Birth - Caesarean Delivery: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 19: | Line 19: | ||
|-bgcolor="F5FAFF" | |-bgcolor="F5FAFF" | ||
| | | | ||
* '''Could Revision of the Embryology Influence Our Cesarean Delivery Technique'''<ref name=PMID28078171><pubmed>28078171</pubmed></ref> "Until today, there is no standardized Cesarean Section method and many variations exist. The main variations concern the type of abdominal incision, usage of abdominal packs, suturing the uterus in one or two layers, and suturing the peritoneal layers or leaving them open. One of the questions is the optimal location of opening the uterus. Recently, omission of the bladder flap was recommended. The anatomy and histology as results from the embryological knowledge might help to solve this question. The working thesis is that the higher the incision is done, the more damage to muscle tissue can take place contrary to incision in the lower segment, where fibrous tissue prevails. In this perspective, a call for participation in a two-armed prospective study is included, which could result in an optimal, evidence-based Cesarean Section for universal use." | |||
* '''Does the presence of a Caesarean section scar affect implantation site and early pregnancy outcome in women attending an early pregnancy (12 weeks gestation) assessment unit?'''<ref name=PMID23585560><pubmed>23585560</pubmed></ref>"Implantation was most frequently posterior (53%) in the CS group and fundal in the non-CS group (42%). Gestation sac implantation was 8.7 mm lower in the CS group. Presenting complaints differed in women with and without a previous CS (P = 0.0009). More frequent vaginal bleeding yet no clearly increased spontaneous abortion rates were noted in the CS group compared with the non-CS group. A weakness of the study is the lack of a reference technique to verify the location of implantation." | * '''Does the presence of a Caesarean section scar affect implantation site and early pregnancy outcome in women attending an early pregnancy (12 weeks gestation) assessment unit?'''<ref name=PMID23585560><pubmed>23585560</pubmed></ref>"Implantation was most frequently posterior (53%) in the CS group and fundal in the non-CS group (42%). Gestation sac implantation was 8.7 mm lower in the CS group. Presenting complaints differed in women with and without a previous CS (P = 0.0009). More frequent vaginal bleeding yet no clearly increased spontaneous abortion rates were noted in the CS group compared with the non-CS group. A weakness of the study is the lack of a reference technique to verify the location of implantation." | ||
* '''NIH Consensus Development Conference Draft Statement on Vaginal Birth After Cesarean: New Insights'''<ref><pubmed>20228855</pubmed></ref> | * '''NIH Consensus Development Conference Draft Statement on Vaginal Birth After Cesarean: New Insights'''<ref><pubmed>20228855</pubmed></ref> | ||
Revision as of 12:55, 16 January 2017
Introduction
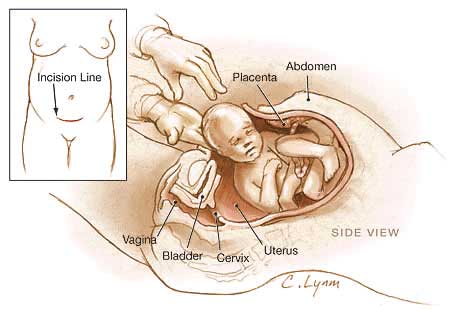
The term "caesarean" comes from the historic description of Julius Ceasar's birth, though probably ficticious as his mother Aurelia survived his birth. The procedure involves surgically cutting skin, abdominal wall and uterus to allow abdominal delivery.
The rate of caesarean delivery compared to normal vaginal birth is variable between countries (12-25%, 20% of all births in Australia) and increasing, particularly in older women. There are a number of different explanations as to why this is occuring, including maternal or fetal complications of either development or delivery.
Importantly this is a maternal surgical procedure which requires time for recovery and there are several studies that have looked also into the effects of caesarean delivery on potential future normal vaginal births.
Please note the UK/Australian "Caesarean" versus USA "Cesarean" spelling differences. Clinically, cesarean section may also be abbreviated to c-section or C/S.
Video Webcast: Hartford Hospital Cesarean Childbirth (September 23rd, 2005)
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Caesarean Birth <pubmed limit=5>Caesarean Birth</pubmed> |
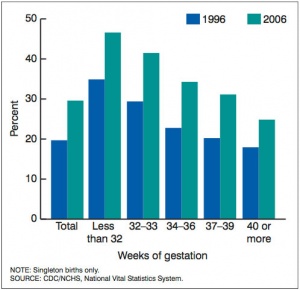
USA Caesarean Rate by Gestational Age
Latest 2013 data[8]

|
|
Trial of Labor
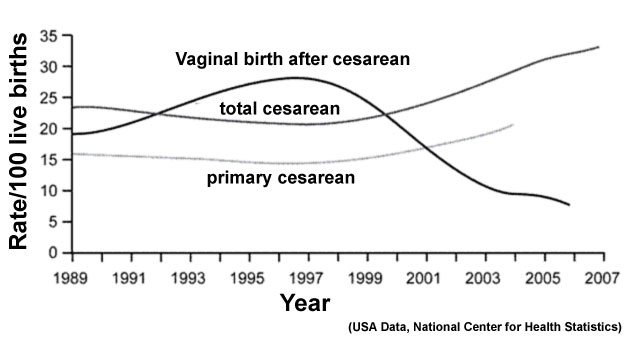
Trial of Labor (TOL) or trial of labor after cesarean (TOLAC) is a term used in relation to the offer for a normal vaginal delivery after a previous cesarean delivery. The resulting birth is described as vaginal birth after cesarean (VBAC), in recent years this option has been decreasing while the general caesarian rate increases.
Positive Factors
(increased likelihood of successful VBAC)
- Maternal age <40 years
- Prior vaginal delivery (particularly prior successful VBAC)
- Favorable cervical factors
- Presence of spontaneous labor
- Nonrecurrent indication that was present for prior cesarean delivery
Negative Factors
(decreased likelihood of successful VBAC)
- Increased number of prior cesarean deliveries
- Gestational age >40 weeks
- Birth weight >4,000 g
- Induction or augmentation of labor
Links: USA Guideline (2005) | NIH Consensus - Vaginal Birth After Cesarean (2010)
Caesarean Classification

There is no standard clinical classification system for caesarean delivery, with at least 27 classifications identified.[10] Recent studies of data from several countries[9] suggests that the 10 group classification system (Robson Classification[11]), or a modification of this system, may be the current best applied system.
Robson Classification
The Robson's classification[11] (10 group classification) is based on several simple obstetrical parameters; parity, previous CS, gestational age, onset of labour, fetal presentation and the number of foetuses. The classification categories are totally inclusive and also mutually exclusive.
- Links: WHO Robson Classification
References
- ↑ <pubmed>28078171</pubmed>
- ↑ <pubmed>23585560</pubmed>
- ↑ <pubmed>20228855</pubmed>
- ↑ <pubmed>19874598</pubmed>
- ↑ <pubmed>20071021</pubmed>
- ↑ <pubmed>20070708</pubmed>
- ↑ <pubmed>22114995</pubmed>
- ↑ Martin JA, Hamilton BE, Osterman MJK, et al. Births: Final data for 2013. National vital statistics reports; vol 64 no 1. Hyattsville, MD: National Center for Health Statistics. 2015. http://www.cdc.gov/nchs/data/nvsr/nvsr64/nvsr64_01.pdf
- ↑ 9.0 9.1 <pubmed>24892928</pubmed>| PLoS One.
- ↑ <pubmed>21283801</pubmed>| PLoS One.
- ↑ 11.0 11.1 <pubmed>11359322</pubmed>
Books
Caesarean Section NICE Clinical Guidelines, No. 13 National Collaborating Centre for Women's and Children's Health (UK). London: RCOG Press; 2004 Apr. ISBN-10: 1-904752-02-0 Bookshelf
Reviews
<pubmed>14974041</pubmed>
- Journal of American Medical Association JAMA Patient Page: Cesarean Delivery (USA) - one page Caesarean delivery information sheet (PDF)
- electronic Med J Aust Caesarean section: a matter of choice? by de Costa, C.M. MJA 1999; 170: 572-573
Articles
<pubmed></pubmed> <pubmed></pubmed> <pubmed>19874628</pubmed>
Search PubMed
Search Pubmed: Caesarean Delivery | Cesarean Delivery
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, June 10) Embryology Birth - Caesarean Delivery. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Birth_-_Caesarean_Delivery
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G