Introduction
This section gives a very brief overview of genital postnatal changes that occur in neonatal, childhood and through to puberty. For sexual development at puberty, we will use resources available online from Endocrinology: An Integrated Approach (NCBI Bookshelf).
Newborn
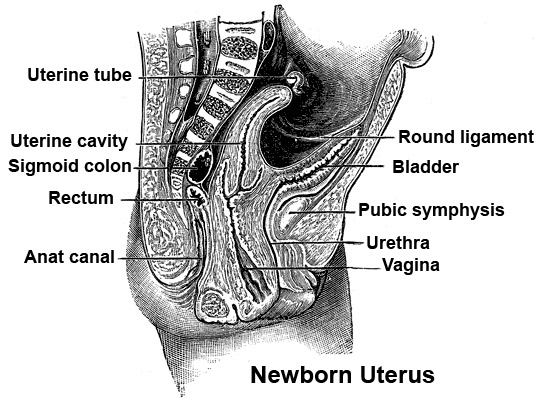
Newborn uterus anatomy
|
- Female tract abnormalities tend to be rarer and when they do occur are also more difficult to detect.
- Male abnormalities are more likely and easily detected asociated with fusion of the urogenital folds, undescended testes or hernia.
- This topic will be discussed on the next abnormalities will be discussed in detail on the next page.
|
|
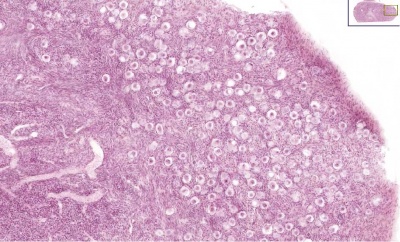
* Ovary - Primordial follicle numbers are highest late fetal to around birth (estimated 2.5 - 7 million) and then decreasing by apopotic cell death.
- At puberty there remain only about 400,000 and only about 10% of these will be released through reproductive life.
(Based on data from: Hassold, etal., Environ Mol Mutagen 1996. 28: 167-175)
|
Puberty
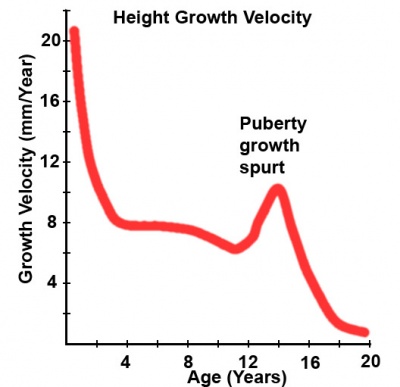
|
Latin, pubertas = "adulthood"
In the teen years the endocrine changes that signal sexual development trigger changes in primary sex organs and the development of secondary sexual characteristics.
- Hypothalamic expression of gonadotropin releasing hormone (GnRH) is a known puberty trigger.
- Recent research suggests that an earlier signal could come from increased neuronal and hypothalamic expression of a peptide family (kisspeptins) and their receptor (G protein-coupled receptor GPR54) in the hypothalamus.
- GnRH then signals the pituitary gland to release luteinizing hormone (LH) and follicle-stimulating hormone (FSH) to start sexual development.
Puberty can occur over a broad range of time and differently for each sex:
- girls - age 7 to 13
- boys - age 9 to 15
- Early onset of puberty (precocious) occurs more frequently in girls than boys, in contrast late onset (delayed) occurs more frquently in boys than girls.
- The physical characteristics that can be generally measured are: genital stage, pubic hair, axillary hair, menarche, breast, voice change and facial hair.
- In 1976, Tanner and Whitehouse established a series of descriptive stages (Tanner Stages) for primary and secondary sexual characteristic development at puberty.
Study the Tanner stages comparing the male and female physiological changes.
|
- Links: Puberty Development | Tanner stages
Female - Hypothalamus Pituitary Gonad (HPG) Axis
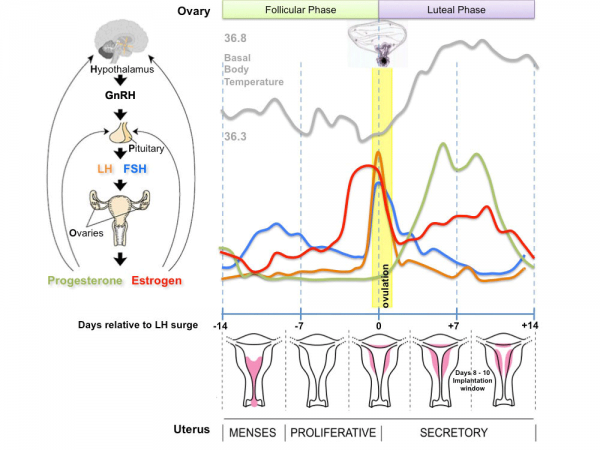
|
Female
- menarche (the first menstruation or a period) usually occurs after the other secondary sex characteristics
- cycles will continue until menopause (permanent cessation of reproductive fertility).
- The diagram shows the hormonal regulation pathway from the brain to the ovary and subsequent impact on uterine changes during the menstral cycle.
GnRH = gonadotropin-releasing hormone (GnRH). This peptide hormone is a decapeptide (10 amino acids) with a short half life (<15 minutes).
LH = Luteinizing Hormone
FSH = Follicle Stimulating Hormone
A similar endocrine axis is also found for regulation of the male gonad.
|
Male - Testosterone
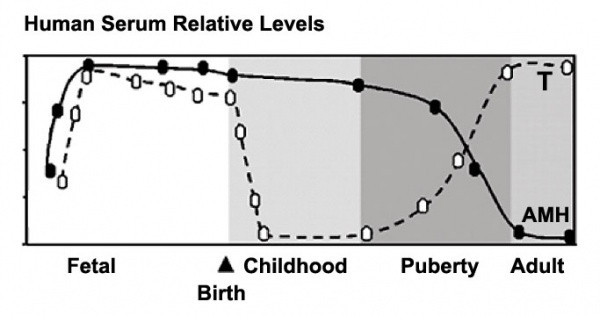
|
Male
Testosterone and Anti-Müllerian Hormone (AMH) relative levels[1]
- Sertoli cells - AMH production.
- Leydig cells - Testosterone production
- Spermatogonia - mitosis
- Spermatozoa - maturation
|
Additional Information
Endocrinology: An Integrated Approach. Nussey S, Whitehead S. Oxford: BIOS Scientific Publishers; 2001.
References
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2026, April 13) Embryology 2011 Lab 8 - Postnatal. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/2011_Lab_8_-_Postnatal
- What Links Here?
- © Dr Mark Hill 2026, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G




