Talk:Birth - Stillbirth and Perinatal Death: Difference between revisions
No edit summary |
No edit summary |
||
| Line 1: | Line 1: | ||
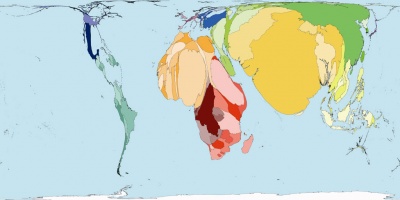
==Stillbirth and Perinatal Death== | |||
[[File:World neonatal death.jpg|center|400px]] | |||
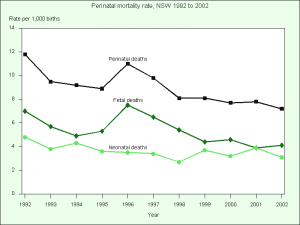
[[File:NSW_perinatal_mortality_rate.png|thumb|NSW perinatal mortality rate]] | |||
Perinatal period is the early postnatal period relating to the birth, statistically it includes the period up to 7 days after birth. Neonatal period is the four weeks/month after birth. [http://embryology.med.unsw.edu.au/Child/birth7.htm Stillbirth and Perinatal Death] | |||
In New South Wales (2002) 613 perinatal deaths were reported. | |||
* Unexplained antepartum deaths: 26.3% of perinatal deaths (or 39.2% of stillbirths) | |||
* Spontaneous preterm labour: 20.6% (less than 37 weeks gestation) | |||
* Congenital abnormality: 16.8% | |||
* Antepartum haemorrhage: 8.5% | |||
* Specific perinatal conditions: 7.3%, of which twin-twin transfusion accounted for 2.3% of deaths | |||
* Hypertension (high blood pressure): 5.5% | |||
* Perinatal infection: 4.4% | |||
* Maternal disease: 4.4% | |||
* Hypoxic peripartum death: 3.8% | |||
Neonatal deaths (four weeks/month after birth) | |||
* extreme prematurity was most common cause (39.6%) | |||
* congenital abnormality (19.3%) | |||
* neurological disease (13.4%) | |||
* cardio-respiratory conditions (11.9%) | |||
* infection (8.4%) | |||
Data: Report of the New South Wales Chief Health Officer, 2004 accessed 19Oct05 | |||
http://www.ncbi.nlm.nih.gov/pubmed/19888051 | http://www.ncbi.nlm.nih.gov/pubmed/19888051 | ||
Revision as of 09:33, 20 June 2010
Stillbirth and Perinatal Death
Perinatal period is the early postnatal period relating to the birth, statistically it includes the period up to 7 days after birth. Neonatal period is the four weeks/month after birth. Stillbirth and Perinatal Death
In New South Wales (2002) 613 perinatal deaths were reported.
- Unexplained antepartum deaths: 26.3% of perinatal deaths (or 39.2% of stillbirths)
- Spontaneous preterm labour: 20.6% (less than 37 weeks gestation)
- Congenital abnormality: 16.8%
- Antepartum haemorrhage: 8.5%
- Specific perinatal conditions: 7.3%, of which twin-twin transfusion accounted for 2.3% of deaths
- Hypertension (high blood pressure): 5.5%
- Perinatal infection: 4.4%
- Maternal disease: 4.4%
- Hypoxic peripartum death: 3.8%
Neonatal deaths (four weeks/month after birth)
- extreme prematurity was most common cause (39.6%)
- congenital abnormality (19.3%)
- neurological disease (13.4%)
- cardio-respiratory conditions (11.9%)
- infection (8.4%)
Data: Report of the New South Wales Chief Health Officer, 2004 accessed 19Oct05
http://www.ncbi.nlm.nih.gov/pubmed/19888051
Experts developed evidence-based characteristics of maternal, fetal, and placental conditions to attribute a condition as a cause of stillbirth. These conditions include infection, maternal medical conditions, antiphospholipid syndrome, heritable thrombophilias, red cell alloimmunization, platelet alloimmunization, congenital malformations, chromosomal abnormalities including confined placental mosaicism, fetomaternal hemorrhage, placental and umbilical cord abnormalities including vasa previa and placental abruption, complications of multifetal gestation, and uterine complications. In all cases, owing to lack of sufficient knowledge about disease states and normal development, there will be a degree of uncertainty regarding whether a specific condition was indeed the cause of death.
Obstet Gynecol Clin North Am. 1992 Jun;19(2):265-80. Neonatal morbidity and mortality secondary to premature rupture of membranes. Klein JM.
Department of Pediatrics, University of Iowa, Iowa City. Abstract PROM is one of the most common complications of pregnancy that has a major impact on neonatal mortality and morbidity. The occurrence of PROM is either directly or indirectly responsible for a large number of premature births and the concomitant mortality and morbidity associated with preterm delivery. PROM turns a pregnancy into a high-risk situation and increases the need for neonatal resuscitation in the delivery room. The incidence of neonatal sepsis increases with PROM, but the overall outcome of the neonate, even with surfactant therapy, is still primarily dependent on the gestational age at the time of delivery. This is most relevant between 24 and 27 weeks' gestation. During this 3-week interval, survival improves by almost 2% for each additional day of in utero maturation (i.e., from 35 to 75%). Thus the benefit to the fetus of prolonging the pregnancy in cases of PROM is immensely worthwhile and should be aggressively pursued as long as there is no significant increase in maternal morbidity.
PMID: 1630737 [PubMed - indexed for MEDLINE]