User:Z3463667
Lab Attendence
--Z3463667 (talk) 13:16, 14 August 2015 (AEST)
--Z3463667 (talk) 12:10, 21 August 2015 (AEST)
--Z3463667 (talk) 12:10, 28 August 2015 (AEST)
--Z3463667 (talk) 12:06, 4 September 2015 (AEST)
--Z3463667 (talk) 12:03, 11 September 2015 (AEST)
--Z3463667 (talk) 12:15, 18 September 2015 (AEST)
--Z3463667 (talk) 12:27, 25 September 2015 (AEST)
--Z3463667 (talk) 12:21, 9 October 2015 (AEDT)
Lab 1 Assessment
Article 1
PMID 26238449
Progesterone elevation on the day of human chorionic gonadotropin administration adversely affects the outcome of IVF with transferred embryos at different developmental stages
The effect progesterone evaluation (PE) during fresh invitro fertilisation (IVF) cycles after hCG administration for oocyte maturation is still unclear. To overcome the possible effect, cleavage-stage embryo’s are replaced with blastocyst-stage embryos before transfer (they are suggested to be unaffected by PE), however it is unclear if the results are reliable. Therefore a study was conducted to investigate the link between PE on the day hCG is administrated and the clinical pregnancy rate (CPR) following IVF/intracytoplasmic sperm injection cycles (ICSI) after embryo transfer at different stages. The levels at which PE had a detrimental effect on CPR was also investigated.
A retrospective study was conducted on a cohort of patients undergoing IVF with gonadotropin and GnRH agonist for ovarian stimulation at a single-centre. Patients were then spilt into two groups, one undergoing cleavage-stage embryo transfer at day 3, and the other undergoing blastocyst-stage transfer at day 5. Patients were assessed clinically to undergo the standard long GnRH protocol or a prolonged protocol.
The pituitary was suppressed by injecting Triptorelin acetate or Diphereline. This was followed by gonadotropin, FSH activity or FSH and LH activity to initiate ovarian stimulation. Oocyte retrieval was conducted and embryo quality graded. CPR was measured as well as implantation rate, fertilisation rate and cleavage rate. Statistical analysis was performed.
It was found that in the day 3 and day 5 group, serum progesterone levels are inversely related to CPR. The detrimental affect of progesterone became evident once serum progesterone reached 1.0ng/ml in the day 3 group and 1.75ng/ml in the day 5 group. The developmental stage at which embryos were transferred was not found to be statistically significant. Therefore it is concluded that on the day that hCG is administered PE was found to decrease CPR in GnRH IVF cycles despite developmental stage of transfer. [1]
Article 2
PMID 26246873
Cut-Off Levels of Anti-Mullerian Hormone for The Prediction of Ovarian Response, In Vitro Fertilization Outcome and Ovarian Hyperstimulation Syndrome
The role of Anti-mullerian hormone (AMH) in the ovary is to inhibit the early stages of follicular development. It appears to be a reliable marker for the number of small antral follicles and as a result can help determine the plan for ovarian stimulation. AMH also decreases from adulthood onwards, and so can help indicate reduced ovarian reserve and dysfunction. Ovarian hyper stimulation syndrome (OHSS) patients have high serum AMH. A study was conducted to compare the average and cut-off AMH levels after oocyte attainment after ovarian stimulation and the association with pregnancy rates. AMH levels endocrinological and pathological risk factor patients were also compared to patients without the risk factors.
Serum and follicular fluid (FF) was collected from patients in their first or second IVF and ICSI cycles. Patients were analysed and their pathological factors compared to normal patients. The correlation between serum and FF AMH levels and the correlation between serum AMH, estradiol, number of follicles, injected dose of recombinant FSH (rFSH - used to induce ovarian stimulation after down-regulation with GnRH agonist) and patient age was analysed. The average and cut-off level of AMH was also evaluated in low, moderate or high responders to ovarian stimulation and pregnancy rates. Three analysis were conducted where AMH levels were analysed. They included one where ovary overreaction was induced (OHSS) and one for polycistic ovarian syndrome (PCOS) which were both compared against the third analysis of normal endocrinological patients.
It was found that AMH levels were significantly higher in FF than serum where AMH levels increased with increasing ovarian response in both. There was a positive correlation present between AMH levels and estradiol, number of follicles, number of retrieved oocytes and number of fertilised oocytes where AMH levels increased with each factor as response increased. There was an inverse correlation with age. The median AMH level in serum (1.76 ng/ml) and FF (2.9 ng/ml) was higher in patients who became pregnant than those who did not (1.0ng/ml in serum and 1.8 ng/ml in FF). AMH cut off level was 0.61 ng/ml in serum and 1.43 ng/ml in FF in low responders, and 1.03 ng/ml in serum and 2.23 ng/ml in FF in high responders. OHSS and PCOS patients had lower level of injected rFSH and higher follicle numbers which suggests higher estradiol than normal patients. A higher number of oocytes were retrieved from OHSS patients. Normal patients had the lowest AMH, PCOS had the highest. In conclusion, AMH can help predict ovarian stimulation response, can be a marker for PCOS and help to avoid OHSS. [2]
--Mark Hill (talk) 16:52, 3 September 2015 (AEST) These are good summaries of these 2 papers (5/5)
Lab 2 Assessment
| Uploading Images in 5 Easy Steps | ||
|---|---|---|
First Read the help page Images and Copyright Tutorial.
Students cannot delete images once uploaded. You will need to email me with the full image name and request deletion, that I am happy to do with no penalty if done before I assess. Non-Table version of this page
|
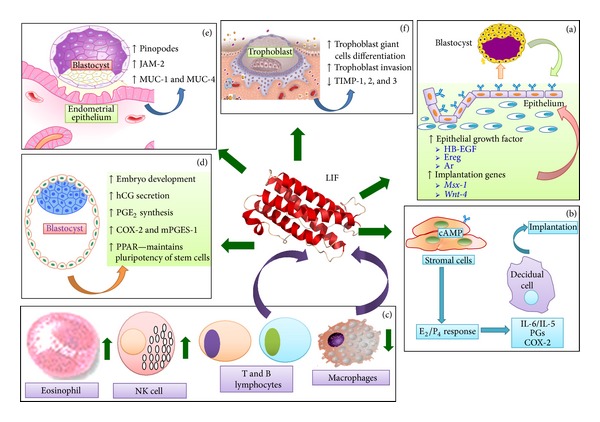
Roles of LIF in embryo implantation[3]
PMID 25152902
--Mark Hill (talk) 16:55, 3 September 2015 (AEST) The image has been uploaded correctly and contains reference, copyright and student template. You could have also uploaded a larger version of this image as it is quite difficult to read at this size. (5/5)
Lab 3 Assessment
Fertility preservation
Variability in the practice of fertility preservation for patients with cancer.
<pubmed>26010087</pubmed> This is an interesting article on how reproductive endocrinologists counselled cancer patients on fertility preservation. This is relevant to our group projects because it gives us an idea of what techniques and services are currently being utilised to help women.
Strategies for fertility preservation in young patients with cancer: a comprehensive approach.
<pubmed>24669162</pubmed> This article recognises that as cancer treatment improves the life span of patients, with it comes the treat to fertility. It is a great article as it clearly states what methods are currently available for addressing fertility preservation in males and females.
Clinical guide to fertility preservation in hematopoietic cell transplant recipients.
<pubmed>24419521</pubmed> This article focuses specifically on patients suffering infertility due to hematopoietic cell transplantation. It lists the options available to the patients whether female or male, which are applicable to patients who underwent other treatments and also lists the barriers to fertility preservation.
Fertility preservation in patients with haematological disorders: a retrospective cohort study.
<pubmed>24140311</pubmed> This article addresses fertility treatment in patients with haematological disorders specifically. However, is it a really good article as it is a cohort study comparing patients at various stages in their cancer journey, such as those who have had prior chemotherapy, those who pursued ovarian stimulation and those who did not pursue fertility treatment at all.
--Mark Hill (talk) 16:55, 3 September 2015 (AEST) These articles are relevant to your group project. Lets hope you can use these in the final project. (5/5)
Lab 4 Assessment
Week 1 and 2 Development
--Mark Hill (talk) 16:55, 3 September 2015 (AEST) These questions are OK. Negative responses (is not, incorrect) are sometimes hit and miss. The third question needed more in the question. You could have also included links to where the student could see the answer in context. (9/10)
ANAT2341 Student 2015 Quiz Questions
Lab 5 Assessment
What is the difference between gastroschisis and omphalocele?
Both omphaocele and gastroschisis are physical abnormalities present at birth, involving the abdominal wall which consist of protrusion of the internal viscera. Gastroschisis is generally a smaller defect in which the abdominal viscera usually protrude through the abdominal wall to the right of an intact umbilical cord. [4] Omphalocele, one of the most common birth defects of variable size involves the extrusion of the intestinal tract at the midline through a malformed umbilical cord. It is usually contained by a sac that is continuous with the umbilical cord. [5] The two conditions are distinguished through their location, size of the defect and whether or not there is a sac covering the extrusion.
Furthermore, in the case of gastrochisis the small bowel and colon have not undergone the normal rotation during development. The dueodenum to the rectum is exposed without peritoneal covering, and floats loosely in the amniotic fluid which causes inflammation. This leads to a shortened intestine with functional abnormalities. [4] The cause of gastrochisis is still not very clear however there are associated risk factors. Incidence is higher in mothers of a younger age, those who had anaemia during pregnancy, used contraception or consumed alcohol early on in pregnancy. [6] A potential theory regarding the cause is intrauterine vascular occlusion of the right umbilical mesenteric artery which explains it’s occurrence to the right of the umbilical cord. This consists of arterial infarction, umbilical ring rupture and intestinal evisceration which is consistent with occasional intestinal atresia. [4]
On the otherhand, omphaocele which has a higher incidence than gastrochisis consists of a familial occurrence. Birth order is unimportant, however higher incidence was reported in increasing maternal age, with a higher rate of miscarriage occurring due to the abnormality. Omphalocele can be induced in animals through the use of irradiation, hypoxia and cytotoxic substances. There is almost always observation of incorrect roation. The cause of omphaocele remains unknown, however it is suggested that in omphacele and gastrochisis the malformation is due to developmental defects during embryological folding accountable for ventral closure. Therefore, one suggestion for Omphacele is a defect in the inhibition of the lateral wall folds in the abdomen. Another suggestion is the faulty migration of myotomes to the abdomen which results in the incomplete muscular closure within the wall which then inhibits intestinal growth and enlargement. The abdomen is protected from inflammation as a result of the amniotic fluid by the intact sac covering. [7]
Lab 7 Assessment
Thyroid hormone transporters and deiodinases in the developing human hypothalamus.
Thyroid hormone (TH) is required for human brain development including hypothalamic development and for proper function. Originally the fetus relies on maternal TH supplies before its own thyroid hormone is functional. However, once its TH receptors are established neurological impairment can occur with a lack of TH.
Friesema et al. (2012), studied the expression of thyroid hormone transporters and deiodinases in the developing hypothalamus. In their study they investigated the expression of D2, D3, and TH transporters MCT8, MCT10 and OATP1C1 to determine the timing of TH signaling in hypothalamic nuclei at different developmental stages. Postmortem hypothalamic specimens were obtained from fetus’ from 17 weeks gestation to 29 months old children. The tissue was fixed, immunocytochemically stained, and intensities were scored by visual inspection.
It was found that D3 (TH inactivator) and MCT8 (for T3 uptake in cells) were present in the youngest samples at 17 weeks gestation where lateral hypothalamic zone differentiation takes place. T3 is degraded and not produced at this point, protecting the brain from early maturation. D2 is expressed after 17 weeks gestation. MCT8, MCT10 and OATP1C1 were expressed with different intensities among subjects during the late second trimester when the hypothalamus starts to take on an adult-like structure. Towards the end of gestation TH transporters and D2 decreased whilst D3 increased indicating a lower demand for T3. TH transporters then increase after birth at term before returning to adult-like levels. It was concluded that there are hypothalamic variations in deiodinases and TH transporters during fetal and neonatal development, however it is unclear if this is physiologically relevant. [8]
Embryonic layers and tissues that contribute to the developing teeth.
Teeth are derived from ectoderm, mesoderm and neural crest cells. The epithelium originates from oral ectoderm and mesenchyme from cranial neural crest cells. The neural crest cells move from the neuro-epithelium margins laterally and ventrally filling the facial prominence with mesenchyme to form the hard and soft tissue within teeth which include dentin, dental pulp, alveolar bone and periodontal ligament. The oral epithelium thickens and cells proliferate to form the dental lamina which invaginates into the mesenchyme which condenses below to form the dental papilla. The papilla gets surrounded by the epithelial bud and the adjacent mesenchyme cells form the dental follicle. This is followed by the bell stage where germ cells increase in size and the final shape is being formed. Established last are the ameloblasts (produce enamel) derived from epithelial cells adjacent to the papilla and odontoblasts (produce dentin) which come from the outer papilla layer and migrate towards the centre. [9]
References
- ↑ <pubmed>26238449</pubmed>
- ↑ <pubmed>26246873</pubmed>
- ↑ <pubmed>25152902</pubmed>
- ↑ 4.0 4.1 4.2 <pubmed>23958094</pubmed>
- ↑ Adesola C. Akinkuotu, Fariha Sheikh, Oluyinka O. Olutoye, Timothy C. Lee, Cariciolo J. Fernandes, Stephen E. Welty, Nancy A. Ayres, Darrell L. Cass, Giant omphaloceles: surgical management and perinatal outcomes, Journal of Surgical Research, 2015, 198(2):388-392, http://dx.doi.org/10.1016/j.jss.2015.03.060.
- ↑ <pubmed>25243388</pubmed>
- ↑ Jay L. Grosfeld, Thomas R. Weber, Congenital abdominal wall defects: Gastroschisis and omphalocele, Current Problems in Surgery, 1982, 19(4):159-213, http://dx.doi.org/10.1016/0011-3840(82)90048-X
- ↑ <pubmed>22723621</pubmed>
- ↑ <pubmed>24009032</pubmed>
Please do not use your real name on this website, use only your student number.
- 2015 Course: Week 2 Lecture 1 Lecture 2 Lab 1 | Week 3 Lecture 3 Lecture 4 Lab 2 | Week 4 Lecture 5 Lecture 6 Lab 3 | Week 5 Lecture 7 Lecture 8 Lab 4 | Week 6 Lecture 9 Lecture 10 Lab 5 | Week 7 Lecture 11 Lecture 12 Lab 6 | Week 8 Lecture 13 Lecture 14 Lab 7 | Week 9 Lecture 15 Lecture 16 Lab 8 | Week 10 Lecture 17 Lecture 18 Lab 9 | Week 11 Lecture 19 Lecture 20 Lab 10 | Week 12 Lecture 21 Lecture 22 Lab 11 | Week 13 Lecture 23 Lecture 24 Lab 12 | 2015 Projects: Three Person Embryos | Ovarian Hyper-stimulation Syndrome | Polycystic Ovarian Syndrome | Male Infertility | Oncofertility | Preimplantation Genetic Diagnosis | Students | Student Designed Quiz Questions | Moodle page