Lecture - Genital Development: Difference between revisions
| Line 256: | Line 256: | ||
This looped animation shows the development of external female genitalia from the indifferent external structure, covering the approximate period of week 9 to 12. | This looped animation shows the development of external female genitalia from the indifferent external structure, covering the approximate period of week 9 to 12. | ||
{{Female external movie}} | |||
[[File:Urogenital_septum_001 icon.jpg|90px|link=Development_Animation_-_Urorectal_Septum]] | [[File:Urogenital_septum_001 icon.jpg|90px|link=Development_Animation_-_Urorectal_Septum]] | ||
| Line 269: | Line 272: | ||
{| | |||
| {{Ovary movie}} | |||
| {{Testis movie}} | |||
| {{Female external movie}} | |||
==Gonad Descent== | ==Gonad Descent== | ||
Revision as of 14:57, 18 September 2012
Introduction
This section of notes covers genital development. Differences in development are dependent on a protein product of the Y chromosome SRY gene. Mesonephric duct (Wolffian Duct) and paramesonephric (Mullerian Duct) contribute the majority of male and female internal genital tract respectively.
Objectives
- Understand the development of the gonads in males and females
- Understand the chromosomal basis of sex determination
- Understand the differences in male/female internal duct develpoment.
- Understand the origins of the external genitalia
- Understand the developmental abnormalities in male and female development.
Textbooks
The Developing Human: Clinically Oriented Embryology

|
Citation: The Developing Human: clinically oriented embryology 9th ed. Keith L. Moore, T.V.N. Persaud, Mark G. Torchia. Philadelphia, PA: Saunders, 2011. (links available to UNSW students) |
Larsen's Human Embryology
|
Citation: Larsen's human embryology 4th ed. Schoenwolf, Gary C; Larsen, William J, (William James). Philadelphia, PA : Elsevier/Churchill Livingstone, c2009. (links available to UNSW students) |
Embryology
Movies
|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||
Objectives
- Understand the development of the gonads in males and females.
- Understand the chromosomal basis of sex determination.
- Understand the differences in male/female internal duct develpoment.
- Understand the origins of the external genitalia.
- Understand the developmental abnormalities in male and female development.
Stages of Sexual Differentiation
- Development of the indifferent gonad - (genital ridge) early embryo
- Differentiation of gonad - (testis or ovary) late embryo, defining event in sexual differentiation
- Differentiation of internal genital organs and ducts - late embryo to fetal
- Differentiation of external genitalia - fetal
- Development of secondary sexual characteristics - puberty
Human Timeline
|
1. Development of the indifferent gonad
|

|
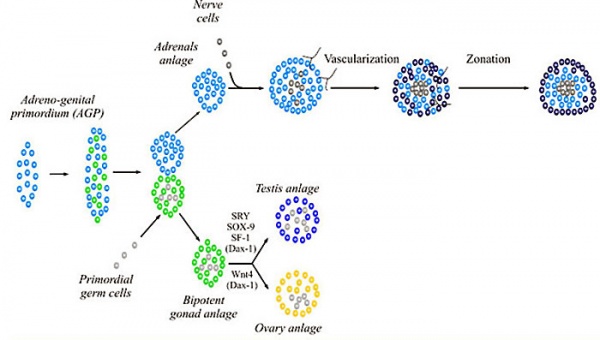
Gonad and adrenal early development (not required to know molecular information)
2. Differentiation of gonad into testis or ovary
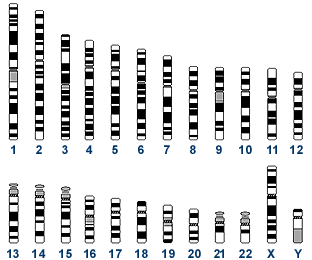
Chromosomal Sex Determination
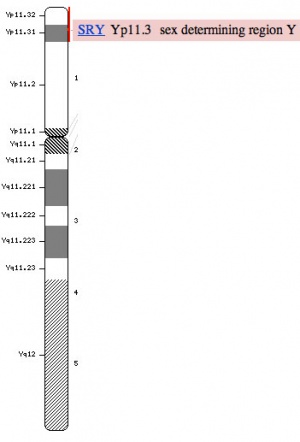
Y chromosome
- Y Chromosome - 59 million base pairs, hypervariable in length, mostly non-functional repeats
- Current known protein-coding genes = 48 including SRY
- SRY encodes a 204 amino acid protein (TDF) that is a member of the HMG (High mobility group) box class of DNA-binding proteins. Transcription factors bind to specific sites of DNA and regulates the transcription (expression) of other genes.
X chromosome
- X Chromosome - 155 million base pairs, contains about 5% of the haploid genome and encodes house-keeping and specialized functions.
- Genes such as Wnt-4 and DAX-1 necessary for initiation of female pathway ovary development
- An early discovery (1961) was that in order to have correct levels of X chromosome gene/protein expression (gene dosage), females must "inactivate" a single copy of the X chromosome in each and every cell. The initiator of the X inactivation process was discovered (1991) to be regulated by a region on the inactivating X chromosome encoding an X inactive specific transcript (XIST), that acts as RNA and does not encode a protein.
- The genetic content of the X chromosome has been strongly conserved between species because these genes have become adapted to working as a single dose - Ohno's law
- X inactivation occurs randomly throughout the embryo, generating a mosaic of maternal and paternally derived X chromosome activity in all tissues and organs. This can be seen in the fur colour of tortoiseshell cats.
Overview - MBoC - Figure 20-18. Influence of Sry on gonad development | image (image provides a good overview of the anatomy of sex determination, I will refer to this in the lecture and practical class)
Supporting Cells
- So called because they "support" the germ cells
Males
- develop as Sertoli cells
- SRY is expressed in the primordia of the supporting cells, transforming them into Sertoli cells that surround the germ cells and form testis cords
- SRY is not expressed in the other cell types of the gonad
- therefore the Sertoli cells instruct the germ cells and the steroid secreting cells to take the male path of development
- Embryonic Sertoli cells secrete anti-Mullerian hormone (AMH)
- Adult Sertoli cells line the inside of the seminiferous tubules and support spermatogenesis.
Females
- develop as Follicle cells (granulosa cells)
- Follicle cells surround and nurture the developing oocytes
- In response to FSH, follicle cells proliferate
- After ovulation, these cells become luteal cells of the corpus luteum secreting progesterone and oestrogens
Steroid secreting cell lineage
Male
- Develop into Leydig cells (interstitial cells) which sit outside the seminiferous tubules
- Secrete testosterone in response to luteinizing hormone from the pituitary
Female
- Develop into theca cells that secrete androstenedione which can be converted by the follicle cells into estrogens
Primordial Germ Cells
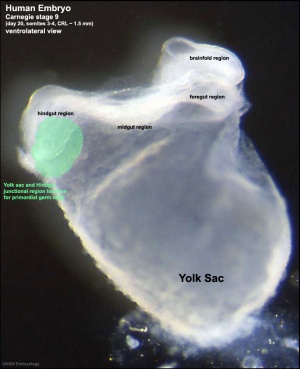
- Primordial germ cells (PGCs) are thought to be the first population of cells to migrate through the primitive streak in early gastrulation (week 3)
- cells then lie at the hindgut yolk sac junctional region
- later migrate into the genital ridge (germinal ridge) in early embryonic development.
| E9.0 Migration | E9.5 Migration | E10.5 Migration |
| Quicktime | Flash | Quicktime | Flash | Quicktime | Flash |
- Not the primordial germ cells which respond to SRY presence or absence, but the supporting cells within the developing gonad.
- Germ cells occasionally migrate by mistake into the developing adrenal gland and in the absence of sertoli cells telling them what to do, abnormally begin to develop as oocytes, even in males
- Links: Germ cell migration pathway
Gametogenesis
- forming PGCs as a small population of migratory cells
- enter the gonad where they undergo several rounds of mitotic cell division
- female - the germ cells enter meiosis and become arrested at the dictyate (diplotene) stage of meiotic prophase 1. All oocytes are at this stage at birth
- male - the germ cells are enclosed by the developing Sertoli cells and are induced to arrest differentiation and cell division as T1 prospermatogonia until after birth.
- Links: Image - Spermatogenesis | Image -Oogenesis
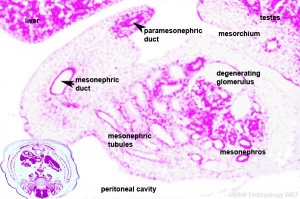
3. Differentiation of internal genital organs and ducts
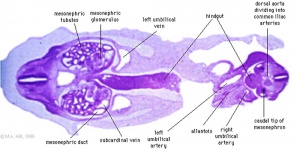
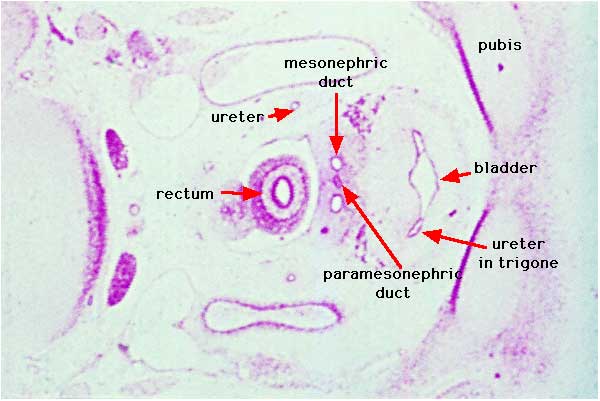
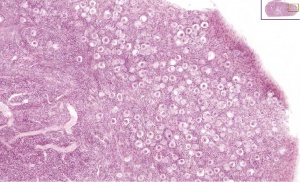
Human embryo (Carnegie stage 22, week 8) pelvic level cross-section.
Male
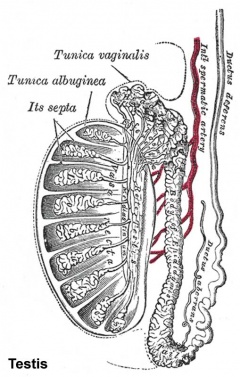
This looped animation shows the development of the male gonad showing medullary sex cords.
The tunica albuginea (white) covers the testis and bands extend inward to form connective tissue septa. |
|
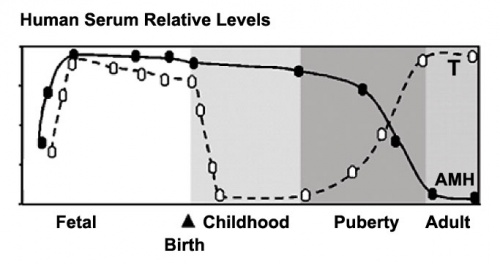
Anti-Mullerian Hormone
Anti-Mullerian hormone (AMH) or Mullerian Inhibiting Substance (MIS) hormone with at least two gonadal related functions:
- In males, it is produced by embryonic Sertoli cells and causes the loss of the paramesonephric (Mullerian) duct system that forms the internal female genital tract.
- In females, it is produced after puberty by follicle cells and suppresses the development of other primary follicles, thus restricting the number of follicles stimulated by FSH.
Female
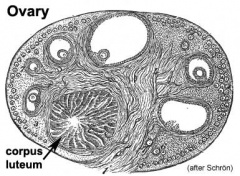
This looped animation shows the development of the female gonad showing cortical sex cords.
|
|
Uterus Development
- Week 7 – duct preservation or regression begins
| Uterus |
| Page | Play |
Paramesonephric duct development
Vagina Development
- The embryonic origin of the vagina has been a historically hotly debated issue with several different contributions and origins described.
- Current molecular studies show the whole vagina is derived from the intermediate mesoderm-derived Müllerian duct (see review [1])
- bone morphogenic protein 4 (BMP4) reshapes the duct into the vaginal primordium.
- exhibits different features from the uterus
- stratified squamous epithelium
- insensitivity to anti-Müllerian hormone
- Links: Vagina Development
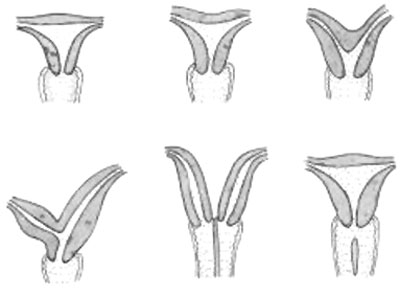
4. Differentiation of External Genitalia
Endocrinology - Diagram of the development of the external genitalia | image
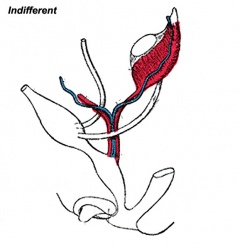
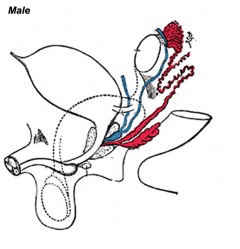
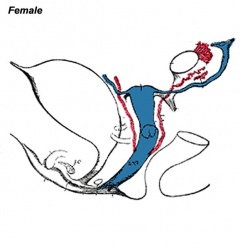
- external genitalia are initially identical and undergo male and female differentiation under the influence or absence of steroidal sex hormones.
- Indifferent stage ‐ cloaca divided by proliferating mesenchyme forming the urorectal septum which separates the ventral urogenital sinus from the dorsal rectum.
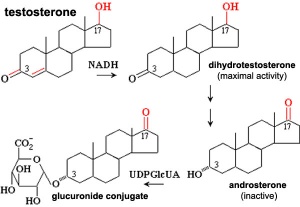
- Difference stage ‐ locally in this region the presence or absence of dihydrotestosterone (DHT), generated from testosterone, determines male/female development.
Dihydrotestosterone (DHT)
- Male presence of DHT
- locally in this region leads to genital tubercle growth, form
- genital folds (urethral) initial maintenance and then fusion, forming perineal and penile raphe.
- labioscrotal swellings (lateral to urethreal folds) become the scrotum.
- Female absence of DHT
- genital tubercle remains small, bends caudally to form the clitoris.
- genital folds (urethral) persist, do not fuse, and form labia minora.
- open urogenital sinus forms a cleft into which urethra and vagina open.
- labioscrotal swellings become the labia majora.
Female
This looped animation shows the development of external female genitalia from the indifferent external structure, covering the approximate period of week 9 to 12.
| Female External |
| Page | Play |
Animation - Urorectal septum and division of the cloacal membrane
Note the original cloacal membrane becomes separated into the urogenital membrane and anal membrane. The urogenital folds beneath the genital tubercle remain separate (unfused), forming the inner labia minora and second outer skin folds form the larger labia majora either side of the developing vestibule of the vagina. Note at the top of the animation, the changing relative size of the genital tubercle as it forms the glans of the clitoris.
Male Genitalia Development
Endocrinology - Box 6.6 The roles of testosterone (T) and 5α-dihydrotestosterone (DHT)
This looped animation shows the development of external male genitalia from the indifferent external structure, covering the approximate period of week 9 to 12.
|
|
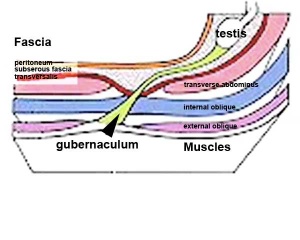
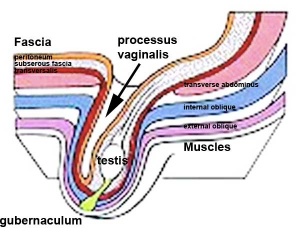
Gonad Descent
Both female and male gonads undergo anatomical descent.
The testis (white) lies in the subserous fascia (spotted) a cavity processus vaginalis evaginates into the scrotum, and the gubernaculum (green) attached to the testis shortens drawing it into the scrotal sac. As it descends it passes through the inguinal canal which extends from the deep ring (transversalis fascia) to the superficial ring (external oblique muscle). Descent of the testes into the scrotal sac begins generally during week 26 and may take several days. The animation shows the path of a single testis. Data from a recent study of male human fetal (between 10 and 35 weeks) gonad position.
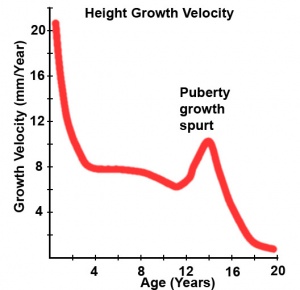
Incomplete or failed descent can occur unilaterally or bilaterally, is more common in premature births, and can be completed postnatally. 5. Postnatal - PubertyPuberty can occur over a broad range of time and differently for each sex:
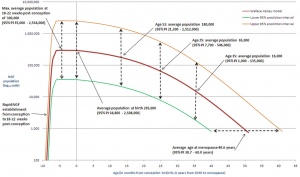
The physical characteristics that can be generally measured are: genital stage, pubic hair, axillary hair, menarche, breast, voice change and facial hair. Male
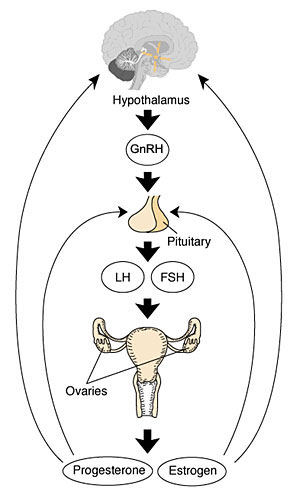
FemaleIn females, menarche (the first menstruation or a period) usually occurs after the other secondary sex characteristics, and will continue until menopause (permanent cessation of reproductive fertility). The diagram shows the hormonal regulation pathway from the brain to the ovary and subsequent impact on uterine changes during the menstral cycle.
A similar endocrine axis is also found for regulation of the male gonad. Puberty Abnormalities
Sex Differences in Adult and Developing Brains
2 sources of sexually dimorphic information
AbnormalitiesSex Reversal
XX males - usually caused by a transfer of some Y chromosome DNA onto the X chromosome
XY females - usually steroidal origin
Human genital abnormalities are currently described as "Disorders of Sex Development" (DSD) and include: chromosomal, gonadal dysfunction, tract abnormalities, external genitalia and gonadal descent. Congenital adrenal hyperplasia
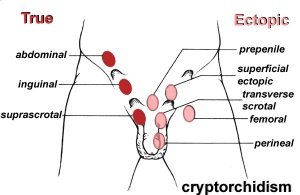
Cryptorchidism
Testis descent is thought to have 2 phases:
Undescended Ovaries
Hydrocele
Tract AbnormalitiesMany different forms
Uterine Duplication (uterus didelphys, double uterus, uterus didelphis) A rare uterine developmental abnormality where the paramesonephric ducts (Mullerian ducts) completely fail to fuse generating two separate uterus parts each connected to the cervix and having an ovary each. Septate Uterus Cervical: cervical agenesis, cervical duplication Vaginal: Mayer-Rokitansky syndrome (MRK anomaly, Rokitansky-Küster-Hauser syndrome, RKH syndrome, RKH) congenital absence of the vagina, dyspareunia, vaginal agenesis. External Genitalia - Hypospadia
Movies
References
Textbooks
Online Textbooks
Reviews<pubmed>17237341</pubmed>| Physiol. Rev. | Figure Links Search
External LinksExternal Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
|