Abnormal Development - Hydatidiform Mole
| Embryology - 20 May 2026 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
| ICD-11 |
|---|
|
JA02.0 Complete hydatidiform mole | JA02.1 Incomplete or partial hydatidiform mole |
Introduction
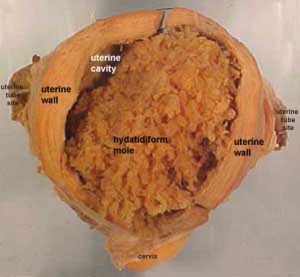
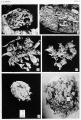
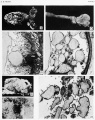
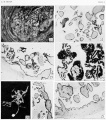
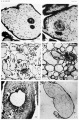
(hydatidiform mole, hydatid mole, molar pregnancy, gestational trophoblastic disease) A type of fertilisation abnormality, when only the conceptus trophoblast layers proliferates and not the embryoblast, no embryo develops, this is called a "hydatidiform mole". Due to the continuing presence of the trophoblastic layer, this abnormal conceptus can also implant in the uterus or ectopically. The trophoblast cells will secrete human chorionic gonadotropin (hCG), as in a normal pregnancy, and may appear maternally and by pregnancy test to be "normal". Prenatal diagnosis by ultrasound analysis demonstrates the absence of a embryo.
- Complete Mole - Only paternal chromosomes.
- Partial Mole - 3 sets of chromosomes ( (triploidy) instead of the usual 2.
There are several forms of hydatidiform mole: partial mole, complete mole and persistent gestational trophoblastic tumor. Many of these tumours arise from a haploid sperm fertilizing an egg without a female pronucleus (the alternative form, an embryo without sperm contribution, is called parthenogenesis). The tumour has a "grape-like" placental appearance without enclosed embryo formation. Following a first molar pregnancy, there is approximately a 1% risk of a second molar pregnancy.
- The incidence of hydatidiform mole varies between ethnic groups, and typically occurs in 1 in every 1500 pregnancies.
- All hydatidiform mole cases are sporadic, except for extremely rare familial cases.
- A maternal gene has been identified for recurrent hydatidiform mole (chromosome 19q13.3-13.4 in a 15.2 cM interval flanked by D19S924 and D19S890).[1]
| Historically | |
|---|---|
| 100px|link=Embryology History - William Smellie
William Smellie |
Hippocrates (c.400 bc) first described a molar pregnancy.
Rembrandt's painting "The Anatomy Lesson of Dr Nicolaes Tulp" (1632), also illustrated a molar pregnancy. William Smellie (1697-1763) in 1752 was the first to introduce the terminology "mole" and "hydatidiform". |
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Hydatidiform Mole | complete hydatidiform molepartial hydatidiform mole | trophoblastic disease |
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
|
International Classification of Diseases
| ICD-11 |
|---|
|
JA02.0 Complete hydatidiform mole - A condition caused by the over-production of cells arising into the placenta during pregnancy. This condition is characterized by a pregnancy with abnormal placental growth in which the chorionic villi become hydropic, slight to severe trophoblast proliferation and invasion of the uterine tissue within 10-16 weeks after conception, a placental mass, 25-30% theca lutein cysts, 15-20% persistent trophoblastic disease, 50% uterine size for dates, and vaginal bleeding, nausea, or vomiting. This condition leads to an absent fetus. JA02.1 Incomplete or partial hydatidiform mole - A condition caused by the over-production of cells arising into the placenta during pregnancy. This condition is characterized by a pregnancy with abnormal placental growth in which the chorionic villi become hydropic, slight to moderate trophoblast proliferation and invasion of the uterine tissue within 10-16 weeks after conception, a placental mass, theca lutein cysts, 1-5% persistent trophoblastic disease, small uterine size for dates, and vaginal bleeding, nausea, or vomiting. This condition leads to some fetal development and a missed abortion. Gestational trophoblastic diseases - A group of conditions characterized as rare, pregnancy-related tumours that appear when cells in the uterus start to grow out of control. The cells that form gestational trophoblastic tumours are called trophoblasts and come from tissue that grows to form the placenta during pregnancy. |
Mole Types
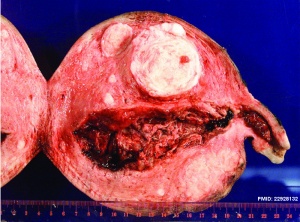
Complete Mole
Only paternal chromosomes.
- Chromosomal genetic material from the ovum (egg) is lost, by an unknown process.
- Fertilization then occurs with one or two sperm and an androgenic (from the male only) conceptus (fertilized egg) is formed.
- With this conceptus the embryo (fetus, baby) does not develop at all but the placenta does grow.
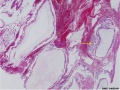
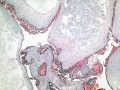
- placenta it is abnormal and forms lots of cysts and has no blood vessels.
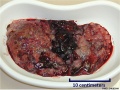
- These cysts look like a cluster of grapes and that is why it is called a hydatidiform ("grape-like") mole.
- A hydatidiform mole miscarries by about 16 to 18 weeks gestational age.
- Since the diagnosis can be made by ultrasound before that time, it is better to have an evacuation of the uterus (D & C) so that there is no undue bleeding and no infection.
- Human chorionic gonadotropin (hCG) levels will assist in making the diagnosis.
Partial Mole
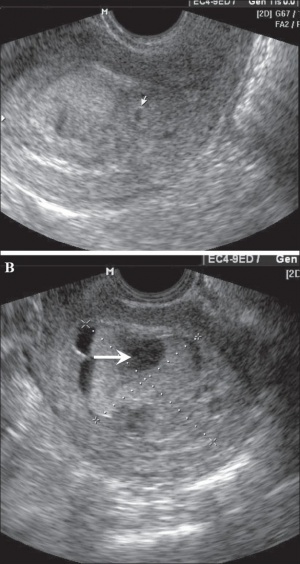
Three sets of chromosomes instead of the usual two and this is called triploidy.
- chromosomal (genetic) material from the ovum (egg) is retained and the egg is fertilized by one or two sperm.
- with partial mole there are maternal chromosomes and there is a fetus.
- the three sets of chromosomes means the fetus is always grossly abnormal and will not survive.
(Text modified from: International Society for the Study of Trophoblastic Diseases, see also JRM Gestational Trophoblastic Disease)
Diagnostic
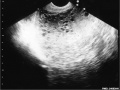
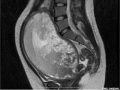
- Ultrasound can indicate the absence of an embryonic heartbeat and a "bunch of grapes" appearance.
- HCG level (>100000 mIU/ml)
- Excessive uterine enlargement
- Theca lutein cyst size ≥6 cm are considered a high risk for developing post molar tumors
A recent retrospective study of a large patient cohort[11] identified clinical characteristics (table below) between the complete and partial hydatidiform moles types. After mole evacuation most patients in both groups reach normal serum hCG concentrations within 14 weeks.
| Mole Type | Average serum hCG | Post hCG normalization | Gestational age |
|---|---|---|---|
| complete | 4400 ng/mL | 7 weeks | 11.5 weeks |
| partial | 875 ng/mL | 6 weeks | 13.0 weeks |
Tumour Growth
Like any tumour, unless removed there is a risk of progression:
- Stage I: Tumor confined to uterus (non-metastatic)
- Stage II: Tumor involving pelvic organs and/or vagina
- Stage III: Tumor involving lungs, with or without involving pelvic structures and/or vagina
- Stage IV: Tumor involving distant organs
| Uterine and ovarian metastasis[12] | Pulmonary metastasis[12] |
|---|---|
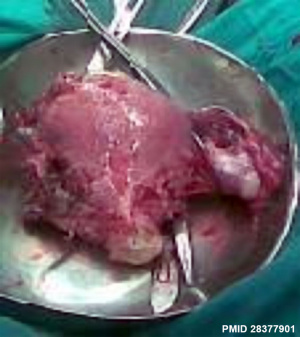
|
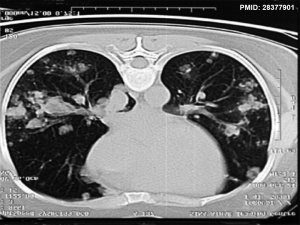
|
Choriocarcinoma
A highly malignant epithelial tumour often associated with hydatidiform mole.
Placental Mesenchymal Dysplasia
A rare disorder due to a similar "grape-like" placental appearance, this rare disorder has been mistaken both clinically and macroscopically for a partial hydatidiform molar pregnancy. Characterized by an increased size placenta with cystic villi and dilated vessels. This disorder also has a high incidence of intrauterine growth restriction (IUGR) and fetal death.
Twin Pregnancy Mole
Hydatidiform mole and co-existent healthy fetus is a very rare condition with only 30 cases documented in detail in the literature.[13]
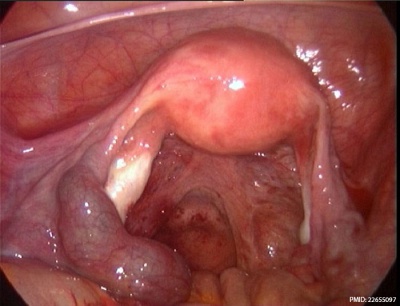
Ectopic Molar Pregnancy
Left-sided unruptured ampullary ectopic pregnancy at laparoscopy.[14]
- Links: Ectopic Implantation
References
- ↑ Moglabey YB, Kircheisen R, Seoud M, El Mogharbel N, Van den Veyver I & Slim R. (1999). Genetic mapping of a maternal locus responsible for familial hydatidiform moles. Hum. Mol. Genet. , 8, 667-71. PMID: 10072436
- ↑ Nguyen NMP, Ge ZJ, Reddy R, Fahiminiya S, Sauthier P, Bagga R, Sahin FI, Mahadevan S, Osmond M, Breguet M, Rahimi K, Lapensee L, Hovanes K, Srinivasan R, Van den Veyver IB, Sahoo T, Ao A, Majewski J, Taketo T & Slim R. (2018). Causative Mutations and Mechanism of Androgenetic Hydatidiform Moles. Am. J. Hum. Genet. , 103, 740-751. PMID: 30388401 DOI.
- ↑ Nguyen NMP, Khawajkie Y, Mechtouf N, Rezaei M, Breguet M, Kurvinen E, Jagadeesh S, Solmaz AE, Aguinaga M, Hemida R, Harma MI, Rittore C, Rahimi K, Arseneau J, Hovanes K, Clisham R, Lenzi T, Scurry B, Addor MC, Bagga R, Nendaz GG, Finci V, Poke G, Grimes L, Gregersen N, York K, Bolze PA, Patel C, Mozdarani H, Puechberty J, Scotchie J, Fardaei M, Harma M, Gardner RJM, Sahoo T, Dudding-Byth T, Srinivasan R, Sauthier P & Slim R. (2018). The genetics of recurrent hydatidiform moles: new insights and lessons from a comprehensive analysis of 113 patients. Mod. Pathol. , 31, 1116-1130. PMID: 29463882 DOI.
- ↑ Chan KK, Wong ES, Wong OG, Ngan HY & Cheung AN. (2018). Identification of nonsynonymous TP53 mutations in hydatidiform moles. Mutat. Res. , 809, 20-23. PMID: 29655027 DOI.
- ↑ Shaaban AM, Rezvani M, Haroun RR, Kennedy AM, Elsayes KM, Olpin JD, Salama ME, Foster BR & Menias CO. (2017). Gestational Trophoblastic Disease: Clinical and Imaging Features. Radiographics , 37, 681-700. PMID: 28287945 DOI.
- ↑ Eagles N, Sebire NJ, Short D, Savage PM, Seckl MJ & Fisher RA. (2015). Risk of recurrent molar pregnancies following complete and partial hydatidiform moles. Hum. Reprod. , 30, 2055-63. PMID: 26202916 DOI.
- ↑ Singer H, Biswas A, Nuesgen N, Oldenburg J & El-Maarri O. (2015). NLRP7, Involved in Hydatidiform Molar Pregnancy (HYDM1), Interacts with the Transcriptional Repressor ZBTB16. PLoS ONE , 10, e0130416. PMID: 26121690 DOI.
- ↑ Cole LA. (2012). Minimally-aggressive gestational trophoblastic neoplasms. Gynecol. Oncol. , 125, 145-50. PMID: 22198244 DOI.
- ↑ Aguilera M, Rauk P, Ghebre R & Ramin K. (2012). Complete hydatidiform mole presenting as a placenta accreta in a twin pregnancy with a coexisting normal fetus: case report. Case Rep Obstet Gynecol , 2012, 405085. PMID: 22928132 DOI.
- ↑ Kinare A. (2008). Fetal environment. Indian J Radiol Imaging , 18, 326-44. PMID: 19774194 DOI.
- ↑ Eysbouts Y, Brouwer R, Ottevanger P, Massuger L, Sweep F, Thomas C & van Herwaarden A. (2017). Serum Human Chorionic Gonadotropin Normogram for the Detection of Gestational Trophoblastic Neoplasia. Int. J. Gynecol. Cancer , 27, 1035-1041. PMID: 28498241 DOI.
- ↑ 12.0 12.1 Aminimoghaddam S & Maghsoudnia A. (2017). Unusual Presentation of Invasive Mole: A Case Report. J Reprod Infertil , 18, 205-209. PMID: 28377901
- ↑ Piura B, Rabinovich A, Hershkovitz R, Maor E & Mazor M. (2008). Twin pregnancy with a complete hydatidiform mole and surviving co-existent fetus. Arch. Gynecol. Obstet. , 278, 377-82. PMID: 18273627 DOI.
- ↑ Bousfiha N, Erarhay S, Louba A, Saadi H, Bouchikhi C, Banani A, El Fatemi H, Sekkal M & Laamarti A. (2012). Ectopic molar pregnancy: a case report. Pan Afr Med J , 11, 63. PMID: 22655097
Reviews
Kalogiannidis I, Kalinderi K, Kalinderis M, Miliaras D, Tarlatzis B & Athanasiadis A. (2018). Recurrent complete hydatidiform mole: where we are, is there a safe gestational horizon? Opinion and mini-review. J. Assist. Reprod. Genet. , 35, 967-973. PMID: 29737470 DOI.
Hui P, Buza N, Murphy KM & Ronnett BM. (2017). Hydatidiform Moles: Genetic Basis and Precision Diagnosis. Annu Rev Pathol , 12, 449-485. PMID: 28135560 DOI.
Candelier JJ. (2016). The hydatidiform mole. Cell Adh Migr , 10, 226-35. PMID: 26421650 DOI.
Kani KK, Lee JH, Dighe M, Moshiri M, Kolokythas O & Dubinsky T. (2012). Gestatational trophoblastic disease: multimodality imaging assessment with special emphasis on spectrum of abnormalities and value of imaging in staging and management of disease. Curr Probl Diagn Radiol , 41, 1-10. PMID: 22085657 DOI.
Ronnett BM, DeScipio C & Murphy KM. (2011). Hydatidiform moles: ancillary techniques to refine diagnosis. Int. J. Gynecol. Pathol. , 30, 101-16. PMID: 21293291 DOI.
Sharp AN, Heazell AE, Crocker IP & Mor G. (2010). Placental apoptosis in health and disease. Am. J. Reprod. Immunol. , 64, 159-69. PMID: 20367628 DOI.
Seckl MJ, Sebire NJ & Berkowitz RS. (2010). Gestational trophoblastic disease. Lancet , 376, 717-29. PMID: 20673583 DOI.
Articles
Kan ASY, Lau ETK, So CH, Chan WP, Wong WC, Lee KC, Pertile MD & Tang MHY. (2018). A fetus coexisting with a complete hydatidiform mole with trisomy 9 of maternal origin. J. Obstet. Gynaecol. Res. , 44, 955-959. PMID: 29436108 DOI.
Hong T, Hills E & Aguinaga MDP. (2017). Radiographically occult pulmonary metastases from gestational trophoblastic neoplasia. Radiol Case Rep , 12, 292-294. PMID: 28491173 DOI.
Jauniaux E & Verheijen R. (2016). Diagnosis and management of hydatidiform mole and its complications: 2000 years of a medical challenge. BJOG , 123, 1183. PMID: 27206034 DOI.
Cavaliere A, Ermito S, Dinatale A & Pedata R. (2009). Management of molar pregnancy. J Prenat Med , 3, 15-7. PMID: 22439034
OMIM
Search PubMed
Search PubMed Now: Hydatidiform Mole
Additional Images
Historic Images
| Historic Disclaimer - information about historic embryology pages |
|---|
| Pages where the terms "Historic" (textbooks, papers, people, recommendations) appear on this site, and sections within pages where this disclaimer appears, indicate that the content and scientific understanding are specific to the time of publication. This means that while some scientific descriptions are still accurate, the terminology and interpretation of the developmental mechanisms reflect the understanding at the time of original publication and those of the preceding periods, these terms, interpretations and recommendations may not reflect our current scientific understanding. (More? Embryology History | Historic Embryology Papers) |
Mall FP. On the frequency of localized anomalies in human embryos and infants at birth. (1917) Amer. J Anat. 22:49-72.
Meyer AW. Hydatiform degeneration in tubal and uterine pregnancy. (1920) Carnegie Instn. Wash. Publ., Contrib. Embryol., 40: 327- 364.
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- PubMed Health Hydatidiform mole
- International Society for the Study of Trophoblastic Diseases
- Sydney Gynaecological Oncology Group Gestational Trophoblastic Disease
- The Journal of Reproductive Medicine Gestational Trophoblastic Disease (1998)
- Dana-Farber Cancer Institute Gynecologic Oncology Program
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2026, Mayıs 20) Embryology Abnormal Development - Hydatidiform Mole. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Abnormal_Development_-_Hydatidiform_Mole
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G