ANAT2241 Female Reproductive System
| ANAT2241 This practical support page content is not part of the virtual science practical class and provides additional information for student self-directed learning purposes. All practical class pages are located on Moodle - ANAT2241 |
General Objective
To know the histological and cytological structure of the major organs of the female reproductive system.
Specific Objectives
- To describe the microanatomy of the ovary and to identify: peritoneal mesothelium, developing ovarian follicles, Graafian and atretic follicles.
- To know the layers of the wall of the uterine tube (Fallopian tube or oviduct).
- To know the structure of the uterus and the morphological changes of the endometrium during the menstrual cycle.
- To know the structure of the mammary glands.
Learning Activities
Examine the following virtual slides, and in course manual identify, draw and label the structures listed and note the function.
Virtual Slides: Female Reproductive System
See also Male Reproductive System
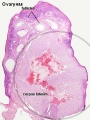
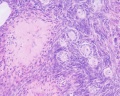
Ovary
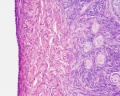
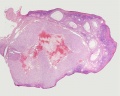
The external surface of the ovary has a cuboidal epithelium (germinal epithelium) overlying a dense connective tissue layer (tunica albuginea). The outer epithelium is continuous with the peritoneum (serosa) forming a peritoneal fold (mesovarium) between the anterior border of the ovary with the posterior layer of the broad ligament of the uterus.
Ovary structure (regions)
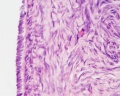
- cortex - cellular connective tissue containing the developing follicles.
- medulla - loose connective tissue containing blood vessels, lymphatics and nerves.
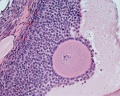
Ovarian Follicle
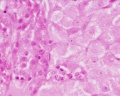
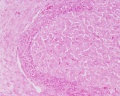
Corpus Luteum
Theca Lutein Cells
Granulosa Lutein Cells
|

|
Corpus Albicans
Hormone secretion in the corpus luteum ceases within 14 days after ovulation if the oocyte is not fertilised. In this case, the corpus luteum degenerates into a corpus albicans - whitish scar tissue within the ovaries.
Ovary Histology
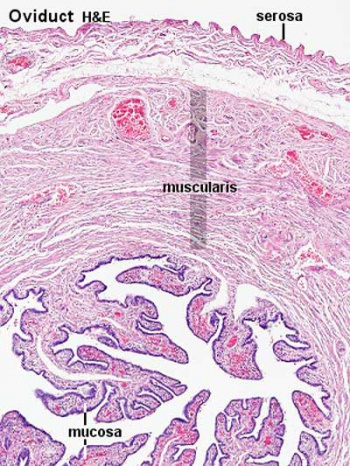
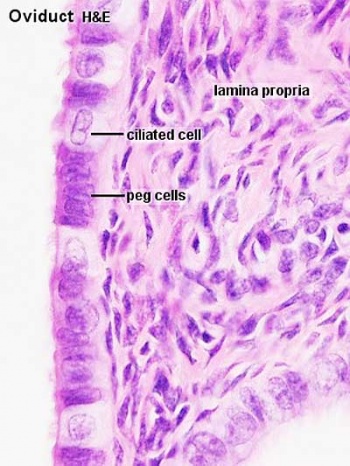
Uterine Tube
(oviduct, Fallopian tube)
- uterine tube acts as a conduit for the oocyte, from the ovaries to the uterus.
- consists of a mucosa and a muscularis.
- peritoneal surface of the oviduct is lined by a serosa and subjacent connective tissue.
Tube Regions
| infundibulum | ampulla | isthmus | intramural |
|---|---|---|---|
| funnel-shaped (up to 10 mm in diameter) end of the oviduct. Finger-like extensions of its margins, the fimbriae, are closely applied to the ovary. Ciliated cells are frequent. | mucosal folds, or plicae, and secondary folds which arise from the plicae divide the lumen of the ampulla into a very complex shape. Fertilization usually takes place in the ampulla. | narrowest portion (2-3 mm in diameter) of the tube located in the peritoneal cavity. Mucosal folds are less complex and the muscularis is thick. An inner, longitudinal layer of muscle is present in the isthmus. | penetrates the wall of the uterus. The mucosa is smooth, and the inner diameter of the duct is very small. |
Uterus
- parts - body (upper two-thirds) and cervix.
- walls - mucosal layer, the endometrium, and a fibromuscular layer, the myometrium.
- peritoneal surface of the uterus is covered by a serosa.
Myometrium
- smooth muscle fibres form several layers with preferred orientations.
- muscular tissue hypertrophies during pregnancy.
- GAP-junctions between cells become more frequent.
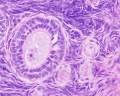
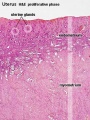
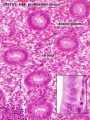
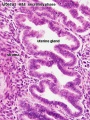
Endometrium
- simple columnar epithelium (ciliated cells and secretory cells) and an underlying thick connective tissue stroma.
- mucosa is invaginated to form many simple tubular uterine glands.
- glands extend through the entire thickness of the stroma.
- stromal cells of the endometrium are embedded in a network of reticular fibres.
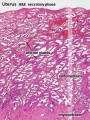
Menstrual cycle
- hormones alter the endometrium.
- only the uterus body mucosa takes part in the menstrual cycle.
- endometrial layers (based on changes)
- basalis - remains during menstruation, functions as a regenerative zone for the functionalis.
- functionalis - lost during menstruation, functions as the site of cyclic changes in the endometrium.
- Uterus Histology Links: Labeled - proliferative phase | Labeled - gland proliferative phase | Labeled - secretory phase | Unlabeled - secretory phase | Unlabeled - late secretory phase | Labeled - gland secretory phase | Menstrual Cycle | Uterine Gland | Uterus Development
- Links: Menstrual Cycle - Histology
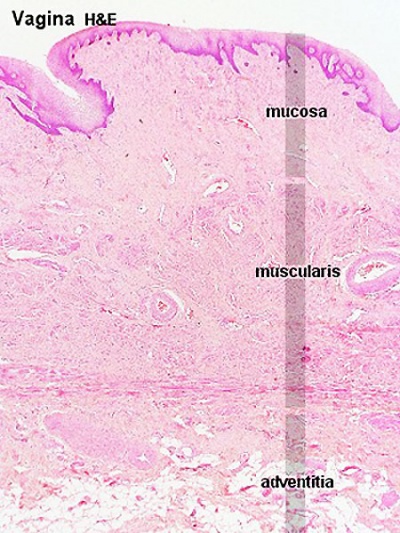
Vagina
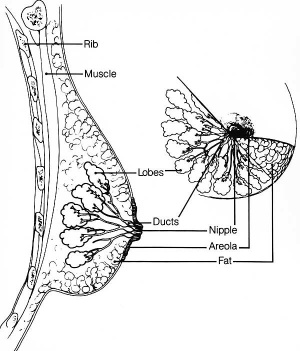
Mammary Gland
The mammary glands are modified glands of the skin and their development is similar to that of sweat glands.
- compound branched alveolar glands, secretory unit is the alveolus
- consist of 15-25 lobes separated by dense interlobar connective tissue and fat.
- each lobe contains an individual gland.
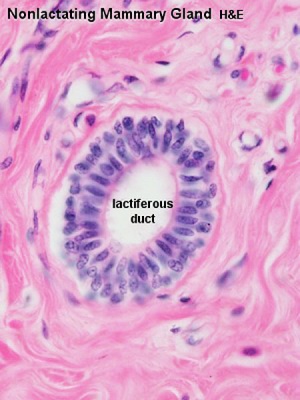
- lactiferous duct - excretory duct of each lobe with own opening on the nipple.
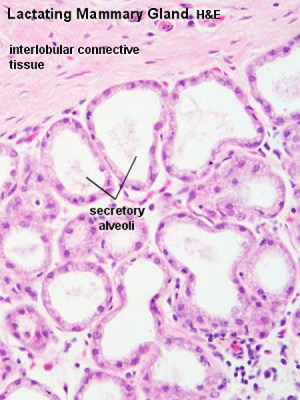
Alveolus
- inner layer of cuboidal secretory epithelial cells
- merocrine secretion, protein micelles are release by exocytosis.
- outer layer of myoepithelial cells
- located between the secretory cells and the surrounding basal lamina.
- contraction helps force the milk from the secretory alveoli into the ducts.
Note - plasma cells in the stroma also secrete antibodies (dimeric IgA) and released into the milk, to provides passive immunity to the suckling young.
| lactiferous duct | lactating mammary gland |
|---|---|
|
|
- Links: Mammary Gland Development | Milk
Terms
- corona radiata - layer of cells of cumulus oophorus remaining attached to zona pellucida of oocyte after ovulation.
- corpus - (Latin, corpus = body).
- corpus albicans - (Latin, corpus = body + albicans = "whitish") a degenerating corpus luteum in the ovary.
- corpus luteum - (Latin, corpus = body + luteum = yellow) major endocrine organ which is the remains of ovarian follicle after ovulation; yellow in ovary of cow where de Graaf (q.v.) first saw it.
- cortex - (Latin = rind, or bark) outer layer of an organ.
- cumulus oophorus - (Latin = cumulus = a little mound + Greek oon = egg + phorus = bearing) part of the wall of an ovarian follicle surrounding and carrying the oocyte.
- fimbria - (Latin, fimbria = a fringe) the fringed open ovarian end of the uterine tube.
- follicle - (Latin, folliculus = little bag).
- hilum - or hilus (Latin,= a trifle; depression in a seed) a depression at vascular entrance/exit of a gland or organ.
- mesovarium - short peritoneal fold connecting the anterior border of the ovary with the posterior layer of the broad ligament of the uterus.
- medulla - (Latin, medulla = pith, marrow) the inner portion of an organ, in contrast to cortex.
- menstrual - (Latin, menstruus = monthly) relating to the monthly female sexual cycle.
- mucosa - (Latin, = mucous membrane) thin layer which lines body cavities and passages formed by epithelium and lamina propria.
- oocyte - (Greek, öon = egg + kytos = hollow vessel (cell) the female germ cell in the ovary.
- parenchyma - (Greek," + enkeim = to pour in) the essential functional cells of an organ as opposed to its stroma.
- salpinx - (Greek, = a trumpet) the uterine tube.
- serosa - (Latin, serum = whey; a pale fluid) a serous membrane lining body cavities.
- stroma - (Greek, = a cover, table-cloth, bedding) term for the internal supporting frame-work of a tissue, or organ, as opposed to its parenchyma.
- tunica albuginea - a dense, white, fibrous sheath enclosing a part or organ.
- uterine tube - (oviduct, Fallopian tube)
- uterus - (Latin, = womb, from uter = a large goatskin bag used as a wine-skin).
- zona pellucida - (Latin, zona = a girdle + perlucere = to shine through) the refractile layer of glycoclayx (ECM) surrounding oocyte in a growing ovarian follicle.
- Histology Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | ANAT2241 Support | Histology | Histology Stains | Embryology Glossary
Ovary Histology
Ovary histology: Tunica Albuginea x20 | Tunica albuginea, Germinal epithelium x40 |
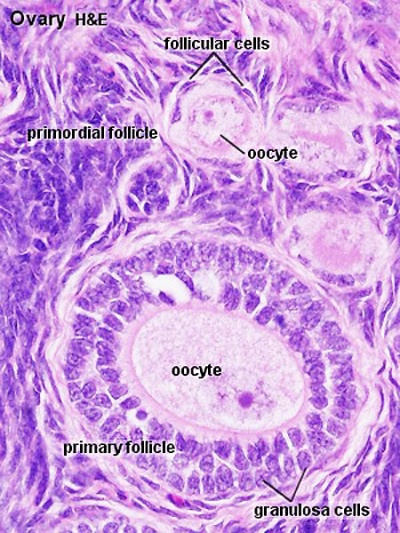
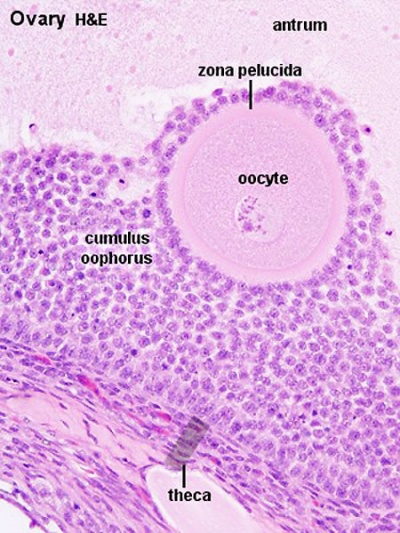
Primary follicle, primordial follicle, oocyte, x40 | Secondary follicle, cumulus oophorus, zona pelucida, granulosa cells, oocyte x20 | Corpus luteum, theca lutein cells, granulosa lutein cells, Loupe | Corpus luteum, theca lutein cells, granulosa lutein cells, x10 | Corpus luteum, theca lutein cells, granulosa lutein cells, x40 | Corpus albicans, primary follicle, primordial follicle, granulosa cells, oocyte x20 | Menstrual Cycle | Ovary Development
Menstrual Histology
Menstrual Cycle - Histology (images are listed in sequence and uterine endometrium from dilatation and curettage)
- Uterine Endometrium: menstrual | mid-proliferative | late proliferative | secretory | late secretory
- Vaginal Smear: early proliferative | mid-proliferative | late proliferative | secretory | late secretory
Links: Menstrual Cycle - Histology | Menstrual Cycle | Papanicolaou stain
Course Links
- Histology Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | ANAT2241 Support | Histology | Histology Stains | Embryology Glossary
| Common Histology Stains | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Practical Support
- Pages can be accessed from any internet connected computer.
ANAT2241 Support Links: The Virtual Microscope | Covering and Lining Epithelia | Glandular Epithelia | CT Components | CT Types | Bone, Bone Formation and Joints | Muscle | Nervous | Blood | Eye | Cardiovascular | Respiratory | Integumentary | Gastrointestinal | Gastrointestinal Organs | Lymphatic and Immune | Endocrine | Urinary | Female Reproductive | Male Reproductive | Histology Stains | Histology Drawings | Practicals Health and Safety 2013 | Moodle - 2019
ANAT2241 This practical support page content is not part of the science practical class and provides only background information for student self-directed learning purposes.
Cite this page: Hill, M.A. (2026, Mayıs 5) Embryology ANAT2241 Female Reproductive System. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/ANAT2241_Female_Reproductive_System
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G