Birth - Stillbirth and Perinatal Death
| Embryology - 17 Apr 2026 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
| Educational Use Only - Embryology is an educational resource for learning concepts in embryological development, no clinical information is provided and content should not be used for any other purpose. |
Introduction
Worldwide about 2.6 million babies are stillborn, 15 million are preterm births ( less than 37 weeks gestation GA), and 32 million are born small for gestational age.
The perinatal period is the early postnatal period relating to the birth, statistically it includes the period up to 7 days after birth. Neonatal period is the four weeks/month after birth.
Stillbirth and perinatal death can be classified by a number of different systems, all still have "unexplained" or "other" as a potential option. in several systems contribute to many of these deaths. Neonatal deaths include a broader age range of infants who have also died after birth from various causes.
Stillbirths with a gestational age of 28 weeks or more are defined as "late fetal deaths".
There are several death classification systems used in different countries around the world, the most recent are the suggested ReCoDe (UK, 2005), the modified Whitfield (Australia/New Zealand, 2004), and the World Health Organization's International Classification of Disease (ICD-10) systems.
A common stillbirth and perinatal death classification is still "unexplained", with recent analysis of data showing fetal growth restriction is a common antecedent.
World Health Organization international definition for perinatal deaths - "Stillbirths and neonatal deaths are defined as third trimester perinatal deaths—greater than or equal to 28 weeks gestational age and/or greater than or equal to 1,000 grams birthweight (WHO 2015)."
The WHO definition differs from the standard definitions used for stillbirths and neonatal deaths in Australia — greater than or equal to 20 weeks' gestational age or greater than and/or equal to 400 grams birthweight.
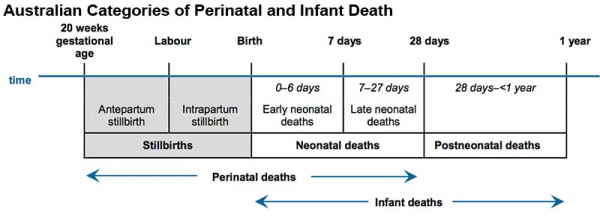
|
| Australian Categories of Perinatal and Infant Death[2] |
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Stillbirth | Perinatal Death |
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
|
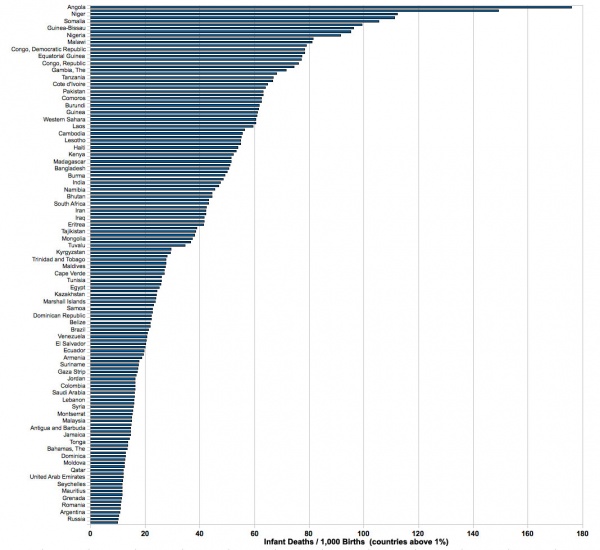
World High Rate Countries
Graph shows the number of infant deaths / 1,000 live births for countries above 1%.
Classification Differences
- World Health Organization - report stillbirths weighing 500g, or born at or after 22 weeks gestational age GA, or 25 cm crown-heel length (CRL), if neither birthweight nor gestational age is known. Restrict stillbirth used for international reporting to those weighing 1,000g (or born at or after 28 weeks gestational age or 35 cm CRL.
- Australia - a baby who is stillborn must be of at least 20 weeks gestational age or weigh 400g or more.
- New Zealand - include all fetal deaths from 20 week gestational age or 400g birthweight[16].
- Canada - includes fetal deaths from 20 week gestational age or 500g birthweight in all provinces except Quebec where only the birthweight criterion applies. [17]
- United States - states to report fetal deaths of 20 or more weeks gestation, but the definition of a ‘fetal death’ specifically excludes deaths that result from induced termination of pregnancy.[18]
- United Kingdom - 24 weeks gestational age and includes all fetal deaths that meet this criterion.
- Europe - the lower limit ranges from 16–26 weeks gestational age and member states vary in their capacity to include late termination of pregnancy that meet their gestation criterion for a stillbirth (Gissler 2012).
Decreased Fetal Movements
Decreased fetal movements (DFM) can occur during the normal fetal period. Pregnancies with multiple occasions of decreased fetal movements are at increased risk of poor perinatal outcomes, including fetal death, intrauterine fetal growth restriction (IUFGR) or preterm birth. An evaluation of women presenting with DFM should involve a thorough history, examination and auscultation of fetal heart, cardiotocography (CTG) and ultrasound if indicated. There are guidelines and position statements available for DFM.
There have been studies using maternal recording of movements, that have limitations of non-compliance and initial analysis shows poor correlation.[19]
A population-based study has also been unable to link, except for some subgroups, maternally perceived DFM to placental pathology.[20]
- Links: fetal | ultrasound | Australia RANZCOG Guideline 2013 PDF | Health 2011 | UK 2011 Guideline No. 57 | USA Reduced fetal movements 2011
Uterine Artery Pulsatility Index
Uterine Artery Pulsatility Index (UT-PI) is a clinical ultrasound technique used for monitoring placental and fetal function. Can be used in second trimester screening in combination with maternal factors and fetal biometry to predict stillbirths and in particular those associated with impaired placentation.PubmedParser error: The PubmedParser extension received invalid XML data. () Maternal factors can include measurement of maternal serum placental growth factor (PLGF) levels.PubmedParser error: The PubmedParser extension received invalid XML data. ()
Australian Data
Australia 2015–2016
Stillbirths and neonatal deaths in Australia 2015 and 2016 (4 July 2019)[4] In 2015 and 2016, 623,701 babies born in Australia to 614,515 women. Approximately 6 stillbirths and 2 neonatal deaths occur each day. Almost 30% of perinatal deaths were caused by congenital anomaly (5,702 perinatal deaths; 4,263 stillbirths and 1,439 neonatal deaths). 9.1 perinatal deaths per 1,000 births (6.8 stillbirths per 1,000 births and 2.3 neonatal deaths per 1,000 live births).
Australia 2013–2014
Stillbirths in Australia 2013–2014[5] 2013 and 2014 - 622,037 babies were born in Australia and 6,037 of those babies died in the perinatal period, 4,419 stillbirths and 1,618 neonatal deaths, perinatal mortality rate was 9.7 per 1,000 births, stillbirth (fetal mortality) rate was 7.1 per 1,000 births, neonatal mortality rate 2.6 per 1,000 live births. Between 1995 and 2014 there has been some reduction in neonatal mortality rate, but the stillbirth rate has remained relatively unchanged.
Australia 2000–2009
| Australian Perinatal Deaths | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Year | 2000 | 2001 | 2002 | 2003 | 2004 | 2005 | 2006 | 2007 | 2008 | 2009 |
| Rate | 10.1 | 10.4 | 9.8 | 9.8 | 9.9 | 10.6 | 9.2 | 8.8 | 8.4 | 9.0 |
| Number | 2,534 | 2,571 | 2,475 | 2,480 | 2,541 | 2,769 | 2,459 | 2,532 | 2,501 | 2,671 |
- Perinatal deaths are all fetal deaths (at least 20 weeks gestation or at least 400 grams birth weight) plus all neonatal deaths (death of a live born baby within 28 completed days of birth).
- Perinatal death rates are calculated per 1,000 all births for the calendar year.
- Source: ABS Births, Australia, 2009 (cat. no. 3301.0); ABS Perinatal Deaths, Australia, 2009 (cat. no. 3304.0).
Australia 1991–2009
- Stillbirths in Australia 1991-2009Hilder L, Li Z, Zeki R & Sullivan EA 2014. Stillbirths in Australia 1991-2009. Perinatal statistics series no. 29. Cat. no. PER 63. Canberra: AIHW. "In 2009, 2,341 babies were stillborn, accounting for almost three quarters of perinatal deaths. In Australia a 'stillbirth' is defined as the birth of a baby who shows no signs of life after a pregnancy of at least 20 weeks gestation or weighing 400 grams or more. Congenital anomalies, or birth defects, are the most common cause of stillbirth in Australia, accounting for 21% of all stillbirths. From 1991 to 2009, the stillbirth rate in Australia was between 6.4 and 7.8 per 1,000 births. The risk of stillbirth occurring between 28 and 41 weeks gestation dropped between 1991 and 2009, however there was an increase in the risk of stillbirths from 20-27 weeks." Reports Australian Statistics
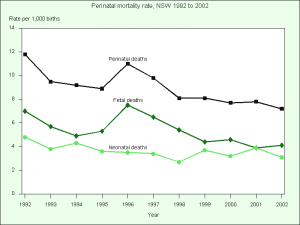
NSW
In New South Wales (2002) 613 perinatal deaths were reported.
- Unexplained antepartum deaths: 26.3% of perinatal deaths (or 39.2% of stillbirths)
- Spontaneous preterm labour: 20.6% (less than 37 weeks gestation)
- Congenital abnormality: 16.8%
- Antepartum haemorrhage: 8.5%
- Specific perinatal conditions: 7.3%, of which twin-twin transfusion accounted for 2.3% of deaths
- Hypertension (high blood pressure): 5.5%
- Perinatal infection: 4.4%
- Maternal disease: 4.4%
- Hypoxic peripartum death: 3.8%
Neonatal deaths (four weeks/month after birth)
- extreme prematurity was most common cause (39.6%)
- congenital abnormality (19.3%)
- neurological disease (13.4%)
- cardio-respiratory conditions (11.9%)
- infection (8.4%)
Data: Report of the New South Wales Chief Health Officer, 2004 accessed 19Oct05
USA Data
USA 2016
Deaths: Leading Causes for 2016[21] This report presents final 2016 data on the 10 leading causes of death in the United States by age, sex, race, and Hispanic origin. Leading causes of infant, neonatal, and postneonatal death are also presented. This report supplements "Deaths: Final Data for 2016," the National Center for Health Statistics' annual report of final mortality statistics. Report PDF
- Leading causes of infant death for 2016 were, in rank order: Congenital malformations, deformations and chromosomal abnormalities; Disorders related to short gestation and low birth weight, not elsewhere classified; Sudden infant death syndrome; Newborn affected by maternal complications of pregnancy; Accidents (unintentional injuries); Newborn affected by complications of placenta, cord and membranes; Bacterial sepsis of newborn; Respiratory distress of newborn; Diseases of the circulatory system; and Neonatal hemorrhage. Important variations in the leading causes of infant death are noted for the neonatal and postneonatal periods.
Infant mortality rates are the most commonly used index for measuring the risk of dying during the first year of life.
- Use the number of live births to approximate the population at risk of dying before the first birthday.
- Calculated by dividing the number of infant deaths in a calendar year by the number of live births registered for the same period and are presented as rates per 100,000 live births.
Neonatal and postneonatal mortality rates are also calculated using live births in the denominator.
USA 2005
Leading causes of infant death for 2005:[23]
- Congenital malformations, deformations and chromosomal abnormalities
- Disorders related to short gestation and low birthweight, not elsewhere classified
- Sudden infant death syndrome
- Newborn affected by maternal complications of pregnancy
- Newborn affected by complications of placenta, cord and membranes
- Accidents (unintentional injuries); Respiratory distress of newborn
- Bacterial sepsis of newborn
- Neonatal hemorrhage
- Necrotizing enterocolitis of newborn.
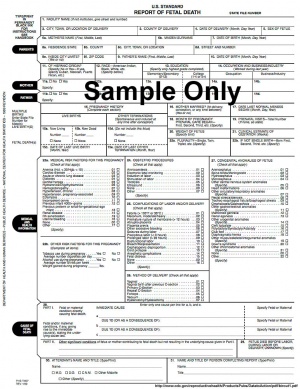
Fetal Death Information
- 2003 Revisions of the U.S. Standard Certificates of Live Birth and Death and the Fetal Death Report. The revision process is generally carried out every 10 to 15 years.
- Maternal, Paternal and medical and health information is collected.
CAUSE/CONDITIONS CONTRIBUTING TO FETAL DEATH
- INITIATING CAUSE/CONDITION
- OTHER SIGNIFICANT CAUSES OR CONDITIONS
- WEIGHT OF FETUS (grams preferred, specify unit)
- ESTIMATED TIME OF FETAL DEATH
- WAS AN AUTOPSY PERFORMED?
- WAS A HISTOLOGICAL PLACENTAL EXAMINATION PERFORMED?
- WERE AUTOPSY OR HISTOLOGICAL PLACENTAL EXAMINATION RESULTS USED IN DETERMINING THE CAUSE OF FETAL DEATH?
Links: 2003 Revisions of the U.S. Standard Certificates of Live Birth and Death and the Fetal Death Report
Germany
Stillbirths in Germany 2003 - 2011[9] Searches in the international peer-reviewed literature, retrospective data collection of 168 stillbirths in 8 hospitals, (in the area of Bonn) with subsequent statistical evaluation (descriptive statistics, t-test and binominal test) were undertaken. This study shows considerable deficits in data documentation, interdisciplinary communication and postmortal examination. Only in 51.8% (87/168) of the cases was a certain or uncertain cause of death found (42.3% placental, 1.2% foetal, 3.6% chromosomal, 4.8% umbilical cord abnormalities). Severe foetal growth restriction (<5(th) percentile) was observed in 29.2%; 44.9% (22/49) of them died at the age of ≥36+0 weeks of gestation." Germany Statistics
Conditions Associated with Stillbirth
Based upon the 2007 National Institute of Child Health and Human Development workshop. [15]
Infection
- Severe maternal illness
- Placental infection leading to hypoxemia
- Fetal infection leading to congenital deformity
- Fetal infection leading damage of a vital organ
- Precipitating preterm labor with the fetus dying in labor
Maternal medical conditions
- Hypertensive disorders
- Diabetes mellitus
- Thyroid disease
- Renal disease
- Liver disease
- Connective tissue disease (systemic lupus erythematosus)
- Cholestasis
Other
- Antiphospholipid syndrome
- Heritable thrombophilias
- Red cell alloimmunization
- Platelet alloimmunization
- Congenital anomaly and malformations
- Chromosomal abnormalities including confined placental mosaicism
- Fetomaternal hemorrhage
- Fetal growth restriction
- Placental abnormalities including vasa previa and placental abruption
- Umbilical cord pathology including velamentous insertion, prolapse, occlusion and entanglement
- Multifetal gestation including twin–twin transfusion syndrome and twin reverse arterial perfusion
- Amniotic band sequence
- Central nervous system lesions
References
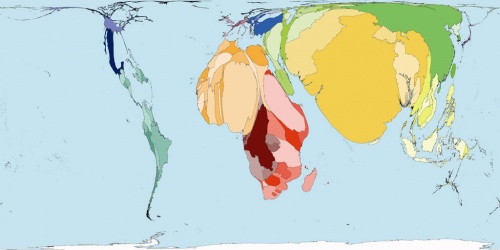
- ↑ Dorling D. (2007). Worldmapper: the human anatomy of a small planet. PLoS Med. , 4, e1. PMID: 17411312 DOI.
- ↑ AIHW: Hilder L, Li Z, Zeki R & Sullivan EA 2014. Stillbirths in Australia 1991-2009. Perinatal statistics series no. 29. Cat. no. PER 63. Canberra: AIHW.
- ↑ Australian Institute of Health and Welfare 2020. Stillbirths and neonatal deaths in Australia . Cat. no. PER 107. Canberra: AIHW. Viewed 28 July 2020, https://www.aihw.gov.au/reports/mothers-babies/stillbirths-and-neonatal-deaths-in-australia
- ↑ 4.0 4.1 Australian Institute of Health and Welfare 2019. Stillbirths and neonatal deaths in Australia 2015 and 2016: in brief. Perinatal statistics series no. 36. Cat. no. PER 102. Canberra: AIHW. PDF
- ↑ 5.0 5.1 Australian Institute of Health and Welfare 2018. Perinatal deaths in Australia: 2013–2014. Cat. no. PER 94. Canberra: AIHW.
- ↑ Wojcieszek AM, Shepherd E, Middleton P, Gardener G, Ellwood DA, McClure EM, Gold KJ, Khong TY, Silver RM, Erwich JJH & Flenady V. (2018). Interventions for investigating and identifying the causes of stillbirth. Cochrane Database Syst Rev , 4, CD012504. PMID: 29709055 DOI.
- ↑ Malacova E, Regan A, Nassar N, Raynes-Greenow C, Leonard H, Srinivasjois R, W Shand A, Lavin T & Pereira G. (2018). Risk of stillbirth, preterm delivery, and fetal growth restriction following exposure in a previous birth: systematic review and meta-analysis. BJOG , 125, 183-192. PMID: 28856792 DOI.
- ↑ Pinar MH, Gibbins K, He M, Kostadinov S & Silver R. (2018). Early Pregnancy Losses: Review of Nomenclature, Histopathology, and Possible Etiologies. Fetal Pediatr Pathol , , 1-19. PMID: 29737906 DOI.
- ↑ 9.0 9.1 Hübner J, Gast AS, Müller AM, Bartmann P & Gembruch U. (2015). [Stillbirths in Germany: Retrospective Analysis of 168 Cases between 2003 and 2011]. Z Geburtshilfe Neonatol , 219, 73-80. PMID: 25901868 DOI.
- ↑ Sullivan EA, Wang YA, Norman RJ, Chambers GM, Chughtai AA & Farquhar CM. (2013). Perinatal mortality following assisted reproductive technology treatment in Australia and New Zealand, a public health approach for international reporting of perinatal mortality. BMC Pregnancy Childbirth , 13, 177. PMID: 24044524 DOI.
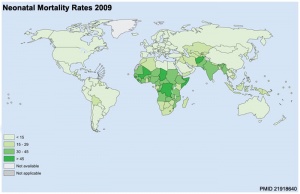
- ↑ Oestergaard MZ, Inoue M, Yoshida S, Mahanani WR, Gore FM, Cousens S, Lawn JE & Mathers CD. (2011). Neonatal mortality levels for 193 countries in 2009 with trends since 1990: a systematic analysis of progress, projections, and priorities. PLoS Med. , 8, e1001080. PMID: 21918640 DOI.
- ↑ Syed M, Javed H, Yakoob MY & Bhutta ZA. (2011). Effect of screening and management of diabetes during pregnancy on stillbirths. BMC Public Health , 11 Suppl 3, S2. PMID: 21501437 DOI.
- ↑ Pasupathy D, Wood AM, Pell JP, Fleming M & Smith GC. (2010). Time of birth and risk of neonatal death at term: retrospective cohort study. BMJ , 341, c3498. PMID: 20634347
- ↑ Luo ZC & Karlberg J. (2001). Timing of birth and infant and early neonatal mortality in Sweden 1973-95: longitudinal birth register study. BMJ , 323, 1327-30. PMID: 11739216
- ↑ 15.0 15.1 Reddy UM, Goldenberg R, Silver R, Smith GC, Pauli RM, Wapner RJ, Gardosi J, Pinar H, Grafe M, Kupferminc M, Hulthén Varli I, Erwich JJ, Fretts RC & Willinger M. (2009). Stillbirth classification--developing an international consensus for research: executive summary of a National Institute of Child Health and Human Development workshop. Obstet Gynecol , 114, 901-14. PMID: 19888051 DOI.
- ↑ Perinatal and Maternal Mortality Review Committee (PMMRC). 2013. Seventh Annual Report of the Perinatal and Maternal Mortality Review Committee: Reporting mortality 2011. Wellington: Health Quality & Safety Commission
- ↑ Public Health Agency of Canada (PHAC). 2008. Canadian Perinatal Health Report, 2008 Edition. Ottawa.
- ↑ Kowaleski J. 1997. State definitions and reporting requirements for live births, fetal deaths, and induced terminations of pregnancy (1997 revision). Hyattsville, Maryland: National Center for Health Statistics.
- ↑ Winje BA, Røislien J, Saastad E, Eide J, Riley CF, Stray-Pedersen B & Frøen JF. (2013). Wavelet principal component analysis of fetal movement counting data preceding hospital examinations due to decreased fetal movement: a prospective cohort study. BMC Pregnancy Childbirth , 13, 172. PMID: 24007565 DOI.
- ↑ Winje BA, Roald B, Kristensen NP & Frøen JF. (2012). Placental pathology in pregnancies with maternally perceived decreased fetal movement--a population-based nested case-cohort study. PLoS ONE , 7, e39259. PMID: 22723978 DOI.
- ↑ 21.0 21.1 Heron M. (2018). Deaths: Leading Causes for 2016. Natl Vital Stat Rep , 67, 1-77. PMID: 30248017
- ↑ Heron M. (2017). Deaths: Leading Causes for 2015. Natl Vital Stat Rep , 66, 1-76. PMID: 29235984
- ↑ Heron M & Tejada-Vera B. (2009). Deaths: leading causes for 2005. Natl Vital Stat Rep , 58, 1-97. PMID: 20361522
Reviews
Paternoster M, Perrino M, Travaglino A, Raffone A, Saccone G, Zullo F, D'Armiento FP, Buccelli C, Niola M & D'Armiento M. (2019). Parameters for estimating the time of death at perinatal autopsy of stillborn fetuses: a systematic review. Int. J. Legal Med. , 133, 483-489. PMID: 30617766 DOI.
Martinez-Portilla RJ, Pauta M, Hawkins-Villarreal A, Rial-Crestelo M, Paz Y Miño F, Madrigal I, Figueras F & Borrell A. (2018). Added value of chromosomal microarray analysis above conventional karyotyping in stillbirth work-up: a systematic review and meta-analysis. Ultrasound Obstet Gynecol , , . PMID: 30549343 DOI.
Articles
Baschieri A, Gordeev VS, Akuze J, Kwesiga D, Blencowe H, Cousens S, Waiswa P, Fisker AB, Thysen SM, Rodrigues A, Biks GA, Abebe SM, Gelaye KA, Mengistu MY, Geremew BM, Delele TG, Tesega AK, Yitayew TA, Kasasa S, Galiwango E, Natukwatsa D, Kajungu D, Enuameh YA, Nettey OE, Dzabeng F, Amenga-Etego S, Newton SK, Manu AA, Tawiah C, Asante KP, Owusu-Agyei S, Alam N, Haider MM, Alam SS, Arnold F, Byass P, Croft TN, Herbst K, Kishor S, Serbanescu F & Lawn JE. (2019). "Every Newborn-INDEPTH" (EN-INDEPTH) study protocol for a randomised comparison of household survey modules for measuring stillbirths and neonatal deaths in five Health and Demographic Surveillance sites. J Glob Health , 9, 010901. PMID: 30820319 DOI.
Goldenberg RL, Muhe L, Saleem S, Dhaded S, Goudar SS, Patterson J, Nigussie A & McClure EM. (2019). Criteria for assigning cause of death for stillbirths and neonatal deaths in research studies in low-middle income countries. J. Matern. Fetal. Neonatal. Med. , 32, 1915-1923. PMID: 30134756 DOI.
Giang HTN, Bechtold-Dalla Pozza S, Tran HT & Ulrich S. (2019). Stillbirth and preterm birth and associated factors in one of the largest cities in central Vietnam. Acta Paediatr. , 108, 630-636. PMID: 30098081 DOI.
Bukowski R, Hansen NI, Pinar H, Willinger M, Reddy UM, Parker CB, Silver RM, Dudley DJ, Stoll BJ, Saade GR, Koch MA, Hogue C, Varner MW, Conway DL, Coustan D & Goldenberg RL. (2017). Altered fetal growth, placental abnormalities, and stillbirth. PLoS ONE , 12, e0182874. PMID: 28820889 DOI.
Pinar H, Koch MA, Hawkins H, Heim-Hall J, Shehata B, Thorsten VR, Carpenter M, Lowichik A & Reddy UM. (2011). The Stillbirth Collaborative Research Network (SCRN) placental and umbilical cord examination protocol. Am J Perinatol , 28, 781-92. PMID: 21717387 DOI.
Search PubMed
July 2010 "Perinatal Death" All (8144) Review (899) Free Full Text (1129)
Search Pubmed: Stillbirth | Perinatal Death
NCBI - Policies and Guidelines | PubMed | Help:Reference Tutorial
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- Stillbirth Foundation Australia
- New York Times Breaking the Silence of Stillbirth 10 Feb 2013
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2026, April 17) Embryology Birth - Stillbirth and Perinatal Death. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Birth_-_Stillbirth_and_Perinatal_Death
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G