Corpus Luteum Development: Difference between revisions
mNo edit summary |
mNo edit summary |
||
| Line 13: | Line 13: | ||
{{Genital Links}} | {{Genital Links}} | ||
{| | {| | ||
| [[File:Regnier de Graaf.jpg| | | [[File:Regnier de Graaf.jpg|100px]]<br>Regnier De Graaf (1641-1673} | ||
| Regnier de Graaf (1641 – 1673) first observed {{corpus luteum}} in the {{ovary}} of a cow by its yellow structure, the yellow colour is caused by accumulation of steroidal hormones. | | Regnier de Graaf (1641 – 1673) first observed {{corpus luteum}} in the {{ovary}} of a cow by its yellow structure, the yellow colour is caused by accumulation of steroidal hormones. | ||
|} | |} | ||
Revision as of 11:37, 6 May 2019
| Embryology - 26 Jun 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Introduction
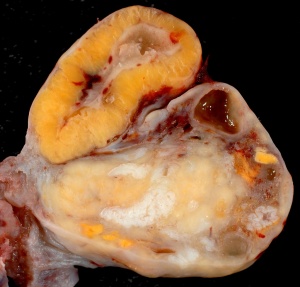
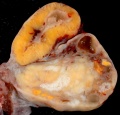
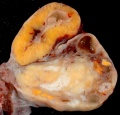
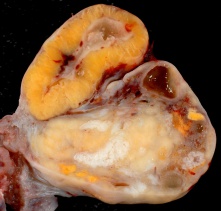
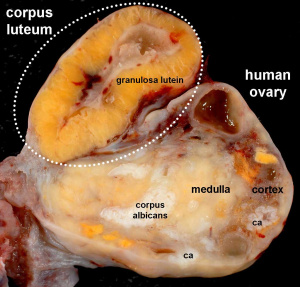
The corpus luteum (Latin, corpus = body, luteum = yellow) develops from the remains of Graffian follicle after ovulation. Functions as an endocrine organ (produce progesterone and estrogens) supporting pregnancy and preventing menstruation (loss of the endometrial lining). Formed during the luteal phase (ovary) (secretory phase, uterus) of the menstrual cycle by proliferation and differentiation (luteinization) of both the follicular granulosa cells (granulosa lutein cells) and thecal cells (theca lutein cells), that together interact to produce progesterone and estrogens (oestrogens). Ovarian luteal cells have an important role in progesterone (P4) production.
Peak luteal function during the menstrual cycle, determined by maximum luteal area, progesterone concentration and estradiol concentration, is observed about 6 days following ovulation.[1]
If fertilization and pregnancy does not occur, the corpus luteum degenerates, through a process called luteolysis, that eliminates the corpus luteum, initially forming a large blood-filled cavity, then the corpus albicans.
Genital Links: genital | Lecture - Medicine | Lecture - Science | Lecture Movie | Medicine - Practical | primordial germ cell | meiosis | endocrine gonad | Genital Movies | genital abnormalities | Assisted Reproductive Technology | puberty | Category:Genital
| ||||
|
 Regnier De Graaf (1641-1673} |
Regnier de Graaf (1641 – 1673) first observed corpus luteum in the ovary of a cow by its yellow structure, the yellow colour is caused by accumulation of steroidal hormones. |
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References Search term: Corpus Luteum | Corpus Albicans | Progesterone | granulosa lutein cells | thecal lutein cells | luteolysis |
Granulosa Lutein Cells
The internal follicular granulosa cells, differentiate into the granulosal lutein cells (large luteal cells). This luteinization change occurs within 30 to 40 hours of the ovulatory LH surge and the cells become are terminally differentiated. The cells begin secreting increasing amounts of both progesterone and some estrogen, that support the luteal phase of the menstrual cycle. Progesterone secretion during non-pregnancy occurs for about 10 days. These cells initially proliferate, become terminally differentiated and stop dividing.
- Search PubMed: granulosa lutein cells
Theca Lutein Cells
The surrounding follicular theca interna cells, differentiate into the thecal lutein cells (small luteal cells). These cells express receptors for luteinizing hormone (LH) to produce androstenedione, that supplies the granulosa cells the precursor for estrogen synthesis.
- Search PubMed: thecal lutein cells
History
| Regnier de Graaf (1641 – 1673) | Ludwig Fraenkel (1870 - 1951) |

|

|
| Regnier de Graaf (1641 – 1673) was the first observer in the ovary of a cow as a yellow structure, the yellow colour was caused by accumulation of steroidal hormones. | Ludwig Fraenkel (1870 - 1951) first identified the endocrine function of the corpus luteum.[4] |
Progesterone
| In 1934 progesterone (progestin) C21H30O2 was first isolated from the corpus luteum and its structure reported by four separate groups of researchers.[5][6][7][8]
|
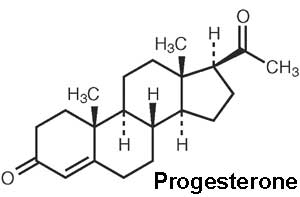
Progesterone molecular structure |
Luteolysis
During a cycle which does not result in pregnancy, the corpus luteum by day 22–24 initially loses the ability to produce progesterone (functional luteolysis). This allows the continued development of new follicles for ovulation and fertilization.
Next the functionally inactive corpus luteum is removed to avoid accumulation of non-functional luteal tissue within the ovary (structural luteolysis). This process of complete deletion will take several menstrual cycles.
Clinically, luteolysis may also occur during ART procedures (stimulated IVF/ICSI cycles) when gonadotropin-releasing-hormone (GnRH)-agonist are used for the final oocyte maturation, this reduces the risk for development of ovarian hyperstimulation syndrome (OHSS).[9] Administration of hCG or high doses of progesterone (P4) can prevent or counteract this induced luteolysis.[10]
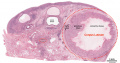
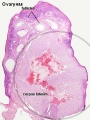
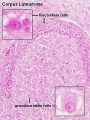
Histology
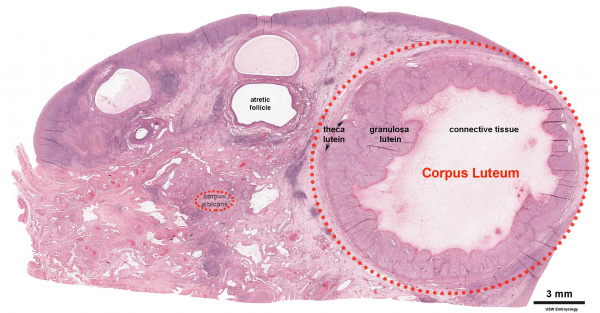
| |
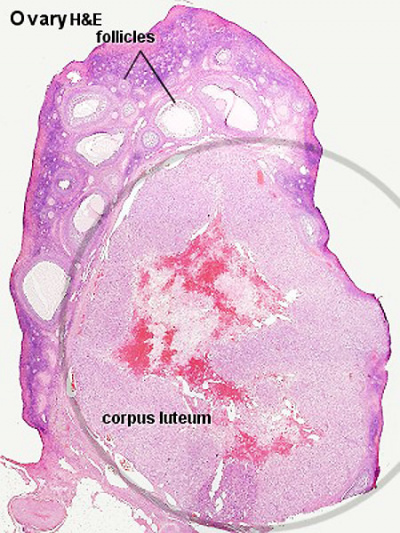
|

|
| Corpus luteum histology | Corpus luteum lutein cells |
Embryo Virtual Slide
| Human Ovary and Corpus Luteum |
| Ovary | Embryo Slides |
| Corpus Luteum Links: anatomy overview | image - histology overview | image - Layers granulosa and theca | image - Layers detail granulosa and theca | image - low power label | image - high power label | image - low power | image - high power | image - corpus albicans | theca and granulosa lutein cells | Granulosa cell | corpus luteum | granulosa lutein cells | theca lutein cells | corpus albicans | ovary | menstrual cycle |
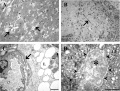
| Historic Papers: 1969 corpus luteum ultrastructure 1 | 1969 corpus luteum ultrastructure 2 |
Corpus Albicans
Corpus albicans histology
(corpora albicantia) (Latin, corpus = body, albicans = whitish) The histological structure formed by luteolysis of the corpus luteum in the ovary. If implantation does not occur and the hormone hCG is not released the corpus luteum degenerates and the structure is white, not yellow, because of the absence of steroid hormone synthesis/accumulation.
| Corpus Luteum Links: anatomy overview | image - histology overview | image - Layers granulosa and theca | image - Layers detail granulosa and theca | image - low power label | image - high power label | image - low power | image - high power | image - corpus albicans | theca and granulosa lutein cells | Granulosa cell | corpus luteum | granulosa lutein cells | theca lutein cells | corpus albicans | ovary | menstrual cycle |
| Historic Papers: 1969 corpus luteum ultrastructure 1 | 1969 corpus luteum ultrastructure 2 |
Animal Models
References
- ↑ Baerwald AR, Adams GP & Pierson RA. (2005). Form and function of the corpus luteum during the human menstrual cycle. Ultrasound Obstet Gynecol , 25, 498-507. PMID: 15846762 DOI.
- ↑ von Versen-Höynck F, Narasimhan P, Selamet Tierney ES, Martinez N, Conrad KP, Baker VL & Winn VD. (2019). Absent or Excessive Corpus Luteum Number Is Associated With Altered Maternal Vascular Health in Early Pregnancy. Hypertension , 73, 680-690. PMID: 30636549 DOI.
- ↑ Xu MQ, Jiang H, Zhang LQ, Sun XL, Luo D, Fu Y, Gao Y, Yuan B & Zhang JB. (2018). MiR-29b affects the secretion of PROG and promotes the proliferation of bovine corpus luteum cells. PLoS ONE , 13, e0195562. PMID: 29617446 DOI.
- ↑ Simmer HH. (1971). The first experiments to demonstrate an endocrine function of the corpus luteum. On the occasion of the 100th birthday of Ludwig Fraenkel (1870-1951). Sudhoffs Arch , 55, 392-417. PMID: 4261581
- ↑ Butenandt A. Neure Ergebnisse auf dem Gebiet der Sexualhormone. Wien Klin Wochenschr. 1934;47:936.
- ↑ Slotta KH, Ruschig H, Fels E. Ȕber der Hormon aus dem Corpus-luteum. Ber Chem Ges. 1934;67:1270.
- ↑ Hartmann M, Wettstein A. Ein krystallisiertes Hormon aus Corpus-luteum. Helv Chim Acta. 1934;17:878.
- ↑ Allen WM & Wintersteiner O. (1934). CRYSTALLINE PROGESTIN. Science , 80, 190-1. PMID: 17817057 DOI.
- ↑ Lawrenz B, Garrido N, Samir S, Ruiz F, Melado L & Fatemi HM. (2017). Individual luteolysis pattern after GnRH-agonist trigger for final oocyte maturation. PLoS ONE , 12, e0176600. PMID: 28459828 DOI.
- ↑ Lawrenz B, Ruiz F, Engelmann N & Fatemi HM. (2017). Individual luteolysis post GnRH-agonist-trigger in GnRH-antagonist protocols. Gynecol. Endocrinol. , 33, 261-264. PMID: 28019139 DOI.
Reviews
Sugino N, Matsuoka A, Taniguchi K & Tamura H. (2008). Angiogenesis in the human corpus luteum. Reprod. Med. Biol. , 7, 91-103. PMID: 29699289 DOI.
Woad KJ & Robinson RS. (2016). Luteal angiogenesis and its control. Theriogenology , 86, 221-8. PMID: 27177965 DOI.
Stouffer RL, Bishop CV, Bogan RL, Xu F & Hennebold JD. (2013). Endocrine and local control of the primate corpus luteum. Reprod Biol , 13, 259-71. PMID: 24287034 DOI.
Bachelot A & Binart N. (2005). Corpus luteum development: lessons from genetic models in mice. Curr. Top. Dev. Biol. , 68, 49-84. PMID: 16124996 DOI.
Stouffer RL. (2003). Progesterone as a mediator of gonadotrophin action in the corpus luteum: beyond steroidogenesis. Hum. Reprod. Update , 9, 99-117. PMID: 12751773
Reynolds LP & Redmer DA. (1999). Growth and development of the corpus luteum. J. Reprod. Fertil. Suppl. , 54, 181-91. PMID: 10692854
Articles
Billhaq DH & Lee S. (2019). A potential function of RLIP76 in the ovarian corpus luteum. J Ovarian Res , 12, 34. PMID: 30999946 DOI.
Garcia MR. (2017). Leptin Contributes to the Development of the Corpus Luteum. Cell Dev Biol , 6, . PMID: 29399429 DOI.
Maroni D & Davis JS. (2011). TGFB1 disrupts the angiogenic potential of microvascular endothelial cells of the corpus luteum. J. Cell. Sci. , 124, 2501-10. PMID: 21693577 DOI.
Historic
BROWNE JS, HENRY JS & VENNING EH. (1947). Studies in corpus luteum function. J. Clin. Endocrinol. Metab. , 7, 446. PMID: 20253396
HARRISON RJ. (1946). The early development of the corpus luteum in the mare. J. Anat. , 80, 160-6. PMID: 20996688
Corner GW. (1937). The Hormone of the Corpus Luteum. Trans Edinb Obstet Soc , 57, 61-80. PMID: 29612342
Allen WM, Butenandt A, Corner GW & Slotta KH. (1935). NOMENCLATURE OF CORPUS LUTEUM HORMONE. Science , 82, 153. PMID: 17811944 DOI.
Shaw W. The origin of the lutein cells of the corpus luteum. (1926) Proc R Soc Med. 19(Obstet Gynaecol Sect): 22-4. PMID 19985092
Dalton JC. Prize essay on the corpus luteum of menstruation and pregnancy. (1851) Philadelphia: T.K. and P.G. Collins.
Lee R. On the structure of the corpus luteum. (1839) Med Chir Trans. 22: 329-37. PMID 20895693
Search Pubmed
Search Pubmed: corpus luteum Development
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Genital Links: genital | Lecture - Medicine | Lecture - Science | Lecture Movie | Medicine - Practical | primordial germ cell | meiosis | endocrine gonad | Genital Movies | genital abnormalities | Assisted Reproductive Technology | puberty | Category:Genital
| ||||
|
| Menstrual Cycle | X Chromosome
Cite this page: Hill, M.A. (2024, June 26) Embryology Corpus Luteum Development. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Corpus_Luteum_Development
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G