Spermatozoa Development: Difference between revisions
| Line 66: | Line 66: | ||
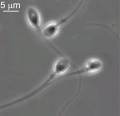
* 60 µm long, actively motile | * 60 µm long, actively motile | ||
* divided into 3 main regions (head, neck and tail) | * divided into 3 main regions ([[S#spermatozoa head|head]], [[S#spermatozoa neck|neck]] and [[S#spermatozoa tail|tail]]) | ||
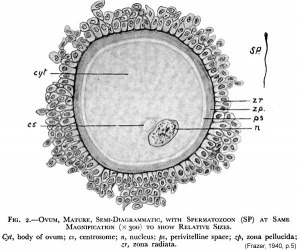
* head - (flattened, 5 µm long by 3 µm wide) the nucleus and acrosome. Posterior part of nuclear membrane forms the basal plate. | * head - (flattened, 5 µm long by 3 µm wide) the nucleus and acrosome. Posterior part of nuclear membrane forms the basal plate. | ||
* neck - (1 µm) attached to basal plate, transverse oriented centriole, contains nine segmented columns of fibrous material, continue as outer dense fibres in tail. | * neck - (1 µm) attached to basal plate, transverse oriented centriole, contains nine segmented columns of fibrous material, continue as outer dense fibres in tail. | ||
Revision as of 09:05, 10 May 2010
Introduction
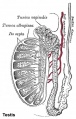
This page introduces the development of spermatozoa, the male haploid gamete cell, produced by meiosis in the seminiferous tubules of the testis (male gonad).
--Mark Hill 19:34, 5 August 2009 (EST) Page under development - notice removed when completed.
Some Recent Findings
- Microgravity promotes differentiation and meiotic entry of postnatal mouse male germ cells. Pellegrini M, Di Siena S, Claps G, Di Cesare S, Dolci S, Rossi P, Geremia R, Grimaldi P. PLoS One. 2010 Feb 4;5(2):e9064. PMID: 20140225 | PLoS One
- "A critical step of spermatogenesis is the entry of mitotic spermatogonia into meiosis. Progresses on these topics are hampered by the lack of an in vitro culture system allowing mouse spermatogonia differentiation and entry into meiosis. Previous studies have shown that mouse pachytene spermatocytes cultured in simulated microgravity (SM) undergo a spontaneous meiotic progression. Here we report that mouse mitotic spermatogonia cultured under SM with a rotary cell culture system (RCCS) enter into meiosis in the absence of any added exogenous factor or contact with somatic cells."
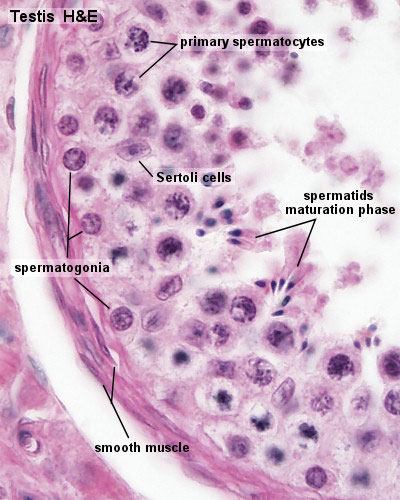
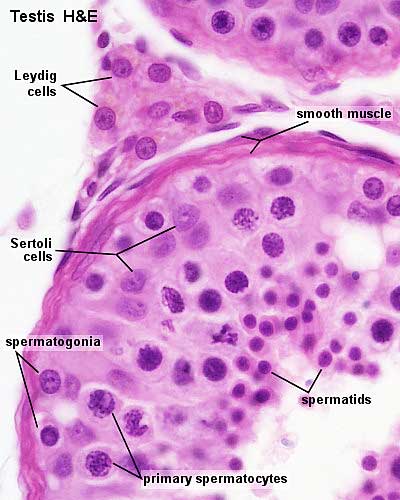
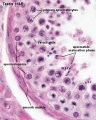
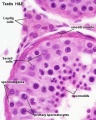
Seminiferous Tubule Histology
- Spermatogonia - are the first cells of spermatogenesis
- Primary spermatocytes - large, enter the prophase of the first meiotic division
- Secondary spermatocytes - small, complete the second meiotic division
- Spermatid - immature spermatozoa
- Spermatozoa - differentiated gamete
- Spermatozoa development: primordial germ cell - spermatogonia - primary spermatocyte - secondary spermatocytes - spermatid - spermatozoa
Other main cell types seen in the histological sections
- Sertoli cells- support cells seen within the seminiferous tubule
- Interstitial cells or Leydig cells - produce hormone
- Smooth muscle - surround seminiferous tubule and contribute to contraction of the tubule
Human Spermatozoa Development
- Spermatogenesis process of spermatagonia mature into spermatazoa (sperm).
- Continuously throughout life occurs in the seminiferous tubules in the male gonad- testis (plural testes).
- At puberty spermatagonia activate and proliferate (mitosis).
- about 48 days from entering meiosis until morphologically mature spermatozoa
- about 64 days to complete spermatogenesis, depending reproduction time of spermatogonia
- follicle stimulating hormone (FSH) - stimulates the spermatogenic epithelium
- luteinizing-hormone (LH) - stimulates testosterone production by Leydig cells
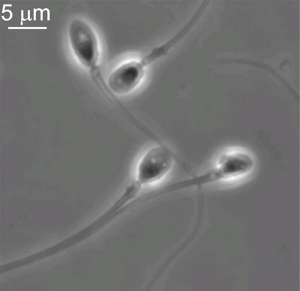
Mature Human Spermatozoa
Features:
| |
| File:spermatozoa animation icon.jpg</wikiflv> | The linked animation shows an overview of key structural components of spermatozoa. |
Links: Figure 20-22. Highly simplified drawing of a cross-section of a seminiferous tubule in a mammalian testis | Sperm Are Produced Continuously in Many Mammals | Figure 20-23. Cytoplasmic bridges in developing sperm cells and their precursors.
References
Reviews
- All you wanted to know about spermatogonia but were afraid to ask. de Rooij DG, Russell LD. J Androl. 2000 Nov-Dec;21(6):776-98. Review. PMID: 11105904 | PDF
Articles
Search
- NCBI Bookshelf spermatozoa | spermatogenesis | spermiogenesis
- Pubmed spermatozoa | spermatogenesis | spermiogenesis
Terms
asthenozoospermia
(asthenospermia) Term for reduced sperm motility and can be the cause of male infertility.
blood-testis barrier
(BTB) Formed by tight junctions, basal ectoplasmic specializations, desmosome-like junctions and gap junctions between adjacent Sertoli cells near the basement membrane of the seminiferous epithelium.
sperm annulus
(Jensen's ring; Latin, annulus = ring) A region of the mammalian sperm flagellum connecting the midpiece and the principal piece. The annulus is a septin-based structure formed from SEPT1, 4, 6, 7 and 12. Septins are polymerizing GTPases that can act as a scaffold forming hetero-oligomeric filaments required for cytokinesis and other cell cycle roles.
spermatogenesis
(Greek, genesis = origin, creation, generation) The term used to describe the process of diploid spermatagonia division and differentiation to form haploid spermatazoa within the testis (male gonad). The process includes the following cellular changes: meiosis, reoorganization of DNA, reduction in DNA content, reorganization of cellular organelles, morphological changes (cell shape). The final process of change in cell shape is also called spermiogenesis.
spermiogenesis
(Greek, genesis = origin, creation, generation) The maturation process of the already haploid spermatazoa into the mature sperm shape and organization. This process involves reorganization of cellular organelles (endoplasmic reticulum, golgi apparatus, mitochondria), cytoskeletal changes (microtubule organization) and morphological changes (cell shape, acrosome and tail formation).
spermatogonia
The cells located in the seminiferous tubule adjacent to the basal membrane that either divide and separate to renew the stem cell population, or they divide and stay together as a pair (Apr spermatogonia) connected by an intercellular cytoplasmic bridge to differentiate and eventually form spermatazoa.
Leydig cell
(interstitial cell) Male gonad (testis) cell which secrete the androgen testosterone, beginning in the fetus. These cells are named after Franz von Leydig (1821 - 1908) a German scientist who histologically described these cells.
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, June 27) Embryology Spermatozoa Development. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Spermatozoa_Development
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G