ANAT2341 Lab 12 - Birth
| Lab 12: Introduction | Embryo to Fetus | Second Trimester | Third Trimester | Birth | Neonatal | Abnormalities | Online Assessment |
Introduction
Birth or parturition is a critical stage in development, representing in mammals a transition from direct maternal support of fetal development, physical expulsion and establishment of the newborns own respiratory, circulatory and digestive systems. These notes only cover the biological processes surrounding birth including fetal signaling changes and maternal signaling changes. Note that there is a growing worldwide trend in developed countries toward caesarean section delivery. There are a great number of comprehensive, scientific and general, books and articles that cover birth, childbirth or parturition. The time surrounding birth is known as the perinatal period.
Childbirth
- Parturition (Latin, parturitio = "childbirth") describes expelling the fetus, placenta and fetal membranes and is probably initiated by fetus not mother.
- Preterm birth - Risks of preterm birth in abnormal low birth weight (intrauterine growth restriction) and high (large for gestational age) categories are 2- to 3-fold greater than the risk among appropriate-for-gestational-age infants.
- Maternal labor - uterine contractions and dilation of cervix, process under endocrine regulation
- Placenta and fetal membranes - (Latin, secundina = "following") expelled after neonate birth
Uterine Myometrial Changes
- Smooth muscle fibers - hypertrophy not proliferation
- Stretching of myometrium - stimulates spontaneous muscular contraction, during pregnancy progesterone inhibits contraction
- Stimulating contraction - increased estrogen levels (placental secretion sensitizes smooth muscle), increased oxytocin levels (fetal oxytocin release- force and frequency of contraction), fetal pituitary prostaglandin production (estrogen and oxytocin stimulate endometrial production of prostaglandin)
Progesterone
- maintains pregnancy - initially synthesized by corpus luteum, then levels maintained by placenta
- hyperpolarizes myometrial cells (-65 mV), reduces excitability and conductivity
- Level in plasma may fall just before parturition, definitely decreases following delivery of placenta
Estrogens
- Group of steroidal hormones, peak when parturition begins
- induce increased synthesis of actomyosin and ATP in myometrial cells
- alter membrane potential (-50 Mv) enhances excitation/conduction
- act to directly increase myometrial contraction
- indirectly by increasing oxytocin from pituitary gland
- Estriol - synthesized by fetus and placenta
Oxytocin
- Peptide hormone (8aa) from maternal posterior pituitary, initiation and maintenance of labour (synthetic form labour induction)
- myometrium sensitivity to oxytocin (increased by estrogen, decreased by progesterone)
- stimulus for release - mechanical stimulation of uterus, cervix and vagina (ethanol inhibits release)
Prostaglandins
- hydroxy fatty acids - sythesized by placenta, amniotic fliud contains mainly PGF2 alpha, causes myometrial contraction (also in maternal plasma)
- prostaglandin F2 alpha (PGF2 alpha) and prostaglandin E2 (PGE2) - used to induce labour (intravenous, oral, intravaginal, intraamniotic)
- Aspirin inhibitor of PG synthesis - leads to increased duration of pregnancy
External Environment
- mainly shown in other species parturition occurs in peaceful undisturbed surroundings, stress may have an inhibitory effect on oxytocin release
- Most human births occur at night (peak at 3am) diurnal rhythm influence
Labour Stages
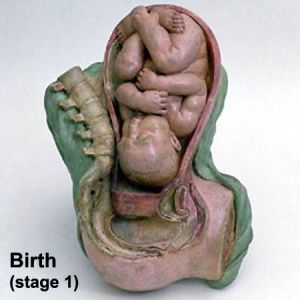
Stage 1 - dilatation
- uterine contractions 10 minutes apart, function to dilate cervix fetal membranes rupture releasing amnion, 7 -12 hours (longer for first child)
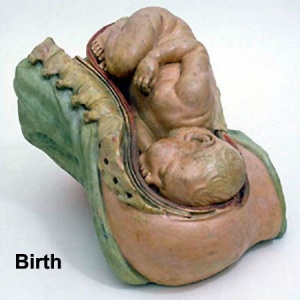
Stage 2 - expulsion
- uterine contractions push fetus through cervix and vagina, contractions 2-3 minutes apart, 20 - 50 minutes
Stage 3 - placental
- following child delivery contractions continue to expel placenta. haematoma separates placenta from uterine wall, separation occurs at spongy layer of decidua basalis, 15 minutes
Stage 4 - recovery
- continued myometrial contraction closes spiral arteries, 2+ hours
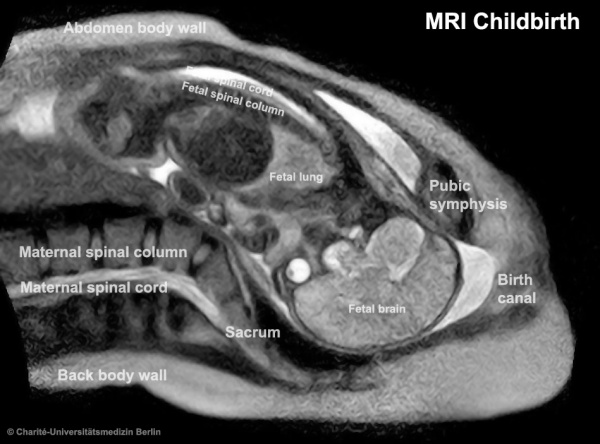
The birth of a child in an “open” MRI (magnetic resonance imaging) scanner that allows a mother-to-be to fit fully into the machine. |
|
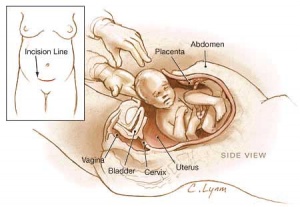
Birth - Caesarean
The rate of caesarean delivery (c-section or C/S) compared to normal vaginal birth is variable between countries (12-25%) and increasing, particularly in older women. There are a number of different explanations as to why this is occuring, including maternal or fetal complications of either development or delivery. The World Health Organization (WHO) recommended rate (10 - 15%).
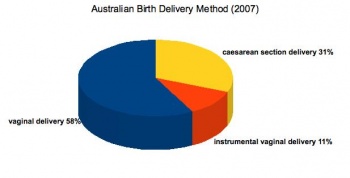
Method of Birth (Australia, 2007)
- 57.9% vaginal births
- 11.2% had an instrumental vaginal delivery (forceps or vacuum extraction)
- 30.9% caesarean section births
- 21.1% in 1998, 30.8% in 2006, rate recently stable
- 83.3% of these were repeat caesarean sections
Links: Birth - Caesarean Delivery
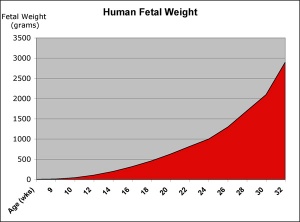
Birth Weights
| Birth weight (grams) | less 500 | 500 – 999 | 1,000 – 1,499 | 1,500 – 1,999 | 2,000 – 2,499 | 2,500 – 2,999 | 3,000 – 3,499 | 3,500 – 3,999 | 4,000 – 4,499 | 4,500 – 4,999 | 5,000 or more |
| Classification | Extremely Low Birth Weight | Very Low Birth Weight | Low Birth Weight | Normal Birth Weight | High Birth Weight | ||||||
The primary causes of VLBW are premature birth (born <37 weeks gestation, and often <30 weeks) and intrauterine growth restriction (IUGR), usually due to problems with placenta, maternal health, or to birth defects. Many VLBW babies with IUGR are preterm and thus are both physically small and physiologically immature.
Birthweight (Australia, 2007)
- 92.1% of liveborn babies had a birthweight in the range 2,500–4,499 grams
- average birthweight was 3,374 grams
- 17,976 (6.2%) low birthweight (weighing less than 2,500 grams)
- 2,956 (1.0%) very low birthweight (weighing less than 1,500 grams)
- 1,288 (0.4%) extremely low birthweight (weighing less than 1,000 grams)
Data: Australia’s mothers and babies 2007 AIHW Perinatal statistics series no. 23
| Practical 12: Embryo to Fetus | Second Trimester | Third Trimester | Birth | Neonatal | Abnormalities |
Additional Information
Stillbirths
Commentary: reducing the world's stillbirths. Goldenberg RL, McClure EM, Belizán JM. BMC Pregnancy Childbirth. 2009 May 7;9 Suppl 1:S1. PMID: 19426464 | [ http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2679407/ PMC2679407]
- "One of the major success stories of modern obstetrics in high-income countries in the last 5 decades is the reduction of stillbirths from rates as high as 50 per 1000 births to about 5 per 1000 births today. Fetal mortality associated with obstructed labour, asphyxia, hypertension, diabetes, Rh disease, placental abruption, post-term pregnancies and infections such as syphilis all have declined. Much of this success has occurred in term births in the intrapartum period so that most stillbirths in high-income countries now occur in the antepartum period and are pre-term."
| Lab 12: Introduction | Embryo to Fetus | Second Trimester | Third Trimester | Birth | Neonatal | Abnormalities | Online Assessment |
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, May 1) Embryology ANAT2341 Lab 12 - Birth. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/ANAT2341_Lab_12_-_Birth
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G