User:Z3289738
Lab Attendance
Lab 1: --Z3289738 11:49, 25 July 2012 (EST)
Lab 2: --Z3289738 10:12, 1 August 2012 (EST)
Lab 3: --Z3289738 10:08, 8 August 2012 (EST)
Lab 4: --Z3289738 10:20, 15 August 2012 (EST)
Lab 5: --Z3289738 10:13, 22 August 2012 (EST)
Lab 6: --Z3289738 10:16, 29 August 2012 (EST)
Lab 7: --Z3289738 10:27, 12 September 2012 (EST)
Lab 8: --Z3289738 10:30, 19 September 2012 (EST)
Individual Assessments
Lab 1 Assessment
Q1. Identify the origin of In Vitro Fertilization and the 2010 nobel prize winner associated with this technique and add a correctly formatted link to the Nobel page.
The idea of In Vitro Fertilization began to formulate in the 1890s, when Walter Heape reported the first known case of embryo transplantation in rabbits. In 1953 John Rock extracted the first intact human fertilized egg. The first successful attempt at IVF was in 1978 by Steptoe and Edward.
Robert G. Edwards, the physiologist who developed the In Vitro Fertilization treatment, was awarded the Nobel Prize in Physiology or Medicine in 2010. Nobel Prize Page
Q2. Identify and add a PubMed reference link to a recent paper on fertilization and describe its key findings (1-2 paragraphs).
This article looks into the process of embryo implantation. It demonstrates how the activation of the epithelial Na(+) channel triggers prostoglandin E(2) release,phosphorylation of teh transcription factor CREB and upregulation of cyclooxygenase 2, the enzyme required for prostaglandin production and implantation. They detected maximum Epithelial Na(+) channel activation at the time of implantation in mice, and that blocking or knocking down this channel in mice resulted in failure to implant. These results indicate the importance of the Epithelial Na(+) Channel in the process of implantation, and the consequences of defects such as miscarriage and low success rates in IVF.
<pubmed> 22729284</pubmed>
Lab 2 Assessment
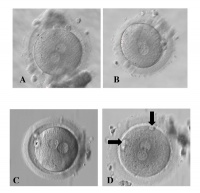
Q1. Upload an image from a journal source relating to fertilization or the first 2 weeks of development as demonstrated in the practical class. Including in the image “Summary” window: An image name as a section heading, Any further description of what the image shows, A subsection labeled “Reference” and under this the original image source, appropriate reference and all copyright information and finally a template indicating that this is a student image.
Q2. Identify a protein associated with the implantation process, including a brief description of the protein's role (1-2 paragraphs)
Trophinin
Trophinin is an membrane adhesive protein expressed on human trophoblastic cells and on uterine endometrium epithelial cells. The protein mediates apical cell adhesion and activate trophectoderm cells for implantation via proliferation and invasion. [1]
Lab 3 Assessment
Q1. Identify the difference between "gestational age" and "post-fertilisation age" and explain why clinically "gestational age" is used in describing human development.
"Gestational age" is measured from the first day of the woman's last menstrual cycle, whereas "post-fertilisation age" measures the time passed since fertilization of the oocyte. Gestational age is more clinically relevant as it is easier to determine the date of the woman's last menstrual cycle than it is to determine the date of fertilization. Furthermore, gestational age can also be determined before and after birth by measuring the size of the head, thigh bone and abdomen (before birth), and the size of the head and weight after birth. Gestational age is therefore used to determine the infant's medical history and medical plan.
Q2. Identify using histological descriptions at least 3 different types of tissues formed from somites.
Somites differentiate to form: (1) the axial skeleton (vertebral body & inter-vertebral disk), (2) dermis and (3) skeletal muscle.
- Cells in the ventromedial half of each somite differentiate into the sclerotome via Sonic hedgehog signalling mechanisms. The Pax 1 transcription factor then converts the sclerotome into chondrocytes (cartilage), which is essential for the functioning of the vertebral column.
- Cells in the dorsolateral portion of the somites differentiate to form the dermomyotone. This is then divided into:
- Dorsal dermatome which later contributes to the formation of the dermis in response to neutropin 3 factors.
- Wnt1 and Wnt3 factors contribute to the formation of the ventral myotome, which is further split into the epaxial myotome (gives rise to erector spinae muscles) and the hypaxial myotome (gives rise to the muscles of the trunk and limbs).
Lab 4 Assessment
Q1. Identify the 2 invasive prenatal diagnostic techniques related to the placenta and 2 abnormalities that can be identified with these techniques.
- Chorionic villus sampling (CVS)is an invasive prenatal diagnostic technique that is used to detect genetic abnormalities such as Down syndrome or cystic fibrosis. During the procedure a sample of the placenta is removed via a needle through the abdomen and then examined in a laboratory. It is commonly performed between 10 and 12 weeks of pregnancy/
- Amniocentesis procedures involve collecting samples of amniotic fluid via a needle through the abdomen to check for genetic abnormalities such as Down syndrome, cystic fibrosis or spina bifida.
Q2. Identify a paper that uses cord stem cells therapeutically and write a brief (2-3 paragraph) description of the paper's findings.
F. Ramirez, D. Steenblock, A. Payne and L. Darnall (2006) Umbilical Cord Stem Cell Therapy for Cerebral Palsy. MED HYPOTHESES RES 3: 679-686 | Umbilical Cord Stem Cell Therapy for Cerebral Palsy
This article describes a six month study to evaluate the effectiveness of umbilical cord stem cells in treatment for various brain injuries and disorders, in particular Cerebral Palsy. The study began in 2004, whereby 8 children between the ages of 3-12 who had been diagnosed with Cerebral Palsy underwent transplants with 1.5 million umbilical cord stem cells. The study reported eight of of eight children showed some improvement in mobility and/or cognitive function. Furthermore, one aphasic child started talking again and another who had been blind since birth was able to see after post-treatment.
The results from this preliminary observational pilot study suggests that umbilical cord stem cells may be a safe and promising treatment for children with cerebral palsy.
Lab 7
a) Class exercises
1. Maturation Hypertrophy - In your groups, design a method to estimate the degree of hypertrophy that occurs during the transition from birth to adulthood. Use the rulers to make rough measurements on the screen and then estimate the degree of hypertrophy as a mean increase in fibre size. Discuss the result as a class. (ie Try estimate the degree of hypertrophy from child to adult cells)
Method: Measured area of the child and adult cells, found an average for each and then worked out the percentage increase.
Answer: 7x increase in area size.
2. The role of satellite cells in muscle hypertrophy - class discussion of data presented in a recent paper - McCarthy et al. 2011. (ie How to we achieve hypertrophy? How do we get proteins into the cells? Degeneration of the myonucleus - Can activate the satellite cells as if the cell is undergoing repair; the nuclei within the cells becomes more active, produces more RNA and the cells get bigger.)
3. Fibre type shift - Discuss an experiment on fiber type shift that has been induced by chronic low frequency stimulation - Martins et al. 2006
b) Assessment
Q1. (a) Provide a one sentence definition of a muscle satellite cell.
Satellite cells are quiescent stem cells present in adult muscle tissue between the basal lamina of a muscle fiber and are responsible for postnatal hypertrophy and regeneration. [2]
Q1. (b) In one paragraph, briefly discuss two examples of when satellite cells are activated?
These cells are normally quiescent in adult muscle, by are activated in response to injury and muscle disease. When activated, the cells begin to proliferate and after aligning they fuse to allow for repair and/or regenration of muscle fibres. Satellite cells assist in the regeneration of muscle tissues in response to muscle injury by either forming multinucleated myotubes or additional quiescent satellite cells. [3]. Furthermore, studies have provided evidence of an increased level of satellite cells in muscular diseases such as Duchenne muscular dystrophy (DMD). [4]
Q2. In one brief paragraph, describe what happens to skeletal muscle fibre type and size when the innervating motor nerve sustains long term damage such as in spinal cord injury?
Spinal cord injuries which lead to long term damage to the innervating motor nerve would result in muscle partial or complete paralysis of muscles, leading to muscle atrophy. [5] This results in a significant decrease in cross-sectional area of the immobilized muscle do to lack of use. [6] Another consequence of the decreased muscle mass is an increased level of connective tissues and fat in order to assist the transfer of forces to the tendons.[7] Furthermore, the composition of muscle fibre types are transformed from a mix of type I and type II fibres to predominantly type II (fast twitch) muscle fibres. [8] This is a result of the muscle no longer being used for endurance-type excersises.