Assisted Reproductive Technology: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 209: | Line 209: | ||
* ART children estimated as 3.3% and 2.0% of all children currently born in Australia and New Zealand respectively. | * ART children estimated as 3.3% and 2.0% of all children currently born in Australia and New Zealand respectively. | ||
<gallery> | 2015 ART Report<ref>Macaldowie A, Lee E & Chambers GM 2015. Assisted reproductive technology in Australia and New Zealand 2013. Sydney: National Perinatal Epidemiology and Statistics Unit, the University of New South Wales. [https://npesu.unsw.edu.au/surveillance/assisted-reproductive-technology-australia-new-zealand-2013 NPESU]</ref> cover image. | ||
* 71,516 ART treatment cycles reported from Australian and New Zealand clinics in 2013 (66,143 and 5,373 respectively). | |||
** 1.9% increase in Australia and 3.8% increase in New Zealand on 2012. | |||
* 13.7 cycles per 1,000 women of reproductive age (15–44 years) in Australia | |||
** compared with 5.9 cycles per 1,000 women of reproductive age in New Zealand. | |||
* 95.1% autologous cycles (womens own oocytes or embryos) | |||
** 36.6% autologous cycles embryos frozen and thawed. | |||
** 37,192 women who undertook 67,980 autologous fresh and/or thaw cycles in Australia and New Zealand | |||
* 1.8 average fresh and/or thaw cycles per woman were undertaken | |||
** more cycles per woman in Australia (1.9 cycles per woman) than in New Zealand (1.5 cycles per woman). | |||
* Preimplantation Genetic Diagnosis (PGD) was performed in 2,740 cycles (19.4% increase), 4.4% of cycles in which embryos were created or thawed. | |||
<gallery caption="Assisted Reproductive Technology in Australia and New Zealand"> | |||
File:Assisted reproductive technology in Australia and New Zealand 2013.jpg|2013 | File:Assisted reproductive technology in Australia and New Zealand 2013.jpg|2013 | ||
File:Assisted reproductive technology in Australia and New Zealand 2012.jpg|2012 | File:Assisted reproductive technology in Australia and New Zealand 2012.jpg|2012 | ||
| Line 217: | Line 230: | ||
</gallery> | </gallery> | ||
= | {| class="wikitable mw-collapsible mw-collapsed" | ||
! Australia Birthweight Data 2002-2010 | |||
|- | |||
| | |||
'''Birthweight percentiles by gestational age for births following assisted reproductive technology in Australia and New Zealand, 2002-2010'''<ref name=PMID24908671><pubmed>24908671</pubmed></ref> | '''Birthweight percentiles by gestational age for births following assisted reproductive technology in Australia and New Zealand, 2002-2010'''<ref name=PMID24908671><pubmed>24908671</pubmed></ref> | ||
| Line 224: | Line 240: | ||
:'''Links:''' [[Australian Statistics]] | [[Birth Weight]] | :'''Links:''' [[Australian Statistics]] | [[Birth Weight]] | ||
= | {| class="wikitable mw-collapsible mw-collapsed" | ||
! Australia 2010 Data | |||
|- | |||
| width=300px|[[File:Assisted_reproductive_technology_in_Australia_and_New_Zealand_2010.jpg|150px|Assisted reproductive technology in Australia and New Zealand 2010.]] | | width=300px|[[File:Assisted_reproductive_technology_in_Australia_and_New_Zealand_2010.jpg|150px|Assisted reproductive technology in Australia and New Zealand 2010.]] | ||
| width=300px|[[File:Assisted reproductive technology in Australia and New Zealand 2009.jpg|150px|Assisted reproductive technology in Australia and New Zealand 2009.]] | | width=300px|[[File:Assisted reproductive technology in Australia and New Zealand 2009.jpg|150px|Assisted reproductive technology in Australia and New Zealand 2009.]] | ||
| Line 286: | Line 302: | ||
===2012=== | ===2012=== | ||
[[File:USA-ART-2012-cover.jpg|thumb|USA ART Report 2012 cover]] | {| class="wikitable mw-collapsible mw-collapsed" | ||
! ART USA 2012 Data | |||
|- | |||
| [[File:USA-ART-2012-cover.jpg|thumb|USA ART Report 2012 cover]] | |||
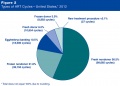
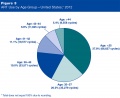
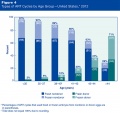
2012 Assisted Reproductive Technology National Summary Report<ref name=USA-ART2012>Centers for Disease Control and Prevention, American Society for Reproductive Medicine, Society for Assisted Reproductive Technology. '''2012 Assisted Reproductive Technology National Summary Report.''' Atlanta (GA): US Dept of Health and Human Services; 2014. http://www.cdc.gov/art/ART2012</ref> | 2012 Assisted Reproductive Technology National Summary Report<ref name=USA-ART2012>Centers for Disease Control and Prevention, American Society for Reproductive Medicine, Society for Assisted Reproductive Technology. '''2012 Assisted Reproductive Technology National Summary Report.''' Atlanta (GA): US Dept of Health and Human Services; 2014. http://www.cdc.gov/art/ART2012</ref> | ||
* ART procedures reported with the intention to transfer at least one embryo (157,662 cycles of the 176,247 total ART cycles performed in 2012). | * ART procedures reported with the intention to transfer at least one embryo (157,662 cycles of the 176,247 total ART cycles performed in 2012). | ||
| Line 304: | Line 322: | ||
</gallery> | </gallery> | ||
:'''Links:''' [http://www.cdc.gov/art/reports/2012/national-summary.html 2012 Assisted Reproductive Technology National Summary Report] | :'''Links:''' [http://www.cdc.gov/art/reports/2012/national-summary.html 2012 Assisted Reproductive Technology National Summary Report] | ||
=== | |} | ||
===ART USA Archive=== | |||
{| class="wikitable mw-collapsible mw-collapsed" | |||
! ART USA 2011 - 2009Data | |||
|- | |||
| '''ART 20011''' | |||
Births Resulting From Assisted Reproductive Technology: Comparing Birth Certificate and National ART Surveillance System Data, 2011<ref name="PMID25493705"><pubmed>25493705</pubmed></ref> | Births Resulting From Assisted Reproductive Technology: Comparing Birth Certificate and National ART Surveillance System Data, 2011<ref name="PMID25493705"><pubmed>25493705</pubmed></ref> | ||
* This report compares data on births resulting from assisted reproductive technology (ART) procedures from 2011 birth certificates with data from the 2011 National ART Surveillance System (NASS) | * This report compares data on births resulting from assisted reproductive technology (ART) procedures from 2011 birth certificates with data from the 2011 National ART Surveillance System (NASS) | ||
| Line 312: | Line 335: | ||
:'''Links:''' [http://www.cdc.gov/nchs/data/nvsr/nvsr63/nvsr63_08.pdf CDC - National ART Surveillance System Data 2011 Report] | :'''Links:''' [http://www.cdc.gov/nchs/data/nvsr/nvsr63/nvsr63_08.pdf CDC - National ART Surveillance System Data 2011 Report] | ||
|- | |||
! ART USA 2010 Data | |||
[http://www.cdc.gov/art/ART2010/NationalSummary_index.htm 2010 Assisted Reproductive Technology National Summary Report] | [http://www.cdc.gov/art/ART2010/index.htm 2010 Assisted Reproductive Technology Report] | |- | ||
| [http://www.cdc.gov/art/ART2010/NationalSummary_index.htm 2010 Assisted Reproductive Technology National Summary Report] | [http://www.cdc.gov/art/ART2010/index.htm 2010 Assisted Reproductive Technology Report] | |||
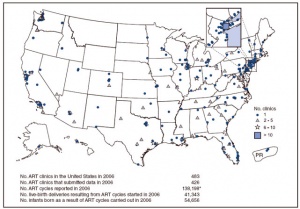
* Number of ART clinics in the United States - 474 | * Number of ART clinics in the United States - 474 | ||
| Line 321: | Line 345: | ||
* Number of live-birth deliveries resulting from ART cycles started - 47,090 | * Number of live-birth deliveries resulting from ART cycles started - 47,090 | ||
* Number of infants born as a result of ART cycles performed - 61,564 | * Number of infants born as a result of ART cycles performed - 61,564 | ||
|- | |||
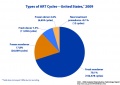
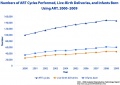
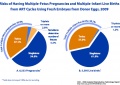
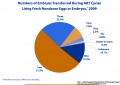
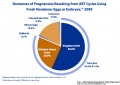
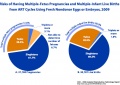
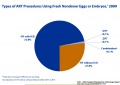
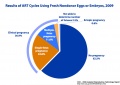
! ART USA 2009 Data | |||
|- | |||
[[File:USA-ART-2009-cover.jpg|thumb|USA ART Report 2009 cover]] | [[File:USA-ART-2009-cover.jpg|thumb|USA ART Report 2009 cover]] | ||
| Line 349: | Line 374: | ||
{{USA ART Report 2009 links}} | {{USA ART Report 2009 links}} | ||
|- | |||
! ART USA 2006 Data | |||
[[File:USA-_ART_clinics_2006.jpg|thumb|USA- ART clinics (2006)]] | |- | ||
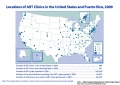
| [[File:USA-_ART_clinics_2006.jpg|thumb|USA- ART clinics (2006)]] | |||
* [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5805a1.htm Assisted Reproductive Technology Surveillance - United States, 2006] | * [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5805a1.htm Assisted Reproductive Technology Surveillance - United States, 2006] | ||
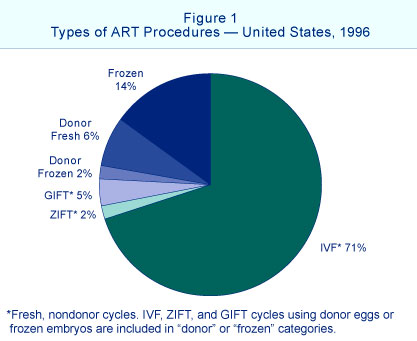
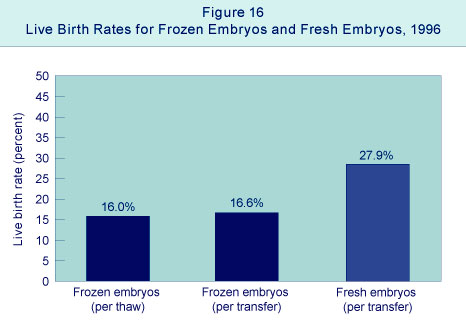
[[File:USA_assisted_reproductive_technology_1996.jpg|right]] | [[File:USA_assisted_reproductive_technology_1996.jpg|right]] | ||
| Line 365: | Line 391: | ||
:'''Report Links:''' [[USA Statistics]] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss6107a1.htm?s_cid=ss6107a1_e 2009] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5805a1.htm?s_cid=ss5805a1_e 2006] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5705a1.htm?s_cid=ss5705a1_e 2005] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5606a1.htm?s_cid=ss5606a1_e 2004] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5504a1.htm 2003] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5402a1.htm 2002] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5301a1.htm 2001] | [ http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5209a1.htm 2000] | :'''Report Links:''' [[USA Statistics]] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss6107a1.htm?s_cid=ss6107a1_e 2009] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5805a1.htm?s_cid=ss5805a1_e 2006] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5705a1.htm?s_cid=ss5705a1_e 2005] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5606a1.htm?s_cid=ss5606a1_e 2004] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5504a1.htm 2003] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5402a1.htm 2002] | [http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5301a1.htm 2001] | [ http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5209a1.htm 2000] | ||
|} | |||
== European Society of Human Reproduction and Embryology == | == European Society of Human Reproduction and Embryology == | ||
Revision as of 14:01, 9 October 2015
| Embryology - 5 Jun 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
| Educational Use Only - Embryology is an educational resource for learning concepts in embryological development, no clinical information is provided and content should not be used for any other purpose. |
Introduction
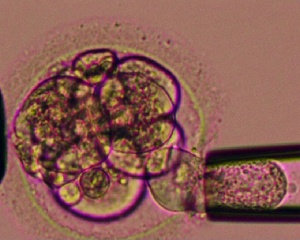
In vitro fertilization is one of now many different reproductive options know collectively as Assisted Reproductive Technologies (ART). These techniques continue to grow worldwide with development of new medical technologies. In vitro fertilization covers the aided fertilization process, in contrast with in vivo fertilization which is the normal uterine occuring fertilization process.
The earliest experiments 1945-48, involved fertilising oocytes that had been collected from women with spermatozoa in a petri dish.[2][3] The first successful IVF was carried out in the UK in 1978 by Edwards RG, et al.[4], receiver of the 2010 Nobel Prize in Medicine.
The Latin, In vitro = "in glass" meaning in essence a test tube as apposed to in vivo (in life or a living body), fertilisation (Aus spelling) and fertilisation (US spelling). Even in vivo fertilization can also now be considered "assisted" through some fertility drug treatments. Both processes have the same biological outcome, fusion of male and female gametes to form a diploid zygote.
In Australia, the first successful IVF occurred in 1980.[5] and during 2005 1,596 IVF babies were born. In the same year in Australia and New Zealand 51,017 treatment cycles were reported, an increase of 13.7% of ART treatment cycles from 2004. In all countries using Assisted Reproductive Technologies (ART), pregnancy rates vary for the different methods of treatment and also between individual IVF or GIFT units. In Australia best clinical pregnancy rate (per 100 oocyte retrieval cycles) by most successful 25% of all clinics increased from 24.9% (1998) to 34.4% (2001) (NPSU data - ART 2002 report)
The Nobel Prize in Physiology or Medicine 2010 - Awarded to Robert G. Edwards "for the development of in vitro fertilization" who battled societal and establishment resistance to his development of the in vitro fertilization procedure, which has so far led to the birth of around 4 million people. (More? Assisted Reproductive Technology | Nobel Prize 2010)
10 April 2013 - Sir Robert Edwards has died aged 87. BBC News
Some Recent Findings
|
| Some older articles |
|---|
* Retransplantation of cryopreserved ovarian tissue: the first live birth in Germany[10] "Cryopreserved ovarian tissue can be retransplanted to restore fertility after radiation or chemotherapy. To date, 15 live births after retransplantation have been reported worldwide. We report the first pregnancy and the first live birth after retransplantation in Germany. This was the first live birth after retransplantation of cryopreserved ovarian tissue in Germany and also the first case with histological confirmation that the oocyte from which the patient conceived could only have come from the retransplanted tissue."
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Assisted Reproductive Technology <pubmed limit=5>Assisted Reproductive Technology</pubmed> |
Trends in ART procedures
- In the last 5 years there has been a shift from day 2-3 embryo (cleavage stage) transfers to day 5-6 embryo (blastocyst) transfers.
- The proportion of blastocyst transfers has increased from 27.1% in 2006 to 52.1% in 2010.
- Increase in the transfer of vitrified (ultra-rapid frozen) embryos. Compared with 2009, the proportion has more than doubled from 18.3% to 38.2%.
- reduction in the rate of multiple birth deliveries, with a decrease from 12% in 2006 to 7.9% in 2010.
- shifting to single embryo transfer, the proportion of which increased from 56.9% in 2006 to almost 70% in 2009 and 2010.
- decrease in the multiple delivery rate was achieved while clinical pregnancy rates remained stable at about 23% per cycle.
Data: Assisted reproductive technology in Australia and New Zealand 2010[13]
18 Ways to Make a Baby
- Natural sex
- Artificial insemination - of mother with father's sperm
- Artificial insemination - of mother with donor sperm
- Artificial insemination - with egg and sperm donors, using surrogate mother
- In vitro fertilization (IVF) - using egg and sperm of parents
- IVF - with Intra-Cytoplasmic Sperm Injection (ICSI)
- IVF - with frozen embryos
- IVF - with Preimplantation Genetic Diagnosis (PGD)
- IVF - with egg donor
- IVF - with sperm donor
- IVF - with egg and sperm donor
- IVF - with surrogate using parents' egg and sperm
- IVF - with surrogate and egg donor
- IVF - with surrogate and sperm donor
- IVF - with surrogate using her egg, sperm from baby's father
- IVF - with surrogate using egg and sperm donors*
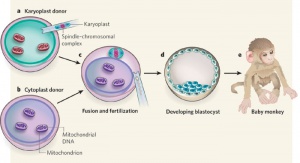
- Cytoplasmic transfer**
- Nuclear transfer and cloning
In Vitro Fertilization
First IVF Baby
Louise Brown was born at 1147 BST on 25 July, 1978, in Oldham, United Kingdom.
- Links: BBC Profile Louise Brown
Blastocyst Formation (in vitro)
The table below shows human blastocyst in vitro changes during week 1 development.[14]
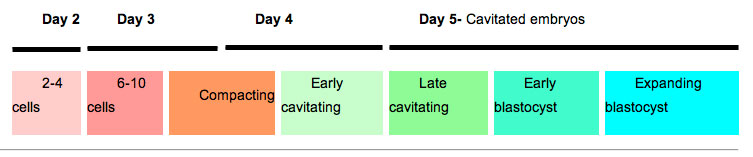
|
|
|
- Links: Week 1 | Blastocyst
Embryo Culture Milestones
- 1944-48 human oocytes fertilised by spermatozoa in vitro[2][3]
- 1949 8 cell mouse embryo -> blastocyst (in saline and egg yolk)
- 1956 8 cell mouse embryo -> blastocyst (first embryo culture medium)
- 1957 2 cell mouse embryo -> blastocyst
- 1958 8 cell mouse embryo -> blastocyst, then transferred to pregnant recipient
- 1960's development of culture requirements for mouse mebryos
- 1965 2 cell mouse embryo -> blastocyst, then transferred into pseudopregnant recipient
- 1968 zygotes from mouse -> blastocysts
- 1968,70 2 & 4 cell rabbit embryos -> blastocyst in serum supplemented medium
- 1970,71 1 & 2 cell rabbit embryos -> blastocyst in defined medium
- 1970,81 Culture of in vitro fertilized human embryo -> 16 cells -> blastula
- 1998 Cloning of adult sheep "dolly"
- 2004 Cloning of human blastocysts
Data modified from[15]
Oldest IVF Mother
There is still risk, ethical and genetic debate about very old women becoming pregnant by IVF.
- 2003 India - A 65-year old Indian woman was the oldest in the world to give birth by IVF.
- 2006 United Kingdom - A 62-year old woman has become the UK's oldest woman to give birth to a child.
- 2008 Australia - A 54-year old woman was Australia's oldest woman pregnant by IVF (most Australian IVF clinics do not treat women over 50)
- 2010 Australia - A 57-year old woman is now the oldest mother to give birth in Australia, has delivered IVF twins in Western Australia.
IVF Sex Ratios
A recent paper looked at Australian assisted reproductive technology (ART) data (2002-2006) studied the effect on human sex ratio at birth by different procedures. PMID:20875033
- "More males were born following in vitro fertilisation single embryo transfer (IVF SET) (53.0%) than intracytoplasmic sperm insemination (ICSI) SET (50.0%), and following blastocyst SET (54.1%) than cleavage-stage SET (49.9%). For a specific ART regimen, IVF blastocyst SET produced more males (56.1%) and ICSI cleavage-stage SET produced fewer males (48.7%). The change in the sex ratio at birth of SET babies is associated with the ART regimen. The mechanism of these effects remains unclear. Fertility clinics and patients should be aware of the bias in the sex ratio at birth when using ART procedures."
Oocyte and Embryo Quality
There have been many attempts to establish morphological, biochemical or molecular markers of oocyte quality with variable results by different groups. Recently studies have also looked at the molecular quality of cumulus and granulosa cells.[16] Earlier studies of this support cell population have looked at markers of mitosis and apoptosis, with positive and negative correlation respectively. Following removal of these support cells, oocyte features such as; nuclear maturation status, meiotic spindle presence, cytoplasm morphology, zona pellucida structure, and polar body presence and structure have all been investigated.[17]
Several different microscopic techniques have also been used to visually analyse oocyte appearance:
- normal light microscopy
- phase contrast microscopy
- differential interference microscopy
- polarized light microscopy - A study has used polarization microscope to identify the spindle in rescue ICSI of unfertilized oocytes appears to result in better normal fertilization rate and less 3PN rate compared to the control group.[18]
- confocal microscopy (not for clinical use)
A 2010 meeting of the Alpha Executive, and ESHRE Special Interest Group of Embryology, held in Istanbul, led to the "Istanbul consensus"[19] [20]established a consensus criteria and terminology for grading oocytes, zygotes and embryos that would be amenable to routine application in any IVF laboratory. The following sub-heading are brief summary points of the complete consensus.
Oocyte Scoring
Optimal oocyte morphology is that of a spherical structure enclosed by a uniform zona pellucida, with a uniform translucent cytoplasm free of inclusions and a size-appropriate polar body. Oocytes undergo both nuclear and cytoplasmic maturation, and that these processes are neither the same nor necessarily even synchronous.
- Cumulus-oocyte complex (COC) scoring - provides a tool for troubleshooting not a correlation with embryo developmental competence. This should be a binary score (0 or 1), with a ‘good' COC (score of 1) defined as having expanded cumulus and a radiating corona.
- Zona pellucida scoring- no specific benefit to measuring zona thickness, as evidence for any effect on outcome. However, it was noted that there could be patient-specific effects, and so a note should be made of exceptional observations regarding the colour or thickness of the zona pellucida.
- Perivitelline space - presence of inclusions in the perivitelline space is anomalous. However, there was insufficient evidence to support any specific prognosis associated with this observation. Therefore, the observation of inclusions should be noted, there is no requirement to count or measure them, only noted if it is exceptionally large.
- Polar body scoring - presence or absence of the first polar body should be noted in the uninseminated oocyte, where possible. Exceptionally large polar body should be noted and should not be inseminated, due to the risk of oocyte aneuploidy.
- Cytoplasm scoring - homogeneous cytoplasm is expected, and that non-homogeneous cytoplasm is of unknown biological significance.
- ‘Granularity' of the cytoplasm is ill-defined, and distinctly different from clustering of organelles.
- Organelle clustering is associated with lower implantation potential.
- smooth endoplasmic reticulum (sER) disks are associated with the risk of a serious, significantly abnormal outcome.
- Vacuolization - observation of large vacuoles in the oocyte should be noted.
- small vacuoles (5–10 µm in diameter) few small fluid filled and transparent are unlikely to be of biological consequence.
- large vacuoles (>14 µm in diameter) are associated with fertilization failure.
Zygote Scoring
Pronuclear scoring - three categories can provide additional information to the fertilization check, and that both should be performed at the same time.
- symmetrical
- non-symmetrical
- abnormal - pronuclei with no NPBs (‘ghost pronuclei’), single nucleolar precursor body (‘bulls-eye pronuclei”).
Cleavage-stage Scoring
- Assessment of cell number - 4 cells on Day 2 and 8 cells on Day 3 and related to embryo cell cleavage rates.
- more slowly than the expected rate have a reduced implantation potential
- faster than the expected rate are likely to be abnormal and have a reduced implantation potential.
- Fragmentation - an extracellular membrane-bound cytoplasmic structure that is <45 µm diameter in a Day-2 embryo and <40 µm diameter in a Day-3 embryo. Relative degrees of fragmentation were defined as:
- mild (<10%)
- moderate (10–25%)
- severe (>25%).
- Multi nucleation - the presence of more than one nucleus in a blastomere, and includes micronuclei, and is associated with a decreased implantation potential, increased level of chromosome abnormality and increased risk of spontaneous abortion.
- Cell size - embryos at the 2-, 4- and 8-cell stages, blastomeres should be even sized. For all other cell stages, one would expect a size difference in the cells, as the cleavage phase has not been completed.
Day 4 Assessment (Morula stage)
- optimal embryo at this stage (92 ± 2 h) would be compacted or compacting, and have entered into a fourth round of cleavage. T the consensus system uses three grades, the reason for a fair or poor grade should also be included.
Day 5 Assessment (Blastocyst stage)
- optimal embryo at this stage (116 ± 2 h) would be a fully expanded through to hatched blastocyst with an ICM that is prominent, easily discernible and consisting of many cells, with the cells compacted and tightly adhered together, and with a TE that comprises many cells forming a cohesive epithelium. It was agreed that while the ICM has a high prognostic value for implantation and fetal development, a functional TE is also essential. The consensus for a blastocyst scoring system was that there should be a combination of stage and score. It was agreed that ‘hatching' is defined as the obvious emergence of the TE with enclosed blastocoel through a thinning zona pellucida. It was also agreed that hatching cannot be reliably assessed in embryos with an artificially breached zona pellucida (with the exception of the breach made during ICSI). The ICM and TE should be graded relative to the Gardner A–C scale, but that a grade of 1–3 (rather than A–C) should be given—with Grade 1 equivalent to Gardner A.
Non-viable Embryo
- a non-viable embryo is an embryo in which development has been arrested for at least 24 h, or in which all the cells have degenerated or lysed.
In Vitro Maturation
In Vitro Maturation (IVM) is a term used to describe a range of techniques for developing ovarian follicles and oocytes outside of the body. These oocytes are generally retrieved from the antral follicles of either unstimulated or minimally stimulated ovaries. The technique has been suggested for polycystic ovary syndrome and other ovarian pathologies for fertility preservation. This is a relatively new approach to human fertility.
Assisted Reproductive Technology (Australia and New Zealand)
- Over 100,000 ART babies born over the last three decades in Australia and New Zealand.
- ART children estimated as 3.3% and 2.0% of all children currently born in Australia and New Zealand respectively.
2015 ART Report[21] cover image.
- 71,516 ART treatment cycles reported from Australian and New Zealand clinics in 2013 (66,143 and 5,373 respectively).
- 1.9% increase in Australia and 3.8% increase in New Zealand on 2012.
- 13.7 cycles per 1,000 women of reproductive age (15–44 years) in Australia
- compared with 5.9 cycles per 1,000 women of reproductive age in New Zealand.
- 95.1% autologous cycles (womens own oocytes or embryos)
- 36.6% autologous cycles embryos frozen and thawed.
- 37,192 women who undertook 67,980 autologous fresh and/or thaw cycles in Australia and New Zealand
- 1.8 average fresh and/or thaw cycles per woman were undertaken
- more cycles per woman in Australia (1.9 cycles per woman) than in New Zealand (1.5 cycles per woman).
- Preimplantation Genetic Diagnosis (PGD) was performed in 2,740 cycles (19.4% increase), 4.4% of cycles in which embryos were created or thawed.
- Assisted Reproductive Technology in Australia and New Zealand
| Australia Birthweight Data 2002-2010 | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Birthweight percentiles by gestational age for births following assisted reproductive technology in Australia and New Zealand, 2002-2010[22]
Average age of women was 35.5 years (35.2 years in 2002). Women aged older than 40 years has increased from 14.3% in 2002 to 15.3% in 2005. Since ANZARD was established in 2002 there has been a significant increase in the number of embryos transfer cycles where women received single-embryo transfers (SET). SET cycles accounted for 48.3% of embryos transfer cycles in 2005, compared to 28.4% in 2002. The increase of SET cycles resulted more singleton deliveries. The proportion of singleton deliveries was 85.9% in 2005, the highest proportion ever reported. Babies born to women who had a single-embryo transfer had better outcomes compared to babies born to women who had a double-embryo transfer (DET). In 2005, there were 3,681 SET babies and 5,589 DET babies. In SET babies, 96.1% were singletons, compared to 61.6% singletons in DET babies. SET babies had a lower proportion of preterm babies (11.7%), compared to 30.6% in DET babies. Similarly, 8.0% of SET liveborn babies were low birthweight, compared to 25.0% in DET liveborn babies. Perinatal mortality rate is a measure of perinatal outcomes. In 2005, for all babies born following ART treatment, the perinatal mortality rate was 14.7 deaths per 1,000 births, a 23.8% decrease from 19.3 deaths per 1,000 births in 2004. The perinatal mortality rate was the lowest among singletons born following SET (7.3 deaths per 1,000 births) in 2005.[24] 2004 - 41,904 IVF treatment cycles were started in Australia 92.6% (38,823) and New Zealand 7.4% (3,081). (More? NPSU Assisted Reproduction Technology Reports) In Vitro Fertilization - ABC News Baby born from frozen embryo "In what's thought to be a world first, a baby has been born in Melbourne using a woman's frozen egg and a donor's frozen sperm which created an embryo that was also frozen, then thawed and implanted into the mother" "JOHN MCBAIN: Oh egg freezing is very difficult. Embryo freezing itself is very well established. We would probably have about 55 per cent of all the babies born from our program, and that's about 1,400 a year, come from frozen embryos. So, that's very well established technology. But even with these embryos, only 70 per cent of the embryos survive the freezing and thawing. With eggs, it's closer to 40 to 50 per cent, and then you have to have the number which don't fertilise following that, and then you have to have those which end up being frozen, possibly not surviving the embryo freezing stage too, and that's a reason we don't promote it." Regulation of Assisted Reproductive TechnologyAssisted Reproductive Technology (ART) , including IVF (or in vitro fertilisation) is regulated in Australia through both legislative and voluntary compliance frameworks. Legislation in three states is underpinned by a national system of accreditation by the Reproductive Technology Accreditation Committee (RTAC) of the Fertility Society of Australia, which is in turn is underpinned by guidelines produced by the NHMRC. This is outlined in more detail below. Current legislation
Reproductive Technology Accreditation Committee (RTAC). RTAC, under the Fertility Society of Australia, administers a national Code of Practice and a system for the accreditation of ART clinics in Australia. Through its Code of Practice, RTAC sets professional and laboratory standards for ART clinical practice. (Information from the NHMRC)
Assisted Reproductive Technology (USA)2012
ART USA Archive
European Society of Human Reproduction and Embryology
Highlights from the 2007 Report
Highlights from the 2001 Report
Human Fertilisation and Embryology Authority UK (HFEA)The UK Human Fertilisation and Embryology Authority (HFEA) was established in August 1991 following the passing of the Human Fertilisation and Embryology Act 1990 (HFE Act). The HFEA's principal tasks are to:
HFEA also provide a downloadable patient booklet: Your Guide to Infertility and website information on Patients' Guide to Donor Insemination (DI) CanadaSociety of Obstetricians and Gynaecologists of Canada summary statements (for January 2005 to December 2012) lists 15 key statements for pregnancy outcomes after assisted human reproduction[26]
SwedenSweden had its first child born after in vitro fertilisation 20 years ago. A recent paper in BMJ looks at the change in multiple birthrates since a change in the early 1990s, to reduce the number of embryos transferred in the clinic from three to two.[27] "The rate of multiple births after in vitro fertilisation increased to a maximum of 29% in 1991 but fell to 18.5% by 2001, resulting in a 70% reduction of preterm births" Controlled Ovarian StimulationA variety of drug based techniques are used to stimulate maternal oocyte development, called controlled ovarian stimulation (COS), for any in vitro fertilization procedure. The recommended for technique will vary for some procedures and also from clinic to clinic and between countries. An example of ovarian stimulation (based on[28])
Gamete BankingBoth men and women undergoing clinical procedures of chemotherapy and/or radiotherapy (ionizing radiation) can have induced gametogenic failure. FemaleWomen undergoing clinical procedures of chemotherapy and/or radiotherapy (ionizing radiation) can have induced premature ovarian failure. Therefore a growing reproductive option has been the collecting of oocytes or ovarian tissue before commencing these procedures and storing ("banking") by cryopreservation for later use. One major issue is coordination of the two procedures, as most cancer therapies commence immediately, and most reproductive procedures require substantial preparation time. Currently the cryopreservation techniques required for ovarian tissue preservation are also improving all the time. In a number of clinics women with breast cancer and of reproductive age are being counselled about their reproductive options.[29] Chemotherapy, alkylating and alkylating-like agents attach to the guanine base of DNA, cross-linking the DNA, preventing replication and cell division. Some examples include: busulfan, carboplatin, chlorambucil, cisplatin, cyclophosphamide, dacarbazine, ifosfamide, thiotepa
MaleA recent paper[12] described the current practice of spermatozoa banking in the United Kingdom in relation to cancer patients. The UK Human Fertilization and Embryology Authority have now extended the period of storage permitted by their regulations to 55 years. They point to a lack of "national and international guidelines for the provision, organization, maintenance and management of the cryopreservation services."
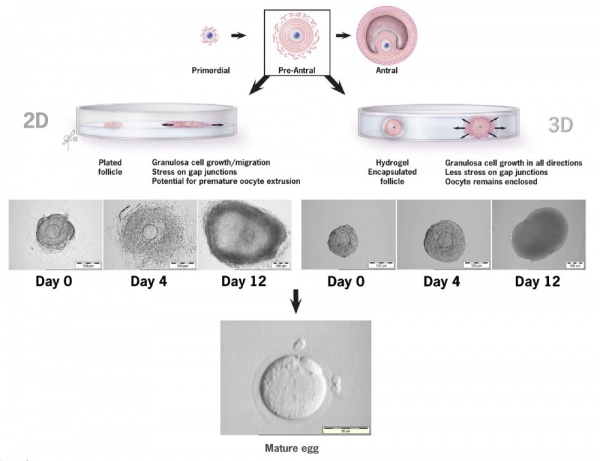
Ovarian ReserveOvarian reserve is a term referring to the evaluation of ovary oocyte (egg) number and quality. A negative finding has been described as Diminished Ovarian Reserve, or an ovarian insufficiency or premature ovarian failure and may be seen in adult childhood cancer survivors and adult patients undergoing a number of therapies. The anti-Müllerian hormone (AMH) level is currently the most sensitive marker of ovarian reserve.[31] Ovarian Follicle Growth in vitro2D and 3D methods of ovarian follicle growth in vitro.[32]
References
ReviewsArticles<pubmed>20124287</pubmed> <pubmed>19147504</pubmed> Search PubmedJuly 2010 "Assisted Reproductive Technology" All (45041) Review (5016) Free Full Text (8551) "in vitro fertilization" All (29785) Review (3172) Free Full Text (6189) Search Pubmed Now: in vitro fertilization | assisted reproduction technology
External LinksExternal Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
TermsFor a full list of terms see ART Glossary
Glossary Links
Cite this page: Hill, M.A. (2024, June 5) Embryology Assisted Reproductive Technology. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Assisted_Reproductive_Technology
|