|
|
| Line 135: |
Line 135: |
| ===Acrosome=== | | ===Acrosome=== |
| Derived from the Golgi apparatus in conjunction with transient specialized bundles of microtubules (manchette). | | Derived from the Golgi apparatus in conjunction with transient specialized bundles of microtubules (manchette). |
| | |
| | ===Nucleus=== |
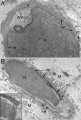
| | The spermatozoa nucleus is compressed and the nuclear DNA chromatin is tightly packed by spermatozoa-specific protamines. |
| | |
| | {| |
| | ! Human Spermatozoa EMRef name=PMID24592371><pubmed>24592371</pubmed>| [http://www.advbiores.net/article.asp?issn=2277-9175;year=2014;volume=3;issue=1;spage=24;epage=24;aulast=Iranpour Adv Biomed Res.]<ref> |
| | |- |
| | | [[File:Human_spermatozoa_nucleus_EM01.jpg|300px]] |
| | | [[File:Human_spermatozoa_nucleus_EM01.jpg|300px]] |
| | |- |
| | | Normal human spermatozoa |
| | | Abnormal human spermatozoa |
| | |} |
| ===Axoneme=== | | ===Axoneme=== |
|
| |
|
Revision as of 09:43, 17 September 2014
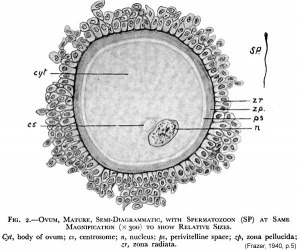
Introduction
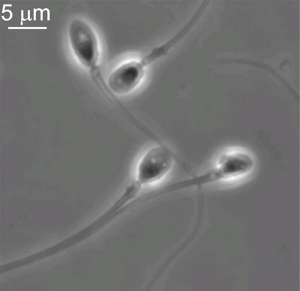
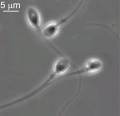
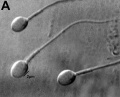
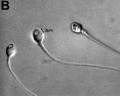
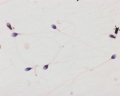
Human spermatozoa (light microscope)

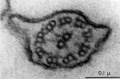
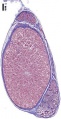
Human spermatozoa (electron microscope)
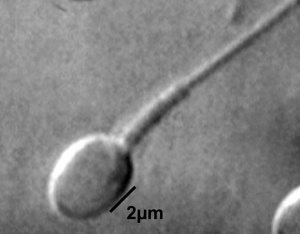
Single human spermatozoa
[1]This page introduces spermatogenesis the development of spermatozoa, the male haploid gamete cell. In humans at puberty, spermatozoa are produced by spermatogonia meiosis in the seminiferous tubules of the testis (male gonad). A second process of spermiogenesis leads to change in cellular organisation and shape before release into the central lumen of the seminiferous tubule. This overall process has been variously divided into specific identifiable stages in different species: 6 in human, 12 in mouse, and 14 in rat. Structurally, the seminiferous tubule epithelium is divided into a basal and an apical (adluminal) compartment by the blood–testis barrier (BTB). (More? Testis Development).
A second unique feature of this process is that during mitosis and meiosis the dividing cells remain connected by cytoplasmic bridges as the cells do not complete cytokinesis. This cellular organization is described as a syncytium, only ending with release into the central lumen of the seminiferous tubule, when the cell cytoplasm is discarded.
- In a healthy adult human male it takes about 48 days from meiosis to produce a mature spermatozoa, and he produces somewhere between 45 to 207 million spermatozoa per day, or about 2,000 every second. (More? Statistics)
Medicine Practical | Fertilization | Category:Spermatozoa
Some Recent Findings
- Morphometric dimensions of the human sperm head depend on the staining method used.[2] "Different staining techniques change the morphometric dimensions of the human sperm head, probably due to the fact that either the fixatives or stains are not iso-osmotic in relation to human semen."
- Redistribution of nuclear pores[3] "The appearance of an electron-lucent nuclear region surrounded by the nascent redundant nuclear envelope indicated a pathway for transporting degradation products through the nuclear pores to the residual cytoplasm. The packaging of the nuclear pores into the redundant nuclear envelope suggests that they play a role in late stages of sperm maturation or in fertilization, as most other unnecessary organelles of sperm are discarded during spermiogenesis or during shedding of the cytoplasmic droplet."
- Calpain modulates capacitation and acrosome reaction[4] "We found that calpain-1 is relocated and translocated from cytoplasm to plasma membrane during capacitation, where it could cleave spectrin, one of the proteins of the plasma membrane-associated cytoskeleton and facilitates acrosome reaction."
- Spermatocytes cultured in simulated microgravity[5] "A critical step of spermatogenesis is the entry of mitotic spermatogonia into meiosis. Progresses on these topics are hampered by the lack of an in vitro culture system allowing mouse spermatogonia differentiation and entry into meiosis. Previous studies have shown that mouse pachytene spermatocytes cultured in simulated microgravity (SM) undergo a spontaneous meiotic progression. Here we report that mouse mitotic spermatogonia cultured under SM with a rotary cell culture system (RCCS) enter into meiosis in the absence of any added exogenous factor or contact with somatic cells."
|
| More recent papers
|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
- This search now requires a manual link as the original PubMed extension has been disabled.
- The displayed list of references do not reflect any editorial selection of material based on content or relevance.
- References also appear on this list based upon the date of the actual page viewing.
References listed on the rest of the content page and the associated discussion page (listed under the publication year sub-headings) do include some editorial selection based upon both relevance and availability.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References
Search term: Spermatozoa Development
<pubmed limit=5>Spermatozoa Development</pubmed>
|
Movies
Seminiferous Tubule
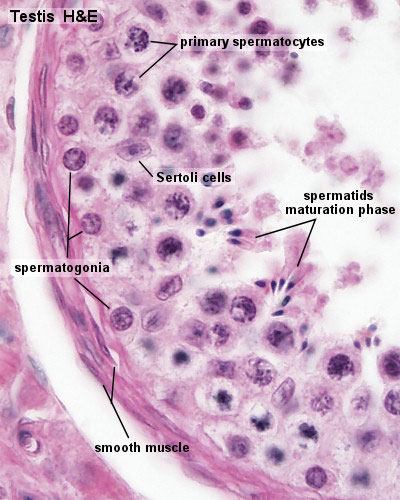 Adult Seminiferous tubule showing spermatozoa developmental stages |
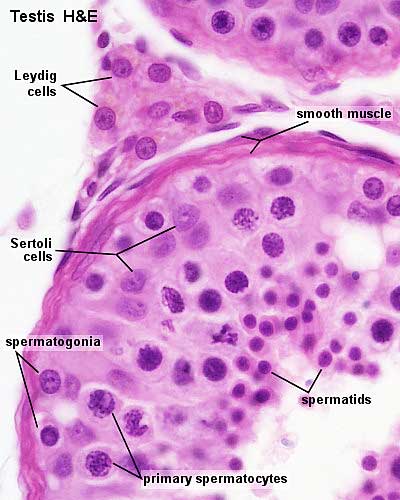 Seminiferous tubule cross-section and supporting cells |
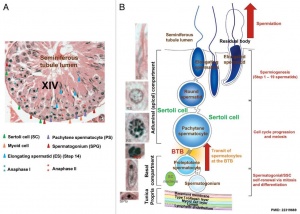
Rat Spermatogenesis cartoon
[6]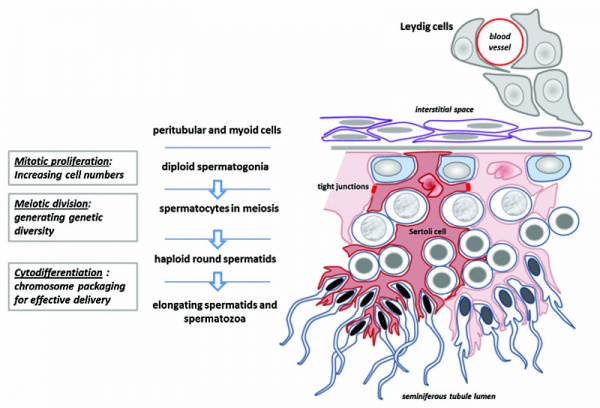
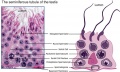
Seminiferous tubule cartoon[7]
- Spermatogonia - are the first cells of spermatogenesis
- Primary spermatocyte - large, enter the prophase of the first meiotic division
- Secondary spermatocytes - small, complete the second meiotic division
- Spermatid] - immature spermatozoa
- Spermatozoa - differentiated gamete
- Spermatozoa development: primordial germ cell - spermatogonia - primary spermatocyte - secondary spermatocytes - spermatid - spermatozoa
- Links: Testis Histology | Testis Development
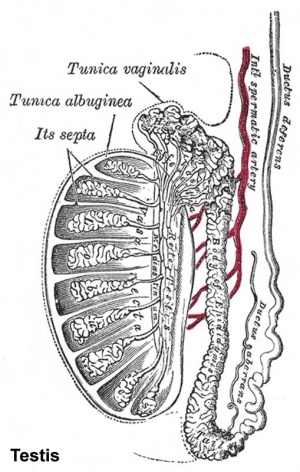
Spermatozoa Structure
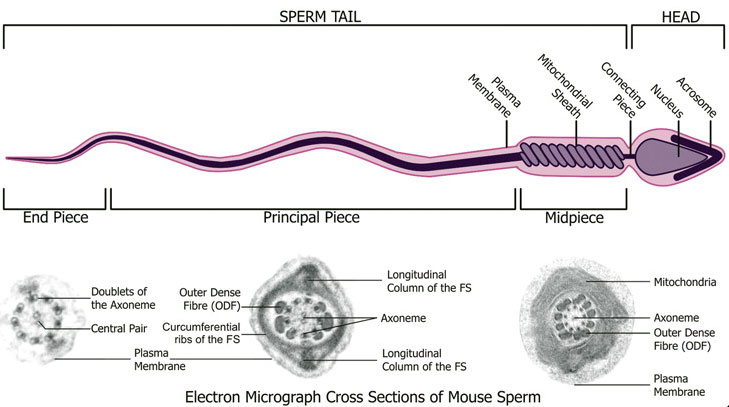
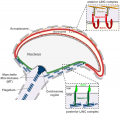
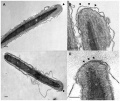
Spermatozoa (mouse) cross-sections of tail (EM) and diagram[8]
Adult Seminiferous tubule showing spermatozoa developmental stages
Seminiferous tubule cross-section and supporting cells
Single human spermatozoon
Human vacuolated spermatozoon
Historic EM spermatozoon tail
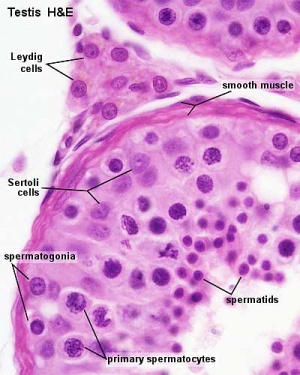
Other main cell types seen in the histological sections
- Sertoli cells- support cells seen within the seminiferous tubule
- Interstitial cells or Leydig cells - produce hormone
- Smooth muscle - surround seminiferous tubule and contribute to contraction of the tubule
Human Spermatozoa Development
- Spermatogenesis process of spermatagonia mature into spermatazoa (sperm).
- Continuously throughout life occurs in the seminiferous tubules in the male gonad- testis (plural testes).
- At puberty spermatagonia activate and proliferate (mitosis).
- about 48 days from entering meiosis until morphologically mature spermatozoa
- about 64 days to complete spermatogenesis, depending reproduction time of spermatogonia
- follicle stimulating hormone (FSH) - stimulates the spermatogenic epithelium
- luteinizing-hormone (LH) - stimulates testosterone production by Leydig cells
Spermatogonia
- spermatogonial stem cells (SSCs) diploid progenitor for spermatozoa.
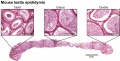
- 1963 Clermont identified spermatogonia as Ap (pale) and Ad (dark) on basis of light microscope staining.[9]
- 60 years - Ap spermatogonia number decrease
- 80 years - Ad spermatogonia number decrease
Sertoli Cells
Named after Enrico Sertoli (1842 - 1910) an Italian (Milan) physiologist and histologist.
- sustentacular cells of seminiferous tubules.
- form a “blood-testis” barrier through junctional complexes
- separate the intra-tubular germinal epithelium into two compartments
- basal compartment - cells are exposed to the extra-tubular environment
- luminal compartment - cells are subject to an environment produced by Sertoli cells and germ cells
Spermatazoa Components
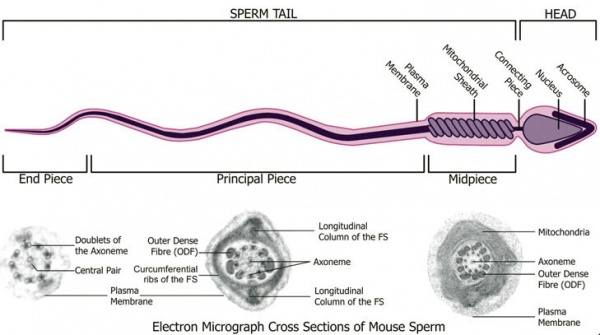
Spermatozoa (mouse) cross-sections of tail (EM) and diagram[8]
Acroplaxome
This structure forms the acrosome plate with intermediate filament bundles of the marginal ring at the leading edge of the acrosome.
Acrosome
Derived from the Golgi apparatus in conjunction with transient specialized bundles of microtubules (manchette).
Nucleus
The spermatozoa nucleus is compressed and the nuclear DNA chromatin is tightly packed by spermatozoa-specific protamines.
Adv Biomed Res.Cite error: Closing </ref> missing for <ref> tag More recently, there have been several different ways of characterising the morphology of human spermatozoa developed mainly in relation to clinical reproductive technologies.
Integrated Sperm Analysis System (ISAS)
A semi-automated computer-aided system that measures spermatozoa head parameters length (L), width (W), area (A), perimeter (P), acrosomal area (Ac), and the derived values L/W and P/A. 20852650
- For each man a homogeneous population of distributions characterized seminal spermatozoa (7,942 cells: median values L 4.4 μm, W 2.8 μm, A 9.8 μm(2), P 12.5 μm, Ac 47.5%, L/W 1.57, P/A 1.27)
- Different men could have spermatozoa of significantly different dimensions.
- Head dimensions for swim-up spermatozoa from different men (4 812 cells) were similar to those in semen, differing only by 2%-5%.
- The values of L, W and L/W fell within the limits given by the World Health Organization (WHO).
- A subpopulation of 404 spermatozoa considered to fit the stringent criteria of WHO 'normal' seminal spermatozoa from both semen and swim-up were characterized by median values (and 95% confidence intervals) of L, 4.3 μm (3.8-4.9), W, 2.9 μm (2.6-3.3), A, 10.2 μm(2) (8.5-12.2), P, 12.4 μm (11.3-13.9), Ac, 49% (36-60), L/W, 1.49 (1.32-1.67) and P/A, 1.22 (1.11-1.35). These median values fall within the 95th centile confidence limits given by WHO, but the confidence intervals for L and W were larger.
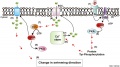
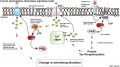
Spermatozoa Chemotaxis
Chemotaxis was first identified in marine species[10], which still remains today as a model system. While the signals may differ, the overall effect is to chemically attack spermatozoa to the oocyte to allow fertilisation to occur.
The following series of 2011 research articles have identified the spermatozoa calcium channel protein (CatSper) as the progesterone activated pathway involved in capacitated spermatozoa chemotaxis.
- The CatSper channel mediates progesterone-induced Ca2+ influx in human sperm[11]
- Progesterone activates the principal Ca2+ channel of human sperm[12]
- Spermatozoa hyperactivated motility[13]
- part of the chemotactic response of human spermatozoa.
- initiated by elevation of intracellular Ca2+
- non-linear with increased velocity and a large amplitude of lateral head displacement
- intense flagellar whiplash movements.
|
|
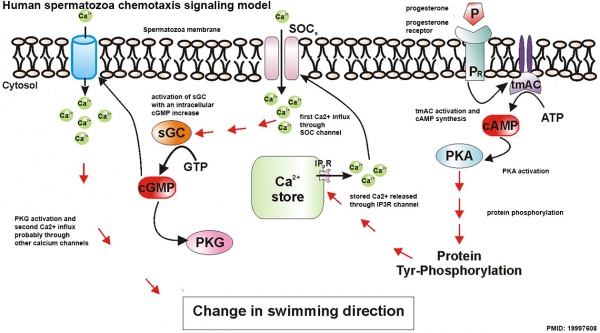
Human Spermatozoa Chemotaxis Model (2009)[14]
See also 2008 review.[15]
Human Spermatazoa Statistics
The following data is based normal human male values for reproductive ages between 20 to 50 years[16]:
- 45 to 207 million spermatozoa produced per day within the two testes
- 2,000 spermatozoa approx per second each day
- Compare this to adult human red blood cell production of about 250,000 million RBCs per day
- 182 million spermatozoa stored (epididymal reserves) up to per epididymis
- 440 million spermatozoa extragonadal stored
- 225 million extragonadal spermatozoa in the ductuli deferentia and caudae epididymides per ejaculation
- 23 million spermatozoa approx (all animals) per gram testicular parenchyma per day
- Transit times
- 0.72 day spermatozoa through the caput
- 0.71 days spermatozoa through the corpus
- 1.76 days spermatozoa through the cauda epididymidis
Histology
Human spermatozoa, x20, Papanicolaou stain
Human spermatozoa, x40, Papanicolaou stain
Human spermatozoa, x100, Papanicolaou stain
Papanicolaou stain (Papanicolaou's stain, Pap stain) a multichromatic (five dyes) staining histological technique developed by George Papanikolaou, used to differentiate cells in smear preparations of various bodily secretions.
- Links: Testis Histology | Histology Stains
Male Abnormalities
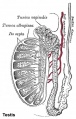
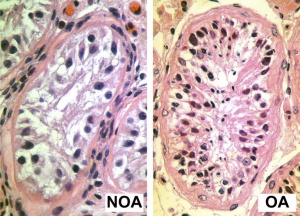 Human Seminiferious Tubule - Non-obstructive azoospermia and Obstructive azoospermia
| Classification
|
Count (Millions/mL)
|
| Azoospermia
|
0
|
| Severe oligozoospermia
|
less than 1
|
| Moderate oligozoospermia
|
1-5
|
| Mild oligozoospermia
|
5-20
|
| Normal
|
greater than 20
|
Oligospermia
(Low Sperm Count) less than 20 million sperm after 72 hour abstinence from sex
Azoospermia
(Absent Sperm) blockage of duct network
Immotile Cilia Syndrome
Lack of sperm motility
Additional Images
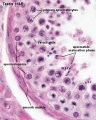
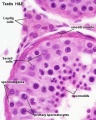
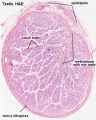
Testis histology, young and mature - H&E
Human testis NANOG expression
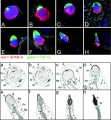
Human spermatozoa acrosomal protein SP-10 PMID 17012309
Human spermatid electron micrograph PMID 17012309
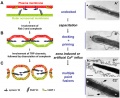
Model capacitation-induced acrosome docking to sperm membrane PMID 19758979
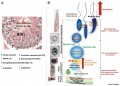
Mouse spermiogenesis model PMID 19758979
Mouse- seminiferous tubule histology PMID 19758979
Mouse- epididymis histology
Mouse- spermatozoa EM and diagram
Mouse - Spatiotemporal progression of annulus during mouse spermiogenesis
Mouse spermatogonia meiotic prophase I stages
Rat Spermatogenesis cartoon PMID 22319669
EM - Capacitation alters the ultrastructure of the apical head and the acrosome of boar sperm
Human spermatozoa - phospholipase C zeta localization PMID 22428063
Chemotaxis Model PMID 19997608
Labeled Chemotaxis Model PMID 19997608
References
Journals
- Spermatogenesis | PubMed - Spermatogenesis "Spermatogenesis is a new quarterly, peer-reviewed journal that will publish high-quality articles covering all aspects of spermatogenesis."
- WHO. WHO Laboratory Manual for the Examination and Processing of Human Semen. 5th ed. Geneva, Switzerland: World Health Organization; 2010. Online PDF
Reviews
<pubmed>20388168</pubmed>
<pubmed>20364093</pubmed>
<pubmed>20144980</pubmed>
<pubmed>19941293</pubmed>
<pubmed>19941292</pubmed>
<pubmed>17988206</pubmed>
<pubmed>12672126</pubmed>
<pubmed>11105904</pubmed>| PDF
Articles
NCBI Bookshelf
MBoC - Sperm | MBoC - Highly simplified drawing of a cross-section of a seminiferous tubule in a mammalian testis | MBoC - Cytoplasmic bridges in developing sperm cells and their precursors
Search
Terms
- asthenozoospermia - (asthenospermia) Term for reduced sperm motility and can be the cause of male infertility.
- blood-testis barrier - (BTB) Formed by tight junctions, basal ectoplasmic specializations, desmosome-like junctions and gap junctions between adjacent Sertoli cells near the basement membrane of the seminiferous epithelium.
- Leydig cell - (interstitial cell) Male gonad (testis) cell which secrete the androgen testosterone, beginning in the fetus. These cells are named after Franz von Leydig (1821 - 1908) a German scientist who histologically described these cells.
- sperm annulus - (Jensen's ring; Latin, annulus = ring) A region of the mammalian sperm flagellum connecting the midpiece and the principal piece. The annulus is a septin-based structure formed from SEPT1, 4, 6, 7 and 12. Septins are polymerizing GTPases that can act as a scaffold forming hetero-oligomeric filaments required for cytokinesis and other cell cycle roles.
- spermatogenesis - (Greek, genesis = origin, creation, generation) The term used to describe the process of diploid spermatagonia division and differentiation to form haploid spermatazoa within the testis (male gonad). The process includes the following cellular changes: meiosis, reoorganization of DNA, reduction in DNA content, reorganization of cellular organelles, morphological changes (cell shape). The final process of change in cell shape is also called spermiogenesis.
- spermatogenesis - (Greek, genesis = origin, creation, generation) The maturation process of the already haploid spermatazoa into the mature sperm shape and organization. This process involves reorganization of cellular organelles (endoplasmic reticulum, golgi apparatus, mitochondria), cytoskeletal changes (microtubule organization) and morphological changes (cell shape, acrosome and tail formation).
- spermatogonia - The cells located in the seminiferous tubule adjacent to the basal membrane that either divide and separate to renew the stem cell population, or they divide and stay together as a pair (Apr spermatogonia) connected by an intercellular cytoplasmic bridge to differentiate and eventually form spermatazoa.
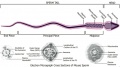
- spermatozoa head - Following spermiogenesis, the first region of the spermatozoa containing the haploid nucleus and acrosome. In humans, it is a flattened structure (5 µm long by 3 µm wide) with the posterior part of nuclear membrane forming the basal plate region. The human spermatozoa is about 60 µm long, actively motile and divided into 3 main regions (head, neck and tail).
- spermatozoa neck - Following spermiogenesis, the second region of the spermatozoa attached to basal plate, transverse oriented centriole, contains nine segmented columns of fibrous material, continue as outer dense fibres in tail. In humans, it forms a short structure (1 µm). The human spermatozoa is about 60 µm long, actively motile and divided into 3 main regions (head, neck and tail).
- spermatozoa tail - Following spermiogenesis, the third region of the spermatozoa that has a (head, neck and tail). The tail is also divided into 3 structural regions a middle piece, a principal piece and an end piece. In humans: the middle piece (5 µm long) is formed by axonema and dense fibres surrounded by mitochondria; the principal piece (45 µm long) fibrous sheath interconnected by regularly spaced circumferential hoops; the final end piece (5 µm long) has an axonema surrounded by small amount of cytoplasm and plasma membrane.
- spermatogonial stem cells - (SSCs) The spermatagonia cells located beside the seminiferous tubule basal membrane that either divide and separate to renew the stem cell population, or they divide and stay together as a pair (Apr spermatogonia) connected by an intercellular cytoplasmic bridge to differentiate and eventually form spermatazoa.
- sperm protein 56 - A component of the spermatozoa acrosomal matrix released to the sperm surface during capacitation.
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- World Health Organization - WHO Laboratory Manual for the Examination and Processing of Human Semen. 5th ed. Geneva, Switzerland: World Health Organization; 2010. Online PDF
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 20) Embryology Spermatozoa Development. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Spermatozoa_Development
- What Links Here?
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G
|