User:Z5019799
Maternal pregnancy is divided into three stages of growth and development - the first trimester which involves organogenesis via cellular proliferation, differentiation, and morphogenesis; the second trimester which is centred around organ development and functioning as well as foetal expansion and recognisable movement (quickening); and the third trimester during which the foetus undergoes rapid weight gain.
Second Trimester Foetal Development
The second trimester encompasses the foetal weeks 12-24, or clinical gestational weeks 14-26, according to the UCSF Medical Centre and is referred to as the "golden period of pregnancy" since many first trimester discomforts such as nausea, fatigue, breast tenderness, and frequent urination are alleviated as the maternal body adapts to the changing gestational physiology - nevertheless increased placental secretions of progesterone, estrogen, and human placental lactogen, as well as increased abdominal pressure can elicit heartburn, constipation, abdominal pain, and leg cramps. During the second trimester of pregnancy, the organ rudiments formed in the embryo stage expand in size and further differentiate in response to cellular signalling and gene cascades to coordinate specialised physiological functions needed to support the growing foetus. In addition to foetal growth and development, the placenta also increases in size to increase foetal blood supply and secretes hormones to redirect maternal glucose, amino acids, and free fatty acids towards the foetus to satisfy its increasing metabolic demands.
Skin and Musculoskeletal System
During the second trimester the musculoskeletal system must develop, through the formation of bones, muscle tissue, joints, and connective tissue (e.g. ligaments, tendons, cartilage) to provide an adequate bony framework to enclose the internal viscera and confer structural support.
- In the embryonic stage, the paraxial mesoderm of the trilaminar embryonic disc differentiates into somites which are re-organised to form the epithelial dermomyotome (cells have tight junctions, regular shape, well organisation) and the mesenchymal sclerotome (loosely arranged and associated cells with large extracellular matrix that lack polarity and rigidity).
- The dermatome forms the dermis (connective tissue underlying epidermis), the myotome forms the epaxial (dorsal) and hypaxial (ventrolateral) muscles of the body wall and limbs, and the sclerotome forms the vertebral column and intervertebral discs.
- In the second trimester, the epaxial and hypaxial muscles of the thorax and abdomen grow, become segmented, and innervated by the dorsal and ventral rami of the spinal nerves respectively. For example the hypaxial muscles form the intercostal muscles in the thorax and the external oblique, internal oblique, transversus abdominis, and rectus abdominis in the abdomen.
- Growth of lone bones occurs by longitudinal expansion at epiphysial plates, widening of the diaphysis, and endochondrial ossification which continues throughout gestation and childhood. The long bones in the upper and lower limbs develop greatly in the second trimester to their expected sizes at childbirth.
- The extensive musculoskeletal development in the second trimester allows the baby to move its limbs - the motehr may feel the baby kick as early as week 15 and usually by week 20 (this is called quickening).
There is also considerable development of skin and fat during the second trimester.
- Skin epidermis, a derivative of the peripheral surface ectoderm, is thinly formed over the baby in week 15 and richly vascularised due to vascular endothelial growth factor and angiogenic growth factor. There is differentiation of the epidermis into its five distinct epithelial layers - stratum basalis, stratum spinosum, stratum granulosum, stratum lucidum, and stratum corneum - and loose connective tissue forms the dermal layer underneath. The epidermis and dermis are interdigitated by invaginating epidermal ridges and projecting dermal papillae which form the fingerprints.
- Langerhan cells (antigen presenting cells), Merkel cells (tactile epithelium), and melanocytes (neural crest derivatives producing pigmentation) migrate into the epidermis.
- The ectoderm also forms accessory structures in the skin - e.g. fingernails (week 14/15), hair follicles, and sebaceous and sweat glands.
- In the fifth month of pregnancy (week 17-22), hair follicles form "soft, downy" lanugo hair which covers the foetal skin, head, and forms eyebrows. The vernix caseosa (week 17) covers the skin and protects the foetus from the surrounding amniotic fluid.
- Fat growth initiates as early as week 15 and becomes significant after week 23 - this is essential brown fat oxidation provides thermal insulation and protection from cold environments in the extra-uterine environment.
Respiratory System
The primary function of the respiratory system is to facilitate gaseous exchange between the external environment and the bloodstream, through diffusion across the lung alveoli, in order to oxygenate pulmonary blood via inhalation and remove carbon dioxide via exhalation. In the embryonic and foetal stages of development, the lung is collapsed and its function is replaced by the placental circulation which coordinates the oxygenation of blood and the diffusion of carbon dioxide into the maternal bloodstream. The respiratory system recevies only 7% of foetal blood supply in utero.
Differentiation of the lateral plate mesoderm gives rise to the mesenchyme of the lung; including its connective tissue, the smooth muscle surrounding the airway and blood vessels, endothelial cells which form vasculature, the cartilage, lympathic drainage systems, and mesothelial cells lining the external pleural surface. Early lung morphogenesis in the second trimester is controlled by various cell signalling proteins such as fibroblast growth factor, sonic hedgehog protein, gives rise to a tree-like system of epithelial tubules and sacs surrounded by vasculature.
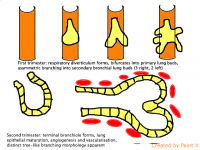
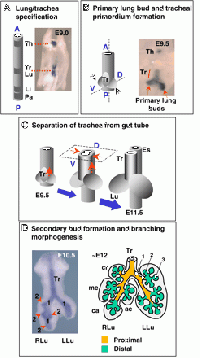
- In the embryonic stage, the endodermal foregut forms a ventral evagination called the respiratory diverticulum which bifurcates into the right and left primary bronchial buds; these structures differentiate into the main bronchi and the respiratory diverticulum forms the trachea and larynx.
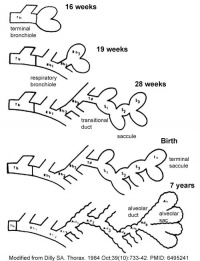
- In the second trimester, the lungs are in the pseudoglandular (weeks 6-16) and undergo expansive branching into bronchopulmonary segments with terminal bronchioles.
- In the canalicular stage (weeks 16-28) of respiratory development, the terminal bronchioles further divide into multiple respiratory bronchioles which form terminal sacs (primitive alveoli) in the early third trimester. The alveoli are canalised by a dense capillary network giving rise to the air-blood tissue barrier.
- Vascular endothelial growth factor and angiogenic growth factor result in the development of respiratory vasculature - a dense network of blood vessels, especially capillaries, form through the recruitment of endothelial cells in close apposition with the lung epithelium. This process continues during the third trimester as the mesenchyme surrounding the alveoli becomes vascularised to facilitate rapid gaseous exchange by diffusion.
- Maturation of lung epithelium initiates in the second trimester through epithelial-to-mesenchymal interactions in the lateral plate mesoderm, resulting in the rudiments of ciliated, secretory, and neuroendocrine epithelium in the proximal bronchioles and Type 1 (squamous supporting cells) and Type 2 (secrete pulmonary surfactant) in the distal alveoli.
Although the lungs are not functional, the foetus may practice breathing by swallowing amniotic fluid which promotes lung growth. Since alveoli development occurs in the late second trimester or early third trimester, pre-term babies born in the second trimester have low concentrations of pulmonary surfactant which is needed to lower the surface tension of alveolar fluid and keep the alveoli patent (open) during inhalation. This can cause pulmonary edema (alveoli filled with proteinaceous fluid) which leads to Respiratory Distress Syndrome as greater intra-thoracic pressure needs to be generated for inhalation. Corticosteroids (cortisol) can be administered to stimulate production of pulonary surfactant.