Ultrasound - Nuchal Translucency
| Embryology - 24 May 2026 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction

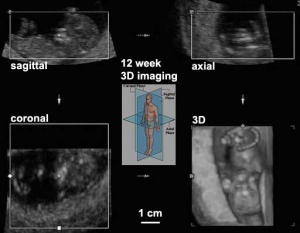
Nuchal translucency (NT) is the normal fluid-filled subcutaneous space that can be measured by ultrasound imaging between GA week 11 to 14 and is used as a diagnostic "soft marker", a measured increase in this space can relate to Trisomy 21 and other neural and chromosomal conditions in the fetus. The normal range of Nuchal Translucency at 13 to 14 GA weeks is 1.6 - 2.4 mm.
The term "soft markers" refers to ultrasound measurements which may not be diagnostic by themselves, but can have an indicative role for further diagnostic analysis of the pregnancy.
The Diagnostic Imaging Committee of the Society of Obstetricians and Gynaecologists of Canada in 2005[2] made the following recommendations:
- The screening ultrasound at 16 to 20 weeks should evaluate 8 markers, 5 of which (thickened nuchal fold, echogenic bowel, mild ventriculomegaly, echogenic focus in the heart, and choroid plexus cyst) are associated with an increased risk of fetal aneuploidy, and in some cases with nonchromosomal problems, while 3 (single umbilical artery, enlarged cisterna magna, and pyelectasis) are only associated with an increased risk of nonchromosomal abnormalities when seen in isolation (II-2 B).
- Identification of soft markers for fetal aneuploidy requires correlation with other risk factors, including history, maternal age, and maternal serum testing results (II-1 A).
- Soft markers identify a significant increase in fetal risk for genetic disease. Timely referral for confirmation, counselling, and investigation is required to maximize management options (III-B).
Ultrasound can also be used in combination with other techniques to locate both embryo and placenta for other prenatal tests (More? prenatal diagnosis).
The ultrasound technique can be used at any stage during pregnancy for fetal and placenta monitoring (More? Placenta Development | Placenta Abnormalities | Prenatal Diagnosis).
| <html5media height="300" width="400">File:Ultrasound_Fetus_02.mp4</html5media> | 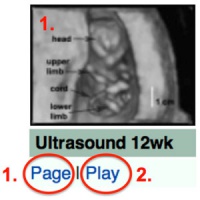
The ultrasound movies can be viewed in two ways:
Abnormal developmental ultrasound and features are listed on a separate page (More? abnormal ultrasound) all content is for educational use only. |
| Page | Play Movie shows a 12 week fetus in 3d in realtime (hence 4D). |
Special thanks to Dr Andrew McLennan, Foetal Medicine Unit, Royal North Shore Hospital for many of the original video materials. |
Some Recent Findings
...Higher-quality measurements were demonstrated in sonologists who performed more ultrasounds per year, those with more years of scanning experience, those who completed the online FMF course, and those periodically audited."
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: First Trimester Nuchal Translucency | Nuchal Translucency Measurement | Nuchal Translucency |
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page. |
Neural
| Neural | |||||||
|---|---|---|---|---|---|---|---|
|
| ||||||
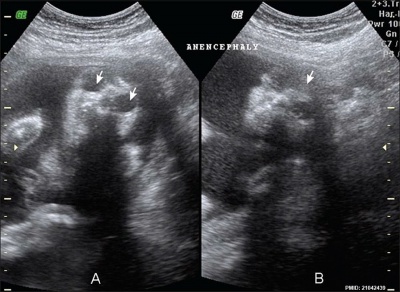
Anencephaly ultrasound[5]
Ultrasound Gestational Age
The following table is based upon Australian data from ultrasound measurements of Crown Rump Length (CRL).[6]
Note that Gestational Age GA differs from fertilisation age by about 2 weeks.
| Gestational Age and Crown-Rump Length (measured by ultrasound) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Fertilization and Gestational Age - Crown-Rump Length (ultrasound) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Additional Images
References
- ↑ Alphonse J, Cox J, Clarke J, Schluter P & McLennan A. (2013). The Effect of Ethnicity on 2D and 3D Frontomaxillary Facial Angle Measurement in the First Trimester. Obstet Gynecol Int , 2013, 847293. PMID: 24288543 DOI.
- ↑ Van den Hof MC & Wilson RD. (2005). Fetal soft markers in obstetric ultrasound. J Obstet Gynaecol Can , 27, 592-636. PMID: 16100637
- ↑ Torrent A, Manrique G, Gómez-Castelló T, Baldrich E, Cahuana M, Manresa JM & Borrell A. (2019). Sonologist's characteristics related to a higher quality in fetal nuchal translucency measured in primary antenatal care centers. Prenat. Diagn. , 39, 934-939. PMID: 31237971 DOI.
- ↑ Maya I, Yacobson S, Kahana S, Yeshaya J, Tenne T, Agmon-Fishman I, Cohen-Vig L, Shohat M, Basel-Vanagaite L & Sharony R. (2017). Cut-off value of nuchal translucency as indication for chromosomal microarray analysis. Ultrasound Obstet Gynecol , 50, 332-335. PMID: 28133835 DOI.
- ↑ Alorainy IA, Barlas NB & Al-Boukai AA. (2010). Pictorial Essay: Infants of diabetic mothers. Indian J Radiol Imaging , 20, 174-81. PMID: 21042439 DOI.
- ↑ 6.0 6.1 Westerway SC, Davison A & Cowell S. (2000). Ultrasonic fetal measurements: new Australian standards for the new millennium. Aust N Z J Obstet Gynaecol , 40, 297-302. PMID: 11065037
Journals
- Journal of Ultrasound in Medicine published by the American Institute of Ultrasound in Medicine.
Books
Molecular Imaging and Contrast Agent Database (MICAD) NBK5330 | PMID:20641179
Articles
Butt K & Lim K. (2014). Determination of gestational age by ultrasound. J Obstet Gynaecol Can , 36, 171-181. PMID: 24518917 DOI.
Lubusky M, Studnickova M, Skrivanek A, Vomackova K & Prochazka M. (2012). Ultrasound evaluation of fetal gender at 12-14 weeks. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub , 156, 324-9. PMID: 22660228 DOI.
Search PubMed
Search PubMed: Ultrasound prenatal diagnosis | Ultrasound
- ART - Assisted Reproductive Technology a general term to describe all the clinical techniques used to aid fertility.
- blastomere biopsy - An ART preimplantation genetic diagnosis technique carried out at cleavage stage (day 3), excluding poor quality embryos, detects chromosomal abnormalities of both maternal and paternal origin. May not detect cellular mosaicism in the embryo.
- blastocyst biopsy - An ART preimplantation genetic diagnosis technique carried out at blastocyst stage (day 4-5), removes several trophoblast (trophoderm) cells, detects chromosomal abnormalities of both maternal and paternal origin and may detect cellular mosaicism.
- cell-free fetal deoxyribonucleic acid - (cfDNA) refers to fetal DNA circulating and isolated from the plasma portion of maternal blood. Can be performed from GA 10 weeks as a first-tier test or as a second-tier test, with women with increased probability on combined first trimester screening offered cfDNA or diagnostic testing.
- false negative rate - The proportion of pregnancies that will test negative given that the congenital anomaly is present.
- false positive rate - The proportion of pregnancies that will test positive given that the congenital anomaly is absent.
- free β human chorionic gonadotrophin - beta-hCG subunit of hCG used as a diagnostic marker for: early detection of pregnancy, Trisomy 21, spontaneous abortion, ectopic pregnancy, hydatidiform mole or choriocarcinoma.
- multiples of the median - (MoM) A multiple of the median is a measure of how far an individual test result deviates from the median and is used to report the results of medical screening tests, particularly where the results of the individual tests are highly variable.
- negative predictive value - The probability that a congenital anomaly is absent given that the prenatal screening test is negative.
- Non-Invasive Prenatal Testing - (NIPT) could refer to ultrasound or other imaging techniques, but more frequently used to describe analysis of cell-free fetal DNA circulating in maternal blood.
- polar body biopsy - (PB biopsy) An ART preimplantation genetic diagnosis technique that removes either the first or second polar body from the zygote. As these are generated by oocyte meiosis they detects chromosomal abnormalities only on the female genetics.
- positive predictive value - The probability that a congenital anomaly is present given that the prenatal screening test is positive.
- pre-implantation genetic diagnosis - (PGD, pre-implantation genetic screening) a diagnostic procedure for embryos produced through Assisted Reproductive Technology (ART, in vitro fertilisation, IVF) for genetic diseases that would generate developmental abnormalities or serious postnatal diseases.
- prenatal screening sensitivity - (detection rate) The probability of testing positive on a prenatal screening test if the congenital anomaly is present.
- prenatal screening specificity - The probability of testing negative on a prenatal screening test if the congenital anomaly is absent.
- quadruple test (maternal serum testing of a-fetoprotein Template:AFP, free B-hCG or total hCG, unconjugated estriol, and inhibin A) is a fetal chromosomal anomaly test usually carried out later in pregnancy (GA 14 to 20 weeks).
- single nucleotide polymorphisms - (SNPs) the variation in a single DNA nucleotide that occurs at a specific position in the genome.
- triple test - (maternal serum testing of a-fetoprotein Template:AFP, free B-hCG or total hCG, and unconjugated estriol) is a fetal chromosomal anomaly test usually carried out later in pregnancy (GA 14 to 20 weeks).
| Other Terms Lists |
|---|
| Terms Lists: ART | Birth | Bone | Cardiovascular | Cell Division | Endocrine | Gastrointestinal | Genital | Genetic | Head | Hearing | Heart | Immune | Integumentary | Neonatal | Neural | Oocyte | Palate | Placenta | Radiation | Renal | Respiratory | Spermatozoa | Statistics | Tooth | Ultrasound | Vision | Historic | Drugs | Glossary |
Terms
- Biparietal diameter - (BPD) used to determine fetal age and normal development (small/large/abnormal) parameters. Measured as the diameter between the 2 sides of the head, measurements after 13 weeks (2.4 cm) to term (9.5 cm).
- cerebroplacental ratio - (CPR) a doppler ultrasound measurement calculated as the simple ratio between the middle cerebral artery pulsatility index (MCA‐PI) and the {{placenta]]l artery pulsatility index (UA‐PI). Fetuses with an abnormal ratio are thought to be a predictor of adverse pregnancy outcome such as: small for gestational age, abnormal fetal heart rate pattern, meconium stained liquor, low Apgar score, and acidosis at birth. PMID 28216258
- Crown-Rump Length - (CRL) measurement used in embryology to more accurately stage the early embryo and fetus. Measured from the curvature at the top (crown) to the curvature at the bottom (rump) of the "C-shaped" early embryo. Used in clinical ultrasound as a measurement between the periods of 7 to 13 weeks as an accurate estimation of the gestational age GA.
- DICOM - (ISO standard 12052:2006) Acronym for Digital Imaging and Communications in Medicine, a clinical standard for handling, storing, printing, and transmitting imaging information.
- Femur length - (FL) is used to determine fetal age and normal development (small/large/abnormal) parameters. The femur is the longest bone in the body and measurements and reflects the longitudinal growth of the fetus (approximately 14 weeks 1.5 cm - term 7.8 cm). It is one of the four typical ultrasound assessments of fetal size and age: Biparietal Diameter (BPD), |Head Circumference (HC), Abdominal Circumference (AC), and Femur Length (FL).
- Fetal size and age - typically measured using 4 ultrasound assessments: Biparietal Diameter (BPD), Head Circumference (HC), Abdominal Circumference (AC), and Femur Length (FL).
- Functional linear discriminant analysis - (FLDA) new growth assessment technique using serial measurements to discriminate between normal and abnormal fetal growth during 2nd and 3rd trimester.
- Head Circumference - (HC) Measured as an ellipse in a horizontal section at the level of the thalamus and the cavum septi pellucidi. 2nd trimester Fetal head growth
- Gestational sac - (GS) size formed initially by the chorionic cavity, after the embryonic period (week 8, GA W10) the amniotic cavity expands and fuses with the chorion. Measured by mean gestation sac diameter.
- inversion mode - an ultrasound processing method of volume analysis for the visualization of fluid-filled fetal structures such as; heart chambers, vessel lumen, stomach, gallbladder, renal pelvis, and the bladder. Post-processing inverts the gray scale of the volume voxels showing the normally anechoic structures in 3D or 4D renderings. This technique has been used to identify cardiac anomalies.
- Linear discriminant analysis - (LDA) to longitudinal data (James and Hastie, 2001)
- Mean gestation sac diameter - (MSD) = (length + height + width)/3. At week 3 (GAweek 5) MSD measures 2-3 mm. Normal MSD (in mm) + 30 = days of pregnancy.
- Mean yolk sac diameter - (MYD) can be used as marker for subsequent embryonic death or abnormalities (PMID 22215774).
- Spatiotemporal image correlation (STIC) - an image acquisition method used mainly for fetal heart analysis. Requires two steps; an automatic volume sweep, then image data analysis according to spatial and temporal domain generating an online dynamic 3D image sequence.
- Transabdominal scan - the ultrasound probe is placed on the external abdomen wall to scan pelvic region structures, conceptus and placenta. Also used to guide prenatal diagnostic techniques of chorionic villus sampling and amniocentesis.
- Transvaginal scan - (TVS) the ultrasound probe is placed inside the vagina and scans for female genital (uterus, ovary) and ectopic pregnancy.
- Termination of pregnancy - (TOP)
| Other Terms Lists |
|---|
| Terms Lists: ART | Birth | Bone | Cardiovascular | Cell Division | Endocrine | Gastrointestinal | Genital | Genetic | Head | Hearing | Heart | Immune | Integumentary | Neonatal | Neural | Oocyte | Palate | Placenta | Radiation | Renal | Respiratory | Spermatozoa | Statistics | Tooth | Ultrasound | Vision | Historic | Drugs | Glossary |
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- Australian Society for Ultrasound Medicine - Guidelines For The Mid Trimester Obstetric Scan PDF (2005)
- American Registry for Diagnostic Medical Sonography - ARDMS Resources for Students and Educators
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2026, Mayıs 24) Embryology Ultrasound - Nuchal Translucency. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Ultrasound_-_Nuchal_Translucency
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G