2015 Group Project 1
| 2015 Student Projects | ||||
|---|---|---|---|---|
| 2015 Projects: Three Person Embryos | Ovarian Hyper-stimulation Syndrome | Polycystic Ovarian Syndrome | Male Infertility | Oncofertility | Preimplantation Genetic Diagnosis | Students | ||||
| 2015 Group Project Topic - Assisted Reproductive Technology | ||||
| This page is an undergraduate science embryology student and may contain inaccuracies in either description or acknowledgements. | ||||
Three Person Embryos
Three Person Embyo is a form of germline fertility treatment by which an oocyte are formed containing maternal and paternal DNA and donated mitochondrial DNA (mtDNA). This can be with the presence or absence of maternal mtDNA. The purpose of this treatment is to prevent the maternal inheritance of hereditary mitochondrial diseases and treat some forms of infertility caused by mtDNA mutation. It is also referred to as Mitochondrial Donation and Mitochondrial replacement-assisted IVF.
<iframe width="560" height="315" src="https://www.youtube.com/embed/0Zs2KntZ7vU" frameborder="0" allowfullscreen></iframe>
History
Timeline of Mitocondrial Donation
1990s
- -1997
- St Barnabas Hospital announces it has achieved a live birth from mitochondrial donation via Ooplasmic transfer [1]
- -1998
- FDA ban use of Ooplasmic transfer techniques in the USA
- First oocyte with DNA transferred from a first polar body fertilized brought to term in a mouse model. [2]
2000s
- -2008
- 13th Nov The Human Fertilization and Embryology Act allows research into the techniques of three person IVF.
- -2009
- First success-full trails spindle transfer in rhesus monkeys [3]
2010s
- -2015
- 29th October regulations to allow the open use of three person IVF via pronuclear transfer in fertility clinics comes into affect in the UK.
Benefits
Mitochondria linked Infertility
https://embryo.asu.edu/pages/ooplasmic-transfer-technology http://www.ncbi.nlm.nih.gov.wwwproxy0.library.unsw.edu.au/pubmed/12470582
Hereditory mitochndrial Disease
Due to the nature of maternal only inheritance of mitochondria between generations. Any offspring of an affected mother will inherit the same disposition to a mitochondrial disease. In the UK its estimated that 152 women per year are at risk of transmitting mtDNA diseases and 778 in the United States[4].
Technical Progression
Three-person in-vitro fertilization is the process where gene replacement exerted to prevent mitochondrial disease passing through generations. Main aproaches to achieve this goal involve the replacement of mitochondrial genome between gametes or embryos [5] [6].
- The first proposed treatment is cytoplasmic transfer, which transfers a small part of ooplasm from one oocyte to another. however, this approach were then considered to be inadequate to prevent the inheritance of diseased mitochondrial. because it adds in donor mitochondria without removing the mutated mtDNA, which will then generate a 'heteroplasmic oocyte' with both mitochondria haplotypes [7].
- New emerged approaches of mitochondrial transmission are pronuclear transfer(PNT), spindle transfer (ST) and Polar body transfer (PBT). however, none of this techniques have been proved on generating healthy human offspring due to the technical difficulty, as well as the ethics issues being recognized worldwide [8].
- Major breakthroughs of these techniques rely on the practice on animal models (mice and primate) [9], early stage human embryo and stem cell studies [10].
Image Source: http://www.popsci.com.au/science/medicine/what-3parent-babies-mean-for-the-future-of-reproductive-medicine,400376
Cytoplasmic transfer
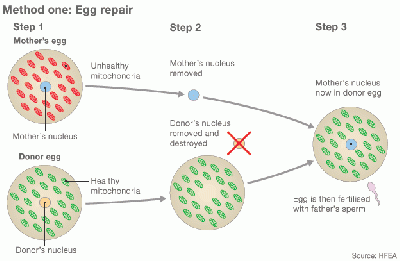
Cytoplasmic transfer is also named Oooplasmic transfer. It is an in vitro fertilization (IVF) technique, which can be performed either as a repair of oocyte or repair of Emryo [11] [12]. In method one, the cytoplasm is withdrew from a donor’s oocyte, and then injected into a patient’s oocyte together with the sperm cells which will then fertilize the oocyte. In Method two, the cytoplasm from donor is injected into a patient’s fertilized oocyte.
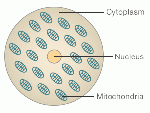
Simplified Cell Structure (The girl with three biological parents)
Diagram of Cytoplasmic transfer (The girl with three biological parents)
Timeline
- 1982, United Kingdom - Audrey Muggleton-Harris's group at MRC Laboratory Animals Center in Surrey, developed the technique and reported the first successful mammalian cytoplasmic transfer in mice.
- 1982 United Kingdon - Muggleton-Harris's group transferred cytoplasm from mice strains whose oocytes divide past the two-cell stage in vitro into mice to overcome the two-cell barrier
- 1997, United States - Jacques Cohen, Richard Scott, Tim Schimmel, Jacob Levron, and Steen Willadsen at the Institute for Reproductive Medicine and Science of St. Barnabas in West Orange, New Jersey, announced the birth of a baby girl after the first successful human cytoplasmic transfer [13].
- 1998 United States – The US Food and Drug Administration (FDA) banned the procedure.
- 2002 United States - one of the children conceived through ooplasmic transfer were diagnosed with pervasive developmental disorder, and indicated mild developmental delays to severe autism.
- 2014 United States - public meetings to discuss mitochondrial manipulation techniques were held by FDA. There was no formal decision made base on the efficacy of Cytoplasmic transfer, but agreements were made on further practice on animal models to provide scientific data.
Human Model
Alana Saarinen is one of only 30 to 50 people in the world who was conceived through a pioneering infertility treatment in the USA. Part of her mitochondria, and mitochondria DNA were from a third person by Cytoplasmic transfer. [[1]]
Heteroplasmy
Heteroplasmy is one of the major concerns arise regarding cytoplasmic transfer in IVF procedure. Severe disease can occur due to a mixture of mtDNA in the offspring’s mitochondria. They may affect the development of the muscle, brain and endocrine system.
Spindle-chromosome transfer
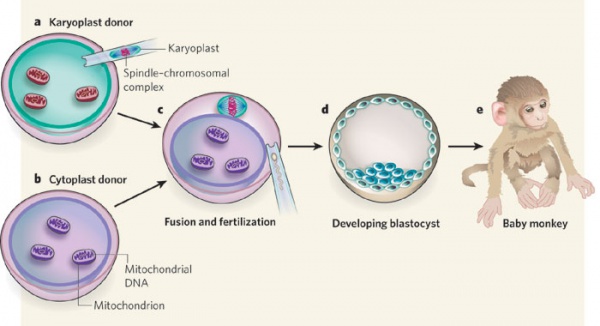
Transfer of the metaphase II spindle from the unfertilized oocyte of an affected woman to an enucleated donor oocyte, spindle transfer between human oocytes, resulting in blastocyst development and embryonic stem cell derivation, with very low levels of heteroplasmy.
(reproduced diagrams to be uploaded)
Primate model
Spindle-chromosome transfer in primates supports normal development to adults and low mtDNA carryover.[14]
Current Research
- PMID 23103867 Towards germline gene therapy of inherited mitochondrial diseases.
Tachibana M, etc. investigated the spindle-chromosomal (ST) complex transfer on human oocytes. they concluded that the mtDNA can be efficiently replaced in human oocytes, although some ST oocytes displayed abnormal fertilization[15].
- PMID 25973765 Extreme-Depth Re-sequencing of Mitochondrial DNA Finds No Evidence of Paternal Transmission in Humans
Extreme-high depth mtDNA re-sequencing can perform up to ~1.2 million-fold coverage, Pyle A, etc. has proved the dogma that mammalian mitochondrial DNA (mtDNA) is strictly maternally inherited. It also indicated that an active mechanism eliminates paternal mtDNA which likely acts at the molecular level[16].
- PMID 19710649 Mitochondrial gene has been efficiently replaced by spindle-chromosomal complex transfer one egg to an enucleated, mitochondrial-replete egg in primate offspring and embryonic stem cells.
None-human primate model were used for study the efficiency of spindle-chormosomal complex transfer.They reported that the reconstructed oocytes were capable of supporting normal fertilization, embryo development and produced healthy offspring. and there were no contribution of spindle donor mtDNA detected in offspring[17]. (Here are copy right and permission issues regarding reuse)
Pronuclear transfer
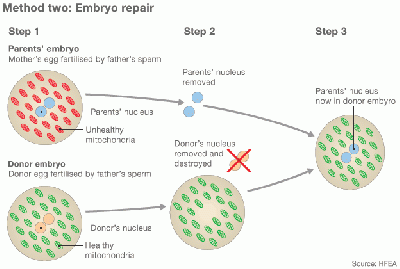
Pronuclear transfer is performed as a repair of embryo. The nuclear genome from the pronuclear stage zygote of an affected woman is transferred to an enucleated donor zygote
- It begins with creating an embryo using the parents’ sperm and eggs.
- At the same time, a second embryo is created using a donor egg with healthy mitochondria and the father’s (or donor) sperm.
- The pronuclei are removed from the single-cell stage embryo (day one). The leftover enucleated embryo with diseased mitochondria is discarded.
- The pronuclei of the second embryo are removed and discarded.
- The parents’ pronuclei can be placed into the second embryo for development.
- The developed embryo will then be transferred into the mother.
It is reported that pronuclear transfer is associated with high levels of mtDNA carryover in mice but low levels in human embryos, carries ethical issues secondary to donor embryo destruction [18]
(reproduced diagrams to be uploaded)
Diagram of Pronuclear transfer [19]
Human Embryo Model
PMID 20393463 Pronuclear transfer in human embryos to prevent transmission of mitochondrial DNA disease[20] As the name suggest this paper looks at pronuclear transfer as way to remove donor mitochondria measured by mt-DNA. And it effectiveness in doing so. And the processes that occur in the oocyte when this method is used
Current Research
Polar body transfer
Polar bodies are small cells formed during the meiotic reductive division of the oocyte. they contains complementary choromosomes (to the mature oocyte) and small amount of cytoplasmic segregation[21].
- Polar body 1 is formed and released during ovulation. it contains a diploid set of chromosomes.
- Polar body 2 is formed during fertilization and can be identified in the zygote. it contains a haploit set of chromosomes.
- Both polar bodies are unable to be fertilized and disintegrate eventually
It has been reported with mice modle that coupling Polar body transfer with Pronuclei transfer or Spindle-choromosome transfer may increase the yield of reconstructed embryos with low mtDNA carryover. [22]
(reproduced diagrams to be uploaded) PMID 24949971
Mice Model
PMID 24949971 Polar body genome transfer for preventing the transmission of inherited mitochondrial diseases [23] The authur adopts polar body transfer to prevent the transmission of mtDNA variants. they also compare the effects of different types of germline genome transfer, including spindle-chromosome transfer, pronuclear transfer, and first and second polar body transfer, in mice. Their pre-clinical model indicate that polar body transfer has better potential in preventing the inheritance of mitochondrial diseases.
Current Research
Other approaches
germinal vesicle nuclear transfer
Ethics
germ line therapy gender selection or medical purposes http://www.fertstert.org/article/S0015-0282(12)01872-9/abstract (lady chooses embryo with low level mito mutations and male)
1.PMID 26239841 The ethical challenges of the clinical introduction of mitochondrial replacement techniques. [24] The first part of the paper evaluates the three concerns about the safety of mitochondrial replacement techniques including whether it is ethical; persons with three genetic contributors and the trust of society. And then, two recommendations are made.
2.PMID 21059727 Ethics of mitochondrial gene replacement: from bench to bedside. [25] Both of the risks and benefits are accessed in this paper after the briefly introduction of mitochondrial replacement techniques. And then the question of when are enough safeguards made to justify introducing mitochondrial gene replacement into the clinic is discussed.
3.PMID 25888328 Mitochondrial replacement to prevent the transmission of mitochondrial DNA disease. [26] This paper discussed about the ethics and feasibility of mitochondrial replacement techniques. The possibility of preventing the transmission of mtDNA disease by MRT is first discussed. Moreover, the four big challenges mainly ethics are discussed.
Legal Status
Permitted
Britain is the only country in the world legally allows the inheritable genetic modification of humans. On February 24, 2015, the House of Lords approved regulations. Earlier in the month, the UK House of Commons also approved the techniques that would create an embryo with genetic material from three different people and result in inheritable genetic modification, with 382 votes in favor and 128 against. [27]
Under Discussion
In USA, the legality of mitochondrial manipulation techniques is still under discussion. On February 25 and 26, 2014, public meetings that included discussion of mitochondrial manipulation techniques were held by The US Food and Drug Administration (FDA). None of the seven public spoke who had contacted the FDA in advance in favor of the techniques. There was no formal decision made base on the efficacy of Cytoplasmic transfer, but agreements were made on further practice on animal models to provide scientific data. On January 27 2015, the Institute of Medicine (IOM) held the first in a series of meetings to fulfill the FDA’s request to consider the Ethical and Social Policy of Novel Techniques for Prevention of Maternal Transmission of Mitochondrial DNA Diseases.
Prohibited
Further Reading
useful publications:
PMID 23608245 The ethics of creating children with three genetic parents. [28]
PMID 24382342 Three-Parent IVF: Gene Replacement for the Prevention of Inherited Mitochondrial Diseases.[29]
PMID 20933103 Mitochondrial function in the human oocyte and embryo and their role in developmental competence.[30]
PMID 26020522 Mitochondrial reshaping accompanies neural differentiation in the developing spinal cord.[31]
PMID 25421171 The impact of mitochondrial function/dysfunction on IVF and new treatment possibilities for infertility.[32]
PMID 25807984 Risks inherent to mitochondrial replacement.[33]
Glossary
Maternal Spindle Transfer: The transfer of nuclear DNA from a patient egg into a donor egg with its nuclear DNA removed, which is then fertilized and implanted via standard IVF.
Ooplasmic Transfer: The injection of ooplasm from a donor egg into a patient egg. Leads to mitochondrial heteroplasmy.
Pronuclear Transfer: The pre-fertilized nuclear DNA form a patient is transferred into a donor egg with its nuclear DNA removed, which is then fertilized and implanted via standard IVF.
References
- ↑ <pubmed> 9250192 </pubmed>
- ↑ <pubmed> 9674999 </pubmed>
- ↑ <pubmed> 19710649 </pubmed>
- ↑ <pubmed> 25629662 </pubmed>
- ↑ <pubmed> 24382342</pubmed>
- ↑ <pubmed> 25573721 </pubmed>
- ↑ <pubmed> 24382342</pubmed>
- ↑ <pubmed>24373414</pubmed>
- ↑ <pubmed> 25229667 </pubmed>
- ↑ <pubmed> 23103869 </pubmed>
- ↑ <pubmed> 24382342</pubmed>
- ↑ <pubmed> 24382342</pubmed>
- ↑ <pubmed> 9250192</pubmed>
- ↑ <pubmed> 25573721 </pubmed>
- ↑ <pubmed> 23103867</pubmed>
- ↑ <pubmed> 25973765 </pubmed>
- ↑ <pubmed> 25973765 </pubmed>
- ↑ <pubmed> 25573721 </pubmed>
- ↑ <pubmed> 25377180</pubmed>
- ↑ <pubmed> 20393463 </pubmed>
- ↑ <pubmed> 24949971 </pubmed>
- ↑ <pubmed> 25573721 </pubmed>
- ↑ <pubmed> 24949971 </pubmed>
- ↑ <pubmed>26239841</pubmed>
- ↑ <pubmed>21059727</pubmed>
- ↑ <pubmed>25888328</pubmed>
- ↑ Gallagher, James (03 February 2015) MPs say yes to three-person babies BBC News Retrieved 09 October 2015.
- ↑ <pubmed> 23608245</pubmed>
- ↑ <pubmed> 24382342</pubmed>
- ↑ <pubmed> 20933103 </pubmed>
- ↑ <pubmed> 26020522 </pubmed>
- ↑ <pubmed> 25421171</pubmed>
- ↑ <pubmed> 25807984</pubmed>