Paper - The Internal Genital Organs of a Female Foetus of 15 cm Length
| Embryology - 27 Apr 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
Fleming AM. The internal genital organs of a female foetus of 15 cm length. (1927) J Anat. 61: 232–246. PubMed 17232868
| Historic Disclaimer - information about historic embryology pages |
|---|
| Pages where the terms "Historic" (textbooks, papers, people, recommendations) appear on this site, and sections within pages where this disclaimer appears, indicate that the content and scientific understanding are specific to the time of publication. This means that while some scientific descriptions are still accurate, the terminology and interpretation of the developmental mechanisms reflect the understanding at the time of original publication and those of the preceding periods, these terms, interpretations and recommendations may not reflect our current scientific understanding. (More? Embryology History | Historic Embryology Papers) |
The Internal Genital Organs of a Female Foetus of 15 cm Length
By Amy M. Fleming, B.SC., M.B., CH.B. (Glas.)
From the Pathological Department of the Royal Samaritan Hospital for Women, Glasgow
Introduction
In order to reach a true understanding of the various malformations of the genital tract, it is important to accumulate descriptions of specimens which appear to be normal. Such an investigation has been made upon the internal genital organs of a female foetus of about 4 months’ development, and the results are set forth in the following paper.
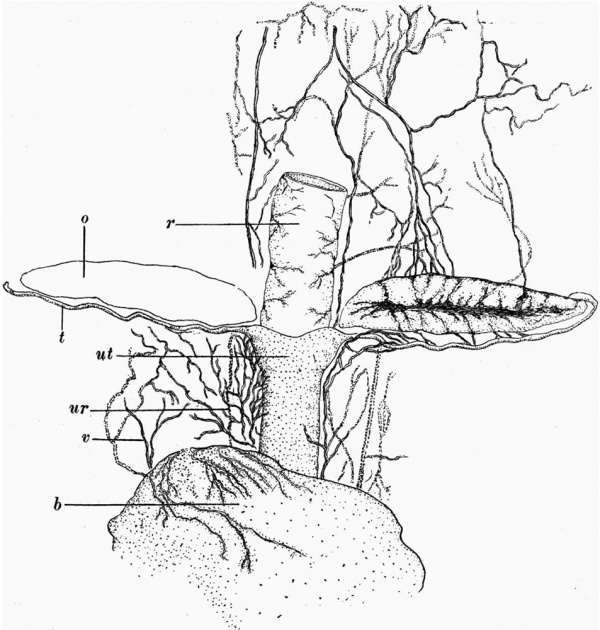
When this foetus was obtained, I was making a study of the peripheral innervation of the uterus in certain mammals. This led me to think that a description of the distribution of the nerve-tissue in this specimen might be of value. The specimen was obtained from a patient who died somewhat suddenly from Hyperemesis Gravidarum. The autopsy was carried out less than 12 hours after death. The contents of the pelvis were removed intact. The uterus was then opened, and the foetus extracted. The foetus looked quite fresh, no signs of maceration being evident. From vertex to breech it measured 15 cm. The pelvic bones and lower part of the vertebral column Were dissected out carefully, and without damage to the contents of the foetal pelvis. The peritoneal cavity was then opened from in front, and the foetus divided across a short distance proximal to the internal genital organs. Unnecessary portions of the anterior abdominal wall and of the muscles of the back were then removed, leaving as complete a block as possible of the organs within the lower abdomen and pelvis. This block was fixed in Kaiserling’s formalin solution, and a complete series of 2872 paraffin sections each 10 microns thick was prepared. These are numbered from the cranial extremity backwards. While the unsectioned block was in xylol, the vessels and other structures showed up so beautifully that a freehand drawing was made of the upper part of the specimen at this stage (fig. 1). The block includes the rectum posteriorly, the bladder anteriorly (portions only of the ureter being distinct on either side), and between these the genital organs. The ovaries are shaped like bay leaves, lying with their long axes horizontal. They lie proximal to and immediately above the Fallopian tubes. They extend from just within the upturned lateral end of the tube to a short distance medial to the opening of the tube into that portion of the uterus which will form the future body. The anterior surface, as indicated in the drawing, is not smooth, but shows a horizontal groove, from which side branches run as shallow sulci towards the proximal and distal borders. The tube on either side passes out from the uterus to terminate in a curve around the lateral extremity of the ovary. In its course it is thrown into small rounded curves encountered in all planes. Relative to its length, the duct is narrower than is the adult Fallopian tube. Other details will be described later.
The drawing shows that the utero-vaginal tube consists of a long cylindrical portion a little narrower than the rectum surmounted by a short broader part which widens out proximally, and which laterally is continued into the tubes. On the cranial extremity of the upper portion a shallow medial sulcus is seen, but no evidence of the presence of a sulcus is found on the anterior surface. There is no indication on the external surface whether the line of demarcation between the distal narrow and the proximal wide portion corresponds to the dividing line between the future body and the cervix, or between the cervix and the vagina.
The blood vessels show up particularly well. On the right-hand side, the loose tissue in which they lie had been slightly damaged during the manipulations of the block, and as a result the proximal portions of the Vessels were displaced outwards. For this reason, their course is not shown in the drawing. With the exception of a few reserved for special staining methods, the sections were stained with haematoxylin and eosin. Microscopically the preservation is good.
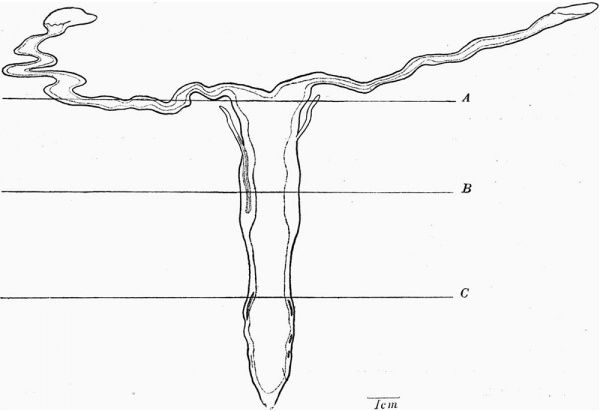
A flat reconstruction of the genital tract (fig. 2) shows its outline, the lumen being indicated by a dotted line. Remnants of Gartner’s ducts, in those parts of their course near to the utero-vaginal canal and to the tubal portion of the uterus, are seen. The tubes are long and narrow, and show the multiple curves already mentioned, but naturally only those apparent in one plane. The free end of the tube has a fimbriated extremity. Its opening faces posteriorly. From the margins of the opening strands of connective tissue are continued laterally in the edge of the mesosalpinx and also towards the ovary. At the other end, the tubes enlarge to form the tubal portion of the body of the uterus. In the reconstruction, the sulcus or the cranial extremity of the uterus at this stage of development is 0-4 mm. deep.
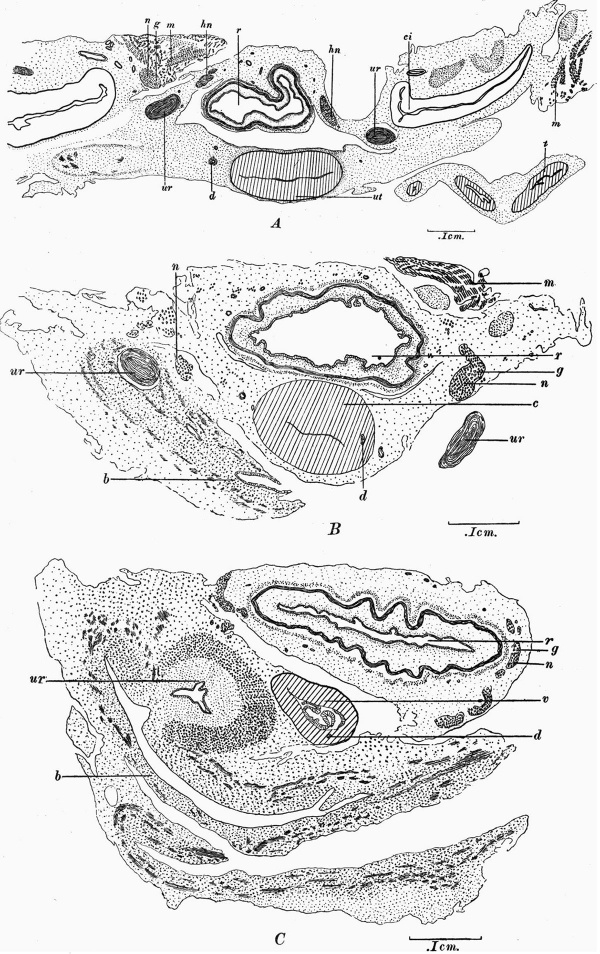
There is no median septum in the cavity. The formation of a single roughly symmetrical uterine cavity has kept pace with the union of the tubes to form the tubal portion of the body of the uterus. The unpaired portion of the generative tract is at this stage divisible into three portions. (1) The most proximal part is somewhat triangular in form, its base forming the future fundus of the uterus. (2) A cylindrical portion with thicker walls and a narrower cavity. (3) A long portion narrower in its proximal than in its distal half and possessing a relatively thin wall. The opening of this portion into the urogenital sinus is still closed by a solid mass of tissue. No sharp line of demarcation is present between these three portions. In length their cavities measure approximately 1-4 mm., 2-8 mm., and 5-6 mm. respectively. Diagrams illustrating the contour of a section from each of these three portions are seen in Fig. 3. The region of the transition between the triangular proximal portion and the remainder is marked externally by the entrance of the ducts of Gartner into the uterine substance. This is therefore probably the dividing line between that portion of the uterine mucous membrane developed from the uterine portion of the tubes and that developed from the utero-vaginal canal. These three portions are taken to correspond with the body of the uterus, cervix and vagina respectively, and later, histological evidence in support of this is given.
Fig. 1. Drawing of upper part of block while in xylol. b = bladder, o = ovary, r = rectum, t=Fallopian tube, ur = ureter, ut = uterus, v = blood vessels.
Fig. 2. Flat reconstructions of the genital tract from the serial section: for description see text. The levels from which Fig. 3 (A, B, C) are taken are indicated.
The Fallopian Tubes
From the reconstruction the tubes differ somewhat in measurement. That on the right is 1-12 cm. in length and varies in breadth from 0-02 to 0-08 cm.; the fimbriated extremity makes up 0-14 cm. of its length. The corresponding measurements on the left are 0-92 cm., 0-02 to 0-04 cm. and 0-14 cm. Both tubes pass outwards until opposite the lateral extremity of the ovary they curve upwards and finally terminate by a distinct inclination backwards, thus ending behind the ovary. Each tube possesses a canal patent throughout its entire length. The lining epithelium consists of cells whose protoplasm stains deeply. The nuclei are oval, intensely stained and large relative to‘ the size of the cells. In places the epithelium is in the form of a single layer which is definitely columnar in parts. In places no epithelium is recognisable because the walls of the tube are almost in apposition; but a potential lumen is always apparent. .
The lumen in its simplest form in cross-section has the appearance of a four-rayed star. In this specimen the two ventral and the two dorsal folds producing this formation are not (as described by Felix (1) in Keibel and Mall in a 50 mm. head~foot length embryo) due almost entirely to difference in height of epithelium, but at this stage are formed of embryonic connective tissue. Towards the outer end of the tube, besides these primary folds, there are secondary ones varying in size and shape.
Regarding the remainder of the wall of the tube, the two coats are distinct which Felix (1) describes in a foetus of 80 mm. trunk length. In my specimen, however, they are approximately equal in thickness. Muscle fibres in the adult sense cannot be recognised. Both coats are well vascularised. The inner has irregularly arranged cells with faintly stained protoplasm and oval deeply stained nuclei. The spindle cells of the outer coat form circular layers. The two coats become ill-defined as they are traced towards the outer end of the tube. The inner coat I regard as the forerunner of the stroma of the mucosa and the outer band as destined to form the muscular layer. This is in agreement with Felix (1) and, in the case of the outer band, with Bryce (2), who, however, makes no statement as to the fate of the inner coat.
The tissue of the entire tube is not sharply demarcated from that of the broad ligament. In the boundary zone between run the main vessels of supply to the tube. Near this, the layers, recognisable as serous and subserous by Felix (1), cannot be made out.
Caudal to the mesovarium the common urogenital mesentery passes forwards and distally to fuse with the connective tissue surrounding the inner end of the tube. Its point of attachment is about 2 mm. lateral to the median sulcus on the cranial aspect of the body of the uterus. The future body will therefore come to include the inner 1 mm. of the present Fallopian tube.
The Body of the Uterus
Regarding that part of the uterus proximal to the level at which the ducts of Gartner enter, we find that the anterior and posterior walls are relatively thick. The walls are formed by a continuation of the two coats already described in the wall of the tube. At this level they become widely separated by a third zone which makes up a considerable thickness of the wall. In this, densely packed clusters of cells are found. The nuclei of the cells of this zone are directed for the most part at right angles to the cavity of the uterus. Into this zone strands of cells turn inwards from the outer circular zone. The presence of these strands suggests that this middle zone represents part of the muscular coat of the fully formed uterus. No sharp demarcation exists between these three portions of the uterine wall. No fully formed smooth muscle bundles are present, but the nearest approach to this is found in the circular zone. N agel (3), (4) found smooth muscle arranged in bundles in embryos of 15-22 cm. length. This muscle appeared first under the peritoneal coat.
The cavity enclosed by these walls forms in transverse section a narrow wavy slit as the anterior and posterior uterine walls are for the most part in apposition. The epithelial lining is similar to that in the tube, although again it is absent in places.
The Cervix
This part, besides being marked off by the relative uniformity of the width of its cavity and by the width of its lateral walls (fig. 3, B), differs from the body in some details. This portion, instead of forming an oval in transverse section, is almost circular. The arrangement of the cells of the middle layer of the wall is more irregular than in the body. The increase in depth of the wall of this part is due to an increase in the outer two layers of the wall, i.e. in those layers which will go to form the muscular coat of the cervix.
The epithelium lining the cervix is similar in appearance to that present in the tube and body of the uterus, and here also at certain levels is absent. In the middle line into the upper part of the cervical canal there is a longitudinal bulging of the anterior wall. Opposite this prominence there is a longitudinal groove in the posterior wall. This prominence represents possibly the first commencement of the arbor vitae. No evidence is found in this specimen of the secondary folds of mucous membrane, which are described by Felix (1) as arising from the base of depressions in the wall of the cervix in embryos of about 150 mm. The lower end of the cavity of the cervix forms a narrow transverse slit.
The Vagina
Distal to this portion having a narrow slit-like lumen, there is a sudden widening of the genital canal, and a thinning of the walls (fig. 3, C). This foetus resembles those described by both Van Eckeren (5) and Mihalkovicz (6). These observers considered that this dilatation was the first sign of division into vagina and uterus. Van Eckeren described it as occurring in the second half of the fourth month. Mihalkovicz found a slight dilatation below the position of the external os, even in an embryo 14 cm. long. On the other hand, Nagel (3) described the first beginning of formation of the portio as an ingrowth of the cubical epithelium into the hind Wall. He found this in an embryo of 12 cm. length, but in one of 14-15 cm. trunk length it did not occur. This is an example of the variation in time at which the portio develops. Other observers bring evidence in support of this variation. Dohrn (7) described the anterior lip in embryos of 15-16 weeks as a halfmoon-shaped prominence on the anterior wall of the genital tract. Tourneux and Legay (8) described embryos of 12-5 and 16 cm. trunk length‘ in which the portio is present, whereas in one of 20 cm. trunk length he found only the anterior lip. Geibel (9) found the formation of the posterior fornix occurring only in the 6th month, no anterior fornix even then being present.
Just as in the more proximal portions of the genital tract, in this specimen the cavity is lined by epithelium, but at various levels it is absent. The epithelium is Stratified and non-vesicular. The nuclei of the cells are oval and small relative to the size of the cell and are rich in chromatin. It may now be noted that the character of the epithelium has been of no value in locating the exact limits of the different regions of the tract.
The structure of the remainder of the wall of the vagina differs from that of the uterus. At the junction of the cervix. and vagina the circular layer described in the cervix becomes very thin. Traced distally it soon disappears as a distinct layer. Otherwise the wall is formed of cells arranged irregularly, although the majority of them run longitudinally, especially in its proximal portion. About 2 mm. from the distal end of the vagina, the urethra becomes intimately associated with the anterior wall, so that the one mass of tissue appears to. embrace both structures. The vagina tapers down to end in a short solid portion. Gland-like projections of the epithelium of the urogenital sinus pass into this. This distal solid portion of the vagina, for the length of about 1 mm., is enveloped in a band of tissue, like that of the wall of the urethra. The cells of this tissue stain more deeply with eosin than do those of the wall of the vagina.
That portion of the wall intervening between the distal end of the vagina and the cavity of the urethra is made up of interwoven bundles of cells. In the distal 2 mm. of this are embedded branching tubules communicating with the urethral canal and lined by epithelium similar to its epithelium. These tubules I regard as representing the prostate gland in the male, which agrees with the finding of Evatt(10) from the examination of a 3% months old female foetus, and of Keibe1(11),(12) who found the openings of these glands similarly situated. On the other hand, Evatt quotes Gustav Pal1in(13) as having found their ducts opening neither into the urethra nor into the vagina, but exactly at the boundary between the two. Around these tubules, in my specimen, spindle-shaped cells are arranged concentrically. In the antero-lateral wall of the urethra only one tubule is seen and it does not penetrate far into the wall of the urethra. The wall of the urethra is thickly beset with minute venous spaces, especially on its antero-lateral aspect.
Fig. 3. A, transverse section no. 871: for level see fig. 2. B, transverse section no. 1169: for level see fig. 2. 0, transverse section no. 1486: for level see fig. 2. b = bladder, c = cervix, ci = common iliac artery, d = Gartner’s duct, g = ganglionic nerve cell, hn = hypogastric nerve, m = striped muscle, n = nerve bundle, r = rectum, t = Fallopian tube, wt = body of uterus, ur = ureter, v = vagina.
Remnants of the Wolffian System and Junctional Tubules
A. In the mesosalpinx, hilum of the ovary, and common urogenital mesentery, there is on either side a number of tubular structures. They lie proximal to the horizontal part of the tube and posterior to the ovary.
The majority of the tubules are clustered together to form the epoophoron which lies lateral to the mesovarium. Opposite and medial to the mesovarium, scattered tubules are found. The tubules are sinuous in their course. Each is cylindrical, lined with a single layer of cubical epithelium placed upon a basement membrane. The nuclei are large and deeply stained. The epithelial tube is surrounded by a condensation of primitive connective tissue cells. There is an inner coat longitudinal in arrangement and an outer ill-defined coat of circularly arranged cells. One of the more lateral of the tubules is distinguished by its larger lumen and by its thicker connective tissue wall-. This is the remnant of the Wolflian duct. It runs more or less parallel to the lateral portion of the Fallopian tube. No muscle cells are seen either in the walls of the Wolflian tubules or of the duct.
Two other types of tubules are found:
(a) The first is a goup of tubules lined by cubical epithelial cells with deeply stained nuclei. Each is surrounded by a very thin connective tissue coat, the cells of which are arranged circularly. The tubules differ from those of the epoophoron in having no well-defined longitudinal connective tissue coat. They lie medial and posterior to the ovarian artery in the common uro- genital mesentery where it is reflected on to the posterior abdominal wall just lateral to the ureter. In this specimen they are better developed on the right than on the left side. One of the tubules is distended with epithelial débris, its contents staining deeply with eosin. The distended part is 0-12 mm. in length. Some of these tubules are replaced by solid cords of cells. No blood-vessels are seen in these cell-clusters. The difference between this connective tissue wall and that of the tubules of the epoophoron may result from a difference in their stage of retrogression. Whether these more medial tubules repre- sent the paroophoron cannot be judged from the study of an isolated specimen. Duthie (14) failed to demonstrate the paroophoron in all twenty specimens examined. Felix (1) quotes Waldeyer(15) as having described it in a position cranial to the medial pole of the ovary and Rielander (16) in older foetuses and children caudal to the lateral half of the ovary. In my specimen these tubules lie cranial to the hilum of the ovary. .
(b) The second type occurs in the region of the ovarian fimbria. Each tube ends blindly and has a cavity irregular in outline. Three are present on the right side, one being in the hilum of the ovary and the other two nearer the tube. The one on the left side lies in an isolated projection from the posterior surface of the ovarian fimbria. No connection can be made out between them and the VVolffian duct and tubules. Each is lined with low cuboidal epithelial cells and is surrounded by a very thin condensation of connective tissue cells arranged circularly.
No smooth muscle fibres are seen in their walls. Duthie (14) describes similar spaces in a human foetus of the 8th month. They probably correspond to the rete or junctional tubules of Allen (17). If they are rete or junctional tubules, the tissue in which they lie must be ovarian or hilum tissue which has made, its way up the ovarian fimbria. Keith‘ and Doran(18) describe the ovarian tissue as running some way up the ovarian fimbria in a human foetus of the 8th month and in the new-born child. The facts that no connection can be made between any of them and the lateral end of the Wolffian duct and that their walls differ markedly from that of the Wolflian duct are against their being remnants of the pronephric duct.
B. Within and near the lower portion of the genital tract are remnants of Gartner’s duct. Meyer(19) found such remnants of Gartner’s duct in the uterus in all specimens at the stage of 2-3 months’ development, but only in 28~5 per cent. of specimens aged 4-6 months. On both sides (fig. 2) portions of Gartner’s duct are seen. On neither side can a connection be traced between these and the other remains of the Wolffian system in the lateral parts of the mesosalpinx. At their proximal end both appear as an ill-defined condensation of the connective tissue of the broad ligament. The duct on the right side begins at section 880 and can be traced down to section 1235. It lies about 0.4 mm. lateral to the wall of the uterus, surrounded by tortuous veins and just posterior to one of the branches of the uterine artery. Passing distally, it approaches the uterine wall. As it does so, its tissues become differentiated into an outer condensed and an inner loose zone. About 1 mm. from its commencement this central loose zone is replaced by the cavity of the duct, which is lined by a layer of deeply staining cubical epithelium. The cells of the outer condensed zone are arranged concentrically. Peripheral to this latter zone, no distinct layer of longitudinally arranged cells, such as was found by Meyer (19), can be made out in this specimen. The duct becomes closely applied to, and eventually enters the wall of the genital tract, where the thin lateral wall of the future body thickens out to form the wall-of the future cervix. As the duct is traced distally within the wall, its lumen enlarges antero-posteriorly and the epithelial lining assumes a columnar form. Its condensed band of connective tissue remains distinct from the tissue surrounding it, not only because of the concentric arrangement of its cells, but also because of their smaller size. As it passes down the cervical wall its cells become less regular in arrangement, so that it is less sharply marked off from the surrounding tissues. It passes gradually more deeply into the wall, until near its termination it lies completely within the circular layer and bulging the deeper layers inwards.
It ceases to be recognised about 0-04 mm. above the proximal end of the future vagina. This remnant in this part of its course is 3-5 mm. long.
On the left side the duct is much shorter. It appears first in section 862,lying in close apposition to the uterine artery about 3 mm. lateral to the wall of the uterus. As in the case of the right duct, no connection with the other vestigial structures in the broad ligament is established. As it is traced distally, it has the form of a poorly demarcated collection of cells with deeply stained rounded nuclei. A concentric arrangement of cells is only seen (fig. 3,A) opposite the minute epithelial lined cavity 0-02 mm. long. The duct cannot be traced beyond section 968, where it merges with the wall of the utero—vaginal canal. The left portion of the duct of Gartner thus measures only 1 mm. in this part of its course.
On neither side is there any trace of Gartner’s duct in the walls of the proximal half of the vagina. In the distal half on the right side two portions of the duct are found, the proximal one, 0-1 mm. in length, possessing a lumen-lined by columnar cells, and the distal, 0-04 mm. in length, having only a solid epithelial core. Both are placed in the antero-lateral wall of the vagina, but their position in the length of the vagina is represented in fig. 2. Between these two portions traces of the wall of the duct can be seen. On the left side the three portions, 0-04, 0-03, 0-02 mm. in length respectively, each possess a lumen lined by epithelium. On neither side are any remnants found at the distal extremity of the wall of the vagina, and no communication is established between the portions of the duct present and the glands opening dorsally from the urethra (cf. Kocks(20) and Bohm (21)). In this specimen, just as in those described by Rieder(22) and by Dohrn (23), the duct of Gartner has been retained more upon the right side than upon the left.
Sympathetic Nerve Distribution
The work of Langley and Anderson (24), (25) has shown that the nerve fibres supplying the uterus and the vagina pass chiefly by the sympathetic in the region of the fourth, fifth and sixth lumbar ganglia. Langley and Anderson(26) showed that a variable number of these fibres formed cell stations in the inferior mesenteric ganglia, and that many, and occasionally all, passed by way of the hypogastric nerves into the more peripheral nerve cells. The position and relations of these nerve cells and their morphology are still imperfectly known. On the course of the hypogastric nerves, Langley and Anderson (27) describe in the cat groups of ganglionic cells on the hypogastric nerves near the cervix, and in the rabbit similar cells at the lateral border of the vagina. From these they find a ganglionate plexus stretching along the vagina. In the guinea-pig Holste(28) found groups of ganglionic cells at the level of the cervix in the supravaginal connective tissue. Labhardt (29) reports that in the human subject Koemer and Polle both describe ganglia in the connective tissue around the upper half of the vagina and the cervix,‘ and that Pissemski, having found a plexus of nerves with ganglia scattered along it, denies the existence of an individual cervical ganglion such as described by Walter, Lee, Frankenhauser, Hashimoto and Jung. More recently, also, Mabuchi (30) has described two lateral, two ventral and a dorsal ganglion at the level of the cervix. As J. Ogata, according to Mabuchi, has shown that ganglionic cells had developed in the uterus, even in a foetus of 4 months, it was considered that valuable information on this subject might be obtained, if the position of these groups was found in a foetus of about 4 months, when the internal genital organs are sufficiently small to permit of a complete series of sections being made. Only in a specimen from a young foetus can suflicient of the broad ligament be included in the sections to permit the localisation of these ganglia.
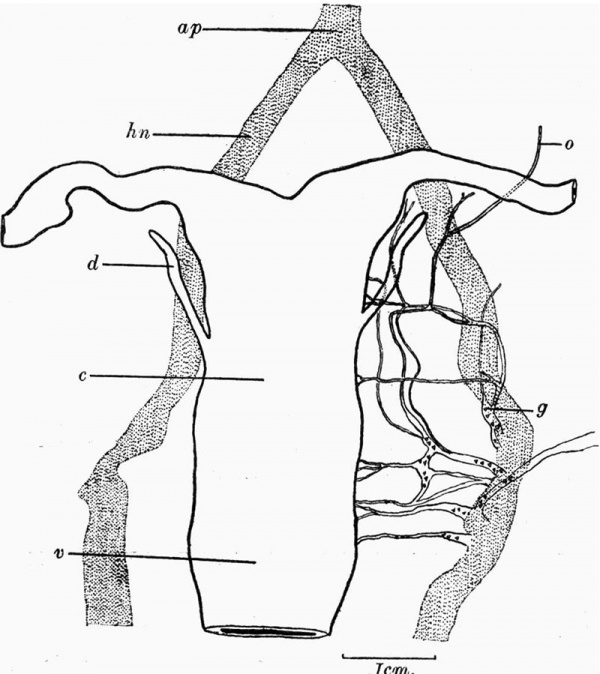
Fig. 4. Flat reconstruction of the nerves from the serial sections. ap = aortic plexus, c = cervix, d = Gartner’s duct, g = position of ganglionic nerve cell, hn = hypogastric nerve, o = nerve to the ovary, v = vagina.
A graphical reconstruction (fig. 4) has therefore been made from this specimen to show the branches of the hypogastric nerve to the uterus, and the position of the groups of ganglionic cells on these branches. The series of sections extended to the inferior mesenteric ganglia, from which bundles of nerve fibres pass to the intestine along with the inferior mesenteric artery.
A median plexus of nerve fibres runs distafly anterior to the aorta. The last-named (fig. 4«) divides about 2 mm. distal to the fundus of the uterus, to form the hypogastric nerves, along the course of which ganglionic nerve cells are scattered. They are most numerous opposite the cervix in those parts from which the branches supplying the uterus and tubes arise. The hypogastric nerves lie about 0-2 mm. lateral to the wall of the uterus.
On the course of the most proximal of the branches of the hypogastric nerve is a mass of ganglionic cells. This branch passes upwards and anteriorly, giving off a transverse branch to the cervix. Continuing its course it divides into two branches which run to the cervix at the level of the future internal os. From these transverse branches bundles of nerve fibres run upwards, to supply the upper part of the body of the uterus and the tubes. From the more lateral of these divisions a small branch is given off which passes into the hilum of the ovary. The original two branches, running to the uterus at the level of the internal os, communicate with the more distal branches of the main hypogastric nerve by lateral communicating unions in the broad ligament, which lie within 0-1 mm. from the wall of the cervix. The more lateral of these two lies behind the other.
Coming back now to the first branch of the hypogastric nerve mentioned above, about 0-5 mm. distal to it a second ganglionated branch runs transversely towards the cervix, and, as described, communicates with the branches already distributed to the uterus. This particular nerve shows two branches, one of which terminates at the middle of the cervix, and the other at the internal os. Another main branch is given off the hypogastric about 0-6 mm. distal to and communicating with this second branch. This branch comes off below the level of the peritoneal reflexion posteriorly. It supplies the lower part of the cervix, and sends a large branch laterally anterior to the ureter. This latter subdivision has ganglionic cells upon its course and distributes branches to. the bladder. Further distally two other branches of the hypogastric, supplying the lower end of the cervix, can be traced to the wall of the cervix. Excluding the first branch of the hypogastric, the communicating branches of which have been described, the remaining branches communicate with one another in an irregular manner.
It was found impossible to trace out the more distal branches supplying the vagina, as they are in such intimate association with the branches both to the rectum and to the urethra and bladder. The connections between the hypogastric plexus and the spinal nerves were necessarily destroyed during the removal of the vertebral column. In this specimen, therefore, the ganglionic cells are not confined to form a single cervical ganglion, but are scattered along the divisions of the hypogastric plexus in the region of the cervix.
Let us consider now what light this specimen thows upon the question as to whether ganglionic cells occur only on that part of the course of the fibres of the hypogastric nerves outside the uterus, or whether ganglionic cells are also present within the substance of the uterine muscle. Much work has been done, using all the commoner special nerve stains, and yet opinion is divided. According to Mabuchi (30), Korner, Polle, Henle, Liischka, Spiegelberg, Hashimoto, Jung, Ogata and Krause, only describe ganglia in connective tissues near the cervix and vagina; and Kilian, Rohrig (31), and Rein (32) failed to find any ganglia in the uterine substance. Dahl(33) has been unable to find ganglionic cells in the human subject, either in the mucous membrane or in the muscle of the uterus and tube. On the other hand, Gawronsky (34) described ganglion-like formations in the uterine parenchyma, such as had been found by Patenko, Kolossoff, Schenk and Herff. In the case of cells resembling ganglionic cells found by Clivio, Kéistlin, Spampani and Mabuchi (30) within uterine muscle, their nature was not proved, as their connection with nerve fibres was not made clear. Keiffer (35) reports the presence of small ganglionic cells within the uterine wall of the cat and the guinea-pig. In this specimen, no cells similar in size andshape and staining reaction to the ganglionic cells on the hypogastric nerves outside the uterus were found within the wall of the vagina, cervix, body or tubes. While the majority of the sections were stained with haematoxylin and with eosin, a series at intervals was stained by a modification of the Unna-Pappenheim method of staining, the methylgreen-pyronin method used by Hynntschak (36). Although these stains showed up the larger bundles of nerve fibres within the uterine muscle, the smaller bundles and individual nerve fibres could not be traced between the cells forming the wall of the uterus. It is therefore impossible to say definitely that no small ganglionic cells are present within the uterine wall, but one can almost certainly exclude the presence of ganglionic nerve cells similar in character to those found on the course of the sympathetic nerves outside the uterus.
Conclusions
- No muscle fibres are found in the tubes, the walls of which are composed of primitive connective tissue. Two zones of cells can be made out. The inner ones are irregularly arranged and the outer ones are larger, more deeply stained, and arranged in concentric circles.
- No trace of a median septum between the portions of the uterine cavity developed from the two-tubes is found.
- The unpaired portion of the internal genital tract is divisible into three parts: (a) a proximal triangular portion with thin lateral and thick anterior and posterior walls - the future body of the uterus, (b) a middle narrow portion, having a circular outline - the future cervix, and (c) a long tapering relatively thin-walled portion - the future vagina, which ends in a short solid mass, abutting on the cavity of the urogenital sinus.
- The transition from the cervix to the vagina occurs as a sudden widening of the genital canal under a narrow slit-like portion - the external os. At this stage no projection into the vaginal canal which would represent the port vaginalis is present.
- Glands corresponding to the prostate gland are found in the postero-lateral wall of the urethra, adjacentto the distal 2 mm. of the vagina.
- That part of Gartner’s duct within the wall of the uterus and vagina, is better preserved on the right than on the left side. A slight dilatation which would represent the ampulla of the duct is seen on the right side.
- There are no muscle fibres in the wall of the uterus, cervix or vagina although they are present in the wall of the bladder, urethra, and urogenital sinus.
- The sympathetic nerve fibres, supplying the internal genital organs, pass down the hypogastric nerves to the level of the cervix, and then pass to the tubes, uterus, cervix and upper portion of’ the Vagina, by several branches which communicate with one another. These branches are intimately associated with branches of the uterine artery.
- Ganglionic cells are scattered along the hypogastric nerves and occur on each of their main branches, but only on that part of their course opposite to the cervix and vagina.
- Within the wall of the genital tract, no cells comparable in size, shape or staining reaction to the ganglionic cells found on the more proximal portions of the sympathetic nerve fibres, are seen.
The work in connection with this paper has been carried out in the pathological laboratory of the Royal Samaritan Hospital for Women, Glasgow, under tenure of a scholarship from the Muirhead Trustees.
Bibliography
(1) Felix W. The development of the urinogenital organs. In Keibel F. and Mall FP. Manual of Human Embryology II. (1912) J. B. Lippincott Company, Philadelphia. pp 752-979.
(2) BRYCE, T. H. (1922). Development of Reproductive Organs. Munro Kerr, Clinical and Operative Gynaecobgy.
(3) NAGEL, W. (1891). “Uber die Entwickelung des Uterus u. der Vagina. beim Menschen.” Arch. far Milcro. Anat. Bd. xxxvn, S. 620-54.
(4) — (1894). “Uber die Entwickelung der innere u. aiissere Genitalien beim Menschlichen Weibe.” Arch f. Bd. xLv, S. 453-77.
(5) ACKEREN, F. VAN. “Beitr5i.ge zur Entwickelungsgeschichte der weiblichen Sexualorgane des Menschen.” Inaug. Diss. Zeitschriflfar wissenschaftliche Zoologie, Bd. xLvm, S. 20. (Cited from Nagel.)
(6) MIHALKOVICZ, G. V. (1885). “Untersucbungen iiber die Entwickelung der Hs.m- u. Geschlectsapparatus der Amnioten.” Intemationelle Monatschnfl fiir Anat. u. Hiatohzgie, Bd. II, S. 348. (Cited from Nagel.)
(7) DOHRN, F. A. R. “Uber die Entwickelung des Hymens.” Schriften der Gesellschaft zur Beforderung der gesammten Naturwisaenschaften zu Marburg, Bd. X, Supplement-Heft 1. (Cited from Nagel.)
(8) TOURNEUX and LEGAY (1884). “Mémoire sur le Développement de l’Uté1-us et du Vagin.” Journal de l’Anatomie, 1884, pp. 300-86.
(9) GEIBEL. “Uber Va.ria.bilit35.t in der Entwickelung der Geschlechtsorgane beim Menschen.” Verhandlungen der physilc.-med. Geaellschaft zu Wiirzburg. (Cited from Nagel.)
(10) Evatt EJ. The development of the prostate gland in the human female, and a study of the homologies of the urethra and vagina of the sexes. (1911) J. Anat. and Physiol. 45: 122-30. PubMed 17232868
(11) KEIBEL, F. (1896). “Zur Entwiokelungsgeschichte des menschlichen Urogenitalapparates. Arch. fiir Anat. u. 1896, S. 55-156.
(12) —- (1897). “Noch einmal zur Entwickelung des Urogenitalsystems beim Menschen. Arch. f. Anat. u. Entwiclcel. 1897, S. 201-3.
(13) PALLIN, G. (1901). “Beitriige zur Anatomie u. Embryologie der Prostate u. der Samenblasen.” Arch. f. Amt. u. Entwickel. 1901, S. 135-76.
(14) DUTHIE, G. M. (1925). “An Investigation of the Occurrence, Distribution and Histological Structure of the Embryonic Remains in the Human Broad Ligament.” Journ. Anat. July 1925, pp. 410-31.
(15) WALDEYER, W. (1870). Eierstoclc 11.. E5. Engelmann. Leipzig. (Cited from Felix.)
(16) RIELANDER (1904). Due Parodphoron. (Vergl. anat. u. path.-anat. Studie ) Marburg. (Cited from Felix.)
(17) ALLEN, B. M. (1906). “The Embryonic Development of the Rete-Cords and Sex—Cords of Ohryeemys.” Amer. Jaurn. of Anal. vol. .v, pp. 79-94.
(18) KEPPH, A. and DORAN, A. (1910). “A demonstration of Specimens Illustrating Cysts of the Female Appendages.” Journ. Obst. and Gynaec. vol. XVIII, pp. 246-54.
(19) MEYER, R. (1909). “Zur Kenntniss des Gartner’schen (oder Wolfi'schen) Ganges besonders in der Vagina u. dem Hymen des Menschen.” Arch. f. Mihr. Anat. u. Entwicht. Bd. LXXIII, S. 751-92.
(20) Kocxs (1882). “Uber die Gartner’schen Giinge beim Weibe.” Arch. f. Bd. xx, S. .487-91.
(21) BOHM (1883). “Uber Erkrankung der Gartner’schen Giinge beim Weibe.” Arch. fiir Gymik. Bd. XXI, S. 176-8.
(22) RIEDER (1884). “Uber die Gartner’schen Kanéile beim menschlichen Weibe.” Arch. fair path. Anat. Bd. xcvr, S. 100-30.
(23) DOHEN (1883). “Uber die Gartner’schen Kaniile beim Weibe.” Arch. fiir Bd. xxI, S. 328-45.
(24) LANGLEY and ANDERSON (1890). “The Innervation of the Pelvic Viscera.” Journ. Physical. vol. xrr, Proc. Physiol. Soc., Dec. 1890.
(25) — (1895). “Innervation of Pelvic and Adjoining Viscera.” Journ. Physiol. vol. xxx, pp. 71-130.
(26) — (1895). “Position of the Nerve Cells on the Course of the Efierent Nerve Fibres.” Jonrn. Phyaiol. vol. xrx, pp. 131-9.
(27) — (1896). “The Innervation of the Pelvic Viseera.” Journ. Phyaiol. vol. xx, pp. 372-406.
(28) HOLSTE (1924). “ Untersuohungen am iiberlebenden Uterus. 2. Mitt. Uterus als Testobjekt.” Arch. f. exp. Path. 14. Pharm. Bd. cr, H. 1}, S. 36-53.
(29) LABHARDT (1906). “Das Ver-halten der Nerven in der Substanz des Uterus.” Arch. fair G'yruiIc. Bd. LXXX, S. 133-211.
(30) MABUCHI (1924). “Morphologische Studien iiber das Verhalten der Nerven in den weiblichen Geschlechtsorganen des Menschen mit besonderer Beriicksichtigung der Ver Einderungen ihres Verhaltens wiihrend der Graviditit u. Menstruation u. in Zunehmenden Alter.” M itt. a. d. med. Fac. d. Kais. Univ. Tokyo, Bd. xxxr, H. 3, S. 385-495.
(31) Rfirmra (1879). “Experim. Untersuchungen iiber die Physiologie der Uterusbewegung.” Arch. f. path. Anal‘. 14.. Physiol. Bd. Lxxxvr, H. 1, S. 1-13.
(32) REIN, G. (1880). “Beitrag zur Lehre von der Innervation des Uterus.” Arch. f. d. gee. Physiol. Bd. xxm, S. 68-84.
(33) DAHL, V. W. (1924). In Die Lebensnerven. Miiller. Springer, Berlin.
(34) GAWRONSKY, N .V. (1894). “Uber Verbreitung und Endigung der Nerven in den weiblichen Genitalien.” Arch. far G~'yru'iIc Bd. xLvn, S. 271.
(35) KEIFFER, H. (1923). “Anatomical Condition of the Wall of the Uterus of the Lesser Mammals at Term.” Joum. Obat. and Gynaec. of the British Emp. vol. xxx, pp. 331-5.
(36) HYNNTSCHAK T. (1923). “Zur Anat. u. Phys. des Nervenapparates der Har-nblase u. des Ureters. 1. Mitt. Uber den Ganglionzellapparat. der Menschlichen Hamblase.” Arb. a.. d. Neural. Inst. a. d. Wiener Univ. Bd. xxrv, H. §, S. 409-53.
Cite this page: Hill, M.A. (2024, April 27) Embryology Paper - The Internal Genital Organs of a Female Foetus of 15 cm Length. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Paper_-_The_Internal_Genital_Organs_of_a_Female_Foetus_of_15_cm_Length
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G