunae is the plural, cavity in bone or cartilage for cell.
- lamellar bone - the highly organized strong bone matrix deposited in concentric sheets with a low proportion of osteocytes. Many collagen fibers parallel to each other in the same layer. Replaces woven bone.
- medullary cavity - (bone marrow) refers to the cavity within the bone, that is lined with cells (endosteum) and filled with bone marrow. in the adult, this can also be identified as either red or yellow marrow.
- mesenchymal progenitor cells - (MPCs) cells able to differentiate in various types of connective tissue, including cartilage, bone and adipose tissue.
- metaphysis - anatomical term that connecting region, that lies between the diaphysis and epiphysial line.
- osteoblast - The mesenchymal cells that differentiate to form the cellular component of bone and produce bone matrix. Mature osteoblasts are called osteocytes. (More? Musculoskeletal Development - Bone)
- osteoclast - Cells that remove bone (bone resorption) by enzymatically eroding the bone matrix. These cells are monocyte-macrophage in origin and fuse to form a multinucleated osteoclast. These cells allow continuous bone remodelling and are also involved in calcium and phosphate metabolism. The erosion cavity that the cells lie iwithin and form is called Howship's lacuna. (More? Musculoskeletal Development - Bone)
- osteocyte - The mature bone-forming cell, which form the cellular component of bone and produce bone matrix. Differentiate from osteoblasts, mesenchymal cells that differentiate to form bone. (More? Musculoskeletal Development - Bone)
- osteon - (Haversian system) the functional unit of compact bone. Consists of a central canal (Haversian canal) surrounded by lamellar bone matrix within which osteocytes reside.
- pedicle - (Latin, pediculus = small foot) part of the vertebral arch forming the segment between the transverse process and the vertebral body.
- periosteum - the cellular region and fibrous layer lying on the outside of the bone.
- primary centre of ossification - the first area where bone growth occurs between the periosteum and cartilage.
- resorptive bay - (Howship's lacuna) the shallow bay or cavity lying directly under an osteoclast. This is the site of bone matrix resorption.
- sclerotome - ventromedial half of each somite that forms the vertebral body and intervertebral disc.
- suture - in the skull a form of articulation where the contiguous margins of the bones are united by a thin layer of fibrous tissue.
- woven bone - the first deposited weaker bone matrix with many osteocytes and a matrix disorganized structure. Replaced by lamellar bone. Seen in developing, healing and bone disease.
| Bone Terms | ||
|---|---|---|
Bone Development
| ||
|
Course Links
- Histology Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | ANAT2241 Support | Histology | Histology Stains | Embryology Glossary
| Common Histology Stains | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Practical Support
- Pages can be accessed from any internet connected computer.
ANAT2241 Support Links: The Virtual Microscope | Covering and Lining Epithelia | Glandular Epithelia | CT Components | CT Types | Bone, Bone Formation and Joints | Muscle | Nervous | Blood | Eye | Cardiovascular | Respiratory | Integumentary | Gastrointestinal | Gastrointestinal Organs | Lymphatic and Immune | Endocrine | Urinary | Female Reproductive | Male Reproductive | Histology Stains | Histology Drawings | Practicals Health and Safety 2013 | Moodle - 2019
ANAT2241 This practical support page content is not part of the science practical class and provides only background information for student self-directed learning purposes.
Cite this page: Hill, M.A. (2026, Mayıs 18) Embryology ANAT2241 Bone, Bone Formation and Joints. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/ANAT2241_Bone,_Bone_Formation_and_Joints
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G