Non-Invasive Prenatal Testing: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 16: | Line 16: | ||
|-bgcolor="F5FAFF" | |-bgcolor="F5FAFF" | ||
| | | | ||
* '''Uptake, outcomes, and costs of implementing non-invasive prenatal testing for Down's syndrome into UK NHS maternity care'''<ref name=PMID27378786><pubmed>27378786</pubmed></ref> "Eight maternity units across the United Kingdom between 1 November 2013 and 28 February 2015. All pregnant women with a current Down's syndrome risk on screening of at least 1/1000. NIPT was prospectively offered to 3175 pregnant women. In 934 women with a Down's syndrome risk greater than 1/150, 695 (74.4%) chose NIPT, 166 (17.8%) chose invasive testing, and 73 (7.8%) declined further testing. Of 2241 women with risks between 1/151 and 1/1000, 1799 (80.3%) chose NIPT. Of 71 pregnancies with a confirmed diagnosis of Down's syndrome, 13/42 (31%) with the diagnosis after NIPT and 2/29 (7%) after direct invasive testing continued, resulting in 12 live births. ...Implementation of NIPT as a contingent test within a public sector Down's syndrome screening programme can improve quality of care, choices for women, and overall performance within the current budget. As some women use NIPT for information only, the Down's syndrome live birth rate may not change significantly. Future research should consider NIPT uptake and informed decision making outside of a research setting." [[Trisomy 21]] | [[Statistics - United Kingdom]] | |||
* '''Fetal aneuploidy screening with cell-free DNA in late gestation'''<ref name=PMID27124739><pubmed>27124739</pubmed></ref>"The aim of this study was to evaluate clinical use of NIPT at gestational ages of 23 weeks and above. A cohort of 5579 clinical patients with singleton gestations of 23 weeks or greater submitting a blood sample for NIPT in an 18-month period were selected for this study. ...Of 5372 reported late-gestation samples, 151 (2.8%) were reported as aneuploidy detected or suspected. In late-gestation samples, the overall observed positive predictive value (PPV) for NIPT was 64.7%, with an observed PPV of 100% in the subset of cases with multiple clinical indications including abnormal ultrasound findings. NIPT is a highly accurate prenatal screening option for women after 23 weeks of gestation. Women who presented for NIPT in the latter stages of pregnancy more frequently specified clinical indications of abnormal ultrasound findings than women who entered screening earlier in pregnancy." | * '''Fetal aneuploidy screening with cell-free DNA in late gestation'''<ref name=PMID27124739><pubmed>27124739</pubmed></ref>"The aim of this study was to evaluate clinical use of NIPT at gestational ages of 23 weeks and above. A cohort of 5579 clinical patients with singleton gestations of 23 weeks or greater submitting a blood sample for NIPT in an 18-month period were selected for this study. ...Of 5372 reported late-gestation samples, 151 (2.8%) were reported as aneuploidy detected or suspected. In late-gestation samples, the overall observed positive predictive value (PPV) for NIPT was 64.7%, with an observed PPV of 100% in the subset of cases with multiple clinical indications including abnormal ultrasound findings. NIPT is a highly accurate prenatal screening option for women after 23 weeks of gestation. Women who presented for NIPT in the latter stages of pregnancy more frequently specified clinical indications of abnormal ultrasound findings than women who entered screening earlier in pregnancy." | ||
* '''Open source non-invasive prenatal testing platform and its performance in a public health laboratory'''<ref name=PMID27027563><pubmed>27027563</pubmed></ref> "o introduce NIPT for fetal autosomal trisomies and gender in a Danish public health setting, using semi-conductor sequencing and published open source scripts for analysis. Plasma derived DNA from a total of 375 pregnant women (divided into 3 datasets) was whole-genome sequenced on the Ion Proton™ platform and analyzed using a pipeline based on WISECONDOR for fetal autosomal aneuploidy detection and SeqFF for fetal DNA fraction estimation. We furthermore validated a fetal sex determination analysis. The pipeline correctly detected 27/27 trisomy 21, 4/4 trisomy 18 and 3/3 trisomy 13 fetuses. Neither false negatives nor false positives (chromosomes 13, 18 and 21) were observed in our validation dataset. Fetal sex was identified correctly in all but one triploid fetus (172/173). SeqFF showed a strong correlation (R2 = 0.72) to Y-chromosomal content of the male fetus samples." | * '''Open source non-invasive prenatal testing platform and its performance in a public health laboratory'''<ref name=PMID27027563><pubmed>27027563</pubmed></ref> "o introduce NIPT for fetal autosomal trisomies and gender in a Danish public health setting, using semi-conductor sequencing and published open source scripts for analysis. Plasma derived DNA from a total of 375 pregnant women (divided into 3 datasets) was whole-genome sequenced on the Ion Proton™ platform and analyzed using a pipeline based on WISECONDOR for fetal autosomal aneuploidy detection and SeqFF for fetal DNA fraction estimation. We furthermore validated a fetal sex determination analysis. The pipeline correctly detected 27/27 trisomy 21, 4/4 trisomy 18 and 3/3 trisomy 13 fetuses. Neither false negatives nor false positives (chromosomes 13, 18 and 21) were observed in our validation dataset. Fetal sex was identified correctly in all but one triploid fetus (172/173). SeqFF showed a strong correlation (R2 = 0.72) to Y-chromosomal content of the male fetus samples." | ||
Revision as of 11:52, 11 July 2016
| Embryology - 11 May 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
| Educational Use Only - Embryology is an educational resource for learning concepts in embryological development, no clinical information is provided and content should not be used for any other purpose. |
Introduction
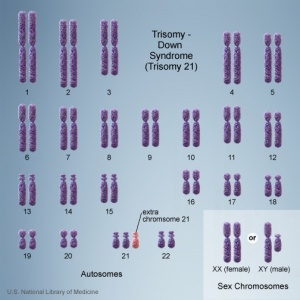
Non-Invasive Prenatal Testing (NIPT) is a new technique that analyzes cell-free fetal DNA circulating in maternal blood. Testing of circulating cell-free fetal DNA (ccffDNA) can be carried out after 10 weeks (between 10-22 weeks) analysis can take a week or more. It has been most useful for replacing amniocentesis in testing for the trisomies; Trisomy 21, Trisomy 18, and Trisomy 13.
There are other pages that refer to postnatal diagnostic testing. (More? Neonatal Diagnosis)
- This Embryology site is a developmental educational resource, it does not provide specific clinical details, you should always refer to a health professional.
| Assisted Reproductive Technology | In Vitro Fertilization | Journal - Prenatal diagnosis
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Non-Invasive Prenatal Testing <pubmed limit=5>Non-Invasive Prenatal Testing</pubmed> |
Costs
A recent 2014 Canadian study[9] identified the cost of NIPT ranges from US$800 to US$2000 in the USA and from US$500 to US$1500 elsewhere.
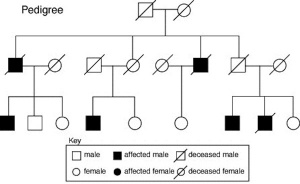
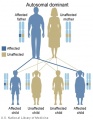
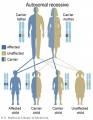
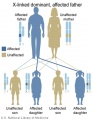
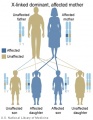
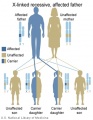
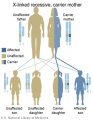
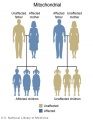
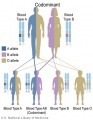
Inheritance Genetics
- Links: Genetic risk maternal age | Trisomy 21
Australia
A recent publication from NHMRC Medical Genetic Testing: information for health professionals (2010). This paper covers background information on all types of genetic tests, not just those associated with prenatal diagnosis.
Types of genetic tests
- Somatic cell genetic testing involves testing tissue (usually cancer) for non-heritable mutations. This may be for diagnostic purposes, or to assist in selecting treatment for a known cancer.
- Diagnostic testing for heritable mutations involves testing an affected person to identify the underlying mutation(s) responsible for the disease. This typically involves testing one or more genes for a heritable mutation.
- Predictive testing for heritable mutations involves testing an unaffected person for a germline mutation identified in genetic relatives. The risk of disease will vary according to the gene, the mutation and the family history.
- Carrier testing for heritable mutations involves testing for the presence of a mutation that does not place the person at increased risk of developing the disease, but does increase the risk of having an affected child developing the disease.
- Pharmacogenetic testing for a genetic variant that alters the way a drug is metabolised. These variants can involve somatic cells or germline changes. Even if these variants are heritable (that is germline changes), the tests are usually of relevance to genetic relatives only if they are being treated with the same type of medication.
USA
A new site developed by NIH "GeneTests" provides medical genetics information resources available at no cost to all interested persons. It contains educational information, a directory of genetic testing laboratories and links to other databases such as OMIM.
- Links: GeneTests | Medline Plus - Genetic Testing
Ethics of Testing
Major developmental abnormalities detected early enough can be resolved far more easily than those discovered late in a pregnancy.
What are the ethical questions that are raised by prenatal testing? Future individual rights or parents rights? But what about diseases, like Huntington's, where a diagnostic test can be made but there are no current treatments for the postnatal (95% of cases adult onset) disease?
Huntington's disease
Guidelines for the molecular genetics predictive test
- Recommendation 2.1 "the test is available only to individuals who have reached the age of majority."
- Recommendation 7.2 "the couple requesting antenatal testing must be clearly informed that if they intend to complete the pregnancy if the fetus is a carrier of the gene defect, there is no valid reason for performing the test."
References
Reviews
<pubmed>26893576</pubmed> <pubmed>26266986</pubmed> <pubmed>25653560</pubmed> <pubmed>26237390</pubmed>
Articles
<pubmed>26864482</pubmed> <pubmed>26000626</pubmed> <pubmed>26996738</pubmed> <pubmed>27064737</pubmed> <pubmed>26850935</pubmed> <pubmed>26553705</pubmed>
Books
<pubmed>25654151</pubmed>| PubMed Health
Search Pubmed
Search Pubmed: Non-Invasive Prenatal Testing
- ART - Assisted Reproductive Technology a general term to describe all the clinical techniques used to aid fertility.
- blastomere biopsy - An ART preimplantation genetic diagnosis technique carried out at cleavage stage (day 3), excluding poor quality embryos, detects chromosomal abnormalities of both maternal and paternal origin. May not detect cellular mosaicism in the embryo.
- blastocyst biopsy - An ART preimplantation genetic diagnosis technique carried out at blastocyst stage (day 4-5), removes several trophoblast (trophoderm) cells, detects chromosomal abnormalities of both maternal and paternal origin and may detect cellular mosaicism.
- cell-free fetal deoxyribonucleic acid - (cfDNA) refers to fetal DNA circulating and isolated from the plasma portion of maternal blood. Can be performed from GA 10 weeks as a first-tier test or as a second-tier test, with women with increased probability on combined first trimester screening offered cfDNA or diagnostic testing.
- false negative rate - The proportion of pregnancies that will test negative given that the congenital anomaly is present.
- false positive rate - The proportion of pregnancies that will test positive given that the congenital anomaly is absent.
- free β human chorionic gonadotrophin - beta-hCG subunit of hCG used as a diagnostic marker for: early detection of pregnancy, Trisomy 21, spontaneous abortion, ectopic pregnancy, hydatidiform mole or choriocarcinoma.
- multiples of the median - (MoM) A multiple of the median is a measure of how far an individual test result deviates from the median and is used to report the results of medical screening tests, particularly where the results of the individual tests are highly variable.
- negative predictive value - The probability that a congenital anomaly is absent given that the prenatal screening test is negative.
- Non-Invasive Prenatal Testing - (NIPT) could refer to ultrasound or other imaging techniques, but more frequently used to describe analysis of cell-free fetal DNA circulating in maternal blood.
- polar body biopsy - (PB biopsy) An ART preimplantation genetic diagnosis technique that removes either the first or second polar body from the zygote. As these are generated by oocyte meiosis they detects chromosomal abnormalities only on the female genetics.
- positive predictive value - The probability that a congenital anomaly is present given that the prenatal screening test is positive.
- pre-implantation genetic diagnosis - (PGD, pre-implantation genetic screening) a diagnostic procedure for embryos produced through Assisted Reproductive Technology (ART, in vitro fertilisation, IVF) for genetic diseases that would generate developmental abnormalities or serious postnatal diseases.
- prenatal screening sensitivity - (detection rate) The probability of testing positive on a prenatal screening test if the congenital anomaly is present.
- prenatal screening specificity - The probability of testing negative on a prenatal screening test if the congenital anomaly is absent.
- quadruple test (maternal serum testing of a-fetoprotein Template:AFP, free B-hCG or total hCG, unconjugated estriol, and inhibin A) is a fetal chromosomal anomaly test usually carried out later in pregnancy (GA 14 to 20 weeks).
- single nucleotide polymorphisms - (SNPs) the variation in a single DNA nucleotide that occurs at a specific position in the genome.
- triple test - (maternal serum testing of a-fetoprotein Template:AFP, free B-hCG or total hCG, and unconjugated estriol) is a fetal chromosomal anomaly test usually carried out later in pregnancy (GA 14 to 20 weeks).
| Other Terms Lists |
|---|
| Terms Lists: ART | Birth | Bone | Cardiovascular | Cell Division | Endocrine | Gastrointestinal | Genital | Genetic | Head | Hearing | Heart | Immune | Integumentary | Neonatal | Neural | Oocyte | Palate | Placenta | Radiation | Renal | Respiratory | Spermatozoa | Statistics | Tooth | Ultrasound | Vision | Historic | Drugs | Glossary |
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- Australian and New Zealand
- Royal Australian College of General Practitioners Australian Family Physician (2014)
- College of Obstetricians and Gynaecologists Intrapartum Fetal Surveillance Clinical Guidelines - Second Edition (June 2011)
- Canada - Society of Obstetricians and Gynaecologists of Canada
- USA
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, May 11) Embryology Non-Invasive Prenatal Testing. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Non-Invasive_Prenatal_Testing
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G