File:ZikaUSA2016graph.jpg
Original file (820 × 531 pixels, file size: 65 KB, MIME type: image/jpeg)
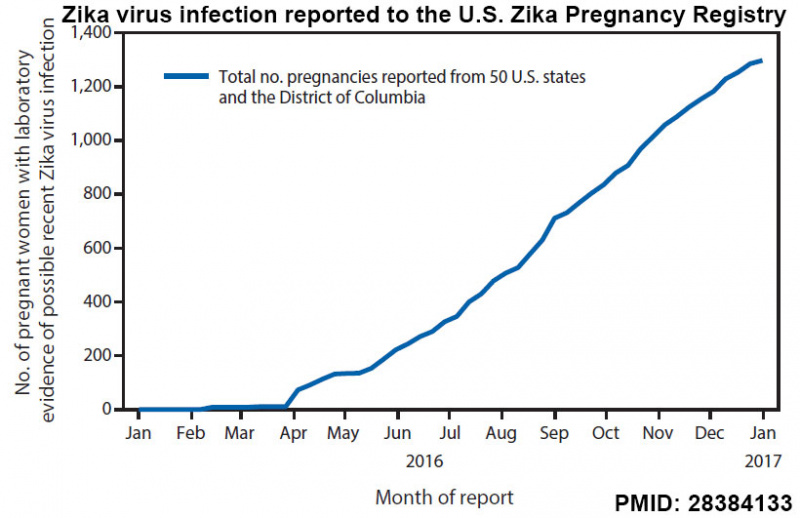
Zika virus infection reported to the U.S. Zika Pregnancy Registry
In collaboration with state, tribal, local, and territorial health departments, CDC established the U.S. Zika Pregnancy Registry (USZPR) in early 2016 to monitor pregnant women with laboratory evidence of possible recent Zika virus infection and their infants.
This report includes an analysis of completed pregnancies (which include live births and pregnancy losses, regardless of gestational age) in the 50 U.S. states and the District of Columbia (DC) with laboratory evidence of possible recent Zika virus infection reported to the USZPR from January 15 to December 27, 2016. Birth defects potentially associated with Zika virus infection during pregnancy include brain abnormalities and/or microcephaly, eye abnormalities, other consequences of central nervous system dysfunction, and neural tube defects and other early brain malformations.
During the analysis period, 1,297 pregnant women in 44 states were reported to the USZPR. Zika virus-associated birth defects were reported for 51 (5%) of the 972 fetuses/infants from completed pregnancies with laboratory evidence of possible recent Zika virus infection (95% confidence interval [CI] = 4%-7%); the proportion was higher when restricted to pregnancies with laboratory-confirmed Zika virus infection (24/250 completed pregnancies [10%, 95% CI = 7%-14%]). Birth defects were reported in 15% (95% CI = 8%-26%) of fetuses/infants of completed pregnancies with confirmed Zika virus infection in the first trimester. Among 895 liveborn infants from pregnancies with possible recent Zika virus infection, postnatal neuroimaging was reported for 221 (25%), and Zika virus testing of at least one infant specimen was reported for 585 (65%).
These findings highlight why pregnant women should avoid Zika virus exposure. Because the full clinical spectrum of congenital Zika virus infection is not yet known, all infants born to women with laboratory evidence of possible recent Zika virus infection during pregnancy should receive postnatal neuroimaging and Zika virus testing in addition to a comprehensive newborn physical exam and hearing screen. Identification and follow-up care of infants born to women with laboratory evidence of possible recent Zika virus infection during pregnancy and infants with possible congenital Zika virus infection can ensure that appropriate clinical services are available.
- Links: Zika Virus | USA Statistics
Reference
<pubmed>28384133</pubmed>
Copyright
U.S. Department of Health & Human Services https://www.hhs.gov/open
Cite this page: Hill, M.A. (2024, April 27) Embryology ZikaUSA2016graph.jpg. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/File:ZikaUSA2016graph.jpg
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G
File history
Click on a date/time to view the file as it appeared at that time.
| Date/Time | Thumbnail | Dimensions | User | Comment | |
|---|---|---|---|---|---|
| current | 11:34, 15 May 2017 |  | 820 × 531 (65 KB) | Z8600021 (talk | contribs) | ==Zika virus infection reported to the U.S. Zika Pregnancy Registry== ===Reference=== <pubmed>28384133</pubmed> Category:Abnormal Development Category:Environmental Abnormalities Category:Virus |
You cannot overwrite this file.
File usage
The following 2 pages use this file: