BGDA Practical - Female Reproductive Tract Histology: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| (76 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
==Introduction== | ==Introduction== | ||
[[File: | [[File:Human_right_ovary_and_tube_1.jpg|thumb|200px|Adult human ovary peritoneal surface (viewed by endoscopy)]] | ||
[[File:BGDsmall.jpg|left]] This current page provides background support information for Medicine phase 1 BGD Histology Practical Virtual Slides. Page does not form part of the BGDA practical class virtual slides. | [[File:BGDsmall.jpg|left]] This current page provides background support information for Medicine phase 1 BGD Histology Practical Virtual Slides. Page does not form part of the BGDA practical class virtual slides. | ||
<br> | |||
<br> | |||
{| | |||
| [[File:Moodle icon2.jpg|link=http://moodle.telt.unsw.edu.au/mod/book/view.php?id=853422]] | |||
| [http://moodle.telt.unsw.edu.au/mod/book/view.php?id=853422 Moodle Lab Slides - Female Reproductive Tract] | |||
Small Moodle icon links appearing below on this page go directly to the Lab Slide.<br>(you must be logged in to Moodle) | |||
Slides: [http://moodle.telt.unsw.edu.au/mod/book/view.php?id=853422 Female] | [http://moodle.telt.unsw.edu.au/mod/book/view.php?id=853422&chapterid=106729 Male] | [http://moodle.telt.unsw.edu.au/mod/book/view.php?id=853422&chapterid=106721 Placenta] | |||
|} | |||
{{Ref-WheatersHistology2006}} | |||
: | * [https://ebookcentral-proquest-com.wwwproxy1.library.unsw.edu.au/lib/unsw/reader.action?docID=1480022&ppg=363 Chapter 19 - Female Reproductive System] | ||
==Objectives== | ==Objectives== | ||
# Gain an overview of the microanatomy of the female reproductive system. | # Gain an overview of the microanatomy of the female reproductive system. | ||
# Undertake a microscopical examination of the ovary, oviduct, uterus, cervix, vagina and mammary | # Undertake a microscopical examination of the ovary, oviduct, uterus, cervix, vagina and mammary glands. The functional significance of the various histological structures identified will be discussed. | ||
glands. The functional significance of the various histological structures identified will be discussed. | |||
==Ovary== | ==Ovary== | ||
[[File: | The external surface of the {{ovary}} has a '''cuboidal epithelium''' (germinal epithelium) overlying a '''dense connective tissue''' layer (tunica albuginea). The outer epithelium is continuous with the peritoneum (serosa) forming a peritoneal fold (mesovarium) between the anterior border of the ovary with the posterior layer of the broad ligament of the uterus. | ||
Ovary structure (regions) | |||
* '''cortex''' - cellular connective tissue containing the developing follicles. | |||
* '''medulla''' - loose connective tissue containing blood vessels, lymphatics and nerves. | |||
===Ovarian Follicle=== | |||
{| | |||
| | |||
Beginning at puberty, the ovarian primordial follicle goes through a number of developmental stages leading to the release of an oocyte at ovulation at about the middle of the menstrual cycle. | |||
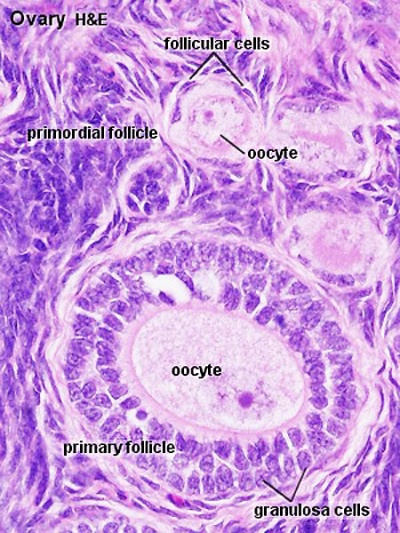
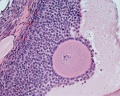
====Primordial Follicle==== | |||
* located in the cortex just beneath tunica albuginea. | |||
* One layer of flattened follicular cells surround the oocyte (about 30 µm in diameter). | |||
* nucleus of the oocyte is positioned eccentric in the cell. It appears very light and contains a prominent nucleolus. | |||
* most organelles of the oocyte aggregate in the centre of the cell, where they form the vitelline body. | |||
====Primary Follicle==== | |||
(preantral) | |||
* first morphological stage that marks the onset of follicular maturation | |||
* previously flattened cell surrounding the oocyte now form a cuboidal or columnar epithelium surrounding the oocyte. | |||
** cytoplasm has a granular appearance, reason also called '''granulosa cells'''. | |||
* continued proliferation of these cells will result in the formation of a stratified epithelium (with a distinct basement membrane) surrounding the oocyte. | |||
* '''zona pellucida''' becomes visible. | |||
** extracellular matrix formed by glycoproteins between interdigitating processes of oocyte and granulosa cells. | |||
* parenchymal cells of the ovary surrounding the growing follicle become organised in concentric sheaths, the '''theca folliculi'''. | |||
| [[File:Ovary follicle 01.jpg|400px]] | |||
|- | |||
| | |||
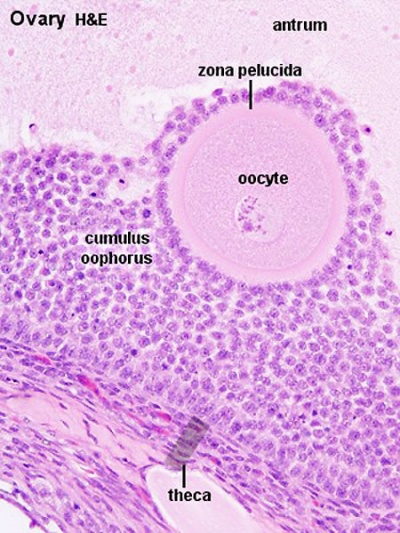
====Secondary Follicle==== | |||
(antral) | |||
* small fluid-filled spaces become visible between the granulosa cells as the follicle reaches a diameter of about 400 µm. | |||
* spaces enlarge and fuse to form the '''follicular antrum''' | |||
** defining feature of the secondary follicle. | |||
* oocyte is now located on one wall of the follicle in the '''cumulus oophorus'''. | |||
* theca folliculi differentiates to form 2 layers the '''theca interna''' and a '''theca externa''' | |||
** theca interna - spindle-shaped or polyhedral cells start to produce estrogens (also increased vascularization). | |||
** theca externa - highly cellular connective tissue with smooth muscle cells. | |||
* oocyte of the secondary follicle reaches a diameter of about 125 µm. | |||
* follicle itself reaches a diameter of about 10-15 mm. | |||
====Preovulatory Follicle==== | |||
(Graafian, tertiary, mature follicle) | |||
* increases further in size (in particular in the last 12h before ovulation). | |||
* '''stigma''' (macula pellucida) ovarian surface swelling formed by enlarging follicle. | |||
** thinning of the capsule, progressive restriction of the blood flow. | |||
* prior to ovulation the cumulus oophorus separates from the follicular wall. | |||
* oocyte floats freely in the follicular antrum, follicular fluid. | |||
** still surrounded by granulosa cells which form the corona radiata. | |||
* '''Ovulation''' - follicle ruptures at the stigma, oocyte, supporting cells and follicular fluid released from the ovary. | |||
| [[File:Ova20he.jpg|400px]] | |||
|} | |||
===Corpus Luteum=== | |||
{| | |||
| | |||
* The {{corpus luteum}} cells work together in the production of ovarian hormones that support the initial pregnancy. | |||
* Initial growth of the corpus luteum requires leutenizing hormone ( LH) from the adenohypophysis. | |||
* Later growth of the corpus luteum requires human chorionic gonadotrophin (hCG) from the implanting conceptus (trophoblast cells). | |||
* Progesterone is synthesized from cholesterol by both the large and small luteal cells upon luteal maturation. | |||
====Theca Lutein Cells==== | |||
* the darker stained cells. | |||
* derived from the theca interna of the original follicle. | |||
* lack microvilli on the surface. | |||
* lack the aromatase enzyme. | |||
* produce androgens for the granulosa lutein cells to convert. | |||
====Granulosa Lutein Cells==== | |||
* the lighter stained cells. | |||
* derived from the granulosa cells of the original follicle. | |||
* contain aromatase enzyme. | |||
* produce estrogen and progesterone from the androgens produced by the theca lutein cells. | |||
<gallery> | |||
Ovary corpus luteum.jpg|ovary overview | |||
File:Corpus luteum.jpg|low power | |||
File:Ovary_histology_002.jpg|theca and granulosa lutein cells | |||
</gallery> | |||
{{Corpus luteum links}} | |||
| [[File:Corpus_luteum_lutein_cells.jpg|400px]] | |||
|} | |||
===Corpus Albicans=== | |||
[[File:Ovary_histology_003.jpg|corpus albicans|thumb|corpus albicans]] | |||
Hormone secretion in the corpus luteum ceases within 14 days after ovulation if the oocyte is not fertilised. In this case, the corpus luteum degenerates into a corpus albicans - whitish scar tissue within the ovaries. | |||
===Ovary Histology=== | |||
<gallery> | <gallery> | ||
File:Ovary_histology_007.jpg|Tunica Albuginea x20 | File:Ovary_histology_007.jpg|Tunica Albuginea x20 | ||
| Line 26: | Line 124: | ||
File:Ovary_histology_003.jpg|Corpus albicans, primary follicle, primordial follicle, granulosa cells, oocyte x20 | File:Ovary_histology_003.jpg|Corpus albicans, primary follicle, primordial follicle, granulosa cells, oocyte x20 | ||
</gallery> | </gallery> | ||
==Uterine Tube== | ==Uterine Tube== | ||
(oviduct, Fallopian tube) | (oviduct, Fallopian tube) | ||
* uterine tube acts as a conduit for the oocyte, from the ovaries to the uterus. | * uterine tube acts as a conduit for the oocyte, from the ovaries to the uterus. | ||
* consists of a mucosa and a muscularis. | * consists of a mucosa and a muscularis. | ||
* peritoneal surface of the oviduct is lined by a serosa and subjacent connective tissue. | * peritoneal surface of the oviduct is lined by a serosa and subjacent connective tissue. | ||
{| | |||
! Overview | |||
! Mucosa | |||
|- | |||
| [[File:Uterine_tube_histology_02.jpg|350px]] | |||
| [[File:Uterine_tube_histology_03.jpg|350px]] | |||
|- | |||
| width=350px| | |||
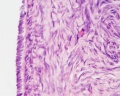
===Muscularis=== | |||
* inner circular muscle layer and an outer longitudinal layer. | |||
* inner longitudinal layer is present in the isthmus and the intramural part. | |||
* peristaltic muscle action for the transport of spermatozoa and oocyte. | |||
| width=350px| | |||
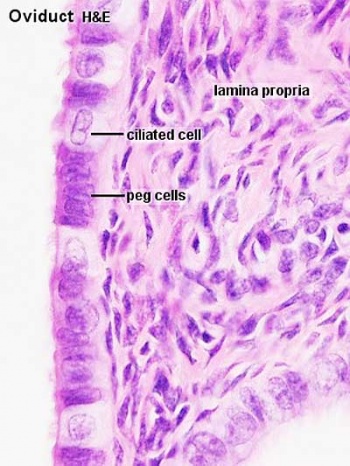
===Mucosa=== | ===Mucosa=== | ||
* ciliated and secretory epithelium resting on a cellular lamina propria. | * ciliated and secretory epithelium resting on a cellular lamina propria. | ||
* number of ciliated cells and secretory cells varies along the tube. | * number of ciliated cells and secretory cells varies along the tube. | ||
* secretory activity varies during the menstrual cycle, and resting secretory cells are also referred to as peg-cells. Some of the secreted substances are thought to nourish the oocyte and the very early embryo. | ** also varied by ovarian hormones during menstrual cycle. | ||
* secretory activity varies during the menstrual cycle, and resting secretory cells are also referred to as '''peg-cells'''. Some of the secreted substances are thought to nourish the oocyte and the very early embryo. | |||
|} | |||
===Tube Regions=== | ===Tube Regions=== | ||
{ | {{Uterine Tube Regions table}} | ||
==Uterus== | ==Uterus== | ||
| Line 79: | Line 179: | ||
* only the uterus body mucosa takes part in the menstrual cycle. | * only the uterus body mucosa takes part in the menstrual cycle. | ||
* endometrial layers (based on changes) | * endometrial layers (based on changes) | ||
# basalis - remains during menstruation, functions as a regenerative zone for the functionalis. | # '''basalis''' - remains during menstruation, functions as a regenerative zone for the functionalis. | ||
# functionalis - lost during menstruation, functions as the site of cyclic changes in the endometrium. | # '''functionalis''' - lost during menstruation, functions as the site of cyclic changes in the endometrium. | ||
<gallery> | |||
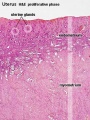
File:Uterus proliferative phase.jpg|Proliferative phase | |||
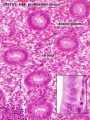
File:Uterine_gland_proliferative_phase.jpg|Gland - proliferative phase | |||
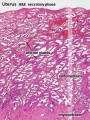
File:Uterus_secretory_phase.jpg|Secretory phase | |||
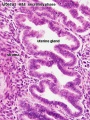
File:Uterine_gland_secretory_phase.jpg|Gland - secretory phase | |||
</gallery> | |||
* '''secretory phase''' - corpus luteum hormone (progesterone) after ovulation promotes production and secretion by the endometrial glands. | |||
{{Uterus_Histology}} | |||
:'''Links:''' [[Menstrual Cycle - Histology]] | |||
==Vagina== | |||
'''Virtual slides''' - [https://www.best.edu.au/s/mjzifezx vagina] | |||
{| | |||
| valigh=top|The wall of the vagina fibromuscular tube consists of 3 layers: | |||
# mucosa | |||
# muscularis | |||
# adventitia | |||
===Mucosa=== | |||
* stratified squamous nonkeratinized epithelium | |||
** deep stratum basalis, intermediate stratum spinosum, superficial layers of flat eosinophilic cells. | |||
** glycogen acted upon by lactobacillus acidophilus to acidify lumen. | |||
** rests on a cellular lamina propria (many leukocytes). | |||
* towards the muscularis some vascular cavernous spaces may be seen (erectile tissue). | |||
===Muscularis=== | |||
* inner circular and outer longitudinal layers of smooth muscle | |||
* '''bulbospongiosus muscle''' - (striated) forms an inferior sphincter around the vagina | |||
===Adventitia=== | |||
* adventitia bordering the muscularis is fairly dense and contains many elastic fibres. | |||
* outer part of the adventitia loose connective tissue with a prominent venous plexus. | |||
| [[File:Vagina_histology_01.jpg|400px]] | |||
|} | |||
==Mammary Gland== | |||
[[File:Mammary_anatomy.jpg|thumb|Adult female mammary anatomy cartoon]] | |||
'''Virtual slides''' - [https://www.best.edu.au/s/z31stgyf Mammary gland inactive] | [https://www.best.edu.au/s/f5lx5kkg Mammary gland active] | |||
The mammary glands are modified glands of the skin and their development is similar to that of sweat glands. | |||
* compound branched alveolar glands, secretory unit is the '''alveolus''' | |||
* consist of 15-25 lobes separated by dense interlobar connective tissue and fat. | |||
* each lobe contains an individual gland. | |||
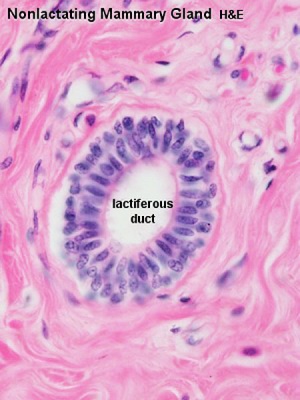
* lactiferous duct - excretory duct of each lobe with own opening on the nipple. | |||
===Alveolus=== | |||
* inner layer of cuboidal '''secretory epithelial cells''' | |||
** apocrine secretion - lipids | |||
** merocrine secretion - proteins (exocytosis) | |||
* outer layer of '''myoepithelial cells''' | |||
** located between the secretory cells and the surrounding basal lamina. | |||
** contraction helps force the milk from the secretory alveoli into the ducts. | |||
Note - plasma cells in the stroma also secrete antibodies (dimeric IgA) and released into the milk, to provides passive immunity to the suckling young. | |||
{| | |||
! width=305px|Lactiferous duct | |||
! width=305px|Lactating mammary gland | |||
! Apocrine secretion | |||
|- | |||
| [[File:Lactiferous_duct_01.jpg|300px]] | |||
| [[File:Mammary_gland_01.jpg|300px]] | |||
| width=200px|[[File:Apocrine secretion animation.gif|150px]] | |||
|} | |||
:'''Links:''' {{mammary gland}} | {{milk}} | |||
==Terms== | |||
* '''corona radiata''' - layer of cells of cumulus oophorus remaining attached to zona pellucida of oocyte after ovulation. | |||
* '''corpus''' - (Latin, ''corpus'' = body). | |||
* '''corpus albicans''' - (Latin, ''corpus'' = body + ''albicans'' = "whitish") a degenerating corpus luteum in the ovary. | |||
* '''{{corpus luteum}}''' - (Latin, ''corpus'' = body + ''luteum'' = yellow) major endocrine organ which is the remains of ovarian follicle after ovulation; yellow in ovary of cow where de Graaf (q.v.) first saw it. | |||
* '''cortex''' - (Latin = rind, or bark) outer layer of an organ. | |||
* '''cumulus oophorus''' - (Latin = ''cumulus'' = a little mound + Greek ''oon'' = egg + ''phorus'' = bearing) part of the wall of an ovarian follicle surrounding and carrying the oocyte. | |||
* '''fimbria''' - (Latin, ''fimbria'' = a fringe) the fringed open ovarian end of the uterine tube. | |||
* '''follicle''' - (Latin, ''folliculus'' = little bag). | |||
* '''hilum''' - or hilus (Latin,= a trifle; depression in a seed) a depression at vascular entrance/exit of a gland or organ. | |||
* '''lactobacillus acidophilus''' (Latin ''acid-loving milk-bacillus'') gram positive bacteria that grows readily at low pH (below pH 5.0) and ferment sugars into lactic acid. | |||
* '''mesothelium''' - epithelium (serosa) that lines the peritoneum, pleurae, and pericardium. Embryonically derived from epithelialisation of {{mesoderm}}. | |||
* '''mesovarium''' - short peritoneal fold connecting the anterior border of the ovary with the posterior layer of the broad ligament of the uterus. | |||
* '''medulla''' - (Latin, ''medulla'' = pith, marrow) the inner portion of an organ, in contrast to cortex. | |||
* '''menstrual''' - (Latin, ''menstruus'' = monthly) relating to the monthly female sexual cycle. | |||
* '''mucosa''' - (Latin, = mucous membrane) thin layer which lines body cavities and passages formed by epithelium and lamina propria. | |||
* '''{{oocyte}}''' - (Greek, ''öon'' = egg + ''kytos'' = hollow vessel (cell) the female germ cell in the {{ovary}}. | |||
* '''parenchyma''' - (Greek," + enkeim = to pour in) the essential functional cells of an organ as opposed to its stroma. | |||
* '''salpinx''' - (Greek, = a trumpet) the uterine tube. | |||
* '''serosa''' - (Latin, ''serum'' = whey; a pale fluid) a serous membrane lining body cavities. | |||
* '''stroma''' - (Greek, = a cover, table-cloth, bedding) term for the internal supporting frame-work of a tissue, or organ, as opposed to its parenchyma. | |||
* '''tunica albuginea''' - a dense, white, fibrous sheath enclosing a part or organ. | |||
* '''uterine tube''' - (oviduct, Fallopian tube) | |||
* '''{{uterus}}''' - (Latin, = womb, from ''uter'' = a large goatskin bag used as a wine-skin). | |||
* '''zona pellucida''' - (Latin, ''zona'' = a girdle + ''perlucere'' = to shine through) the refractile layer of glycoclayx (ECM) surrounding oocyte in a growing ovarian follicle. | |||
{{Histology Glossary}} | |||
==Additional Information== | |||
<br> | |||
{{Med Prac additional Information}} | |||
===Development=== | |||
'''Links:''' {{female}} | {{ovary}} | {{oocyte}} | {{uterus}} | {{vagina}} | |||
===Follicle Classification=== | |||
Be aware that there are several different nomenclatures used for classifying the stages of follicle maturation. | |||
{{Follicle class table}} | |||
'''Ovarian reserve''' - refers to the number of oocytes available (for possible fertilization) at the different times during female reproductive life.{{#pmid:20111701|PMID20111701}} | |||
{| class="wikitable mw-collapsible mw-collapsed" | |||
! Oocyte terms | |||
|- | |||
| {{Oocyte terms}} | |||
|} | |||
===Mammary Gland=== | |||
{{Tanner stages collapse table}} | |||
<br> | |||
After the infant ceases breast feeding, weaning, the mammary gland milk-producing epithelial cells undergo a process called "involution", that requires cell {{apoptosis}} (programmed cell death). | |||
[[File:Mammary_involution.jpg|400px]] | |||
===Breast Cancer=== | |||
In 1994, two breast cancer susceptibility genes were identified BRCA1 on chromosome {{Chr17}} and BRCA2 on chromosome {{Chr13}}. | |||
When an individual carries a mutation in either BRCA1 or BRCA2, they are at an increased risk of being diagnosed with breast or ovarian cancer at some point in their lives. Normal function of these genes was to participate in repairing radiation-induced breaks in double-stranded DNA. It is though that mutations in BRCA1 or BRCA2 might disable this mechanism, leading to more errors in DNA replication and ultimately to cancerous growth. (text modified from: NCBI genes and disease) | |||
==References== | |||
<references/> | |||
{{BGDAFooter}} | |||
Latest revision as of 11:45, 3 June 2019
Introduction
This current page provides background support information for Medicine phase 1 BGD Histology Practical Virtual Slides. Page does not form part of the BGDA practical class virtual slides.
| Moodle Lab Slides - Female Reproductive Tract
Small Moodle icon links appearing below on this page go directly to the Lab Slide. |
Young, B., Lowe, J., Stevens, A. & Heath, J. (2006) Wheater’s Functional Histology. A Text and Colour Atlas 5th ed. Churchill Livingstone, Edinburgh. ISBN 0-443-06850X. UNSW Online
Objectives
- Gain an overview of the microanatomy of the female reproductive system.
- Undertake a microscopical examination of the ovary, oviduct, uterus, cervix, vagina and mammary glands. The functional significance of the various histological structures identified will be discussed.
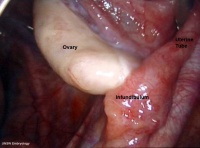
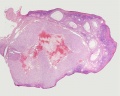
Ovary
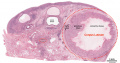
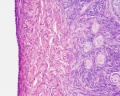
The external surface of the ovary has a cuboidal epithelium (germinal epithelium) overlying a dense connective tissue layer (tunica albuginea). The outer epithelium is continuous with the peritoneum (serosa) forming a peritoneal fold (mesovarium) between the anterior border of the ovary with the posterior layer of the broad ligament of the uterus.
Ovary structure (regions)
- cortex - cellular connective tissue containing the developing follicles.
- medulla - loose connective tissue containing blood vessels, lymphatics and nerves.
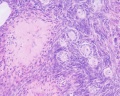
Ovarian Follicle
Corpus Luteum
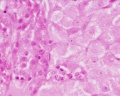
Theca Lutein Cells
Granulosa Lutein Cells
|

|
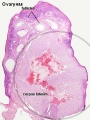
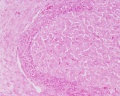
Corpus Albicans
Hormone secretion in the corpus luteum ceases within 14 days after ovulation if the oocyte is not fertilised. In this case, the corpus luteum degenerates into a corpus albicans - whitish scar tissue within the ovaries.
Ovary Histology
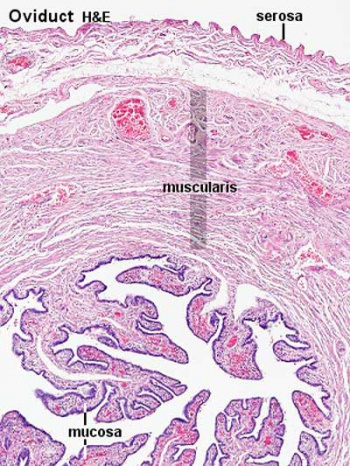
Uterine Tube
(oviduct, Fallopian tube)
- uterine tube acts as a conduit for the oocyte, from the ovaries to the uterus.
- consists of a mucosa and a muscularis.
- peritoneal surface of the oviduct is lined by a serosa and subjacent connective tissue.
Tube Regions
Uterus
- parts - body (upper two-thirds) and cervix.
- walls - mucosal layer, the endometrium, and a fibromuscular layer, the myometrium.
- peritoneal surface of the uterus is covered by a serosa.
Myometrium
- smooth muscle fibres form several layers with preferred orientations.
- muscular tissue hypertrophies during pregnancy.
- GAP-junctions between cells become more frequent.
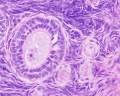
Endometrium
- simple columnar epithelium (ciliated cells and secretory cells) and an underlying thick connective tissue stroma.
- mucosa is invaginated to form many simple tubular uterine glands.
- glands extend through the entire thickness of the stroma.
- stromal cells of the endometrium are embedded in a network of reticular fibres.
Menstrual cycle
- hormones alter the endometrium.
- only the uterus body mucosa takes part in the menstrual cycle.
- endometrial layers (based on changes)
- basalis - remains during menstruation, functions as a regenerative zone for the functionalis.
- functionalis - lost during menstruation, functions as the site of cyclic changes in the endometrium.
- secretory phase - corpus luteum hormone (progesterone) after ovulation promotes production and secretion by the endometrial glands.
- Uterus Histology Links: Labeled - proliferative phase | Labeled - gland proliferative phase | Labeled - secretory phase | Unlabeled - secretory phase | Unlabeled - late secretory phase | Labeled - gland secretory phase | Menstrual Cycle | Uterine Gland | Uterus Development
- Links: Menstrual Cycle - Histology
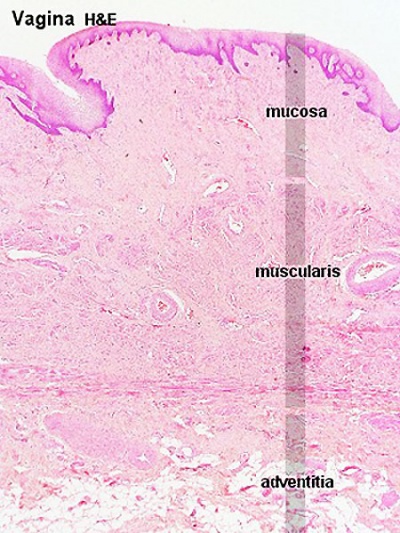
Vagina
Virtual slides - vagina
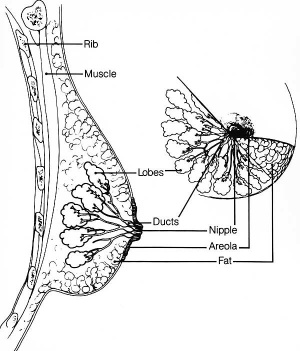
Mammary Gland
Virtual slides - Mammary gland inactive | Mammary gland active
The mammary glands are modified glands of the skin and their development is similar to that of sweat glands.
- compound branched alveolar glands, secretory unit is the alveolus
- consist of 15-25 lobes separated by dense interlobar connective tissue and fat.
- each lobe contains an individual gland.
- lactiferous duct - excretory duct of each lobe with own opening on the nipple.
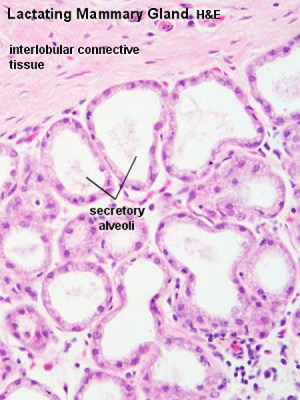
Alveolus
- inner layer of cuboidal secretory epithelial cells
- apocrine secretion - lipids
- merocrine secretion - proteins (exocytosis)
- outer layer of myoepithelial cells
- located between the secretory cells and the surrounding basal lamina.
- contraction helps force the milk from the secretory alveoli into the ducts.
Note - plasma cells in the stroma also secrete antibodies (dimeric IgA) and released into the milk, to provides passive immunity to the suckling young.
| Lactiferous duct | Lactating mammary gland | Apocrine secretion |
|---|---|---|
|
|

|
- Links: mammary gland | milk
Terms
- corona radiata - layer of cells of cumulus oophorus remaining attached to zona pellucida of oocyte after ovulation.
- corpus - (Latin, corpus = body).
- corpus albicans - (Latin, corpus = body + albicans = "whitish") a degenerating corpus luteum in the ovary.
- corpus luteum - (Latin, corpus = body + luteum = yellow) major endocrine organ which is the remains of ovarian follicle after ovulation; yellow in ovary of cow where de Graaf (q.v.) first saw it.
- cortex - (Latin = rind, or bark) outer layer of an organ.
- cumulus oophorus - (Latin = cumulus = a little mound + Greek oon = egg + phorus = bearing) part of the wall of an ovarian follicle surrounding and carrying the oocyte.
- fimbria - (Latin, fimbria = a fringe) the fringed open ovarian end of the uterine tube.
- follicle - (Latin, folliculus = little bag).
- hilum - or hilus (Latin,= a trifle; depression in a seed) a depression at vascular entrance/exit of a gland or organ.
- lactobacillus acidophilus (Latin acid-loving milk-bacillus) gram positive bacteria that grows readily at low pH (below pH 5.0) and ferment sugars into lactic acid.
- mesothelium - epithelium (serosa) that lines the peritoneum, pleurae, and pericardium. Embryonically derived from epithelialisation of mesoderm.
- mesovarium - short peritoneal fold connecting the anterior border of the ovary with the posterior layer of the broad ligament of the uterus.
- medulla - (Latin, medulla = pith, marrow) the inner portion of an organ, in contrast to cortex.
- menstrual - (Latin, menstruus = monthly) relating to the monthly female sexual cycle.
- mucosa - (Latin, = mucous membrane) thin layer which lines body cavities and passages formed by epithelium and lamina propria.
- parenchyma - (Greek," + enkeim = to pour in) the essential functional cells of an organ as opposed to its stroma.
- salpinx - (Greek, = a trumpet) the uterine tube.
- serosa - (Latin, serum = whey; a pale fluid) a serous membrane lining body cavities.
- stroma - (Greek, = a cover, table-cloth, bedding) term for the internal supporting frame-work of a tissue, or organ, as opposed to its parenchyma.
- tunica albuginea - a dense, white, fibrous sheath enclosing a part or organ.
- uterine tube - (oviduct, Fallopian tube)
- uterus - (Latin, = womb, from uter = a large goatskin bag used as a wine-skin).
- zona pellucida - (Latin, zona = a girdle + perlucere = to shine through) the refractile layer of glycoclayx (ECM) surrounding oocyte in a growing ovarian follicle.
- Histology Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | ANAT2241 Support | Histology | Histology Stains | Embryology Glossary
Additional Information
| Additional Information - Content shown under this heading is not part of the material covered in this class. It is provided for those students who would like to know about some concepts or current research in topics related to the current class page. |
Development
Links: Female | ovary | oocyte | uterus | vagina
Follicle Classification
Be aware that there are several different nomenclatures used for classifying the stages of follicle maturation.
| Class | Alternate nomenclature | Type | Number of Cells | Size (diameter µm) | Size ultrasound (mm) |
|---|---|---|---|---|---|
| primordial follicle | small | 1, 2, 3 | 25 | less than 50 | |
| primary follicle | preantral | 4 5 |
26 - 100 101 - 300 |
up to 200 | |
| secondary follicle | antral small antral large antral |
6 7 |
3001 - 500 501 - 1000 |
500 1000 - 6000 |
less than 18 |
| preovulatory follicle | Graafian | 8 | greater than 1000 | greater than 6000 | 18 – 28 |
| Links: ovary | oocyte | menstrual cycle | |||||
Ovarian reserve - refers to the number of oocytes available (for possible fertilization) at the different times during female reproductive life.[1]
| Oocyte terms | ||
|---|---|---|
| Oocyte Development
Note there are additional specific term glossaries available listed at bottom of this table.
|
Mammary Gland
| Tanner Stages (Expand to open) | ||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||
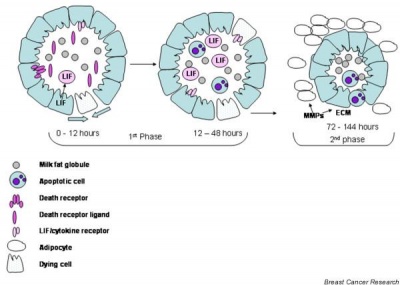
After the infant ceases breast feeding, weaning, the mammary gland milk-producing epithelial cells undergo a process called "involution", that requires cell apoptosis (programmed cell death).
Breast Cancer
In 1994, two breast cancer susceptibility genes were identified BRCA1 on chromosome 17 and BRCA2 on chromosome 13.
When an individual carries a mutation in either BRCA1 or BRCA2, they are at an increased risk of being diagnosed with breast or ovarian cancer at some point in their lives. Normal function of these genes was to participate in repairing radiation-induced breaks in double-stranded DNA. It is though that mutations in BRCA1 or BRCA2 might disable this mechanism, leading to more errors in DNA replication and ultimately to cancerous growth. (text modified from: NCBI genes and disease)
References
- ↑ Wallace WH & Kelsey TW. (2010). Human ovarian reserve from conception to the menopause. PLoS ONE , 5, e8772. PMID: 20111701 DOI.
- ↑ Marshall WA & Tanner JM. (1969). Variations in pattern of pubertal changes in girls. Arch. Dis. Child. , 44, 291-303. PMID: 5785179
- ↑ Marshall WA & Tanner JM. (1970). Variations in the pattern of pubertal changes in boys. Arch. Dis. Child. , 45, 13-23. PMID: 5440182
BGDA: Lecture 1 | Lecture 2 | Practical 3 | Practical 6 | Practical 12 | Lecture Neural | Practical 14 | Histology Support - Female | Male | Tutorial
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, May 4) Embryology BGDA Practical - Female Reproductive Tract Histology. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/BGDA_Practical_-_Female_Reproductive_Tract_Histology
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G