Gastrointestinal Tract - Abnormalities: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 259: | Line 259: | ||
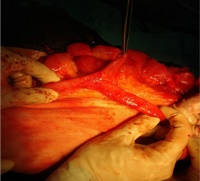
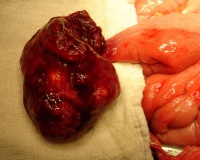
| [[File:Mark_Hill.jpg|90px|left]] This historic 1916 textbook by Cullen describes the umbilical region development and abnormalities including [[Book_-_Umbilicus_(1916)_8|Chapter 8]] on [[Book_-_Umbilicus_(1916)_8|Meckel's diverticulum]]. | | [[File:Mark_Hill.jpg|90px|left]] This historic 1916 textbook by Cullen describes the umbilical region development and abnormalities including [[Book_-_Umbilicus_(1916)_8|Chapter 8]] on [[Book_-_Umbilicus_(1916)_8|Meckel's diverticulum]]. | ||
<br> | <br> | ||
<gallery caption "[[Book_-_Umbilicus_(1916)_8|Chapter 8 Figures]]"> | |||
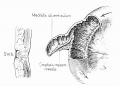
File:Cullen1916 fig92.jpg|92 Meckel's Diverticulum | |||
File:Cullen1916 fig93.jpg|93 Meckel's Diverticulum attached to abdominal wall | |||
File:Cullen1916 fig94.jpg|94 Large Meckel's Diverticulum | |||
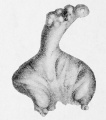
File:Cullen1916 fig95.jpg|95 Lobulated Extremity | |||
File:Cullen1916 fig96.jpg|96 Hernial Protrusions | |||
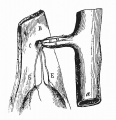
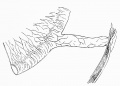
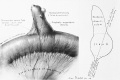
File:Cullen1916 fig97.jpg|97 Short Meckel's Diverticulum] | |||
File:Cullen1916 fig98.jpg|98 Accessory Pancreas | |||
File:Cullen1916 fig99.jpg|99 Meckel's Diverticulum Tying Loop of Small Bowel | |||
File:Cullen1916 fig100.jpg|100 Diverticulum Tying off Loop of Small Bowel | |||
File:Cullen1916 fig101.jpg|101 Ileum Volvulus | |||
File:Cullen1916 fig102.jpg|102 Fatal Intestinal Obstruction | |||
File:Cullen1916 fig103.jpg|103 Meckel's Diverticulum Inversion | |||
</gallery> | |||
|- | |- | ||
|} | |} | ||
Revision as of 07:10, 29 October 2018
| Embryology - 17 Jun 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
The "simple tube" of the gastrointestinal tract and its associated organs have many different tract and organ specific gastrointestinal abnormalities. Due to the complex nature (different germ layer contributions, organogenisis) of the growth, elongation and folding of the tract, there are also several mechanical disorders of folding (rotation). Musculoskeletal abnormalities of the anterior body wall can also result in gastrointestinal abnormalities.
Note that as this system begins function (digestively) postnatally, unless there is a determined genetic history within the family, several abnormalities only become evident postnatally, in particular, metabolic disorders often identified by the Guthrie test.
International Classification of Diseases
| ICD10 Other congenital malformations of the digestive system (Q38-Q45) | ||||||
|---|---|---|---|---|---|---|
| XVII Congenital Malformations - Other congenital malformations of the digestive system (Q38-Q45) | ||||||
| Q38 Other congenital malformations of tongue, mouth and pharynx
Excl.: macrostomia (Q18.4) microstomia (Q18.5)
| ||||||
Q39 Congenital malformations of oesophagus
| ||||||
Q40 Other congenital malformations of upper alimentary tract
| ||||||
| Q41 Congenital absence, atresia and stenosis of small intestine
Incl.: congenital obstruction, occlusion and stricture of small intestine or intestine NOS Excl.: meconium ileus (E84.1)
| ||||||
| Q42 Congenital absence, atresia and stenosis of large intestine
Incl.: congenital obstruction, occlusion and stricture of large intestine
| ||||||
Q43 Other congenital malformations of intestine
| ||||||
Q44 Congenital malformations of gallbladder, bile ducts and liver
| ||||||
| Q45 Other congenital malformations of digestive system
Excl.: congenital: diaphragmatic hernia (Q79.0) hiatus hernia (Q40.1)
| ||||||
|
World Health Organisation. International Statistical Classification of Diseases and Related Health Problems. (1992) 10th Revision (ICD-10). Geneva: WHO ICD-10 - 2016 Online (English) | ||||||
Links: Gastrointestinal Abnormalities
| ||||||
| ICD10 - Gastrointestinal | Genital | Renal | Integumentary |
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Abnormal Development Gastrointestinal Tract <pubmed limit=5>Abnormal Development Gastrointestinal Tract</pubmed> |
Movies
|
|
|
|
Statistics
Australian
|
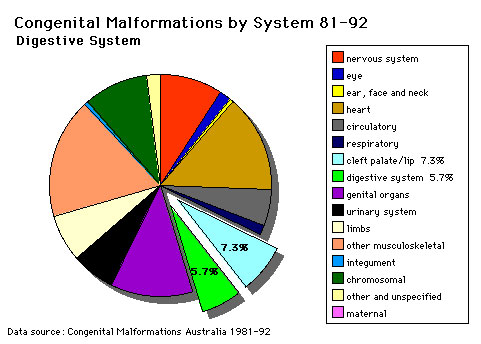
The pie diagram shows the relative contribution of major gastrointestinal tract abnormalities as a percentage of the total number of congenital abnormalities in Australia beween 1981 - 92.
Note that the digestive system represents approximately 6% of all major congenital abnormalities. One of the most common abnormalities occurring in (2% - 3% population) is Meckel's Diverticulum. The mouth (cleft lip, cleft palate) is part of the digestive tract, but more accurately reflects an abnormality of face formation. |
| Data shown as a percentage of all major abnormalities based upon published statistics using the same groupings as Congenital Malformations Australia 1981-1992 P. Lancaster and E. Pedisich ISSN 1321-8352. |
| Australian GIT Abnormalities (2002-2003) |
|---|
Oesophageal atresia/stenosis - (2.0 per 10,000 births) ICD-10 Q39.0–Q39.3
|
Small intestinal atresia/stenosis - (2.4 per 10,000 births) ICD-10 Q41.0-Q41.2
|
Anorectal atresia/stenosis - ( 3.1 per 10,000 births) ICD-10 Q42.0–Q42.3
|
Hirschsprung’s disease - (1.3 per 10,000 births) ICD-10 Q43.1
|
Exomphalos - (Omphalocele) (2.1 per 10,000 births) ICD-10 Q79.2
|
Gastroschisis - (2.6 per 10,000 births) ICD-10 Q79.3
|
|
| Australian Palate Abnormalities (2002-2003) |
|---|
| Cleft lip with or without cleft palate (9.2 per 10,000 births) ICD-10 Q36.0, Q36.1, Q36.9, Q37.0–Q37.5, Q37.8, Q37.9 |
A congenital anomaly characterised by a partial or complete clefting of the upper lip, with or without clefting of the alveolar ridge or the hard palate. Excludes a midline cleft of the upper or lower lip and an oblique facial fissure (going towards the eye).
|
| Cleft palate without cleft lip (8.1 per 10,000 births) ICD-10 Q35.0–Q35.9 |
A congenital anomaly characterised by a closure defect of the hard and/or soft palate behind the foramen incisivum without a cleft lip. This anomaly includes sub-mucous cleft palate, but excludes cleft palate with a cleft lip, a functional short palate and high narrow palate.
|
|
USA Selected
CDC National estimates for selected GIT related major birth defects (2004–2006).
| Birth Defects | Cases per Births (1 in ...) | Estimated Annual Number of Cases |
|---|---|---|
| Cleft palate without cleft lip | 1,574 | 2,651 |
| Cleft lip with and without cleft palate | 940 | 4,437 |
| Esophageal atresia/tracheoesophageal fistula | 4,608 | 905 |
| Rectal and large intestinal atresia/stenosis | 2,138 | 1,952 |
| Gastroschisis | 2,229 | 1,871 |
| Omphalocele | 5,386 | 775 |
| Diaphragmatic hernia | 3,836 | 1,088 |
| Trisomy 21 (Down syndrome) | 691 | 6,037 |
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Abnormal Development Gastrointestinal Tract <pubmed limit=5>Abnormal Development Gastrointestinal Tract</pubmed> |
Lumen Abnormalities
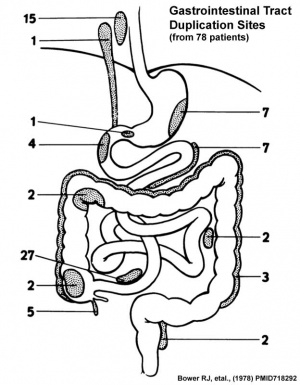
There are several types of abnormalities (atresia, stenosis and duplication) that impact upon the continuity of the gastrointestinal tract lumen.
Atresia
An interruption of the lumen (esophageal atresia, duodenal atresia, extrahepatic biliary atresia, anorectal atresia). See oesophageal Atresia review[7]
- Pyloric atresia (PA) - a very rare condition (incidence 1 in 100,000 newborns) and about 1% of all intestinal atresias.
| Oesophageal Atresia[8] | |
|---|---|
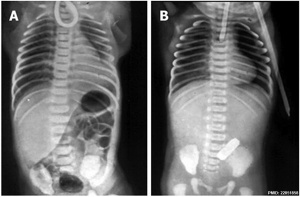
|
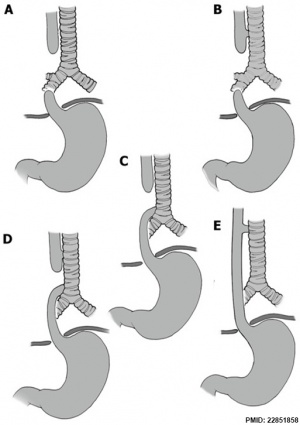
|
| Oesophageal atresia x-ray | Classification of Oesophageal atresia |
Stenosis
A narrowing of the lumen (esophageal stenosis, duodenal stenosis, pyloric stenosis)
- esophageal stenosis[9]
Duplication
An incomplete recanalization resulting in parallel lumens, this is really a specialized form of stenosis.
Oesophagus
The current International Classification of Diseases (ICD-10) code XVII Congenital Malformations Q39 Congenital malformations of oesophagus
- Q39.0 Atresia of oesophagus without fistula Atresia of oesophagus NOS
- Q39.1 Atresia of oesophagus with tracheo-oesophageal fistula Atresia of oesophagus with broncho-oesophageal fistula
- Q39.2 Congenital tracheo-oesophageal fistula without atresia Congenital tracheo-oesophageal fistula NOS
- Q39.3 Congenital stenosis and stricture of oesophagus
- Q39.4 Oesophageal web
- Q39.5 Congenital dilatation of oesophagus
- Q39.6 Diverticulum of oesophagus Oesophageal pouch
- Q39.8 Other congenital malformations of oesophagus Absent Congenital displacement Duplication (of) oesophagus
- Q39.9 Congenital malformation of oesophagus, unspecified
Note ICD-10 is currently being updated to ICD-11 and will have new replacement coding.
Oesophageal Atresia with Tracheo-Oesophageal Fistula
(Q39.1 Atresia of oesophagus with tracheo-oesophageal fistula Atresia of oesophagus with broncho-oesophageal fistula, OA/TOF)
- ICD-11 (beta) LB12.2 Atresia of oesophagus "Oesophageal atresia encompasses a group of congenital anomalies with an interruption in the continuity of the oesophagus, with or without persistent communication with the trachea. In 86% of cases there is a distal tracheooesophageal fistula, in 7% of cases there is no fistulous connection, while in 4% of cases there is a tracheooesophageal fistula without atresia. The remaining cases are made up of patients with OA with proximal, or both proximal and distal, tracheooesophageal fistula."
This abnormality has been shown to be associated with Tbx1 mutations that also include DiGeorge syndrome.[10]
Intestinal Malrotation
A recent study[11] has suggested that malrotation may result from the stunted embryonic development of intestinal secondary loops.
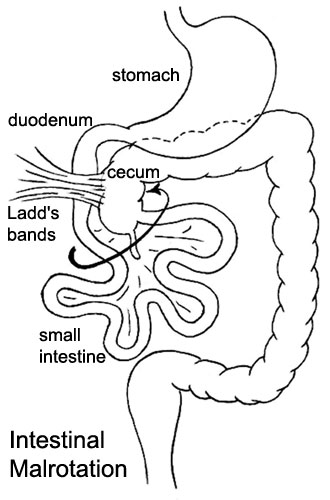
|
Presents clinically in symptomatic malrotation as:
Neonates - bilious vomiting and bloody stools. Newborn - bilious vomiting and failure to thrive. Infants - recurrent abdominal pain, intestinal obstruction, malabsorption/diarrhea, peritonitis/septic shock, solid food intolerance, common bile duct obstruction, abdominal distention, and failure to thrive. |
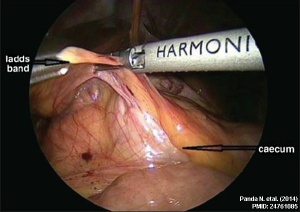
Ladd's Bands[12] A series of bands crossing the duodenum which can cause duodenal obstruction. |
Volvulus
Twisting of the midgut (bowel) which causes obstruction to the flow of material. Can include a variable loss of local blood supply which leads to tissue death.
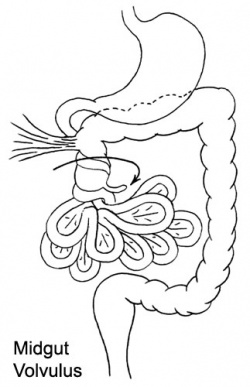
|
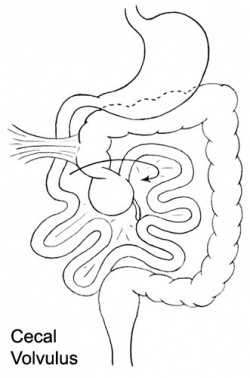
|
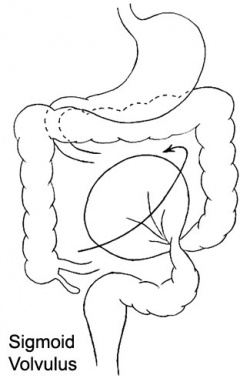
|
Diagnosis is generally by upper gastrointestinal radiologic examination or less frequently by barium enema or CT scan.
Corrective surgery is generally by the Ladd's procedure, even with surgical treatment there is still significant associated complications and long-term morbidity.
What abnormal embryological processes could interfere with normal rotation and fixation of the gut?
Search PubMed: intestinal+malrotation
OMIM: Volvulus of Midgut
Links: Medlineplus - childhood volvulus | AAFP - Bilious Vomiting in the Newborn | Pediatric education - Neonatal Bilious Emesis |
Situs Inversus Viscera
Disturbance of the lateralisation of the liver may produce transposition of some or all of the foregut and its derivatives.
Also in situs inversus the anatomical relations of the duodenum, pancreas, bile ducts and portal veins may be reversed or disordered.
Heterotaxia is a term used to describe the rare congenital defect where the major visceral organs are distributed left-right abnormally within the chest and abdomen.
Search PubMed: Situs Inversus Viscera | Heterotaxia
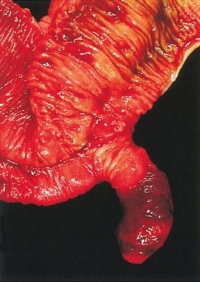
Meckel's Diverticulum
ICD-11 LB15.0 Meckel diverticulum
This GIT abnormality is a very common (incidence of 1–2% in the general population) and results from improper closure and absorption of the omphalomesenteric duct (vitelline duct) in development. This transient developmental duct connects the yolk to the primitive gastrointestinal tract.
In addition to Meckel's diverticulum there are a range of other vitelline duct abnormalities, which depend on the degree from a completely patent duct at the umbilicus to lesser remnants (cysts, fibrous cords connecting umbilicus to distal ileum, granulation tissue at umbilicus, or umbilical hernias).
| Historic Embryology |
|---|
| This historic 1916 textbook by Cullen describes the umbilical region development and abnormalities including Chapter 8 on Meckel's diverticulum.
|
- Links: Yolk Sac - Meckel's Diverticulum | OMIM - Meckel's Diverticulum | Pubmed - Meckel's Diverticulum | Pubmed - omphalomesenteric duct | Pubmed - vitelline duct
Intestinal Aganglionosis
(intestinal aganglionosis, Hirschsprung's disease, aganglionic colon, megacolon, congenital aganglionic megacolon, congenital megacolon) A condition caused by the lack of enteric nervous system (neural ganglia) in the intestinal tract responsible for gastric motility (peristalsis). In general, its severity is dependent upon the amount of the GIT that lacks intrinsic ganglia, due to developmental lack of neural crest migration into those segments. (More? Neural Crest System - Abnormalities)
Historically, Hirschsprung's disease takes its name from Dr Harald Hirschsprung (1830-1916) a Danish pediatrician (of German extraction). In 1886, he presented at the German Society of Pediatrics conference in Berlin a case of 2 infants who died of complications of bowel obstruction (H. Hirschsprung, Stuhltragheit Neugeborener in Folge von Dilatation und Hypertrophie des Colons, Jhrb f Kinderh 27 (1888), pp. 1-7). Later autopsies identified a dilatation and hypertrophy of large intestine, and the rectum appeared normally narrow. Hirschsprung suggested that the condition was an inborn disease and named it congenital megacolon.
The first indication in newborns is an absence of the first bowel movement, other symptoms include throwing up and intestinal infections. Clinically this is detected by one or more tests (barium enema and x ray, manometry or biopsy) and can currently only be treated by surgery. A temoporary ostomy (Colostomy or Ileostomy) with a stoma is carried out prior to a more permanent pull-through surgery.
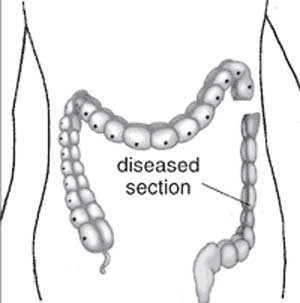
|

|
|
| Ostomy - Aganglionic portion removed | Stoma - intestine attached to the abdomen wall | |
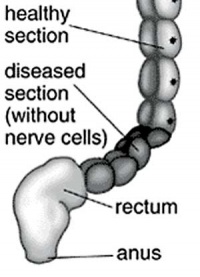
|
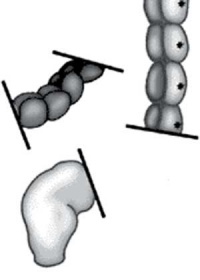
|
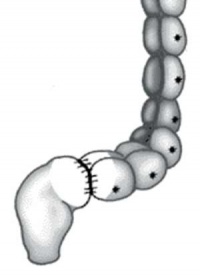
|
| Short section of the colon without smooth muscle neural ganglia | Aganglionic segment removed | Reattachment |
Images: NIH - NIDDK - Hirschsprungs
- Links: Enteric Nervous System | Neural Crest System - Abnormalities | NIH - NIDDK - Hirschsprungs | MedlinePlus - Hirschsprung's disease | OMIM 142623 | Search PubMed
Gastroschisis
By definition, gastroschisis is a body wall musculoskeletal defect, not a gastrointestinal tract defect, which in turn impacts upon GIT development.
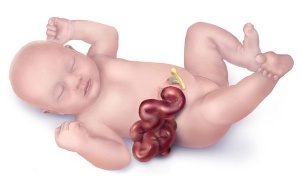
| Gastroschisis (paraomphalocele, laparoschisis, abdominoschisis, abdominal hernia) is an abdominal wall defect associated with evisceration of the intestine (2.5 cases/10,000 births), occuring more frequently in young mothers (less than 20 years old). There have been reports that this abnormality is increasing in incidence.
The abnormality is usually situated to the right of the umbilicus and abdominal contents, mainly gastrointestinal, are found outside the anterior body wall. International Classification of Diseases, 9th Revision diagnosis (756.79) and procedure (54.71) code for gastroschisis (2003 to 2008). |
|
| Can occur in isolation and also in association with other gastrointestinal anomalies (intestinal atresia, perforation, necrosis or volvulus). Defects in other organ systems have been reported in up to 35% of children. Both environments and genetic factors contribute to this disorder. Some studies suggest yolk sac and related vitelline structures[13] or a vascular disruption[14] or are associated with the pathogenesis. A study has also shown that herpesvirus does not play a role in the etiology of gastroschisis.[15]
| |
Gastroschisis patients are commonly small for gestational age (SGA, birth weight < 10th centile). Frequency line graphs of the birth weight distribution.[16]
|
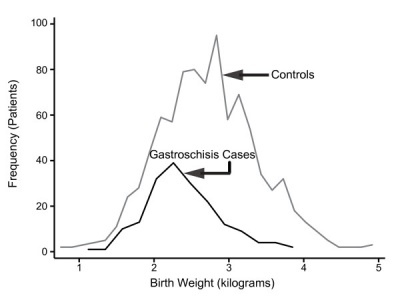
|
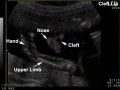
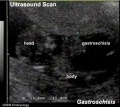
Gastroschisis Ultrasound
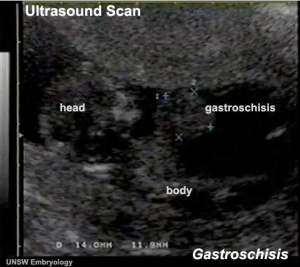
|
<html5media height="390" width="440">File:Gastroschisis 001.mp4</html5media> |
Gastroschisis Classification
There has been a recent attempt to classify gastroschisis in order to measure clinical outcomes.[17]
- Simple gastroschisis - intact continuous bowel that is not compromised or breached at delivery or presentation
- Complex gastroschisis - presence of one or more of intestinal atresia, perforation or intestinal necrosis at delivery or presentation, or missed atresia
Omphalocele
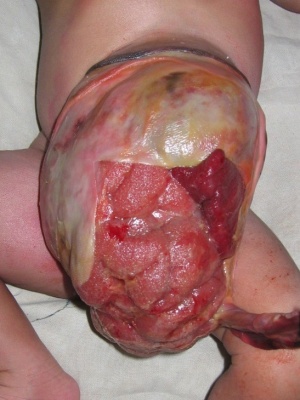
An abnormality appearing similar to gastroschisis, involves "covered by membranes" and a lack of normal return of the bowel to the abdominal cavity and has a different position relative to the umbilical cord. The origin differs, as this is a failure of midgut loops to return to the body cavity after initial herniation into the umbilical cord during week 6 - 10.
- omphalocele - herniation of the bowel, liver and other organs into the intact umbilical cord, the tissues being covered by membranes unless the latter are ruptured
- gastroschisis - intact umbilical cord and evisceration of the bowel through a defect in the abdominal wall, generally to the right of the cord, with no membrane covering
Short-Bowel Syndrome
Not generally a developmental abnormality, but related to therapeutic intervention in GIT abnormalities or disease.
Short bowel syndrome is a group of problems affecting people who have had half or more of their small intestine removed. The most common reason for removing part of the small intestine is to treat Crohn's disease. Short bowel syndrome is treated through changes in diet, intravenous feeding, vitamin and mineral supplements, and medicine to relieve symptoms. (NDDIC)
- Links: Better Health Short Bowel syndrome | National Digestive Diseases Information Clearinghouse Short Bowel syndrome
Obstetric Cholestasis
A recent paper in the British Medical Journal discusses this pregnancy associated disease.
"Obstetric cholestasis (or intrahepatic cholestasis of pregnancy) remains widely disregarded as an important clinical problem, with many obstetricians still considering its main symptom, pruritus, a natural association of pregnancy. Obstetric cholestasis is associated with cholesterol gallstones. It may be extremely stressful for the mother but also carries risks for the baby." Piotr Milkiewicz, Elwyn Elias, Catherine Williamson, and Judith Weaver BMJ 2002; 324: 123-124
Small Bowel Obstruction
The are two major forms of small bowel obstruction are from either external (extrinsic) or internal (intrinsic) causes. Listed below are a few examples of both causes.
- Extrinsic Causes - adhesions, closed loop, strangulation, hernia and extrinsic masses
- Intrinsic Causes - intestinal malrotation, Crohn disease, adenocarcinoma, tuberculosis, radiation enteropathy, intramural hemorrhage, intussusception and intraluminal causes.
(More? see PMID 11353110)
Necrotizing Enterocolitis
Necrotizing enterocolitis (NE) is the death of intestinal tissue that occurs postnatally in mainly in premature and low birth weight infants (1 in 2,000 - 4,000 births). The underdeveloped gastointestinal tract appears to be susceptible to bacteria, normally found within the tract,to spread widely to other regions where they damage the tract wall and may enter the bloodstream.
Those with a higher risk for this condition include:
- Premature infants
- Infants who are fed concentrated formulas
- Infants in a nursery where an outbreak has occurred
- Infants who have received blood exchange transfusions
Meconium Plug Syndrome
(functional immaturity of the colon) Term used to describe a transient disorder of the newborn colon, which is characterized by delayed passage of meconium (more than 24 to 48 h), intestinal dilatation and yellow/green vomiting. More common in premature infants and can be determined by radiological dye study.
A recent study[20] by looked at thecorrelation of meconium plug as identified radiologically covering 1994 to 2007, of 77 patients (mean gestational age 37.4 weeks, birth weight, 2977 g) Hirschsprung's disease was found in 10 patients (13%). "Although all patients with plugs and persistent abnormal stooling patterns should prompt a rectal biopsy and genetic probe, the incidence of Hirschsprung's and cystic fibrosis may not be as high as previously reported."
Appendix Duplication
Appendix duplication is an extremely rare congenital anomaly (0.004% to 0.009% of appendectomy specimens) first classified according to their anatomic location by Cave in 1936[21] and a later modified by Wallbridge in 1963[22], subsequently two more types of appendix abnormalities have been identified.[23][24]
Modified Cave-Wallbridge Classification (table from[25])
| Classification of types of appendix duplication |
Features |
| A | Single cecum with various degrees of incomplete duplication |
| B1 (bird type) | Two appendixes symmetrically placed on either side of the ileocecal valve |
| B2 (tenia coli type) | ne appendix arises from the cecum at the usual site, and the second
appendix branches from the cecum along the lines of the tenia at various distances from the first |
| B3 | One appendix arises from the usual site, and the second appendix arises from
the hepatic flexura |
| B4 | One appendix arises from the usual site, and the second appendix arises from
the splenic flexura |
| C | Double cecum, each with an appendix |
| Horseshoe appendix | One appendix has two openings into a common cecum |
| Triple appendix | One appendix arises from the cecum at the usual site, and two additional appendixes arise from the colon |
Anorectal Malformations

(ARMs) A group of many different abnormalities that can involve the distal anus and rectum as well as the urinary and genital tracts, for review see[26]. Occurring with an incidence of approximately 1 in 5000 live births.
|
Classification of non-syndromic anorectal malformations (ARM) | |
| Males |
Recto-perineal fistula |
| Recto-urethral-bulbar fistula | |
| Recto-urethral-prostatic fistula | |
| Recto-bladderneck fistula | |
| Imperforated anus without fistula | |
| Complex and unusual defects | |
|
| |
| Females |
Recto-perineal fistula |
| Recto-vestibular fistula | |
| Cloaca with short common channel (< 3 cm) | |
| Cloaca with long common channel (> 3 cm) | |
| Imperforated anus without fistula | |
|
| |
| Complex and unusual defects |
Cloacal extrophy, covered cloacal extra |
| Posterior cloaca | |
| Associated to presacral mass | |
| Rectal atresia | |
|
| |
|
Table Levitt and Peña (2007)[26] | |
Anal Atresia
Anal atresia or imperforate anus is an abnormality of incomplete anorectal region development occurring in about 1 in 5,000 infants. Resulting in accumulation of stool within the colon.
- rectum may end and not connect with the anus
- rectum may connect anatomically to the wrong region (urethra, bladder, or vagina).
- anus may be very narrowed or missing altogether.
Congenital Cloaca
Anal muscles and vagina wall do not form leading to a variable opening composing all or some of the rectum, vagina and bladder. Surgically requires a colostomy and other procedures to transfers a muscle from another part of the body to create a functioning sphincter at the anus.
References
- ↑ Orgul G, Soyer T, Yurdakok M & Beksac MS. (2018). Evaluation of pre- and postnatally diagnosed gastrointestinal tract obstructions. J. Matern. Fetal. Neonatal. Med. , , 1-6. PMID: 29606013 DOI.
- ↑ Danzer E, Gerdes M, D'Agostino JA, Bernbaum J, Hoffman C, Rintoul NE, Herkert LM, Flake AW, Adzick NS & Hedrick HL. (2015). Patient characteristics are important determinants of neurodevelopmental outcome during infancy in giant omphalocele. Early Hum. Dev. , 91, 187-93. PMID: 25676186 DOI.
- ↑ Pini Prato A, Rossi V, Mosconi M, Holm C, Lantieri F, Griseri P, Ceccherini I, Mavilio D, Jasonni V, Tuo G, Derchi M, Marasini M, Magnano G, Granata C, Ghiggeri G, Priolo E, Sposetti L, Porcu A, Buffa P & Mattioli G. (2013). A prospective observational study of associated anomalies in Hirschsprung's disease. Orphanet J Rare Dis , 8, 184. PMID: 24267509 DOI.
- ↑ Raghoebir L, Biermann K, Buscop-van Kempen M, Wijnen RM, Tibboel D, Smits R & Rottier RJ. (2013). Disturbed balance between SOX2 and CDX2 in human vitelline duct anomalies and intestinal duplications. Virchows Arch. , 462, 515-22. PMID: 23568430 DOI.
- ↑ Ngan ES, Garcia-Barceló MM, Yip BH, Poon HC, Lau ST, Kwok CK, Sat E, Sham MH, Wong KK, Wainwright BJ, Cherny SS, Hui CC, Sham PC, Lui VC & Tam PK. (2011). Hedgehog/Notch-induced premature gliogenesis represents a new disease mechanism for Hirschsprung disease in mice and humans. J. Clin. Invest. , 121, 3467-78. PMID: 21841314 DOI.
- ↑ Bower RJ, Sieber WK & Kiesewetter WB. (1978). Alimentary tract duplications in children. Ann. Surg. , 188, 669-74. PMID: 718292
- ↑ Spitz L. (2007). Oesophageal atresia. Orphanet J Rare Dis , 2, 24. PMID: 17498283 DOI.
- ↑ Pinheiro PF, Simões e Silva AC & Pereira RM. (2012). Current knowledge on esophageal atresia. World J. Gastroenterol. , 18, 3662-72. PMID: 22851858 DOI.
- ↑ Michaud L, Coutenier F, Podevin G, Bonnard A, Becmeur F, Khen-Dunlop N, Auber F, Maurel A, Gelas T, Dassonville M, Borderon C, Dabadie A, Weil D, Piolat C, Breton A, Djeddi D, Morali A, Bastiani F, Lamireau T & Gottrand F. (2013). Characteristics and management of congenital esophageal stenosis: findings from a multicenter study. Orphanet J Rare Dis , 8, 186. PMID: 24289834 DOI.
- ↑ Mc Laughlin D, Murphy P & Puri P. (2014). Altered Tbx1 gene expression is associated with abnormal oesophageal development in the adriamycin mouse model of oesophageal atresia/tracheo-oesophageal fistula. Pediatr. Surg. Int. , 30, 143-9. PMID: 24356861 DOI.
- ↑ Soffers JH, Hikspoors JP, Mekonen HK, Koehler SE & Lamers WH. (2015). The growth pattern of the human intestine and its mesentery. BMC Dev. Biol. , 15, 31. PMID: 26297675 DOI.
- ↑ Panda N, Bansal NK, Narasimhan M & Ardhanari R. (2014). Laparoscopic correction of intestinal malrotation in adult. J Minim Access Surg , 10, 90-2. PMID: 24761085 DOI.
- ↑ Stevenson RE, Rogers RC, Chandler JC, Gauderer MW & Hunter AG. (2009). Escape of the yolk sac: a hypothesis to explain the embryogenesis of gastroschisis. Clin. Genet. , 75, 326-33. PMID: 19419415 DOI.
- ↑ Salinas-Torres VM, Salinas-Torres RA, Cerda-Flores RM & Martínez-de-Villarreal LE. (2018). Genetic variants conferring susceptibility to gastroschisis: a phenomenon restricted to the interaction with the environment?. Pediatr. Surg. Int. , 34, 505-514. PMID: 29550988 DOI.
- ↑ Francis SS, Wiemels JL, Yang W & Shaw GM. (2018). Herpesvirus Infection in Infants with Gastroschisis. Epidemiology , , . PMID: 29634591 DOI.
- ↑ Payne NR, Simonton SC, Olsen S, Arnesen MA & Pfleghaar KM. (2011). Growth restriction in gastroschisis: quantification of its severity and exploration of a placental cause. BMC Pediatr , 11, 90. PMID: 22004141 DOI.
- ↑ Molik KA, Gingalewski CA, West KW, Rescorla FJ, Scherer LR, Engum SA & Grosfeld JL. (2001). Gastroschisis: a plea for risk categorization. J. Pediatr. Surg. , 36, 51-5. PMID: 11150437 DOI.
- ↑ Akakpo-Numado GK, Gnassingbe K, Boume MA, Sakiye KA, Mihluedo-Agbolan K, Attipou K & Tekou H. (2012). Emergency treatment of a ruptured huge omphalocele by simple suture of its membrane. Ann Surg Innov Res , 6, 2. PMID: 22325297 DOI.
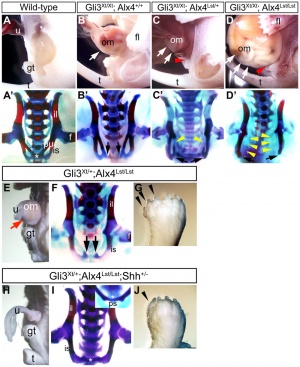
- ↑ Matsumaru D, Haraguchi R, Miyagawa S, Motoyama J, Nakagata N, Meijlink F & Yamada G. (2011). Genetic analysis of Hedgehog signaling in ventral body wall development and the onset of omphalocele formation. PLoS ONE , 6, e16260. PMID: 21283718 DOI.
- ↑ Keckler SJ, St Peter SD, Spilde TL, Tsao K, Ostlie DJ, Holcomb GW & Snyder CL. (2008). Current significance of meconium plug syndrome. J. Pediatr. Surg. , 43, 896-8. PMID: 18485962 DOI.
- ↑ Cave AJ. (1936). Appendix Vermiformis Duplex. J. Anat. , 70, 283-92. PMID: 17104589
- ↑ WALLBRIDGE PH. (1962). Double appendix. Br J Surg , 50, 346-7. PMID: 13998581
- ↑ Mesko TW, Lugo R & Breitholtz T. (1989). Horseshoe anomaly of the appendix: a previously undescribed entity. Surgery , 106, 563-6. PMID: 2772830
- ↑ Tinckler LF. (1968). Triple appendix vermiformis--a unique case. Br J Surg , 55, 79-81. PMID: 5635427
- ↑ Canbay E & Akman E. (2011). Appendix perforation in appendix duplication in a man: a case report. J Med Case Rep , 5, 162. PMID: 21513538 DOI.
- ↑ 26.0 26.1 26.2 Levitt MA & Peña A. (2007). Anorectal malformations. Orphanet J Rare Dis , 2, 33. PMID: 17651510 DOI.
Reviews
Martin V & Shaw-Smith C. (2010). Review of genetic factors in intestinal malrotation. Pediatr. Surg. Int. , 26, 769-81. PMID: 20549505 DOI.
Strouse PJ. (2004). Disorders of intestinal rotation and fixation ("malrotation"). Pediatr Radiol , 34, 837-51. PMID: 15378215 DOI.
Levy AD & Hobbs CM. (2004). From the archives of the AFIP. Meckel diverticulum: radiologic features with pathologic Correlation. Radiographics , 24, 565-87. PMID: 15026601 DOI.
Chitkara DK, Nurko S, Shoffner JM, Buie T & Flores A. (2003). Abnormalities in gastrointestinal motility are associated with diseases of oxidative phosphorylation in children. Am. J. Gastroenterol. , 98, 871-7. PMID: 12738470 DOI.
D'Agostino J. (2002). Common abdominal emergencies in children. Emerg. Med. Clin. North Am. , 20, 139-53. PMID: 11826631
Boudiaf M, Soyer P, Terem C, Pelage JP, Maissiat E & Rymer R. (2001). Ct evaluation of small bowel obstruction. Radiographics , 21, 613-24. PMID: 11353110 DOI.
Articles
Jones KL, Benirschke K & Chambers CD. (2009). Gastroschisis: etiology and developmental pathogenesis. Clin. Genet. , 75, 322-5. PMID: 19419414 DOI.
Feldkamp ML, Carey JC & Sadler TW. (2007). Development of gastroschisis: review of hypotheses, a novel hypothesis, and implications for research. Am. J. Med. Genet. A , 143A, 639-52. PMID: 17230493 DOI.
Cassart M, Massez A, Lingier P, Absil AS, Donner C & Avni F. (2006). Sonographic prenatal diagnosis of malpositioned stomach as a feature of uncomplicated intestinal malrotation. Pediatr Radiol , 36, 358-60. PMID: 16465538 DOI.
Ashraf A, Abdullatif H, Hardin W & Moates JM. (2005). Unusual case of neonatal diabetes mellitus due to congenital pancreas agenesis. Pediatr Diabetes , 6, 239-43. PMID: 16390394 DOI.
Beaudoin S, Mathiot-Gavarin A, Gouizi G & Bargy F. (2005). Familial malrotation: report of three affected siblings. Pediatr. Surg. Int. , 21, 856-7. PMID: 16205928 DOI.
Drewett M, Michailidis GD & Burge D. (2006). The perinatal management of gastroschisis. Early Hum. Dev. , 82, 305-12. PMID: 16563666 DOI.
Vegunta RK, Wallace LJ, Leonardi MR, Gross TL, Renfroe Y, Marshall JS, Cohen HS, Hocker JR, Macwan KS, Clark SE, Ramiro S & Pearl RH. (2005). Perinatal management of gastroschisis: analysis of a newly established clinical pathway. J. Pediatr. Surg. , 40, 528-34. PMID: 15793730 DOI.
Salomon LJ, Mahieu-Caputo D, Jouvet P, Jouannic JM, Benachi A, Grebille AG, Dumez Y & Dommergues M. (2004). Fetal home monitoring for the prenatal management of gastroschisis. Acta Obstet Gynecol Scand , 83, 1061-4. PMID: 15488122 DOI.
Langer JC. (2003). Abdominal wall defects. World J Surg , 27, 117-24. PMID: 12557047 DOI.
Search PubMed
Search Pubmed: gastrointestinal tract abnormalities | intestinal malrotation | Situs Inversus Viscera | Gastroschisis | Intestinal Aganglionosis
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- NIH National Institute of Diabetes and Digestive and Kidney Diseases Hirschsprung Disease | Anatomic Problems of the Colon
- BMC Gastroenterology
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, June 17) Embryology Gastrointestinal Tract - Abnormalities. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Gastrointestinal_Tract_-_Abnormalities
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G



![97 Short Meckel's Diverticulum]](/embryology/images/thumb/6/62/Cullen1916_fig97.jpg/120px-Cullen1916_fig97.jpg)