Endocrine - Adrenal Development: Difference between revisions
No edit summary |
|||
| Line 8: | Line 8: | ||
{{Template:Endocrine Links}} | [[2009_Lecture_12|Lecture - Neural Crest Development]] | [http://embryology.med.unsw.edu.au/Notes/endocrine9.htm original page] | {{Template:Endocrine Links}} | [[2009_Lecture_12|Lecture - Neural Crest Development]] | [http://embryology.med.unsw.edu.au/Notes/endocrine9.htm original page] | ||
==Some Recent Findings== | ==Some Recent Findings== | ||
| Line 30: | Line 18: | ||
* '''Development and Function of the Human Fetal Adrenal Cortex: A Key Component in the Feto-Placental Unit'''<ref><pubmed>21051591</pubmed></ref> "The steroidogenic activity is characterized by early transient cortisol biosynthesis, followed by its suppressed synthesis until late gestation, and extensive production of dehydroepiandrosterone and its sulfate, precursors of placental estrogen, during most of gestation. The gland rapidly grows through processes including cell proliferation and angiogenesis at the gland periphery, cellular migration, hypertrophy, and apoptosis." (See also [[Fetal Development]]) | * '''Development and Function of the Human Fetal Adrenal Cortex: A Key Component in the Feto-Placental Unit'''<ref><pubmed>21051591</pubmed></ref> "The steroidogenic activity is characterized by early transient cortisol biosynthesis, followed by its suppressed synthesis until late gestation, and extensive production of dehydroepiandrosterone and its sulfate, precursors of placental estrogen, during most of gestation. The gland rapidly grows through processes including cell proliferation and angiogenesis at the gland periphery, cellular migration, hypertrophy, and apoptosis." (See also [[Fetal Development]]) | ||
|} | |} | ||
==Adrenal Overview== | |||
* Richly vascularized - arterioles passing through cortex, capillaries from cortex to medulla, portal-like circulation | |||
* Fetal Cortex - produces a steroid precursor (DEA), converted by placenta into estrogen | |||
* Adult Medulla - produces adrenalin (epinephrine), noradrenaline (norepinephrine) | |||
* Fetal adrenal hormones - influence lung maturation | |||
===Cortical Hormones=== | |||
(steroids) Cortisol, Aldosterone, Dehydroepiandrosterone | |||
* zona glomerulosa - regulated by renin-angiotensin-aldosterone system controlled by the juxtaglomerular apparatus of the kidney. | |||
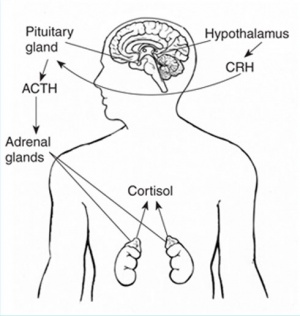
* zona fasciculata - regulated by hypothalamo-pituitary axis with the release of CRH and ACTH respectively. | |||
===Medullary Hormones=== | |||
(amino acid derivatives) Epinephrine, Norepinephrine | |||
==Adrenal Development== | ==Adrenal Development== | ||
Revision as of 14:15, 28 August 2011
Introduction
The developing adrenal gland has both an interesting origin and an intruiging fetal role. Furthermore recent studies suggest that the adrenal cortex share a common embryonic origin with the early gonad. The adrenal gland and placenta also act in synergy, and the notes endocrine placenta should also be read.
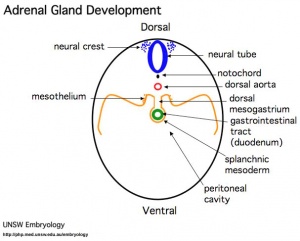
The 2 adrenal glands (suprarenal gland, glandulæ suprarenales) are named by their anatomical postion sitting above the 2 kidneys (renal). The 2 main parts of the adrenals have different embryonic origins. The inside core adrenal medulla is neural crest in origin. Mesenchyme surrounding these cells differentiates to form a fetal cortex. This fetal cortex is later replaced by the adult cortex. The outside adrenal cortex is derived from mesothelium and can be further divided into 3 distinct layers (zona reticularis, zona fasiculata, zona glomerulosa) each with distinct hormonal functions.
During fetal development, adrenal hormones are involved with the maturation of the lung and other developing systems.
| Lecture - Neural Crest Development | original page
Some Recent Findings
|
Adrenal Overview
- Richly vascularized - arterioles passing through cortex, capillaries from cortex to medulla, portal-like circulation
- Fetal Cortex - produces a steroid precursor (DEA), converted by placenta into estrogen
- Adult Medulla - produces adrenalin (epinephrine), noradrenaline (norepinephrine)
- Fetal adrenal hormones - influence lung maturation
Cortical Hormones
(steroids) Cortisol, Aldosterone, Dehydroepiandrosterone
- zona glomerulosa - regulated by renin-angiotensin-aldosterone system controlled by the juxtaglomerular apparatus of the kidney.
- zona fasciculata - regulated by hypothalamo-pituitary axis with the release of CRH and ACTH respectively.
Medullary Hormones
(amino acid derivatives) Epinephrine, Norepinephrine
Adrenal Development
- Fetal Adrenals - fetal cortex later replaced by adult cortex
- Week 6 - fetal cortex, from mesothelium adjacent to dorsal mesentery; Medulla, neural crest cells from adjacent sympathetic ganglia
- Adult cortex - mesothelium mesenchyme encloses fetal cortex
Adrenal Cortex
- Late Fetal Period - differentiates to form cortical zones
- Birth - zona glomerulosa, zona fasiculata present
- Year 3 - zona reticularis present
Adrenal Medulla
- neural crest origin, migrate adjacent to coelomic cavity, initially uncapsulated and not surrounded by fetal cortex, cells have neuron-like morphology
- 2 cell types - secrete epinepherine (adrenaline) 80%; secrete norepinepherine (noradrenaline* 20%
- Media:Adrenal_medulla.mov
Development Overview
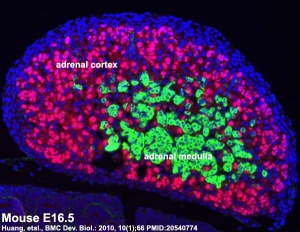
Medulla - Neural crest cells migrate toward the coelomic cavity wall and form the adrenal medulla. These chromaffin (chromaphil) cells originally named because of their staining (yellow) with chromium salts. (More? [#Medulla Adrenal Medulla])
Cortex - Week 4 celomic epithelium (mesothelium) cells proliferate initially forming small buds that separate from the epithelium. Week 6 these now mesenchymal cells first form the fetal adrenal cortex which will be later replaced by the adult cortex. (More? [#Cortex Adrenal Cortex])
Adrenal Cortex
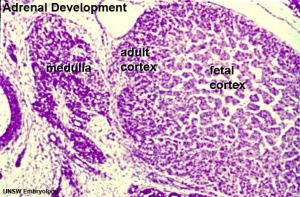
|
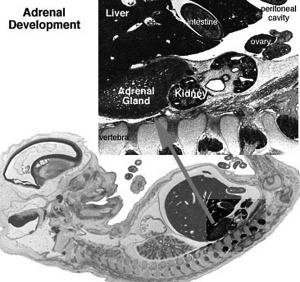
|
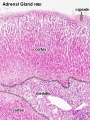
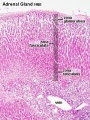
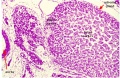
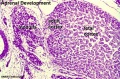
| Human Embryo (7 weeks, stage 22) adrenal gland showing the fetal and permanent adrenal cortex. Note that the medulla of the adrenal gland is not yet encapsulated by the cortex. | Human Fetus (10 week, 40mm, parasagittal section) shows location of the developing adrenal gland. The spongy appearance at the centre of the adrenal is the degenerating fetal cortex. The dense region around the outside of the adrenal is the developing adult cortex.) |
Week 4 - coelomic epithelium (mesothelium) cells proliferate initially forming small buds that separate from the epithelium.
Week 6 - these now mesenchymal cells surrounding the developing medulla cells differentiate first form the fetal adrenal cortex which will be later replaced by the adult cortex.
Week 8 to 9 - fetal adrenal cortex synthesizes cortisol and is maximal at 8-9 weeks post conception (wpc) under the regulation of ACTH (also stimulates androstenedione and testosterone secretion).[4]
Adult cortex - mesothelium mesenchyme encloses fetal cortex.
Late Fetal Period - differentiates to form cortical zones.
Birth - zona glomerulosa, zona fasiculata present.
Year 3 - zona reticularis present.
Fetal Cortex
Fetal adrenal cortical growth involves several cellular processes: hypertrophy, hyperplasia, apoptosis, and migration.
In the second and third trimesters a steroid precursor dehydroepiandrosterone (DHEA) and sulphated derivative (DHEAS) which is converted by placenta into estrogen.
Three functional zones:
- Fetal zone - throughout gestation expresses enzymes required for DHEA-S synthesis.
- Transitional zone - initially identical to the fetal zone but later (after 25-30 weeks) expresses enzymes that suggest glucocorticoid synthesis.
- Definitive zone - after 22-24 weeks expresses enzymes that suggest mineralocorticoid synthesis.
Neonatal
- human males produce high levels of DHEA) and DHEAS
- decline within a few months of birth
- due to regression of the adrenal fetal zone
Adult
- zona reticularis (ZR) source for production of DHEA and DHEAS
Adult Cortex
Early Adult Cortex (week 12)
- Reticularis - narrow band, many small cells and capillaries androgens. source for production of DHEA and DHEAS
- Fasiculata - high lipid content, pale foamy cells cortisol, corticosterone, cortisone.
- Glomerulosa - small cells, cords or oval groups, aldosterone.
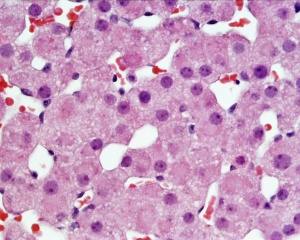
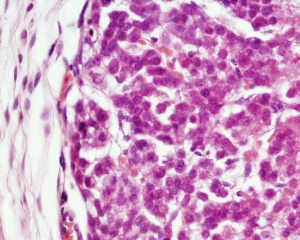
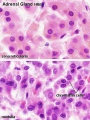
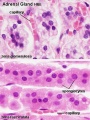
Adult Histology
Molecular
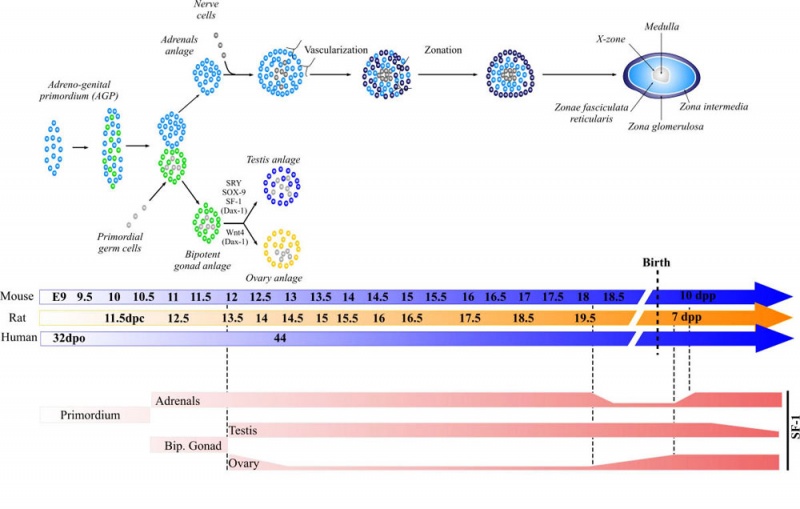
Steroidogenic Factor 1
Adrenal and gonad steroidogenic factor 1 (SF-1) expression in different species [5]
- 53 kDa protein called Ad4BP (Adrenal 4 Binding Protein) or SF-1 (Steroidogenic Factor 1)
- classical DNA-binding domain (DBD) characterized by two Cys2-Cys2 zinc fingers in the N-terminal region
- SF-1 binds DNA as a monomer
- high homology with the drosophila Ftz-F1 transcription factor that controls fushi tarazu homeotic gene expression
Steroidogenic Factor 1 Mutation Effects
| Organism | Human | ||
| Genotype | SF-1 -/- | SF-1 +/- | SF-1 -/+ or SF-1 -/- |
| Adrenal | Agenesis | Histological defects
Hyporesponse to stress Compensatory growth defects |
Insufficiency (agenesis or dysgenesis) |
| Testis | Agenesis
Sex reversal |
Sex reversal | |
| Ovary | Agenesis | Normal | |
| Ventro-Medial Hypothalamus | Agenesis
Obesity caused by absence of the VMH (8 weeks) |
||
| Pituitary | Defects of gonadotrope cells | ||
Table modified from review.[5]
SoxE
Sry-box (Sox) 8, and Sox10 are expressed in the neural crest and in neural crest cells migrating to the adrenal gland.[6]
DAX1
CYP17
Abnormalities
Congenital Adrenal Hyperplasia
(CAH) A family of inherited disorders of adrenal steroidogenesis enzymes which impairs cortisol production by the adrenal cortex.
Enzymes most commonly affected: 21-hydroxylase (21-OH), 11beta-hydroxylase, 3beta-hydroxysteroid dehydrogenase.
Enzymes less commonly affected: 17alpha-hydroxylase/17,20-lyase and cholesterol desmolase.
Classical CAH - androgen excess leads newborn females with external genital ambiguity and postnatal progressive virilization in both sexes.
Pheochromocytomas
(PCC) Catecholamine-producing (neuro)endocrine tumor located in the adrenal medulla. Similar catecholamine-producing tumors outside the adrenal gland are called paragangliomas (PGL).
Cushing's Syndrome
(hypercortisolism) A relatively rare metabolic hormonal disorder caused by prolonged exposure of the body’s tissues to high levels of the adrenal hormone cortisol, most commonly affects adults aged between 20 to 50 and also the obese with type 2 diabetes.
Adrenocortical Tumour
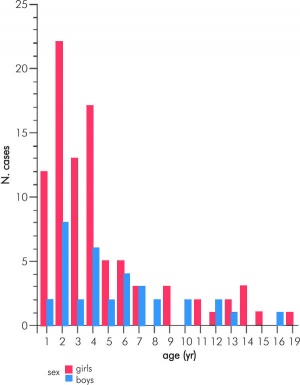
Adrenocortical tumours (ACT) can occur at all ages and have a bimodal distribution with peaks of incidence at about 5 years of age and again at 40 to 50 years of age. Clinically, a routine hormonal profile for suspected patients includes measurements of serum (8am, 11pm) cortisol, testosterone, DHEA-S, androstenedione, 17-hydroxyprogesterone, aldosterone, and plasma renin activity.[7]
References
Online Textbooks
Endocrinology: An Integrated Approach Nussey, S.S. and Whitehead, S.A. Oxford, UK: BIOS Scientific Publishers, Ltd; 2001. 4.7. Embryology of the adrenal gland | The Adrenal Gland | Anatomical and functional zonation in the adrenal cortex
Developmental Biology (6th ed) Gilbert, Scott F. Sunderland (MA): Sinauer Associates, Inc.; c2000. Figure 13.6. Final differentiation of a trunk neural crest cell committed to become either an adrenomedullary (chromaffin) cell or a sympathetic neuron
Molecular Biology of the Cell (4th Edn) Alberts, Bruce; Johnson, Alexander; Lewis, Julian; Raff, Martin; Roberts, Keith; Walter, Peter. New York: Garland Publishing; 2002. table 15-1. Some Hormone-induced Cell Responses Mediated by Cyclic AMP | Cells Can Respond Abruptly to a Gradually Increasing Concentration of an Extracellular Signal
Health Services/Technology Assessment Text (HSTAT) Bethesda (MD): National Library of Medicine (US), 2003 Oct. Adrenal Gland search Results
Search NLM Online Textbooks- "adrenal development" : Endocrinology | Molecular Biology of the Cell | The Cell- A molecular Approach
Reviews
<pubmed>18670886</pubmed> <pubmed>18493131</pubmed> <pubmed>17046275</pubmed> <pubmed>16928368</pubmed> <pubmed>16807499</pubmed> <pubmed>9888597</pubmed> <pubmed>9183569</pubmed>| Endocrine Reviews
Articles
<pubmed>20010965</pubmed> <pubmed>19723922</pubmed> <pubmed>17537799</pubmed> <pubmed>16585961</pubmed> <pubmed>16093324</pubmed> <pubmed>11319516</pubmed> <pubmed>9888597</pubmed>"The rapid growth of the human fetal adrenal gland, which is primarily a reflection of the growth of the unique fetal zone, is regulated by ACTH acting indirectly to stimulate the expression of locally produced growth factors, of which IGF-II and bFGF appear to play key roles. Through most of gestation, the outer definitive zone appears to function as a reservoir of progenitor cells which move centripetally to populate the rest of the gland. At the end of pregnancy, the fetal zone undergoes senescence through an apoptotic process. Activin and TGF-beta are capable of inducing apoptosis in the fetal zone. Corticotropin-releasing hormone, which is produced by the placenta in markedly increased amounts at the end of gestation, may orchestrate a variety of processes, including direct stimulation of fetal adrenal steroidogenesis, culminating in the initiation of parturition."
Search PubMed
Search April 2010
- Adrenal Development - All (646) Review (52) Free Full Text (84)
- Congenital Adrenal Hyperplasia - All (2091) Review (211) Free Full Text (314)
Search Pubmed: adrenal development | Congenital Adrenal Hyperplasia
Additional Images
Terms
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, June 27) Embryology Endocrine - Adrenal Development. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Endocrine_-_Adrenal_Development
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G