2018 Group Project 1
The Contribution of Neural Crest Cells to the Adrenal Medulla
| Projects 2018: 1 Adrenal Medulla | 3 Melanocytes | 4 Cardiac | 5 Dorsal Root Ganglion |
Project Pages are currently being updated (notice removed when completed)
Introduction
Z5014972 (talk) 12:47, 14 August 2018 (AEST)z5014972 good review article https://link.springer.com/article/10.1007%2Fs12022-009-9070-6
The neural crest of an embryo differentiates and migrates to form various components of the body. One of these tissues is the medulla of the adrenal gland which is involved in the production of adrenalin and noradrenalin. This project will comprehensively outline the history of neural crest research, the embryonic developmental time course, tissue and organ structure, molecular mechanisms, abnormalities, animal models and current research.
History
Describing the neural crest
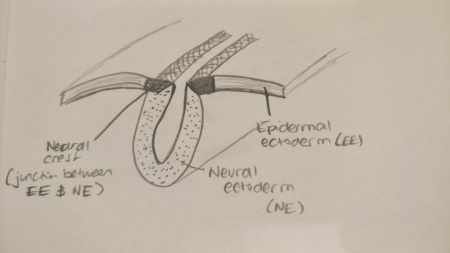
The "neural crest" is a structure in the embryo and is the junction between the neural and epidermal ectoderm. It is exclusive to vertebrates and forms a range of structures[1]. The neural crest contributes a large number of cells of varying structure and function that directly or indirectly contribute to the development of tissues and organs within the body [2]. In 1868, the neural crest cells were first identified in a chick embryo as a collection of cells known as "Zwischenstrang" by Professor Wilhelm His [3]. Wilhelm His was among the first to provide an explanation for the mechanics governing the developing embryo as well as the physiology and the organs that the differing germinal regions would eventually give rise to. In 1878, the term neural ridge was used to describe this collection of cells but the term neural crest was later coined by Arthur Milnes Marshall in 1879 in a paper he worked on disseminating the knowledge from his research on the development of cranial nerves in chicken embryos. [2].
1890s-1950s The neural crest is the point of origin for spinal/cranial ganglia and neurons. This theory received little criticism and was not contested much by other researchers prior to the 1890s. This is owing to the fact that the neural crest is quite closely related to the neural tube and thus this relationship makes sense. This discovery was made by His and Marshall, however, they found this out independently of one another.In the 1890s, Julia Platt, claimed that odontoblasts as well as the cartilages forming the facial and pharyngeal arch skeletons came from the ectoderm. This created much debate and was contested by many[3].
This is because this theory completely contradicted the germ-layer theory, whereby skeletal tissues originate at the mesoderm and not the ectoderm. The controversies this finding created brought about a slowing down of research, as demonstrated by a gap of almost 40 years between the theory that skeletal tissues originating from the neural crest. Today, it is known that the neural crest does indeed play a role in the development of the skeleton in vertebrates, particularly, the cranial neural crest. Although these studies were occurring, the focus was still primarily on researching pigment cells and ganglia of the spine up until the 1950s, when Sven Hörstadius' major work on the neural crest was published, titled "The Neural Crest: Its properties and derivatives in the light of experimental research". This work focused on experimental data tracing the development of the cartilaginous skeleton derived from the neural crest [2].
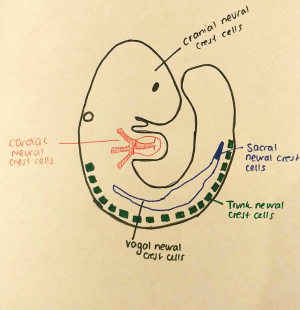
1960s - 1970s In the 1960s, the migration patterns of neural crest cells were studied in avian embryos (birds). This was a shift from studying the embryos of amphibians. This was inspired by studies conducted in the 1960s on neural crest cells migrating from the brain and spinal cord, known as trunk and cranial neural crest cells [2]. The cranial neural crest eventually becomes the bones, cartilage and connective tissues forming the foundation of the face, ears and teeth. The trunk neural crest cells can either become melanocytes or can migrate into sclerotomes which are later contributors to the cartilage of the spine and the dorsal root ganglia [3]. The cells in the trunk neural crest that migrate vertically become the sympathetic ganglia, the nerves proximal to the aorta and the adrenal medulla [4]. In the 1970s many detailed maps signifying the pathways of many of the neural crest cells appeared as well as an understanding that the environment in which the neural crest cells are found plays a major role in their final development as well as the occurrences of abnormalities in the fetus [2].
1980s - 21st century
From the 1980s-1990s, the causative agent of organ transformation from one to another (homeotic patterning), as well as the Hox genes which regulate the axis of most symmetrical animal embryos were founded and studied. The neural crest, which previously was divided into the cranial and trunk regions, was now further divided into the vagal and sacral neural crest, the cardiac neural crest and the cephalic neural crest [2]. The vagal & sacral neural crest gives rise to the parasympathetic ganglia found in the gut. Without these ganglia, peristalsis, is not possible [4]. The cardiac neural crest contributes to the valves, septa and major blood vessels of the heart, as well as connective tissues and cartilage[2]. This is important for the structure of the heart as well as its overall function, enabling it to move blood around the body efficiently as well as keep pulmonary and aortic circulation separated [4].
Today, knowledge of the neural crest cells, their migration patterns, modes of differentiation, derivatives and apoptosis (cell death) are being studied extensively. This is being done on a comparative basis between different organisms, to add further evidence for evolution [2]. The neural crest is definitely forging a "crest" between the fields of developmental and evolutionary biology, as it is a structure shared exclusively by all vertebrates. Invertebrates do not derive their specialised cells from the neural crest as they do not have one, rather, they derive these from the endomesoderm [1].
Future directions
Since its discovery by His, the neural crest field has made great progress, from studies performed on the structure, to analysis of the molecules and whether certain aspects of the neural crest are specific to a single species of organism, or to all vertebrates collectively. Future work on the cranial neural crest needs to be done as well as identifying and categorising the networks responsible for the proliferation and death of cells, as well as how the cells move and migrate, as well as the gene regulatory networks (GRNs) that regulate the synthesis of proteins. Advances in technology will undeniably lead us to more answers on the subject [1].
Developmental time course
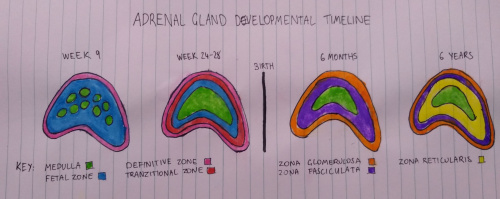
The adrenal gland has two distinct sections, the cortex and the medulla, both with different embryonic origins. The cortex accounts for 90% of the adrenal glands and arises from intermediate mesoderm. The medulla only accounts for 10% of the adult adrenal glands, however it has neural crest embryonic origin. The medulla consists of chromaffinoblast cells which are migrant neuroblast cells from the neural crest, therefore the adrenal medulla is a component of the sympathetic nervous system.[5] Neural crest cells replicate in week 7 and begin to differentiate in week 8, the cells then migrate to the developing adrenal gland in week 9 of development.[6][7] The neural crest cells infiltrate the cortex and the chromaffin cells are scattered islands in the cortex.[8] Throughout development the cells will become more compact in the centre of the gland, during this period of development the adrenal gland is growing rapidly. The gland is abnormally large until the second trimester and the medulla is much thicker prenatally.[7][5]
Embryonic origins
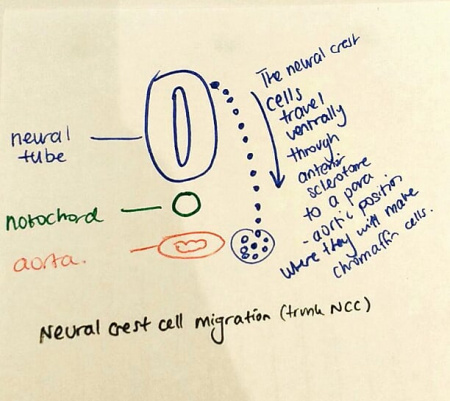
The adrenal gland is made up of the adrenal cortex and adrenal medulla, which both have different embryonic origins. The adrenal medulla arises from the neural crest tissue, found near the level of the coeliac plexus & sympathetic ganglion at somites 18-24 [9]. Specifically, this neural crest tissue comes from the trunk neural crest cells (see above figure to determine the approximate location in an embryo) [4]. The trunk neural crest coordinates the development of the endocrine system, secretory cells, the peripheral nervous system and, to some degree, skeletal development, as well as innervation of the intestine [10]. The trunk neural cells arise caudally, undergo an epithelial to mesenchymal transition and follow three migratory pathways [11].
- A dorsolateral pathway (between ectoderm and somites), these become melanocytes, travel up to the point of the dermis and become a major part of the hair follicles and skin [4]. - A ventrolateral pathway (through the somites) - A ventromedial pathway (between neural tube and posterior schlerotome)[11].
Migration of neural crest cells from the sympathetic ganglion is what leads to the development of the adrenal medulla. In week 8 of development, immature cells called neuroblasts migrate through to the inner portion of the medulla, where they become the adrenal medulla [12]. Chromaffin cells are neuroendocrine cells and are found in the sympathetic ganglia and make up the majority of the adrenal medulla[12]. They synthesise and release a range of hormones in the body and arise from the temporary neural crest. The term chromaffin was inspired by the staining capacity of these cells when they came into contact with chrome salts. They make, store, export and use catecholamines, responsible for making noradrenaline and originate at the caudal region of somites 18-24 of the neural crest, also known as the adrenomedullary region [12].
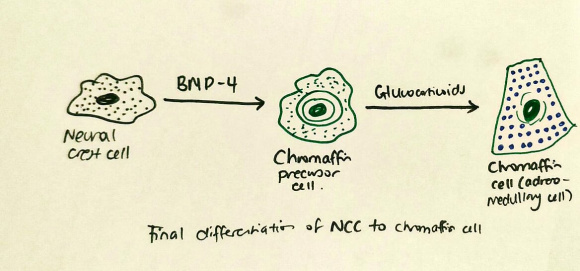
For cells to leave the neural crest and begin their migration, certain conditions need to be met, that is, the cells need to be loosely connected, their tight junctions becoming relaxed, initiated by "Slug protein" and a loss of N-Cadherin which also leads to the loosening of these junctions. The surrounding matrix as well as chemotactic and stem cell factors of the neural tube are then what dictates how the neural crest cells move, some proteins stopping their migration to that area and others encouraging the movement [4]. After splitting apart, the first neural crest cells move ventrally and pass into the spaces between the somites and then, through the anterior portions of each segment until they arrive at the para-aortic sites, where they become the cells of the sympathetic ganglia and the adrenal medulla [12]. BMP-4 (bone morphogenetic protein 4) then acts on these neural crest cells, preventing them from becoming cells that have a neural function and causing them to become chromaffin cells at the adrenal medulla. Glucocorticoids then play a role in maintenance of chromaffin cells in postnatal life, this was only found recently, as previously it was thought that glucocorticoids were responsible entirely for the differentiation of neural crest cells into chromaffin, or adrenomedullary cells [13].
Developmental/adult function
Normal Structure and Function of the Adrenal Medulla
The cells of the adrenal medulla are derived from the neural crest as opposed to the mesodermal origins of the cortex. The medulla contains secretory cells called chromaffin cells, due to the agents they produce when oxidised, such as chromate. These cells secrete epinephrine and norepinephrine in response to various substances such as acetylcholine.
There are three types of cells in the adult adrenal medulla:
1) Epinephrine cells
2) Norepinephrine cells
3) Small granule-containing cells (SGCs)
These cells also produce various other peptides such as substance P and neurotensin. The adrenal medulla also contains presynaptic sympathetic ganglion cells. [14]
These cells have unique neuroendocrine characteristics as a result of their neural-crest origin. They receive preganglionic innervation by thoracic splanchnic nerves, and could almost be considered a specialised sympathetic ganglion. With postganglgionic bodies, cells of the medulla are densely clustered around their vasculature for the secretion of hormones into the bloodstream to moderate the concentration of epinephrine and norepinephrine.
Related Anatomy
The tissue and organ structure of the adrenal medulla should be understood with regard to its specialised function within the sympathetic nervous system.
The medullary region of the adrenal glands is tasked with the endocrine secretions of adrenaline and nor-adrenaline in response to environmental stressors that are signalled for by the sympathetic nervous system. That is, the secretion of fight-or-flight response hormones in order to restrict vasculature to the trunk and increase vascular activity in the peripheral musculature.
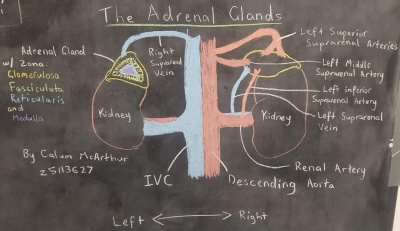
The adrenal glands are supplied by several branches of the great vessels in the abdominal cavity. The secreted catecholamines in the medulla are directly able to pass to the blood stream this way.
These adrenal glands and their contents are retroperitoneal in the adult and varied in shape, with the left often being semilunar and right being pyramidal. Nervous supply of the adrenal glands is achieved by contributions from the splanchnic nerves of the celiac plexus. [15]
Role of the Adrenal Medulla
Understanding the biochemistry of catecholamines is necessary to see how the adrenal medulla is designed in the stages of embryology and how it is suited for life in the neonate and adult.
The epinephrine and norepinephrine in the neonate and adult work by primarily changing the osmoregulatory state of vasculature in organs. With the exclusion of their neuromodulatory and neurotransmitter functions, epinephrine and norepinephrine are mainly tasked with the control of sympathetic and parasympathetic supplies.
Norepinephrine is a constrictor of peripheral vasculature by antagonising the action of surface receptors expressed on the endothelium of blood vessels, specifically Alpha-1 and Alpha-2 receptors, such that vascular resistance increases.
Epinephrine is both a vasoconstrictor and vasodilator, depending on what receptors it attaches to. As a non-selective adrenergic agonist, it acts on Alpha-1, Alpha-2, Beta-1, Beta-2 and Beta-3 receptors that are found throughout the body's tissues, yielding many different physiological responses. [16]
Molecular mechanisms/factors/genes
Genes and Transcription Factors Involved with the Adrenal Medulla's Development
Members of the SOX (SRY-Box) gene family have multiple key contributors to Neural Crest in the Adrenal Medulla.
Mouse models have demonstrated that SOX-10 knock-outs (mice whose DNA has been engineered to not express SOX-10) do not have an adrenal medulla. There has also been suggestion that SOX-8,9 and 10 are all strongly related to the migratory patterning of neural crest cells to the developing adrenal glands.
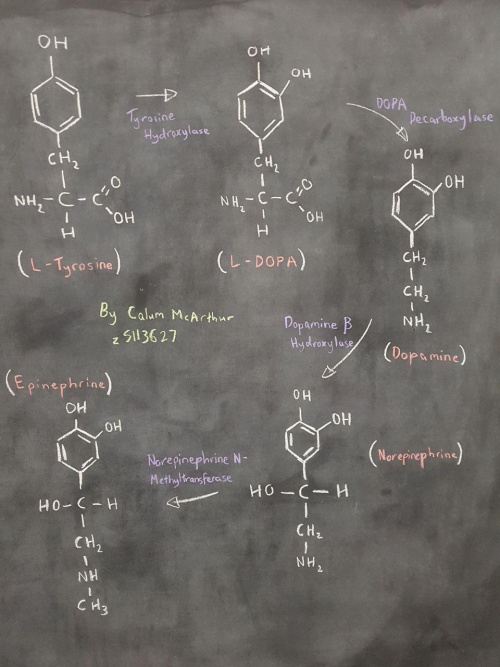
The TH gene (for Tyrosine Hydroxylase) encodes the aforementioned enzyme in the adrenal medulla and central nervous system. Tyrosine Hydroxylase is crucial in biochemical pathways and cascades for the synthesis of catecholamines and other CNS neurotransmitters. The conversion from L-Tyrosine to L-DOPA is dependent upon the catalytic action of Tyrosine Hydroxylase. From there, L-DOPA can make Dopamine and eventually Epinephrine and Norepinephrine as well.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2291442/ https://www.ncbi.nlm.nih.gov/pubmed/19396395
Abnormalities/abnormal development
Abnormalities of the Adrenal Medulla are much less common than its mesoderm-derived shell of the Adrenal Gland. Pheochromocytoma is the most notorious abnormality of the Adrenal Medulla.
Animal models
Animal models are an integral part of research in embryology. In particular due to the moral concerns regarding the use of humans in scientific research. As a result different animals are used as substitutes to simulate the same environments and hope to achieve results that would also be able to represent humans as well. Prenatal adrenal gland development has been described in a number of scientific reports dating from the 1900s to studies in more recent years. These involved a variety of animal models such as ox, sheep, swine and most commonly mice.
Chromaffin cells (in rat models)
There has been extensive research conducted into the adrenal chromaffin cells and their embryological developments. As explained above nueral crest cells are pluripotent meaning they are able to differentiate into multiple different cells. The neural crest cells give rise to chromaffin cells of the adrenal medulla.
To study the formation process of the adrenal medulla in the embryonic period, we visualized chromaffin cells of rat embryos at 13 to 17 days of gestation using anti-tyrosine hydroxylase (TH) antiserum, and created three-dimensional images from serial tissue sections. Between 13 and 15 days of gestation, TH-positive cells (chromaffin cells) migrated from a group of TH-positive cells present dorsal to the adrenal primordium via the medial cranial end of the adrenal primordium into the adrenal primordium. At or after 16 days of gestation, the adrenal capsule was formed except on the ventral aspect of the cranial end of the adrenal gland, from which TH-positive cells penetrated into the adrenal gland.(Pubmed: 15240937)
Past research has reported that nueral crest cells migrate into sympathetic ganglia and the adrenal cortex and almost completely convert t chromaffin cells by 19 days of gestation, forming the adrenal medulla. Since TH is used in this study as an indicator of chromaffin cells (adrenal medullary cells) is an enzyme involved in the early stage of the synthetic pathway of adrenaline and noradrenaline, the TH - positive cells observed in this study may include not only chromaffin cells but also sympathetic ganglion cells and SIF cells. It was previously thught that when neural crest - derived cells migrated via the sympatheti chain gangli into the adrenal gland or preaortic ganglion, they took different pathways to the respective destination at the time of passage through the ganglia of the sympathetic trunk. However, the reconstructed images in this study showed that the pathway of neural crest - deriveed cells from the ganglia of the sympathetic trunk to the adrenal medulla overlapped with the pathway to the preaortic ganglion. We speculate that neural crest cells use the same pathway to migrate to the ganglia of the sympathetic trunk, to the adrenal gland, and to the preaortic ganglion, this onclusion is good agreement of the suggestion by Ahoren. Ahonen suggested that some neural crest cells continue migration from the chain ganglia to the lateral sides of aorta, where they form the perirenal ganglia and adrenal medulla, and finally to the ventral side of the aorta to form the preaortic sympathetic tissue. However, that report only showed the several transverse sections of the fetal trunk for the a demonstration of the migration route of neural crest cells. In this study, using three dimensional reconstructed images, we aimed to observe how TH-labeled chromaffin cells penetrate into the adrenal anlage to form the adrenal medulla and whether the migration route of TH - positive cells from the adrenal connects the preaortic sympathetic ganglia (M.Yamato, R. Yanai, K. Arishima, 2004)
Prenatal adrenal gland development has been described in numerous published reports covering a wide variety of species, including the ox (Katznelson, 1966; Wrobel and Suss, 1999), sheep (Davies, 1950; Wintour et al., 1975; Upadhyay and Zamboni, 1982; Naaman‐Reperant and Durand, 1997; Grino, 2004), swine (Sokolov et al., 2006) and mouse (Waring, 1935; Ikeda et al., 1994; Sass, 1996; Nyska and Maronpot, 1999; Bland et al., 2003; Val et al., 2007). Adrenal gland development also has been extensively described for humans as well (Kolliker, 1879; Minot, 1892; Zuckerkandl, 1912; Wieman, 1920; Ikeda et al., 1981; Langlois et al., 2002; Hanley and Arit, 2006).
https://www.sciencedirect.com/science/article/pii/S0925477302004550 http://dev.biologists.org/content/develop/126/13/2935.full.pdf
Current research (labs)
The findings presented until now have focused on the mechanisms controlling migration along the dorsolateral path. In comparison, our understanding of the mechanisms controlling NCC migration along the ventral path are complicated by the fact that this population comprises multiple precursors that form different derivatives in distinct regions of the embryo. For example, ventrally migrating NCCs either stop within the sclerotome in close association with the neural tube to form neurons and glia of the sensory nervous system (i.e. the dorsal root ganglia [DRG]), while other NCCs continue to migrate further ventrally to form the autonomic nervous system (i.e. sympathetic ganglia and chromaffin cells of the adrenal gland)
Adrenomedullary chromaffin cells are catecholamine (CA)-producing cells originating from trunk neural crest (NC) via sympathoadrenal progenitors (SAPs). We generated NC and SAPs from human embryonic stem cells (ESCs) and induced pluripotent stem cells (iPSCs) in vitro via BMP2/FGF2 exposure, ascertained by qPCR and immunoexpression of SOX10, ASCL1, TFAP2α, and PHOX2B, and by fluorescence-activated cell sorting selection for p75NTR and GD2, and confirmed their trunk-like HOX gene expression. We showed that continuing BMP4 and curtailing FGF2 in vitro, augmented with corticosteroid mimetic, induced these cells to upregulate the chromaffin cell-specific marker PNMT and other CA synthesis and storage markers, and we demonstrated noradrenaline and adrenaline by Faglu and high-performance liquid chromatography. We showed these human cells' SAP-like property of migration and differentiation into cells expressing chromaffin cell markers by implanting them into avian embryos in vivo and in chorio-allantoic membrane grafts. These cells have the potential for investigating differentiation of human chromaffin cells and for modeling diseases involving this cell type.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5768882/
Glossary
Reference list
- ↑ 1.0 1.1 1.2 Bronner ME & LeDouarin NM. (2012). Development and evolution of the neural crest: an overview. Dev. Biol. , 366, 2-9. PMID: 22230617 DOI.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Hall BK. (2008). The neural crest and neural crest cells: discovery and significance for theories of embryonic organization. J. Biosci. , 33, 781-93. PMID: 19179766
- ↑ 3.0 3.1 3.2 Bronner ME. (2012). Formation and migration of neural crest cells in the vertebrate embryo. Histochem. Cell Biol. , 138, 179-86. PMID: 22820859 DOI.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 Gilbert SF. Developmental Biology. 6th edition. Sunderland (MA): Sinauer Associates; 2000. The Neural Crest. Available from: https://www.ncbi.nlm.nih.gov/books/NBK10065/
- ↑ 5.0 5.1 El-Nahla SM, Imam HM, Moussa EA, Elsayed AK & Abbott LC. (2011). Prenatal development of the adrenal gland in the one-humped camel (Camelus dromedarius). Anat Histol Embryol , 40, 169-86. PMID: 21175739 DOI.
- ↑ Ross IL & Louw GJ. (2015). Embryological and molecular development of the adrenal glands. Clin Anat , 28, 235-42. PMID: 25255746 DOI.
- ↑ 7.0 7.1 Kempná P & Flück CE. (2008). Adrenal gland development and defects. Best Pract. Res. Clin. Endocrinol. Metab. , 22, 77-93. PMID: 18279781 DOI.
- ↑ Quinn TA, Ratnayake U, Dickinson H, Nguyen TH, McIntosh M, Castillo-Melendez M, Conley AJ & Walker DW. (2013). Ontogeny of the adrenal gland in the spiny mouse, with particular reference to production of the steroids cortisol and dehydroepiandrosterone. Endocrinology , 154, 1190-201. PMID: 23354096 DOI.
- ↑ Barwick TD, Malhotra A, Webb JA, Savage MO & Reznek RH. (2005). Embryology of the adrenal glands and its relevance to diagnostic imaging. Clin Radiol , 60, 953-9. PMID: 16124976 DOI.
- ↑ Vega-Lopez GA, Cerrizuela S & Aybar MJ. (2017). Trunk neural crest cells: formation, migration and beyond. Int. J. Dev. Biol. , 61, 5-15. PMID: 28287247 DOI.
- ↑ 11.0 11.1 Gammill LS & Roffers-Agarwal J. (2010). Division of labor during trunk neural crest development. Dev. Biol. , 344, 555-65. PMID: 20399766 DOI.
- ↑ 12.0 12.1 12.2 12.3 Huber K, Kalcheim C & Unsicker K. (2009). The development of the chromaffin cell lineage from the neural crest. Auton Neurosci , 151, 10-6. PMID: 19683477 DOI.
- ↑ Unsicker K, Huber K, Schober A & Kalcheim C. (2013). Resolved and open issues in chromaffin cell development. Mech. Dev. , 130, 324-9. PMID: 23220335 DOI.
- ↑ Livett BG, Marley PD, Wan DC & Zhou XF. (1990). Peptide regulation of adrenal medullary function. J. Neural Transm. Suppl. , 29, 77-89. PMID: 1694230
- ↑ Rosol TJ, Yarrington JT, Latendresse J & Capen CC. (2001). Adrenal gland: structure, function, and mechanisms of toxicity. Toxicol Pathol , 29, 41-8. PMID: 11215683 DOI.
- ↑ Nakashima A, Hayashi N, Kaneko YS, Mori K, Sabban EL, Nagatsu T & Ota A. (2009). Role of N-terminus of tyrosine hydroxylase in the biosynthesis of catecholamines. J Neural Transm (Vienna) , 116, 1355-62. PMID: 19396395 DOI.