User:Z3291324
Attendance
Lab 1 --Z3291324 12:56, 28 July 2011 (EST), Lab 2 --z3291324 11:47, 4 August 2011 (EST), Lab 3 --z3291324 12:53, 11 August 2011 (EST), Lab 4 --z3291324 12:35, 18 August 2011 (EST), Lab 6 --z3291324 12:53, 1 September 2011 (EST), Lab 7 --z3291324 12:24, 15 September 2011 (EST, Lab 8 --z3291324 11:13, 22 September 2011 (EST)--Jacqueline Ellero 12:58, 29 September 2011 (EST)--z3291324 12:59, 29 September 2011 (EST) --z3291324 12:52, 6 October 2011 (EST) --z3291324 12:09, 13 October 2011 (EST)--z3291324 12:14, 20 October 2011 (EST)
Lab 1
Identify the origin of In Vitro Fertilization and the 2010 nobel prize winner associated with this technique.
The first pregnancy achieved through IVF occurred in 1973. However, the first successful IVF birth occurred in 1978 (Louise Brown.) Robert Edwards and Patrick Steptoe carried out this successful conception. Robert Edwards later received the 2010 Nobel Prize in Physiology or Medicine for this development.
Identify a recent paper on fertilisation and describe its key findings.
Halliday, J., Oke, K., Breheny, S., Algar, E., & D, J. A. (2004). Beckwith-Wiedemann syndrome and IVF: a case-control study. Am J Hum Genet, 75(3), 526-528.
This article provides evidence suggesting that children conceived through IVF are significantly more likely to develop imprinting disorders such as Beckwith-Wiedemann syndrome and Angelman syndrome (9 times greater.) It is unknown why IVF causes this increase although suggestions include uniparental disomy of the chromosome and unidentified mutations.
Identify 2 congenital anomalies.
Anencephaly: caused by a failure of the rostral end of the neural tube to close resulting in a lack of brain development. Trisomy 21: caused by the presence of additional genetic material on chromosome 21, either in part or full.
--Mark Hill 09:58, 3 August 2011 (EST) Where are your Lab 1 assessment answers? Need to added before Lab 2.
Lab 2
Identify the ZP protein that spermatozoa binds and how is this changed (altered) after fertilisation
Spermatozoa bind to the zona pellucida glycoprotein 3 proteins, which are located on the surface of the zona pellucida. After the spermatozoa binds, it releases enzymes from its acrosome to dissolve the zona pellucida allowing it to fuse with the ovum. After fusion, the ovum exocytoses cortical granules. The cortical reaction alters the ZP3 protein preventing polyspermic fertilisation.
Identify a review and a research article related to your group topic
Goldmuntz, E., Geiger, E., & Benson, D. W. (2001). NKX2.5 mutations in patients with tetralogy of fallot. Circulation, 104(21), 2565-2568. - Research article which looks into some genetic causes of tetralogy of fallot.
Apitz, C., Webb, G. D., & Redington, A. N. (2009). Tetralogy of Fallot. Lancet, 374(9699), 1462-1471. - Review article which describes the condition, some symptoms, treatment options and complications.
Lab 3
What is the maternal dietary requirement for late neural development?
Iodine is required for late neural development. A deficiency in iodine may result in cretinism. The daily requirement for pregnant mothers is roughly 200ug.
Lab 4 Online Assessment
- The allantois, identified in the placental cord, is continuous with what anatomical structure?
- Identify the 3 vascular shunts, and their location, in the embryonic circulation.
- Identify the Group project sub-section that you will be researching. (Add to project page and your individual assessment page)
"
"
Lab 4
The allantois, identified in the placental cord, is continuous with what anatomical structure?
The allantois is an out-pocketing of the yolk sac. It extends into the connecting stalk. The allantois becomes the urachus in the adult (the median umbilical ligament.)
Identify the 3 vascular shunts, and their location, in the embryonic circulation.
1. Ductus arteriosus (connecting the pulmonary artery to the aortic arch). This allows blood entering the right ventricle to bypass the fluid filled lungs. 2. Foramen ovale (between the left and right atria). This allows blood from the right atrium to be shunted into the left atrium to avoid the fluid filled lungs. 3. Ductus venosus (shunts blood from the umbilical vein directly to the inferior vena cava).
Identify the Group project sub-section that you will be researching.
I will be researching the four abnormalities of tetralogy of fallot (pathophysiology) and diagnostic methods.
Lab 5
Which side (L/R) is most common for diaphragmatic hernia and why?
Left sided diaphragmatic hernias are more common (in about 85-90% of cases). This is likely due to the earlier closure of the right pleuroperitoneal opening. Diaphragmatic hernias may be life threatening in new borns due to the incomplete development and inhalation of the lung. --z3291324 21:08, 31 August 2011 (EST)
Lab 6
What week of development do the palatal shelves fuse?
The two palatal shelves fuse in week 9.
What animal model helped elucidate the neural crest origin and migration of cells?
The chick (and later also the quail) helped the discovery of the neural crest origin and migration of cells.
What abnormality results from neural crest not migrating into the cardiac outflow tract?
Failure of the neural crest to migrate into the cardiac outflow tract could produce abnormalities including persistent truncus arteriosus (the truncus arteriosus fails to divide into a pulmonary artery and aorta). Other abnormalities include elongation or mispositioning of the outflow tract and cushion hypoplasia. --z3291324 21:05, 14 September 2011 (EST)
Lab 7
Are satellite cells (a) necessary for muscle hypertrophy and (b) generally involved in hypertrophy?
a) satellite cells ar enot necessary for muscle hypertrophy b) but they are a normal part of hypertrophy.
Why does chronic low frequency stimulation cause a fast to slow fibre type shift?
Chronic low frquency stimulation causes a fast to slow shift because the muscle fibre is continuously stimulated as if it were a slow fibre. The protein percentages of the muscle fibre gradually change until it more closely resembles a slow fibre. --z3291324 10:56, 21 September 2011 (EST)
Evaluation of trisomy 21
Introduction: The introduction does not contain enough information. A more general introduction to trisomy 21 is needed.
Links: There is a good use of links to other sites for further information.
Headings: Clear use of headings. However, perhaps epidemiology and prevalence would be better placed near the start of the page.
Symptoms: There could be a general section on symptoms before going into more detaila bout the heart and limb defects. The defects, especially the heart defects could be explained in much more detail.
Images: Images are used well however, there could be more detailed captions describing what the pictures mean, especially the graphs.
Referencing: The referencing is done well and shows that a wide variety of appropriate sources were used to produce the page.
Glossary: The glossary/terms list is a good idea however, it could be extended to include more words for example, complicated anatomical terms referring to the heart. There is evidence of significant research.
Learning objectives: The page is related well to learning objectives of embryology. For example, the information on genetic causes and chromosomes. --z3291324 11:14, 21 September 2011 (EST)
Lab 8
Group 1
Introduction: Good introduction. Clearly explained. An image would be good to accompany some of the text.
Epidemiology: Easy to understand and good images.
Etiology: The picture on the right hand side could be bigger so that it is easier to read and understand. The information is written well but seems a bit disjointed because of where the pictures are placed. Maybe move the one on the left hand side so it doesn’t break up the paragraph.
Clinical manifestations: I think this section would be better in paragraphs with some of the points explained in more detail eg gonadal dysgenesis, hypothyroidism etc.
Diagnosis: The text is good. The table seems a bit overtaken by images. I think it needs some more text to balance it out eg. explain what brachycephaly is.
Treatment: text is good, however, some sections could be explained more clearly eg. what is coarctation of the aorta? This section needs some images.
Current and future research: definitely needs some images to balance out the text.
Glossary: Glossary is good. Maybe put an asterisk next to words in the project that are in the glossary.
Group 2
Introduction: Introduction is good. The pictures look great.
Historical background: I like the timeline. I think the picture needs a caption underneath explaining who the people are.
Epidemiology: Needs some pictures to break up the text.
Etiology: This section is quite difficult to understand. I think a lot of terms need explaining eg. hemizygous deletion, microdeletion and halpingoinsufficiency.
Pathophysiology: This section is much easier to understand and flows quite well. The pictures should be bigger though.
Diagnostic tests: great section! Good layout and easy to read. The symptoms picture could be a bit bigger and it would be good if there were pictures for the bottom two.
Clinical manifestations: Again, great section. The table could use some more pictures though to balance out all the text.
Treatment: Needs some more pictures.
Current and future research: This section is quite well explained and has a good level of detail.
Group 3
Introduction: I think you need to explain what the disease is before you explain the genetics behind it. Also, this section seems more like a summary of the whole project. I think you could change it a bit to include more general information on the background of the disease before going into detail.
History: I think this section would be good if all the text was incorporated into the timetable and some pictures added to balance out the text.
Epidemiology: Good section overall however, the pictures could be a lot bigger.
Etiology: Good section but I think the picture needs a caption to explain what the diagram is referring to.
Pathogenesis: This section is clearly explained. The pictures are great but need to be bigger.
Signs and symptoms: The table is good but I think it would look much better if you added pictures for all the sections.
Diagnosis: Similar advice to most other sections- the text is good but I think you should add some pictures to demonstrate some of the abnormalities.
Management: The picture would be good with a caption to explain what the diagram means.
Defects: The table is good but a couple of the pictures are far too small.
Current research: Good section, but again, needs some pictures!
Group 4
Introduction: Introduction is alright but could be more detailed.
History: This section is good but the timeline would be better with more information/ more detailed explanation of the points already there.
Epidemiology: This section seems too concerned with the occurrence of the HD. I think this section could use some more general epidemiological information as well.
Genetics: This section is explained clearly and done quite well. The pictures need to be bigger though.
Pathogenesis: This section is good. The image could be a tiny bit bigger and would be better if it had a caption explaining the different parts of the diagram.
Clinical manifestations: This section could be longer/more detailed. You could explain some of the symptoms. Eg.what is chorea? Also, the picture is good but needs to be much bigger.
Diagnosis: This section doesn’t seem to actually explain how HD is diagnosed. Where is the diagnosis? Also, the picture is good but needs a more detailed caption.
Treatment: This table is not very nice to read and seems a bit complicated. I think it would work better simplified and put into paragraphs.
Future research: Good pictures and text. I think the images need more explaining. Eg. where is the caudate located in the brain. Maybe arrows could show this.
Group 5
Introduction: Good pictures but they need to be bigger. Also, this section seems like a brief summary of the sections to come. I think it would be good if you included some more general background information on fragile x.
History: This section could be longer. The table would look good with some pictures in it.
Epidemiology: Great section and I like the diagram but some of the words in the diagram are hard to read.
Genetics: This section is reasonably well explained. The genetic terms need more explaining though.
Development: Good section but needs some pictures.
Signs and symptoms: Great section. Well written, flows well and easy to understand. Needs more pictures though.
Diagnosis: This section seems a bit short. Maybe you could explain how the diagnostic techniques work.
Treatment: The table seems too text heavy. Maybe add some pictures to break up the text.
Recent research: overall, good section.
Group 7
Introduction: Good but would be better with some pictures.
History: I think this section would be better if all the text was incorporated into the timeline instead of having the two separate sections.
Epidemiology: This section seems very incomplete.
Etiology: Again, this section seems incomplete. The genetics components of the disease need more detailed explaining because they are hard to understand.
Pathogenesis: This section seems quite complicated and disjointed. One of the pictures is very large. It would be better if it was a bit smaller and had a caption explaining it.
Signs and symptoms: I think it would look better if the table was put into sentences and the signs and symptoms were put into the table instead.
Complications: This section is very brief and seems quite complicated. Terms like halpingoinsuffiency need further explaining.
Diagnosis: Good. The table is great. Would look better if it was centred and had a caption to go with it.
Treatment: I think this section needs to be more detailed.
Current research: Would look better with more pictures.
Group 8
History: Timeline could be more detailed.
Epidemiology: I think you should put the headings on a separate line above the information and add some pictures.
Aetiology: This section is very detailed but the pictures are difficult to see. They need to be bigger but some of the hand drawn ones need darker text and more detailed captions.
Pathogenesis: Great diagrams. Looks really good with lots of pictures. Well explained. The diagrams could be a bit bigger though.
Symptoms and diagnosis: Good information but could be organised more neatly. The table looks like it has a lot of text and not enough pictures.
Treatment: needs some pictures to balance out the text
Current research: This section needs more detail. It would be better in paragraphs not dot points.
Group 9
Introduction and history: These sections need pictures. It is difficult to read such a large block of text.
Genetics: Good section overall. The genetics could be explained in a bit more detail and the pictures could be a bit bigger.
Diagnosis: Good section- well written and clearly explained.
Epidemiology: Would be better in paragraphs not dot points.
Phenotype table: I think it would look better if the colours were changed so that it looks more professional.
Cardiac/genitourinary/endocrine: These sections need more pictures to break up all the text.
Cognitive phenotype: This section is by far the most detailed and well explained section. It would be much better with pictures though. Great work.
Group 10
Introduction: Good introduction. The picture could be a bit bigger. Also, a picture of the chromosome would be great.
History and epidemiology: Both sections are clear and flow well. Pictures are needed to break up the text though.
Genetics: The image is great and the text is well written.
Pathogenesis: The pathogenesis is well explained. Again, pictures would be good in this section to improve it.
Clinical manifestations: Good section. Clear, easy to understand.
Diagnosis: This section might need some more detail added. You could explain how each of the diagnostic tests work
Current and future treatment: This section is worded well but looks a little bit disjointed. I think it would be better having it either all in text or all in the table.
Group 11
Introduction: The introduction needs a lot more work. More detail required.
History: The history and timeline could be collapsed into one section. It would look better without so much spacing between the paragraphs.
Diagnosis: This section is well done but needs pictures.
Etiology: This section could be expanded upon. I think it would be good if you explained how each of the developmental errors occur.
Developmental staging: You could explain what the stages are. A non-embryology student might not understand the different stages.
Types of cleft palate: The images are great and the text is good but I think this section would be better off in pathophysiology for example, not its own section.
Pathophysiology: The text is good but again, more pictures are needed to break up the text.
Genetics: This section could be explained in more detail. Pictures needed.
Anatomy: This section is well done
Treatment, problems and future directions: All of these sections look like a good start but each dot point needs to be explained in more detail. --z3291324 23:32, 28 September 2011 (EST)
Lab 10
1. An environmental teratogen that can lead to hearing loss is cytomegalovirus.
2. The auditory tube relies upon only one muscle to open it during fetal life (tensor veli palatini). In the adult, two muscles (tensor veli palatini and levator veli palatini) open the auditory tube.
In the adult, the auditory tube runs downwards to drain into the lateral wall of the nasopharynx. During fetal life, the tube is almost horizontal.
The tube is smaller and narrower in fetal life.
3. Stickler syndrome is a craniofacial disorder affecting the inner ear. http://www.omim.org/entry/604841
Contribution to group project
As of 2.30pm 12/10/2011
Introduction
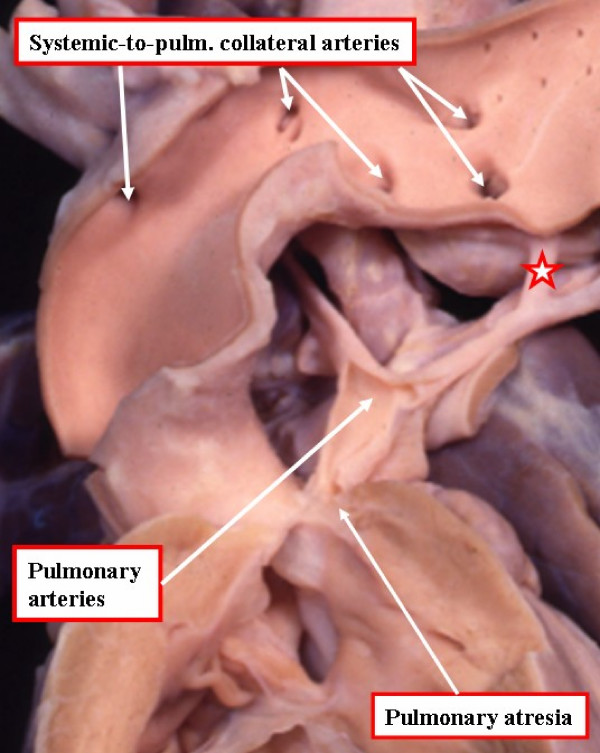
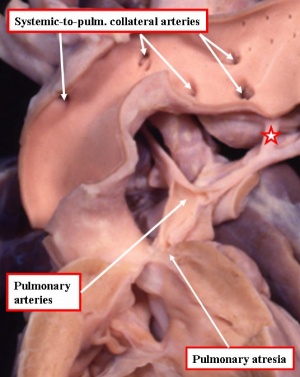
Tetralogy of Fallot (TOF) is a congenital heart disease affecting approximately 3 in 10000 people. It is the most common form of congenital heart disease, accounting for about 1 in 10 cases. [1] TOF was named after Etienne-Louis Fallot for his description of the anatomy and physiology of the defects associated with the disease.[2] TOF is believed to be caused by a genetic mutation of chromosomes 5,20 and 25, which impact the development of the neonatal heart. These genetic mutations contribute to the four characteristic defects of TOF:
- Pulmonary stenosis: a narrowing of the blood flow path from the right ventricle to the lungs.
- Overiding aorta: an aorta which is continuous with both ventricles instead of just the left one.
- Ventricular septal defect: the septum dividing the left and right ventricles is incomplete
- Right ventricular hypertrophy: enlargement of the cells in the right ventricle. [3]
TOF patients are given the name 'blue babies' because they often have a slightly blue appearance due to the decreased circulating oxygen levels. Some common symptoms in TOF patients include turning blue while crying, collapsing due to tet spells during exercise, dizziness and fatigue.
Etienne Fallot, Helen Taussig and Alfred Blalock have significantly contributed to the understanding of the cardiac anomalies and treatment options associated with TOF. Currently, surgery is the most successful treatment option, however palliative care and medical treatment is also available. Due to technology advancements, doctors are able to detect TOF more accurately and treat patients quicker, allowing an increase in survival rate and a favourable long term prognosis.
Whilst the understanding of this disease has grown greatly, future treatment options are continuously being explored. These include developing durable and efficient surgical procedures, shunts and valves.
Pathophysiology and Abnormalities
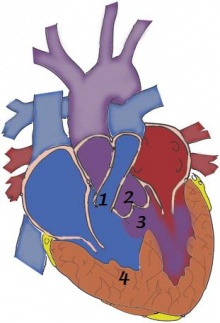
The four pathological features of tetralogy of fallot are:
These features result from the disruption of the aortic and pulmonary outflow tracts. The severity of symptoms is determined by the extent of right ventricular outflow obstruction.[3]
Pulmonary stenosis - Pulmonary stenosis may be caused by a narrowing of the pulmonary valve (valvular stenosis) or the outflow tract of the right ventricle (infundibular stenosis). [4] The narrowing of either the valve or the infundibulum obstructs the flow of blood from the right ventricle into the pulmonary circulation. Consequently, this results in a reduced flow of oxygenated blood in the systemic circulation. If the degree of pulmonary stenosis is mild, a left to right shunt forms. (The higher pressure in the left ventricle causes blood to pass through the septal defect into the right ventricle). However, if the pulmonary stenosis is significant, a right to left shunt will form. [5] This occurs because the stenosis raises the pressure in the right ventricle and forces blood directly into the left ventricle. This is important because deoxygenated blood can now enter the systemic circulation and problems such as cyanosis, dizziness and fainting can occur. The pathophysiology of pulmonary stenosis usually worsens with age because the pulmonary orifice stays the same size despite an increase in the size of the heart. [6]
Overriding aorta - Instead of being positioned directly over the left ventricle, the aorta is displaced anterosuperiorly (in front of and above). The aortic valve is located directly above the interventricular septal defect allowing blood from both the left and right ventricles to pass through the aortic valve. [7] This biventricular connection allows both oxygenated (from left ventricle) and deoxygenated blood (from right ventricle) to enter the systemic circulation. The degree to which the overriding aorta is continuous with the right ventricle determines the severity of symptoms. [8]
Ventricular septal defect - The interventricular septum dividing the left and right ventricles is incomplete at its superior, membranous end. [9] During ventricular contraction, blood from the left ventricle is forced into the right ventricle and then re-enters the pulmonary circulation. This extra volume of blood places pressure of the pulmonary system and compensatory pulmonary hypertension and right ventricular hypertrophy may occur. If the right ventricular pressure exceeds that of the left, the left to right shunt is reversed and the patient will experience cyanosis because deoxygenated blood is bypassing the lungs and entering the systemic circulation. [10]
Right ventricular hypertrophy - Hypertrophy of the right ventricle is a compensatory response to pulmonary stenosis. Because the pulmonary outflow tract is narrowed, the right ventricle must pump harder to meet the oxygen demands of the body. [11]
|
Diagnostic Tests
| Diagnostic technique | How the technique works | Presentation in a TOF patient | Image |
| Physical examination | TOF is often diagnosed during fetal life by echocardiography.[9]
If TOF is not detected during fetal life, certain signs and symptoms at birth may alert the need for further investigation. |
Signs and symptoms include mild to moderate cyanosis, which worsens when the baby cries, difficulty feeding and difficulty gaining weight. However, TOF often goes undiagnosed until adult life. Most adult patients will appear normal, however, some may present with cyanosis and clubbing of the fingers. The jugular venous pressure is usually normally (raised jugular venous pressure often indicates right ventricular failure). If the aorta is pushed to the right (so it is continuous with both the left and right ventricle), a lift below the right sternoclavicular joint may be noted. [12] | 
|
| Heart murmurs | Heart murmurs are sounds caused by the turbulent flow of blood. They are heard using a stethoscope. They are often the result of problems including valvular stenosis (narrowing of valves), valvular regurgitation (leakage of valves due to incomplete closure) or defects in the heart wall allowing blood to flow in unusual directions. [13] | Examination of the heart of a patient with TOF may reveal a loud second heart sound (produced by the closure of the pulmonary valve). A harsh systolic ejection murmur may be heard and a palpable thrill may be felt along the left sternal border. [14] These sounds occur because the pulmonary outflow tract is obstructed. Although this murmur is often present, sometimes it may be short or difficult to hear and is often missed on physical examination. A pansystolic (occurring throughout the whole of systole) murmur may also be heard. This type of murmur occurs due to the ventricular septal defect between the left and right ventricles. The increased pressure in the left ventricle forces blood back into the right ventricle, causing a murmur, which lasts the whole of systole (contraction phase). [15] | 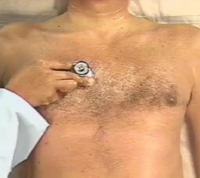
|
| Electrocardiogram | Once TOF is suspected, electrocardiogram and chest radiographs are performed. Electrocardiography is used to assess the electrical activity of the heart. The electrical activity is detected by electrodes, which are placed on the skin of the patient and recorded by an external device. [16] | The electrocardiogram is extremely important in detecting a right bundle branch block (a block in the electrical conducting system of the heart), which is common in patients with TOF. An electrocardiogram will also reveal a heart that is deviated slightly to the right and an enlarged right ventricle due to the ventricular hypertrophy.[12] | 
|
| Chest radiograph | A chest radiograph (or chest x-ray) uses ionising radiation to develop an image of the patient’s chest. It is used to diagnose many conditions including conditions of the thorax and structures within the thoracic cavity including the heart, lungs and major blood vessels entering and leaving the heart. Chest radiographs are often used to screen for certain diseases but further tests are required for a definitive diagnosis.[17] | In a patient with TOF, a chest radiograph will demonstrate a prominent right ventricular shadow, giving the heart a boot-like appearance, which is typical of patients with TOF. The right ventricular hypertrophy causes the apex of the right ventricle to rise on top of the relatively unfilled left ventricle, giving the heart its boot-shaped appearance on examination. [3] The radiograph will also show a right-sided aorta in approximately one-quarter of patients.[12] | 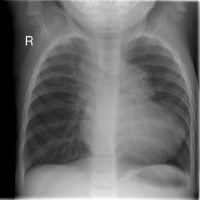
|
| Echocardiogram | An echocardiogram (also called a cardiac ultrasound) is performed to confirm the above findings. Echocardiography uses ultrasound to produce two-dimensional (and now also three-dimensional) images of the heart. It assesses cardiac tissue, valve function, the velocity of blood flow and any abnormal communications within the heart.[18] | The echocardiogram identifies important abnormalities of the heart including obstruction of the pulmonary outflow tract, the size of the pulmonary arteries, the degree of aortic override and the size of the defect in the interventricular septum. [3] | 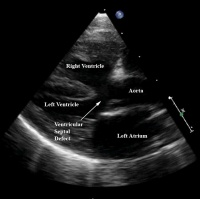
|
| Magnetic resonance imaging | Magnetic resonance imaging (MRI) is evolving as the most important technique for evaluating the size and functioning of the right ventricle. An MRI machine uses a magnetic field to produce a detailed image of the scanned area of the body. It is especially useful in viewing soft tissues as it provides greater contrast than techniques such as x-ray. [19] | MRI’s are important in assessing pulmonary valve competence and the severity of regurgitation (the amount of blood that flows back into the right ventricle due to the incomplete closure of the pulmonary valves) in patients with TOF. It can measure the volume and mass of the right and left ventricles and can assess the degree of pulmonary outflow tract obstruction. Finally, MRIs are important in measuring the degree of ventricular septal defect.[12] | 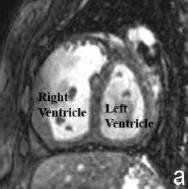
|
Internal links
Cardiovascular development abnormalities http://embryology.med.unsw.edu.au/Notes/heart2.htm#Fallot
Advanced cardiac embryology http://embryology.med.unsw.edu.au/embryology/index.php?title=Advanced_Cardiac_Embryology
Cardiovascular system development http://embryology.med.unsw.edu.au/embryology/index.php?title=Cardiovascular_System_Development
Cardiovascular development lecture http://embryology.med.unsw.edu.au/embryology/index.php?title=2009_Lecture_21
Lab 11
Name the components that give rise to the interatrial septum and the passages that connect the right and left atria
The septum primum and septum secundum give rise to the interatrial septum. The passage that initially connects the atria is the foramen primum but later in development, it is the foramen ovale and foramen secundum.
Identify the cardiac defects that arise through abnormal development of the outflow tract
These include tetralogy of fallot, transposition of great vessels, and double outlet of the right ventricle.
Lab 12
Give examples of 3 systems that continue to develop postnatally
Reproductive (external genital features), respiratory and neural development continue to develop postnatally.
Identify the abnormalities detected by the Guthrie Test and link to one abnormality listed in OMIM
The Guthrie test is performed on newborn infants to detect phenylketonuria. It can also be used to detect cystic fibrosis, congenital adrenal hyperplasia, congenital hypothyroidism, galactosaemia and a number of amino acid disorders.
Link to OMIM cystic fibrosis: http://www.omim.org/entry/219700
- ↑ <pubmed>1689816</pubmed>
- ↑ <pubmed>19683809</pubmed>
- ↑ 3.0 3.1 3.2 3.3 <pubmed></pubmed>19144126 Cite error: Invalid
<ref>tag; name 'PMID19144126' defined multiple times with different content - ↑ <pubmed>14132270</pubmed>
- ↑ <pubmed>15934690 </pubmed>
- ↑ Kumar V, Abbas AK, Fausto N, Mitchell RN (2007). Robbins Basic Pathology. 8th edn. Saunders/Elsevier: Philadelphia, PA.
- ↑ Kumar V, Abbas AK, Fausto N, Mitchell RN (2007). Robbins Basic Pathology. 8th edn. Saunders/Elsevier: Philadelphia, PA.
- ↑ <pubmed>11520451</pubmed>
- ↑ 9.0 9.1 <pubmed>19683809</pubmed>
- ↑ Kumar V, Abbas AK, Fausto N, Mitchell RN (2007). Robbins Basic Pathology. 8th edn. Saunders/Elsevier: Philadelphia, PA.
- ↑ <pubmed>3068155</pubmed>
- ↑ 12.0 12.1 12.2 12.3 <pubmed>8272784</pubmed>
- ↑ http://www.nhlbi.nih.gov/health/health-topics/topics/heartmurmur/
- ↑ Kumar V, Abbas AK, Fausto N, Mitchell RN (2007). Robbins Basic Pathology. 8th edn. Saunders/Elsevier: Philadelphia, PA
- ↑ Cite error: Invalid
<ref>tag; no text was provided for refs namedPMID21048055 - ↑ Braunwald E. (Editor), Heart Disease: A Textbook of Cardiovascular Medicine, Fifth Edition, p. 108, Philadelphia, W.B. Saunders Co., 1997
- ↑ http://www.nlm.nih.gov/medlineplus/ency/article/003804.htm
- ↑ http://www.nlm.nih.gov/medlineplus/ency/article/003869.htm
- ↑ Squire LF, Novelline RA (1997). Squire's fundamentals of radiology (5th ed.). Harvard University Press