2014 Group Project 5
| 2014 Student Projects | ||||
|---|---|---|---|---|
| 2014 Student Projects: Group 1 | Group 2 | Group 3 | Group 4 | Group 5 | Group 6 | Group 7 | Group 8 | ||||
| The Group assessment for 2014 will be an online project on Fetal Development of a specific System.
This page is an undergraduate science embryology student and may contain inaccuracies in either description or acknowledgements. | ||||
Integumentary
Introduction
This page concerns the development of the integumentary system in the fetal stage of development, particularly its organs i.e. the skin, glands, hair, teeth, and nails. It explores the mechanism of development as well as the timeline of development. This page also outlines some recent findings on the development of the integumentary system, as well as historic findings. Finally, this page also explores some of the congenital abnormalities of the integumentary system, its mechanism or pathogenesis, clinical manifestations, and how they are treated or managed.
Development Overview
Skin
The skin consists of 2 layers: the outer layer (epidermis) and a deeper connective tissue layer (dermis).
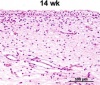
- The epidermis is derived from the ectoderm. Initially it exists as only a single layer of ectodermal cells at 7-8 days of gestation. However, by about 13-14 weeks after gestation, a 3- layered structure of fetal epidermis exists- consisting of the stratum basale, 1 or 2 intermediate layers and the periderm. The peridermal cells eventually become desquamated and form part of the vernix cervix.
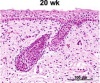
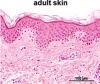
- The 5 definitive layers of the adult skin are evident in the human fetus after 22-24 weeks of gestation. Indirect influences form the dermis help differentiate the epidermis into: stratum basale, stratum spinosium, stratum granulosum, stratum lucidum and stratum corneum.
- The somatic mesoderm is the embryonic origin of the dermis. The mesoderm of the dermatones of the body, also contribute to the development of the dermis. Specifically though, in the head and neck region of the body, the dermis is derived from neural crest cells.
- The dermis is initially composed of just mesenchymal cells- loosely aggregated mesodermal cells. These mesenchymal cells later develop into fibroblasts- which function to secrete collagen and lay-down elastic fibers into the extracellular matrix.
3 other specialised cells of the epidermis also exists- these include melanoblasts, Langherhan cells and Merkel cells.
- Melanoblasts- are derived from neural crest cells that have migrated into the stratum basale. Mid-pregnancy, melanosomes are observed, differentiating the melanoblasts into melanocytes
- Langheran cells- are derived from bone marrow (originally form mesoderm) and migrate into the epidermis. They have the function of antigen presentation.
- Merkel cells- still have an uncertain origin. They have a function related to mechanoreception.
<pubmed>19701759</pubmed> <pubmed>PMC2113922</pubmed>
Glands
| Gland Type | Description |
|---|---|
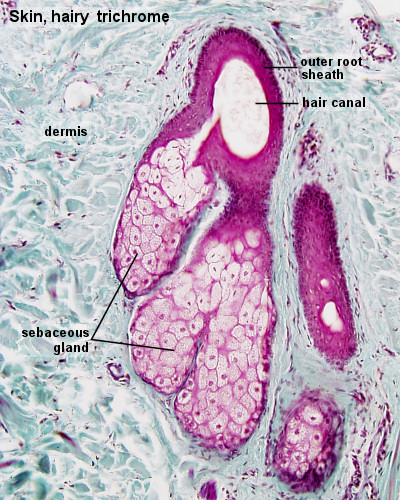
| Sebaceous Glands | *Sebaceous glands develop from the epithelial wall of the hair follicle.
Vernix caseosa is a material produced by sebaceous glands in the foetus in the last trimester of development [1] and is characterised by it’s cheese-like appearance around the neonate at birth. The functions of vernix caseosa include: |
| Mammary Glands | *Mammary glands develop from the mammary ridge- a downgrowth of the epidermis (ectoderm) into the underlying dermis (mesoderm). This occurs at about week 6 of development. Prior to puberty, the mammary glands are anatomically indistinguishable. |
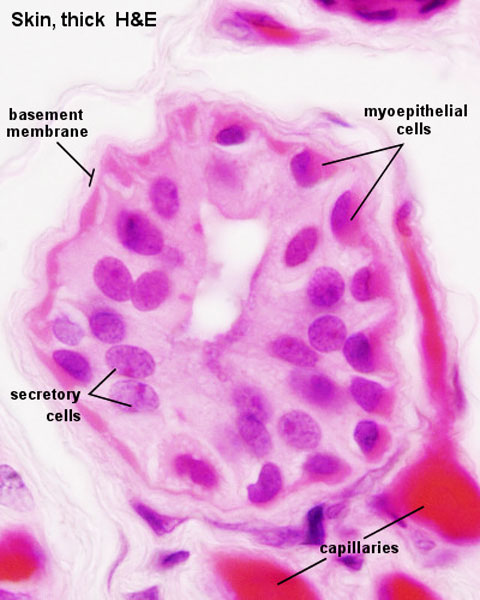
| Sweat Glands | *Eccrine and apocrine sweat glands develop from the downgrowths of the epidermis into the underlying dermis. It has been seen and detected in studies from week 21. |
- Cite this page: Hill, M.A. (2014) Embryology Integumentary System - Gland Development. Retrieved October 7, 2014, from https://php.med.unsw.edu.au/embryology/index.php?title=Integumentary_System_-_Gland_Development
Hair
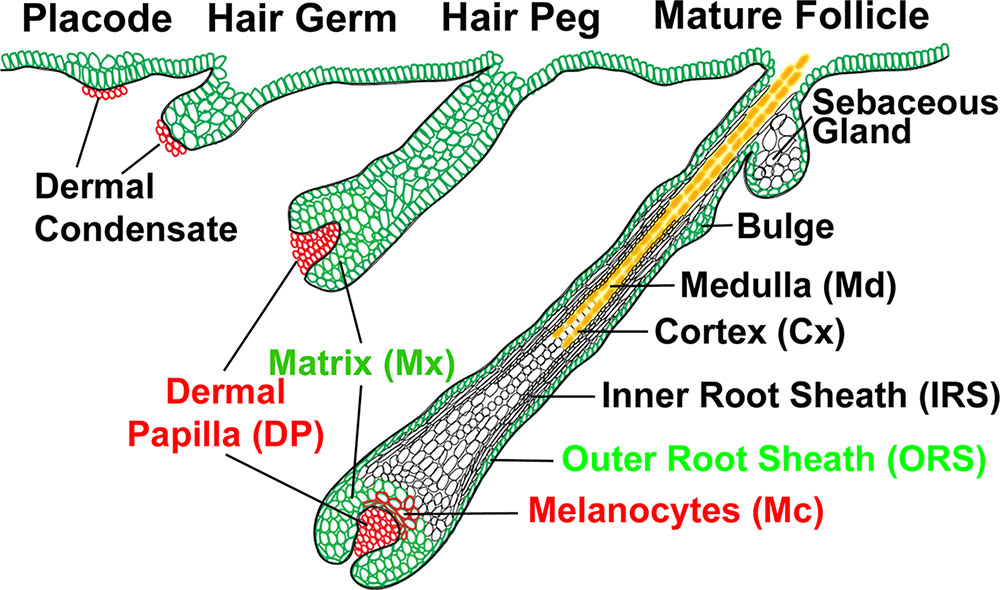
Hair originates from the ectoderm. At about 12 weeks, it is believed that specific signals from the dermis begin to induce hair follicle formation. Through reciprocal interactions, cells from the stratum basale grow into the underlying dermis. The epithelial cells influenced by these dermal signals, develop a placode- a thickening of the columnar cells. Signalling from the placode than leads to the development of a dermal condensate, which further induces the downward growth of the placode. The hair follicle, continues to proliferate and enclose the dermal condensate, forming a deep, club-shaped hair bud, with an invaginated dermal papillae. These dermal papillae are rapidly infiltrated by blood vessels and nerve endings. The epithelial cells within the hair bulb, then begin to differentiate into the germinal matrix – which grow, proliferate and keratinise to form the hair shaft and internal root sheet. Other epithelial cells outside of the hair bud, form the external hair sheeth. Mesodermal cells of the dermis that surround the invaginating hair follicle form the dermal root sheeth and the arrecrtor pili muscles for hairs.
<pubmed>20590427 </pubmed> <pubmed>11841536 </pubmed> <pubmed>1566372 </pubmed>
Nail
- Nails also develop from the epidermis.
- The development and growth of the fingernails occurs earlier in week 10, compared to the toe nails- which only start developing in week 14.
- Nail development grows first on the tips of the digits, before actually migrating,-with their innervation-onto the dorsal surface. Nails reach the digit fingertips at approximately week 32, while for toenails, it occurs a bit later- at week 36.
- The nail fold is thickened epidermis, with keratinisation of the proximal end forming the nail plate
- Cite this page: Hill, M.A. (2014) Embryology Integumentary System - Nail Development. Retrieved October 7, 2014, from https://php.med.unsw.edu.au/embryology/index.php?title=Integumentary_System_-_Nail_Development
Teeth
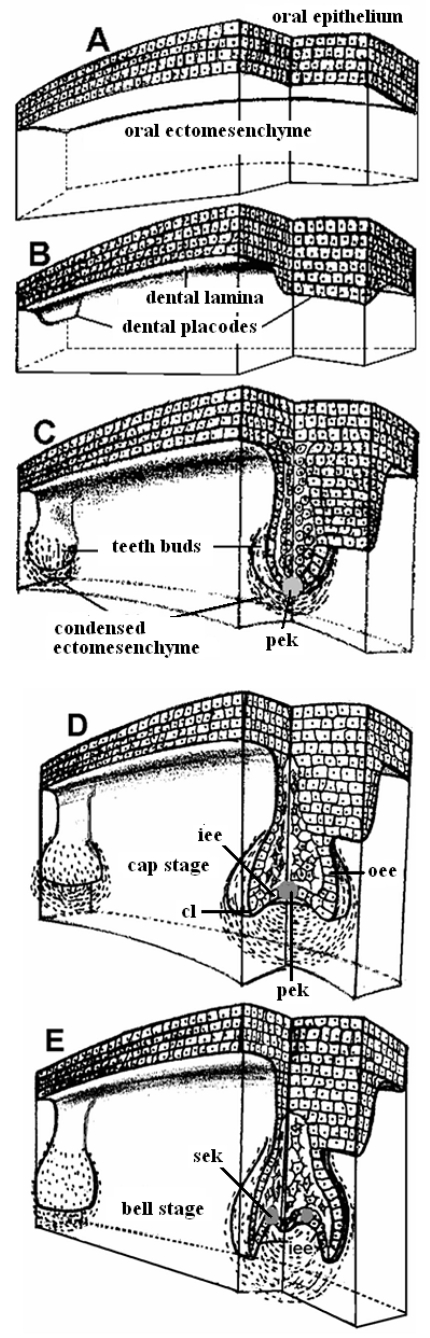
The ectoderm and the associated underlying layer of neural crest cells, are the origin for teeth development. As the oral epithelium grows and proliferates, it has a downward movement into the underlying neural crest layer. This leads to the formation of the dental lamina. These dental lamina, then, gives rise to tooth buds. These tooth buds, later form and develop into enamel organs. With further development, these enamel organs give rise to ameloblasts- which produce enamel. The dental papilla, on the other hand is formed by the neural crest cells which underlie the enamel organs. These dental papillae than give rise to the dental pulp and odontoblasts- which produce predentin and dentin, in the adult body.
| Stage | Week | Description |
|---|---|---|
| (A) Lamina | Week 6 | The oral ectoderm, closely interacts with the neural crest ectomesenchyme. In the Lamina stage, teeth may grow only within the epithelium. |
| (B) Placode | Week 7 | The dental lamina and and the dental placodes arise, due to specific signals from adjacent epithelial cells |
| (C) Bud | Week 8 | Tooth buds are formed, as the epithelium cells interact with the messenchyme. This occurs at the sides of the dental placodes. Also, as opposed to the earlier Lamina stage, in the Bud stage, teeth may now only grow within the ectomesenchyme |
| (D) Cap | Week 11 | After folding, the bud takes upon the shape of an inverted cap |
| (E) Bell | Week 14 | The bud refolds once again, this time taking upon the shape of a bell |
References
<pubmed>19266065</pubmed>| PMCID: PMC2651620
Int J Biol Sci. 2009; 5(3): 226–243. Published online 2009 February 24.
Copyright © Ivyspring International Publisher. This is an open-access article distributed under the terms of the Creative Commons License (http://creativecommons.org/licenses/by-nc-nd/3.0/). Reproduction is permitted for personal, noncommercial use, provided that the article is in whole, unmodified, and properly cited.
Some Recent Findings
|
|

|
|
| More Recent Papers |
|---|
|
<pubmed>23826487</pubmed> <pubmed>22342389</pubmed> <pubmed>24911066</pubmed> <pubmed>25143675</pubmed> |
Historic Findings
Knowledge of the Integumentary expands in conjunction with technological developments that allow observation of microscopic structures. Historically animal models have been used to map the stages in the development of the fetal integumentary system.
Skin
In 1900 Bardeen C. R used the pig animal model to study the histogenesis of the dermomyotomes and nervous appratus. Bardeen and other scientists established that the human skin results from the union of the epithelial material derived from the ectoderm (epidermis) and the connective tissue origination from the mesoderm (dermis).
http://journals.lww.com/plasreconsurg/Citation/1949/07000/CLINICAL_ASPECTS_OF_EMBRYOLOGICAL_SKIN.8.aspx Bardeen, C. R. (1900). The development of the musculature of the body wall in the pig, including its histogenesis and its relations to the myotomes and to the skeletal and nervous apparatus. Johns Hopkins Hosp. Rep, 9, 367-399.
Glands
Sebacious glands / Sweat glands / Mamailliary
In the 1968 Robins and Breathnatch investigated the development on the sebacious and apocrine swelling in the skin, which where closely associated with development of the hair follicle. They observed differentiation of desmosomes and development of cytoplasmic contents of the cell.
Hair
STRUCTURE : The major anatomic details of hair development in the human foetus have been established by studies with light microscopy. Electron microscopy was not commonly used to until recently and so little was known about the ultrastructure of the skin. Over the past few years, reports have been published on the epidermal melanocytes and periderm. In 1968 Breathnach and Smith determined the fine structure of the cells of follicle and dermal papilla in the first two weeks of fetal development. The Peripheral Nerves, the sweat duct and nail development were also explored and the interrelationship of cells at particular foetal stages was deduced. These studies, and other laboratory animals, have provided information on the differentiation of cells and tissue of some functional importance and underline the role of cells and tissues.
DEVELOPMENT: In 1958 Pinkus established the following stages of fetal hair follicle development: pre-germ, hair-germ, hair-peg,andbulbous-peg stages. Pinkus also determined that the developed hair fibres grow through the epidermis and appears at the level of the skin at around 19-21 weeks of development. The lanugo (foetal) hair is extremely fine with no medulla and a tip free of pigment.
Robertson, J. R. (Ed.). (2002). Forensic examination of hair. CRC Press.
The mechanism of fetal hair follicle development was noted to be a cycling phenomenon in 1959 by Chase and Eaton's experiments. Development begins with the downwards growth of the follicle structure from the level of the dermis. The follicle is a processes during the quiecent phase thought he adipose layer during gowth and differntiation. They also established that upward movement of hair inovlves the addition of next cells from the matrix of the follicle and an enlargement of each cell. Furthermore their research also showed that the epidermal and dermal layers were dynamic and interacting with each other. The most significant developments in the understanding of hair follicle development came from studies investigating the differentiation pattern of cells as the follicle develops. [1]
<pubmed>5656140</pubmed> <pubmed>4097391</pubmed>
Determined that the hair fibre finally breaks through the epidermis and appres about the skin at around 19-21 weeks of development. The lanugo (foetal) hair is extremely fine with no medulla and a tip free of pigment.
Nail
Prior to the 1950’s there had not been a great deal of research into the area of foetal nail development. This was primarily due to the difficulty in obtaining normal foetal specimens. Furthermore, the histological staining techniques used to prepare slides of nail tissue, required prolonged periods of decalcification. This process often damage the specimen and little detail could be seen during the microscopic examinations. As a result, the histological features and developmental stages of the nail could not be deduced. From a clinical perspective, the incomprehensive understanding the "normal nail" features made it difficult for dermatologists to correctly diagnose abnormalities. [2]
It was in 1954 that Barton and Lewis conducted a through microscopic examination of foetal and adult nail. It is clear that Barton and Lewis conducted an investigation with one underlying aim. They hoped that a through understanding of the normal development, anatomy and physiology would assist physicians in diagnosing and treating abnormalities. A number of key features in nail anatomy were identified and named. The Nail Plate, Nail Root, underlying Nail Bed, Eponychium and Hyponychium. [3]
In 1963 Nardo Zaias conducted a study on the Embryology of the Human Nail. This investigation contributed to our understanding of different stages in foetal nail development. Zaias studied an number of foetal specimens at different stages in development. As a result, Zaias was able to propose a rough timeline highlighting morphological hallmarks in normal nail development. [4]
| Header text | Header text |
|---|---|
| Week 9 | The primitive nail beings to from |
| Week 10 | The primary nail field is establish |
| Week 11 | Distal ridges of nail bed keratinise. |
| Week 13 | Early nail matrix. |
| Week 20 | Nail plate begins to grow over the nail bed. |
| Week 24 | Free nail plate is visible to the naked eye. |
Today research into the field of foetal nail development continues. Technology allows exploration beyond staging the macroscopic and microscopic morphological changes. We are now able to understand the molecular signalling with in the epidermis which drives this process.
Teeth
<pubmed>5267156</pubmed>
Abnormalities
Aplasia Cutis Congenita
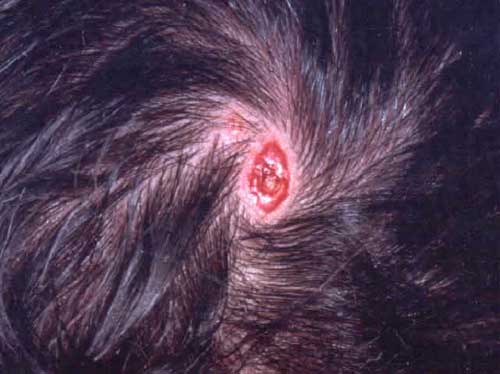
Aplasia cutis congenita (ACC) is a rare skin abnormality, characterised by the absence of all layers of the skin. It is most common to occur on the scalp (70%), specially the vertex. In severe cases, the defect can go as deep as the bone or the dura. Other sites of ACC include the skin of the limb regions. “ACC occurs in approximately 1 in 10000 live births, with a female-to-male ratio of 7:5.” The specific aetiologic agent for ACC is still unknown. It has been suggested to be genetic and/or environmental. The damage to the vertex is suggested to be the result of the biomechanical stretch at this area when the fetal brain is growing.[5]
Presently, ACC is managed via conservative treatments or surgical treatments. Conservative treatments refer to basic wound treatments and preventing infection with the use dressings and antibiotics. Surgical treatments, specifically scalp reconstruction procedures, aim to reconstruct the damage to the skin through skin grafts, local scalp flaps, and pericardial scalp flaps. Large defects are often treated using surgical treatments.[6]
Dystrophic Epidermolysis Bullosa
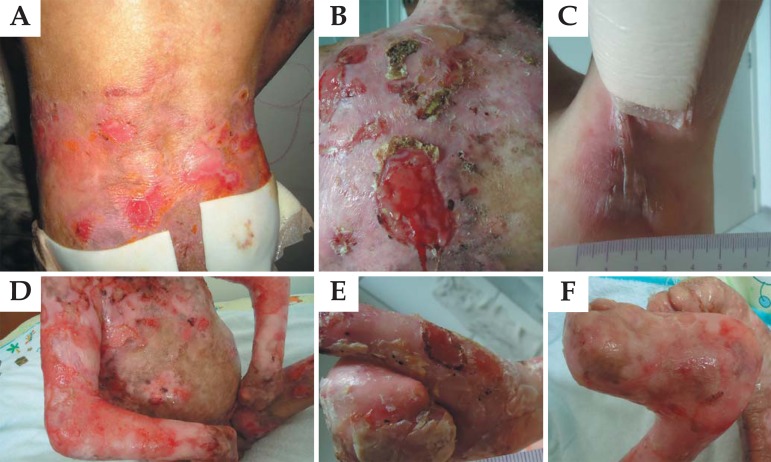
Dystrophic Epidermolysis Bullosa (DEB), a type of epidermolysis bullosa, is a genetic disease of the skin, usually present at birth or at an early age[8]. Currently, around 400,000 - 500,000 people are affected with the disease[8]. It is characterised by the fragility of the skin[8], where it blisters upon minimal trauma and scars[9], usually at the extremities[8]. It is caused by a mutation in collagen VII gene (COL7A1)[9][10], which is responsible for the the formation of anchoring fibrils[9]. Anchoring fibrils are responsible for dermal-epidermal adherence[9], that is why it’s loss of function results to blistering of the skin. In some cases, even teeth and nails are affected. Teeth of patients with DEB have enamel defects and when combined with poor oral hygiene, it may lead to decay. Nails of DEB patients are often dystrophic and will eventually be lost.[8]
There are currently no known cures for DEB; however there are techniques to manage the clinical manifestations of the disease, which include:
- wound care[9]
- preventing factors that may cause blistering[9]
- using aqueous disinfectants - highly effective[9]
- dental care[8]:
- -use of topical fluoride
- -careful prophylaxis
- -use of topical antibiotics to prevent secondary infections[10]
One study is currently exploring the potential of protein therapy as a treatment for DEB. Their results show that intradermal injection of recombinant human collagen 7 in mice with DEB led to “restoration of C7 and anchoring fibrils.”[11] Other techniques that aim to restore C7 include:
- bone marrow transplant- improved blistering in mice specimen and increase survival rates[10]
- hematopoietic cell transplant (HCT)- increased deposition of C7 in injured skin[10]
Congenital Alopecia Areata
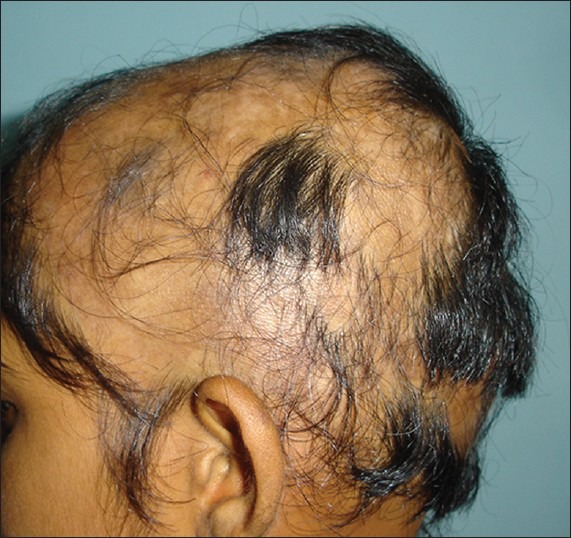
Alopecia areata (AA) is an abnormality of the hair affecting anagen hair follicles, characterised by well-demarcated patches of hair loss. It is non-scarring and can occur on the scalp and/or the body. 90% of AA cases occur on the scalp. 5%-10% of patients with AA lose all hair on their scalp; this is called alopecia totalis. While others lose all of their body hair, this is called alopecia universalis. [13] Its pathogenesis is considered to be both genetic and autoimmune. There is an abnormality with the genes related to the immune system and to the hair follicles. And histopathology shows signs of lymphatic infiltration of the hair follicles and the loss of these scalp lymphocytes allow hair follicles to recover.[14] High frequencies of catagen and telogen hair follicles are also present in areas affected by AA.[13]
There is currently no cure for AA. There are several treatments to combat AA but none of these have led to remission of the disease, the most effective being corticosteroids and topical immunotherapy.[13] A new method of treating alopecia areata is currently being studied. Transepidermal drug delivery (TED) is a new treatment that functions by creating micro-channels in the epidermis. By doing so, drug delivery to the skin is improved. This treatment was highly effective and had lower rates of side effects, e.g. pain, compared to previous treatments.[15]
Harlequin Ichthyosis
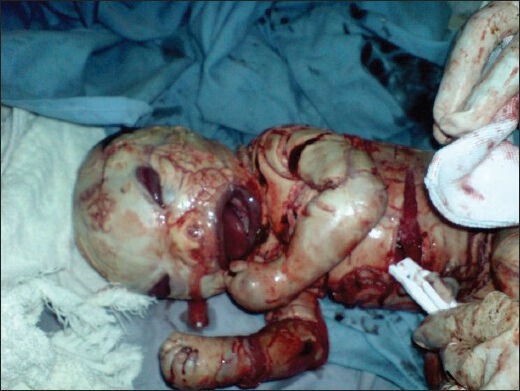
Congenital ichthyosis is an autosomal recessive disease of the skin, characterised by visible and excessive scaling of the skin and hyperkeratosis, i.e. thickening of stratum corneum layer of the epidermis and in some cases, hypohidrosis, i.e. the lack of ability to sweat. [17] Harlequin ichthyosis (HI) occurs only in 1 in 1,000,000 babies. It is life-threatening in the first few weeks and/or months of the neonate.[17] The thick skin can restrict movement of the baby and sometimes constrict extremities and lead to necrosis then autoamputation.[18] Babies with HI are also characterised by bilateral ectropion (everted eyelids), eclabium (everted lips), and underdeveloped nose.[18] In 50% of HI cases, respiratory failure is often the cause of death.[19] This disease is caused by a nonsense mutation in the ATP-binding-cassette A12 (ABCA12) gene, which is responsible for encoding a lipid transporter essential for the regulation of lamellar bodies. [17][18][19]
There is currently no known cure for this disease. Management techniques include:
- Monitoring in neonatal intensive care units.
- -Temperature within the incubator is controlled to avoid fluctuation in body temperature and to stop sweating. [17]
- Mechanical removal of excess scales from the skin [17]
- Bathing to remove excess scales from the skin[17]
- Topical therapy - to reduce hyperkeratosis. [17][19]
- Use of oral retinoids - known to have high rates of survival.[19]
Hypohidrotic Ectodermal Dysplasia
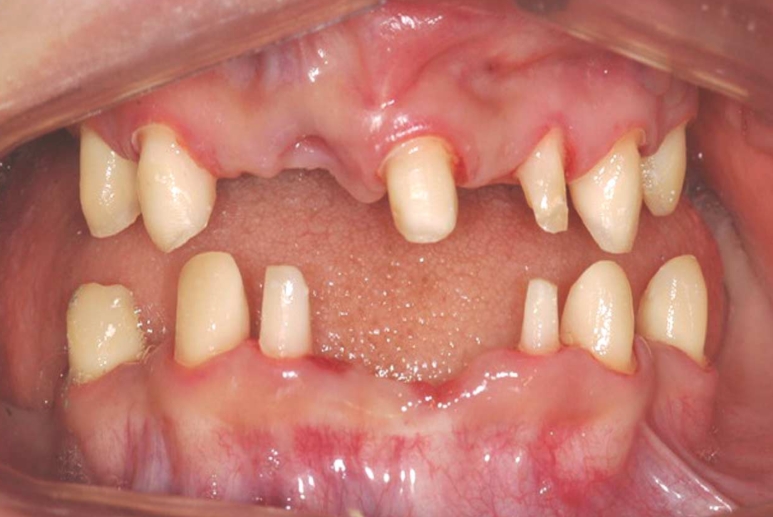
Hypohidrotic ectodermal dysplasia (HED) is the most of all ectodermal dysplasias, caused by an abnormality in the development of ectodermal tissues, which inlude skin, hair, teeth, sweat glands, and nails.[21][22] Patients with ectodermal dysplasia often have sparse hair and oligodontia, which is a condition where teeth are missing and are poorly developed.[21][22] Sweating is a very important function in the body in terms of thermoregulation. HED is mainly characterised by hypohidrosis due to the lack of sweat glands in the skin, which could lead to hyperpyrexia and sometimes death. In neonates, the mortality rate of HED reaches up to 30%, with the first year of life having the highest risk. [21] HED is caused by a genetic abnormality of the ectodysplasin A gene (EDA) and passed on by X-linked inheritance. The mutations of this gene results in the poor sweating ability or none at all in a person. The effects of this abnormality is usually more severe in males than in females. [23][22]
There is currently no pharmacological therapies for HED but there are methods applied to prevent the disease from aggravating. Neonates with HED are placed in incubators and monitored to prevent them from overheating. Management of this disease gets easier as the patient ages. Adults with HED can control their thermoregulation by staying in cool environments or drinking cold drinks to lower the body temperature. Currently, there are studies that aim to find a cure for this abnormality, e.g. gene replacement therapy in animal models.[22]
References
- ↑ <pubmed>5656140</pubmed>
- ↑ <pubmed>13206419</pubmed>
- ↑ <pubmed>--</pubmed>
- ↑ <pubmed>14003041</pubmed>
- ↑ <pubmed>22549580</pubmed>
- ↑ <pubmed>23147310</pubmed>
- ↑ <pubmed>23739692</pubmed>
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 <pubmed>25284524</pubmed>
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 <pubmed>19945622</pubmed>
- ↑ 10.0 10.1 10.2 10.3 <pubmed>24860657</pubmed> Cite error: Invalid
<ref>tag; name 'PMID24860657' defined multiple times with different content Cite error: Invalid<ref>tag; name 'PMID24860657' defined multiple times with different content Cite error: Invalid<ref>tag; name 'PMID24860657' defined multiple times with different content - ↑ <pubmed>19018253</pubmed>
- ↑ <pubmed>23960401</pubmed>
- ↑ 13.0 13.1 13.2 <pubmed>17269961</pubmed>
- ↑ <pubmed>16338213</pubmed>
- ↑ <pubmed>25260052</pubmed>
- ↑ <pubmed>24520234</pubmed>
- ↑ 17.0 17.1 17.2 17.3 17.4 17.5 17.6 <pubmed>19824737</pubmed>
- ↑ 18.0 18.1 18.2 <pubmed>23419760</pubmed>
- ↑ 19.0 19.1 19.2 19.3 <pubmed>24124810</pubmed>
- ↑ <pubmed>21165248 </pubmed>
- ↑ 21.0 21.1 21.2 <pubmed>20682465</pubmed>
- ↑ 22.0 22.1 22.2 22.3 <pubmed>24678015</pubmed>
- ↑ <pubmed>21357618</pubmed>