2014 Group Project 1
| 2014 Student Projects | ||||
|---|---|---|---|---|
| 2014 Student Projects: Group 1 | Group 2 | Group 3 | Group 4 | Group 5 | Group 6 | Group 7 | Group 8 | ||||
| The Group assessment for 2014 will be an online project on Fetal Development of a specific System.
This page is an undergraduate science embryology student and may contain inaccuracies in either description or acknowledgements. | ||||
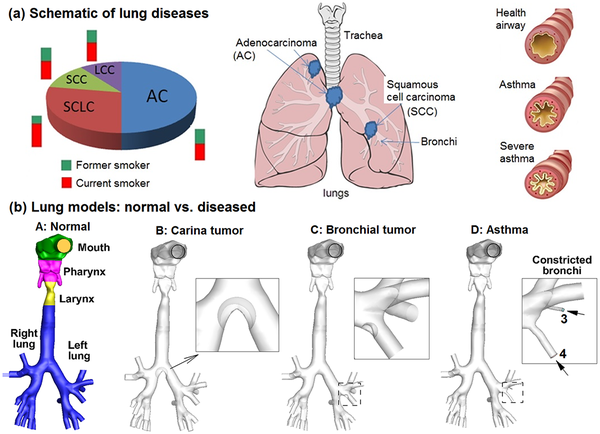
Respiratory
Introduction
Airway and blood vessel interaction during lung development.
A retinoic acid–dependent network in the foregut controls formation of the mouse lung primordium.
Lung epithelial branching program antagonizes alveolar differentiation.
The respiratory system allows the body to take in oxygen and exhale carbon dioxide through a process called breathing. the respiratory system moves the air in from the nose to the pharynx, larynx, trachea, bronchus and alveoli, which is where gas exchange occurs. During the embryonic and fetal stage the respiratory system is developing. The embryonic stage is the first 1-8 weeks and anything after that till about week 37 or birth is the fetal stage. However the respiratory system does not carry out gas exchange until birth. Whilst the embryo and fetus are in the mother, gas exchange occurs through the placenta. Once born the baby's lungs are drained and fill up with air automatically. The lungs do not inflate completely till about 2 weeks of the new born and the surfactant in each alveoli helps keep the lungs open and prevents it from collapsing.
Conducting zone
The conducting zone is made up nose to bronchioles and its function is to filter, warm, and moisten air and conduct it into the lung. the conducting zone includes the nose, pharynx. larynx, trachea, bronchi and bronchioles. Nares are the opening into the nose and is where nasal cavity is lined with cilia, mucous membrane and consists of blood filled capillaries.
Oral Cavity
Pharynx
Larynx
Bronchi
Bronchiole
Respiratory zone The respiratory zone is where the oxygen and the carbon dioxide exchange with the blood. 10% of gas exchange is due to the alveolar ducts and the bronchioles, the other 90% is because of the alveoli.
Terminal Bronchioles
Alveolar ducts
Alveoli
5 stages of take place when the lungs develop;
Embryonic stage - week 4-5 Lung buds are formed from ventral wall of foregut where lobar division occurs.
Pseudoglandular stage - week 5-17 The conducting epithelium tubes surrounded by thick mesenchyme are formed, extensive airway branching. By two months there would have formed all of the segmental bronchi. At this stage the more distal structures are lined with cuboidal epithelium.
Canalicular stage - week 16-25 The bronchioles have formed and there is now an increase in capillary which are in contact with cuboidal epithelium and beginning of alveolar epithelium development. the lung morphology changes dramatically. the future air-blood tissue barrier is formed as a result of the differentiation of the pulmonary epithelium. the differentiation of the future conducting airways of the lung from the future gas exchange region is distinguishable.
Saccular stage - week 24-40 alveolar ducts and air sacs are developed and the terminal sac. the saccules widen and lengthen the airspac. the future gas exchange region expands dramatically. fibroblasts also differentiate , they produce extra matrix, collagen and elastin. Vascular tree and also grows in length and diameter during this time.
Alveolar stage- late fetal to 8 years of age the secondary septation occurs and there is a significant increase of number and size in capillaries and the alveolar. during the 1-3 years postnatally the alveoli continue to form increasing the gas exchange surface area.
After birth
Current Research, Models and Findings
Physiological factors in fetal lung growth
<pubmed>3052746</pubmed>
This article looks at the current findings of different physiological factors that affect normal neonatal, functioning lungs upon during fetal development. The size of the paired organ to be able to exchange carbon dioxide with oxygen for the very first time at birth, is crucial to be able to withstand that pressure. As we know surfactant, is a lipid-protein composite. It is crucial to the function of the neonatal lung because:
A. Its high viscosity and low surface tension stabilize the diameter of the alveoli and prevent their collapse after each expiration.
B. Because the alveoli remain partially open, they are expanded on inspiration with much less expenditure of energy. [ANAT 2241 LEC 11-Respriation]
However, current research suggests that the production of surfactant which is reliant on hormonal factors, have little influence on fetal lung growth. In contrast, the following physiological lung growth factors were found to permit the lungs to express their inherent growth potential.
[this will be looked at further as the research project progresses]
Lung morphogenesis revisited: old facts, current ideas
<pubmed>11002333</pubmed>
Classical ideas -4 basic rules vs their review
Genetic control of lung development
<pubmed>12890942</pubmed>
Current concepts of lung development
Effects of hormones on fetal lung development
<pubmed>15550344</pubmed>
The fetal respiratory system as target for antenatal therapy
<pubmed>24753844</pubmed>
Historic findings
Historical knowledge predating modern imaging techniques has most often been confirmed by contemporary studies that provided evidence for the claims of early respiratory development. At times, theories put forward for fetal respiratory development were enhanced with further detail, whereas elsewhere paradigms were shifted and challenged due to the availability of proof otherwise [1]. The understanding of the development of the upper and lower respiratory system during the fetal period from week 8 onwards, as well as their respective functions, have been around since the 19th Century [2].
Surfactant
- 1929: The earliest recorded observation regarding the necessary presence of something in the lungs was proposed by Swiss physiologist Kurt von Neergaard through experiments performed observing the surface tension within the alveoli [3]. Unfortunately these findings were largely disregarded until decades later when they resurfaced in importance.
- 1954: Research on warfare chemicals by Pattle, Radford and Clements led to the understanding of the physical properties of surfactant [4].
- 1959: The final link to provide a sound understanding of the importance of surfactant was by Mary Ellen Avery and Jere Mead. They had published a study showing that premature neonates were dying from respiratory distress syndrome (RDS) due to insufficient pulmonary surfactant [5]. The lung extracts obtained from hyaline membranes of babies with RDS showed this deficiency.
References
1. Developmental Biology, 6th edition
By
Scott F Gilbert.
Swarthmore College
Sunderland (MA): Sinauer Associates; 2000.
ISBN-10: 0-87893-243-7
- Links: | Developmental Biology
Comparative embryology with detail on historical understandings of early respiratory development observed in various species. Accessible through PubMed.
2. Human Embryology and Morphology, 1902 By Arthur Keith London: Edward Arnold.
Historical images of past understandings on respiratory development
3. YouTube Video explaining early respiratory development
4. Lavoisier
<pubmed>5323506</pubmed>
Abnormalities
Newborn Respiratory Distress Syndrome (Hyaline Membrane Disease)
Newborn Respiratory Distress Syndrome (NRDS), also known as Hyaline Membrane Disease is characterised by the lack of or inability to synthesise surfactant in the premature lung of neonates.
The incidence of NRDS occurs in babies suffering form immature lung development, usually from premature birth with increased severity and incidence in correlation to decreased gestational age [1]. Preterm births do not allow for full lung maturation of the preterm infant due to process in which the respiratory system forms (from upper respiratory tree to lower). Type II Pneumocytes secrete surfactant into the alveoli, reducing surface tension and thus preventing the collapse of the alveolus – they are the last respiratory cells to differentiate. Preterm infants usually lack Type II Pneumocytes in their lung tissue causing the instability of their alveoli, oedema from immature alveolar capillaries and hyaline membrane formation[2].
NRDS mostly occurs in preterm neonates but can occur in post-term and term babies for a variety of reasons including:[3]
- Intrauterine Asphyxia – commonly caused by wrapping umbilical cord around the neck of the neonate, impairing development[1]
- Maternal diabetes – high levels of insulin can delay surfactant synthesis[4]
- Multiple pregnancy (twins, triplets etc) – associated with high rates of preterm births and resulting lung immaturity [4]
- Rapid labour, fetal distress, placenta previa, preeclampsia, placental abruption – that impair lung maturation in final stages of pregnancy [4]
- Preterm Caesarean delivery – not allowing for lung maturation[5]
- Genetic abnormalities that impair surfactant synthesis (ABCA3)[6]
- Meconium Aspiration Syndrome (MAS) - causes damage to the lower respiratory tract after aspiration of Meconium in amniotic fluid[7].
Meconium Aspiration Syndrome (MAS)
Meconium Aspiration Syndrome (MAS) affects newborn infants in response to some form of fetal stress during the third trimester and/or parturition, often due to: acute hypoxia, intrauterine hypoxia (often caused by the wrapping of the umbilical cord around the neck of the baby) and other physiological maturational events. [7][8].
Stress on the baby before or during labor can cause relaxation of the anal sphincter leading to expulsion of Meconium by the foetus into the surrounding amniotic fluid which can then be aspirated by the fetus, damaging the upper respiratory tract and possibly the lower respiratory tract. [9].
Problems associated with Meconium aspiration include[7]:
- Pulmonary gas exchange deficiency -caused by damage to the lower respiratory tract epithelium.
- Pneumitis and pneumonia - due to chemical damage and irritation from Meconium interaction with the airways.
- Blockage of the airways
References
- ↑ 1.0 1.1 <pubmed>20468585</pubmed>
- ↑ <pubmed>6071188</pubmed>
- ↑ <pubmed>10829971</pubmed>
- ↑ 4.0 4.1 4.2 <pubmed>20848797</pubmed> Cite error: Invalid
<ref>tag; name 'PMID20848797' defined multiple times with different content Cite error: Invalid<ref>tag; name 'PMID20848797' defined multiple times with different content - ↑ <pubmed>14629318</pubmed>
- ↑ <pubmed>15044640</pubmed>
- ↑ 7.0 7.1 7.2 <pubmed>10612363</pubmed>
- ↑ <pubmed>16651329</pubmed>
- ↑ <pubmed>19399004</pubmed>
<pubmed>22151899</pubmed> <pubmed>22214468</pubmed> <pubmed>12547712</pubmed>
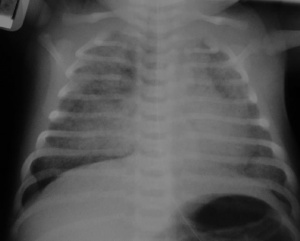
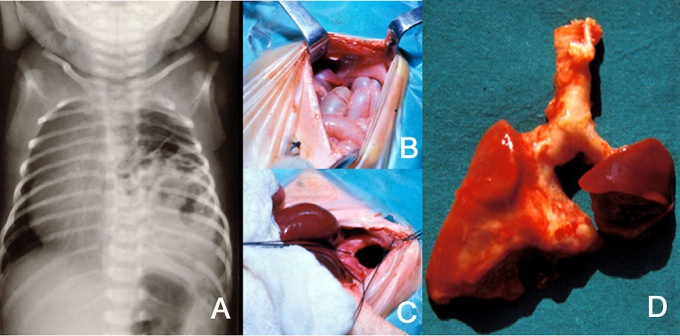
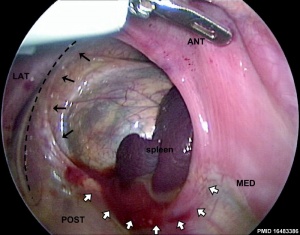
Congenital Diaphragmatic Hernia
A: Thoracic X-Ray of newborn showing CDH. Loops of bowel can be seen compressing on the developing left lung in the pleural cavity. B: Loops of bowel seen enters through the diaphragmatic Hernia. C: Surgical procedure to the contents of the hernia back into the correct anatomical position. D: Extreme hypoplasia of left lung and slight hypoplasia of right lung revealed in autopsy of newborn suffering from CDH.
- Down-regulation of sonic hedgehog expression in pulmonary hypoplasia is associated with congenital diaphragmatic hernia.
- Computer simulation analysis of normal and abnormal development of the mammalian diaphragm.
- Outcomes of congenital diaphragmatic hernia: a population-based study in Western Australia.
- Congenital diaphragmatic hernia.
Laryngo-tracheo-oesophageal clefts
- Bronchopulmonary Dysplasia.
- Surfactant Metabolism Dysfunction and Childhood Interstitial Lung Disease (chILD).
- Evaluation of fetal vocal cords to select candidates for successful fetoscopic treatment of congenital high airway obstruction syndrome: preliminary case series.
- The epidemiology of meconium aspiration syndrome: incidence, risk factors, therapies, and outcome.
- Antenatal infection/inflammation and postnatal lung maturation and injury.