2009 Lecture 10
Respiratory Development
Introduction
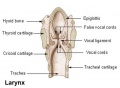
The respiratory system does not carry out its physiological function (of gas exchange) until after birth. The respiratory tract, diaphragm and lungs do form early in embryonic development. The respiratory tract is divided anatomically into 2 main parts: 1. upper respiratory tract, consisting of the nose, nasal cavity and the pharynx; 2. lower respiratory tract consisting of the larynx, trachea, bronchi and the lungs.
The respiratory "system" usually includes descriptions of not only the functional development of the lungs, but also related musculoskeletal (diaphragm) and vascular (pulmonary) development.
- iLecture Audio Lecture Date: 25-08-2009 Lecture Time: 12:00 Venue: BioMed E Speaker: Mark Hill Respiration
- 2010 Lecture - Respiration Development | Science 2010
Lecture Objectives
- Understanding of embryonic lung development
- Understanding of 4 stages of lung development
- Understanding of diaphragm development
- Brief understanding of respiratory vascular development
- Brief understanding of respiratory abnormalities
- Brief understanding of molecular mechanisms
Textbook References
- Human Embryology Larson Chapter 9 p229-260
- The Developing Human: Clinically Oriented Embryology (6th ed.) Moore and Persaud Chapter 12 p271-302
Additional Textbooks
- Before We Are Born (5th ed.) Moore and Persaud Chapter 13 p255-287
- Essentials of Human Embryology Larson Chapter 9 p123-146
- Human Embryology Fitzgerald and Fitzgerald Chapter 19,20 p119-123
- Anatomy of the Human Body 1918 Henry Gray 1. The Respiratory Apparatus
Developmental Overview
Week 4 - laryngotracheal groove forms on floor foregut.
Week 5 - left and right lung buds push into the pericardioperitoneal canals (primordia of pleural cavity)
Week 6 - descent of heart and lungs into thorax. Pleuroperitoneal foramen closes.
Week 7 - enlargement of liver stops descent of heart and lungs.
Month 3-6 - lungs appear glandular, end month 6 alveolar cells type 2 appear and begin to secrete surfactant.
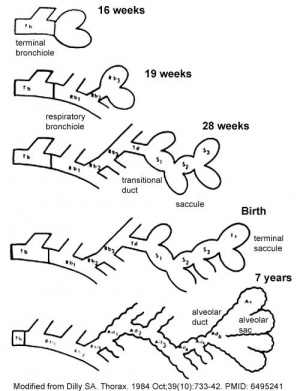
Month 7 - respiratory bronchioles proliferate and end in alveolar ducts and sacs.
Lung Development
- week 4 - 5 embryonic
- week 5 - 17 pseudoglandular
- week 16 - 25 canalicular
- week 24 - 40 terminal sac
- late fetal - 8 years alveolar
Germ Layers
Endoderm and splanchnic mesoderm form majority of conducting and alveoli. Ectoderm will contribute the neural innervation. (this does not cover the origins of the supporting musculoskeletal components)
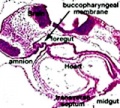
Foregut development
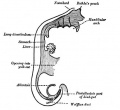
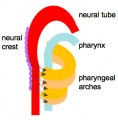
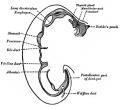
From the oral cavity the next portion of the foregut is initially a single gastrointestinal (oesophagus) and respiratory (trachea) common tube, the pharynx which lies behind the heart. Note that the respiratory tract will form from a ventral bud arising at this level.
- Oral cavity
- Pharynx (esophagus, trachea)
- Respiratory tract
- Stomach
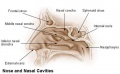
Upper respiratory tract
- part of foregut development
- anatomically the nose, nasal cavity and the pharynx
- the pharynx forms a major arched cavity within the pharyngeal arches
MH - pharyngeal arches will be described in head development lecture
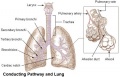
Lower respiratory tract
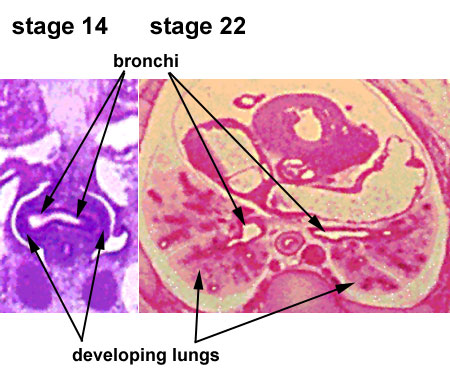
- The lungs go through an embryonic and 4 distinct histological phases of development
Growth initially of branched "conducting" system of bronchial tree, followed by later development of the "functional units" of the alveoli.
- embryonic - week 4 - 5 (stage 14 above)
- pseudoglandular - week 5 - 17 (stage 22 above)
- canalicular - week 16 - 25
- terminal sac - week 24 - 40
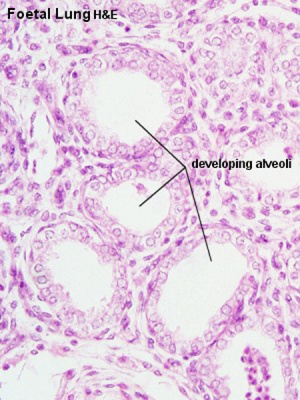
- alveolar - late fetal - 8 years (Latin, alveus = cavity or hollow)
- in late fetal development respiratory motions and amniotic fluid are thought to have a role in lung maturation.
- Development of this system is not completed until late fetal just before birth.
- Therefore premature babies have difficulties associated with insufficient surfactant (end month 6 alveolar cells type 2 appear and begin to secrete surfactant).
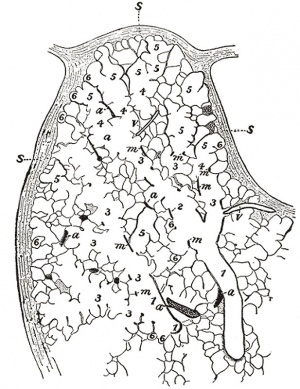
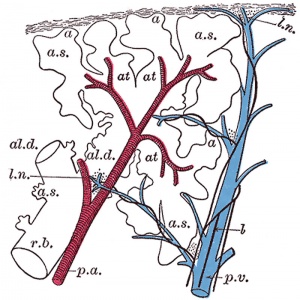
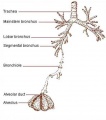
Lung morphogenesis
- lung buds ( endoderm epithelial tubes) grow/push into mesenchyme covered with pleural cells (lung border)
- generates a tree-like network by repeated:
- elongation
- terminal bifurcation
- lateral budding
Fetal lung volume
Each lung volume as determined by ultrasound and matched to gestational age (PMID: 16388511)
- 12-13 weeks 0.05 mL
- 19-22 weeks 0.5 mL
- 29-32 weeks 1.9 mL
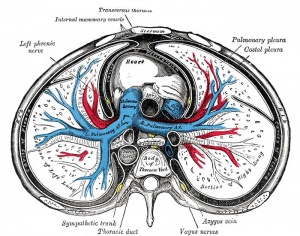
Pleural Cavity
- The anatomical body cavity in which the lungs develop and lie.
- The pleural cavity forms in the lateral plate mesoderm as part of the early single intraembryonic coelom.
- This cavity is initially continuous with pericardial and peritoneal cavities and form initially as two narrow canals
- later becomes separated by folding (pleuropericardial fold, pleuroperitoneal membrane) and the later formation of the diaphragm
pleuropericardial fold - (pleuropericardial membrane) An early embryonic fold which restricts the communication between pleural cavity and pericardiac cavity, contains both the cardinal vein and phrenic nerve.
pleuroperitoneal membrane - An early embryonic membrane that forms inferiorly at the septum transversum to separate peritoneal cavity from pleural cavity.
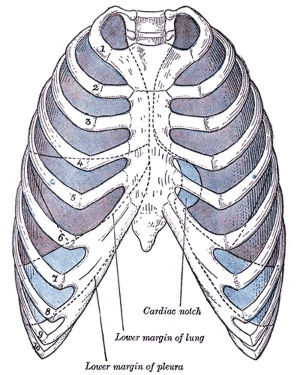
Pleura
- serous membrane covers the surface of the lung and the spaces between the lobes
- arranged as a closed invaginated sac
- two layers (pulmonary, parietal) continuous with each other, the potential space between them is the pleural cavity
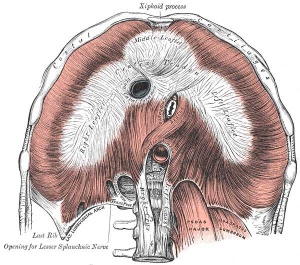
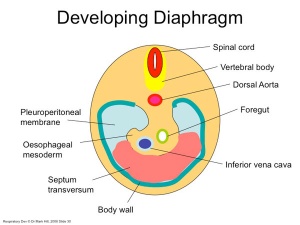
Diaphragm
Not respiratory tract but musculoskeletal development, there are 5 elements that contribute to the diaphragm
- septum transversum- central tendon
- 3rd to 5th somite- musculature of diaphragm
- ventral pleural sac- connective tissue
- mesentry of oesophagus- connective tissue around oesophasus and IVC
- pleuroperitoneal membranes- connective tissue around central tendon
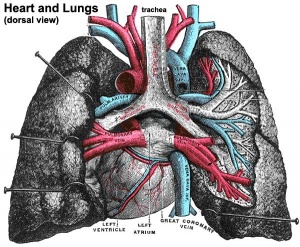
Pulmonary Circulation
- the pulmonary system not "functional" until after birth
- pulmonary arteries - 6th aortic arch arteries
- pulmonary veins - are incorporated into the left atrium wall
- bronchial arteries - branches from dorsal aorta
The First Breath
- The respiratory system does not carry out its physiological function (gas exchange) prenatally and remain entirely fluid-filled until birth.
- At birth, fluid in the upper respiratory tract is expired and fluid in the lung aveoli is rapidly absorbed this event has also been called "dewatering of the lung".
- The lung epithelia has to now rapidly change from its prenatal secretory function to that of fluid absorbtion.
The exchange of lung fluid for air leads to:
- fall in pulmonary vascular resistance
- increase in pulmonary blood flow
- thinning of pulmonary arteries (stretching as lungs increase in size)
- blood fills the alveolar capillaries
In the heart, pressure in the right side of the heart decreases and pressure in the left side of the heart increases (more blood returning from pulmonary).
Respiratory Tract Abnormalities
Tracheoesophageal Fistula
(Tracheo-Oesophageal Fistula, Oesophageal Atresia) - Oesophageal Atresia with or without tracheo-oesophageal fistula
Lobar Emphysema (Overinflated Lung)
- There is an overinflated left upper lobe
- There is a collapsed lower lobe
- The left lung is herniating across the mediastinum
Congenital Diaphragmatic Hernia
Failure of the pleuroperitoneal foramen (foramen of Bochdalek) to close allows viscera into thorax. Intestine, stomach or spleen can enter the pleural cavity, compressing the lung.
Azygos Lobe
Common condition (0.5% of population). The right lung upper lobe expands either side of the posterior cardinal. There is also some course variability of the phrenic nerve in the presence of an azygos lobe.
Congenital Laryngeal Webs
Laryngeal abnormality due to embryonic (week 10) incomplete recanalization of the laryngotracheal tube during the fetal period. Rare abnormality occuring mainly at the level of the vocal folds (glottis).
Meconium Aspiration Syndrome
(MAS) Meconium is the gastrointestinal contents that accumulate in the intestines during the fetal period. Fetal stress in the third trimester, prior to/at/ or during parturition can lead to premature meconium discharge into the amniotic fluid and sunsequent ingestion by the fetus and damage to respiratory function. Damage to placental vessels meconium myonecrosis may also occur.
Newborn Respiratory Distress Syndrome
(Hyaline Membrane Disease) medline plus | eMedicine
Bronchopulmonary Dysplasia
A chronic lung disease which can occur following premature birth. The definition of bronchopulmonary dysplasia (BPD) has in recent years changed from a severe lung injury and associated repair, to more of a disruption of lung development.
Take the Quiz
UNSW Embryology Links
- Lecture 10 2008
- Respiratory Tract Notes Introduction
- Movie links Endoderm
- System Notes
- Development Timeline
Links
- Embryo Images by Drs. Kathleen K. Sulik and Peter R. Bream Jr. notes/images sections on respiratory development
- Anatomy of the Human Body 1918 Henry Gray 1. The Respiratory Apparatus
Terms
alveolar - (Latin, alveus = cavity or hollow) Term used in relation to the alveoli of the lungs. The final functional sac of the respiratory tree where gas exchange occurs between the alveolar space and the pulmonary capillaries.
alveolar stage - (Latin, alveus = cavity or hollow) Term used to describe the final histological/developmental stage (Pseudoglandular, Fetal Canalicular, Terminal sac, Alveolar) of lung development. This stage occurs from late fetal/neonate. The final functional sac of the respiratory tree exists, where gas exchange occurs between the alveolar space and the pulmonary capillaries.
alveolar duct - respiratory tract that in the adult has alveoli opening into it and has no cuboidal epithelium.
alveoli - (Latin, alveus = cavity or hollow) The final functional sac of the respiratory tree where gas exchange occurs between the alveolar space and the pulmonary capillaries.
amnion - An extraembryonic membrane]ectoderm and extraembryonic mesoderm in origin and forms the innermost fetal membrane, produces amniotic fluid. This fluid-filled sac initially lies above the trilaminar embryonic disc and with embryoic disc folding this sac is drawn ventrally to enclose (cover) the entire embryo, then fetus. The presence of this membane led to the description of reptiles, bird, and mammals as amniotes.
amniotic fluid - The fluid that fills amniotic cavity totally encloses and cushions the embryo. Amniotic fluid enters both the gastrointestinal and respiratory tract following rupture of the buccopharyngeal membrane. The late fetus swallows amniotic fluid.
atmospheric pressure - Term describing the pressure of the air outside of the body.
atresia - (Greek, a = without + tresis = perforation) Term used for anatomical closing or absence of a cavity or opening that should exist. Used as an antomical, pathological and clinical term: esophageal atresia, biliary atresia, duodenal atresia, jejunal atresia, choanal atresia, urethral atresia, bronchial atresia.
buccal - (Latin, bucca = cheek) A term used to relate to the mouth (oral cavity).
buccopharyngeal membrane - (oral membrane) (Latin, bucca = cheek) A membrane which forms the external upper membrane limit (cranial end) of the early gastrointestinal tract (GIT). This membrane develops during gastrulation by ectoderm and endoderm without a middle (intervening) layer of mesoderm. The membrane lies at the floor of the ventral depression (stomadeum) where the oral cavity will open and will breakdown to form the initial "oral opening" of the gastrointestinal tract. The equivilent membrane at the lower end of the gastrointestinal tract is the cloacal membrane.
canalicular stage - (fetal canalicular, canalicular phase) Term used to describe lung development, after early embryonic the second of the histological/developmental stages (Pseudoglandular, Fetal Canalicular, Terminal sac, Alveolar). This stage occurs during the fetal period from week 16 to 24. During this stage there is lung bud mesenchymal angiogenesis and cellular differentiation into different stromal cell types (fibroblasts, myoblasts and chondrocytes).
ciliated pseudostratified columnar epithelium - forms mucous membrane that lines the trachea and the nasal cavity and nasopharynx epithelium.
coelom - Term used to describe a space. There are extraembryonic and intraembryonic coeloms that form during vertebrate development. The single intraembryonic coelom will form the 3 major body cavities: pleural, pericardial and peritoneal.
ductus arteriosus - A vascular shunt between the pulmonary artery and descending aorta, which allows fetal right heart output (most, 88%) to go to systemic circulation. This shunt closes normally at birth.
elastic theory - The hypothesis that lung acinar development during the saccular stage is guided by the preprogrammed location of a surrounding elastic network.
epiglottis - (Greek, epi = above, upon) cartilaginous part of the larynx above the [G.htm#glottis glottis], which in infancy directs food into the esophagus and not the trachea. Embryologically develops in the foregut from the hypobranchial eminence. Postnatal anatomical development in humans involves a maturational descent in infancy (4 and 6 months of age). Contains lymphoid tissue (larynx-associated lymphoid tissue, LALT and Bronchus-associated lymphoid tissue, BALT).
expiration - (exhalation) The process of letting air out of the lungs during the breathing cycle. Due to the combination of relaxation of the diaphragm and elastic recoil of tissue decreases the thoracic volume and increases the intraalveolar pressure.
fistula - An abnormal communication between 2 structures (organs, vessels, cavities) that do not normally connect.
foregut - The first of the three part/division (foregut - midgut - hindgut) of the early forming gastrointestinal tract. The foregut runs from the buccopharyngeal membrane to the midgut and forms all the tract (esophagus and stomach) from the oral cavity to beneath the stomach. In addition, a ventral bifurcation of the foregut will also form the respiratory tract epithelium.
goblet cells - produce mucus that traps airborne particles and microorganisms, nearby ciliated cells propel the mucus upward, where it is either swallowed or expelled.
hypopharyngeal eminence - (hypobranchial eminence) An early embryonic structure in the developing head. A narrow midline mesodermal (mesenchymal) exension lying within the floor curve of the developing pharynx. Fusion of 3rd pharyngeal arches and precursor of root of tongue. Early developing thyroid cells also migrate into this structure as cords of cells. (More? [../Notes/head.htm Head Notes] | [../Notes/endocrine8.htm Endocrine Development - Thyroid])
hyaline cartilage - type of cartilage located in the tracheal wall to provide support and prevent the trachea from collapsing. Note that the tracheal wall has a region of posterior soft tissue to allow for expansion of the esophagus, which is immediately posterior to the trachea.
inspiration - (inhalation) The process of taking air into the lungs. Due to diaphragm contraction and the thoracic cavity increasing in volume. This decreases the intraalveolar pressure leading to air flows into the lungs.
intraalveolar pressure - Term describing the pressure inside the alveoli of the lungs, which changes during inspiration and expiration.
intrapleural pressure - Term describing the pressure within the pleural cavity.
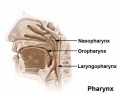
laryngopharynx - (hypopharynx) The portion of the pharynx that extends from the hyoid bone down to the lower margin of the larynx.
laryngotracheal groove - Early embryonic foregut developmental feature, forms on the anterior (ventral) wall of pharynx and gives rise to larynx, trachea, respiratory tree.
larynx - Site of the the vocal folds in the neck below the division of pharynx into the trachea and the esophagus. Embryologically develops from the foregut with the lining derived from endoderm and the cartilage from pharyngeal arch 4 and 6. Beginning as a simple foregut groove, the [#laryngotracheal_groove laryngotracheal groove] which folds to form the laryngotracheal bud, then the larynx and trachea.
lung bud - The term describing the primordia of lung development. Foregut endoderm branches into the surrounding visceral mesoderm, forming the trachea, which brances again into the bronchi and thsi process is repeated over and over again through development. Establishing the major respiratory branches first, followed by minor branches, then terminal branches, then immature alveoli which later mature to form teh functional end structures of the lung.
nasopharynx - The portion of the pharynx posterior to the nasal cavity and extends inferiorly to the uvula.
oropharynx - The portion of the pharynx that is posterior to the oral cavity.
paranasal sinuses - Air-filled cavities surrounding the nasal cavity and open into it, which combine in function to: reduce skull weight, produce mucus, and act as resonating chambers affecting voice quality. Located within in the frontal, maxilae, ethmoid, and sphenoid bones with the same name as the bones in which they are located.
parietal pleura - Forms the outer lining of pleural cavity. Mesoderm of the thoracic cavity body wall and derived from epithelia of pericardioperitoneal canals from intraembryonic coelom. The other inner pleural layer is the visceral pleura (splanchnic mesodermal in origin).
pharynx - (throat) Forms the initial segment of the upper respiratory tract divided anatomically into three regions: nasopharynx, oropharynx, and laryngopharynx (hypopharynx). Anatomically extends from the base of the skull to the level of the sixth cervical vertebra.
pleura - A double-layered serous membrane enclosing each lung. Visceral pleura layer is firmly attached to the surface of the lung. Parietal pleura layer lines the wall of the thorax. At the lung hilum, the visceral pleura is continuous with the parietal pleura. The pleural cavity between the visceral and parietal pleurae contains a thin film of serous fluid that is produced by the pleura.
pleural cavity - Anatomical body cavity in which the lungs develop and lie. The pleural cavity forms in the lateral plate mesoderm as part of the early single intraembryonic coelom. This cavity is initially continuous with pericardial and peritoneal cavities and later becomes separated by folding ([#pleuropericardial_fold pleuropericardial fold], [#pleuroperitoneal_membrane pleuroperitoneal membrane]) and the later formation of the diaphragm. The pleural cavities form initially as two narrow canals. Note the single intraembryonic coelom forms all three major body cavities: pericardial, pleural, peritoneal.
pleural fluid - A thin film of serous fluid that is produced by the pleura layers and acts as a lubricant, reducing the friction as the two layers slide against each other, and also helps to hold the two layers together as the lungs inflate and deflate.
pleuropericardial fold - (pleuropericardial membrane) An early embryonic fold which restricts the communication between pleural cavity and pericardiac cavity, contains both the cardinal vein and phrenic nerve.
pleuroperitoneal membrane - An early embryonic membrane that forms inferiorly at the septum transversum to separate peritoneal cavity from pleural cavity. (More? [../Notes/coelom.htm Coelom Notes])
radial alveolar count - The number of alveoli between respiratory bronchioles and the end of the acinus, a measurement used in postnatal lung growth.
respiratory bronchiolus - respiratory tract in the adult which has alveoli opening into it and has part of the wall lined by ciliated epithelium. In the canalicular period it is lined by flattened epithelium, which then becomes a mixture of flattened and cuboidal epithelium during the terminal sac period.
sacculation - A general anatomical term meaning to formed a series of sac-like expansions. In lung development, the term refers to the process of lung epithelial cell differentiation, vascular remodeling and thinning of the mesenchyme. This process leads to enlargement of the diameter and surface area of the alveolar sacs. Distal epithelial cells form 2 populations: 1. cells flattens, thins, and spreads to form type I cells; 2. cells remain cuboidal, acquire surfactant filled lamellar bodies and differentiate into type II cells.
saccule - respiratory tract that forms a large, thin walled air space lined by flattened epithelium (28 weeks to 2 months after birth).
septum transversum - (transverse septum) A mesodermal region in the early embryo. Identified externally as the junctional site between amnion and yolk sacs, and internally (within the embryo) lying directly beneath the heart and at the foregut/midgut junction. This ventro-dorsal "plate" of mesoderm contributes several structures including: the central tendon of diaphragm and some of the liver. The transverse septum has an important structural role in early embryonic development and is pierced by the gastrointestinal tract.
stenosis - Term used to describe an abnormal narrowing, usually in relation to a tube. For example, blood vessel, gastrointestinal tract or respiratory tract.
stomadeum - (stomadeum) A ventral surface depression on the early embryo head surrounding the buccopharyngeal membrane, which lies at the floor of this depression. This surface depression lies between the maxillary and mandibular components of the first pharyngeal arch.
surfactant - a detergent secreted by Type 2 alveolar cells between alveolar epithelium. Functions to lower surface tension, allowing lungs to remain inflated. Note: In humans, these cells and their secretion develop towards the very end of the third trimester, just before birth. Hence the respiratory difficulties associated with premature births (Newborn Respiratory Distress Syndrome, Hyaline membrane disease). (More? [../Notes/respire2.htm Respiratory Abnormalities] | [../Notes/respire2.htm#hyaline+membrane Newborn Respiratory Distress Syndrome])
terminal bronchiolus - respiratory tract forming the last airway before a respiratory bronchiolus.
terminal sac stage (terminal sac phase) Term used to describe fetallung development (late fetal week 24 to 36) the second last histological/developmental stage (Pseudoglandular, Fetal Canalicular, Terminal sac, Alveolar). During this stage branching and growth of the terminal sacs occurs, with cellular differentiation of the type -II pneumonocytes and type - I pneumonocytes. The final functional sac of the respiratory tree occurs at the next neonatal period, where gas exchange occurs between the alveolar space and the pulmonary capillaries.
transitional duct - respiratory tract lined by flattened epithelium, which connects the respiratory bronchiolus to the saccules during the terminal sac period. This structure later forms the alveolar duct.
visceral pleura - Forms the inner lining of pleural cavity, covering and attached to the lungs. Embryonically derived from the splanchnic mesoderm.
Waldereyer's Ring - Term used to describe the pharyngeal, palatine, and lingual tonsils which are located in the pharynx.
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Course Content 2009
Embryology Introduction | Cell Division/Fertilization | Cell Division/Fertilization | Week 1&2 Development | Week 3 Development | Lab 2 | Mesoderm Development | Ectoderm, Early Neural, Neural Crest | Lab 3 | Early Vascular Development | Placenta | Lab 4 | Endoderm, Early Gastrointestinal | Respiratory Development | Lab 5 | Head Development | Neural Crest Development | Lab 6 | Musculoskeletal Development | Limb Development | Lab 7 | Kidney | Genital | Lab 8 | Sensory - Ear | Integumentary | Lab 9 | Sensory - Eye | Endocrine | Lab 10 | Late Vascular Development | Fetal | Lab 11 | Birth, Postnatal | Revision | Lab 12 | Lecture Audio | Course Timetable
Cite this page: Hill, M.A. (2026, Mayıs 21) Embryology 2009 Lecture 10. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/2009_Lecture_10
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G