Birth - Preterm
| Embryology - 27 Apr 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
| Educational Use Only - Embryology is an educational resource for learning concepts in embryological development, no clinical information is provided and content should not be used for any other purpose. |
Introduction

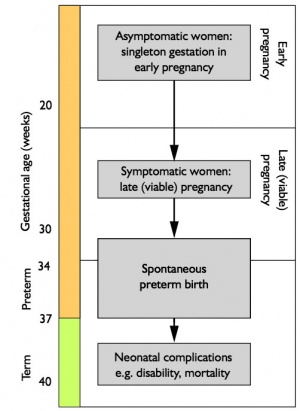
Preterm delivery (PTD) or preterm birth is defined as birth before 37 completed weeks of gestation (GA). In the USA the preterm birth rate declined in 2008 to 12.3 percent, from 12.8 percent in 2006. The preterm birth rates also declined from 2006 to 2008 for mothers of all age groups under age 40.[3] Very premature infants have associated clinical problems that may include: neonatal respiratory distress syndrome, bronchopulmonary dysplasia, cerebroventricular haemorrhage and a range of brain pathologies. Risk factors for mothers include a prior history of preterm birth, underweight, obesity, diabetes, high blood pressure, smoking, infection, age (either under 17 or over 40), genetics, multiple pregnancy (twins, triplets, and more) and pregnancies spaced too closely together. Human viability (50% chance of survival) is currently about GA 23 to 24 weeks in developed countries and is better in female than male infants.
- In the United States, more than 30,000 babies per year are born before the 28th week of pregnancy.
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Preterm Birth |
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
|
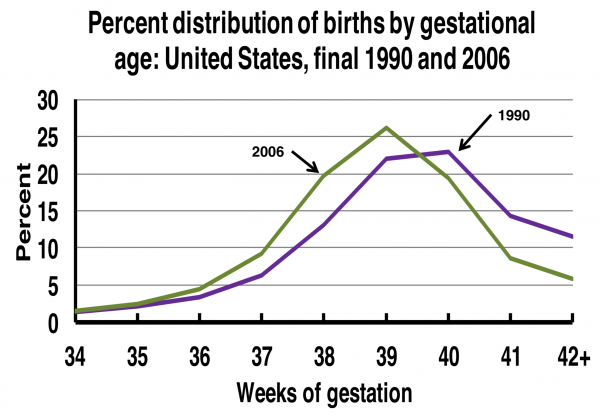
Premature Birth
| Year | < 34 weeks % | 34-36 weeks % | total preterm % |
|---|---|---|---|
| 1990 | 3.3 | 7.3 | 10.6 |
| 1995 | 3.3 | 7.7 | 11 |
| 2000 | 3.4 | 8.2 | 11.6 |
| 2005 | 3.6 | 9.1 | 12.7 |
| Data from Prevention of preterm birth: a renewed national priority[20] | |||
Improving Outcomes
Recent landmarks in improving extremely premature infant outcomes[21]
- 1970s to early 1990s - continuous positive airway pressure, mechanical ventilation, and exogenous surfactant.
- late 1990s - antenatal steroids during premature labor.
- early 2000s - avoiding chronic postnatal administration of steroids to infants.
Growth Chart for Preterm Babies
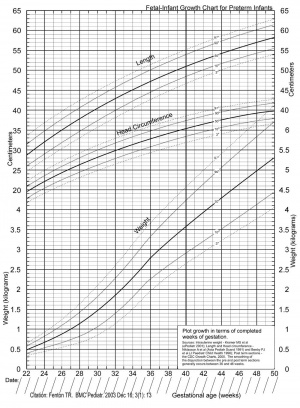
- 1976 - the Babson and Benda "fetal-infant growth graph" for preterm infants was commonly used in neonatal intensive care.[23]
- 1996 - the Beeby graph based upon New South Wales Midwives Data Collection (MDC) from 1990 to 1994 inclusive (n = 422139).[24]
- 1999 - the National Institute of Child Health and Human Development Neonatal Research Network (NICHD) USA graph.[25]
- 2003 - improved version of the Babson and Benda graph based upon literature review and intrauterine data.[22]
Statistics
Australia
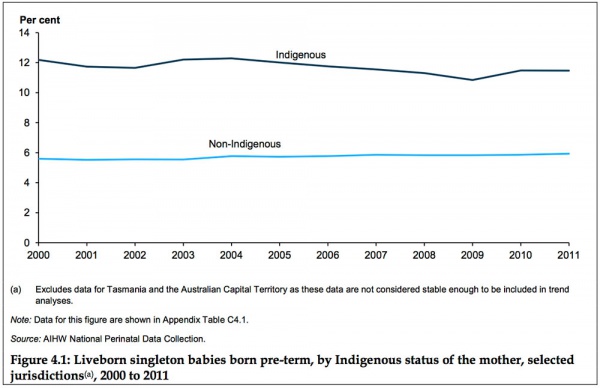
Data in this graph from AIHW 2014 Report, Birthweight of babies born to Indigenous mothers.[26]
Patterns and outcomes of preterm hospital admissions during pregnancy in NSW, 2001-2008[27]
NSW is the largest by population of all Australian states (7,238,819 or 32.4% 2010 estimate). The following information is from the abstract of the above paper published in March 2012.
- Women who were admitted to hospital in weeks 20-36 of pregnancy (preterm) and gave birth to a liveborn singleton infant in New South Wales during 2001-2008. Numbers of preterm admissions of pregnant women who were discharged without giving birth, were transferred to higher care, or who gave birth.
- 110 439 pregnancies (16.0%) involved at least one preterm admission. After their initial preterm admission:
- 71.9% of women were discharged.
- 6.3% were transferred.
- 21.8% gave birth.
- Median gestational age at admission was 33 weeks and median time to discharge, transfer or giving birth was 1 day.
- Of the women who were admitted or were transferred with suspected preterm labour, only 29% and 38%, respectively, gave birth.
- As gestational age increased, the proportion of women transferred decreased and the proportion giving birth increased.
- Links: Australian Statistics
USA
Late preterm birth[28] "The American College of Obstetricians and Gynecologists suggests that preterm birth rates have also increased because of a dramatic rise in late preterm births, defined as births between 34 weeks and 36-6/7 weeks of gestation. Late preterm newborns are the fastest growing subset of neonates, accounting for approximately 74% of all preterm births and about 8% of total births."
| Class | Age | Rate (per 100 births) |
|---|---|---|
| Total preterm | less than gestation age GA 37 weeks | 12.7 |
| Extremely preterm | less than gestation age GA 28 weeks | 0.8 |
| Early preterm | less than gestation age GA 34 weeks | 3.6 |
| Late preterm | gestation age GA 34–36 weeks | 9.0 |
| Data: USA Preterm birth rates national Vital Statistics System, United States, 2007. Links: preterm birth | USA Statistics | ||
See also Preterm Birth: Causes, Consequences, and Prevention (2007).[29]
- Links: USA Statistics
Singapore
A Comparison of the Short-term Morbidity and Mortality Between Late Preterm and Term Newborns[30]
- Late preterm babies are defined as those born between 34 to 36 completed weeks. There has been a recent increased awareness that this group of babies has a higher incidence of morbidity as compared to term babies. The aim of this study was to evaluate the short-term morbidities occurring in this group of babies managed in the neonatal unit at Singapore General Hospital (SGH). January 2005 to December 2008 a total of 6826 babies were admitted.
- Ten percent (681 out of 6826) of babies were late preterm babies, making up 63% (681 out of 1081) of all preterm babies.
- Late preterm babies had significantly greater need for resuscitation at birth.
- increased risks of developing hyaline membrane disease (2.5% vs 0.1%)
- transient tachypnoea of the newborn (TTN) (8.1% vs 1.7%)
- pneumonia (7.0% vs 2.8%)
- patent ductus arteriosus (PDA) (4.3% vs 1.1%)
- hypotension (0.7% vs 0%)
- apnoea (3.7% vs 0%)
- gastrointestinal (GI) bleeding (1.5% vs 0.3%)
- polycythaemia (2.2% vs 1.0%)
- anaemia (3.4% vs 1.2%)
- thrombocytopenia (3.2% vs 0.6%)
- hypoglycaemia (6.6% vs 1.7%)
- neonatal jaundice requiring phototherapy (41.1% vs 12.2%)
- sepsis (1.7% vs 0.6%).
Ultrasound Short Cervix
Evaluation of the cervical morphology and biometry with transvaginal ultrasonography at 16-24 weeks of gestation is a useful tool to predict the risk of preterm birth in low- and high-risk singleton pregnancies. The following points are from a recent review on transvaginal sonography for both the prediction and management of spontaneous preterm labour.[31]
Cervical Length (CV)
- > 30 mm - present cervical gland area have a 96-97% negative predictive value for preterm delivery at <37 weeks.
- ≤25 mm - irrespective of other risk factors, use of progesterone.
- ≤ 25 mm - asymptomatic cervical shortening with prior spontaneous preterm delivery, prophylactic cerclage procedure should be performed.
Fetal Fibronectin
A recent study has identified fetal fibronectin (fFN) levels as an indicator for spontaneous preterm birth in symptomatic women.[32] The sample is collected from the maternal vagina and test machines/kits that can measure this level.
- Links: OMIM 135600
Dexamethosone
When given to mothers in preterm labour, dexamethosone, a steroid used to treat asthma, helps speed up the development of the baby’s lungs. At a cost of about US$1, two shots can stop premature babies from going into respiratory distress when they are born. This can prevent 400,000 deaths annually.
Kangaroo Mother Care
A neonatal care technique involving holding the infant skin-to-skin on the mother's chest, keeping the baby warm and facilitates breastfeeding.
Keeping preterm babies warm is especially important because their tiny bodies lose heat rapidly, making them highly vulnerable to illness, infection and death. This could prevent 450 000 deaths annually.[1]
Magnesium Sulfate
Epsom Salt (magnesium sulfate, magnesium sulphate) is an inorganic salt originally used to inhibit labor (labor-inhibiting), slowing or halting uterine contractions (tocolytic agent). Inhibitory mechanism not clear, but thought to; compete with calcium at the level of plasma membrane voltage-gated channels, hyperpolarize the plasma membrane, inhibit myosin light-chain kinase activity by competing with intracellular calcium.
While described as not effective for inhibiting labor, it has more recently been recommended for neuroprotection in very preterm birth.[33] (magnesium sulphate)
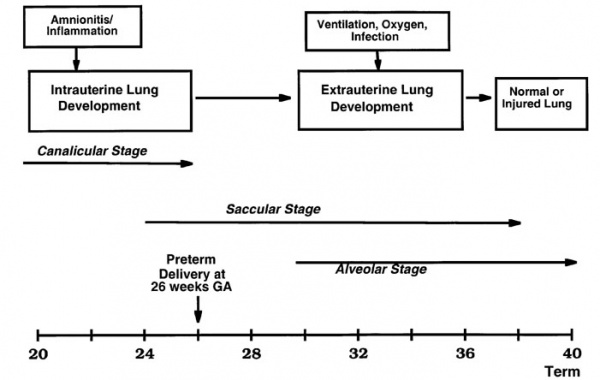
Respiratory Development
Preterm delivery and overview of related potential fetal and neonatal effects on lung development.[34]
- Links: respiratory abnormalities
Neural Development
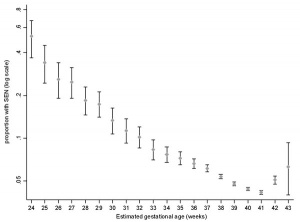
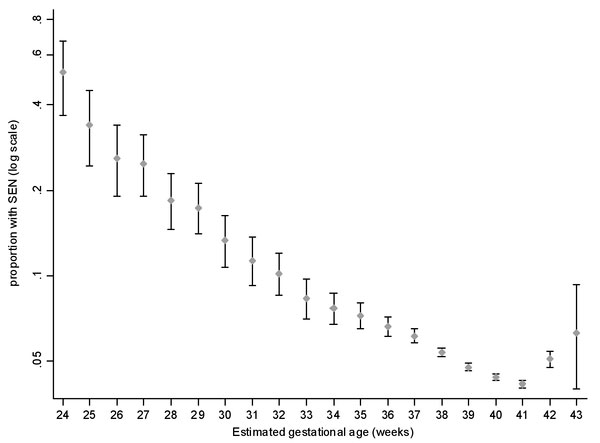
A recent UK population-based study[35] "These findings show that gestational age at delivery strongly affects a child's subsequent risk of having an special educational need (SEN) in a dose-dependent manner across the whole range of gestational age. Furthermore, because early term delivery is much more common than preterm delivery, these findings show that early term delivery is responsible for more cases of SEN than preterm delivery."
Cortical structural abnormalities in very preterm children at 7years of age[36] "Comparison of 24 children born very preterm (VPT) to 24 healthy term-born children revealed reductions in total cortical gray matter volume, white matter volume, cortical surface area and gyrification index. Regional cortical shape abnormalities in VPT children included the following: shallower anterior superior temporal sulci, smaller relative surface area in the inferior sensori-motor cortex and posterior superior temporal cortex, larger relative surface area and a cingulate sulcus that was shorter or more interrupted in medial frontoparietal cortex. These findings indicate a complex pattern of regional vulnerabilities in brain development that may contribute to the diverse and long-lasting neurobehavioral consequences that can occur after very premature birth."
Moro Reflex
Preterm birth infants (28 to 33 weeks) have an incomplete form of the Moro reflex and postnatal persistence (beyond 4 or 5 months) occurs in infants with severe neurological defects.
| The Moro reflex or "startle reflex" describes a primitive reflex, an involuntary response (reflex) that is present at birth and that normally disappears after 3 or 4 months.
The reflex may have 4 parts:
|
<html5media height="240" width="360">File:Newborn_ab_23.mp4</html5media> |
Sensory Development
Retinopathy of Prematurity
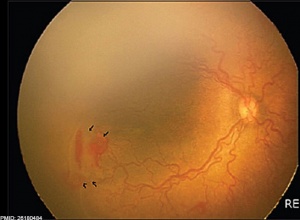
(ROP) A vascular proliferative disorder that affects the incompletely vascularized retina in premature neonates, birth weight 1250 grams or less and born before 31 weeks gestation GA are at highest risk. Classified as type 2 progressing to type 1, this is a primary cause of childhood blindness. Due to retinal immaturity, neovascularization occurs leading to retinal traction and retinal detachment, eventually affecting vision.
USA Statistics
- 14,000-16,000 of low birthweight (<1.25 kg) infants are affected by some degree of ROP.
- disease improves and leaves no permanent damage in milder cases of ROP.
- 90% of all infants with ROP are in the milder category and do not need treatment.
- About 1,100-1,500 infants annually develop ROP that is severe enough to require medical treatment.
- About 400-600 infants each year in the US become legally blind from ROP.
(Data NIH - National Eye Institute)
- Links: Vision Abnormalities | Birth - Preterm | Sensory - Vision Development | NIH - ROP | American Association for Pediatric Ophthalmology)
Metabolism
Both preterm and small-for-gestational-age infants have fewer glycogen and fat stores than full-term neonates. This condition when combined with a maternal diabetic pregnancy, can lead to transient hypoglycemia during the first days of life.
Maternal Obesity
The following text information is from a recent systematic review and meta-analyses of maternal obesity[19]
What is already known on this topic
- The effect of overweight or obesity in women on risk of preterm birth is debated in the literature
- Uncertainty is reflected in national guidelines, although it is widely believed that the risk of having an infant of low birth weight is decreased in overweight or obese women
What this study adds
- Overweight or obese women have increased risks of preterm birth before 32 weeks and induced preterm birth before 37 weeks, and, accounting for publication bias, preterm birth before 37 weeks overall
- The beneficial effects of overweight or obesity on low birth weight were greater in developing than developed countries and disappeared after accounting for publication bias
- Overweight and obese women should be counselled before pregnancy on their perinatal risks, and appropriate surveillance should be considered during pregnancy
Bacterial Infection Fetal Membranes
- Differing prevalence and diversity of bacterial species in fetal membranes from very preterm and term labor.[38]
- "Intrauterine infection may play a role in preterm delivery due to spontaneous preterm labor (PTL) and preterm prolonged rupture of membranes (PPROM). Because bacteria previously associated with preterm delivery are often difficult to culture, a molecular biology approach was used to identify bacterial DNA in placenta and fetal membranes. ...A greater spread and diversity of bacterial species were found in tissues of women who had very preterm births. It is unclear to what extent the greater bacterial prevalence observed in all vaginal delivery groups reflects bacterial contamination or colonization of membranes during labor. Bacteria positive preterm tissues are associated with histological chorioamnionitis and a pronounced maternal immune paresis."
Screening
- Screening to prevent spontaneous preterm birth.[2]
- "For primary prevention, an effective, affordable and safe intervention applied to all mothers without preceding testing is likely to be the most cost-effective approach in asymptomatic women in early pregnancy. For secondary prevention among women at risk of preterm labour in later pregnancy, a management strategy based on the results of testing is likely to be more cost-effective."
Inhaled Nitric Oxide Therapy
NIH Consensus Development Conference (2010) conclusions
- Taken as a whole, the available evidence does not support use of inhaled nitric oxide in early routine, early rescue, or later rescue regimens in the care of premature infants <34 weeks gestation who require respiratory support.
- There are rare clinical situations, including pulmonary hypertension or hypoplasia, that have been inadequately studied in which inhaled nitric oxide may have benefit in infants <34 weeks gestation. In such situations, clinicians should communicate with families regarding the current evidence on its risks and benefits as well as remaining uncertainties.
- Basic research and animal studies have contributed to important understandings of inhaled nitric oxide benefits on lung development and function in infants at high risk of bronchopulmonary dysplasia. These promising results have only partly been realized in clinical trials of inhaled nitric oxide treatment in premature infants. Future research should seek to understand this gap.
- Predefined subgroup and post hoc analyses of previous trials showing potential benefit of inhaled nitric oxide have generated hypotheses for future research for clinical trials. Prior strategies shown to be ineffective are discouraged unless new evidence emerges. The positive results of one multicenter trial, which was characterized by later timing, higher dose, and longer duration of treatment, require confirmation. Future trials should attempt to quantify the individual effects of each of these treatment-related variables (timing, dose, and duration), ideally by randomizing them separately.
- Based on assessment of currently available data, hospitals, clinicians, and the pharmaceutical industry should avoid marketing inhaled nitric oxide for premature infants <34 weeks gestation.
- Links: NIH Consensus Development Conference: Inhaled Nitric Oxide Therapy for Premature Infants October 27-29, 2010 | draft consensus statement
Enteral Nutrition
Enteral nutrition (tube feeding) is often required for preterm or sick infants. Nutritient delivery as fluid into the gastrointestinal tract. Can be used to describe postnatal nutrition through milk as well as a clinical method for delivering nutrition to patients. The method usually involves either a nasogastric or nasoenteral feeding tube into the stomach. An alternative, generally in adults, is a surgical tube placed directly through the skin into the stomach or intestine (gastrostomy or jejunostomy).
References
- ↑ 1.0 1.1 1.2 Born Too Soon: The Global Action Report on Preterm Birth
- ↑ 2.0 2.1 Honest H, Forbes CA, Durée KH, Norman G, Duffy SB, Tsourapas A, Roberts TE, Barton PM, Jowett SM, Hyde CJ & Khan KS. (2009). Screening to prevent spontaneous preterm birth: systematic reviews of accuracy and effectiveness literature with economic modelling. Health Technol Assess , 13, 1-627. PMID: 19796569 DOI.
- ↑ NCHS Data Brief Number 39, May 2010
- ↑ Tiensuu H, Haapalainen AM, Karjalainen MK, Pasanen A, Huusko JM, Marttila R, Ojaniemi M, Muglia LJ, Hallman M & Rämet M. (2019). Risk of spontaneous preterm birth and fetal growth associates with fetal SLIT2. PLoS Genet. , 15, e1008107. PMID: 31194736 DOI.
- ↑ Nunthapiwat S, Sekararithi R, Wanapirak C, Sirichotiyakul S, Tongprasert F, Srisupundit K, Luewan S & Tongsong T. (2019). Second Trimester Serum Biomarker Screen for Fetal Aneuploidies as a Predictor of Preterm Delivery: A Population-Based Study. Gynecol. Obstet. Invest. , , 1-8. PMID: 30602167 DOI.
- ↑ Boardman JP, Ireland G, Sullivan G, Pataky R, Fleiss B, Gressens P & Miron V. (2018). The Cerebrospinal Fluid Inflammatory Response to Preterm Birth. Front Physiol , 9, 1299. PMID: 30258368 DOI.
- ↑ Ngo TTM, Moufarrej MN, Rasmussen MH, Camunas-Soler J, Pan W, Okamoto J, Neff NF, Liu K, Wong RJ, Downes K, Tibshirani R, Shaw GM, Skotte L, Stevenson DK, Biggio JR, Elovitz MA, Melbye M & Quake SR. (2018). Noninvasive blood tests for fetal development predict gestational age and preterm delivery. Science , 360, 1133-1136. PMID: 29880692 DOI.
- ↑ Lo J, Zivanovic S, Lunt A, Alcazar-Paris M, Andradi G, Thomas M, Marlow N, Calvert S, Peacock J & Greenough A. (2018). Longitudinal assessment of lung function in extremely prematurely born children. Pediatr. Pulmonol. , 53, 324-331. PMID: 29316378 DOI.
- ↑ Shimony JS, Smyser CD, Wideman G, Alexopoulos D, Hill J, Harwell J, Dierker D, Van Essen DC, Inder TE & Neil JJ. (2016). Comparison of cortical folding measures for evaluation of developing human brain. Neuroimage , 125, 780-790. PMID: 26550941 DOI.
- ↑ Amiya RM, Mlunde LB, Ota E, Swa T, Oladapo OT & Mori R. (2016). Antenatal Corticosteroids for Reducing Adverse Maternal and Child Outcomes in Special Populations of Women at Risk of Imminent Preterm Birth: A Systematic Review and Meta-Analysis. PLoS ONE , 11, e0147604. PMID: 26841022 DOI.
- ↑ Dunietz GL, Holzman C, McKane P, Li C, Boulet SL, Todem D, Kissin DM, Copeland G, Bernson D, Sappenfield WM & Diamond MP. (2015). Assisted reproductive technology and the risk of preterm birth among primiparas. Fertil. Steril. , 103, 974-979.e1. PMID: 25707336 DOI.
- ↑ Upadhyay K, Pourcyrous M, Dhanireddy R & Talati AJ. (2015). Outcomes of neonates with birth weight⩽500 g: a 20-year experience. J Perinatol , 35, 768-72. PMID: 25950920 DOI.
- ↑ Backes CH, Rivera BK, Haque U, Bridge JA, Smith CV, Hutchon DJ & Mercer JS. (2014). Placental transfusion strategies in very preterm neonates: a systematic review and meta-analysis. Obstet Gynecol , 124, 47-56. PMID: 24901269 DOI.
- ↑ Khatibi A, Brantsaeter AL, Sengpiel V, Kacerovsky M, Magnus P, Morken NH, Myhre R, Gunnes N & Jacobsson B. (2012). Prepregnancy maternal body mass index and preterm delivery. Am. J. Obstet. Gynecol. , 207, 212.e1-7. PMID: 22835494 DOI.
- ↑ Noble KG, Fifer WP, Rauh VA, Nomura Y & Andrews HF. (2012). Academic achievement varies with gestational age among children born at term. Pediatrics , 130, e257-64. PMID: 22753563 DOI.
- ↑ Nosarti C, Reichenberg A, Murray RM, Cnattingius S, Lambe MP, Yin L, MacCabe J, Rifkin L & Hultman CM. (2012). Preterm birth and psychiatric disorders in young adult life. Arch. Gen. Psychiatry , 69, E1-8. PMID: 22660967 DOI.
- ↑ Tepper NK, Farr SL, Cohen BB, Nannini A, Zhang Z, Anderson JE, Jamieson DJ & Macaluso M. (2012). Singleton preterm birth: risk factors and association with assisted reproductive technology. Matern Child Health J , 16, 807-13. PMID: 21516300 DOI.
- ↑ Khashan AS, Baker PN & Kenny LC. (2010). Preterm birth and reduced birthweight in first and second teenage pregnancies: a register-based cohort study. BMC Pregnancy Childbirth , 10, 36. PMID: 20618921 DOI.
- ↑ 19.0 19.1 McDonald SD, Han Z, Mulla S & Beyene J. (2010). Overweight and obesity in mothers and risk of preterm birth and low birth weight infants: systematic review and meta-analyses. BMJ , 341, c3428. PMID: 20647282
- ↑ Curhan GC, Willett WC, Rimm EB, Spiegelman D, Ascherio AL & Stampfer MJ. (1996). Birth weight and adult hypertension, diabetes mellitus, and obesity in US men. Circulation , 94, 3246-50. PMID: 8989136
- ↑ Glass HC, Costarino AT, Stayer SA, Brett CM, Cladis F & Davis PJ. (2015). Outcomes for extremely premature infants. Anesth. Analg. , 120, 1337-51. PMID: 25988638 DOI.
- ↑ 22.0 22.1 Fenton TR. (2003). A new growth chart for preterm babies: Babson and Benda's chart updated with recent data and a new format. BMC Pediatr , 3, 13. PMID: 14678563 DOI.
- ↑ Babson SG & Benda GI. (1976). Growth graphs for the clinical assessment of infants of varying gestational age. J. Pediatr. , 89, 814-20. PMID: 978333
- ↑ Beeby PJ, Bhutap T & Taylor LK. (1996). New South Wales population-based birthweight percentile charts. J Paediatr Child Health , 32, 512-8. PMID: 9007782
- ↑ Ehrenkranz RA, Younes N, Lemons JA, Fanaroff AA, Donovan EF, Wright LL, Katsikiotis V, Tyson JE, Oh W, Shankaran S, Bauer CR, Korones SB, Stoll BJ, Stevenson DK & Papile LA. (1999). Longitudinal growth of hospitalized very low birth weight infants. Pediatrics , 104, 280-9. PMID: 10429008
- ↑ AIHW 2014. Birthweight of babies born to Indigenous mothers. Cat. no. IHW 138. Canberra: AIHW. Viewed 5 August 2014 http://www.aihw.gov.au/publication-detail/?id=60129548202
- ↑ Badgery-Parker T, Ford JB, Jenkins MG, Morris JM & Roberts CL. (2012). Patterns and outcomes of preterm hospital admissions during pregnancy in NSW, 2001-2008. Med. J. Aust. , 196, 261-5. PMID: 22409693
- ↑ Loftin RW, Habli M, Snyder CC, Cormier CM, Lewis DF & Defranco EA. (2010). Late preterm birth. Rev Obstet Gynecol , 3, 10-9. PMID: 20508778
- ↑ Institute of Medicine (US) Committee on Understanding Premature Birth and Assuring Healthy Outcomes; Behrman RE, Butler AS, editors. Preterm Birth: Causes, Consequences, and Prevention. Washington (DC): National Academies Press (US); 2007. Available from: http://www.ncbi.nlm.nih.gov/books/NBK11362
- ↑ Tan JH, Poon WB, Lian WB & Ho SK. (2014). A Comparison of the Short-term Morbidity and Mortality Between Late Preterm and Term Newborns. Ann. Acad. Med. Singap. , 43, 346-54. PMID: 25142470
- ↑ Arisoy R & Yayla M. (2012). Transvaginal sonographic evaluation of the cervix in asymptomatic singleton pregnancy and management options in short cervix. J Pregnancy , 2012, 201628. PMID: 22523687 DOI.
- ↑ Abbott DS, Radford SK, Seed PT, Tribe RM & Shennan AH. (2013). Evaluation of a quantitative fetal fibronectin test for spontaneous preterm birth in symptomatic women. Am. J. Obstet. Gynecol. , 208, 122.e1-6. PMID: 23164760 DOI.
- ↑ Doyle LW. (2012). Antenatal magnesium sulfate and neuroprotection. Curr. Opin. Pediatr. , 24, 154-9. PMID: 22227787 DOI.
- ↑ Jobe AH & Ikegami M. (2001). Antenatal infection/inflammation and postnatal lung maturation and injury. Respir. Res. , 2, 27-32. PMID: 11686862
- ↑ 35.0 35.1 MacKay DF, Smith GC, Dobbie R & Pell JP. (2010). Gestational age at delivery and special educational need: retrospective cohort study of 407,503 schoolchildren. PLoS Med. , 7, e1000289. PMID: 20543995 DOI.
- ↑ Zhang Y, Inder TE, Neil JJ, Dierker DL, Alexopoulos D, Anderson PJ & Van Essen DC. (2015). Cortical structural abnormalities in very preterm children at 7 years of age. Neuroimage , 109, 469-79. PMID: 25614973 DOI.
- ↑ Gadkari SS, Kulkarni SR, Kamdar RR & Deshpande M. (2015). Successful Surgical Management of Retinopathy of Prematurity Showing Rapid Progression despite Extensive Retinal Photocoagulation. Middle East Afr J Ophthalmol , 22, 393-5. PMID: 26180484 DOI.
- ↑ Jones HE, Harris KA, Azizia M, Bank L, Carpenter B, Hartley JC, Klein N & Peebles D. (2009). Differing prevalence and diversity of bacterial species in fetal membranes from very preterm and term labor. PLoS ONE , 4, e8205. PMID: 19997613 DOI.
Books
- Deshpande SN, van Asselt ADI, Tomini F, et al. Rapid fetal fibronectin testing to predict preterm birth in women with symptoms of premature labour: a systematic review and cost analysis. Southampton (UK): NIHR Journals Library; 2013 Sep. (Health Technology Assessment, No. 17.40.) Available from: http://www.ncbi.nlm.nih.gov/books/NBK261021/
- Institute of Medicine (US) Committee on Understanding Premature Birth and Assuring Healthy Outcomes; Behrman RE, Butler AS, editors. Preterm Birth: Causes, Consequences, and Prevention. Washington (DC): National Academies Press (US); 2007. Available from: http://www.ncbi.nlm.nih.gov/books/NBK11362/
- Likis FE, Andrews JC, Woodworth AL, et al. Progestogens for Prevention of Preterm Birth [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2012 Sep. (Comparative Effectiveness Reviews, No. 74.) Available from: http://www.ncbi.nlm.nih.gov/books/NBK109368/
Reviewss
Matei A, Saccone G, Vogel JP & Armson AB. (2019). Primary and secondary prevention of preterm birth: a review of systematic reviews and ongoing randomized controlled trials. Eur. J. Obstet. Gynecol. Reprod. Biol. , , . PMID: 30772047 DOI.
Khanprakob T, Laopaiboon M, Lumbiganon P & Sangkomkamhang US. (2012). Cyclo-oxygenase (COX) inhibitors for preventing preterm labour. Cochrane Database Syst Rev , 10, CD007748. PMID: 23076936 DOI.
Likis FE, Edwards DR, Andrews JC, Woodworth AL, Jerome RN, Fonnesbeck CJ, McKoy JN & Hartmann KE. (2012). Progestogens for preterm birth prevention: a systematic review and meta-analysis. Obstet Gynecol , 120, 897-907. PMID: 22955308 DOI.
Alfirevic Z, Milan SJ & Livio S. (2012). Caesarean section versus vaginal delivery for preterm birth in singletons. Cochrane Database Syst Rev , , CD000078. PMID: 22696314 DOI.
Articles
Iacobelli S, Kermorvant-Duchemin E, Bonsante F, Lapillonne A & Gouyon JB. (2012). Chloride Balance in Preterm Infants during the First Week of Life. Int J Pediatr , 2012, 931597. PMID: 22505945 DOI.
Search Pubmed
July 2010 "Preterm Birth" All (31665) Review (3598) Free Full Text (4781)
Search Pubmed: Preterm Birth | Ultrasound Short Cervix
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- WHO Report 2012 Born Too Soon: The Global Action Report on Preterm Birth
- The Partnership (PMNCH) - joins the maternal, newborn and child health (MNCH) communities into an alliance of more than 350 members to ensure that all women, infants and children not only remain healthy, but thrive. Born Too Soon: The Global Action Report on Preterm Birth
- Sydney Local Health District Pamphlet - Enteral Nutrition for the Preterm Infant PDF
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 27) Embryology Birth - Preterm. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Birth_-_Preterm
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G