User:Z3415141: Difference between revisions
| Line 89: | Line 89: | ||
1. Provide a brief time course and overview of embryonic development of either the human testis or ovary. (2-3 paragraphs) | 1. Provide a brief time course and overview of embryonic development of either the human testis or ovary. (2-3 paragraphs) | ||
Human Testes Embryonic Development | |||
It is towards the seventh week of development that the male gonad develops into the testis. Before this time the gonads of both sexes are identical as they are undifferentiated. It is the differentiation which is dependant upon the XY chromosomes that determines whether the gonads turn into testes or ovaries. Fertilisation determines the genetic sex and a male be complete with the XY chromosome complex<ref name="PMID24003159"><pubmed>24003159</pubmed></ref>.The Y chromosome is the key for the testes formation. It has a testis-determining effect on the medulla of the undifferentiated gonad as it contains the Y-linked gene SRY which produces the protein product Testis Determining Factor (TDF). TDF upregulates other transcription factors including SOX9. The SOX-9 is said to work with Sf1 to produce AMH in sertoli cells to inhibit female reproductive system creation<ref name="PMID9774680"><pubmed>9774680</pubmed></ref>. | '''Human Testes Embryonic Development''' | ||
It is towards the seventh week of development that the male gonad develops into the testis. Before this time the gonads of both sexes are identical as they are undifferentiated. It is the differentiation which is dependant upon the XY chromosomes that determines whether the gonads turn into testes or ovaries. Fertilisation determines the genetic sex and a male be complete with the XY chromosome complex<ref name="PMID24003159"><pubmed>24003159</pubmed></ref>.The Y chromosome is the key for the testes formation. It has a testis-determining effect on the medulla of the undifferentiated gonad as it contains the Y-linked gene SRY which produces the protein product Testis Determining Factor (TDF). TDF upregulates other transcription factors including SOX9. The SOX-9 is said to work with Sf1 to produce AMH (Anti-Müllerian hormone) in sertoli cells to inhibit female reproductive system creation<ref name="PMID9774680"><pubmed>9774680</pubmed></ref>. | |||
Ultimately the expression of the SRY protein leads to the development of primary sex cords which proliferate from the coelomic epithelium and then extend and condense into the medulla of the gonad. These cords then branch and their ends become the rete testes. The more present sex cords then become the seminiferous cords which then form the tunica albuginea after they loose their connection with the germinal epithelium. The cords then develop into the seminiferous tubules. These tubules then become separated by mesenchyme which allows the interstitial cells of leydig to arise. Because the seminefrous tubules come from a dual origin on a cellular level their walls are composed of both the supporting sertoli cells which come from the germinal epithelium and the undifferentiated male germ cell spermatagonia which come from the primordial germ cells. Further down the track of development the germinal epithelium is flattened to form the mesothelium on the surface of the testis. The rete testis become continuous with the persistent mesonephric tubules. These tubules are involved in the formation of the excretory tracts of the testis forming the efferent ductules which open into adjacent mesonephric ducts<ref name="PMID22944459"><pubmed>22944459</pubmed></ref>. | Ultimately the expression of the SRY protein leads to the development of primary sex cords which proliferate from the coelomic epithelium and then extend and condense into the medulla of the gonad. These cords then branch and their ends become the rete testes. The more present sex cords then become the seminiferous cords which then form the tunica albuginea after they loose their connection with the germinal epithelium. The cords then develop into the seminiferous tubules. These tubules then become separated by mesenchyme which allows the interstitial cells of leydig to arise. Because the seminefrous tubules come from a dual origin on a cellular level their walls are composed of both the supporting sertoli cells which come from the germinal epithelium and the undifferentiated male germ cell spermatagonia which come from the primordial germ cells. Further down the track of development the germinal epithelium is flattened to form the mesothelium on the surface of the testis. The rete testis become continuous with the persistent mesonephric tubules. These tubules are involved in the formation of the excretory tracts of the testis forming the efferent ductules which open into adjacent mesonephric ducts<ref name="PMID22944459"><pubmed>22944459</pubmed></ref>. | ||
Revision as of 18:04, 7 October 2014
Welcome to the 2014 Embryology Course!
- Links: Timetable | How to work online | One page Wiki Reference Card | Moodle
- Each week the individual assessment questions will be displayed in the practical class pages and also added here.
- Copy the assessment items to your own page and provide your answer.
- Note - Some guest assessments may require completion of a worksheet that will be handed in in class with your student name and ID.
| Individual Lab Assessment |
|---|
|
| Lab 12 - Stem Cell Presentation Assessment | More Info | |
|---|---|---|
| Group | Comment | Mark (10) |
| 1/8 |
|
7 |
| 2 |
|
7.5 |
| 3 |
|
7.5 |
| 4 |
|
8.5 |
| 5 |
|
8.5 |
| 6 |
|
8.5 |
| 7 |
|
7.5 |
Lab Attendance
Lab 1--Z3415141 (talk) 12:48, 6 August 2014 (EST)
Lab 2--Z3415141 (talk) 11:15, 13 August 2014 (EST)
Lab 3--Z3415141 (talk) 11:13, 20 August 2014 (EST)
Lab 4--Z3415141 (talk) 13:01, 27 August 2014 (EST)
Lab 5----Z3415141 (talk) 13:04, 3 September 2014 (EST)
Lab 6--Z3415141 (talk) 11:19, 10 September 2014 (EST)
Lab 7--Z3415141 (talk) 12:08, 17 September 2014 (EST)
Lab 8--Z3415141 (talk) 14:15, 24 September 2014 (EST)
Online Assessment
Online Assessment 1
<pubmed>25100106</pubmed>
Some women for personal reasons prefer to take subcutaneous progesterone for luteal phase support when undergoing in vitro fertilization (IVF) in an attempt to avoid some of the side effects of vaginal progesterone. In attempting to work out whether the luteal phase of IVF better supports the ongoing pregnancy rate with the use of either the new aqueous preparation of subcutaneous progesterone or vaginal progesterone 800 random women aged between 18-42 years undergoing IVF received an embryo transfer where 3 oocytes were randomly placed in either a preparation progesterone administered subcutaneously or vaginal progesterone. If a viable pregnancy was to occur, then progesterone treatment continued for up to 12 weeks of the gestation process.
It was found that the pregnancy rate for vaginal progesterone (44.4%) in comparison to subcutaneous progesterone (41.6%) was consistently higher. While luteal phase support has clearly shown to improve pregnancy rates in women in the past this research shows that those women whom chose to go with the subcutaneous progesterone preparations are less likely to have a successful pregnancy than those who go with the traditional vaginal progesterone in supporting the luteal phase of IVF. It is important to note though due to the relatively small sample and dosage sizes of this study and the fairly small difference between the two groups shows that more testing should be completed before the results of this study should be considered fully conclusive.
<pubmed>25105102</pubmed>
A women’s worst nightmare is the sign of vaginal bleeding symbolism what may be a miscarriage. This study examined the effects of progesterone supplementation during the luteal phase on the possibility of miscarriage and live birth rate in natural frozen-thawed embryo transfer (FTET) cycles 228 women who underwent FTET cycles over a period between 2009- 2012 were examined.
The women were split up into two groups where one would receive progesterone support during the luteal phase and another that did not receive any progesterone support during the pregnancy. Overall there were no major differences in the women’s characteristics. This included the number of oocytes received, matured and fertilised. However, miscarriage rate was significantly lower in the group that received the progesterone as well as the live birth rate in comparison to those that did not receive any progesterone. The implications of this study loom large for women undergoing FTET cycles as it shows that if the luteal phase is supported with progesterone than the probability of a women’s worst nightmare can be decreased.
Online Assessment 2
Online Assessment 3
Midgut Formation during the development of the human fetus
1. <pubmed>18606147</pubmed> 2. <pubmed>14745932</pubmed> 3. <pubmed>24414177</pubmed>
Online Assessment 4
1. Identify a paper that uses cord stem cells therapeutically and write a brief (2-3 paragraph) description of the paper's findings.
The neuroprotective mechanisms and effects of implanted cord-derived msenchymal stem cells from a human umbilical cord(hUC-MSCs) were examined in ischemic stroke. An improvement in infarct volume and neurobehavioral function in the hUC-MSCs was discoverewd.
To do so the hUC-MSCs were cultured after they were isolated from the subendothetelial/endothelial layers of the umbilical cord of a human. Twenty days after the of induction of in vitro neuronal differentiation the cultured hUC-MSCs showed morphological features similar to those neurons. However there was no detection of functional neuron type channels.
From the discovery that the morphological differences meant that the cells were now able to produce neurotrophic factors but had not become active neuronal cells it was concluded that this may be related to the neuroprotective effects of hUC-MSCs.
<pubmed>18634757</pubmed>
2. There are a number of developmental vascular "shunts" present in the embryo, that are closed postnatally. Identify these shunts and their anatomical location.
Ductus Venosus: Joins the descending aorta and left pulmonary artery.
Ductus Arteriosus: connects the pulmonary artery directly to the ascending aorta.
Foamen Ovale: An opening between the septum of the left and right atria of the heart.
Online Assessment 5
Extrahepatic Billary Atresia is categorised by destruction of the Billary tree due to an ascending inflammatory localised process. As an irreversible condition, it is a lethal abnormality and patients left untreated can yield to complications of end-stage liver disease and Billary cirrhosis.
The abnormality is not greatly understood currently. It is believed that a multiple of causes are responsible for the inflammatory condition and research has shown that females are slightly more likely than males to be affected. Parental factors, infectious triggers and genetics are currently assumed to be the cause of the condition.
<pubmed>22609296</pubmed>
Online Assessment 6
Worked on group task.
Online Assessment 7
1. <pubmed> 25238858</pubmed> This study examined the point in development in which the suprachiasmatic nucleus (SCN) first has the capacity to generate circadian oscillations. Using mice to track the circadian clock protein, PER2. The hypothalamic explants expressed consistent oscillations firstly when isolated between 15 and 16 days postfertilisation. Explants from any other brain area were shown to not express any oscillations. It was concluded that within a day of genesis around the same age of the first trimester in humans, the autonomously develops mechanisms sufficient to couple and synchronise its cells and also the SCN gains the ability to express circadian oscillations.
Online Assessment 8
1. Provide a brief time course and overview of embryonic development of either the human testis or ovary. (2-3 paragraphs)
Human Testes Embryonic Development It is towards the seventh week of development that the male gonad develops into the testis. Before this time the gonads of both sexes are identical as they are undifferentiated. It is the differentiation which is dependant upon the XY chromosomes that determines whether the gonads turn into testes or ovaries. Fertilisation determines the genetic sex and a male be complete with the XY chromosome complex[1].The Y chromosome is the key for the testes formation. It has a testis-determining effect on the medulla of the undifferentiated gonad as it contains the Y-linked gene SRY which produces the protein product Testis Determining Factor (TDF). TDF upregulates other transcription factors including SOX9. The SOX-9 is said to work with Sf1 to produce AMH (Anti-Müllerian hormone) in sertoli cells to inhibit female reproductive system creation[2].
Ultimately the expression of the SRY protein leads to the development of primary sex cords which proliferate from the coelomic epithelium and then extend and condense into the medulla of the gonad. These cords then branch and their ends become the rete testes. The more present sex cords then become the seminiferous cords which then form the tunica albuginea after they loose their connection with the germinal epithelium. The cords then develop into the seminiferous tubules. These tubules then become separated by mesenchyme which allows the interstitial cells of leydig to arise. Because the seminefrous tubules come from a dual origin on a cellular level their walls are composed of both the supporting sertoli cells which come from the germinal epithelium and the undifferentiated male germ cell spermatagonia which come from the primordial germ cells. Further down the track of development the germinal epithelium is flattened to form the mesothelium on the surface of the testis. The rete testis become continuous with the persistent mesonephric tubules. These tubules are involved in the formation of the excretory tracts of the testis forming the efferent ductules which open into adjacent mesonephric ducts[3].
References
2. Include an image from the historic genital embryology section of the online notes in your description.
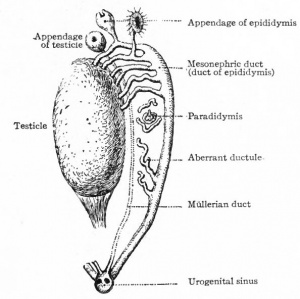
Persistent portions of the mesonephros in the male
Diagram persistent portions of the mesonephros