Lecture - Early Vascular Development
| Embryology - 19 May 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
This lecture is an introduction to the events in early embryonic development that relate to mesoderm and early cardiovascular development. Texts frequently separate heart development from vascular development in order to simplify their descriptions of cardiovascular development, although the two are functionally and embryonically connected.
Note that later in the course, the late development of the heart and vascular changes will be further discussed. The complexity of septation, cardiac outflow separation, remodelling of the peripheral vasculature, and the pre- to post-natal changes may also contribute to the relatively large proportion of birth defects associated with this system. These events of vascular development are covered in a later lecture.
It is important to note also that we are just beginning to understand vascular development which involves the careful orchestration of a variety of moleculular mechanisms. Development does appear to be an independent mechanism preceding both skeletal and smooth muscle development and using different regulatory mechanisms. In the next few years, there are certain to be new molecules identified as well as an understanding and appreciation of new roles for known molecules.
- Vasculogenesis - formation of new blood vessels assemble from individual precursor cells.
- Angiogenesis - sprouting of new vessels occurs from pre-existing vessels.
Lecture Objectives
- Understanding of mesoderm development
- Understanding of heart tube formation and early development
- Understanding of early blood vessel and blood development
- Brief understanding of vascular growth and regression
- Brief understanding of vascular growth factors
Lecture Resources
| Movies | ||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
|
| References | |
|---|---|
| Hill, M.A. (2020). UNSW Embryology (20th ed.) Retrieved May 19, 2024, from https://embryology.med.unsw.edu.au |
|
| Moore, K.L., Persaud, T.V.N. & Torchia, M.G. (2015). The developing human: clinically oriented embryology (10th ed.). Philadelphia: Saunders. | The following chapter links only work with a UNSW connection. |
| Schoenwolf, G.C., Bleyl, S.B., Brauer, P.R. & Francis-West, P.H. (2009). Larsen's human embryology (4th ed.). New York; Edinburgh: Churchill Livingstone. | The following chapter links only work with a UNSW UNSW Library subscription
|
| ECHO360 Recording |
|---|
|
Links only work with currently enrolled UNSW students. Lecture 7 - Rich Media Playback | Vodcast Playback | Podcast Playback |
Development Overview
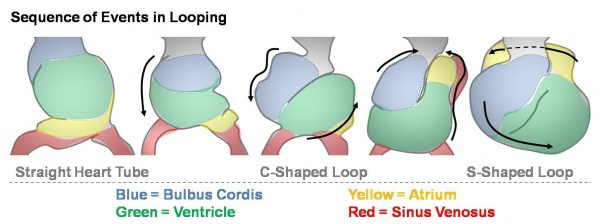
The heart develops from cardiogenic mesoderm that originally lies above the cranial end of the developing neural tube. Enlargement of the cranial neural fold brings this region ventrally to its correct anatomical position. The original paired cardiac tubes fuse, with the "ventricular" primordia initially lying above the "atria". Growth of the cardiac tube flexes it into an "S-shape" tube, rotating the "ventricles" downward and pushing the "atria" upward.
This is then followed by septation, a complex process which converts this simple tube into a four chambered heart and covered in a later lecture and lab. A key part of this process is the separation of cardiac outflow (truncus arteriosus) into a separate pulmonary and aortic arch outflow. During embryonic development there is extensive remodelling of the initially right and left symmetrical cardiovascular system and a contribution from the neural crest to some vessels.
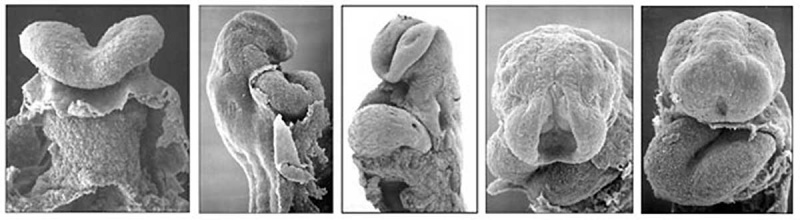
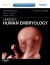
|
| The Human Heart from day 10 to 25 (scanning electron micrograph) |
Timecourse
Angiogenesis
- Begins week 3 in extraembryonic mesoderm and then embryonic splanchnic mesoderm
- Begins as the formation of blood islands
- Earliest islands - yolk sac, connecting stalk and chorion (Area vasculosa)
- Growth factors stimulate growth and development - Vascular Endothelial Growth Factor (VEGF) and Placental Growth Factor (PlGF, PGF)
- Growing blood vessels follow a gradient generated by target tissues/regions of Vascular Endothelial Growth Factor (VEGF) to establish a vascular bed. Recent findings suggest that Notch signaling acts as an inhibitor for this system, preventing sprouting of blood vessels. Notch is a transmembrane receptor protein involved in regulating cell differentiation in many developing systems.
- PIGF is also a VEGF released from the placental trophoblast cells.
- angioblasts form clusters called "blood islands"
- blood islands extend and fuse together to form a primordial vascular network
Blood islands
- Blood islands contain cells (haemangioblasts) which are capable of differentiating into 2 populations of cells
- Vascular precursors (angioblasts) - form endothelial cells
- Blood cell precursors (haemocytoblasts)
- These angioblasts migrate, coalesce into cords and form a lumen. This process of vessel formation is called vasculogenesis and is dominant in very early embryogenesis e.g. formation of the dorsal aorta
- Sprouting from pre-existing vessels is called angiogenesis e.g. brain is an organ which is vascularized by this process
- Note: the vascular tree undergoes constant remodeling as the embryo grows.
Blood vessel lumen formation
Blood formation
Red blood cells
Early vascular systems
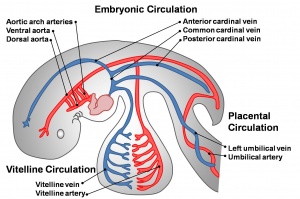
- one vascular system with 3 components - vitelline, embryonic (system) and placental
- each component has own system of artery and vein
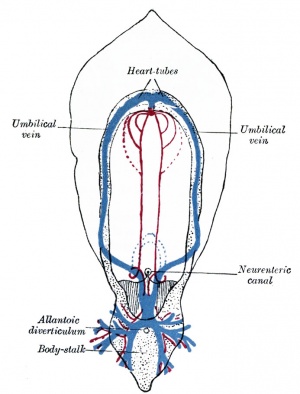
Vitelline blood vessels
- Angioblasts form a network of vessels over the yolk sac and connecting stalk
- Join into two main vessels, the vitteline veins (omphalomesenteric)
- Pass through vitello-intestinal duct (yolk sac stalk)
- Enter caudal end of cardiac tube
- Vitelline Arteries - arises from dorsal aorta, contribute to adult GIT arteries (fuse to become superior mesenteric artery (midgut)
- Vitelline Veins - empties into sinus venosus, contribute to the adult portal system
Embryo blood vessels
- (systemic) will form the most of the cardiovascular system
- some vessels have neural crest contribution
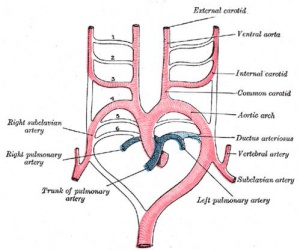
- Arterial blood flow - aortic sac → aortic arches → dorsal aorta →umbilical artery
- dorsal aorta,
- paired initially , later fuses from T4 to L4 (gives off segmental arteries)
- connect to ventral aorta via pharyngeal arches arteries.
- caudally, give rise to umbilical arteries
- laterally, give rise to intersegmental arteries
- dorsal aorta,
- Veins - 3 pairs of veins empty into the sinus venosus of the heart
- vitelline, umbilical (right and left from developing placenta enter caudal cardiac tube; only left persists)
- cardinal veins - anterior, common, posterior
|
|
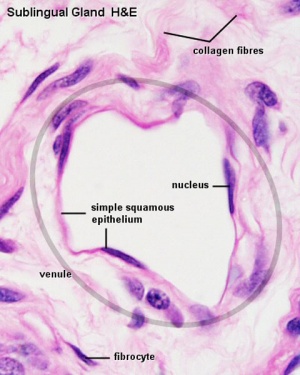
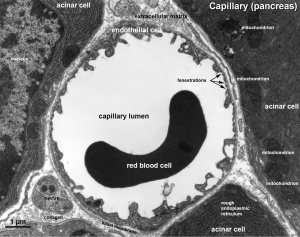
| Vein histology | Blood capillary (EM) |
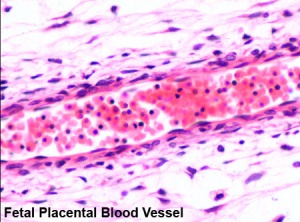
Placental blood vessels
(Placenta development covered in next lecture)
- form initially in the connecting stalk (then umbilical cord) and anastomose in chorion
- extend maternally - toward the chorionic villi
- extend embryonically - toward the sinus venosus and dorsal aorta
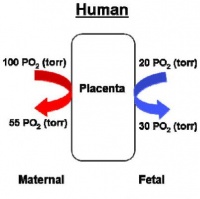
- Arteries - paired and carry deoxygenated blood (from dorsal aorta) and waste products to the placental villi
- Veins - paired initially then only left at end of embryonic period and carry oxygenated blood to the embryo (sinus venosus)
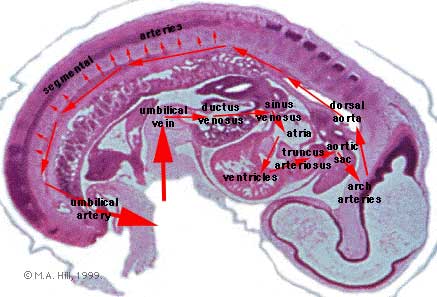
Blood flow through the embryo
High pressure pathway
Maternal Blood | -> umbilical vein -> liver -> anastomosis -> sinus venosus -> atria ventricles-> truncus arteriosus -> aortic sac -> aortic arches-> dorsal aorta-> pair of umbilical arteries | Maternal Blood.
Low pressure pathway
- Head - Large veins lateral to dorsal aortae. These are the superior or anterior cardinal veins. Their function is to drain the head region.
- Body - Large veins lateral to dorsal aortae. These are the inferior or posterior cardinal veins. Their function is to drain the lower part of the embryo.
Blood vessel remodeling
Early vascular development is laterally symmetrical (paired left and right). With embryo development this scheme is extensively remodelled leading to an asymmetric adult system in the body.
Complex balance between Stimulators and Inhibitors of Angiogenisis.
- Links: Blood Vessel Development
Vascular Endothelial Growth Factor (VEGF)
- belongs to the platelet derive growth factor (PDGF) family.
- required for early stages of blood vessel patterning.
- required later for endothelial cell maintenance in tissues.
- autocrine VEGF loop from endothelial cell secretion involved in vascular growth.
- 4 protein isoforms generated from a single gene.
VEGF protein family - VEGF (or VEGF-A), VEGF-B, VEGF-C, VEGF-D and placental growth factor (PGF),
VEGF receptors - VEGFR-1, -2 and -3.
- Cells expressing the receptors are directed in their growth.
- Note that there are other growth factor families (FGF, Tie, TGF-β, netrins, semaphorins) that can also influence vessel growth.
- Some angiogenic factors also involved in organ development (liver).
Heart Development
MH - Later development of the heart (septation) will be covered in another lecture.
Early heart development
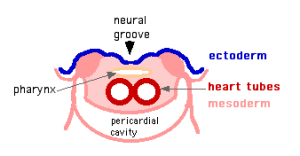
- Mesenchymal condensation in splanchnic mesenchyme = cardiogenic plate
- Following bending and folding, the plate comes to lie dorsal to pericardial coelom
- Plate undergoes bilateral canalisation to form 2 cardiac tubes:
- cranial part of cardiac tubes = ventral aortae which will later join the existing dorsal aortae
- Caudally the tubes will join vitelline and umbilical veins
- Cardiac tubes fuse to form single heart tube that sinks into coelom (= future pericardial sac)
- At this stage, the heart is an endothelial tube surrounded by visceral layer of pericardium (epicardium)
- From the time of the fusion of cardiac tubes, the walls undergo fibrillary movements (forerunner of cardiac contraction)
- Later, space between epicardium and cardiac endothelium fills with jelly-like material (cardiac jelly), which becomes invaded by cells of deep layer of epicardium. These are the myoblasts (future cardiac muscle)
- Combined layer of epicardium and invaded jelly = myoepicardial mantle.
- Epicardial layer also gives rise to blood islands which form vascular network (future coronary vessels)
- Heart tube (now within the pericardial coelom) begins to undergo internal and external changes.
Heart layers
- pericardium - covers the heart. Formed by 3 layers consisting of a fibrous pericardium and a double layered serous pericardium (parietal layer and visceral epicardium layer).
- myocardium - muscular wall of the heart. Thickest layer formed by spirally arranged cardiac muscle cells.
- endocardium - lines the heart. Epithelial tissue lining the inner surface of heart chambers and valves.
Heart looping
|
|
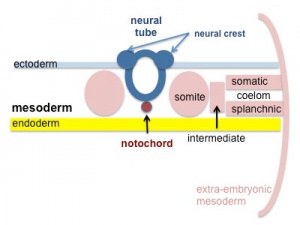
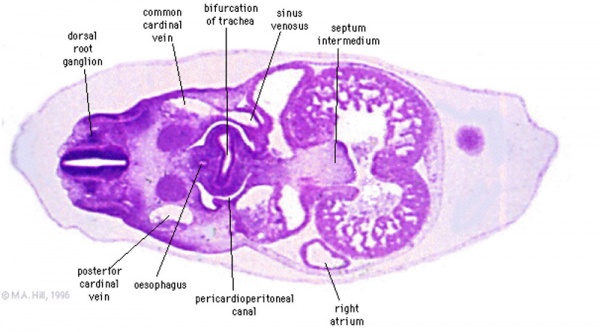
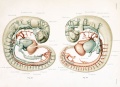
Transverse section- Heart is 2 tubes that fuse in the midline anterior to pharynx.
The pericardial cavity can be imagined as the top of the "horseshoe" of the intraembryonic coelom. (where the arms become the pleural cavity and the ends fuse anteriorly to form a single peritoneal cavity).
This view shows the initial positioning of the ventricles above the atria. The ventricles are rotated into their correct anatomical position by the growth of the heart tube, bending into an "S" shape.
Initially...
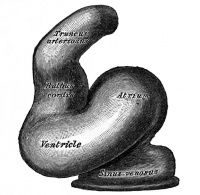
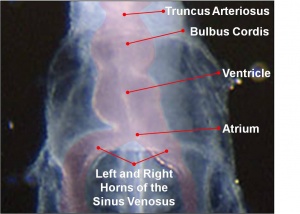
- Heat tube develops a series of constrictions:
- Truncus arteriosus – ventral aortae meet - OUTFLOW
- Bulbus cordis
- Ventricle
- Atrium
- Sinus venosus – caudal end of tube, receiving 4 veins - INFLOW
- Rapid growth – ‘buckling’ and ‘twisting’
- Heart tube bends ventrally into pericardial coelom
- Ventricle enlargens, absorbs lower part of bulbus cordis (bulboventricular loop)
- Ventricle also twists to left- atrium and sinus venosus come to lie dorsal to bulbus cordis and lower part of truncus arteriosus
- Venous inflow comes to lie directly dorsal to the arterial outflow.
- Possible abnormality – dextro-rotation, the heart bends or twists to the right. Maybe associated by other abnormalities.
- Later, sinus venosus becomes absorbed into atrium
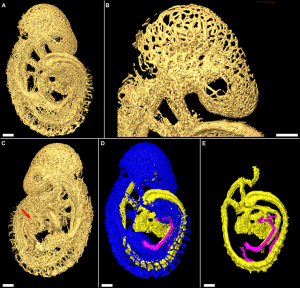
Heart neural crest
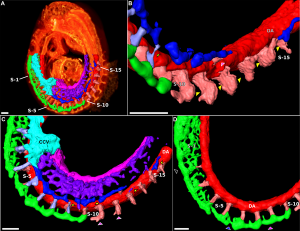
- The mouse model shows that the heart also has contributions from neural crest E8.5 mouse neural crest
- between the levels of post-otic hindbrain to somite 4, with the most contribution from somite 2 level.
- 7 somite stage - Migration of cardiac neural crest from the neural tube begins. (level post-otic hindbrain and somite 4)
- Pathways dorsolateral, medial, and between somites.
- Then through peri-aortic mesenchyme (lateral to pharynx), through pharyngeal arches (3, 4, 6) into the aortic sac.
- 32 somite stage: Colonisation of the outflow tract mesenchyme.
Data from: Chan WY, Cheung CS, Yung KM, Copp AJ. Chan WY, Cheung CS, Yung KM, Copp AJ. Cardiac neural crest of the mouse embryo: axial level of origin, migratory pathway and cell autonomy of the splotch (Sp2H) mutant effect. Development. 2004 Jul;131(14):3367-79. PMID: 15226254
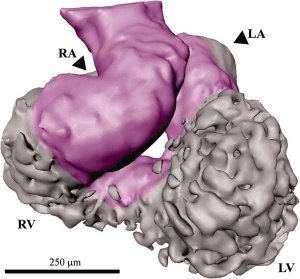
Embryonic heart rate
- Ultrasonographic measurement of embryonic heart rate (EHR) shows a steady increase from Stage 9-10 (75 beats/minute) to Stage 18 (130 beats/minute) and on to Stage 20, following which a gradual decrease in EHR occurs
- Maximal EHR is reached when morphological development of the embryonic heart is completed.
- Links: Embryonic Heart Rate
Internet Links
Embryo Images Unit: Embryo Images Online Early Cell Populations (cardiogenic section) | Cardiovascular Development | Week 3 Development | Week 4 Development | Heart Chambers and Outflow Tract | Atrioventricular Septation | Outflow Tract Septation | Ventricular Septation | Atrial Septation | Atrial Walls Aortic Arch Vessels | Changes at Birth
References
Online Textbooks
- Developmental Biology by Gilbert, Scott F. Sunderland (MA): Sinauer Associates, Inc.; c2000 The Heart | Figure 15.6. Cascade of heart development} | [http://www.ncbi.nlm.nih.gov/books/bv.fcgi?&rid=dbio.figgrp.3698 Figure 15.3. Formation of the chick heart from the splanchnic lateral plate mesoderm | Figure 15.4. Fusion of the right and left heart rudiments to form a single cardiac tube | Figure 15.5. Specification of the atrium and ventricles occurs even before heart looping
- Molecular Biology of the Cell 4th ed. Alberts, Bruce; Johnson, Alexander; Lewis, Julian; Raff, Martin; Roberts, Keith; Walter, Peter New York and London: Garland Science; c2002 - Figure 21-35. The vertebrate body plan as a dorsoventral inversion of the insect body plan Figure 22-40. The four classes of muscle cells of a mammal
Terms
For more cardiovascular term definitions and links to related topics use the glossary.
angioblast - the stem cells in blood islands generating endothelial cells which will form the walls of both arteries and veins. (More? Blood Vessel)
angiogenesis - the formation of blood vessels also called vasculogenesis in the embryo.
anlage (German, anlage = primordium) structure or cells which will form a future more developed or differentiated adult structure.
blood islands - earliest sites of blood vessel and blood cell formation, seen mainly on yolk sac chorion.
cardinal veins - paired main systemic veins of early embryo, anterior, common, posterior.
cardiogenic region - region above prechordal plate in mesoderm where heart tube initially forms.
ectoderm - the layer (of the 3 germ cell layers) which form the nervous system from the neural tube and neural crest and also generates the epithelia covering the embryo.
endoderm - the layer (of the 3 germ cell layers) which form the epithelial lining of the gastrointestinal tract (GIT) and accessory organs of GIT in the embryo.
endocardium - lines the heart. Epithelial tissue lining the inner surface of heart chambers and valves.
endothelial cells - single layer of cells closest to lumen that line blood vessels.
extraembryonic mesoderm - mesoderm lying outside the trilaminar embryonic disc covering the yolk sac, lining the chorionic sac and forming the connecting stalk. Contributes to placental villi development.
haemocytoblasts - stem cells for embryonic blood cell formation.
anastomose - to connect or join by a connection (anastomosis) between tubular structures.
chorionic villi - the finger-like extensions which are the functional region of the placental barrier and maternal/fetal exchange. Develop from week 2 onward as: primary, secondary, tertiary villi.
estrogens - support the maternal endometrium.
growth factor - usually a protein or peptide that will bind a cell membrane receptor and then activates an intracellular signaling pathway. The function of the pathway will be to alter the cell directly or indirectly by changing gene expression. (eg VEGF, shh)
maternal decidua - region of uterine endometrium where blastocyst implants. undergoes modification following implantation, decidual reaction.
maternal sinusoids - placental spaces around chorionic villi that are filled with maternal blood. Closest maternal/fetal exchange site.
mesoderm - the middle layer of the 3 germ cell layers of the embryo. Mesoderm outside the embryo and covering the amnion, yolk and chorion sacs is extraembryonic mesoderm.
myocardium - muscular wall of the heart. Thickest layer formed by spirally arranged cardiac muscle cells.
pericardium - covers the heart. Formed by 3 layers consisting of a fibrous pericardium and a double layered serous pericardium (parietal layer and visceral epicardium layer).
pharyngeal arches (=branchial arches, Gk. gill) series of cranial folds that form most structures of the head and neck. Six arches form but only 4 form any structures. Each arch has a pouch, membrane and groove.
placenta - (Greek, plakuos = flat cake) refers to the discoid shape of the placenta, embryonic (villous chorion)/maternal organ (decidua basalis)
placental veins - paired initially then only left at end of embryonic period, carry oxygenated blood to the embryo (sinus venosus).
protein hormone - usually a protein distributed in the blood that binds to membrane receptors on target cells in different tissues. Do not easliy cross placental barrier.
sinus venosus - cavity into which all major embryonic paired veins supply (vitelline, placental, cardinal).
splanchnic mesoderm - portion of lateral plate mesoderm closest to the endoderm when coelom forms.
steroid hormone - lipid soluble hormone that easily crosses membranes to bind receptors in cytoplasm or nucleus of target cells. Hormone+Receptor then binds DNA activating or suppressing gene transcription. Easliy cross placental barrier.
syncitiotrophoblast extraembryonic cells of trophoblastic shell surrounding embryo, outside the cytotrophoblast layer, involved with implantation of the blastocyst by eroding extracellular matrix surrounding maternal endometrial cells at site of implantation, also contribute to villi. (dark staining, multinucleated).
truncus arteriosus - an embryological heart outflow structure, that forms in early cardiac development and will later divides into the pulmonary artery and aorta. Term is also used clinically to describe the malformation where only one artery arises from the heart and forms the aorta and pulmonary artery.
vascular endothelial growth factor - (VEGF) protein growth factor family that stimulates blood vessel growth, a similar factor can be found in the placenta (PIGF).
vitelline blood vessels - blood vessels associated with the yolk sac.
waste products - products of cellular metabolism and cellular debris, e.g.- urea, uric acid, bilirubin.
| ANAT2341 Course Timetable | |||
|---|---|---|---|
| Week (Mon) | Lecture 1 (Mon 1-2pm) | Lecture 2 (Tue 3-4pm) | Practical (Fri 1-3pm) |
| Week 2 (1 Aug) | Introduction | Fertilization | Lab 1 |
| Week 3 (8 Aug) | Week 1 and 2 | Week 3 | Lab 2 |
| Week 4 (15 Aug) | Mesoderm | Ectoderm | Lab 3 |
| Week 5 (22 Aug) | Early Vascular | Placenta | Lab 4 |
| Week 6 (29 Aug) | Gastrointestinal | Respiratory | Lab 5 |
| Week 7 (5 Sep) | Head | Neural Crest | Lab 6 |
| Week 8 (12 Sep) | Musculoskeletal | Limb Development | Lab 7 |
| Week 9 (19 Sep) | Renal | Genital | Lab 8 |
| Mid-semester break | |||
| Week 10 (3 Oct) | Public Holiday | Stem Cells | Lab 9 |
| Week 11 (10 Oct) | Integumentary | Endocrine | Lab 10 |
| Week 12 (17 Oct) | Heart | Sensory | Lab 11 |
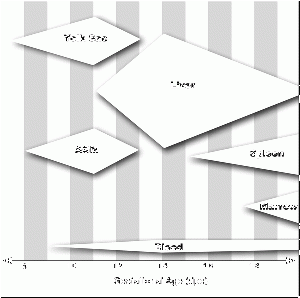
| Week 13 (24 Oct) | Fetal | Birth and Revision | Lab 12 |
|
ANAT2341 2016: Moodle page | ECHO360 | Textbooks | Students 2016 | Projects 2016 | |||