Talk:Menstrual Cycle
| About Discussion Pages |
|---|
On this website the Discussion Tab or "talk pages" for a topic has been used for several purposes:
Glossary Links
Cite this page: Hill, M.A. (2026, Mayıs 21) Embryology Menstrual Cycle. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Talk:Menstrual_Cycle |
Menstrual Cycle Graphs
- Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition. Walker HK, Hall WD, Hurst JW, editors. Boston: Butterworths; 1990. Birth Control | Figure 174.1 A 28-day menstrual cycle. Not all cycles are 28 days long. It is the phase before ovulation that varies in length.
2020
Hidalgo-Lopez E, Mueller K, Harris T, Aichhorn M, Sacher J & Pletzer B. (2020). Human menstrual cycle variation in subcortical functional brain connectivity: a multimodal analysis approach. Brain Struct Funct , , . PMID: 31894405 DOI.
Human menstrual cycle variation in subcortical functional brain connectivity: a multimodal analysis approach.
Abstract Increasing evidence suggests that endogenous sex steroid changes affect human brain functional connectivity, which could be obtained by resting-state fMRI (RS-fMRI). Nevertheless, RS studies on the menstrual cycle (MC) are underrepresented and yield inconsistent results. We attribute these inconsistencies to the use of various methods in exploratory approaches and small sample sizes. Hormonal fluctuations along the MC likely elicit subtle changes that, however, may still have profound impact on network dynamics when affecting key brain nodes. To address these issues, we propose a ROI-based multimodal analysis approach focusing on areas of high functional relevance to adequately capture these changes. To that end, sixty naturally cycling women underwent RS-fMRI in three different cycle phases and we performed the following analyses: (1) group-independent component analyses to identify intrinsic connectivity networks, (2) eigenvector centrality (EC) as a measure of centrality in the global connectivity hierarchy, (3) amplitude of low-frequency fluctuations (ALFF) as a measure of oscillatory activity and (4) seed-based analyses to investigate functional connectivity from the ROIs. For (2)-(4), we applied a hypothesis-driven ROI approach in the hippocampus, caudate and putamen. In the luteal phase, we found (1) decreased intrinsic connectivity of the right angular gyrus with the default mode network, (2) heightened EC for the hippocampus, and (3) increased ALFF for the caudate. Furthermore, we observed (4) stronger putamen-thalamic connectivity during the luteal phase and stronger fronto-striatal connectivity during the pre-ovulatory phase. This hormonal modulation of connectivity dynamics may underlie behavioural, emotional and sensorimotor changes along the MC. KEYWORDS: Amplitude of low-frequency fluctuations (ALFF); Eigenvector centrality mapping (ECM); Intrinsic connectivity networks (ICN); Menstrual cycle; Resting state; Seed-based connectivity PMID: 31894405 DOI: 10.1007/s00429-019-02019-z
2018
Subcortical structural changes along the menstrual cycle: beyond the hippocampus
Sci Rep. 2018 Oct 30;8(1):16042. doi: 10.1038/s41598-018-34247-4.
Pletzer B1, Harris T2, Hidalgo-Lopez E2.
Abstract
Animal studies have robustly shown hormone related changes in spine density in various brain areas, specifically the hippocampus. Literature on hormone dependent gray matter volume changes in humans is however less consistent. While various areas have been reported to change along the menstrual cycle in women, many do not survive multiple-comparisons correction and only hippocampal changes have been replicated. We attribute these problems to small sample sizes and inconsistent definitions of menstrual cycle phases. In the present study a large sample of 55 women was scanned three times along their menstrual cycle in concisely defined time windows of hormonal changes. Accordingly this is the first study using a large enough sample size to assess menstrual cycle dependent changes in human brain structure with sufficient power. Results confirm a significant estradiol-dependent pre-ovulatory increase in gray matter volumes of the bilateral hippocampus, but also show a significant, progesterone-dependent increase in gray matter volumes of the right basal ganglia after ovulation. No other areas were affect by hormonal changes along the menstrual cycle. These hormone driven menstrual cycle changes in human brain structure are small, but may be the underlying cause of menstrual cycle dependent changes in cognition and emotion. PMID: 30375425 PMCID: PMC6207699 DOI: 10.1038/s41598-018-34247-4
2017
A Theory for the Origin of Human Menopause
Front Genet. 2017 Jan 6;7:222. doi: 10.3389/fgene.2016.00222. eCollection 2016.
Takahashi M1, Singh RS1, Stone J1.
Abstract
A complete and compelling evolutionary explanation for the origin of human menopause is wanting. Menopause onset is defined clinically as the final menses, confirmed after 1 year without menstruation. The theory proposed herein explains at multiple levels - ultimately genetic but involving (1) behavioral, (2) life history, and (3) social changes - the origin and evolution of menopause in women. Individuals in Lower Paleolithic human populations were characterized by short lifespans with diminished late-age survival and fertility, similar to contemporary chimpanzees, and thence were subject to three changes. (1) A mating behavior change was established in which only young women reproduced, thereby rendering as effectively neutral female-specific late-onset fertility-diminishing mutations, which accumulated subsequently. (2) A lifespan increase was manifested adaptively, revealing the reproductive senescence phenotype encoded in late-onset fertility-diminishing mutation genotypes, which, heretofore, had been unexpressed in the shorter lifespan. (3) A social interaction change emerged exaptively, when older non-reproductive women exclusively started assisting in rearing grandchildren rather than giving birth to and caring for their own children, ultimately leading to menstrual cycle cessation. The changes associate in a one-to-one manner with existing, non-mutually exclusive hypotheses for the origin of human menopause. Evidence for each hypothesis and its associated change having occurred are reviewed, and the hypotheses are combined in a synthetic theory for the origin of human menopause. The new theory simultaneously addresses the main theoretical problem with each hypothesis and yields predictions for future testing. KEYWORDS: adaptation; exaptation; fertility; genetic theory; lifespan; mating behavior; neutral evolution; senescence
PMID 28111590 PMCID: PMC5216033 DOI: 10.3389/fgene.2016.00222
2016
PLoS One. 2016 Dec 16;11(12):e0168402. doi: 10.1371/journal.pone.0168402. eCollection 2016. Menstrual Cycle Irregularity and Metabolic Disorders: A Population-Based Prospective Study. Rostami Dovom M1, Ramezani Tehrani F1, Djalalinia S2, Cheraghi L3, Behboudi Gandavani S1, Azizi F4. Author information Abstract The regularity of menstrual cycles is considered an indicator of women's reproductive health. Previous studies with a cross-sectional design have documented the relationship between menstrual cycle irregularities, insulin-resistance and the future risks for metabolic disorders. Limited data documented by prospective studies can lead to premature conclusions regarding the relationship between menstrual cycle irregularities and other conditions influencing women's health. The present study therefore, using a prospective design aimed to assess the risk of metabolic disorders in women with a history of irregular menstrual cycles, was based on the data gathered from the Tehran Lipid and Glucose study (TLGS) an ongoing prospective cohort study initiated in 1999. Participants of the current study were 2128 women, aged between 18-49 years, followed for 15 years. Based on their menstrual cycles, the women were divided into two groups: (i) women with regular menstrual cycles (n = 1749), and (ii) those with irregular menstrual cycles (n = 379). The proportional COX regression model was used to compare hazard ratios (HRs) between the groups for the proposed events, including diabetes mellitus (DM), pre-diabetes (pre-DM), hypertension (HTN), pre-hypertension (pre-HTN) and dyslipidemia. It was found that during a 15-year follow up, there were 123 cases of DM, 456 cases of pre-DM, 290 cases of HTN, 481 cases of pre-HTN, and 402 cases of dyslipidemia. Compared to those with regular cycles, women with irregular menstrual cycles were found to have an increased risk for DM2 (age adjusted Hazard Ratios (HRs), 2.01; 95% confidence intervals (CI:1.59-3.50), the increased risk for DM, associated with irregular cycles remained significant after the adjustment for Body Mass Index (BMI), fasting blood sugar (FBS), family history of diabetes, and parity (HRS, 1.73; 95% CI: 1.14-2.64). There was no significant difference in the increased risk for pre-DM between the groups (age adjusted HRs, 1.33, 95% CI: 1.05-1.69). However, after the adjustment of BMI, FBS and family history of pre-DM, compared to those with regular menstrual cycles, irregular menstrual cycles showed an increased risk for pre-DM (HRs, 1.33; 95% CI: 1.05-1.69). No statistically significant difference was found in the increasing risk for other proposed events between the groups demonstrating that menstrual cycle irregularities could be considered a marker of metabolic disorders and a predisposing factor of the increased risk for diabetes mellitus and pre-diabetes in women with irregular menstrual cycles. PMID: 27992506 PMCID: PMC5161370 DOI: 10.1371/journal.pone.0168402
2012
Stromal-to-epithelial transition during postpartum endometrial regeneration
PLoS One. 2012;7(8):e44285. doi: 10.1371/journal.pone.0044285. Epub 2012 Aug 27.
Huang CC, Orvis GD, Wang Y, Behringer RR. Author information
Abstract
Endometrium is the inner lining of the uterus which is composed of epithelial and stromal tissue compartments enclosed by the two smooth muscle layers of the myometrium. In women, much of the endometrium is shed and regenerated each month during the menstrual cycle. Endometrial regeneration also occurs after parturition. The cellular mechanisms that regulate endometrial regeneration are still poorly understood. Using genetic fate-mapping in the mouse, we found that the epithelial compartment of the endometrium maintains its epithelial identity during the estrous cycle and postpartum regeneration. However, whereas the stromal compartment maintains its identity during homeostatic cycling, after parturition a subset of stromal cells differentiates into epithelium that is subsequently maintained. These findings identify potential progenitor cells within the endometrial stromal compartment that produce long-term epithelial tissue during postpartum endometrial regeneration.
PMID 22970108
The nerve of ovulation-inducing factor in semen
Proc Natl Acad Sci U S A. 2012 Sep 11;109(37):15042-7. Epub 2012 Aug 20.
Ratto MH, Leduc YA, Valderrama XP, van Straaten KE, Delbaere LT, Pierson RA, Adams GP. Source Faculty of Veterinary Sciences and Faculty of Agricultural Sciences, Universidad Austral de Chile, Valdivia, Chile.
Abstract
A component in seminal fluid elicits an ovulatory response and has been discovered in every species examined thus far. The existence of an ovulation-inducing factor (OIF) in seminal plasma has broad implications and evokes questions about identity, tissue sources, mechanism of action, role among species, and clinical relevance in infertility. Most of these questions remain unanswered. The goal of this study was to determine the identity of OIF in support of the hypothesis that it is a single distinct and widely conserved entity. Seminal plasma from llamas and bulls was used as representative of induced and spontaneous ovulators, respectively. A fraction isolated from llama seminal plasma by column chromatography was identified as OIF by eliciting luteinizing hormone (LH) release and ovulation in llamas. MALDI-TOF revealed a molecular mass of 13,221 Da, and 12-23 aa sequences of OIF had homology with human, porcine, bovine, and murine sequences of β nerve growth factor (β-NGF). X-ray diffraction data were used to solve the full sequence and structure of OIF as β-NGF. Neurite development and up-regulation of trkA in phaeochromocytoma (PC(12)) cells in vitro confirmed NGF-like properties of OIF. Western blot analysis of llama and bull seminal plasma confirmed immunorecognition of OIF using polyclonal mouse anti-NGF, and administration of β-NGF from mouse submandibular glands induced ovulation in llamas. We conclude that OIF in seminal plasma is β-NGF and that it is highly conserved. An endocrine route of action of NGF elucidates a previously unknown pathway for the direct influence of the male on the hypothalamo-pituitary-gonadal axis of the inseminated female.
PMID 22908303
Follicle-Stimulating Hormone Accelerates Mouse Oocyte Development In Vivo
Biol Reprod. 2012 Apr 18. [Epub ahead of print]
Demeestere I, Streiff AK, Suzuki J, Al-Khabouri S, Mahrous E, Tan SL, Clarke HJ. Abstract During folliculogenesis, oocytes grow and acquire developmental competence in a mutually dependent relationship with their adjacent somatic cells. Follicle-stimulating hormone (FSH) plays an essential and well-established role in the differentiation of the somatic follicular cells, but its function in the development of the oocyte has still not been elucidated. We report here the oocytes of Fshb(-/-) mice, which cannot produce FSH, grow at the same rate and reach the same size as those of wild-type mice. Consistent with this observation, the granulosa cells of Fshb(-/-) mice express the normal quantity of mRNA encoding Kit ligand, which has been implicated in oocyte growth. Oocytes of Fshb(-/-) mice also accumulate normal quantities of cyclin B1 and CDK1 proteins and mitochondrial DNA. Moreover, they acquire the ability to complete meiotic maturation in vitro and undergo the transition from non-surrounded nucleolus to surrounded nucleolus. However, these events of late oocyte development are significantly delayed. Following in vitro maturation and fertilization, however, only a small number of embryos derived from oocytes of Fshb(-/-) mice reach the blastocyst stage. Administration of equine chorionic gonadotropin, which provides FSH activity, 48 h before in vitro maturation increases the number of blastocysts subsequently obtained. These results indicate that FSH is not absolutely required for oocyte development in vivo but this process occurs more rapidly in its presence. We suggest that FSH may coordinate the development of the germ-line and somatic compartments of the follicle, ensuring that ovulation releases a developmentally competent egg.
PMID 22517620
Anti-mullerian hormone: a potential new tool in epidemiologic studies of female fecundability
Am J Epidemiol. 2012 Feb 15;175(4):245-9. Epub 2012 Jan 12.
Baird DD, Steiner AZ.
Abstract
The objective of the present commentary is to suggest that epidemiologists explore the use of anti-Müllerian hormone (AMH) as a new measurement tool in fecundability studies. The authors briefly summarize the advantages and limitations of the 3 current approaches to studies of fecundability. All 3 approaches involve the collection of time-to-pregnancy or attempt-time data, and most are limited to participants who plan their pregnancies. AMH is produced by ovarian follicles during their early growth stages and is measured clinically to assess ovarian reserve (the number of remaining oocytes). Unlike time to pregnancy, serum AMH level can be assessed regardless of pregnancy-attempt status. Measurements are not significantly affected by phase of the menstrual cycle, oral contraceptive use, or early pregnancy. The authors suggest that AMH measurement can be a valuable addition to traditionally designed fecundability studies. In addition, this hormone should be investigated as an independent measure of fecundability in studies that focus on exposures hypothesized to target the ovary.
PMID 22247047
2011
Age at menarche, menstrual characteristics, and risk of preeclampsia
ISRN Obstet Gynecol. 2011;2011:472083. Epub 2011 Dec 29.
Abetew DF, Enquobahrie DA, Dishi M, Rudra CB, Miller RS, Williams MA. Source Center for Perinatal Studies, Swedish Medical Center, Seattle, WA 98104, USA. Abstract We examined associations of age at menarche and menstrual characteristics with the risk of preeclampsia among participants (n = 3,365) of a pregnancy cohort study. Data were collected using in-person interviews and medical record abstraction. Logistic regression was used to estimate adjusted odds ratio (OR) and 95% confidence interval (95% CI). There was a significant inverse association between age at menarche and risk of preeclampsia (P value for trend < 0.05). Association of long cycle length (>36 days) with higher risk of preeclampsia was present only among women who had prepregnancy body mass index <25 kg/m(2) (interaction P value = 0.04). Early menarche is associated with higher risk of preeclampsia. Prepregnancy weight may modify associations of long menstrual cycles with risk of preeclampsia.
PMID 22263114
A study on the menstruation of Korean adolescent girls in Seoul
Korean J Pediatr. 2011 May;54(5):201-6. Epub 2011 May 31.
Lee JC, Yu BK, Byeon JH, Lee KH, Min JH, Park SH. Source Department of Pediatrics, Korea University School of Medicine, Seoul, Korea.
Abstract
PURPOSE: Westernized eating habits have been associated with early-age menstruation, which increases the incidence of dysmenorrhea and premenstrual syndrome among adolescent girls. We therefore surveyed changes in menarche timing and the general menstrual characteristics of adolescent girls in Seoul, Korea.
METHODS: We surveyed 538 teenage girls who visited our hospital between July and November 2007. Items explored included age at menarche, general menstrual characteristics, occurrence of premenstrual syndrome and treatment thereof, and an association between present dysmenorrhea and a family history of the condition.
RESULTS: Average age at menarche was 12.6 years, with 29% (n=156) subjects beginning menstruation at age 12 years. The prevalence of dysmenorrhea was 82% (n=435). The main symptoms were abdominal (53.2%) and lower back pain (34.2%), and 15.2% of girls who experienced such symptoms required medication. Present dysmenorrhea, and a family history thereof, were statistically correlated (P<0.05). In addition, 58.8% (n=316) of teenage girls had symptoms of premenstrual syndrome. The most frequent psychological symptoms were fatigue (36.4%) and nervousness (38.7%), whereas the most common physical symptom was menstrual cramps (46.5%). Most subjects (87.6%) tolerated the symptoms of premenstrual syndrome without medication; 11.4% took medicines including painkillers; but only 0.1% of subjects visited a doctor.
CONCLUSION: The average age at menarche in Korean girls was 12.6 years, thus younger than in the past. Most teenage girls experienced dysmenorrhea and premenstrual syndrome, but few consulted a doctor. Organized treatment plans are required to manage menstrual problems in teenage girls.
- "In Korea, research on the age of menarche commenced in 192325), and has continued since that time. Mean age at menarche has generally decreased; from 14.8 years in 1962 to about 14 years in 1973, 14.4 years in 1979, 13.4 years in 1986, 12.5 years in 1988, and 12.4±1.1 years in 199326). Regionally, age at menarche was 1 year earlier in Seoul than in other regions of Korea27). Age at menarche was 16.2 years in urban women and 16.3 years in rural women28), and 13.4 years in women living in large cities and 13.7 years in those residing in small cities or rural areas29). We found that the mean age at menarche was 12.6 years, confirming the recent trend toward earlier menarche in Koreans. Also, age at menarche did not differ greatly from that in European nations or the USA."
PMID: 21829411 http://www.ncbi.nlm.nih.gov/pubmed/21829411 http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3145904
Reconstruction of endometrium from human endometrial side population cell lines
PLoS One. 2011;6(6):e21221. Epub 2011 Jun 21. Cervelló I, Mas A, Gil-Sanchis C, Peris L, Faus A, Saunders PT, Critchley HO, Simón C. Source Fundación IVI-Instituto Universitario IVI, Universidad de Valencia, INCLIVA, Valencia, Spain.
Abstract
Endometrial regeneration is mediated, at least in part, by the existence of a specialized somatic stem cell (SSC) population recently identified by several groups using the side population (SP) technique. We previously demonstrated that endometrial SP displays genotypic, phenotypic and the functional capability to develop human endometrium after subcutaneous injection in NOD-SCID mice. We have now established seven human endometrial SP (hESP) cell lines (ICE 1-7): four from the epithelial and three from the stromal fraction, respectively. SP cell lines were generated under hypoxic conditions based on their cloning efficiency ability, cultured for 12-15 passages (20 weeks) and cryopreserved. Cell lines displayed normal 46XX karyotype, intermediate telomerase activity pattern and expressed mRNAs encoding proteins that are considered characteristic of undifferentiated cells (Oct-4, GDF3, DNMT3B, Nanog, GABR3) and those of mesodermal origin (WT1, Cardiac Actin, Enolase, Globin, REN). Phenotype analysis corroborated their epithelial (CD9+) or stromal (vimentin+) cell origin and mesenchymal (CD90+, CD73+ and CD45-) attributes. Markers considered characteristic of ectoderm or endoderm were not detected. Cells did not express either estrogen receptor alpha (ERα) or progesterone receptor (PR). The hESP cell lines were able to differentiate in vitro into adipocytes and osteocytes, which confirmed their mesenchymal origin. Finally, we demonstrated their ability to generate human endometrium when transplanted beneath the renal capsule of NOD-SCID mice. These findings confirm that SP cells exhibit key features of human endometrial SSC and open up new possibilities for the understanding of gynecological disorders such as endometriosis or Asherman syndrome. Our cell lines can be a valuable model to investigate new targets for endometrium proliferation in endometriosis.
PMID: 21712999 PMCID: PMC3119688 http://www.ncbi.nlm.nih.gov/pubmed/21712999
http://www.plosone.org/article/info%3Adoi%2F10.1371%2Fjournal.pone.0021221
The normal menstrual cycle in women
Anim Reprod Sci. 2011 Apr;124(3-4):229-36. Epub 2010 Sep 3.
Mihm M, Gangooly S, Muttukrishna S. Source Division of Cell Sciences, Faculty of Veterinary Medicine, University of Glasgow, Glasgow, UK.
Abstract
The menstrual cycle in women is characterised by high variability in cycle length (26-35 days), 5-day menses, a fertile phase from 5 days before to the day of ovulation, and low fertility which is dependent on cycle length and age. All women show an FSH rise at the luteal-follicular transition, stimulating a cohort of follicular growth and inhibin B secretion in the early follicular phase. The ovulatory dominant follicle (DF) is selected in the mid-follicular phase, and as this DF grows it increasingly secretes oestradiol and inhibin A for a week before ovulation. Gonadotrophin responsiveness, IGF binding protein expression and degradation, and vascularisation have been identified to be crucial for DF selection and progression. Two-thirds of women show two follicle waves and 1/3 show 3 follicle waves per cycle. Three-wave women have longer cycles, and a later oestradiol rise and LH surge. The corpus luteum secretes progesterone, oestradiol and inhibin A in response to LH pulses, and reaches its peak in terms of size, secretions, and vascularization 6-7 days after ovulation. Luteal regression is passive and independent of the uterus, but can be prevented by hCG, the luteotrophic signal from the trophoblast, from 8 days after conception. Reductions in systemic steroid and protein hormone concentrations may be responsible for the FSH rise characteristic of premenopausal women. The functional layer of the endometrium shows steroid hormone-dependent proliferation, differentiation, and shedding in the absence of the trophoblast. Menstruation is initiated by progesterone responsive decidual cells, and executed by PGE and PGF2α, vasoconstriction and matrix metalloprotease secretion by leukocytes. Ovarian function and also hormone fluctuations during the menstrual cycle are similar to oestrous cycles of cows and mares, justifying research into comparative aspects of menstrual and oestrous cycles in monovulatory species.
Copyright © 2010 Elsevier B.V. All rights reserved.
PMID: 20869180 http://www.ncbi.nlm.nih.gov/pubmed/20869180
Decidualization and angiogenesis in early pregnancy: unravelling the functions of DC and NK cells
J Reprod Immunol. 2011 Mar;88(2):86-92. Epub 2011 Jan 11.
Blois SM, Klapp BF, Barrientos G. Source Charité Centrum 12 für Innere Medizin und Dermatologie, Reproductive Immunology Research Group, University Medicine of Berlin, Germany. sandra.blois@charite.de
Abstract
Differentiation of endometrial stromal cells and formation of new maternal blood vessels at the time of embryo implantation are critical for the establishment and maintenance of gestation. The regulatory functions of decidual leukocytes during early pregnancy, particularly dendritic cells (DC) and NK cells, may be important not only for the generation of maternal immunological tolerance but also in the regulation of stromal cell differentiation and the vascular responses associated with the implantation process. However, the specific contributions of DC and NK cells during implantation are still difficult to dissect mainly due to reciprocal regulatory interactions established between them within the decidualizing microenvironment. The present review article discusses current evidence on the regulatory pathways driving decidualization in mice, suggesting that NK cells promote uterine vascular modifications that assist decidual growth but DC directly control stromal cell proliferation, angiogenesis and the homing and maturation of NK cell precursors in the pregnant uterus. Thus, successful implantation appears to result from an interplay between cellular components of the decidualizing endometrium involving immunoregulatory and pro-angiogenic functions of DC and NK cells.
Copyright © 2010 Elsevier Ireland Ltd. All rights reserved.
PMID: 21227511
Comprehensive analysis of leukocytes, vascularization and matrix metalloproteinases in human menstrual xenograft model
PLoS One. 2011 Feb 17;6(2):e16840.
Guo Y, He B, Xu X, Wang J.
Graduate School, Peking Union Medical College, Beijing, People's Republic of China. Abstract In our previous study, menstrual-like changes in mouse were provoked through the pharmacologic withdrawal of progesterone with mifepristone following induction of decidualization. However, mouse is not a natural menstruation animal, and the menstruation model using external stimuli may not truly reflect the occurrence and development of the human menstrual process. Therefore, we established a model of menstruation based on human endometrial xenotransplantation. In this model, human endometrial tissues were transplanted subcutaneously into SCID mice that were ovarectomized and supplemented with estrogen and progestogen by silastic implants with a scheme imitating the endocrinological milieu of human menstrual cycle. Morphology, hormone levels, and expression of vimentin and cytokeratin markers were evaluated to confirm the menstrual-like changes in this model. With 28 days of hormone treatment, transplanted human endometrium survived and underwent proliferation, differentiation and disintegration, similar to human endometrium in vivo. Human CD45+ cells showed a peak of increase 28 days post-transplantation. Three days after progesterone withdrawal, mouse CD45+ cells increased rapidly in number and were significantly greater than human CD45+ cell counts. Mouse CD31+ blood vascular-like structures were detected in both transplanted and host tissues. After progesterone withdrawal, the expression levels of matrix metalloproteinases (MMP) 1, 2, and 9 were increased. In summary, we successfully established a human endometrial xenotransplantation model in SCID mice, based on the results of menstrual-like changes in which MMP-1, 2 and 9 are involved. We showed that leukocytes are originated from in situ proliferation in human xenografts and involved in the occurrence of menstruation. This model will help to further understand the occurrence, growth, and differentiation of the endometrium and the underlying mechanisms of menstruation.
PMID: 21379384 http://www.ncbi.nlm.nih.gov/pubmed/21379384
2010
Characterization of chaotic dynamics in the human menstrual cycle
Nonlinear Biomed Phys. 2010 Oct 5;4(1):5.
Derry G, Derry P. Source Department of Physics, Loyola University Maryland, Baltimore, MD 21210, USA. gderry@loyola.edu. Abstract ABSTRACT:
BACKGROUND: The human menstrual cycle is known to exhibit a significant amount of unexplained variability. This variation is typically dismissed as random fluctuations in an otherwise periodic and predictable system. Given the many delayed nonlinear feedbacks in the multiple levels of the reproductive endocrine system, however, the menstrual cycle can properly be construed as the output of a nonlinear dynamical system, and such a system has the possibility of being in a chaotic trajectory. We hypothesize that this is in fact the case and that it accounts for the observed variability.
RESULTS: Here, we test this hypothesis by performing time series analyses on data for 7749 menstrual cycles from 40 women in the 20-40 year age range, using the database maintained by the Tremin Research Program on Women's Health. Both raw menstrual cycle length data and a formal time series constructed from this data are utilized in these analyses. Employing phase space reconstruction techniques with a maximum embedding dimension of 12, we find appropriate scaling behavior in the correlation sums for these data, indicating low dimensional deterministic dynamics. A correlation dimension of Dc ≈ 5.2 is measured in the scaling regime. This result is confirmed by recalculation using the Takens estimator and by surrogate data tests. We interpret this result as an approximation to the fractal dimension of a strange attractor governing chaotic dynamics in the menstrual cycle. We also use the time series to calculate the correlation entropy (K2 ≈ 0.008/τ) and the maximal Lyapunov exponent (λ ≈ 0.005/τ) for the system, where τ is the sampling time of the series.
CONCLUSIONS: Taken collectively, these results constitute significant evidence that the menstrual cycle is the result of chaos in a nonlinear dynamical system. This view of the menstrual cycle has potential implications for clinical practice, modelling of the endocrine system, and the interpretation of the perimenopausal transition.
Figure 1 Examples of data. Menstrual cycle length data during 20-40 year age interval, illustrating typical observed variability (A) http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2959058/figure/F1/
PMID: 20923559 http://www.ncbi.nlm.nih.gov:80/pubmed/20923559
Menstrual cycle and hormonal contraceptive use modulate human brain structure
Brain Res. 2010 Aug 12;1348:55-62. Epub 2010 Jun 13.
Pletzer B, Kronbichler M, Aichhorn M, Bergmann J, Ladurner G, Kerschbaum HH.
Department of Cell Biology, Paris-Lodron-University Salzburg, Hellbrunnerstrasse 34, 5020 Salzburg, Austria. Belinda.Pletzer@sbg.ac.at Abstract Sex differences in human brain structure have repeatedly been described, but results are inconsistent. However, these studies hardly controlled for cycle phase of women or the use of hormonal contraceptives. Our study shows that these factors are not negligible, but have a considerable influence on human brain structure. We acquired high-resolution structural images from the brains of 14 men, 14 women, who did not use, and 14 women, who did use hormonal contraceptives. Women, who did not use hormonal contraceptives, were scanned twice, once during their early follicular and once during their mid-luteal cycle-phase. Regional gray matter volumes were compared by voxel-based morphometry. Men had larger hippocampi, parahippocampal and fusiform gyri, amygdalae and basal ganglia than women. Women showed larger gray matter volumes in the prefrontal cortex, pre- and postcentral gyri. These sex-dependent effects were modulated by menstrual cycle phases and hormonal contraceptives. We found larger volumes in the right fusiform/parahippocampal gyrus during early follicular compared to mid-luteal cycle phase. Women using hormonal contraceptives showed significantly larger prefrontal cortices, pre- and postcentral gyri, parahippocampal and fusiform gyri and temporal regions, compared to women not using contraceptives.
PMID: 20550945
http://www.ncbi.nlm.nih.gov/pubmed/20550945
2009
Ovarian aging: mechanisms and clinical consequences
Endocr Rev. 2009 Aug;30(5):465-93. Epub 2009 Jul 9.
Broekmans FJ, Soules MR, Fauser BC.
Department of Reproductive Medicine and Gynecology, University Medical Center, Utrecht, The Netherlands. f.broekmans@umcutrecht.nl Abstract Menopause is the final step in the process referred to as ovarian ageing. The age related decrease in follicle numbers dictates the onset of cycle irregularity and the final cessation of menses. The parallel decay in oocyte quality contributes to the gradual decline in fertility and the final occurrence of natural sterility. Endocrine changes mainly relate to the decline in the negative feedback from ovarian factors at the hypothalamo-pituitary unit. The declining cohort of antral follicles with age first results in gradually elevated FSH levels, followed by subsequent stages of overt cycle irregularity. The gradual decline in the size of the antral follicle cohort is best represented by decreasing levels of anti-Mullerian hormone. The variability of ovarian ageing among women is evident from the large variation in age at menopause. The identification of women who have severely decreased ovarian reserve for their age is clinically relevant. Ovarian reserve tests have appeared to be fairly accurate in predicting response to ovarian stimulation in the assisted reproductive technology (ART) setting. The capacity to predict the chances for spontaneous pregnancy or pregnancy after ART appears very limited. As menopause and the preceding decline in oocyte quality seem to have a fixed time interval, tests that predict the age at menopause may be useful to assess individual reproductive lifespan. Especially genetic studies, both addressing candidate gene and genome wide association, have identified several interesting loci of small genetic variation that may determine fetal follicle pool development and subsequent wastage of his pool over time. Improved knowledge of the ovarian ageing mechanisms may ultimately provide tools for prediction of menopause and manipulation of the early steps of folliculogenesis for the purpose of contraception and fertility lifespan extension.
PMID: 19589949
Human studies on genetics of the age at natural menopause: a systematic review
Abstract
BACKGROUND Timing of natural menopause has great implications for fertility and women's health. Age at natural menopause (ANM) is largely influenced by genetic factors. In the past decade, several genetic studies have been conducted to identify genes in ANM, which can help us unravel the biological pathways underlying this trait and the associated infertility and health risks. After providing an overview of the results of the genetic studies performed so far, we give recommendations for future studies in identifying genetic factors involved in determining the variation in timing of natural menopause.
METHODS The electronic databases of Pubmed and Embase were systematically searched until September 2009 for genetic studies on ANM, using relevant keywords on the subject. Additional papers identified through hand search were also included.
RESULTS Twenty-eight papers emerged from our literature search. A number of genetic regions and variants involved in several possible pathways underlying timing of ANM were identified, including two possible interesting regions (9q21.3 and chromosome 8 at 26 cM) in linkage analyses. Recent genome-wide association studies have identified two genomic regions (19q13.42 and 20p12.3), containing two promising candidate genes (BRKS1 and MCM). In the candidate gene association studies on ANM, very few consistent associations were found.
CONCLUSION A number of genetic variants have been discovered in association with ANM, although the overall results have been rather disappointing. We have described possible new strategies for future genetic studies to identify more genetic loci involved in the variation in menopausal age.
http://humupd.oxfordjournals.org/content/16/4/364.abstract
PMID: 20071357
Expression of nodal signalling components in cycling human endometrium and in endometrial cancer
http://www.rbej.com/content/7/1/122
2005
Ultrasound image attributes of human ovarian dominant follicles during natural and oral contraceptive cycles
Reprod Biol Endocrinol. 2005 Apr 13;3:12. Birtch RL, Baerwald AR, Olatunbosun OA, Pierson RA. Source Department of Obstetrics, Gynecology and Reproductive Sciences, College of Medicine, University of Saskatchewan, Saskatoon, Saskatchewan, Canada. birtch@erato.usask.ca
Abstract
BACKGROUND: Computer-assisted analyses were used to examine ultrasound image attributes of human dominant ovarian follicles that developed during natural and oral contraceptive (OC) cycles. We hypothesized that image attributes of natural cycle follicles would quantitatively differ from those in OC cycles and that OC cycle follicles would possess image attributes indicative of atresia.
METHODS: Dominant ovarian follicles of 18 clinically normal women were compared using transvaginal ultrasonography for the 7 days before ovulation during a natural cycle (n = 9) or the 7 days before peak estradiol in women using OC (n = 11). Follicles were analyzed using region and line techniques designed to compare the image attributes numerical pixel value (NPV), pixel heterogeneity (PH) and area under the curve (AUC).
RESULTS: NPV was higher in OC cycle follicles with region analysis and tended to be higher with line analysis (p = 0.005 and p = 0.06, respectively). No differences were observed in two other image attributes (AUC and PH), measured with either technique, between natural and OC cycle follicles.
CONCLUSION: The increased NPV value of OC cycle follicles and lack of differences in PH and AUC values between natural cycle and OC cycle follicles did not support the hypothesis that OC cycle follicles would show ultrasonographically detectable signs of atresia. Image attributes observed in OC cycle follicles were not clearly indicative of atresia nor were they large enough to preclude preovulatory physiologic status in OC cycle follicles.
PMID: 15829004 http://www.ncbi.nlm.nih.gov/pubmed/15829004
2002
Yasmin: the reason why
Eur J Contracept Reprod Health Care. 2002 Dec;7 Suppl 3:13-8; discussion 42-3.
Thorneycroft IH.
Mobile Ob-Gyn Center, Lunar Research and Department of Obstetrics and Gynecology, University of South Alabama College of Medicine, Alabama 36607, USA. Abstract Oral contraceptives have been available for a little over 40 years and, during that time, many different formulations have been introduced. There have been dramatic dosage reductions of both the estrogen and progestogen components and various progestogens have been introduced over time. The properties of most progestogens used in oral contraceptives are very similar, differing mainly in potency. Oral contraceptives with progestogens having new and unique properties are needed. World-wide, around 20-30% of women of childbearing age use oral contraceptives and their use declines after the age of 35 years, with an accompanying increase in the rates of unintended pregnancy and elective termination. Incorrect use likewise gives rise to high unintended pregnancy rates. Use in Europe is higher than in other regions. Discontinuation because of unwanted effects and misperceptions is very common. Common misperceptions that prevent women from initiating oral contraceptive use are weight gain, cancer risks and that bleeding indicates a significant problem. Unwanted effects that commonly give rise to discontinuation are bleeding, nausea, weight gain, mood changes, breast tenderness and headaches. Discontinuation rates are high, particularly in the first year, and adolescents have the highest rates of discontinuation. Correct consistent use must be encouraged by taking pills at a regular time each day and by reinforcing that bleeding and other unwanted effects are not medically serious. Reinforcement of the non-contraceptive health benefits is very important and it needs to be emphasized that long-term use enhances these non-contraceptive benefits. Most non-contraceptive benefits are due to the progestogen component and its inhibition of ovulation. The new drospirenone-containing oral contraceptive (Yasmin, Schering AG, Berlin, Germany) offers the traditional non-contraceptive benefits; however, due to its unique antimineralocorticoid and antiandrogenic properties, new and unique benefits have been observed. Acne is well controlled, as would be expected from its inhibition of ovulation, antiandrogenic activity and lack of attenuation of the estrogen-mediated increase in sex hormone binding globulin. Its antimineralocorticoid activity gives rise to a reduction in fluid-related symptoms. The oral contraceptive containing 3 mg drospirenone with 30 microg ethinylestradiol DRSP/EE) has excellent efficacy since drospirenone is a potent progestogen, the corrected Pearl index being 0.09. This index is lower than those of many other oral contraceptives. Cycle control is excellent and comparable to that experienced with other oral contraceptives. A significant and consistent weight loss was seen with DRSP/EE compared to a reference preparation containing desogestrel. Day-to-day compliance and the duration of intake of an oral contraceptive are dependent on the woman's satisfaction with the pill she is taking. DRSP/EE meets these expectations and, with its new and unique non-contraceptive benefits, offers a real new choice to women.
PMID: 12659402
1998
Oxytocin and vasopressin receptors in human and uterine myomas during menstrual cycle and early pregnancy
Hum Reprod Update. 1998 Sep-Oct;4(5):594-604.
Fuchs AR, Behrens O, Maschek H, Kupsch E, Einspanier A.
Department of Obstetrics and Gynecology, Cornell University Medical College, New York, NY 10021, USA. annariitta@aol.com Abstract The purpose of this study was to determine the specificity and concentration of oxytocin (OT) and arginine vasopressin (AVP) binding sites in non-pregnant (NP) human and rhesus monkey endometrium, myometrium and fibromyomas, and to determine the cellular localization of OT receptor (OTR). Besides [3H]AVP, [125I]LVA, a specific VP1 receptor subtype antagonist, was used to determine vasopressin receptor (VPR) concentrations. Samples were obtained from 42 pre-menopausal and three pregnant women (5, 13 and 35 weeks gestation), and several NP and pregnant monkeys. Specificity of binding was assessed in competition experiments with unlabelled agonists and antagonists of known pharmacological potency. Cellular localization of OTR was determined by immunohistochemistry. In NP human uterine tissues, [3H]AVP was bound with higher affinity and greater binding capacity than [3H]OT, whereas in pregnant women and in NP and pregnant rhesus monkeys, uterine OT binding capacity was greater. OT and AVP binding sites discriminated very poorly between OT and AVP; [125I]LVA binding sites were more selective than [3H]AVP. Their ligand specificity and binding kinetics indicated the presence of two distinct populations of binding sites for OT and AVP in primate uterus. Endometrium of NP women and monkeys had low OTR and VPR concentrations. Myometrial and endometrial OTR and VPR were down-regulated in midcycle and in early human pregnancy, they were up-regulated in the secretory phase and second half of pregnancy. Immunoreactive OTR in NP uterus was localized in patches of myometrial muscle cells and small numbers of endometrial epithelial cells.
PMID: 10027613
1996
Contralateral selection of dominant follicle favours pre-embryo development
Hum Reprod. 1996 Sep;11(9):1958-62.
Fukuda M, Fukuda K, Andersen CY, Byskov AG. Source Fukuda Ladies Clinic, Hyogo, Japan.
Abstract
Ovulation was studied using vaginosonography in a total of 410 natural cycles of 123 women undergoing infertility treatment [267 intrauterine insemination (IUI) cycles of 103 women and 143 in-vitro fertilization (IVF) cycles of 50 women]. None of the women received ovarian stimulation. Each follicle was measured daily from 14 mm in diameter until formation of corpus luteum or oocyte retrieval. Contralateral ovulation as compared with the preceding cycle occurred in 57% of the 410 cycles. Contralateral ovulations occurred in 72% of cycles with a follicular phase < 13 days. In cycles with a follicular phase of > 14 days, ovulations occurred at random. The length of follicular phase in contralateral ovulation cycles (15.2 +/- 3.2 days) was significantly (P < 0.05) shorter than that of ipsilateral ovulation cycles (15.8 +/- 2.8). During the 57% contralateral ovulations in 143 IVF cycles, the rates of oocyte retrieval (89%), fertilization (69%), cleavage (90%) and embryo transfer (56%) were significantly higher than those of ipsilateral ovulations (69, 51, 64 and 23% respectively). The pregnancy rate of contralateral ovulations (9%) was also higher, though not significantly, than that of ipsilateral ovulations (3%), although the pregnancy rates per transfer were similar (16 and 14% respectively). The total pregnancy rate of both IUI and IVF was higher in contralateral than in ipsilateral ovulation cycles (8.1 and 4.0% respectively). The dominant follicles in contralateral ovulation cycles showed significantly higher oestradiol/androstenedione ratio (P < 0.025) and oestradiol/testosterone + androstenedione ratio (P < 0.025) and lower androstenedione (P < 0.05) than those of ipsilateral ovulation cycles. There was no significant difference in oestradiol, progesterone and testosterone. These results indicate that the dominant follicles in contralateral ovulation cycles are healthier than those of ipsilateral ones. Local intra-ovarian factors, e.g. from the corpus luteum, may negatively affect the health of the dominant follicle and the enclosed oocyte. Therefore contralateral selection of the dominant follicle in the succeeding cycle may favour pre-embryo development. The chance of conceiving during a natural cycle may be affected by the site of ovulation in the preceding cycle.
PMID: 8921071 http://www.ncbi.nlm.nih.gov/pubmed/8921071
secretory phase
Endometrial stromal cells (ESCs) differentiate into decidual cells in the mid and the late secretory phases, regardless of whether pregnancy has been established.
Postnatal Cycle Flexibility
A recent paper has demonstrated that the human menstral cycle can be modulated postnatally by environmental conditions as measured by changes in progesterone based upon age of migration from a relatively poor environment (Bangladesh) to a relatively better environment (UK). Childhood conditions influence adult progesterone levels. Núñez-de la Mora A, Chatterton RT, Choudhury OA, Napolitano DA, Bentley GR. PLoS Med. 2007 May;4(5):e167. PMID: 17503960 | PLoS Medicine
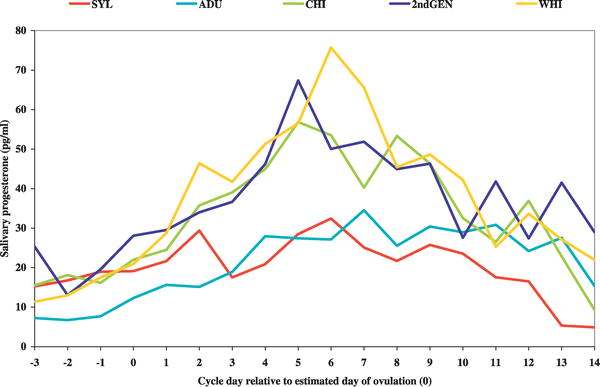 |
SYL - resident Bangladeshi sedentees from Sylhet
ADU - adult migrants CHI - child migrants 2ndGEN - second-generation British-Bangladeshis WHI - British women of European descent Unadjusted mean luteal progesterone index values. Ovulation dates were estimated from oestradiol data available for the same individual menstrual cycles. (More? PLoS Medicine - Article) |
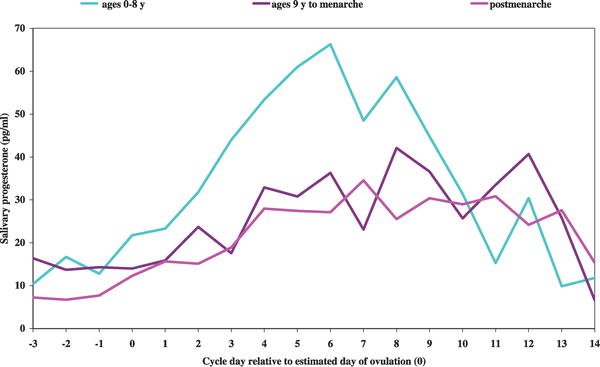 |
Women who migrated during infancy and early childhood (ages 0–8 y) had a significantly earlier age at menarche.
Women who migrated after menarche, length of time spent in the UK had no significant impact on luteal progesterone levels. (More? PLoS Medicine - Article) |
Data: Nunez-de la Mora A, Chatterton RT, Choudhury OA, Napolitano DA, Bentley GR. Childhood Conditions Influence Adult Progesterone Levels. PLoS Med. 2007 May 15;4(5):e167 (More? PLoS Medicine - Article)
Menstruation in Adolescents
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2644006/?tool=pubmed
- precocious puberty has been defined as any pubertal development occurring before age 8
- paper shows earlier timings
- range for menstrual cycles in adolescents is wider than in adults
- adult normal cycle length is defined as being between 21 and 34 days.
terminologies and definitions used to describe abnormalities of menstrual bleeding
Can we achieve international agreement on terminologies and definitions used to describe abnormalities of menstrual bleeding? Fraser IS, Critchley HO, Munro MG, Broder M. Hum Reprod. 2007 Mar;22(3):635-43. Epub 2007 Jan 4. PMID: 17204526 | Hum Reprod.
- terminologies and definitions around the symptom of abnormal uterine bleeding (AUB)
- The major recommendations were to replace terms such as menorrhagia, metrorrhagia, hypermenorrhoea and dysfunctional uterine bleeding.
- four key ‘menstrual dimensions’ should be cycle regularity, frequency of menstruation, duration and volume of menstrual flow.
- Regularity should be specified as irregular, regular or absent.
- Frequency should be specified as frequent, normal or infrequent.
- Duration should be specified as prolonged, normal or shortened.
- Volume should be specified as heavy, normal or light.
Table VII. Suggested normal limits for menstrual parameters in the mid-reproductive years
Clinical dimensions of menstruation and menstrual cycle Descriptive terms Normal limits (5th–95th percentiles) Frequency of menses (days) Frequent <24 Normal 24–38 Infrequent >38 Regularity of menses (cycle to cycle variation over 12 months; in days) Absent — Regular Variation ± 2 to 20 days Irregular Variation greater than 20 days Duration of flow (days) Prolonged >8.0 Normal 4.5–8.0 Shortened <4.5 Volume of monthly blood loss (ml) (Hallberg et al., 1966) Heavy >80 Normal 5–80 Light <5
corpus luteum
Luteal blood flow and luteal function. Takasaki A, Tamura H, Taniguchi K, Asada H, Taketani T, Matsuoka A, Yamagata Y, Shimamura K, Morioka H, Sugino N. J Ovarian Res. 2009 Jan 14;2:1. PMC2633338]
- During corpus luteum formation
- active angiogenesis occurs after the ovulatory LH surge
- corpus luteum becomes one of the most highly vascularized organs in the body PMID: 9500609
- corpus luteum blood flow
- necessary to provide luteal cells with the large amounts of cholesterol needed for progesterone synthesis
- to deliver progesterone to the circulation.
Sleep, Hormones, and Circadian Rhythms throughout the Menstrual Cycle
Sleep, Hormones, and Circadian Rhythms throughout the Menstrual Cycle in Healthy Women and Women with Premenstrual Dysphoric Disorder. Shechter A, Boivin DB. Int J Endocrinol. 2010;2010:259345. Epub 2010 Jan 18. PMID: 20145718 | PMC2817387
- relationship exists between the sleep-wake cycle and hormone secretion
- melatonin, cortisol, thyroid stimulating hormone (TSH), and prolactin (PRL), vary across the 24-hour day and are highly regulated by the circadian and sleep-wake cycles.
- sleep complaints commonly occur during the postovulatory luteal phase (LP) in healthy women
- premenstrual dysphoric disorder (PMDD) - a DSM-IV classified menstrual cycle-related mood disorder
endometrial and ovarian characteristics using three dimensional power Doppler ultrasound
http://www.rbej.com/content/7/1/151
patients who finally conceived was the presence of a triple-line pattern in the endometrium
Quantity and quality of retrograde menstruation: a case control study
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2789082/?tool=pubmed
- menstruation is associated with a higher concentration of endometrial cells in peritoneal fluid (PF)
- comparison with the nonmenstrual phase of the cycle, analysis of PF during menstruation showed an increased concentration of leucocytes (3.3 × 109/L vs 0.8 × 109/L, P = 0.03), erythrocytes (0.3 × 1012/L vs 0.02 × 1012/L, P = 0.006), hematocrit (0.03 L/L vs 0.003 L/L, P = 0.01) and hemoglobin (0.8 g/dL vs 0.1 g/dL, P = 0.01).
luteal phase changes
Suggested changes include:
- fluid retention, weight gain, increased energy demands, changes in glucose uptake, a slower gastrointestinal transit time, altered lipid profiles, altered vitamin D, calcium, magnesium and iron metabolism, emotional hypersensitivity, generalized pain, and changes in dietary habits.
Changes in serum calcium, magnesium and inorganic phosphorus levels during different phases of the menstrual cycle. Dullo P, Vedi N. J Hum Reprod Sci. 2008 Jul;1(2):77-80. PMID: 19562050
Women's sexual interest
http://www.ncbi.nlm.nih.gov/pubmed/19306881
Women's sexual interest changes with hormonal fluctuations across the menstrual cycle.
- "The observed increase in activation in the right medial orbitofrontal cortex (OFC) during the follicular phase may reflect a hormonally mediated increase in appetitive motivation and may prime women towards increased sexual interest and behavior around ovulation."
Progesterone and Progestin Receptors in the Brain
http://www.ncbi.nlm.nih.gov/pubmed/18436712 http://endo.endojournals.org/cgi/content/full/149/6/2737
