Trisomy Mosaicism: Difference between revisions
(Created page with "{{Header}} {{Educational Warning}} ==Introduction== thumb|Chromosomes in trisomy 21 This page gives a general introduction to information abou...") |
mNo edit summary |
||
| (11 intermediate revisions by the same user not shown) | |||
| Line 5: | Line 5: | ||
This page gives a general introduction to information about the genetic abnormality of {{trisomy mosaicism}}. The term "trisomy" refers to the abnormal copy number of a specific chromosome in all cells, that is 3 copies instead of 2. The abnormality is identified by the chromosome that is present as 3 copies within the cell. In humans, the most common trisomy is {{trisomy 21}} or Down syndrome. Other identified human trisomies include {{Trisomy 13}}, {{Trisomy 18}} and {{Trisomy X}}. | This page gives a general introduction to information about the genetic abnormality of {{trisomy mosaicism}}. The term "trisomy" refers to the abnormal copy number of a specific chromosome in all cells, that is 3 copies instead of 2. The abnormality is identified by the chromosome that is present as 3 copies within the cell. In humans, the most common trisomy is {{trisomy 21}} or Down syndrome. Other identified human trisomies include {{Trisomy 13}}, {{Trisomy 18}} and {{Trisomy X}}. | ||
In contrast, a "mosaicism" is a rare chromosome disorder characterized by having an extra copy of a chromosome in a proportion, but not all, of a person’s cells. These are examples of a class of very rare and not inherited genetic disorders. | In contrast, a "mosaicism" is a rare chromosome disorder characterized by having an extra copy of a chromosome in a proportion, but not all, of a person’s cells. These are examples of a class of very rare and not inherited genetic disorders. Mosaicism can arise initially meiotically, with a subsequent post-zygotic 'trisomy rescue' event, with adverse outcomes. Some mosaics could also be initially chromosomally normal, and arise purely post-zygotically.{{#pmid:29945889|PMID29945889}} | ||
<br> | <br> | ||
| Line 17: | Line 17: | ||
|-bgcolor="F5FAFF" | |-bgcolor="F5FAFF" | ||
| | | | ||
* | * '''Mosaic trisomy 22 in a 4-year-old boy with congenital heart disease and general hypotrophy: A case report'''{{#pmid:30259573|PMID30259573}} "Trisomy 22 mosaicism is a rare autosomal anomaly with survival compatibility. Recognition of the complete trisomy 22 which is incompatible with life from the mosaic form is critical for genetic counseling. Affected mosaic cases have prevalent clinical presentations such as webbed neck, developmental delay, abnormal ears, cardiac disorders, and microcephaly. Phenotype of these patients is milder than full chromosomal aneuploidy, and the severity of the phenotype depends on the count of trisomic cells. We describe a 4-year-old boy with mosaic trisomy 22 from healthy parents and no family history of any genetic disorders in the pedigree. METHOD AND RESULTS: The patient had determined dysmorphic clinical features including facial asymmetry, cleft palate, gastroenteritis, hydronephrosis, developmental delay, genital anomalies, dysplastic toenails, flattened nasal bridge, congenital heart defect, hearing loss, cryptorchidism, and hypotonic muscle. He is the first reported with hypothyroidism and larynx wall thickness in worldwide and the first with atrial septal defect (ASD) from Iran. Chromosomal analyses using G-banding indicated a de novo Mos 47,XY,+22(6)/46,XY(44) karyotype with no other chromosomal structural changes." | ||
* '''Rare autosomal trisomies: Important and not so rare'''{{#pmid:29956348|PMID29956348}} "Noninvasive prenatal testing (NIPT) can assess chromosomes other than 13, 18, 21, X and Y. These rare autosomal trisomies (RATs) can adversely affect pregnancy outcome. METHODS: A prospective study of NIPT using the Illumina sequencing platform assessing all chromosomes were reported for further management. RESULTS: There were 28 RATs identified in 23 388 samples (one in 835), the most common being trisomy 7 (n = 6), followed by trisomy 16 (n = 4) and trisomy 22 (n = 3). Abnormal outcomes occurred in 16 cases: miscarriage (n = 6), true fetal mosaicism (n = 5), and fetal structural anomaly on ultrasound (n = 5). Growth restriction was seen in eight cases and correlated with very low-pregnancy-associated plasma protein-A levels. Two of the 17 live born babies had a structural anomaly, and one had a phenotype similar to mosaic trisomy 16 despite a normal microarray result. Rare autosomal trisomies are not rare and often associated with poor obstetric outcomes. They should be discussed with the clinician to guide management. Pregnancy outcomes varied by chromosome being generally favourable for some (eg, trisomy 7) and poor for others (eg, trisomy 22). In the presence of a RAT, pregnancy-associated plasma protein-A is predictive of placental dysfunction and fetal growth restriction." | |||
* '''Unexpected finding of uniparental disomy mosaicism in term placentas: Is it a common feature in trisomic placentas?'''{{#pmid:30187503|PMID30187503}} "Non-invasive prenatal testing (NIPT) detects placental chromosome aberrations. When amniocentesis reveals a normal karyotype, confined placental mosaicism (CPM) may be assumed. In order to confirm this, placental cytogenetic studies were performed. METHOD: NIPT was conducted in the course of the Dutch TRIDENT study. Placentas of 10 cases with NIPT results indicating an autosomal trisomy and showing a normal (N = 9) or low mosaic karyotype (N = 1) in amniotic fluid (AF) were investigated. The cytotrophoblast as well as the mesenchymal core of two to four placental chorionic villi biopsies were studied with single nucleotide polymorphism (SNP) array. Clinical outcome data were collected. RESULTS: In 10/10 cases, CPM was proven. In 3/10 cases trisomy/uniparental disomy (UPD)/biparental disomy (BPD) mosaicism was discovered. In 2/3 cases, all three cell lines were present in the placenta, whereas BPD was found in AF. In 1/3 cases trisomy 22/UPD22 was present in AF while trisomy 22/BPD22 mosaicism was found in the placenta. Five of 10 pregnancies were affected with pre-eclampsia, low birth weight, preterm delivery, and/or congenital malformations. CONCLUSION: The presence of trisomy/UPD/BPD mosaicism in 3/10 cases that we investigated proves that trisomic zygote rescue may involve multiple rescue events during early embryogenesis. UPD mosaicism, when present in crucial fetal tissues, may explain the abnormal phenotype in undiagnosed cases." | |||
|} | |} | ||
{| class="wikitable mw-collapsible mw-collapsed" | {| class="wikitable mw-collapsible mw-collapsed" | ||
| Line 27: | Line 29: | ||
Search term: [http://www.ncbi.nlm.nih.gov/pubmed/?term=Trisomy+Mosaicism ''Trisomy Mosaicism''] | Search term: [http://www.ncbi.nlm.nih.gov/pubmed/?term=Trisomy+Mosaicism ''Trisomy Mosaicism''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Trisomy+22+Mosaicism ''Trisomy 22 Mosaicism''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Trisomy+18+Mosaicism ''Trisomy 18 Mosaicism''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Trisomy+17+Mosaicism ''Trisomy 17 Mosaicism''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Trisomy+14+Mosaicism ''Trisomy 14 Mosaicism''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Trisomy+12+Mosaicism ''Trisomy 12 Mosaicism''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Trisomy+9+Mosaicism ''Trisomy 9 Mosaicism''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Trisomy+8+Mosaicism ''Trisomy 8 Mosaicism''] | [http://www.ncbi.nlm.nih.gov/pubmed/?term=Trisomy+2+Mosaicism ''Trisomy 2 Mosaicism''] | ||
|} | |} | ||
| Line 34: | Line 36: | ||
|- | |- | ||
| {{Older papers}} | | {{Older papers}} | ||
* '''Hepatoblastoma in a mosaic trisomy 18 child with hemihypertrophy'''{{#pmid:26795740|PMID26795740}} "To date, there are 12 reported cases of hepatoblastoma in trisomy 18 patients, three of whom had a mosaic chromosome pattern. We report on an 18-month-old child who had hemihypertrophy and developmental delay, was found to have hepatoblastoma on surveillance ultrasound scan, and was subsequently diagnosed with mosaic trisomy 18 on array comparative genomic hybridisation from a peripheral blood sample and molecular cytogenetic analysis of the tumour specimen. Although hemihypertrophy has been associated with mosaic trisomies, there are only a couple of published case reports of hemihypertrophy or asymmetry in mosaic trisomy 18 patients and none in the reported cases of hepatoblastoma in a mosaic trisomy 18 setting. We have reviewed the published case reports of hepatoblastoma in trisomy 18 patients and found that they seem to tolerate the intensive treatment very well if there are no significant comorbidities" | |||
* [https://www.genomes2people.org/research/babyseq/ '''The BabySeq Project'''] "The BabySeq Project is a first-of-its-kind randomized clinical trial designed to examine how best to use genomics in clinical pediatric medicine by creating and safely testing methods for integrating sequencing into the care of newborns." [https://clinicaltrials.gov/ct2/show/NCT02422511 Clinical Trials] | |||
|} | |} | ||
| Line 41: | Line 47: | ||
==Trisomy 18 Mosaicism== | ==Trisomy 18 Mosaicism== | ||
[[File:Mosaic Trisomy 18 hepatoblastoma CT.jpg|thumb|alt=Mosaic Trisomy 18 hepatoblastoma CT|Mosaic Trisomy 18 hepatoblastoma CT{{#pmid:26795740|PMID26795740}}]] | |||
Constellation of congenital abnormalities in an infant: a new syndrome or tissue-specific mosaicism for trisomy 18?{{#pmid:8779322|PMID8779322}} - "Blood lymphocyte and skin fibroblast karyotypes were normal. He died in the neonatal period of postoperative complications. On interphase fluorescence in-situ hybridization (FISH) using autopsy specimens, a significant number of cells in the liver (17%) were trisomic for chromosome 18, compared to normal control liver tissue. However, interphase FISH analyses of blood lymphocytes, skin fibroblasts, and kidney tissue were normal." | |||
{{ | See also {{Trisomy 18}} | ||
==Trisomy 17 Mosaicism== | ==Trisomy 17 Mosaicism== | ||
| Line 54: | Line 62: | ||
==Trisomy 12 Mosaicism== | ==Trisomy 12 Mosaicism== | ||
{{#pmid:11146464|PMID11146464}} - "meiotic origin of the trisomy, maternal meiosis I, was determined. Mosaic aneuploidy was suspected because of pigmentary dysplasia, a frequent but non-specific finding in chromosomal mosaicism. The severe phenotype of this child, who died in infancy with a complex heart malformation, was probably a result of the high percentage of trisomic cells. Cytogenetic and interphase fluorescent in situ hybridization analyses showed a highly variable distribution of aneuploid cells in the nine tissues studied, from none in blood and ovary to 100% in spleen and liver." | Trisomy 12 mosaicism confirmed in multiple organs from a liveborn child.{{#pmid:11146464|PMID11146464}} - "meiotic origin of the trisomy, maternal meiosis I, was determined. Mosaic aneuploidy was suspected because of pigmentary dysplasia, a frequent but non-specific finding in chromosomal mosaicism. The severe phenotype of this child, who died in infancy with a complex heart malformation, was probably a result of the high percentage of trisomic cells. Cytogenetic and interphase fluorescent in situ hybridization analyses showed a highly variable distribution of aneuploid cells in the nine tissues studied, from none in blood and ovary to 100% in spleen and liver." | ||
==Trisomy 10 Mosaicism== | |||
[[File:Trisomy 10 mosaicism karyotype.jpg|thumb|alt=Trisomy 10 mosaicism karyotype|Trisomy 10 mosaicism karyotype{{#pmid:30081864|PMID30081864}}]] | |||
Mosaicism trisomy 10 in a 14-month-old child with additional neurological abnormalities{{#pmid:30081864|PMID30081864}} - "Trisomy 10 is very rarely diagnosed, especially in living persons. Most reports of trisomy 10 pertain to prenatal diagnosis of trisomy 10 in the fetus. In addition, trisomy 10 has been reported as part of partial chromosomal abnormalities in some leukemic cells and tumor specimens. Only 6 cases of mosaicism trisomy 10 have been reported so far. None of these reports pertain to living children with neurological abnormalities." | |||
Cardiovascular Abnormalities | |||
[[File:Trisomy 10 mosaicism cardiovascular abnormalities.jpg|600px]] | |||
'''a''' - patent ductus arteriosus '''b''' - patent foramen ovale | |||
==Trisomy 9 Mosaicism== | ==Trisomy 9 Mosaicism== | ||
| Line 66: | Line 83: | ||
==Trisomy 2 Mosaicism== | ==Trisomy 2 Mosaicism== | ||
{{#pmid:15539872|PMID15539872}} [https://rarediseases.info.nih.gov/diseases/5331/trisomy-2-mosaicism NIH - rare diseases] - "Features of trisomy 2 mosaicism may include intrauterine growth restriction (IUGR), any of various birth defects, distinctive facial features, growth delay, developmental delays, and intellectual disabilities.[1][2] However, children with trisomy 2 mosaicism with no significant medical problems have been reported (although long-term follow-up was not available)." | Prenatal diagnosis of trisomy 2 mosaicism{{#pmid:15539872|PMID15539872}} [https://rarediseases.info.nih.gov/diseases/5331/trisomy-2-mosaicism NIH - rare diseases] - "Features of trisomy 2 mosaicism may include intrauterine growth restriction (IUGR), any of various birth defects, distinctive facial features, growth delay, developmental delays, and intellectual disabilities.[1][2] However, children with trisomy 2 mosaicism with no significant medical problems have been reported (although long-term follow-up was not available)." | ||
==Genetic Abnormality Topics== | ==Genetic Abnormality Topics== | ||
These statistics do not directly relate to trisomy mosaicism frequency, but that of genetic risk related to maternal age for all abnormalities. | |||
===Genetic Risk Maternal Age=== | ===Genetic Risk Maternal Age=== | ||
{{Genetic risk maternal age table}} | {{Genetic risk maternal age table}} | ||
| Line 80: | Line 99: | ||
===Reviews=== | ===Reviews=== | ||
{{#pmid:30012427}} | |||
{{#pmid:28284509}} | |||
===Articles=== | ===Articles=== | ||
Revision as of 15:56, 19 March 2019
| Embryology - 19 Apr 2024 |
|---|
| Google Translate - select your language from the list shown below (this will open a new external page) |
|
العربية | català | 中文 | 中國傳統的 | français | Deutsche | עִברִית | हिंदी | bahasa Indonesia | italiano | 日本語 | 한국어 | မြန်မာ | Pilipino | Polskie | português | ਪੰਜਾਬੀ ਦੇ | Română | русский | Español | Swahili | Svensk | ไทย | Türkçe | اردو | ייִדיש | Tiếng Việt These external translations are automated and may not be accurate. (More? About Translations) |
| Educational Use Only - Embryology is an educational resource for learning concepts in embryological development, no clinical information is provided and content should not be used for any other purpose. |
Introduction
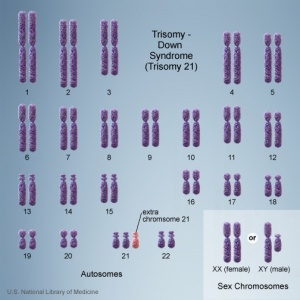
This page gives a general introduction to information about the genetic abnormality of trisomy mosaicism. The term "trisomy" refers to the abnormal copy number of a specific chromosome in all cells, that is 3 copies instead of 2. The abnormality is identified by the chromosome that is present as 3 copies within the cell. In humans, the most common trisomy is Trisomy 21 or Down syndrome. Other identified human trisomies include Trisomy 13, Trisomy 18 and Trisomy X.
In contrast, a "mosaicism" is a rare chromosome disorder characterized by having an extra copy of a chromosome in a proportion, but not all, of a person’s cells. These are examples of a class of very rare and not inherited genetic disorders. Mosaicism can arise initially meiotically, with a subsequent post-zygotic 'trisomy rescue' event, with adverse outcomes. Some mosaics could also be initially chromosomally normal, and arise purely post-zygotically.[1]
Some Recent Findings
|
| More recent papers |
|---|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References
|
| Older papers |
|---|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
|
Trisomy 22 Mosaicism
Rare Disease Database - The characteristic features of mosaic trisomy 22 typically include prenatal and postnatal growth failure or delay, asymmetrical development of the two sides of the body (hemidystrophy), congenital heart defects. While some patients with mosaic trisomy 22 have abnormal cognitive development, normal development has been documented for some children."
Trisomy 18 Mosaicism
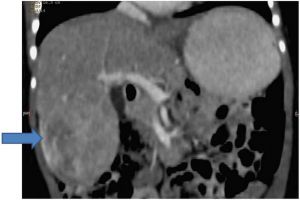
Constellation of congenital abnormalities in an infant: a new syndrome or tissue-specific mosaicism for trisomy 18?[6] - "Blood lymphocyte and skin fibroblast karyotypes were normal. He died in the neonatal period of postoperative complications. On interphase fluorescence in-situ hybridization (FISH) using autopsy specimens, a significant number of cells in the liver (17%) were trisomic for chromosome 18, compared to normal control liver tissue. However, interphase FISH analyses of blood lymphocytes, skin fibroblasts, and kidney tissue were normal."
See also Trisomy 18
Trisomy 17 Mosaicism
NIH - rare diseases - "Some cases of trisomy 17 mosaicism detected during pregnancy have been confirmed in the baby after birth. The symptoms reported include: developmental delays, body asymmetry, slow growth, and cerebellar hypoplasia. Again, signs and symptoms may vary in these individuals depending on which cells and how many cells contain an extra chromosome 17."
Trisomy 14 Mosaicism
Rare Disease Database - "The disorder may be characterized by growth delays before birth (intrauterine growth retardation); failure to grow and gain weight at the expected rate (failure to thrive) during infancy; delays in the acquisition of skills requiring the coordination of mental and physical abilities (psychomotor delays); and mental retardation. Affected infants also have distinctive abnormalities of the head and facial (craniofacial) region, such as a prominent forehead; deeply set, widely spaced eyes; a broad nasal bridge; and low-set, malformed ears. Additional craniofacial abnormalities may include an unusually small lower jaw (micrognathia); a large mouth and thick lips; and incomplete closure or abnormally high arching of the roof of the mouth (palate). Many affected infants also have structural malformations of the heart (e.g., tetralogy of Fallot). In some cases, additional physical abnormalities may also be present."
Trisomy 12 Mosaicism
Trisomy 12 mosaicism confirmed in multiple organs from a liveborn child.[7] - "meiotic origin of the trisomy, maternal meiosis I, was determined. Mosaic aneuploidy was suspected because of pigmentary dysplasia, a frequent but non-specific finding in chromosomal mosaicism. The severe phenotype of this child, who died in infancy with a complex heart malformation, was probably a result of the high percentage of trisomic cells. Cytogenetic and interphase fluorescent in situ hybridization analyses showed a highly variable distribution of aneuploid cells in the nine tissues studied, from none in blood and ovary to 100% in spleen and liver."
Trisomy 10 Mosaicism
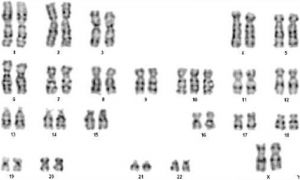
Mosaicism trisomy 10 in a 14-month-old child with additional neurological abnormalities[8] - "Trisomy 10 is very rarely diagnosed, especially in living persons. Most reports of trisomy 10 pertain to prenatal diagnosis of trisomy 10 in the fetus. In addition, trisomy 10 has been reported as part of partial chromosomal abnormalities in some leukemic cells and tumor specimens. Only 6 cases of mosaicism trisomy 10 have been reported so far. None of these reports pertain to living children with neurological abnormalities."
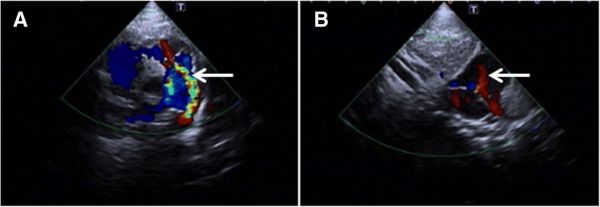
Cardiovascular Abnormalities
a - patent ductus arteriosus b - patent foramen ovale
Trisomy 9 Mosaicism
Rare Disease Database - "Associated symptoms and findings may vary greatly in range and severity, depending on the percentage of cells with the extra chromosome. However, common features include growth deficiency before birth (intrauterine growth restriction or IUGR); structural malformations of the heart that are present at birth (congenital heart defects); and/or distinctive differences in the shape of the skull and facial (craniofacial) region, such as a sloping forehead, a bulbous nose, short eyelid folds (palpebral fissures), deeply set eyes, and/or low-set ears. The syndrome may also be characterized by musculoskeletal, genital, kidney (renal), and/or additional physical anomalies. Intellectual disability is common and varies in severity."
Trisomy 8 Mosaicism
NIH - rare diseases - "The signs and symptoms vary, but may include distinctive facial features; intellectual disability; and joint, kidney, cardiac, and skeletal abnormalities. Males are more frequently affected than females."
Trisomy 2 Mosaicism
Prenatal diagnosis of trisomy 2 mosaicism[9] NIH - rare diseases - "Features of trisomy 2 mosaicism may include intrauterine growth restriction (IUGR), any of various birth defects, distinctive facial features, growth delay, developmental delays, and intellectual disabilities.[1][2] However, children with trisomy 2 mosaicism with no significant medical problems have been reported (although long-term follow-up was not available)."
Genetic Abnormality Topics
These statistics do not directly relate to trisomy mosaicism frequency, but that of genetic risk related to maternal age for all abnormalities.
Genetic Risk Maternal Age
Table Data[10][11][12]
| |||
References
- ↑ Griffin DK & Ogur C. (2018). Chromosomal analysis in IVF: just how useful is it?. Reproduction , 156, F29-F50. PMID: 29945889 DOI.
- ↑ Kalayinia S, Shahani T, Biglari A, Maleki M, Rokni-Zadeh H, Razavi Z & Mahdieh N. (2019). Mosaic trisomy 22 in a 4-year-old boy with congenital heart disease and general hypotrophy: A case report. J. Clin. Lab. Anal. , 33, e22663. PMID: 30259573 DOI.
- ↑ Scott F, Bonifacio M, Sandow R, Ellis K, Smet ME & McLennan A. (2018). Rare autosomal trisomies: Important and not so rare. Prenat. Diagn. , 38, 765-771. PMID: 29956348 DOI.
- ↑ Van Opstal D, Diderich KEM, Joosten M, Govaerts LCP, Polak J, Boter M, Saris JJ, Cheung WY, van Veen S, van de Helm R, Go ATJI, Knapen MFCM, Papatsonis DNM, Dijkman A, de Vries F, Galjaard RH, Hoefsloot LH & Srebniak MI. (2018). Unexpected finding of uniparental disomy mosaicism in term placentas: Is it a common feature in trisomic placentas?. Prenat. Diagn. , 38, 911-919. PMID: 30187503 DOI.
- ↑ 5.0 5.1 Ahmad N, Wheeler K, Stewart H & Campbell C. (2016). Hepatoblastoma in a mosaic trisomy 18 child with hemihypertrophy. BMJ Case Rep , 2016, . PMID: 26795740 DOI.
- ↑ Shashi V, Golden WL, von Kap-Herr C & Wilson WG. (1996). Constellation of congenital abnormalities in an infant: a new syndrome or tissue-specific mosaicism for trisomy 18?. Am. J. Med. Genet. , 62, 38-41. PMID: 8779322 <38::AID-AJMG8>3.0.CO;2-S DOI.
- ↑ DeLozier-Blanchet CD, Roeder E, Denis-Arrue R, Blouin JL, Low J, Fisher J, Scharnhorst D & Curry CJ. (2000). Trisomy 12 mosaicism confirmed in multiple organs from a liveborn child. Am. J. Med. Genet. , 95, 444-9. PMID: 11146464
- ↑ 8.0 8.1 Gao Y, Ma YC, Ju YH & Li YN. (2018). Mosaicism trisomy 10 in a 14-month-old child with additional neurological abnormalities: case report and literature review. BMC Pediatr , 18, 266. PMID: 30081864 DOI.
- ↑ Sifakis S, Velissariou V, Papadopoulou E, Petersen MB & Koumantakis E. (2004). Prenatal diagnosis of trisomy 2 mosaicism: a case report. Fetal. Diagn. Ther. , 19, 488-90. PMID: 15539872 DOI.
- ↑ Hook EB. (1981). Rates of chromosome abnormalities at different maternal ages. Obstet Gynecol , 58, 282-5. PMID: 6455611
- ↑ Hook EB, Cross PK & Schreinemachers DM. (1983). Chromosomal abnormality rates at amniocentesis and in live-born infants. JAMA , 249, 2034-8. PMID: 6220164
- ↑ Schreinemachers DM, Cross PK & Hook EB. (1982). Rates of trisomies 21, 18, 13 and other chromosome abnormalities in about 20 000 prenatal studies compared with estimated rates in live births. Hum. Genet. , 61, 318-24. PMID: 6891368
Reviews
Mavridi A, Ntali G, Theodora M, Stamatelopoulos K & Michala L. (2018). A Spontaneous Pregnancy in a Patient with Turner Syndrome with 45,X/47,XXX Mosaicism: A Case Report and Review of the Literature. J Pediatr Adolesc Gynecol , 31, 651-654. PMID: 30012427 DOI.
Grati FR, Malvestiti F, Branca L, Agrati C, Maggi F & Simoni G. (2017). Chromosomal mosaicism in the fetoplacental unit. Best Pract Res Clin Obstet Gynaecol , 42, 39-52. PMID: 28284509 DOI.
Articles
Search Pubmed
Search Pubmed: genetic developmental abnormality
Terms
- anaphase - (Greek, ana = up, again) Cell division term referring to the fourth mitotic stage, where the paired chromatids now separate and migrate to spindle poles. This is followed by telophase.
- Mitosis Phases: prophase - prometaphase - metaphase - anaphase - telophase
- anaphase B - Cell division term referring to the part of anaphase during which the poles of the mitotic spindle move apart. (More? Cell Division - Mitosis)
- aneuploidy - Genetic term used to describe an abnormal number of chromosomes mainly (90%) due to chromosome malsegregation mechanisms in maternal meiosis I.
- disomy - Genetic term referring to the presence of two chromosomes of a homologous pair in a cell, as in diploid. See chromosomal number genetic disorders uniparental disomy and aneuploidy. Humans have pairs usually formed by one chromosome from each parent.
- meiosis I (MI) The first part of meiosis resulting in separation of homologous chromosomes, in humans producing two haploid cells (N chromosomes, 23), a reductional division.
- Meiosis I: Prophase I - Metaphase I - Anaphase I - Telophase I
- meiosis II - (MII) The second part of meiosis. In male human spermatogenesis, producing of four haploid cells (23 chromosomes, 1N) from the two haploid cells (23 chromosomes, 1N), each of the chromosomes consisting of two sister chromatids produced in meiosis I. In female human oogenesis, only a single haploid cell (23 chromosomes, 1N) is produced.
- Meiosis II: Prophase II - Metaphase II - Anaphase II - Telophase II
- prometaphase - (Greek, pro = before) Cell division term referring to the second mitotic stage, when the nuclear envelope breaks down into vesicles. Microtubules then extend from the centrosomes at the spindle poles (ends) and reach the chromosomes. This is followed by metaphase.
- Philadelphia chromosome - (Philadelphia translocation) Genetic term referring to a chromosomal abnormality resulting from a reciprocal translocation between chromosome 9 and 22 (t(9;22)(q34;q11)). This is associated with the disease chronic myelogenous leukemia (CML).
- prophase - (Greek, pro = before) Cell division term referring to the first mitotic stage, when the diffusely stained chromatin resolves into discrete chromosomes, each consisting of two chromatids joined together at the centromere.
- telophase - Cell division term referring to the fifth mitotic stage, where the vesicles of the nuclear envelope reform around the daughter cells, the nucleoli reappear and the chromosomes unfold to allow gene expression to begin. This phase overlaps with cytokinesis, the division of the cell cytoplasm.
- trisomy mosaicism - a rare chromosome disorder characterized by having an extra copy of a chromosome in a proportion, but not all, of a person’s cells.
- uniparental disomy - Genetic term referring to cells containing both copies of a homologous pair of chromosomes from one parent and none from the other parent.
| Cell Division Terms (expand to view) | ||
|---|---|---|
meiosis | mitosis
| ||
|
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- Australia NHMRC - Genetics in Family Medicine: The Australian Handbook for General Practitioners Testing and pregnancy PDF (2007)
- Online Mendelian Inheritance in Man
- NHGRI Catalog of Published Genome-Wide Association Studies | PDF
- Genome-Wide Associations (GWA) Karyogram
- Idiogram Album David Adler
- NSW Centre for Genetics Education - Fact Sheets
- The BabySeq Project | Clinical Trials - "The BabySeq Project is a first-of-its-kind randomized clinical trial designed to examine how best to use genomics in clinical pediatric medicine by creating and safely testing methods for integrating sequencing into the care of newborns."
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 19) Embryology Trisomy Mosaicism. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Trisomy_Mosaicism
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G