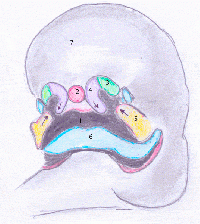2011 Group Project 11
| Note - This page is an undergraduate science embryology student group project 2011. |
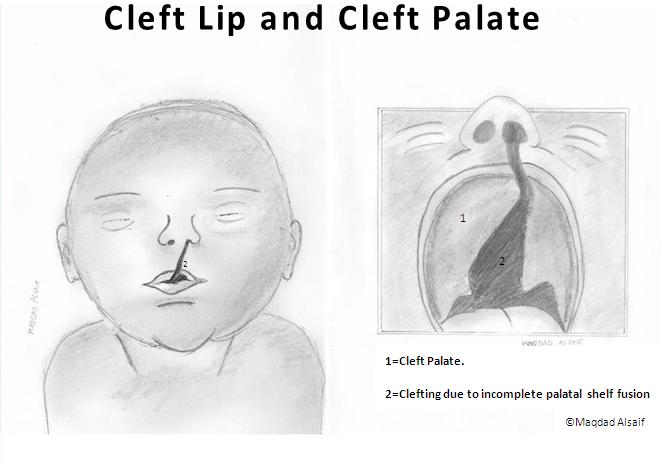
Cleft Palate and Lip
Introduction
The clefting of the palate and the upper lip is a congenital deformity that results from developmental abnormality during gestation. The deformity can present itself individually as a cleft lip or palate, or together, as cleft lip and palate. Until 1986, there was limited understanding about the condition. Since then, there has been remarkable improvement in the overall understanding of the genetic and prenatal origin of the condition as well as improved surgical and treatment procedures[1].
The condition has been attributed to numerous syndromes of which Trisomy 13 has been identified as the most commonly associated chromosomal anomaly. Malformations associated with Trisomy 13 have been found to occur in the face, and many other regions which include but are not limited to the skeletal system and the gastrointestinal system.
Whilst the condition has been known to inflict heavy emotional trauma on the parents and the child, as well as being able to induce many complications in the patient, it is generally treatable with surgical intervention. Treatment of clefts is extremely specific to individuals, depending on the overall health of the child and the severity and location of the cleft(s). Surgery to repair a cleft lip is usually done between 10 and 12 weeks of age. Palatoplasty is the term used to describe cleft repair procedure which is ideally performed between nine and 18 months. Additional surgeries are often needed to achieve the best results. In addition to surgery, the patient may receive extensive follow up treatment from a multidisciplinary team of professionals addressing consequent issues of speech, hearing, growth, dental, and psychological development.
Current researchers around the world are focused on prevention of this complicated abnormality by identifying the genetic and environmental drivers of cleft lip and palate. There is elevated research interest in early screening and effective neonatal detection of the condition which will help the parents and their families prepare psychologically for the long term consequences of a child born with the condition [2]
History
In ancient times, many congenital deformities, including the cleft lip and palate, were considered to be evidence of the existence of an evil spirit in the affected child. The reaction of the birth of a deformed child has varied widely from culture to culture where the infant was often removed from the tribe or cultural unit and left to die in the surrounding wilderness. This was a practice that was common in Antiquity and still happens today in certain parts of African tribes. In Sparta, the unfortunate newborns were abandoned on Mount Tagete, while in Rome they were drowned in the Tarpeian rock [3].
The renowned philosopher, Plato, discussed it in one of his dialogues in the Republic, explaining that it was indeed a means of eradicating evil omens and preserving the soundness of the race.[4]
This state of lack of knowledge is evident up until 1889, when Keating published his opinion that a series of congenital anomalies were provoked in each case, by the mother looking at a person with similar deformity during her pregnancy.[5] The first persuasive explanation regarding the actual causation of the condition offered by Philippe Frederick Blandin between 1838 to1896 has revolutionised the perception of the condition. It sparked interest among physicians to investigate further into embryological development and the possible origin of clefting.[6]
From 1896 to the 19th century, both understanding and the surgery of cleft lip witnessed remarkable improvements. Surgeons around the world continued to research and propose refinements on the early procedure striving to accomplish precise and reproducible methods.
- In 1295- 1351, Jean Yperman noted that cleft had a congenital origin classifying the various forms of the condition and outlining corresponding treatment principles. [3]
- In 1460, Heinrich von Pfolsprundt passed stitches through all the layers to repair the cleft instead of simply suturing the skin accomplishing a better repair of the lip. [3]
- In 1537-1619, Fabricius ab Aquapendente first described the embryological basis of cleft lip. [3]
- In 1561, Pierre Franco and Ambroise Pare described the techniques of correction of both unilateral and bilateral cleft lips in Traite des Hernies using dry sutures, pins and a triangular bandage. He emphasized that an accurate surgery procedure can produce an inconspicuous scar, an outcome which was “particularly desirable when the patient was a girl”.[7]
- In 1795, Pierre Joseph DeSault, a French pioneer of bilateral cleft surgery at La Charité and Hôtel-Dieu in Paris, developed a new method for teaching anatomy and taught the procedure of bilateral cleft surgery[8]
- In 1808, Meckel published his theory of the embryological development of the lips which stated that the lips formed from five distinct processes which eventually united, three for the upper lip and two for the lower lip. [3]
- In 1838, Philippe Frederick Blandin suggested that facial cleft resulted from a failure of the premaxilla and the maxillary segments to unite at a later stage in development. [9]
- In 1844, Germanicus Mirault introduced a triangular flap from the lateral side into a gap created by making a horizontal incision on the medial side of the lip creating a nostril floor and reducing the linear scar on the lip. [3]
- In 1872, Jacob August Estlander, a Finnish surgeon, introduced a method to correct the mid-face retrusion that was left by the bilateral lip repair process. He recommended a wedge resection of the vomer which allowed the protruding premaxilla to be pushed back. [3]
- In 1935, Faltin, another Finnish surgeon, recommended that the procedure described by Jacob A Estander be abandoned because it routinely left serious maxillary retrusion. [10]
- In 1960, Peter Randall standardized the triangular flap repair method with accurate and reproducible measurements. [11]
- In 1965, W. M. Manchester introduced a procedure for the bilateral cleft surgery. [12]
- In 2000, Hua Xi Kou Qiang demonstrated that simultaneous primary palate repair and alveolar bone grafting are safe for unoperated cleft palate patients, and this procedure should be performed in unoperated cleft palate patients above 8 years old. [13]
- In 2008, J Y Wong published a study describing that craniofacial anthropometry using the 3dMDface System is applicable and reliable. Application of software algorithms merging the different overlapping images into a single three-dimensional image can remarkably improve landmark identification[14]
- In 2010, B Mishra along with a team of Indian doctors published a study concluding that Nasoalveolar molding can be a useful adjunct for management of cleft lip nasal deformity. It serves as a cost-effective technique that can diminish the number of future surgeries such as alveolar bone grafting and secondary rhinoplasties in under developed countries[15]
Epidemiology
The true prevalence rate of cleft lip and palate is subject to controversy. Current genetic research does not address and differentiate between syndromic and non syndromic cases. A lack of awareness of the categories and prevalence rates can lead to poor genetic counselling which leads to stronger negative effects on families. Generally cleft lip with or without cleft palate is believed to be 1 case per 700 live births while the prevalence of non syndromic cleft palate alone is believed to be 1 case per 2000 live births. [16] Population-based studies will be more appropriate in investigating a worldwide epidemiology. In addition, one should also consider spontaneous abortions, elective terminations, stillborn foetuses, and babies that died shortly after birth to get the true numbers of associated anomalies. It is also essential that every child should be thoroughly examined immediately after birth for the associated anomalies, because children with severe malformation may not survive long. Research has identified that the distribution of clefting is influenced by the sex of the individual. [17]
Nonsyndromic cleft lip with or without cleft palate has higher prevalence among males while non syndromic cleft palate is more prevalent among females. Interestingly the rate of occurrence in one of two monozygotic twins is 50%. Even though the frequency of nonsyndromic cleft palate differs very little between racial lines, distribution of cleft lip with or without cleft varies widely with ethnicity. While Native Americans have the highest rate of occurrence, African Americans show the lowest. [17]
The rate of non syndromic cleft palate occurrence is summarised as follows: [16]
- 1 case per 1500-3000 Caucasians
- 1 case per 200-5000 African Americans
- 1 case per 1600-4000 Asians
- 1 case per 1700 Native Americans
Estimate of cleft lip with or without cleft palate is as follows:[17]
- 1 case per 775-1000 Caucasians
- 1 case per 1300-5000 African Americans
- 1 case per 400-850 Asians
- 1 case per 230-1000 Native Americans
Twice as many males as females are affected by this condition. In contrast, nonsyndromic cleft palate occurs in an equal male-to-female distribution. Besides gender and racial distribution, recent epidemiological evidence strongly suggests that infants born with clefts have a shorter lifespan and may have a higher incidence of cancer and psychological disorders[18]
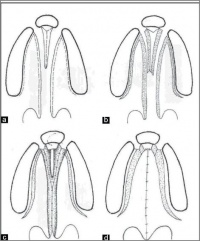
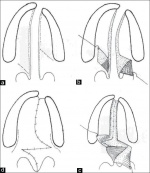
Types of Cleft Palate/Lip
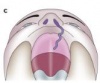
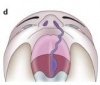
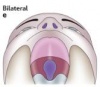
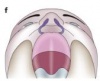
There are different types of both cleft palates and cleft lips, each with varying degrees of severity. Cleft palates and lips may either occur together or individually. Variations of cleft palate/lips include:
| Type | Comment | Picture |
|---|---|---|
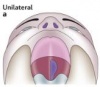
| Unilateral Cleft Palate | This type of cleft refers to a cleft of the soft palate that occurs on one side of the palate. The cleft starts medially and extends laterally. | |
| Unilateral Cleft Lip | This type of cleft refers to a cleft of the lip that has only occurred on one side of the lip. | |
| Unilateral cleft lip with a cleft hard palate | This refers to a cleft that has extended through the lip and into the hard palate. This cleft is only on one side of the lip and palate. | |
| Unilateral cleft lip with cleft hard and soft palate | This type of cleft refers to a cleft that extends through the lip, hard palate and into the soft palate. This cleft also occurs on one side only. | |
| Bilateral cleft palate | This refers to a cleft of the soft palate which occurs on both sides of the palate and appears as an opening medially. | |
| Bilateral cleft lip | This refers to a cleft of the lip that has occurred on both sides of the lip. There are many variations of this. | |
| Bilateral cleft lip with cleft hard palate | This refers to a cleft of the lip that has extended into the hard palate and occurs on both sides. | |
| Bilateral cleft lip with cleft hard and soft palate | This refers to a cleft that has occurred on both sides of the lip and has extended into both the hard and soft palates resulting in a medial opening of the soft palate.[19] |
There are many variations of a cleft lip. Cleft lips may occur unilaterally or bilaterally. A unilateral cleft lip presents with only one cleft, either complete or incomplete. As with a cleft palate, a cleft lip may also be incomplete or complete. The bilateral cleft lip may also be further divided into Binderoid bilateral complete cleft lip and palate, bilateral complete cleft lip and intact secondary palate, bilateral incomplete cleft lip and asymmetrical bilateral (complete/incomplete) cleft lip. [20]
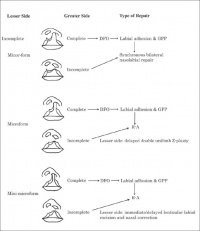
One in four bilateral cleft lips are asymmetrical. They are incomplete on one side and complete on the other. The incomplete side of the bilateral cleft lip varies in severity and the level of severity impacts on the treatment. These lesser forms of incomplete bilateral cleft lips can be divided into minor-form, micro-form, and mini-microform depending on the degree of the disruption at the vermilion-cutaneous junction. [20]
Minor-form, micro-form and mini-microform are categorised based on defining features. Minor-form and micro-form both have deficient vermilion on the medial side of the cleft whilst the mini-microform has a discontinuous vermilion-cutaneous junction. The level of nasal deformity also contributes to the differences with the range of nasal deformity ranging from visible nasal deformity in the minor-form to only a depressed sill in the mini-microform.
Other features of the minor-form include:
- Hypoplastic median tubercle
- Notched vermilion-cutaneous junction extending 3 mm or more above the normal Cupid’s bow peak
- Cutaneous groove and muscular depression (accentuated by puckering)
Other features of the micro-form include:
- Muscular depression along the philtral line, sometimes with a prominent medial component of the philtral ridge
- Medial vermilion-cutaneous point less than 3 mm above the normal Cupid’s bow peak
- Variable glabrous strip in the lower cutaneous lip
Other features of the mini-microform include:
- Variable muscular depression, particularly below the nostril sill
- Level Cupid’s bow peaks
- Notched free mucosal margin [21]
Aetiology
Cleft lip and palate often occur together, however, present different aetiologies. The development of cleft palate and lip have been attributed to various genetic factors, environmental factors, or a mixture of the two. [22]
Cleft lip and cleft palate have been identified to be caused by developmental problems incurred during any stage of the developmental process. The inadequate growth of the palatine shelves, the failure of the shelves to elevate at the correct time and their failure to fuse at the boundaries have been identified to be the more common factors that lead to cleft palate. On the other hand, cleft lip has been attributed to a plethora of developmental issues that include the underdevelopment of the mesenchyme of the maxillary prominence and the medial nasal process. It is these developmental issues that have been blamed on environmental factors, genetic factors or an interplay between the two. [23] [22] [24]
Environmental factors that include the consumption of alcohol, drugs that contain Vitamin A, and dietary deficiencies are just some of the numerous potential causagents of clefting. The process during which the palatal shelves undergo fusion for instance is particularly vulnerable to the effects of multiple toxic substances, environmental pollutants or nutritional imbalances. [23][22]
On the genetic front, clefting has been identified to be prevalent in some family lines, indicating the presence of a genetic component to the condition. In some cases, clefting has been isolated to be a byproduct of other disorders and syndromes, such as the Patau or the Stickler's syndrome. However, in many other cases, it is difficult to isolate a primary syndrome that can be attributed to cause clefting. This could possibly be attributed to the incomplete genetic understanding of midfacial development. [23]
Development
The development of cleft palate and/or lip can be attributed primarily to growth issues during embryonic and fetal development, which takes place across 4 weeks. The palate and the lips develop from 3 of the 5 prominences that surround the stomodeum of the fetus: the frontonasal prominence, the right maxillary prominence and the left maxillary prominence.[25]
At week 5 , the surface ectoderm of the ventrolateral part of the frontonasal prominence undergoes thickening to form the nasal placodes. The remaining portions of the frontonasal processes then grow and bulge around these placodes to form the nasal pits and the nasal processes. The mesenchyme of the maxillary process continues to grow, pushing the nasal pits medially. The upper lip consists of the maxillary processes and both the medial and lateral nasal processes- which have commenced fusion.[25]
At the beginning of week 6 the maxillary and medial nasal processes undergo rapid growth and push the lateral nasal processes rostrally. The medial nasal process and the maxillary process also undergo fusion distally. Active fusion takes place between the lateral nasal and medial nasal processes- commencing initially at the posterior part of the nasal pits, and proceeding henceforth in an anterior direction.[25]
From week 6 and week 7, epithelial fusion continues between the maxillary, and the 2 nasal processes.[25] The maxillary processes continue fast growth and this results in the protrusion of the nasal pits and medial nasal processes mediofrontally.[26] The ongoing growth and confluence of the medial nasal and maxillary mesenchyme result in the groove located in between the medial nasal processes leveling out and becoming smooth. Fusion between the medial and lateral nasal processes takes place, resulting in nasal pits to be transformed into nasal chambers and ducts.[25]
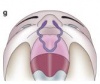
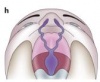
Week 7 heralds the connection of the nostrils to the posterior oral cavity. The medial nasal and maxillary processes also undergo fusion, resulting in the remodeling of the lower edge of the nostrils. By the end of week 7 and beginning of week 8, the epithelial seams and the mesenchymal confluence between the medial nasal and maxillary processes disintegrate, thereby completing the formation of the upper lip. During this period, at about day 45, bilateral palatal shelves arise from the maxillary processes. Initially, these processes grow vertically down the side of the tongue, but then subsequently elevate to a horizontal position about the dorsal surface of the tongue. A midline epithelial seam, which undergoes degeneration to form a continuous mesenchyme, is then formed as the medial edge of the palatal shelves fuse. In the mesenchyme of the hard palate, the osteogenic blastemata for the palatal processes of the maxillary and palatine bones differentiate, while in the soft palate, patterned myogenic blastemata develop. Palatal development usually ends with the adhesion and subsequent fusion of the palatal shelves in the 9th week of fetal development.[27]
Research has indicated that an abnormality in any stage of palate development could potentially lead to a clefting of the palate.[27] Similarly, an abnormality that leads to a failure of fusion to successfully take place between the various processes can lead to cleft lips.[25]
Neuroembryology and Functional Anatomy of Craniofacial Clefts
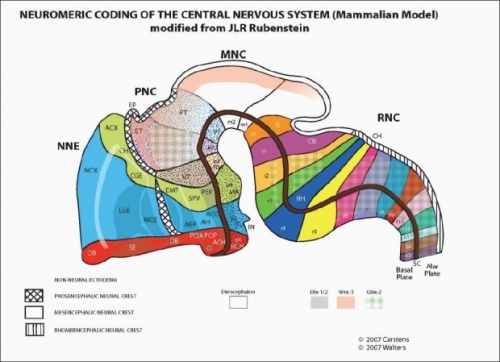
Embryological anatomy is the foundation upon which all treatment methods for craniofacial anomalies such as cleft must be based. Craniofacial clefts characterize states of inappropriate (excess or deficiency)distribution within and between specific developmental fields. The neuromeric mapping of the embryo is the primary denominator for understanding normal anatomy and pathology of the head and neck. [28]
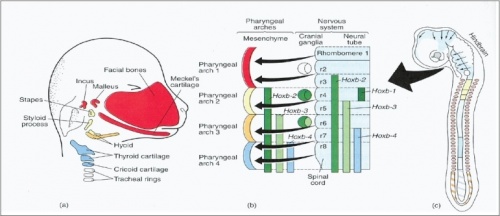
The central nervous system of the human embryo develops in discrete segmental craniocaudal units called neuromeres. Specific genes known as Hox genes define the anatomical boundaries of each neuromere. [29]
The neural crest in each neuromeric level is responsible for supplying it's specified zones of ectoderm and mesoderm; corresponding proteins are also expressed by the neural crest cells that complement the proteins secreted by the neural tube. The unique genetic markers associated with each neuromere can assist to identify the origins of craniofacial tissues that are eventually developed[30]
The neuromeric model facilitates a precise mapping of the anatomical site of origin for the zones of ectoderm and endoderm supplied by a particular area of the nervous system. The density of neural crest cell population in these areas also can help us understand their individual roles in generating the structures they do.[28]
The neural crest cells migrate and differentiate to develop specific craniofacial tissues. These zones are called development fields. The neural crest cells from each neuromere also instigate the formation of nerves and arteries which will eventually supply the individual fields. [31] These fields migrate from their origin in a strictly synchronised spatio-temporal sequence. They then cluster around the developing brain and self assemble which defines the interconnection between fields. The correct development of one field might be reliant on the presence and positioning of another field. As a consequence any abnormality in an individual field may influence the development of an otherwise regular adjacent field. Craniofacial clefts feature an excess, deficiency or absence of an embryonic development field and the resultant impact on its contiguous fields. [32]
Different mechanisms which cause interruption in neural crest cell movement give rise to different classes of field abnormalities evident in the developing face.
- Errors in the neuromere of origin result in premigratory deficiencies.
- Neural crest population dying before reaching their destination result in migratory deficiencies
- Faulty communication among mesenchyme and epithelial “target zone,” or a faulty epithelial “programme” result in post migratory deficiencies.
Thus the ultimate common pathway to field anomalies is inadequate stimulation of vascular support for emergent tissues in the specified zone.
There are four dimensions of development that field anomalies effect in a developing embryo’s facial morphology. These are known as the four Ds of cleft progression and are responsible for a specific dimension of cleft formation as listed below: [33]
- deficiency is axial
- displacement is coronal
- distortion is temporal
- division is sagittal
The pathological sequence follows the order of axis specification in the embryo. [34]
A deficiency exists in the functional matrix to begin with which gives rise to the piriform margin. This is then followed by the formation of an abnormal development field. This results into a pattern of displacement in the soft tissue envelope on either side of the cleft. This gives rise to a deficiency in the soft tissue closure of the nasal floor and lip. The effects of such deficiency cause an abnormal anatomy of the septum. Subsequent growth of the osteocartilagenous nasal vault, uncoupling of regular interaction between the skeletal structures, as well as abnormal forces exerted by the per oral musculature result in the characteristic opening-up of the cleft site. [35]
Genes Involved in Clefting
Research interest, in the origin of cleft lip/palate as well as the genetic and environmental factors that induce the condition, picked up in the 1940s. Since then, various studies have been undertaken to elucidate the ambiguity behind this embryonic abnormality. It is widely accepted now that a combination of environmental and genetic factors contribute to the increase in likelihood of clefting of the palate or upper lip during development. Some of the genes that have been identified to have a vital role in the development of CL/CP include:
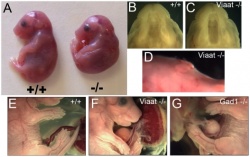
Glutamate decarboxylase 1 (Gad1) and Vesicular inhibitory amino acid transporter (Viaat)
Earlier studies have indicated that GABA signalling plays a significant role in the development of central nervous system and palate formation. It has been hypothesised that two of the variants of GABA signalling pathway contribute to the normal formation of craniofacial structures. These are namely; glutamate decarboxylase 1 (Gad1) and vesicular inhibitory amino acid transporter (Viaat). In a study conducted in mice, the alteration or mutation of these two genes has lead to the development of oral clefts such as cleft palate. This has been performed by the inactiviation of the GABA receptors during the CNS development. As a result, inactivation of these two genes causes a disruption in the palate development. This suggested that the presence of Gad1 and Viaat is important for the central nervous system for normal development of the palate. Therefore, mutations or alterations of these genes in the GABA signalling pathway lead to the non-neural defects including cleft palate as fetal movements during development have been altered.[36]
Transforming Growth Factor α (TGFA)
TGFA is regarded as one of the significant genes that have been studied extensively due to its relevance to the oral clefts. TGFA is a trans-membrane protein that is expressed at the medial edge epithelium (MEE) of fusing palatal shelves. The receptor of this gene, epidermal growth factor receptor (EGFR) is expressed on the degenerating MEE. In a study conducted on mice, it was found that the deletion or alteration of this receptor contributed mostly to the facial medio-lateral defects and high occurance of cleft palate formation. [37] [38]
Transforming Growth Factor β 3 ( TGF β3)
Transforming growth factor family consists of more than 30 ligands, which is believed to be involved in a numerous number of biological functions such as proliferation, differentiation, epithelium-mesenchymal transformation, and apoptosis. TFG β3 is a type of protein, known as a cytokine, which is involved in cell differentiation, embryogenesis and development.
This protein was detected in the epithelial component of the vertical palatal shelf which peaks between 14-14.5 days, prior to the contact of the palatal shelves. Potential roles of the TGF β3 in cellular adhesion, and extracellular formation during the process of palate development have been demonstrated both in vivo and in vitro. The alteration or mutation of this factor via smoking or other factors may result in the failure of epithelial cells during the development of the palate to fuse together. Consequently, the foetus is likely to develop cleft palate abnormality. [38]
Muscle segment homeobox 1 (MSX1)
Muscle segment homeobox 1 (MSX1) is a protein which is encoded by MSX1 gene. The transcripts of this protein are found in several locations such as thyrotrope-derived TSH cells, and thyrotropic tumor TtT97, pituitary cells, and most importantly expressed during embryogenesis. [41] [42] Due to the abundant expression sites of MSX family, it is hypothesized that these proteins might have an essential role in early development of the embryo. [43] It has been discovered that MSX1, a transcriptional repressor, is significant in craniofacial, limb, odontogenesis, and nervous system development and tumor growth inhibition. Alteration in any kind, including mutation of this gene, may result in the formation of nonsyndromic cleft lip and/or palate. The phenotypes of MSX1 merely depends on the locus of mutation which can affect the protein structure and function. For instance, Ser105Stop mutation was found to cause a complete deletion or absence of the MSX1 homoeodomain. This in particular impairs the development of craniofacial structures and causes clefts. [38]
Environmental Factors in Clefting
Environmental factors have been noted to play a large role in inducing clefting during the developmental process. Certain toxins and drugs, as well as the lack of proper nutrition, have been identified to induce especially detrimental effects in certain processes within development as a whole. Three major environmental factors that are able to induce clefting during embryonic and fetal development are smoking, the consumption of alcohol and the lack of proper nutrition.
Smoking Cleft lip and palate is considered to be one of the possible defects associated with maternal smoking. It was found that smoking cigarettes during the period of pregnancy sometimes is associated with cleft defects. The maternal glutathione s-transferase θ-1 (GSTT1) genotype, together with smoking was found to elevate the risk of cleft lip and/or cleft palate by a ratio of 4.9. Moreover, the gene MSX1 genotypes along with maternal smoking resulted to an even higher ratio of oral defects by 7.16 times. [38] [44]
Alcohol Several studies have shown that the teratogenic impacts of heavy alcohol exposure contributed to the incidence of cleft lip and/or cleft palate. It was reported that about 9-18% of infants who have experienced high alcohol exposure ended up with oral abnormalities such as cleft lip/cleft palate. [45] However, a low level of alcohol consumption does not seem to elevate the risk of oral defects. The gene MSX1 was reported to be a major gene that could result in cleft palate or cleft lip. Furthermore, the gene MSX1 was more likely to be altered with the consumption of four drinks or more. It was found that cytochrome proteins may play a significant role in metabolism of endogenous morphogens in the developing fetus. Variants such as CYP2E1, or CYP1A2 were found to increase the risk of oral defects when they were altered or mutated. As a result, the structural development of the fetus was affected. [38] [46]
Dietary (Folic Acid) Maternal nutrition during pregnancy contributes highly to the normal development of the fetus, especially oral and palate development. In studies conducted on mice, the development of the palate was delayed due to the deficiency in folic acid supply. Moreover, insufficient dietary intake of B-complex vitamins and deficiency or excessive amount of vitamin A have been associated with high incidence of abnormal cleft formation. [47] MTHFR (5,10 methylenetetrahydrofolate reductase) is an enzyme of the metabolism of folate and homocysteine and is involved in substrate methylation and in the synthesis of nucleotides. The gene is located on chromosome 1p36.3. It was found that the absent or reduced levels of MTHFR could homocystinuria. It was observed that a high level of homocysteine was detected in mothers with cleft babies as compared with mothers who have normal levels of MTHFR. It has also been hypothesised that variants of enzymes managing the folate metabolism contribute to the oral cleft formations. The gene encoding of the MTHFR enzyme is known to have two common variants; C677T and A1298C. The link between MTHFR variants and cleft lip and/or palate incidences has been much less studied in the literature. [48] [46]
Pathophysiology
The embryonic development of the upper lip and nose requires a precise genetic sequence of events. This cranio-facial development pathway is a very complex process and therefore there are several points during development at which cleft lip or palate can occur. During the third and eighth week, five major facial prominences are fused together. The lips then develop between the third and seventh week followed by the palate between the fifth and twelfth week. Due to this intricate process, multiple genetic and environmental factors will vary in their affect on the type and severity of cleft lip and palate and lead to the malfunction of the various tissues involved.
The maxillary, medial nasal and lateral prominences fuse together via a combination of processes including apoptosis, epithelial bridging and subepithelial-mesenchymal penetration. Cleft lip and cleft palate result when these tissues fail to fuse. Some research suggests that this abnormality is secondary to a defect of mesenchymal growth or epithelial bridging. There is evidence that intracellular signaling pathways and a wide range of errors in genetic programming may interfere with the fusion of median nasal and maxillary prominences. Consequently, the blood supply and musculature are often compromised and lead to malfunction of the lip and palate.[49]
For example, in a unilateral cleft lip, the deep fibres of the orbicularis oris muscle are interrupted by the presence of the cleft and insert into the nasal base (the side of the defect), however, in a normal infant, these muscles will form a concentric muscle around the mouth. Furthermore, the superficial layer of the orbicularis oris muscle changes direction and forms superiorly, parallel to the edges of the cleft and inserts inferior to the columella. This can be seen when infants smile as the base of the nose would spread out laterally.[50]
Usually, fusion of both lateral palatal shelves as well as nasal septum in the anterior posterior direction from the incisive foreman to the uvula is essential for the palate development to progress. The occurrence of cleft palate is often linked with a split uvula. Functional impairment and secondary complications often occur with the gap between both the nasal and oral cavities including problems with speaking, ear infections/hearing loss, aesthetic problems, dental anomalies, psychosocial problems and hyper-nasal voice resonance due to the leakage of air from the nasal cavity.
[51]
Syndromes and Anomalies Associated with Cleft
Cleft lip and/or palate is said to be related to more than 100 syndromes, and Trisomy 13 is the most commonly associated chromosomal anomaly. Associated malformations occur most commonly in the facial region (21%), followed by the ocular system, central nervous system, skeletal system, cardiovascular system, neck, auricular system, gastrointestinal system and urogenital system. [52]
Median facial dysplasia-A facial anomaly associated with cleft
Median facial dysplasia is a definable group of patients typically featuring midline facial deficiencies often accompanied with unilateral or bilateral cleft lip with or without cleft palate. [53] This type of facial underdevelopment usually extends into the corpus callosum of the brain. If there is <90% abnormality in the circumference of the brain, these patients may have associated anomalies of the brain, especially in the frontal corpus callosum. This will then have compromised development of the midface which leads to very early dish face, class III occlusion and severe maxillary hypoplasia. Early detection of these anomalies help to plan the course of treatment.
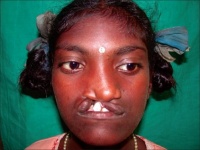
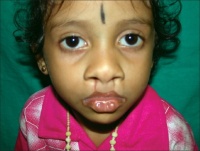
Van der Woude syndrome with lower lip pits-Most common syndrome associated with cleft
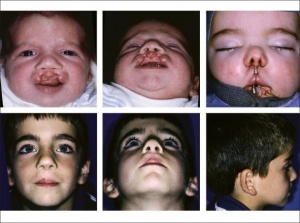
This syndrome has been identified as one of the most commonly occurring syndromes associated with oral cleft. It is known to be transmitted as an autosomal dominant allele within the gene. The lower lip pits as evident in the picture on the right is the characteristic of the condition. The locations of these pits are found to be situated bilaterally in the lower lip where the dry and wet vermilion are. They can be either oval or transverse in form. [54]
The following conditions often coexist in patients with the syndrome:
- hypodontia-a condition where the patient has missing teeth
- missing maxillary
- mandibular second premolar teeth
- absent maxillary lateral incisor
- ankyloglossia- also known as tongue tie a congenital oral anomaly which results in limited mobility of the tongue tip
Other rare extra-oral symptoms that may be present include:
- accessory nipples
- congenital heart defects
- Hirschsprung disease(HSCR)-is a congenital disease which causes blockage of the large intestine due to improper muscle movement in the bowel[55]
- popliteal web
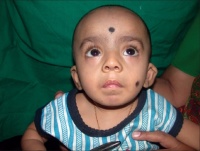
Velocardiofacial syndrome-An anomaly associated with cleft resulting from Chromosome 22q abnormality
Velocardiofacial syndrome (VCFS) is an autosomal dominant condition which results from a deletion on the long arm of chromosome 22 in the“q11”region (deletion22q11). It is the most common sub-microscopic deletion syndrome and is known to occur in 1 out of 2000 live births. [56] In excess of a hundred phenotypic features can result from this defect as it affects every major part of the body.
VCFS is most frequently associated to:
- cleft palate
- cardiac anomaly
- characteristic facial appearance (vertical maxillary excess, malar flattening, relative mandibular retrusion, narrow palpebral fissure and small ears)
- minor learning problems
- speech and feeding problems
Close connections have been reported between VCFS and DiGeorge syndrome. The DiGeorge syndrome features small or absent thymus, tonsils, adenoids and hypocalcaemia. These children may have medial displacement of the carotid artery over the cervical vertebrae and this should be considered while planning any type of pharyngeal surgery like pharyngeal flap for Velo pharyngeal incompetence (VPI) correction. The majority of these patients will require continual support for their learning difficulties. [56]
Diagnosis
Cleft lip and palate occurrence varies among continents, races and populations from one in 700 to one in 1500 newborns. [57][58]Hence it is of clinical as well as social significance that effective diagnostic measures are available early enough into the pregnancy so as to offer families ample time to understand the consequences of having a baby with such deformity.
While the birth of a child with clefting can have a severe emotional impact on the parents, antenatal diagnosis with ultrasonography helps to reduce the impact and prepare the parents psychologically. Most parents that received prenatal counselling following the diagnosis of cleft lip and/or palate antenatally (85%) felt that the information had prepared them psychologically for the birth of their child, and 92% indicated that they had never considered the possibility of voluntary termination of pregnancy. Prenatal diagnosis of cleft lip and/or palate has the additional advantage of allowing plastic surgeons to achieve early lip repair.[59] Prenatal ultrasound detection of the fetal face remains a matter of clinical research due to several technical difficulties associated with the examination of the fetus.[60]
The common obstacles faced during cleft lip and/or palate examination are as follows:
- shadowing effects of the superior alveolar ridge, and the fetal prone position[61]
- failure to identify the soft palate in three-dimensional (3D) ultrasound techniques as the soft palate is not in the same horizontal plane as the hard palate[62]
Cleft Soft Palate Detection
These technical challenges imply that the opportunity of prenatal screening for isolated defects of the soft palate is remote at present. Considering the additional time and effort involved in achieving satisfactory insonation and visualization, these methods are usually restricted to certain cases in which a cleft lip or hard palate is suspected. Isolated defects in the soft palate are relatively easier to repair surgically, and their emotional trauma on the parents if they are not diagnosed antenatally is far less severe than in newborns with cleft lip or cleft hard palate.[59]
Cleft Hard Palate Detection
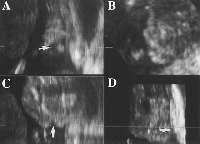
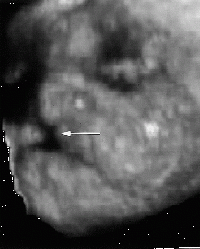
A combination of three different methods of 3D ultrasounds has been tested to measure detection accuracy of hard palate anomalies (See Table 1 and 2). The three methods are:
- reverse face
- flipped face
- oblique face
To date, none of the three methods (reverse face, flipped face or oblique face) have been found to be notably superior to the others. Therefore a combination of all three tests should be carried out for any fetus provided that there are adequate volume acquisition and reasonable time to examine the images offline. However, in cases where an immediate diagnosis is required, the fastest method is the oblique-face approach. On the other hand when initial volume acquisition is inadequate and image quality is less than optimum, the reverse-face view or the oblique-face view in coronal planes is the most effective technique to use. [59]
Accurate ultrasound imaging of the secondary palate also requires the presence of fluid between the fetal tongue and palate, as well as curving of the plane so that the acquired volume follows the concave structure of the palate with either the oblique-face or flipped-face view. In some cases these views can reveal useful details about the soft palate which can be potentially be used in prenatal diagnosis of defects in future cases.
| Feature | Reverse-face view (% (n)) | Flipped-face view (% (n)) | Oblique-face view (% (n)) |
|---|---|---|---|
| Lip | 100 (10/10) | 100 (10/10) | 100 (10/10) |
| Alveolar ridge | 100 (9/9) | 100 (9/9) | 100 (9/9) |
| Hard palate | 71.4 (5/7) | 85.7 (6/7) | 100 (7/7) |
| Soft palate | 0 (0/7) | 14 (1/7) | 14 (1/7) |
Table 1. Percentage of fetuses with cleft lip and palate (n = 10) in which abnormal findings were well visualized using each technique [59]
| Feature | Reverse-face view (% (n)) | Flipped-face view (% (n)) | Oblique-face view (% (n)) |
|---|---|---|---|
| Lip | 100 (50/50) | 100 (50/50) | 100 (50/50) |
| Alveolar ridge | 100 (50/50)) | 100 (50/50) | 100 (50/50) |
| Hard palate | 78 (39/50) | 84 (42/50) | 86 (43/50) |
| Soft palate | 0 (0/50) | 16 (8/50) | 26 (13/50) |
Table 2. Percentage of fetuses with cleft lip and palate (n = 50) in which abnormal findings were well visualized using each technique [59]
Treatment
Cleft abnormalities are generally treatable and can be completely corrected. Initial surgery should be performed between 6-12 months of age, however, there are many surgeons who operate between 12-18 months. Often at least a part of the surgery is performed between 10-12 years and very rarely an operation is required in late adolescence. Treatment for cleft abnormalities is usually over a course of 10-12 years depending on the severity and type of abnormality.[63]
There are three major objectives of a cleft lip or palate operation:
- To produce anatomical closure of the defect
- To create an apparatus for development and production of normal speech
- To minimize the maxillary growth disturbances and dento-alveolar deformities[63]
There are three general surgical techniques as summarized briefly in the following table with line images where available.
| Category | Surgical technique | Description of surgical procedure | Image(If Available) |
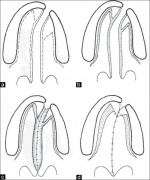
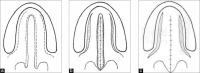
| Hard Palate Repair Techniques | Veau-Wardill-Kilner pushback (V-Y) | V-Y procedure is performed so that the whole mucoperiosteal flap and the soft palate are displaced backward and the palate is lengthened. [64] However, it leaves an extensive raw area anteriorly and laterally along the alveolar margin with exposed bare membranous bone. The raw area heals with secondary intention. This causes shortening of the palate and results in velopharyngeal incompetence. The raw area adjacent to the alveolar margin also results in alveolar arch deformity and dental malalignment. To increase the lengthening of the soft palate a horizontal back-cut in the nasal lining at the junction of hard and soft palate is done. This leaves a large raw area on the nasal surface which is left open. This may contract after healing with secondary intention and may undo the palatal lengthening. Since there is single-layer repair in the region of the back-cut, the incidence of palatal fistula is high. [63] | |
| Von Langenbeck bipedicle flap (W) | Method of uranoplasty (palatoplasty) using mucoperiosteal flaps for the repair of the hard palate region. This maintains the anterior attachment of the mucoperiosteal flap to the alveolar margin to make it a bipedicle flap. Originally only the cleft edges were incised, a lateral incision was made, the flap was elevated from the hard palate, the palatine musculature was divided and finally the sutures were applied. This technique is still used in isolated cleft palate repair. The muscle dissection and muscle suturing are done as additional procedures to create a muscle sling. This technique has recently been modified by Malek.[63] |
| |
| Bardach’s two-flap (V) | This is a modification of the von Langenbeck technique in which the incision is made along the cleft margin and the alveolar margin. These are joined anteriorly to free the mucoperiosteal flaps. These flaps are based on the greater palatine vessels. The soft plate is repaired in a straight line. The levator palati muscle dissection and reconstruction of the muscle sling is performed as in intravelar veloplasty. This popular technique is commonly used. [63] |
| |
| Alveolar extension palatoplasty (AEP) | In this technique the entire lingual gingivoperiosteal tissue is incorporated into the mucoperiosteal flap. This is expected to lengthen and widen the flap to cover the larger defect. This is expected to reduce the maxillary hypoplasia.[65] The radiograph will also show a right-sided aorta in approximately one-quarter of patients.[63] | Image not available | |
| Vomer flap | Vomerine mucoperiosteal tissue is very versatile. The vomer flap is utilised for repair of the cleft anteriorly in the hard palate region and the alveolar region and is invariably used as a superiorly based turnover flap. Many varieties of vomer flaps have been described for use in unilateral and bilateral cleft palates for nasal lining and oral mucosa resurfacing.[65] | Image not available | |
| Raw area free palatoplasty | This technique is exactly like the two-flap palatoplasty. Here the palatal lengthening is performed by the nasal mucosa back-cut, however, the raw area is covered with a local flap like the vomer flap or the buccal mucosal flap. On the oral side too an attempt is made to suture all the lateral incisions. This way no raw area is left on either surface. Healing of the palate occurs with primary intention, hence secondary deformities and shortening of the palate is less likely to occur. [63] | Image not available | |
| Soft palate repair techniques | Intravelar veloplasty | The dissection of the levator palati from the posterior border of the hard palate, nasal and oral mucosa and posterior repositioning. Consists of independent suturing of the muscle with that of the opposite side for the reconstruction of the levator sling. The majority of the surgeons dissect the muscle but the extent varies. Also known as radical muscle dissection.[65] | Image not available |
| Furlow double opposing Z-plasty | The cleft margin forms the central limb. The muscle is incorporated into the posteriorly based triangular flap on the left side for ease of dissection.[66] The hard palate region is closed by making an incision along the cleft margin, elevating the mucoperiosteum from the medial side and taking advantage of the high arch, the cleft is closed in two layers without making a lateral incision. On transposition of the triangles there is an effective lengthening of the soft palate, the suture line is horizontal and there is good overlap of the levator muscle. This technique has recently been modified by Malek. [63] | ||
| Primary pharyngeal flap | Used to improve the speech in children with cleft palate however, the majority of these patients will not develop velopharyngeal incompetence after classical palatoplasty as this creates an abnormal anatomy after pharyngeal flap surgery leading to complications.[65] | Image not available | |
| Two stage palatal repair | This technique has evolved over time. Initially, the soft palate was repaired along with the lip at around four to six months of age and the hard palate was repaired at the age of 10-12 years. This was later reduced to four to five years. This delay significantly reduced the cleft width in the hard palate region and was easy to close without the need for extensive dissection. This reduced the maxillary hypoplasia significantly. However, the speech result was compromised. Since then a two-stage functional palatoplasty was introduced. A method of cleft palate repair is described, based on a functional repair of the soft palate, followed by closure of the hard palate later taking into account the anatomy and physiology of the palatal mucosa.[63] | Image not available | |
| Protocol based techniques | Hole in one | In developing countries repeated hospitalization is a drawback for independent surgery for cleft lip and cleft palate. To avoid this, some of the surgeons popularized a one-stage repair of the full extent of the cleft. This is performed in children above 10 months of age.[65] | Image not available |
There are many complications that can occur after the surgical procedure including:
- Haemorrhage
- Respiratory obstruction
- Hanging Palate
- Splitting of the repair
- Oronasal fistula formation
- Bifid uvula
- Velopharyngeal Incompetence
- Abnormal speech
- Maxillary hypoplasia
- Dental malpositioning and malalignment
- Otitis media
Treatment usually requires a team of health care professionals over an extended period of time to work together to completely correct the problem. As seen below there can be many complications that arise from cleft palate abnormality and surgery and therefore a wholistic approach should be taken.
Any one or combination of the following health care professionals could be used to treat a cleft lip/palate patient:
- Surgeons (craniofacial, plastic, oral) to correct or recontruct the facial structure and appearance of the face
- Psychologists to work through issues regarding self esteem, social skills and behaviour
- Neonatal professionals to help with feeding problems that can arise
- Dietician to help with nutritional deficiencies caused by feeding problems
- Dentist/Orthodontist to correct structure/growth of the teeth
- Speech pathologist to resolve any speech problems
- Audiologist to treat hearing problems or potential hearing loss
Complications Associated with Cleft Palate
| Feeding Problems in Infants | Teething Issues | Speech Issues | Ear Infections | Social Problems |
| Inability to suck effectively while feeding on breast milk or bottled milk | Missing teeth | Nasal voice | Most children with Cleft Palate are prone to middle ear infection | Suffer isolation and alienation |
| Milk entering the nasal cavity which may lead to choking or pulmonary aspiration | Increased number of cavities | May develop nodules on the vocal cord due to vocal abuse | Hearing Loss | Depression related to social inacceptance |
| Malocclusion of teeth-This happens when teeth are bunched together or on top of each other | Delayed speech and language development | May be associated with repeated ear infection | ||
| Stuttering | Psychological Problems | |||
| Cluttering | ||||
| Speed sound disorders |
Various research into the lifestyle of people with facial anomalies, shows that it is a challenging task to learn to deal with the various social issues that come with living a life with a face that has an abnormal appearance.[67] Other research has shown that as well as managing the challenges of having anomalies in their physical appearance, children also have to deal with superficial psychological issues. [68]
Besides these psychological issues, the physical problem of having a malformed or incompleted hard palate has related physical issues.
- Eating problems: Due to an incompletely formed or an opening in the palate, food and liquids can travel through the mouth into the nose. To manage this issue specifically designed baby bottles and nipples are available which keep fluids flowing downward toward the stomach. Certain patients with a cleft palate may need to wear an artificial palate to help them eat and ensure that they receive ample nutrition until surgical treatment is commenced.
- Ear infections and hearing loss: Patients with cleft palate are at higher risk of ear infections due to the fact that they are more susceptible to fluid buildup in the middle ear. Untreated ear infections can cause permanent hearing loss. This can be avoided by regular checkups of hearing and the implantation of tubes in the air drums that aid in drainage of fluid.
- Speech problems: Cleft lip or cleft palate patients are also at risk of having trouble speaking. Issues like having nasal sound and speech sound disorders are quite common. They can often be fixed by surgery however a speech pathologist is required to manage speech difficulties.
- Dental problems: Patients with clefts often have missing, extra, malformed, or displaced teeth. Extensive orthodontic treatments are required to manage these issues. Additionally, cleft palate patients often have an alveolar ridge defect. The alveolus is the hard palate that contains teeth. A defect in the alveolus can displace or rotate permanent teeth, prevent permanent teeth from growing, and impeding the alveolar ridge from taking full form. These problems can be addressed by oral surgery.[69]
Recent Research Article
New approach to detecting VWS by IRF6 Screening of Syndromic and a priori Non-Syndromic Cleft Lip and Palate Patients
As we discussed earlier Van der Woude syndrome (VWS) - one of the most common cleft syndrome, is typically caused by the mutation of a dominant IRF6 gene. A recent study conducted in 2010 identified a mutation in 62.7% of the syndromic families tested and 3.3% of non syndromic patients.
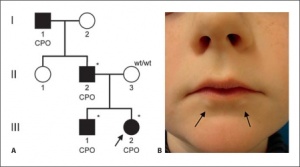
Interestingly, new insights into one of the non-syndromic families with an autosomal dominant inheritance (family B) was explored. The family history revealed the presence, at birth, of lower lip pits in two members and the diagnosis was revised as VWS one. A new sign in the lower lip was noticed in one subject within family B. Stimulating the interests of the researchers, a similar lower lip sign was also found in one individual from one other family (family A). The observation was the presence of two distinct nodules below the lower lip visible from the outside. This triggered a reexamination of all other patients previously cleared as not having VMS syndrome.
It was concluded from the findings that IRF6 should be screened when:
- any doubt rises about the normality of the lip and
- when there is familial history of CL/Ps with a dominant inheritance [2]
Resources for Patients, Parents and Health Professionals
Professor David, a South Australian physician has dedicated years of personal commitment to establishing the Australian Cranio Maxillo Facial Foundation and related organisations in Adelaide; he also founded the Asian Pacific Craniofacial Association and the Australian and New Zealand Society of Craniofacial Surgeons. He is also involved in training and establishing multidisciplinary teams in public and private hospitals across the Asia Pacific region. In addition, his contributions are internationally recognized as past President of the International Society of Craniofacial Surgery. His team of experts provide long term treatment plan to patients with craniofacial abnormalities. http://www.craniofacial.com.au/aboutus.html
CleftPALS is a volunteer based non-profit organisation of parents and professionals involved in the treatment of the cleft condition. CleftPALS work to support parents who have young children that have been born with a cleft. CleftPALS can assist with reliable and supportive information if an Ultrasound Detection of a cleft condition has occurred. There are branches in most states including NSW and Victoria. http://www.cleftpalsnsw.org.au/
Operation Cleft is an Australia based charity providing free cleft lip and palate surgery to underprivileged children in Bangladesh. http://www.operationcleft.org.au/
Related Links
Internal
Ultrasound Detection of Cleft Lip | Human Abnormal Development | Face and Ear
External
Smiles For Kids | Australian Congenital Anomalies Monitoring System (ACAMS) | Australian Institute of Health and Welfare (AIHW)
Glossary
Adenoids also known as pharyngeal tonsil, or nasopharyngeal tonsil are a mass of lymphoid tissue located posterior to the nasal cavity, in the roof of the nasopharynx, where the nose blends into the throat
Alveolar bone refers to the thickened ridge of bone that contains the tooth sockets on bones that bear teeth
Alveolar margin refers to one of the two jaw ridges found on the roof of the mouth, between the teeth and the hard palate or on the bottom of the mouth behind the lower teeth
Ankyloglossia also known as tongue tie a congenital oral anomaly which results in limited mobility of the tongue tip
Antenatal refers to the period of time before birth and during pregnancy
Apoptosis is programmed cell death where a series of biochemical events that ultimately result in the engulfment and recycling of cellular material
Asymmetrical refers to a structure that is out of proportioned or at a state of imbalance
Auricular system the organs involved with the hearing system
Bilateral means anatomical structures occurring on two sides also called two sided
Bipedicle flap the space created by undermining skin between two parallel incisions during skin reconstruction
Cleft lip is the presence of one or two vertical fissures (clefts) in the upper lip
Cleft palate refers to the congenital condition in which the palate at the roof of the mouth fails to fuse, resulting in direct communication between the nasal and oral cavities
Cluttering is a speech disorder similar to stuttering
Columella is a little column which is found as a central anatomical structure in a bony shell
Congenital is a term used to describe conditions present from birth
Corpus callosum is an anatomical feature which connects the left and right cerebral hemispheres facilitating communication between the two hemispheres.
Craniofacial anthropometry measurement of the bones in the skull
Craniocaudal also called head to tail refers to the long axis of the body in humans
Cupid’s bow peak the bow is the double curve of the lip and the peak is the top of each curve
Cutaneous is an anatomical term that indicates anything of or relating to the skin
Cytochrome protein are membrane bound proteins that contain heme groups carrying out electron transport
Dento-alveolar describes a tooth and the part of the alveolar bone that immediately surrounds it
Differentiation is a term used in cellular biology which refers to a process whereby less specialized cells become more specialized
Dish face a condition in which the face appears somewhat concave because of underdevelopment of the nasal and maxillary regions
Dissection the process of cutting away or disassembling something to observe the internal features
Dorsal refers to anatomical structures that relate to the back or spinal part of the body in vertebrates
Dysplasia refers to the inability to grow or develop a normal tissue, to become an organ
Ectoderm is one of the three germ cell layers in the very early embryo that differentiates to form the nervous system, tooth enamel, lining of mouth, anus, nostrils, sweat glands, hair and nails
Ectomesenchyme similar to mesenchyme and comes from neural crest cells and plays a role in forming the teeth, bones, muscles and brachial arches
Embryogenesis is the process involved in the development of an embryo to the foetus
Endoderm is the bottom layer of the three germ cell layers in the early trilaminar embryo (ectoderm, mesoderm and endoderm) formed by gastrulation. It differentiates to give rise to the epithelia and glands of the gastrointestinal tract, respiratory tract and the renal bladder.This layer also contributes to the associated gastrointestinal tract organ development (liver and pancreas)
Endogenous refers to substances that originate from within an organism, tissue, or cell
Epithelial is pertaining to cells that line hollow organs and glands and those that make up the outer surface of the body
Fistula is an abnormal communication between two body surfaces
Frontonasal refers to abnormality or condition that relates to the frontal and the nasal bones
Gestation refers to the the period of development from conception till birth
Glabrous refers to skin is external skin that naturally is hairless. It is found on the ventral portion of the fingers, palmar surfaces of hands, soles of feet, lips, labia minora, and penis
Grafting refers to the transplantation of skin
Hemorrhage the loss of blood from the circulatory system and is the medical term for bleeding
Hirschsprung disease is a congenital disease which causes blockage of the large intestine due to improper muscle movement in the bowel
Homocysteine is a non essential amino acid which is biosynthesized in the body methionine via a multi-step process
Hypocalcaemia is a condition which occurs due to low levels of calcium in the blood
Hypodontia a condition where the patient has missing teeth
Hypoplasia is the failure of development of an organ to a full, mature size
Hypoplastic see Hypoplasia
Incisive foreman key landmark in the bony palate
Inferior an anatomical word for something that is beneath or directed downwards
Insonation exposure to, or treatment with ultrasound
Intravelar veloplasty a surgical technique used to repair a cleft palate which involves the dissection of the Levator Palati muscle
In vitro within an artificial environment outside a living organism
In vivo within a living organism
Lateral anatomical expression meaning of, at towards, or from the side or sides
Levator palati is the elevator muscle of the soft palate
Lingual gingivoperiosteal tissue involved in the mouth
Locus the site on the body where a pathogen enters
Malformation abnormal or anomalous formation of structure
Maxilla a pair of irregularly shaped bones which form the upper jaw
Medially an anatomical word for being closer to the middle
Mediofrontally describes the middle line of the frontal region of the face
Mesenchyme part of the mesoderm of an embryo that gives rise to connective tissue, blood, lymph etc
Mesoderm the middle embryonic germ layer
Monozygotic used to describe twins derived from a single fertilised ovum
Morphology structure of an organism
Morphogen refers to chemicals that regulate the growth of specialized cells and also direct the location of specialized cell types within a tissue eg. sonic hedgehog
Mucoperiosteal flap is a flap of mucosal tissue reflected from a bone
Mucosa refers to a mucous membrane
Musculature refers to the arrangement of muscle in the body or a specific body part
Myogenic blastemata the formative, undifferentiated material from which muscular tissue is formed
Nasoalveolar describes the region in the nose where the ala attaches over the maxilla
Neural crest cell a group of specialized cells from the neuroectoderm that lies along the outer surface of each side of the neural tube in the early stages of embryonic development and give rise to certain spinal, cranial, and sympathetic ganglia
Neural tubeis a hollow structure which form the spinal cord and brain in embryos.
Neuromericrefers to structurs known (Neuromeres) that are defined transient segments of the early developing brain in embryos.
Non syndromic is defined as a condition that is not related to a familiar pattern of symptoms (syndrome).
Nucleotideis a compound consists of nucleosides linked to a phosphate groups. They are the fundamental unit of nucleic acids like DNA.
Ocularrefers to the eye.
Odontogenesisrefers to the process by the teeth are developed in embryos.
Orbicularis orisrefers to the muscle surrounding the mouth.
Osteocartilagenous nasal vaultrefers to the bony and cartiligenous structures in the nose.
Otitis media inflammation of the middle ear
Palate the roof of the mouth, separating the cavities of the nose and the mouth in vertebrates
Palatoplasty is surgery of the palate
Phenotype observable physical characteristics of an organism influenced by both genetic and environmental factors
Philtral line the lines on either side of the philtrum, which is the depression of the upper lip
Placode a thickened plate of ectoderm from which a sensory organ usually develops
Posterior anatomical expression for towards the back in position or near the hind end of the body
Prenatal see Antenatal
Proliferation growing rapidly in size or number
Prominence a projection, bulge or protuberance
Pulmonary aspiration refers to the entry of material (such as food or drink, or stomach contents) from the oropharynx or gastrointestinal tract into the larynx (voice box) and lower respiratory tract
Resection surgical removal of an organ, tissue or bone
Retrusion being posterior to the normal position
Rhinoplasty refers to plastic surgery of the nose
Rostrally an anatomical term of location referring to the direction towards the nose
Speech sound disorders refer to difficulty in producing particular speech sounds (most often certain consonants, such as /s/ or /r/)
Stomodeum an invagination of the surface ectoderm of the embryo from which the mouth is developed
Stuttering is a speech disorder where the speech is disrupted by involuntary repetitions and prolongations of sound
Superior an anatomical term for situated higher or above
Syndromic describes a set of symptoms occuring together and presenting as a syndrome
Teratogenic is a substance or something that cause birth defects in infants
Thymus a lymphoid organ that is located in the superior mediastinum and lower part of the neck and is necessary in early life for the normal development of immunological function
Thyrotropic refers to the effect or influence on thyroid gland
Trisomy 13 also known as Patau syndrome is a chromosal abnormality where the patient has an additional chromosome due to a process known as disjunction during meiosis
TSH cell also known as thyrotrope cell is located in the anterior pituitary gland which synthesise and secret Thyroid stimulating hormone the anterior pituitary gland
Ultrasonography also known as diagnostic sonography is an ultrasound-based diagnostic imaging technique used for visualizing subcutaneous anatomical structures e.g. tendons, muscles, joints, vessels and internal organs for possible pathology or lesions and often used during pregnancy
Unilateral occurring on one side
Uvula a small, conical shape, fleshy mass of tissue suspended from the center of the soft palate and above the throat
Velopharyngeal incompetence is an anatomical deficiency in the soft palate resulting in its malfunction often leading to speech problems
Ventrolateral anatomical structure extending from ventral to the lateral side
Vermilion the border between the lip and the surrounding skin
Vomer a thin flat bone in the midline of the nose
Vomerine mucoperiosteal the lining of the vomer bone consisting of both mucus membrane and periosteum
References
- ↑ Blandin PF. Operation to remedy a division of the velum palati or cover of the palate. New York J Med. 1838;10:203
- ↑ 2.0 2.1 <pubmed>21045959</pubmed>
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 <pubmed>19884680</pubmed>
- ↑ Converse JM, Hogan VM, McCarthy JG. Cleft lip and palate. In: Converse JM, editor. Reconstructive Plastic Surgery. 2nd ed. Philadelphia: Saunders; 1977. p. 1930
- ↑ Keating JM. Cyclopaedia of the diseases of the children. Philadelphia: Lippincott; 1889.
- ↑ Blandin PF. Operation to remedy a division of the velum palati or cover of the palate. New York J Med. 1838;10:203
- ↑ Franco P. Traite des Hernies. Lyons: Thibauld Payan; 1561
- ↑ <pubmed>14733424</pubmed>
- ↑ Blandin PF. Operation to remedy a division of the velum palati or cover of the palate. New York J Med. 1838;10:203
- ↑ Faltin R. History of plastic surgery in Finland. Finsk Lak Sallsk Handl. 1937;80:97
- ↑ Randall P. Triangular flap operation for unilateral clefts of the lip. Plast Reconstr Surg. 1959;23:331
- ↑ <pubmed>5842977</pubmed>
- ↑ <pubmed>12539652</pubmed>
- ↑ <pubmed>18452351</pubmed>
- ↑ <pubmed>20694165</pubmed>
- ↑ 16.0 16.1 <pubmed> 6750816</pubmed>
- ↑ 17.0 17.1 17.2 <pubmed> 2762398</pubmed>
- ↑ <pubmed>18218836</pubmed>
- ↑ <pubmed>21331089</pubmed>
- ↑ 20.0 20.1 <pubmed>19884685</pubmed>
- ↑ <pubmed>18971733</pubmed>
- ↑ 22.0 22.1 22.2 Moore KL, Persuad TVN. The Pharyngeal Apparatus. In: Moore KL, editor. The Developing Human. 8th ed.Modern Practice in Orthognathic and Reconstructive Surgery. Philadelphia: Saunders; 2008. pp. 160-95.
- ↑ 23.0 23.1 23.2 <pubmed>15479962</pubmed>
- ↑ <pubmed>5673878</pubmed>
- ↑ 25.0 25.1 25.2 25.3 25.4 25.5 <pubmed>16292776</pubmed>
- ↑ <pubmed>4083112</pubmed>
- ↑ 27.0 27.1 <pubmed>3074914</pubmed>
- ↑ 28.0 28.1 <pubmed>19884675</pubmed>
- ↑ <pubmed>2566383</pubmed>
- ↑ <pubmed>1680562</pubmed>
- ↑ <pubmed>12086669</pubmed>
- ↑ Hall BK. The embryonic development of bone. Am Sci. 1988;76:174–81.
- ↑ <pubmed>10726512</pubmed>
- ↑ Precious DA, Delaire J. Surgical considerations in patients with cleft deformities. In: Bell WH, editor. Modern Practice in Orthognathic and Reconstructive Surgery. Philadelphia: WB Saunders; 1992. pp. 390–25.
- ↑ Delaire J. The potential role of facial muscles in monitoring maxillary growth and morphogenesis. In: DS Carlson, McNamara JA., Jr, editors. Muscle Adaptation and Craniofacial Growth. Craniofacial Growth Monograph 8. Ann Arbor, MI: Center for Human Growth and Development, University of Michigan; 1998. pp. 157–80
- ↑ <pubmed>20333300</pubmed>
- ↑ <pubmed>16495466</pubmed>
- ↑ 38.0 38.1 38.2 38.3 38.4 <pubmed>18383123</pubmed>
- ↑ <pubmed>14729481</pubmed>
- ↑ <pubmed>10433915</pubmed>
- ↑ <pubmed>9369446</pubmed>
- ↑ <pubmed>10215616</pubmed>
- ↑ <pubmed>1973146</pubmed>
- ↑ <pubmed>3565662</pubmed>
- ↑ <pubmed>9632044</pubmed>
- ↑ 46.0 46.1 <pubmed>19881024</pubmed>
- ↑ <pubmed>12672677</pubmed>
- ↑ <pubmed>11967921</pubmed>
- ↑ <pubmed>2938624</pubmed>
- ↑ <pubmed>21331089</pubmed>
- ↑ <pubmed>3100859</pubmed>
- ↑ Nyberg DA, Sickler GK, Hegge FN, Kramer DJ, Kropp RJ. Fetal cleft lip with or without cleft palate: ultrasound classification and correlation with outcome. Radiology 1995; 195: 677–684
- ↑ <pubmed>8480000</pubmed>
- ↑ <pubmed>17477759</pubmed>
- ↑ <pubmed>17087425</pubmed>
- ↑ 56.0 56.1 <pubmed>9152551</pubmed>
- ↑ <pubmed>7857899</pubmed>
- ↑ <pubmed>3422598</pubmed>
- ↑ 59.0 59.1 59.2 59.3 59.4 <pubmed>19109803</pubmed>
- ↑ <pubmed>18504771</pubmed>
- ↑ <pubmed>15027008</pubmed>
- ↑ <pubmed>17252526</pubmed>
- ↑ 63.0 63.1 63.2 63.3 63.4 63.5 63.6 63.7 63.8 <pubmed>8272784</pubmed>
- ↑ <pubmed>3310812</pubmed>
- ↑ 65.0 65.1 65.2 65.3 65.4 <pubmed>19144126</pubmed>
- ↑ <pubmed>3786527</pubmed>
- ↑ <pubmed>3262457</pubmed>
- ↑ Winter RM, Baraister M. London dysmorpholgy Database, London neurogenetics database and Dysmorphology photo library on CD-ROM (version 3) Oxford: Oxford University press; 2001
- ↑ <pubmed>21733361</pubmed>
Textbooks
Schoenwolf, G.C., Bleyl, S.B., Brauer, P.R. and Francis-West, P.H. (2009). Larsen’s Human Embryology (4th ed.). New York; Edinburgh: Churchill Livingstone. pp. 563-575
2011 Projects: Turner Syndrome | DiGeorge Syndrome | Klinefelter's Syndrome | Huntington's Disease | Fragile X Syndrome | Tetralogy of Fallot | Angelman Syndrome | Friedreich's Ataxia | Williams-Beuren Syndrome | Duchenne Muscular Dystrolphy | Cleft Palate and Lip