Testis Development: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 285: | Line 285: | ||
:'''Links:''' [http://www.ncbi.nlm.nih.gov/omim/603693 OMIM - Fog2] | :'''Links:''' [http://www.ncbi.nlm.nih.gov/omim/603693 OMIM - Fog2] | ||
=== | ===Gadd45g=== | ||
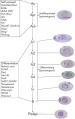
[[File:Gadd45g and sex determination model.jpg|thumb|Gadd45g and Sex Determination Model<ref name=PMID23516551><pubmed>23516551</pubmed></ref>]] | |||
Growth Arrest- And Dna Damage-Inducible Gene (GADD45, GAMMA; GADD45G) | Growth Arrest- And Dna Damage-Inducible Gene (GADD45, GAMMA; GADD45G) | ||
| Line 299: | Line 294: | ||
:'''Links:''' [http://omim.org/entry/604949 OMIM - Gadd45g]] | :'''Links:''' [http://omim.org/entry/604949 OMIM - Gadd45g]] | ||
===Gata4=== | |||
* transcription factor | |||
* dosage critical for fetal testis development in mice<ref name=PMID17848526 /> | |||
===Eif2s3y=== | |||
==References== | ==References== | ||
Revision as of 22:58, 3 December 2013
| Embryology - 26 Apr 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
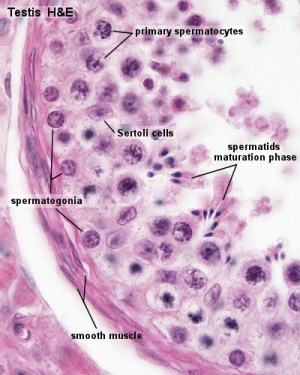
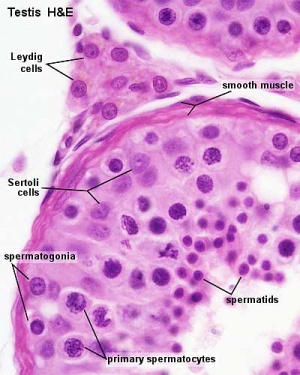
The male gonad is the testis. The initial difference in male and female gonad development are dependent on testis-determining factor (TDF) the protein product of the Y chromosome SRY gene. Recent studies have indicated that additional factors may also be required for full differentiation. The seminiferous tubules are considered the parenchyma of the testis. Within the developing testis the three main differentiating cell types are: gamete forming cells (spermatogonia), support cells (Sertoli cells) and hormone secreting cells (Leydig or interstitial cells).
In humans postnatally, at approximately 2 months of age, primordial germ cells (gonocytes) are replaced by adult dark (Ad) and pale (Ap) spermatogonia that make up the spermatogonial stem cell (SSC) population that at puberty will commence differentiation into spermatozoa.
| Y Chromosome | Puberty | Endocrine - Gonad
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Testis Embryology <pubmed limit=5>Testis Embryology</pubmed> |
Movies
|
|
|
|
- Links: Movies
Development Overview
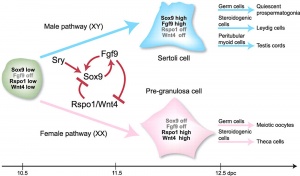
Sex Determination
- Humans (week 5-6)
- Germ cells migrate into gonadal ridge
- Gonads (male/female) identical at this stage, Indifferent
Gonad Development
- dependent on sex chromosome
- Y testes
- No Y ovary
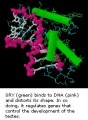
SRY
SRY protein (Testes determining factor, TDF) binds DNA Transcription factor, Bends DNA 70-80 degrees
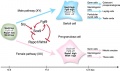
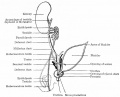
Internal Genital Organs
- All embryos form paired
- Mesonephric duct, see kidney development
- Paramesonephric duct, Humans 7th week Invagination of coelomic epithelium Cord grows and terminates on urogenital sinus
- Male Gonad (testes) secretes Mullerian duct inhibitory factor (MDIF) which causes regression of paramesonephric duct
- Male Gonad (testes) secretes Testosterone which retains mesonephric duct
External Genital Organs
- All embryos initially same (indifferent)
- Testosterone differentiates male
Week 8
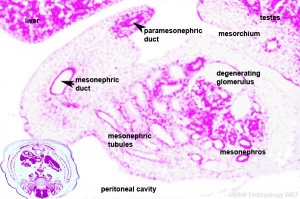
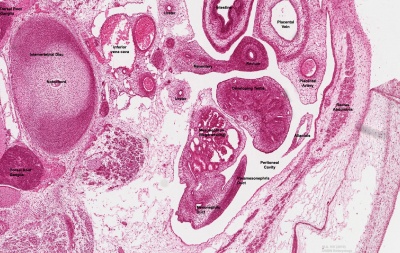
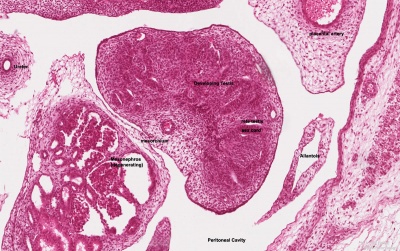
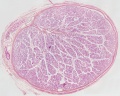
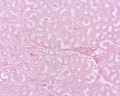
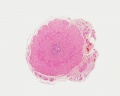
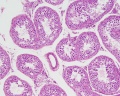
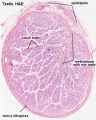
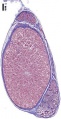
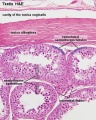
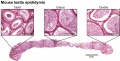
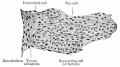
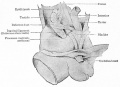
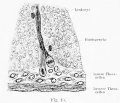
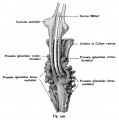
Developing testis is shown to the centre right. These images show the position, size and histological development of the testis in week 8 of human development (Carnegie stage 22, last embryonic week).
- Human Stage 22: Testis - labeled overview | Testis - unlabeled overview | Testis - unlabeled detail | Testis - labeled detail | testis | Carnegie stage 22 | Movie - Urogenital stage 22
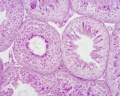
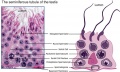
Sertoli Cells
These are the support cells located within the seminiferous tubule. Their differentiation is regulated by the presence of a Y chromosome and in turn regulates Leydig cell differentiation. Sertoli cells direct testis morphogenesis, organizing testis cord formation, establishing testis vasculature and inducing differentiation of peritubular myoid cells and fetal Leydig cells. At puberty the immature Sertoli cells cease to proliferate and differentiate.
Sertoli cell functions include:
- regulation of spermatogenesis through endocrine FSH and testosterone
- regulation of the intratubular and intercellular environment adluminal to the tight junctional complexes
- meiotic and post-meiotic germ cells are sequestered by Sertoli-Sertoli junctional complexes
- generate adluminal compartment isolated from both serum and lymph
- attachment of germ cells through unique intermediate filament (desmosome-like junctions) and microfilament (actin- ectoplasmic specializations, ESs) junctions[7]
- to prevent premature sloughing of immature germ cells from the seminiferous epithelium
- desmosome-like junctions are initially present (up to step 8 spermatids)
- ectoplasmic specializations then replace this junction (in step 8 spermatids)
(see also review[8])
Ultrastructural description of human Sertoli cells[9]
- 7 weeks - first morphologically recognised in testicular cords, organised as primordial germ cells surrounded by pre-Sertoli cells.
- 7 to 8 weeks - basal lamina of the cords becomes distinguishable, pre-Sertoli cells the rough endoplasmic reticulum develops.
- 14 to 20 weeks - pre-Sertoli cells maintain their general morphology whereas the most significant change is the maximum development of Leydig cells.
Molecular factors:
- Follicle Stimulating Hormone (FSH) -> Krüppel-like factor 4 (KLF4)
- Krüppel-like factor 4 (KLF4) - zinc finger transcription factor, terminal differentiation of epithelial cells.
- Epidermal Growth Factor (EGF)
- Transforming Growth Factor-beta (TGFbeta)
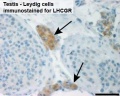
Leydig Cells
Interstitial or Leydig cells, named after german zoologist Franz von Leydig (1821 - 1908).
These cells produce the male testicular androgens and have a role during life prenatally (fetal) and postnatally during puberty onward.
Fetal Leydig Cells
Have a hormonal role in male genitalia differentiation and are lost postnatally. These cells arise approximately at 6 weeks (human) and 12.5 dpc (mouse) and there appears to be differences in hormonal sensitivity between the species. Their initial differentiation requires both luteinizing hormone (LH) and adrenocorticotrophic hormone (ACTH) and therefore normal pituitary development.
Activin A - acts upon Sertoli cells to promote their embryonic proliferation[10]
(More? Endocrine - Pituitary Development)
Adult Leydig Cells
Have a hormonal role in puberty, secondary sex characteristics and sexual maturation. Their initial differentiation from peritubular mesenchymal cells does not require gonadotropin, but development and function are dependent upon luteinizing hormone (LH).
The cells differentiate with three discrete stages (newly formed, immature, mature) leading to a decrease in proliferation and increasing testosterone biosynthetic capacity. Insulin-like growth factor I (IGF-I) stimulates proliferation of immature cells and promotes their maturation. Testosterone and estrogen inhibit the process of precursor cell differentiation and may be responsible for the cessation of proliferation in the adult Leydig cells.
Peritubular Myoid Cells
These cells surround the seminiferous tubules and express androgen receptors from fetal life through to adulthood.
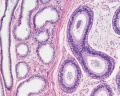
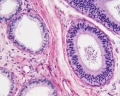
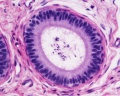
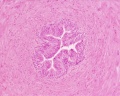
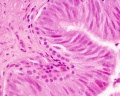
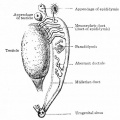
Epididymis
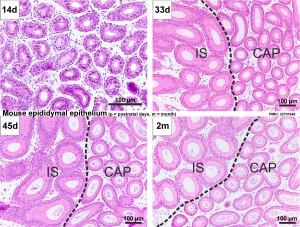
Both the ductus epididymis and ductus deferens differentiate from the mesonephric duct (Wollfian duct) elongation (cell proliferation). In the case of the epididymis, elongation also is associated with extensive coiling, the adult human epididymis about 6 metres in length (mouse 1m, rat 3m). Embryonic growth is regulated by androgens, members of the PCP pathway, and inhibin beta A. While postnatally androgens and other growth factors may have roles in final maturation. (see review[12]) The ductus epididymis is lined by a very tall pseudostratified columnar epithelium, consisting of principal cells with long stereo cilia.
Following puberty, the epididymis is involved in maturation of the spermatozoa released from the seminiferous tubules and their storage.
- middle segment - site of final functional maturation of the spermatozoa.
- terminal segment - site of storage of the mature spermatozoa.
Anatomically the adult epididymis consists of 3 regions:
- body or central portion.
- head (globus major) upper enlarged extremity.
- tail (globus minor) lower pointed extremity, continuous with the ductus deferens (vas deferens).
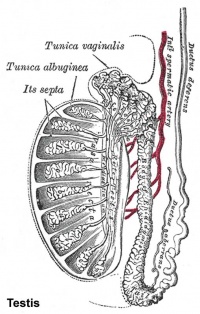
The head is intimately connected with the upper end of the testis by means of the efferent ductules of the gland; the tail is connected with the lower end by cellular tissue, and a reflection of the tunica vaginalis (tunica vaginalis propria testis) the serous covering of the testis.
The lateral surface, head and tail of the epididymis are free and covered by the serous membrane; the body is also completely invested by it, excepting along its posterior border; while between the body and the testis is a pouch, named the sinus of the epididymis (digital fossa). The epididymis is connected to the back of the testis by a fold of the serous membrane.
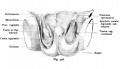
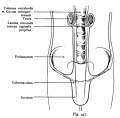
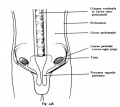
Testis Descent
Testis descent is thought to have 2 phases:
- transabdominal descent - dependent on insulin-like hormone 3 (INSL3).
- inguinoscrotal descent - dependent on androgens.
The regulation of testis descent is still being investigated and several different factors have been identified that may have roles in descent. The first stage of testicular descent occurs 10–15 weeks of gestation with the testes moving to the inguinal region.
The gubernaculum (gubernaculum Hunteri) is the caudal inguinoscrotal ligament that connects the testis to the lower abdomen. The cranial suspensory ligament (mesonephric ligament) is the cranial ligament that connects the tesitis to the posterior abdominal wall.
- Insulin-like factor 3 (INSL3, relaxin-like factor) from fetal leydig cells acting through its receptor (Rxfp2) and BMP and WNT signaling pathways to promote testis descent.
- Calcitonin gene-related peptide (CGRP) from genitofemoral nerve suggested to mediate the inguinoscrotal testicular descent.
- Epidermal growth factor (EGF) may promote by activating the androgen responsive systems.
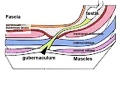
|
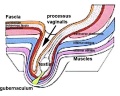
|
| |||
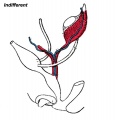
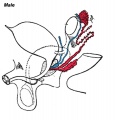
| Before Descent | End of Descent | Testis Descent Movie |
- Links: OMIM - INSL3
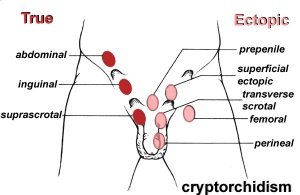
Cryptorchidism
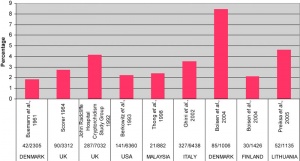
- abnormality of either unilateral or bilateral testicular descent, occurring in up to 30% premature and 3-4% term males.
- Descent may complete postnatally in the first year, failure to descend can result in sterility.
Testis descent is thought to have 2 phases:
- transabdominal descent - dependent on insulin-like hormone 3 (INSL3).
- inguinoscrotal descent - dependent on androgens.
Management of cryptorchidism in children: guidelines.[14] "Cryptorchidism is best diagnosed clinically, and treated by surgical orchiopexy at age 6-12 months, without a routine biopsy. If no testis is palpable, or if other signs of hypovirilisation such as hypospadias are present, the chromosomal sex and hormonal status must be assessed. Laparoscopy is the best way of diagnosing and managing intra-abdominal testes."
Anorchia
Clinical term for (embryonic testicular regression, vanishing testis syndrome) the absence of testes in a 46,XY individual with a male phenotype. Rare abnormality with an incidence of about 1 in 20,000 male births, and occurs more frequently with cryptorchidism (1 in 177 cases).
A recent study has identified undetectable plasma concentrations of anti-Müllerian hormone (AMH) and inhibin B and an elevated plasma FSH, together with 46,XY complement are sufficient for diagnosis of anorchia. Genetic analysis showed that NR5A1 and other genes (INSL3, SRY, LGR8 , MAMLD1) implicated in gonadal development and testicle descent were also not mutated.[15]
Puberty
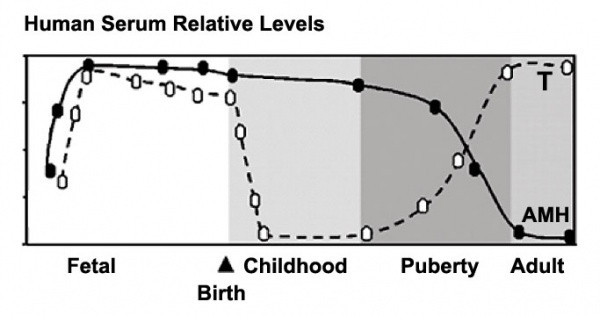
Human Male Testosterone and Anti-Müllerian Hormone (AMH) relative levels[16]
- AMH production by Sertoli cells .
- Testosterone production by Leydig cells.
In humans at puberty, hormonal and morphological changes occur within the gonad and other systems (secondary sex characteristics). Within the testis the immature Sertoli cells cease to proliferate and differentiate. Spermatogonium proliferate and spermatogenesis begins, and it takes about 70 days for cells to mature from the diploid spermatogonium to a primary spermatocyte. This maturation occurs in waves along the seminiferous tubules.
Links: Puberty Development
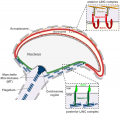
Blood-Testis Barrier
Within the testis seminiferous tubules the Sertoli cells located near the basement membrane act as an initial cellular barrier with many functions, but often described as forming a "blood-testis barrier". (see review[17]
Functions:
- prevent substances reaching the developing spermatozoa (through drug transporters)
- establish a basal and adluminal (apical) compartment (specialized microenvironment)
- provide an immunological privilege status of the testis (anti-sperm antibodies are not developed)
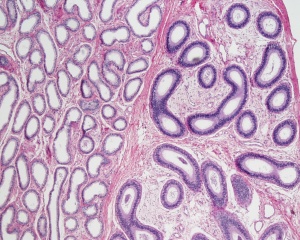
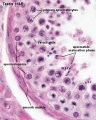
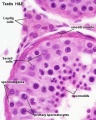
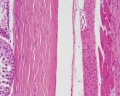
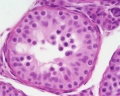
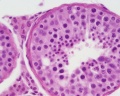
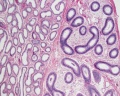
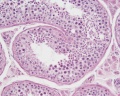
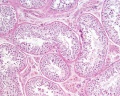
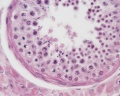
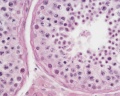
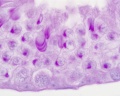
Histology
Testis Histology Links: Testis Development | Spermatozoa Development | Histology
- Human (young): overview labeled | overview unlabeled | convoluted seminiferous tubules x10 | x40 | x40 | tunica albuginea x20
- Human (adult): overview x2 | convoluted seminiferous tubules labeled | x10 | x20 | x40 | x40 | epididymis ductulus efferens | ductus epididymidis | epithelium | overview x4 | x10 | x20 | x40 | ductus deferens labeled overview | epithelium | overview x2 | x10 | x40
- Human Stage 22: Testis - labeled overview | Testis - unlabeled overview | Testis - unlabeled detail | Testis - labeled detail | testis | Carnegie stage 22 | Movie - Urogenital stage 22
- Mouse: postnatal epididymis | 14 days postnatal | 33 days postnatal | 45 days postnatal | 2 months postnatal
| Spermatozoa Development (expand to see terms) | ||
|---|---|---|
|
Note there are additional glossaries associated with genital, spermatozoa, oocyte and renal.
See also: Spermatozoa Terms collapse table
|
Genital Links: genital | Lecture - Medicine | Lecture - Science | Lecture Movie | Medicine - Practical | primordial germ cell | meiosis | endocrine gonad | Genital Movies | genital abnormalities | Assisted Reproductive Technology | puberty | Category:Genital
| ||||
|
Molecular
Sry
- Y chromosome gene for a transcription factor
- member of the high mobility group (HMG)-box family of DNA binding proteins
- human - 204 amino acid protein [18]
- Links: OMIM - Sry
Sox9
- autosomal transcription factor
- Development of XY females - presence of only a single functional copy of the transcription factor encoding genes SOX9, SF1, or WT1 (Note- not all XY humans are sex-reversed if only a single copy of a normal SF1 or WT1 allele is present)
- A nuclear export signal within the high mobility group domain regulates the nucleocytoplasmic translocation of SOX9 during sexual determination[19]
Other roles
- Cartilage - essential for chondrocyte differentiation
- Hearing - otic placode formation, maintenance of progenitors in the otic epithelium
- Links: Sox9 | Cartilage Development | Inner Ear Development
Fog2
- transcription factor, named Friend of Gata2
- human - (8q23) 1,151 amino acid nuclear protein that contains 8 zinc finger motifs[20]
- dosage critical for fetal testis development in mice[21]
- Links: OMIM - Fog2
Gadd45g
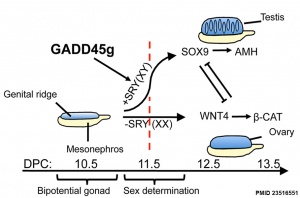
Growth Arrest- And Dna Damage-Inducible Gene (GADD45, GAMMA; GADD45G)
A Recent mouse study[1] has shown that Gadd45g protein has a role in primary sex differentiation. Knockout mice (Gadd45g(-/-) XY gonads) resulted in a a sex reversal.
- Links: OMIM - Gadd45g]
Gata4
- transcription factor
- dosage critical for fetal testis development in mice[21]
Eif2s3y
References
- ↑ 1.0 1.1 1.2 <pubmed>23516551</pubmed>
- ↑ <pubmed>21493716</pubmed>
- ↑ <pubmed>20807406</pubmed>| PMC2940779 | BMC Biol.
- ↑ <pubmed>20413907</pubmed>| PDF
- ↑ <pubmed>20040496</pubmed>
- ↑ <pubmed>21674038</pubmed>
- ↑ <pubmed>20403872</pubmed>
- ↑ <pubmed>7711190</pubmed>| Biol Reprod.
- ↑ <pubmed>11732573</pubmed>
- ↑ <pubmed>20498064</pubmed>|http://www.pnas.org/content/107/23/10526.long PNAS]
- ↑ <pubmed>22701646</pubmed>| PLoS One.
- ↑ <pubmed>21441421</pubmed>| J. Androl.
- ↑ <pubmed>18032558</pubmed>| Hum Reprod Update.
- ↑ <pubmed>18726735</pubmed>
- ↑ Brauner R, Neve M, Allali S, Trivin C, Lottmann H, Bashamboo A, McElreavey K. Clinical, biological and genetic analysis of anorchia in 26 boys. PLoS One. 2011;6(8):e23292. Epub 2011 Aug 10. PMID 21853106 PLoS One.
- ↑ <pubmed>16544032</pubmed>| Arq Bras Endocrinol Metabol.
- ↑ <pubmed>21134990</pubmed>| J Endocrinol.
- ↑ <pubmed>8434602</pubmed>
- ↑ <pubmed>12169669</pubmed>| PMC123233 | PNAS
- ↑ <pubmed>10438528</pubmed>
- ↑ 21.0 21.1 <pubmed>17848526</pubmed>PMC1986601 | PNAS
Reviews
<pubmed></pubmed> <pubmed></pubmed> <pubmed>24240231</pubmed> <pubmed>21441421</pubmed>| J. Androl.
Articles
<pubmed></pubmed> <pubmed></pubmed> <pubmed>21147849</pubmed> <pubmed>20664245</pubmed> <pubmed>20610195</pubmed> <pubmed>15379965</pubmed>
Search PubMed
Search Pubmed: Testis Development | Epididymis Development | Sry | Sox9 |
Additional Images
Historic Images
| Historic Disclaimer - information about historic embryology pages |
|---|
| Pages where the terms "Historic" (textbooks, papers, people, recommendations) appear on this site, and sections within pages where this disclaimer appears, indicate that the content and scientific understanding are specific to the time of publication. This means that while some scientific descriptions are still accurate, the terminology and interpretation of the developmental mechanisms reflect the understanding at the time of original publication and those of the preceding periods, these terms, interpretations and recommendations may not reflect our current scientific understanding. (More? Embryology History | Historic Embryology Papers) |
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- Blue Histology - Male Reproductive System
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Genital Links: genital | Lecture - Medicine | Lecture - Science | Lecture Movie | Medicine - Practical | primordial germ cell | meiosis | endocrine gonad | Genital Movies | genital abnormalities | Assisted Reproductive Technology | puberty | Category:Genital
| ||||
|
| Y Chromosome | Week 1 - Spermatogenesis | Ovary | Puberty | original page
Cite this page: Hill, M.A. (2024, April 26) Embryology Testis Development. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Testis_Development
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G