Paper - Congenital atresia of the oesophagus: Difference between revisions
mNo edit summary |
|||
| Line 25: | Line 25: | ||
==Introduction - Pathological Types== | ==Introduction - Pathological Types== | ||
So many varieties of congenital malformation of the (esophagus have been described that the true nature of the least rare variety of all is often overlooked; this is an atresia or interruption in the continuity of the (esophagus, with, usually, a fistula between the trachea and the distal segment. In 1929 Vogt made a classification of the different types of atresia :— | |||
So many varieties of congenital malformation of the (esophagus have | |||
been described that the true nature of the least rare variety of all is often | |||
overlooked; this is an atresia or interruption in the continuity of the | |||
(esophagus, with, usually, a fistula between the trachea and the distal | |||
segment. In 1929 Vogt made a classification of the different types of | |||
atresia :— | |||
TYPE I.—Complete absence of (esophagus. | TYPE I.—Complete absence of (esophagus. | ||
TYPE II.—Atresia of the (esophagus with an upper and lower | TYPE II.—Atresia of the (esophagus with an upper and lower oesophageal segment, each ending in a blind pouch. | ||
oesophageal segment, each ending in a blind pouch. | |||
TYPE III.—Atresia of the (esophagus with tracheo-(esophageal | TYPE III.—Atresia of the (esophagus with tracheo-(esophageal fistula. | ||
fistula. | |||
(A) With fistula between upper segment and trachea. | (A) With fistula between upper segment and trachea. (13) With fistula between lower segment and trachea. (C) With fistula between both segments and trachea. | ||
(13) With fistula between lower segment and trachea. | |||
(C) With fistula between both segments and trachea. | |||
Eighty per cent. of all cases of atresia are of Type III(B), Fig. 1. That is | Eighty per cent. of all cases of atresia are of Type III(B), Fig. 1. That is to say, the upper segment ends blindly at about the level of the vena azygos arch, or 10 to 12 cm. from the anterior alveolar margin; it is dilated and hypertrophied and remarkably constant in size and shape. The lower segment shows more variation; it springs from the back of the trachea, usually within 1 cm. of the bifurcation, or from the bifurcation itself; within these limits it varies considerably, so that it may overlap the upper segment or it may be separated from it. | ||
to say, the upper segment ends blindly at about the level of the vena | |||
azygos arch, or 10 to 12 cm. from the anterior alveolar margin; it is | |||
dilated and hypertrophied and remarkably constant in size and shape. | |||
The lower segment shows more variation; it springs from the back of | |||
the trachea, usually within 1 cm. of the bifurcation, or from the bifurcation | |||
itself; within these limits it varies considerably, so that it may overlap | |||
the upper segment or it may be separated from it. | |||
The lower segment is nearly always thin-walled and usually about half | The lower segment is nearly always thin-walled and usually about half the calibre of the upper segment. It may be of nearly uniform diameter throughout its length or it may taper as it approaches the trachea. | ||
the calibre of the upper segment. It may be of nearly uniform diameter | |||
throughout its length or it may taper as it approaches the trachea. | |||
These characteristics and variations are of great importance in | These characteristics and variations are of great importance in determining the feasability of anastomosis. | ||
determining the feasability of anastomosis. | |||
C d e | C d e Fig. l. (a) Type III(B), the most common type, accounting for 80 per cent. of all cases. | ||
Fig. l. | |||
(a) Type III(B), the most common type, accounting for | |||
80 per cent. of all cases. | |||
(b) Next most common type. | (b) Next most common type. (c), (d) and (e) All rare. | ||
(c), (d) and (e) All rare. | |||
Type II accounts for most of the cases which do not fall into the | Type II accounts for most of the cases which do not fall into the characteristic group. Type HI(A) and Type III(c) are rare. | ||
characteristic group. Type HI(A) and Type III(c) are rare. | |||
Cameron Haight encountered an example of a single fistula between | Cameron Haight encountered an example of a single fistula between (esophagus and trachea which was not associated with atresia. | ||
(esophagus and trachea which was not associated with atresia. | |||
Historical Note | Historical Note | ||
Gibson, Physician-General to the Army and a grandson of Oliver | Gibson, Physician-General to the Army and a grandson of Oliver Cromwell, described this condition in 1697 and it was mentioned by Durston some 27 years earlier. | ||
Cromwell, described this condition in 1697 and it was mentioned by | |||
Durston some 27 years earlier. | |||
About 250 years elapsed before successful methods of management | About 250 years elapsed before successful methods of management were devised and carried out. The subject was not forgotten during this time. Martin published a case report in 1821, and in 1884 MacKenzie was able to collect records of 43 cases. In 1910 Sir Arthur Keith searched the museums of London and found 14 examples of atresia. He described accurately what we now know to be the most usual type, and gave a satisfactory account of the developmental errors underlying the condition. | ||
were devised and carried out. The subject was not forgotten during this | |||
time. Martin published a case report in 1821, and in 1884 MacKenzie was | |||
able to collect records of 43 cases. In 1910 Sir Arthur Keith searched the | |||
museums of London and found 14 examples of atresia. He described | |||
accurately what we now know to be the most usual type, and gave a | |||
satisfactory account of the developmental errors underlying the condition. | |||
The only type of operation carried out at this period was a simple | The only type of operation carried out at this period was a simple gastrostomy. | ||
gastrostomy. | |||
Honourable exception must be accorded to Richter, who attempted a | Honourable exception must be accorded to Richter, who attempted a rational operation on two infants in 1913, a year memorable for Torek’s successful removal of the thoracic oesophagus for carcinoma. | ||
rational operation on two infants in 1913, a year memorable for Torek’s | |||
successful removal of the thoracic oesophagus for carcinoma. | |||
By 1933 some 300 cases had been reported in the literature; most of | By 1933 some 300 cases had been reported in the literature; most of the reports emphasised the rarity and hopelessness of the condition, while a few of the more adventurous expressed the pious hope that the condition might one day yield to surgery. | ||
the reports emphasised the rarity and hopelessness of the condition, while | |||
a few of the more adventurous expressed the pious hope that the condition | |||
might one day yield to surgery. | |||
Two popular misconceptions have discouraged attempts at treatment, | Two popular misconceptions have discouraged attempts at treatment, first the alleged extreme rarity of the lesion, and second the mistaken idea that this anomaly is usually associated with other and equally serious malformations. | ||
first the alleged extreme rarity of the lesion, and second the mistaken | |||
idea that this anomaly is usually associated with other and equally serious | |||
malformations. | |||
The second misconception is the more insidious in that it gives that | The second misconception is the more insidious in that it gives that final stamp of hopelessness to what is already a very diflicult surgical problem. It is true that Plass (1919) foundthat about half the recorded cases show associated anomalies. But it must also be remembered that in 45 consecutive cases, Cameron Haight found that only one patient had an additional deformity which was incompatible with life. | ||
final stamp of hopelessness to what is already a very diflicult surgical | |||
problem. It is true that Plass (1919) foundthat about half the recorded | |||
cases show associated anomalies. But it must also be remembered that | |||
in 45 consecutive cases, Cameron Haight found that only one patient | |||
had an additional deformity which was incompatible with life. | |||
The possible presence of other abnormalities, particularly imperforate | The possible presence of other abnormalities, particularly imperforate anus, must be recognised, but this recognition must not be used as an argument for regarding the condition as hopeless. | ||
anus, must be recognised, but this recognition must not be used as an | |||
argument for regarding the condition as hopeless. | |||
Most authors have commented on the extreme rarity of the condition | Most authors have commented on the extreme rarity of the condition —the popular figure given being 1 in 50,000 births. Guthrie (1945), searching the material at the Royal Hospital for Sick Children, Glasgow, found that between 1915 and 1944, in 6,916 consecutive post mortem examinations, malformations of the oesophagus were found in 38 subjects, and no fewer than 24 of these provided examples of atresia (1 in 284 autopsies). Six other patients who did not come to autopsy presented suggestive clinical features. At the Postgraduate Medical School of London, from 1935 to 1942, four cases of atresia were found in 10,543 deliveries, or one in 2,635 deliveries. When it is considered that nearly every one of the autopsy cases investigated by Guthrie showed pulmonary complications of great severity, it is reasonable to assume that a number of these infants succumb without the true nature of the lesion being recognised. | ||
—the popular figure given being 1 in 50,000 births. Guthrie (1945), | |||
searching the material at the Royal Hospital for Sick Children, Glasgow, | |||
found that between 1915 and 1944, in 6,916 consecutive post mortem | |||
examinations, malformations of the oesophagus were found in 38 subjects, | |||
and no fewer than 24 of these provided examples of atresia (1 in 284 | |||
autopsies). Six other patients who did not come to autopsy presented | |||
suggestive clinical features. At the Postgraduate Medical School of | |||
London, from 1935 to 1942, four cases of atresia were found in 10,543 | |||
deliveries, or one in 2,635 deliveries. When it is considered that nearly | |||
every one of the autopsy cases investigated by Guthrie showed pulmonary | |||
complications of great severity, it is reasonable to assume that a number | |||
of these infants succumb without the true nature of the lesion being | |||
recognised. | |||
The Surgical Problem | The Surgical Problem | ||
Attempts at feeding fill the blind upper segment so that its contents | Attempts at feeding fill the blind upper segment so that its contents spill over into the trachea to evoke attacks of cyanosis, and, before long, aspiration pneumonia. Even if feeding is avoided, the blind upper sac fills with mucus and saliva unless aspiration is carried out at frequent intervals. Gastrostomy feeds too find their way into the lungs through the distal oesophagus and its tracheal fistula, unless the anomaly is one of the rare forms in which there is a blind lower segment. Apart from the fact that gastric contents may pass into the lungs with fatal results, air passing from the trachea into the stomach sometimes causes considerable gastric distension. A type of spurious or see-saw respiration may even be observed, air passing backwards and forwards from the lungs to the stomach by way of trachea, fistula and oesophagus ; this gastric respiration produces a rapidly increasing anoxia. | ||
spill over into the trachea to evoke attacks of cyanosis, and, before long, | |||
aspiration pneumonia. Even if feeding is avoided, the blind upper sac | |||
fills with mucus and saliva unless aspiration is carried out at frequent intervals. Gastrostomy feeds too find their way into the lungs through the | |||
distal oesophagus and its tracheal fistula, unless the anomaly is one of the | |||
rare forms in which there is a blind lower segment. Apart from the fact | |||
that gastric contents may pass into the lungs with fatal results, air passing | |||
from the trachea into the stomach sometimes causes considerable gastric distension. A type of spurious or see-saw respiration may even be | |||
observed, air passing backwards and forwards from the lungs to the | |||
stomach by way of trachea, fistula and oesophagus ; this gastric respiration | |||
produces a rapidly increasing anoxia. | |||
In an attempt to save these infants, Steele carried out gastrostomy in | In an attempt to save these infants, Steele carried out gastrostomy in 1888. Others followed his example, but all gastrostomies were unsuccessful because of the regurgitation into the lungs. Brenneman (1918) hoped to overcome this difficulty by substituting a jejunostomy for gastrostomy, but again without success. Richter, in 1913, recognised the importance of the fistula and advocated transpleural ligature of the lower (esophagus | ||
1888. Others followed his example, but all gastrostomies were unsuccessful because of the regurgitation into the lungs. Brenneman (1918) hoped | |||
to overcome this difficulty by substituting a jejunostomy for gastrostomy, | |||
but again without success. Richter, in 1913, recognised the importance | |||
of the fistula and advocated transpleural ligature of the lower (esophagus | |||
Fig. 2. Stages in the development of the operation. | |||
Fig. 2. | |||
Stages in the development of the operation. | |||
(a) Simple gastrostomy. | (a) Simple gastrostomy. | ||
(b) Gastrostomy + ligature at cardiac end of the | (b) Gastrostomy + ligature at cardiac end of the (esophagus. | ||
(esophagus. | |||
(c) Formation of a gastric spur. | (c) Formation of a gastric spur. | ||
(d) Formation of stomach tube together with ligature of | (d) Formation of stomach tube together with ligature of lower (esophagus. | ||
lower (esophagus. | |||
(e) Gastrostomy + direct approach to the fistula and | (e) Gastrostomy + direct approach to the fistula and ligature. | ||
ligature. | |||
(f) Exteriorization of both segments. | (f) Exteriorization of both segments. (g) Gastrostomy + (esophagostomy and ligature of fistula. | ||
(g) Gastrostomy + (esophagostomy and ligature of fistula. | |||
(h) Present operation—direct approach and anastomosis. | (h) Present operation—direct approach and anastomosis. | ||
together with gastrostomy. His two cases were unsuccessful, and it must | together with gastrostomy. His two cases were unsuccessful, and it must be noted that he made no provision for keeping the blind upper segment empty. Direct anastomosis by means of the Murphy button was advocated by Von Hacker in 1926 (quoted by Lanman, 1940), but without success. | ||
be noted that he made no provision for keeping the blind upper segment | |||
empty. Direct anastomosis by means of the Murphy button was advocated | |||
by Von Hacker in 1926 (quoted by Lanman, 1940), but without success. | |||
By 1929 there was more general realisation of the nature of the problem, | By 1929 there was more general realisation of the nature of the problem, and its solution was seen to require 1- 1. Prevention of the blind upper segment from filling up and overflowing. | ||
and its solution was seen to require 1- | |||
1. Prevention of the blind upper segment from filling up and | |||
overflowing. | |||
II. Prevention of the regurgitation of gastric contents through the | II. Prevention of the regurgitation of gastric contents through the fistula into the trachea. | ||
fistula into the trachea. | |||
III. Successful feeding of the infants. | III. Successful feeding of the infants. | ||
During the next few years all sorts of methods were adopted to achieve | During the next few years all sorts of methods were adopted to achieve these results, and the names of Mixter, Leven, Gage and Ochsner, Gamble and Ladd are all associated with multiple operations which include cervical oesophagostomy, various types of gastrostomy, transection of the stomach and ligature of the fistula. Out of all these attempts only two were completely successful at this time; the staged operations performed by Ladd in 1939, and Leven in 1940. | ||
these results, and the names of Mixter, Leven, Gage and Ochsner, Gamble | |||
and Ladd are all associated with multiple operations which include | |||
cervical oesophagostomy, various types of gastrostomy, transection of | |||
the stomach and ligature of the fistula. Out of all these attempts only | |||
two were completely successful at this time; the staged operations | |||
performed by Ladd in 1939, and Leven in 1940. | |||
The multiple-stage operation presents the patient and the surgeon with | The multiple-stage operation presents the patient and the surgeon with so difficult a succession of hurdles even if the infant survives the early procedures, that Lanman ventured a primary anastomosis by the extrapleural route in 1936, but none of his patients survived. | ||
so difficult a succession of hurdles even if the infant survives the early | |||
procedures, that Lanman ventured a primary anastomosis by the extrapleural route in 1936, but none of his patients survived. | |||
Haight and Townsley reported in 1941 the first completely successful | Haight and Townsley reported in 1941 the first completely successful direct anastomosis, and the tendency now is to favour direct anastomosis wherever possible. The development of the operation is shown in Fig. 2. | ||
direct anastomosis, and the tendency now is to favour direct anastomosis | |||
wherever possible. The development of the operation is shown in Fig. 2. | |||
The transpleural and extrapleural routes have each had their supporters. | The transpleural and extrapleural routes have each had their supporters. Haight and Townsley used the latter in their first successful case. The anastomosis is less diflicult by the transpleural route and the operation seems to be well tolerated, but up to the present time this approach has, generally speaking, proved unsuccessful, although Singleton and Knight report the case of a patient who lived for over seven months following the transpleural operation, and whose death then was probably due to a fistula of the trachea, unsuspected during life, with the upper blind segment of the (esophagus (Vogt’s Type III(c)). | ||
Haight and Townsley used the latter in their first successful case. The | |||
anastomosis is less diflicult by the transpleural route and the operation | |||
seems to be well tolerated, but up to the present time this approach has, | |||
generally speaking, proved unsuccessful, although Singleton and Knight | |||
report the case of a patient who lived for over seven months following | |||
the transpleural operation, and whose death then was probably due to a | |||
fistula of the trachea, unsuspected during life, with the upper blind | |||
segment of the (esophagus (Vogt’s Type III(c)). | |||
Impressed with the difliculties which I experienced in carrying out the | Impressed with the difliculties which I experienced in carrying out the extrapleural operation, both in the postmortem room and in the operating theatre, I concentrated at first on the right transpleural approach, but have been forced to the conclusion that in the anastomosis of such a delicate structure as the infant’s oesophagus, it is diflicult to avoid leakage, and if the leak occurs inside the pleural cavity it is likely to be fatal. My own experience, which has impressed me with the value of the extrapleural procedure, has been gained in the following cases :— | ||
extrapleural operation, both in the postmortem room and in the operating | |||
theatre, I concentrated at first on the right transpleural approach, but | |||
have been forced to the conclusion that in the anastomosis of such a | |||
delicate structure as the infant’s oesophagus, it is diflicult to avoid leakage, | |||
and if the leak occurs inside the pleural cavity it is likely to be fatal. My own experience, which has impressed me with the value of the extrapleural procedure, has been gained in the following cases :— | |||
OPERATIONS ON CASES or CONGENITAL ATRESIA or OESOPHAGUS 1938-1946. FRANKLIN | OPERATIONS ON CASES or CONGENITAL ATRESIA or OESOPHAGUS 1938-1946. FRANKLIN | ||
Sex and Birth | Sex and Birth Case Date Age Weight Procedure Survival Remarks -(Hours) and Type | ||
Case Date Age Weight Procedure Survival Remarks | |||
-(Hours) and Type | |||
4:417 1 1: | 4:417 1 1: | ||
1 21.11.38 M. 61b. 7oz. Ligature of cardia and 7 days Silk ligature slowly cut | 1 21.11.38 M. 61b. 7oz. Ligature of cardia and 7 days Silk ligature slowly cut 72 III(B) gastrostomy through and re-established . the fistula 2 16.10.41 M. Prem. 41b. 5oz. Transpleural (R). 17 hours Pneumonia 84 III(B) Anastomosis 3 31.5.42 F. Prem. 51b. 8oz. Transpleural (R). Fistula Died on Massive collapse of both 148 III(B) ligated_ and divided, table lungs tube tied into lower segment 4 2.11.43 F. Prem. 41b. 3oz. Transpleural (R). 5} days Leakage of anastomosis. 72 III(B) Anastomosis Case reported (O’REILLY, l N.. FRANKLIN. R. H.. and DALEY, M. D.. 1944) 5 6.11.45 F. Prem. Transpleural (R). 43 hours _ Pneumonia III(,a) Tube tied into each segment ' 6 13.1.46 F. | 51b. 8oz. Transpleural (R). 52 hours Pneumonia 28 III(B) Fistula ligated and | divided. Gastrostomy 7 21.2.46 F. 51b. 6oz. Extrapleural approach 27 hours Pulmonary collapse I 120 III(n) attempted. Pleura tore badly._ Anastomosis with difficulty 8 i27.l0.46 F. 71b. 2oz. Transpleural (R). 25 hours Consolidation both lungs. I 72 II No fistula. Lower scg- Patent ductus arteriosus. ment ended 1-5 cm. No gastric gas bubble was above diaphragm. seen at X-ray—this should I Gastrostomy | have led to the correct diagnosis of type 9 10.1.47 F. 71b. 7oz. Extrapleural (R). Alive and Gastrostomy carried out 72 HI(B) Anastomosis well 6 days after anastomosis. Gastrostomy tube re. moved after 12 days. Infant now takes food normally and has made I good progress. (Previously re orted, FRANKLIN, R. .. 1947) 10 24.4.47 F. 61b. 7oz. Extrapleural (R). Alive and Gastrostomy _was not 48 III(a) Anastomosis well necessary in this case. The | ||
72 III(B) gastrostomy through and re-established | |||
. the fistula | |||
2 16.10.41 M. Prem. 41b. 5oz. Transpleural (R). 17 hours Pneumonia | |||
84 III(B) Anastomosis | |||
3 31.5.42 F. Prem. 51b. 8oz. Transpleural (R). Fistula Died on Massive collapse of both | |||
148 III(B) ligated_ and divided, table lungs | |||
tube tied into lower | |||
segment | |||
4 2.11.43 F. Prem. 41b. 3oz. Transpleural (R). 5} days Leakage of anastomosis. | |||
72 III(B) Anastomosis Case reported (O’REILLY, | |||
l N.. FRANKLIN. R. H.. and | |||
DALEY, M. D.. 1944) | |||
5 6.11.45 F. Prem. Transpleural (R). 43 hours _ Pneumonia | |||
III(,a) Tube tied into each | |||
segment ' | |||
6 13.1.46 F. | 51b. 8oz. Transpleural (R). 52 hours Pneumonia | |||
28 III(B) Fistula ligated and | |||
| divided. Gastrostomy | |||
7 21.2.46 F. 51b. 6oz. Extrapleural approach 27 hours Pulmonary collapse | |||
I 120 III(n) attempted. Pleura tore | |||
badly._ Anastomosis | |||
with difficulty | |||
8 i27.l0.46 F. 71b. 2oz. Transpleural (R). 25 hours Consolidation both lungs. | |||
I 72 II No fistula. Lower scg- Patent ductus arteriosus. | |||
ment ended 1-5 cm. No gastric gas bubble was | |||
above diaphragm. seen at X-ray—this should | |||
I Gastrostomy | have led to the correct | |||
diagnosis of type | |||
9 10.1.47 F. 71b. 7oz. Extrapleural (R). Alive and Gastrostomy carried out | |||
72 HI(B) Anastomosis well 6 days after anastomosis. | |||
Gastrostomy tube re. moved after 12 days. | |||
Infant now takes food | |||
normally and has made | |||
I good progress. (Previously re orted, | |||
FRANKLIN, R. .. 1947) | |||
10 24.4.47 F. 61b. 7oz. Extrapleural (R). Alive and Gastrostomy _was not | |||
48 III(a) Anastomosis well necessary in this case. The | |||
infant made a smooth | infant made a smooth H recovery and has since progressed well. (Previously ilwegizggted. FRANKLIN, R. H.. | ||
H recovery and has since progressed well. (Previously | |||
ilwegizggted. FRANKLIN, R. H.. | |||
Diagnosis | Diagnosis | ||
Cyanosis associated with excess of mucus in the nasopharynx may be | Cyanosis associated with excess of mucus in the nasopharynx may be noted at birth in many normal infants. Improvement in these occurs after aspiration, but the child suffering from atresia has recurrent attacks of cyanosis which are usually severe enough to excite notice, but which are often attributed to other causes, such as tentorial tears and atelectasis. When feeds are started all the symptoms are accentuated, the child is often avid for its feed and sucks strongly, only to be overwhelmed by an attack of spluttering and cyanosis, accompanied by the complete regurgitation of the feed. Aspiration of the nasopharynx effects an immediate improvement, but the symptoms recur as soon as feeding is attempted again. | ||
noted at birth in many normal infants. Improvement in these occurs | |||
after aspiration, but the child suffering from atresia has recurrent attacks | |||
of cyanosis which are usually severe enough to excite notice, but which | |||
are often attributed to other causes, such as tentorial tears and atelectasis. | |||
When feeds are started all the symptoms are accentuated, the child is | |||
often avid for its feed and sucks strongly, only to be overwhelmed by an | |||
attack of spluttering and cyanosis, accompanied by the complete regurgitation of the feed. Aspiration of the nasopharynx effects an immediate | |||
improvement, but the symptoms recur as soon as feeding is attempted | |||
again. | |||
These symptoms are so striking and alarming that they seldom escape | These symptoms are so striking and alarming that they seldom escape notice, and it cannot be too strongly emphasised that such a train of symptoms usually indicate oesophageal atresia. Midwives and others who have the care of infants in the first hours of life, should be taught that atresia is the commonest cause of persistent choking and cyanosis in the newborn child. | ||
notice, and it cannot be too strongly emphasised that such a train of | |||
symptoms usually indicate oesophageal atresia. Midwives and others | |||
who have the care of infants in the first hours of life, should be taught | |||
that atresia is the commonest cause of persistent choking and cyanosis | |||
in the newborn child. | |||
Once the suspicion of atresia has been raised, all mouth feeding is | Once the suspicion of atresia has been raised, all mouth feeding is stopped and the nasopharynx is aspirated at frequent intervals. | ||
stopped and the nasopharynx is aspirated at frequent intervals. | |||
To confirm the diagnosis, a well-lubricated rubber catheter is passed | To confirm the diagnosis, a well-lubricated rubber catheter is passed through the mouth and down the oesophagus. Its arrest 10-12 cm. from the anterior alveolar margin is practically diagnostic of atresia. | ||
through the mouth and down the oesophagus. Its arrest 10-12 cm. from | |||
the anterior alveolar margin is practically diagnostic of atresia. | |||
Final confirmation of the diagnosis is radiological, but the practice of | Final confirmation of the diagnosis is radiological, but the practice of giving a Barium swallow is to be condemned. The emulsion is almost certain to spill over into the lungs and the child’s slender chance of survival is still further reduced. The best method to adopt is as follows :— | ||
giving a Barium swallow is to be condemned. The emulsion is almost | |||
certain to spill over into the lungs and the child’s slender chance of survival | |||
is still further reduced. The best method to adopt is as follows :— | |||
The infant is screened and a careful assessment is made of the condition | The infant is screened and a careful assessment is made of the condition of the lungs; the stomach and intestines are then examined for the presence of air. If air is present in the stomach and intestines below an (esophageal atresia it is proof that a fistula exists between the lower segment and trachea. The converse is usually, but not invariably, true. | ||
of the lungs; the stomach and intestines are then examined for the | |||
presence of air. If air is present in the stomach and intestines below an | |||
(esophageal atresia it is proof that a fistula exists between the lower | |||
segment and trachea. The converse is usually, but not invariably, true. | |||
A catheter is now passed into the upper segment and l to 2 cc. of | A catheter is now passed into the upper segment and l to 2 cc. of lipiodol is gently introduced under direct observation against the screen. | ||
lipiodol is gently introduced under direct observation against the screen. | |||
The appearance of the blind segment is characteristic, and as soon as it | The appearance of the blind segment is characteristic, and as soon as it has been observed and the rare presence of a fistula in the upper segment excluded, the lipiodol is withdrawn (Figs. 3, 4 and 5). Bronchoscopic examination has been used to inspect the fistula and so confirm the diagnosis (Pilcher). Apart from the passage of a catheter into the blind sac and frequent aspiration, the important features in the management of the diagnostic stage are negative rather than positive. The chief safety factors are the avoidance of any further feeding and of unskilled attempts at X-ray diagnosis. | ||
has been observed and the rare presence of a fistula in the upper segment | |||
excluded, the lipiodol is withdrawn (Figs. 3, 4 and 5). Bronchoscopic | |||
examination has been used to inspect the fistula and so confirm the | |||
diagnosis (Pilcher). Apart from the passage of a catheter into the blind | |||
sac and frequent aspiration, the important features in the management | |||
of the diagnostic stage are negative rather than positive. The chief safety | |||
factors are the avoidance of any further feeding and of unskilled attempts | |||
at X-ray diagnosis. | |||
Management after the Diagnosis has been Confirmed | Management after the Diagnosis has been Confirmed | ||
The complete diagnosis not only confirms the presence of atresia, but | The complete diagnosis not only confirms the presence of atresia, but in many cases discloses the precise nature of the deformity. It must be emphasised once more that 80 per cent. of the cases fall into the characteristic group of (esophageal atresia with fistula between trachea and lower oesophageal segment. | ||
in many cases discloses the precise nature of the deformity. It must be | |||
emphasised once more that 80 per cent. of the cases fall into the characteristic group of (esophageal atresia with fistula between trachea and lower | |||
oesophageal segment. | |||
The preparation of the patient for operation requires the full collaboration of an expert paediatrician, as well as the whole-time services of an | The preparation of the patient for operation requires the full collaboration of an expert paediatrician, as well as the whole-time services of an intelligent and conscientious nurse. In fact, without these two essentials before and after operation, any surgical intervention is almost certain to fail. | ||
intelligent and conscientious nurse. In fact, without these two essentials | |||
before and after operation, any surgical intervention is almost certain to | |||
fail. | |||
The three essentials in the pre-operative period are : to keep the blind | The three essentials in the pre-operative period are : to keep the blind sac empty by aspiration, to improve the state of the lungs by changing the child’s position frequently and systematically, and to administer the | ||
sac empty by aspiration, to improve the state of the lungs by changing the | |||
child’s position frequently and systematically, and to administer the | |||
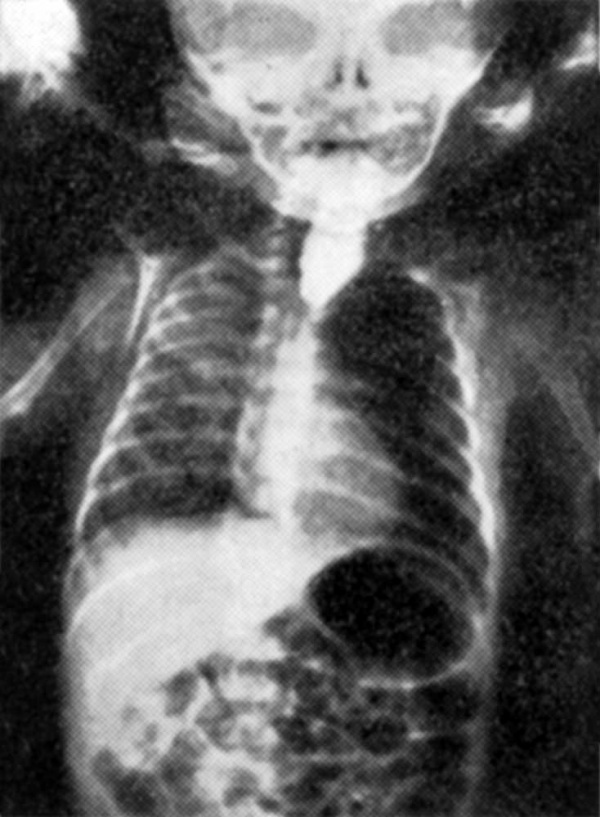
X-ray showing large air bubble in Blind upper segment filled with iodised | X-ray showing large air bubble in Blind upper segment filled with iodised | ||
stomach and blind upper esophageal oil. Care has been taken not to allow | stomach and blind upper esophageal oil. Care has been taken not to allow segment filled with iodised oil. any to spill over into the larynx. | ||
segment filled with iodised oil. any to spill over into the larynx. | |||
Fig. 5 | Fig. 5 An earlier case in which the importance of great care in X-ray diagnosis was not fully appreciated and the iodised oil has spilled over into the lungs. Although the oesophagus was restored and is seen to be functioning, the_pulrnonary condition contributed to the unsuccessful result in this case. | ||
An earlier case in which the importance of great care in | |||
X-ray diagnosis was not fully appreciated and the iodised | |||
oil has spilled over into the lungs. Although the oesophagus was restored and is seen to be functioning, the_pulrnonary | |||
condition contributed to the unsuccessful result in this case. | |||
requisite fluid parenterally. The fluid requirement is difficult to assess, | requisite fluid parenterally. The fluid requirement is difficult to assess, and giving too much is probably more dangerous than giving too little. | ||
and giving too much is probably more dangerous than giving too little. | |||
The operation | The operation | ||
The child is secured in a prone position over a rubber hot-water bottle, | The child is secured in a prone position over a rubber hot-water bottle, half-filled with warm water. A small pad is placed under the right shoulder | ||
half-filled with warm water. A small pad is placed under the right shoulder | |||
‘and the head is turned to the right. Local anaesthesia (1 per cent. Procain) | ‘and the head is turned to the right. Local anaesthesia (1 per cent. Procain) | ||
is used for the skin incision and the anaesthetist concentrates on keeping | is used for the skin incision and the anaesthetist concentrates on keeping the upper oesophageal segment empty and administering oxygen unde pressure from time to time. T | ||
the upper oesophageal segment empty and administering oxygen unde | |||
pressure from time to time. T | |||
The incision is curved (Fig. 6), starting 1 cm. lateral to the spine, | The incision is curved (Fig. 6), starting 1 cm. lateral to the spine, over the second rib, passing downwards parallel to the spine over the third and fourth ribs and then outwards crossing the fifth rib obliquely and ending over the sixth rib. Part of the fifth rib is resected subperiosteally, extreme care being necessary to avoid opening the pleura. The correct extrapleural plane having been found, the incision is deepened through the chest wall with division of the fourth, third and second ribs and their intercostal bundles. The pleura is carefully displaced until the vena azygos arch is seen. This usually marks the lower end of the upper blind segment and it is divided between ligatures with great care. | ||
over the second rib, passing downwards parallel to the spine over the | |||
third and fourth ribs and then outwards crossing the fifth rib obliquely | |||
and ending over the sixth rib. Part of the fifth rib is resected subperiosteally, extreme care being necessary to avoid opening the pleura. The | |||
correct extrapleural plane having been found, the incision is deepened | |||
through the chest wall with division of the fourth, third and second | |||
ribs and their intercostal bundles. The pleura is carefully displaced until | |||
the vena azygos arch is seen. This usually marks the lower end of the | |||
upper blind segment and it is divided between ligatures with great care. | |||
Scar after mediastinal incision. | Scar after mediastinal incision. Fig. 6 | ||
Fig. 6 | |||
The lower oesophageal segment emerges from the posterior surface of | The lower oesophageal segment emerges from the posterior surface of the trachea or from the bifurcation itself. Gentle movement of the catheter in the upper segment helps in identification. The fistula is ligatured close to the trachea and divided, with conservation of as much as possible of the lower segment, and traction sutures are introduced into each segment to avoid handling them unnecessarily. | ||
the trachea or from the bifurcation itself. Gentle movement of the | |||
catheter in the upper segment helps in identification. The fistula is | |||
ligatured close to the trachea and divided, with conservation of as much | |||
as possible of the lower segment, and traction sutures are introduced | |||
into each segment to avoid handling them unnecessarily. | |||
Anastomosis is undertaken if it seems feasible without undue tension, | Anastomosis is undertaken if it seems feasible without undue tension, and it is performed with the use of fine silk and small, curved, eyeless round-bodied needles. Various methods of anastomosis have been described, but none of them is easy. The structures are delicate and readily damaged, and there is a great tendency for the stitches to cut out. A catheter introduced into the (esophagus from the mouth during the later stages is of great help. On completion of the anastomosis the area is well dusted with penicillin powder, the wound is closed around a small rubber drain, and the oesophageal tube is removed. | ||
and it is performed with the use of fine silk and small, curved, eyeless | |||
round-bodied needles. Various methods of anastomosis have been | |||
described, but none of them is easy. The structures are delicate and readily damaged, and there is a great tendency for the stitches to cut out. | |||
A catheter introduced into the (esophagus from the mouth during the | |||
later stages is of great help. On completion of the anastomosis the area | |||
is well dusted with penicillin powder, the wound is closed around a small | |||
rubber drain, and the oesophageal tube is removed. | |||
If anastomosis has proved impossible, Humphreys has advised that the | If anastomosis has proved impossible, Humphreys has advised that the first stage of a multiple-stage operation be carried out. A finger is passed along the back of the trachea into the base of the neck near the suprasternal notch. An incision is made between the right sternomastoid and the trachea, and through this the upper segment is drawn to establish a cervical oesophagostomy. If a fistula is present it is ligated and divided at this first stage, but failure to effect an anastomosis may be due to the absence of a fistula ; the blind ends of the oesophagus being further apart when atresia is uncomplicated (Type II) than when a tracheo-oesophageal fistula is present as well (Type III(B)). | ||
first stage of a multiple-stage operation be carried out. A finger is passed | |||
along the back of the trachea into the base of the neck near the suprasternal notch. An incision is made between the right sternomastoid and | |||
the trachea, and through this the upper segment is drawn to establish a | |||
cervical oesophagostomy. If a fistula is present it is ligated and divided | |||
at this first stage, but failure to effect an anastomosis may be due to the | |||
absence of a fistula ; the blind ends of the oesophagus being further apart | |||
when atresia is uncomplicated (Type II) than when a tracheo-oesophageal | |||
fistula is present as well (Type III(B)). | |||
After-care | After-care | ||
The child is nursed in an oxygen tent and the same care is taken to | The child is nursed in an oxygen tent and the same care is taken to aspirate the nasopharynx as before operation. A small blood transfusion (100 cc.) may be given, followed by an intravenous drip of N/5 glucose saline. The fluid and salt balance must be controlled with great care and is best entrusted to a skilled paediatrician. | ||
aspirate the nasopharynx as before operation. A small blood transfusion | |||
(100 cc.) may be given, followed by an intravenous drip of N/5 glucose | |||
saline. The fluid and salt balance must be controlled with great care and | |||
is best entrusted to a skilled paediatrician. | |||
Immediately after the operation, feeds of penicillin solution (10,000 | Immediately after the operation, feeds of penicillin solution (10,000 units) hourly are started by mouth. The mediastinal drainage tube is removed on the third or fourth day and the patency of the oesophagus is tested radiographically with iodised oil; if the reconstructed oesophagus conducts the oil without leakage, feeds of expressed breast milk are begun. | ||
units) hourly are started by mouth. The mediastinal drainage tube is | |||
removed on the third or fourth day and the patency of the oesophagus is | |||
tested radiographically with iodised oil; if the reconstructed oesophagus | |||
conducts the oil without leakage, feeds of expressed breast milk are | |||
begun. | |||
Gastrostomy is performed only if the swallow of iodised oil demonstrates a mediastinal leak; even if it is shown to be necessary by this | Gastrostomy is performed only if the swallow of iodised oil demonstrates a mediastinal leak; even if it is shown to be necessary by this criterion, its performance is best deferred until the seventh or eighth day after oesophageal repair. | ||
criterion, its performance is best deferred until the seventh or eighth day | |||
after oesophageal repair. | |||
Results in Other Centres | Results in Other Centres Ha1'ght’.<' results to 1946 :— | ||
Ha1'ght’.<' results to 1946 :— | |||
45 consecutive patients. | 45 consecutive patients. | ||
42 had associated tracheo-oesophageal fistula ; one additional patient | 42 had associated tracheo-oesophageal fistula ; one additional patient had a tracheo-oesophageal fistula without (esophageal atresia. | ||
had a tracheo-oesophageal fistula without (esophageal atresia. | |||
36 patients were explored. | 36 patients were explored. | ||
| Line 448: | Line 199: | ||
9 patients survived operation from 6 months to 4% years. | 9 patients survived operation from 6 months to 4% years. | ||
Only one patient in this series had an additional anomaly | Only one patient in this series had an additional anomaly which was incompatible with life. | ||
which was incompatible with life. | |||
Ladd’s results to 1944 :— | Ladd’s results to 1944 :— | ||
34 patients explored. | 34 patients explored. 28 patients submitted to a staged operation ; nine living. 6 patients treated by primary anastomosis ; two living. Ladd’s first success was a staged operation in November, 1939; an antethoracic (Esophagus was constructed and the child was reported alive at the age of 4;} years. | ||
28 patients submitted to a staged operation ; nine living. | |||
6 patients treated by primary anastomosis ; two living. | |||
Ladd’s first success was a staged operation in November, 1939; | |||
an antethoracic (Esophagus was constructed and the child | |||
was reported alive at the age of 4;} years. | |||
Conclusions | Conclusions | ||
This paper is presented in the hope that midwives and paediatricians | This paper is presented in the hope that midwives and paediatricians will regard all newborn infants who sufl"er from attacks of cyanosis and choking, together with the regurgitation of feeds, to be subjects of atresia of the oesophagus until the oesophagus can be shown, by the clinical and radiological methods described, to be normal. | ||
will regard all newborn infants who sufl"er from attacks of cyanosis and | |||
choking, together with the regurgitation of feeds, to be subjects of atresia | |||
of the oesophagus until the oesophagus can be shown, by the clinical and | |||
radiological methods described, to be normal. | |||
If this attitude is inculcated and lethal attempts at feeding are stopped | If this attitude is inculcated and lethal attempts at feeding are stopped until the condition of the oesophagus has been determined by the simple passage of a catheter, we shall have more frequent opportunities of treating these little patients before aspiration pneumonia has jeopardised their chances of recovery. | ||
until the condition of the oesophagus has been determined by the simple | |||
passage of a catheter, we shall have more frequent opportunities of | |||
treating these little patients before aspiration pneumonia has jeopardised | |||
their chances of recovery. | |||
The radiologist can contribute to the success of the operation by | The radiologist can contribute to the success of the operation by refraining from any form of examination which risks filling the lungs with opaque medium and the surgeon can prepare himself for a difficult operative procedure by a study of the varied pathology of (Esophageal atresia and of the methods which have proved successful in its treatment. | ||
refraining from any form of examination which risks filling the lungs with | |||
opaque medium and the surgeon can prepare himself for a difficult | |||
operative procedure by a study of the varied pathology of (Esophageal | |||
atresia and of the methods which have proved successful in its treatment. | |||
REFERENCES | REFERENCES | ||
| Line 492: | Line 225: | ||
HOLT, F. J., HAIGHT, C. and HODGES, F. J. (1946) Radiology 47, 457. | HOLT, F. J., HAIGHT, C. and HODGES, F. J. (1946) Radiology 47, 457. | ||
GIBSON, T. (1697) The Anatomy of humane bodies epitomized, 5th Ed. London, p. 239. | GIBSON, T. (1697) The Anatomy of humane bodies epitomized, 5th Ed. London, p. 239. MACKENZIE, M. (1884) Diseases of the throat and nose. | ||
MACKENZIE, M. (1884) Diseases of the throat and nose. | |||
KEITH, A. (1910) Brit. Med. J. 1, 301. | KEITH, A. (1910) Brit. Med. J. 1, 301. | ||
| Line 523: | Line 255: | ||
Carroll & Co. | Carroll & Co. | ||
O’REILLY, N., FRANKLIN, R. H. and DALEY, M. D. (1944) Arch. Dis. Child. 19, 131. | O’REILLY, N., FRANKLIN, R. H. and DALEY, M. D. (1944) Arch. Dis. Child. 19, 131. FRANKLIN, R. H. (1947) Lancet 2, 243. | ||
FRANKLIN, R. H. (1947) Lancet 2, 243. | |||
HUMPHREYS, G. H. (1944) Surgery 15, 801. | HUMPHREYS, G. H. (1944) Surgery 15, 801. | ||
{{Footer}} | {{Footer}} | ||
[[File:Franklin1948 fig03.jpg|600px]] | [[File:Franklin1948 fig03.jpg|600px]] | ||
Revision as of 14:12, 29 November 2017
| Embryology - 26 Apr 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Franklin RH. Congenital atresia of the oesophagus. (1948) Ann R Coll Surg Engl. 2(2): 69–79.
| Historic Disclaimer - information about historic embryology pages |
|---|
| Pages where the terms "Historic" (textbooks, papers, people, recommendations) appear on this site, and sections within pages where this disclaimer appears, indicate that the content and scientific understanding are specific to the time of publication. This means that while some scientific descriptions are still accurate, the terminology and interpretation of the developmental mechanisms reflect the understanding at the time of original publication and those of the preceding periods, these terms, interpretations and recommendations may not reflect our current scientific understanding. (More? Embryology History | Historic Embryology Papers) |
Congenital Atresia of the Oesophagus=
Hunterian Lecture delivered at the Royal College of Surgeons of England
on 16th January, 1947 by
R. H. Franklin, M.B., B.S., F.R.C.S.,
Department of Surgery, Postgraduate Medical School of London
Introduction - Pathological Types
So many varieties of congenital malformation of the (esophagus have been described that the true nature of the least rare variety of all is often overlooked; this is an atresia or interruption in the continuity of the (esophagus, with, usually, a fistula between the trachea and the distal segment. In 1929 Vogt made a classification of the different types of atresia :—
TYPE I.—Complete absence of (esophagus.
TYPE II.—Atresia of the (esophagus with an upper and lower oesophageal segment, each ending in a blind pouch.
TYPE III.—Atresia of the (esophagus with tracheo-(esophageal fistula.
(A) With fistula between upper segment and trachea. (13) With fistula between lower segment and trachea. (C) With fistula between both segments and trachea.
Eighty per cent. of all cases of atresia are of Type III(B), Fig. 1. That is to say, the upper segment ends blindly at about the level of the vena azygos arch, or 10 to 12 cm. from the anterior alveolar margin; it is dilated and hypertrophied and remarkably constant in size and shape. The lower segment shows more variation; it springs from the back of the trachea, usually within 1 cm. of the bifurcation, or from the bifurcation itself; within these limits it varies considerably, so that it may overlap the upper segment or it may be separated from it.
The lower segment is nearly always thin-walled and usually about half the calibre of the upper segment. It may be of nearly uniform diameter throughout its length or it may taper as it approaches the trachea.
These characteristics and variations are of great importance in determining the feasability of anastomosis.
C d e Fig. l. (a) Type III(B), the most common type, accounting for 80 per cent. of all cases.
(b) Next most common type. (c), (d) and (e) All rare.
Type II accounts for most of the cases which do not fall into the characteristic group. Type HI(A) and Type III(c) are rare.
Cameron Haight encountered an example of a single fistula between (esophagus and trachea which was not associated with atresia.
Historical Note
Gibson, Physician-General to the Army and a grandson of Oliver Cromwell, described this condition in 1697 and it was mentioned by Durston some 27 years earlier.
About 250 years elapsed before successful methods of management were devised and carried out. The subject was not forgotten during this time. Martin published a case report in 1821, and in 1884 MacKenzie was able to collect records of 43 cases. In 1910 Sir Arthur Keith searched the museums of London and found 14 examples of atresia. He described accurately what we now know to be the most usual type, and gave a satisfactory account of the developmental errors underlying the condition.
The only type of operation carried out at this period was a simple gastrostomy.
Honourable exception must be accorded to Richter, who attempted a rational operation on two infants in 1913, a year memorable for Torek’s successful removal of the thoracic oesophagus for carcinoma.
By 1933 some 300 cases had been reported in the literature; most of the reports emphasised the rarity and hopelessness of the condition, while a few of the more adventurous expressed the pious hope that the condition might one day yield to surgery.
Two popular misconceptions have discouraged attempts at treatment, first the alleged extreme rarity of the lesion, and second the mistaken idea that this anomaly is usually associated with other and equally serious malformations.
The second misconception is the more insidious in that it gives that final stamp of hopelessness to what is already a very diflicult surgical problem. It is true that Plass (1919) foundthat about half the recorded cases show associated anomalies. But it must also be remembered that in 45 consecutive cases, Cameron Haight found that only one patient had an additional deformity which was incompatible with life.
The possible presence of other abnormalities, particularly imperforate anus, must be recognised, but this recognition must not be used as an argument for regarding the condition as hopeless.
Most authors have commented on the extreme rarity of the condition —the popular figure given being 1 in 50,000 births. Guthrie (1945), searching the material at the Royal Hospital for Sick Children, Glasgow, found that between 1915 and 1944, in 6,916 consecutive post mortem examinations, malformations of the oesophagus were found in 38 subjects, and no fewer than 24 of these provided examples of atresia (1 in 284 autopsies). Six other patients who did not come to autopsy presented suggestive clinical features. At the Postgraduate Medical School of London, from 1935 to 1942, four cases of atresia were found in 10,543 deliveries, or one in 2,635 deliveries. When it is considered that nearly every one of the autopsy cases investigated by Guthrie showed pulmonary complications of great severity, it is reasonable to assume that a number of these infants succumb without the true nature of the lesion being recognised.
The Surgical Problem
Attempts at feeding fill the blind upper segment so that its contents spill over into the trachea to evoke attacks of cyanosis, and, before long, aspiration pneumonia. Even if feeding is avoided, the blind upper sac fills with mucus and saliva unless aspiration is carried out at frequent intervals. Gastrostomy feeds too find their way into the lungs through the distal oesophagus and its tracheal fistula, unless the anomaly is one of the rare forms in which there is a blind lower segment. Apart from the fact that gastric contents may pass into the lungs with fatal results, air passing from the trachea into the stomach sometimes causes considerable gastric distension. A type of spurious or see-saw respiration may even be observed, air passing backwards and forwards from the lungs to the stomach by way of trachea, fistula and oesophagus ; this gastric respiration produces a rapidly increasing anoxia.
In an attempt to save these infants, Steele carried out gastrostomy in 1888. Others followed his example, but all gastrostomies were unsuccessful because of the regurgitation into the lungs. Brenneman (1918) hoped to overcome this difficulty by substituting a jejunostomy for gastrostomy, but again without success. Richter, in 1913, recognised the importance of the fistula and advocated transpleural ligature of the lower (esophagus
Fig. 2. Stages in the development of the operation.
(a) Simple gastrostomy.
(b) Gastrostomy + ligature at cardiac end of the (esophagus.
(c) Formation of a gastric spur.
(d) Formation of stomach tube together with ligature of lower (esophagus.
(e) Gastrostomy + direct approach to the fistula and ligature.
(f) Exteriorization of both segments. (g) Gastrostomy + (esophagostomy and ligature of fistula.
(h) Present operation—direct approach and anastomosis.
together with gastrostomy. His two cases were unsuccessful, and it must be noted that he made no provision for keeping the blind upper segment empty. Direct anastomosis by means of the Murphy button was advocated by Von Hacker in 1926 (quoted by Lanman, 1940), but without success.
By 1929 there was more general realisation of the nature of the problem, and its solution was seen to require 1- 1. Prevention of the blind upper segment from filling up and overflowing.
II. Prevention of the regurgitation of gastric contents through the fistula into the trachea.
III. Successful feeding of the infants.
During the next few years all sorts of methods were adopted to achieve these results, and the names of Mixter, Leven, Gage and Ochsner, Gamble and Ladd are all associated with multiple operations which include cervical oesophagostomy, various types of gastrostomy, transection of the stomach and ligature of the fistula. Out of all these attempts only two were completely successful at this time; the staged operations performed by Ladd in 1939, and Leven in 1940.
The multiple-stage operation presents the patient and the surgeon with so difficult a succession of hurdles even if the infant survives the early procedures, that Lanman ventured a primary anastomosis by the extrapleural route in 1936, but none of his patients survived.
Haight and Townsley reported in 1941 the first completely successful direct anastomosis, and the tendency now is to favour direct anastomosis wherever possible. The development of the operation is shown in Fig. 2.
The transpleural and extrapleural routes have each had their supporters. Haight and Townsley used the latter in their first successful case. The anastomosis is less diflicult by the transpleural route and the operation seems to be well tolerated, but up to the present time this approach has, generally speaking, proved unsuccessful, although Singleton and Knight report the case of a patient who lived for over seven months following the transpleural operation, and whose death then was probably due to a fistula of the trachea, unsuspected during life, with the upper blind segment of the (esophagus (Vogt’s Type III(c)).
Impressed with the difliculties which I experienced in carrying out the extrapleural operation, both in the postmortem room and in the operating theatre, I concentrated at first on the right transpleural approach, but have been forced to the conclusion that in the anastomosis of such a delicate structure as the infant’s oesophagus, it is diflicult to avoid leakage, and if the leak occurs inside the pleural cavity it is likely to be fatal. My own experience, which has impressed me with the value of the extrapleural procedure, has been gained in the following cases :—
OPERATIONS ON CASES or CONGENITAL ATRESIA or OESOPHAGUS 1938-1946. FRANKLIN
Sex and Birth Case Date Age Weight Procedure Survival Remarks -(Hours) and Type
4:417 1 1:
1 21.11.38 M. 61b. 7oz. Ligature of cardia and 7 days Silk ligature slowly cut 72 III(B) gastrostomy through and re-established . the fistula 2 16.10.41 M. Prem. 41b. 5oz. Transpleural (R). 17 hours Pneumonia 84 III(B) Anastomosis 3 31.5.42 F. Prem. 51b. 8oz. Transpleural (R). Fistula Died on Massive collapse of both 148 III(B) ligated_ and divided, table lungs tube tied into lower segment 4 2.11.43 F. Prem. 41b. 3oz. Transpleural (R). 5} days Leakage of anastomosis. 72 III(B) Anastomosis Case reported (O’REILLY, l N.. FRANKLIN. R. H.. and DALEY, M. D.. 1944) 5 6.11.45 F. Prem. Transpleural (R). 43 hours _ Pneumonia III(,a) Tube tied into each segment ' 6 13.1.46 F. | 51b. 8oz. Transpleural (R). 52 hours Pneumonia 28 III(B) Fistula ligated and | divided. Gastrostomy 7 21.2.46 F. 51b. 6oz. Extrapleural approach 27 hours Pulmonary collapse I 120 III(n) attempted. Pleura tore badly._ Anastomosis with difficulty 8 i27.l0.46 F. 71b. 2oz. Transpleural (R). 25 hours Consolidation both lungs. I 72 II No fistula. Lower scg- Patent ductus arteriosus. ment ended 1-5 cm. No gastric gas bubble was above diaphragm. seen at X-ray—this should I Gastrostomy | have led to the correct diagnosis of type 9 10.1.47 F. 71b. 7oz. Extrapleural (R). Alive and Gastrostomy carried out 72 HI(B) Anastomosis well 6 days after anastomosis. Gastrostomy tube re. moved after 12 days. Infant now takes food normally and has made I good progress. (Previously re orted, FRANKLIN, R. .. 1947) 10 24.4.47 F. 61b. 7oz. Extrapleural (R). Alive and Gastrostomy _was not 48 III(a) Anastomosis well necessary in this case. The
infant made a smooth H recovery and has since progressed well. (Previously ilwegizggted. FRANKLIN, R. H..
Diagnosis
Cyanosis associated with excess of mucus in the nasopharynx may be noted at birth in many normal infants. Improvement in these occurs after aspiration, but the child suffering from atresia has recurrent attacks of cyanosis which are usually severe enough to excite notice, but which are often attributed to other causes, such as tentorial tears and atelectasis. When feeds are started all the symptoms are accentuated, the child is often avid for its feed and sucks strongly, only to be overwhelmed by an attack of spluttering and cyanosis, accompanied by the complete regurgitation of the feed. Aspiration of the nasopharynx effects an immediate improvement, but the symptoms recur as soon as feeding is attempted again.
These symptoms are so striking and alarming that they seldom escape notice, and it cannot be too strongly emphasised that such a train of symptoms usually indicate oesophageal atresia. Midwives and others who have the care of infants in the first hours of life, should be taught that atresia is the commonest cause of persistent choking and cyanosis in the newborn child.
Once the suspicion of atresia has been raised, all mouth feeding is stopped and the nasopharynx is aspirated at frequent intervals.
To confirm the diagnosis, a well-lubricated rubber catheter is passed through the mouth and down the oesophagus. Its arrest 10-12 cm. from the anterior alveolar margin is practically diagnostic of atresia.
Final confirmation of the diagnosis is radiological, but the practice of giving a Barium swallow is to be condemned. The emulsion is almost certain to spill over into the lungs and the child’s slender chance of survival is still further reduced. The best method to adopt is as follows :—
The infant is screened and a careful assessment is made of the condition of the lungs; the stomach and intestines are then examined for the presence of air. If air is present in the stomach and intestines below an (esophageal atresia it is proof that a fistula exists between the lower segment and trachea. The converse is usually, but not invariably, true.
A catheter is now passed into the upper segment and l to 2 cc. of lipiodol is gently introduced under direct observation against the screen.
The appearance of the blind segment is characteristic, and as soon as it has been observed and the rare presence of a fistula in the upper segment excluded, the lipiodol is withdrawn (Figs. 3, 4 and 5). Bronchoscopic examination has been used to inspect the fistula and so confirm the diagnosis (Pilcher). Apart from the passage of a catheter into the blind sac and frequent aspiration, the important features in the management of the diagnostic stage are negative rather than positive. The chief safety factors are the avoidance of any further feeding and of unskilled attempts at X-ray diagnosis.
Management after the Diagnosis has been Confirmed
The complete diagnosis not only confirms the presence of atresia, but in many cases discloses the precise nature of the deformity. It must be emphasised once more that 80 per cent. of the cases fall into the characteristic group of (esophageal atresia with fistula between trachea and lower oesophageal segment.
The preparation of the patient for operation requires the full collaboration of an expert paediatrician, as well as the whole-time services of an intelligent and conscientious nurse. In fact, without these two essentials before and after operation, any surgical intervention is almost certain to fail.
The three essentials in the pre-operative period are : to keep the blind sac empty by aspiration, to improve the state of the lungs by changing the child’s position frequently and systematically, and to administer the
X-ray showing large air bubble in Blind upper segment filled with iodised
stomach and blind upper esophageal oil. Care has been taken not to allow segment filled with iodised oil. any to spill over into the larynx.
Fig. 5 An earlier case in which the importance of great care in X-ray diagnosis was not fully appreciated and the iodised oil has spilled over into the lungs. Although the oesophagus was restored and is seen to be functioning, the_pulrnonary condition contributed to the unsuccessful result in this case.
requisite fluid parenterally. The fluid requirement is difficult to assess, and giving too much is probably more dangerous than giving too little.
The operation
The child is secured in a prone position over a rubber hot-water bottle, half-filled with warm water. A small pad is placed under the right shoulder
‘and the head is turned to the right. Local anaesthesia (1 per cent. Procain)
is used for the skin incision and the anaesthetist concentrates on keeping the upper oesophageal segment empty and administering oxygen unde pressure from time to time. T
The incision is curved (Fig. 6), starting 1 cm. lateral to the spine, over the second rib, passing downwards parallel to the spine over the third and fourth ribs and then outwards crossing the fifth rib obliquely and ending over the sixth rib. Part of the fifth rib is resected subperiosteally, extreme care being necessary to avoid opening the pleura. The correct extrapleural plane having been found, the incision is deepened through the chest wall with division of the fourth, third and second ribs and their intercostal bundles. The pleura is carefully displaced until the vena azygos arch is seen. This usually marks the lower end of the upper blind segment and it is divided between ligatures with great care.
Scar after mediastinal incision. Fig. 6
The lower oesophageal segment emerges from the posterior surface of the trachea or from the bifurcation itself. Gentle movement of the catheter in the upper segment helps in identification. The fistula is ligatured close to the trachea and divided, with conservation of as much as possible of the lower segment, and traction sutures are introduced into each segment to avoid handling them unnecessarily.
Anastomosis is undertaken if it seems feasible without undue tension, and it is performed with the use of fine silk and small, curved, eyeless round-bodied needles. Various methods of anastomosis have been described, but none of them is easy. The structures are delicate and readily damaged, and there is a great tendency for the stitches to cut out. A catheter introduced into the (esophagus from the mouth during the later stages is of great help. On completion of the anastomosis the area is well dusted with penicillin powder, the wound is closed around a small rubber drain, and the oesophageal tube is removed.
If anastomosis has proved impossible, Humphreys has advised that the first stage of a multiple-stage operation be carried out. A finger is passed along the back of the trachea into the base of the neck near the suprasternal notch. An incision is made between the right sternomastoid and the trachea, and through this the upper segment is drawn to establish a cervical oesophagostomy. If a fistula is present it is ligated and divided at this first stage, but failure to effect an anastomosis may be due to the absence of a fistula ; the blind ends of the oesophagus being further apart when atresia is uncomplicated (Type II) than when a tracheo-oesophageal fistula is present as well (Type III(B)).
After-care
The child is nursed in an oxygen tent and the same care is taken to aspirate the nasopharynx as before operation. A small blood transfusion (100 cc.) may be given, followed by an intravenous drip of N/5 glucose saline. The fluid and salt balance must be controlled with great care and is best entrusted to a skilled paediatrician.
Immediately after the operation, feeds of penicillin solution (10,000 units) hourly are started by mouth. The mediastinal drainage tube is removed on the third or fourth day and the patency of the oesophagus is tested radiographically with iodised oil; if the reconstructed oesophagus conducts the oil without leakage, feeds of expressed breast milk are begun.
Gastrostomy is performed only if the swallow of iodised oil demonstrates a mediastinal leak; even if it is shown to be necessary by this criterion, its performance is best deferred until the seventh or eighth day after oesophageal repair.
Results in Other Centres Ha1'ght’.<' results to 1946 :—
45 consecutive patients.
42 had associated tracheo-oesophageal fistula ; one additional patient had a tracheo-oesophageal fistula without (esophageal atresia.
36 patients were explored.
26 patients were submitted to intrathoracic restoration of oesophagus.
9 patients survived operation from 6 months to 4% years.
Only one patient in this series had an additional anomaly which was incompatible with life.
Ladd’s results to 1944 :—
34 patients explored. 28 patients submitted to a staged operation ; nine living. 6 patients treated by primary anastomosis ; two living. Ladd’s first success was a staged operation in November, 1939; an antethoracic (Esophagus was constructed and the child was reported alive at the age of 4;} years.
Conclusions
This paper is presented in the hope that midwives and paediatricians will regard all newborn infants who sufl"er from attacks of cyanosis and choking, together with the regurgitation of feeds, to be subjects of atresia of the oesophagus until the oesophagus can be shown, by the clinical and radiological methods described, to be normal.
If this attitude is inculcated and lethal attempts at feeding are stopped until the condition of the oesophagus has been determined by the simple passage of a catheter, we shall have more frequent opportunities of treating these little patients before aspiration pneumonia has jeopardised their chances of recovery.
The radiologist can contribute to the success of the operation by refraining from any form of examination which risks filling the lungs with opaque medium and the surgeon can prepare himself for a difficult operative procedure by a study of the varied pathology of (Esophageal atresia and of the methods which have proved successful in its treatment.
REFERENCES
VOGT, E. C. (1929) Amer. J. Roentg. 22, 463.
HAIGHT, C. (1944) Trans. Amer. Surg. Ass. 62, 623.
———:(1944) Ann. Surg. 120, 623.
HAIGHT, C. and TowNsLEY, H. A. (1943) Surg. Gynec. Obstet. 76, 672.
HOLT, F. J., HAIGHT, C. and HODGES, F. J. (1946) Radiology 47, 457.
GIBSON, T. (1697) The Anatomy of humane bodies epitomized, 5th Ed. London, p. 239. MACKENZIE, M. (1884) Diseases of the throat and nose.
KEITH, A. (1910) Brit. Med. J. 1, 301.
RICHTER, H. M. (1913) Surg. Gynec. Obstet. 17, 397.
PLASS, E. D. (1919) Johns Hopkins Hosp. Report, 18, 258.
GUTHRIE, K. J. (1945) J. Path. and Bact. 57, 367.
BRENNEMAN, J. (1918) Amer. J. Dis. Child. 16, 143.
LANMAN, T. H. (1940) Arch. Surg. 41, 1060.
LEVEN, N. L. (1939) J. Thoracic Surg. 9, 213.
——:(1941) Ibid. 10, 648.
GAGE, M. and OCHSNER, A. (1936) Ann. Surg. 103, 725.
GAMBLE, H. A. (1938) Ann. Surg. 107, 701.
LADD, W. E. (1944) New Eng. J. Med. 230, 625.
SINGLETON, A. C. and KNIGHT, M. D. (1944) Ann. Surg. 119, 556.
TURNER, G. Gray (1946) Injuries and diseases of the avsophagus. London, Cassell.
Carroll & Co.
O’REILLY, N., FRANKLIN, R. H. and DALEY, M. D. (1944) Arch. Dis. Child. 19, 131. FRANKLIN, R. H. (1947) Lancet 2, 243.
HUMPHREYS, G. H. (1944) Surgery 15, 801.
Cite this page: Hill, M.A. (2024, April 26) Embryology Paper - Congenital atresia of the oesophagus. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Paper_-_Congenital_atresia_of_the_oesophagus
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G