Gastrointestinal Tract - Gall Bladder Development: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 22: | Line 22: | ||
* '''Muscularis mucosae versus muscularis propria in gallbladder, cystic duct, and common bile duct: smoothelin and desmin immunohistochemical study'''<ref name="PMID21074688"><pubmed>21074688</pubmed></ref> "The muscle layer in the cystic duct and common bile duct is not well defined, and it is unresolved whether it represents muscularis mucosae or muscularis propria. ... Based on our findings, we conclude that, in the gallbladder wall, the muscle layer is muscularis propria and there is no muscularis mucosae present. In the cystic duct and common bile duct, only an attenuated and incomplete muscle layer of muscularis mucosae is present; because there is no muscularis propria, there probably is limited contractile function." | * '''Muscularis mucosae versus muscularis propria in gallbladder, cystic duct, and common bile duct: smoothelin and desmin immunohistochemical study'''<ref name="PMID21074688"><pubmed>21074688</pubmed></ref> "The muscle layer in the cystic duct and common bile duct is not well defined, and it is unresolved whether it represents muscularis mucosae or muscularis propria. ... Based on our findings, we conclude that, in the gallbladder wall, the muscle layer is muscularis propria and there is no muscularis mucosae present. In the cystic duct and common bile duct, only an attenuated and incomplete muscle layer of muscularis mucosae is present; because there is no muscularis propria, there probably is limited contractile function." | ||
|} | |} | ||
{| class="wikitable collapsible collapsed" | {| class="wikitable mw-collapsible mw-collapsed" | ||
! More recent papers | ! More recent papers | ||
|- | |- | ||
Revision as of 18:09, 19 June 2014
| Embryology - 29 May 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
This section of notes gives an overview of Gall Bladder and hillary tree development, histology and abnormalities associated with the biliary system. In the adult, the gall bladder is a site of bile salt storage and concentration, to then be released into the duodenum where they act to solubilize dietary lipids by their detergent effect. Bile salts are a cholesterol derivative (breakdown product).
The transverse septum differentiates to form the hepatic diverticulum and the hepatic primordium, these two structures together will go on to form different components of the mature liver and gall bladder.
The hepatic diverticulum divides into two parts: pars hepatica (larger cranial part, primordium of the liver) and pars cystica (smaller ventral invagination, primordium of gall bladder).
The pars cystica vacuolates and expands, the stalk becoming the cystic duct. This structure is initially hollow, then solid (by proliferation of epithelial lining), and then recanalized occurs by vacuolation of this expanded epithelium. There are several opinions as to whether the duct has a solid phase or remains patent throughout development.[1][2]
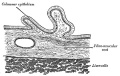
See also Gall Bladder Histology.
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Gall Bladder Embryology <pubmed limit=5>Gall Bladder Embryology</pubmed> |
Embryonic Development
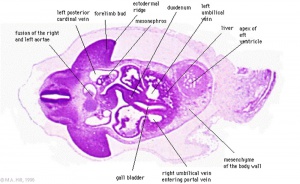
Stage 13
Early embryonic gall bladder (Carnegie stage 13, Week 4)
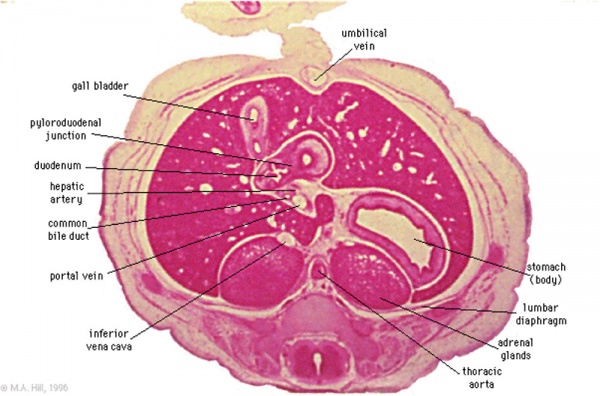
Stage 22
Late embryonic gall bladder (Carnegie stage 22, Week 8)
Abnormalities
Infections
These mainly relate to postnatal infections. Recent studies in the mouse have identified that gastrointestinal tract listeria infections can relocate to the gall bladder and reside there, leading to later reinfection of the gastrointestinal tract.
- Links: Bacterial Infection
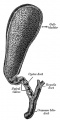
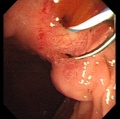
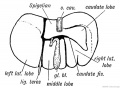
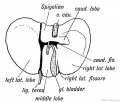
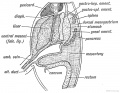
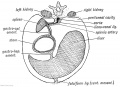
Additional Images
See also Gall Bladder Histology
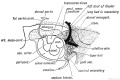
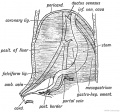
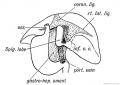
Chapter XVIII. The Organs of Digestion Keith, A. (1902) Human Embryology and Morphology. London: Edward Arnold.
References
Reviews
<pubmed>21074731</pubmed> <pubmed>20152372</pubmed> <pubmed>18484608</pubmed> <pubmed>15853977</pubmed> <pubmed>15382016</pubmed>
Articles
<pubmed>21078254</pubmed> <pubmed>20191134</pubmed> <pubmed>16273658</pubmed>
Search Pubmed
July 2010
Search Bookshelf Gall Bladder Development
Search Pubmed Now: Gall Bladder Development | Cholangiocyte Development |
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, May 29) Embryology Gastrointestinal Tract - Gall Bladder Development. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Gastrointestinal_Tract_-_Gall_Bladder_Development
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G